User login
Late-week discharges to home after CRC surgery prone to readmission
BOSTON – The day of the week a patient is discharged from the hospital may have an impact the likelihood of readmission.
Patients discharged home from the hospital on a Thursday after colorectal cancer surgery are more likely to be readmitted within 30 days than those discharged on any other day of the week, investigators found.
In contrast, there were no significant day-dependent differences in readmission rates among patients discharged to a skilled nursing facility or acute rehabilitation program, although patients admitted to clinical facilities had higher overall readmission rates, reported Anna Gustin and coinvestigators at the Levine Cancer Institute at the Carolinas Medical Center in Charlotte, N.C.
“For a patient discharged on a Thursday, if you’re going to get an infection, it’s going to be probably during the weekend, when it’s difficult to contact your primary physician, and when other resources are not as readily available,” said Ms. Gustin, who conducts epidemiologic research at Levine Cancer Center and is also a pre-med student and Japanese major at Wake Forest University in Winston-Salem, N.C.
In a study presented in a poster session at the annual Society of Surgical Oncology Cancer Symposium, Ms. Gustin and her coauthors looked at factors influencing readmission rates among patients undergoing surgery for primary, nonmetastatic colorectal cancer resections.
They drew on the to evaluate outcomes for 93,04 SEER-(Surveillance, Epidemiology, and End Results) Medicare database seven patients aged 66 years and older treated for primary colorectal cancer from 1998 through 2009.
They looked at potential contributing factors such as patient demographics, socioeconomic status, length of stay, days of admission and discharge, and discharge setting (home or clinical facility).
They use multivariate logistic regression models to analyze readmission rates at 14 and 30 days after initial discharge.
Focusing on home discharges, they found that as the week progressed, there was a significant likelihood that a patient discharged home would be readmitted (P less then .001 by chi-square and Cochran-Armitage tests). As noted before, the highest rate of readmission was for patients discharged on Thursday, at 12.4%, compared with 10.1% for patients discharged on Sunday, the discharge day least likely to be associated with rehospitalization.
In multivariate analysis, factors significantly associated with risk for 30-day readmission included male vs. female (hazard ratio, 1.16), black vs. other race (HR, 1.22), length of stay 5, 6-7, or 8-10 vs. 12 or more days (HR, 0.48, 0.59, 0.77, respectively), Charlson comorbidity index score 0, 1 or 3 vs. 3 (HR, 0.59, 0.73, 0.82, respectively), and home discharge vs. other (HR, 0.66; all above comparisons significant as shown by 95% confidence intervals).
The authors concluded that although home discharge itself reduces the likelihood of readmission, “improvements in preparing patients for discharge to home are needed. Additional outpatient interventions could rescue patients from readmission.”
They also suggested reexamining staffing policies and weekend availability of resources for patients, and call for addressing disparities in readmissions based on race, sex, length of stay, and comorbidities.
The study was internally supported. The authors reported having no relevant disclosures.
BOSTON – The day of the week a patient is discharged from the hospital may have an impact the likelihood of readmission.
Patients discharged home from the hospital on a Thursday after colorectal cancer surgery are more likely to be readmitted within 30 days than those discharged on any other day of the week, investigators found.
In contrast, there were no significant day-dependent differences in readmission rates among patients discharged to a skilled nursing facility or acute rehabilitation program, although patients admitted to clinical facilities had higher overall readmission rates, reported Anna Gustin and coinvestigators at the Levine Cancer Institute at the Carolinas Medical Center in Charlotte, N.C.
“For a patient discharged on a Thursday, if you’re going to get an infection, it’s going to be probably during the weekend, when it’s difficult to contact your primary physician, and when other resources are not as readily available,” said Ms. Gustin, who conducts epidemiologic research at Levine Cancer Center and is also a pre-med student and Japanese major at Wake Forest University in Winston-Salem, N.C.
In a study presented in a poster session at the annual Society of Surgical Oncology Cancer Symposium, Ms. Gustin and her coauthors looked at factors influencing readmission rates among patients undergoing surgery for primary, nonmetastatic colorectal cancer resections.
They drew on the to evaluate outcomes for 93,04 SEER-(Surveillance, Epidemiology, and End Results) Medicare database seven patients aged 66 years and older treated for primary colorectal cancer from 1998 through 2009.
They looked at potential contributing factors such as patient demographics, socioeconomic status, length of stay, days of admission and discharge, and discharge setting (home or clinical facility).
They use multivariate logistic regression models to analyze readmission rates at 14 and 30 days after initial discharge.
Focusing on home discharges, they found that as the week progressed, there was a significant likelihood that a patient discharged home would be readmitted (P less then .001 by chi-square and Cochran-Armitage tests). As noted before, the highest rate of readmission was for patients discharged on Thursday, at 12.4%, compared with 10.1% for patients discharged on Sunday, the discharge day least likely to be associated with rehospitalization.
In multivariate analysis, factors significantly associated with risk for 30-day readmission included male vs. female (hazard ratio, 1.16), black vs. other race (HR, 1.22), length of stay 5, 6-7, or 8-10 vs. 12 or more days (HR, 0.48, 0.59, 0.77, respectively), Charlson comorbidity index score 0, 1 or 3 vs. 3 (HR, 0.59, 0.73, 0.82, respectively), and home discharge vs. other (HR, 0.66; all above comparisons significant as shown by 95% confidence intervals).
The authors concluded that although home discharge itself reduces the likelihood of readmission, “improvements in preparing patients for discharge to home are needed. Additional outpatient interventions could rescue patients from readmission.”
They also suggested reexamining staffing policies and weekend availability of resources for patients, and call for addressing disparities in readmissions based on race, sex, length of stay, and comorbidities.
The study was internally supported. The authors reported having no relevant disclosures.
BOSTON – The day of the week a patient is discharged from the hospital may have an impact the likelihood of readmission.
Patients discharged home from the hospital on a Thursday after colorectal cancer surgery are more likely to be readmitted within 30 days than those discharged on any other day of the week, investigators found.
In contrast, there were no significant day-dependent differences in readmission rates among patients discharged to a skilled nursing facility or acute rehabilitation program, although patients admitted to clinical facilities had higher overall readmission rates, reported Anna Gustin and coinvestigators at the Levine Cancer Institute at the Carolinas Medical Center in Charlotte, N.C.
“For a patient discharged on a Thursday, if you’re going to get an infection, it’s going to be probably during the weekend, when it’s difficult to contact your primary physician, and when other resources are not as readily available,” said Ms. Gustin, who conducts epidemiologic research at Levine Cancer Center and is also a pre-med student and Japanese major at Wake Forest University in Winston-Salem, N.C.
In a study presented in a poster session at the annual Society of Surgical Oncology Cancer Symposium, Ms. Gustin and her coauthors looked at factors influencing readmission rates among patients undergoing surgery for primary, nonmetastatic colorectal cancer resections.
They drew on the to evaluate outcomes for 93,04 SEER-(Surveillance, Epidemiology, and End Results) Medicare database seven patients aged 66 years and older treated for primary colorectal cancer from 1998 through 2009.
They looked at potential contributing factors such as patient demographics, socioeconomic status, length of stay, days of admission and discharge, and discharge setting (home or clinical facility).
They use multivariate logistic regression models to analyze readmission rates at 14 and 30 days after initial discharge.
Focusing on home discharges, they found that as the week progressed, there was a significant likelihood that a patient discharged home would be readmitted (P less then .001 by chi-square and Cochran-Armitage tests). As noted before, the highest rate of readmission was for patients discharged on Thursday, at 12.4%, compared with 10.1% for patients discharged on Sunday, the discharge day least likely to be associated with rehospitalization.
In multivariate analysis, factors significantly associated with risk for 30-day readmission included male vs. female (hazard ratio, 1.16), black vs. other race (HR, 1.22), length of stay 5, 6-7, or 8-10 vs. 12 or more days (HR, 0.48, 0.59, 0.77, respectively), Charlson comorbidity index score 0, 1 or 3 vs. 3 (HR, 0.59, 0.73, 0.82, respectively), and home discharge vs. other (HR, 0.66; all above comparisons significant as shown by 95% confidence intervals).
The authors concluded that although home discharge itself reduces the likelihood of readmission, “improvements in preparing patients for discharge to home are needed. Additional outpatient interventions could rescue patients from readmission.”
They also suggested reexamining staffing policies and weekend availability of resources for patients, and call for addressing disparities in readmissions based on race, sex, length of stay, and comorbidities.
The study was internally supported. The authors reported having no relevant disclosures.
Key clinical point: Patients discharged home on a Thursday following surgery for primary colorectal cancer are more likely to be readmitted with 30 days than are patients discharged home on any other day of the week.
Major finding: The highest rate of readmission was for patients discharged on Thursday, at 12.4%, compared with lowest rate of 10.1% for patients discharged on Sunday.
Data source: Retrospective SEER-Medicare database review of records on 93,047 patients treated for colorectal cancer.
Disclosures: The study was internally supported. The authors reported having no relevant disclosures.
Neoadjuvant chemo reduces extent of axillary dissection in some breast cancers
BOSTON – The majority of patients with hormone receptor–negative breast cancer in the United States get chemotherapy in the adjuvant setting, but neoadjuvant chemotherapy is gaining in use, and is associated with a higher likelihood of breast-conserving surgery for some women with advanced disease, as well as less extensive axillary node dissection.
A review of data on more than 130,000 patients with breast tumors negative for both estrogen and progesterone receptors (ER–/PR–) showed that among patients with clinical stage T3 disease, 26% of those who had received neoadjuvant chemotherapy were able to have breast-conserving surgery, compared with 20% of patients who had received adjuvant chemotherapy, reported Dr. Carlos A. Puig and his colleagues from the Mayo Clinic in Rochester, Minn.
“Patients treated with neoadjuvant chemotherapy have less extensive axillary surgery and a lower rate of nodal positivity,” he added at the annual Society of Surgical Oncology Cancer Symposium.
The data showed that nearly a third of all patients with clinically node-positive disease (cN1-3) who received neoadjuvant chemotherapy had pathologically node-negative disease at the end of therapy.
The aggressive biology of ER–/PR– tumors makes them suitable targets for chemotherapy in the neoadjuvant setting, Dr. Puig said. Overall survival among patients with ER–/PR– who receive neoadjuvant chemotherapy is comparable to that of patients who receive chemotherapy in the adjuvant setting. Neoadjuvant regimens can also downstage tumors before surgery, and a pathologic complete response to chemotherapy delivered prior to surgery is prognostic for outcomes.
Trends in chemotherapy
Dr. Puig and his colleagues combed through the National Cancer Data Base, looking for trends in national practice patterns of use of neoadjuvant chemotherapy in ER–/PR– breast cancer from 2004 through 2012.
They identified a total of 108,128 patients with invasive ER–/PR– breast cancer who received adjuvant chemotherapy, and 24,848 who received neoadjuvant chemo; an additional 43,969 patients who did not receive chemotherapy were excluded from the analysis.
Factors significantly associated with the choice to administer neoadjuvant chemotherapy included age younger than 50, no comorbidities vs. one or two comorbidities on the Charlson/Deyo index, academic/research center vs. community cancer program, higher clinical T stage, and higher clinical N stage.
There was a gradual increase in the use of neoadjuvant chemotherapy over time, from 14.2% in 2004 to 22.3% of all patients in 2012 (P less than .001).
The overall breast-conserving surgery rates were lower among patients who had chemotherapy in the neoadjuvant setting – 33.2% vs. 54.7% (P less than .001). The rates of conservative surgery increased over time, from 32% in 2004 to 36% in 2012 (P less than .001), but decreased over the same period in patients who had adjuvant chemotherapy, from 58% to 51%, respectively.
In a breakdown of surgery type by clinical T stage, mastectomy was more frequently performed in patients who had undergone neoadjuvant treatment, compared with adjuvant therapy, except for stage T3 disease. A higher percentage of those with T3 tumors who had neoadjuvant therapy had breast-conserving surgery in comparison with women who had T3 tumors and adjuvant therapy (26.2% vs. 20.2%, respectively; P less than .001).
To identify the extent of axillary surgery, the authors considered one to five nodes removed to be a surrogate for sentinel lymph node biopsy, and six or more nodes as a surrogate for axillary lymph node dissection.
They found that among patients with clinical stage N1 through N3 who received neoadjuvant chemotherapy, 31.8% converted to pathologically node-negative status.
Dr. Puig noted that the study was limited by the retrospective design and the lack of data on HER2 receptor status, making it impossible to distinguish between ER–/PR– and triple-negative tumors. In addition, they did not have data on genetic testing that could affect surgical choices, such as the presence of BRCA1 or BRCA2.
Following Dr. Puig’s presentation, Dr. Monica Morrow, chief of breast surgery at Memorial Sloan-Kettering Cancer Center, New York, commented that the study put together “patients in whom we would consider there to be an absolute indication for neoadjuvant chemotherapy – meaning T4, N2-N3 – and patients where it’s optional.” The study results suggested that not all patients who should receive neoadjuvant therapy were getting it “which is a little disturbing,” Dr. Morrow said.
She also noted that the decrease in the use of axillary lymph node dissection began prior to publication of studies suggesting that it might be safe to do so.
Dr. Puig and Dr. Morrow had no relevant disclosures.
BOSTON – The majority of patients with hormone receptor–negative breast cancer in the United States get chemotherapy in the adjuvant setting, but neoadjuvant chemotherapy is gaining in use, and is associated with a higher likelihood of breast-conserving surgery for some women with advanced disease, as well as less extensive axillary node dissection.
A review of data on more than 130,000 patients with breast tumors negative for both estrogen and progesterone receptors (ER–/PR–) showed that among patients with clinical stage T3 disease, 26% of those who had received neoadjuvant chemotherapy were able to have breast-conserving surgery, compared with 20% of patients who had received adjuvant chemotherapy, reported Dr. Carlos A. Puig and his colleagues from the Mayo Clinic in Rochester, Minn.
“Patients treated with neoadjuvant chemotherapy have less extensive axillary surgery and a lower rate of nodal positivity,” he added at the annual Society of Surgical Oncology Cancer Symposium.
The data showed that nearly a third of all patients with clinically node-positive disease (cN1-3) who received neoadjuvant chemotherapy had pathologically node-negative disease at the end of therapy.
The aggressive biology of ER–/PR– tumors makes them suitable targets for chemotherapy in the neoadjuvant setting, Dr. Puig said. Overall survival among patients with ER–/PR– who receive neoadjuvant chemotherapy is comparable to that of patients who receive chemotherapy in the adjuvant setting. Neoadjuvant regimens can also downstage tumors before surgery, and a pathologic complete response to chemotherapy delivered prior to surgery is prognostic for outcomes.
Trends in chemotherapy
Dr. Puig and his colleagues combed through the National Cancer Data Base, looking for trends in national practice patterns of use of neoadjuvant chemotherapy in ER–/PR– breast cancer from 2004 through 2012.
They identified a total of 108,128 patients with invasive ER–/PR– breast cancer who received adjuvant chemotherapy, and 24,848 who received neoadjuvant chemo; an additional 43,969 patients who did not receive chemotherapy were excluded from the analysis.
Factors significantly associated with the choice to administer neoadjuvant chemotherapy included age younger than 50, no comorbidities vs. one or two comorbidities on the Charlson/Deyo index, academic/research center vs. community cancer program, higher clinical T stage, and higher clinical N stage.
There was a gradual increase in the use of neoadjuvant chemotherapy over time, from 14.2% in 2004 to 22.3% of all patients in 2012 (P less than .001).
The overall breast-conserving surgery rates were lower among patients who had chemotherapy in the neoadjuvant setting – 33.2% vs. 54.7% (P less than .001). The rates of conservative surgery increased over time, from 32% in 2004 to 36% in 2012 (P less than .001), but decreased over the same period in patients who had adjuvant chemotherapy, from 58% to 51%, respectively.
In a breakdown of surgery type by clinical T stage, mastectomy was more frequently performed in patients who had undergone neoadjuvant treatment, compared with adjuvant therapy, except for stage T3 disease. A higher percentage of those with T3 tumors who had neoadjuvant therapy had breast-conserving surgery in comparison with women who had T3 tumors and adjuvant therapy (26.2% vs. 20.2%, respectively; P less than .001).
To identify the extent of axillary surgery, the authors considered one to five nodes removed to be a surrogate for sentinel lymph node biopsy, and six or more nodes as a surrogate for axillary lymph node dissection.
They found that among patients with clinical stage N1 through N3 who received neoadjuvant chemotherapy, 31.8% converted to pathologically node-negative status.
Dr. Puig noted that the study was limited by the retrospective design and the lack of data on HER2 receptor status, making it impossible to distinguish between ER–/PR– and triple-negative tumors. In addition, they did not have data on genetic testing that could affect surgical choices, such as the presence of BRCA1 or BRCA2.
Following Dr. Puig’s presentation, Dr. Monica Morrow, chief of breast surgery at Memorial Sloan-Kettering Cancer Center, New York, commented that the study put together “patients in whom we would consider there to be an absolute indication for neoadjuvant chemotherapy – meaning T4, N2-N3 – and patients where it’s optional.” The study results suggested that not all patients who should receive neoadjuvant therapy were getting it “which is a little disturbing,” Dr. Morrow said.
She also noted that the decrease in the use of axillary lymph node dissection began prior to publication of studies suggesting that it might be safe to do so.
Dr. Puig and Dr. Morrow had no relevant disclosures.
BOSTON – The majority of patients with hormone receptor–negative breast cancer in the United States get chemotherapy in the adjuvant setting, but neoadjuvant chemotherapy is gaining in use, and is associated with a higher likelihood of breast-conserving surgery for some women with advanced disease, as well as less extensive axillary node dissection.
A review of data on more than 130,000 patients with breast tumors negative for both estrogen and progesterone receptors (ER–/PR–) showed that among patients with clinical stage T3 disease, 26% of those who had received neoadjuvant chemotherapy were able to have breast-conserving surgery, compared with 20% of patients who had received adjuvant chemotherapy, reported Dr. Carlos A. Puig and his colleagues from the Mayo Clinic in Rochester, Minn.
“Patients treated with neoadjuvant chemotherapy have less extensive axillary surgery and a lower rate of nodal positivity,” he added at the annual Society of Surgical Oncology Cancer Symposium.
The data showed that nearly a third of all patients with clinically node-positive disease (cN1-3) who received neoadjuvant chemotherapy had pathologically node-negative disease at the end of therapy.
The aggressive biology of ER–/PR– tumors makes them suitable targets for chemotherapy in the neoadjuvant setting, Dr. Puig said. Overall survival among patients with ER–/PR– who receive neoadjuvant chemotherapy is comparable to that of patients who receive chemotherapy in the adjuvant setting. Neoadjuvant regimens can also downstage tumors before surgery, and a pathologic complete response to chemotherapy delivered prior to surgery is prognostic for outcomes.
Trends in chemotherapy
Dr. Puig and his colleagues combed through the National Cancer Data Base, looking for trends in national practice patterns of use of neoadjuvant chemotherapy in ER–/PR– breast cancer from 2004 through 2012.
They identified a total of 108,128 patients with invasive ER–/PR– breast cancer who received adjuvant chemotherapy, and 24,848 who received neoadjuvant chemo; an additional 43,969 patients who did not receive chemotherapy were excluded from the analysis.
Factors significantly associated with the choice to administer neoadjuvant chemotherapy included age younger than 50, no comorbidities vs. one or two comorbidities on the Charlson/Deyo index, academic/research center vs. community cancer program, higher clinical T stage, and higher clinical N stage.
There was a gradual increase in the use of neoadjuvant chemotherapy over time, from 14.2% in 2004 to 22.3% of all patients in 2012 (P less than .001).
The overall breast-conserving surgery rates were lower among patients who had chemotherapy in the neoadjuvant setting – 33.2% vs. 54.7% (P less than .001). The rates of conservative surgery increased over time, from 32% in 2004 to 36% in 2012 (P less than .001), but decreased over the same period in patients who had adjuvant chemotherapy, from 58% to 51%, respectively.
In a breakdown of surgery type by clinical T stage, mastectomy was more frequently performed in patients who had undergone neoadjuvant treatment, compared with adjuvant therapy, except for stage T3 disease. A higher percentage of those with T3 tumors who had neoadjuvant therapy had breast-conserving surgery in comparison with women who had T3 tumors and adjuvant therapy (26.2% vs. 20.2%, respectively; P less than .001).
To identify the extent of axillary surgery, the authors considered one to five nodes removed to be a surrogate for sentinel lymph node biopsy, and six or more nodes as a surrogate for axillary lymph node dissection.
They found that among patients with clinical stage N1 through N3 who received neoadjuvant chemotherapy, 31.8% converted to pathologically node-negative status.
Dr. Puig noted that the study was limited by the retrospective design and the lack of data on HER2 receptor status, making it impossible to distinguish between ER–/PR– and triple-negative tumors. In addition, they did not have data on genetic testing that could affect surgical choices, such as the presence of BRCA1 or BRCA2.
Following Dr. Puig’s presentation, Dr. Monica Morrow, chief of breast surgery at Memorial Sloan-Kettering Cancer Center, New York, commented that the study put together “patients in whom we would consider there to be an absolute indication for neoadjuvant chemotherapy – meaning T4, N2-N3 – and patients where it’s optional.” The study results suggested that not all patients who should receive neoadjuvant therapy were getting it “which is a little disturbing,” Dr. Morrow said.
She also noted that the decrease in the use of axillary lymph node dissection began prior to publication of studies suggesting that it might be safe to do so.
Dr. Puig and Dr. Morrow had no relevant disclosures.
Key clinical point: Neoadjuvant chemotherapy can benefit some patients with advanced hormone receptor–negative breast cancer.
Major finding: Among patients with cT3 disease, 26% who had neoadjuvant chemotherapy were able to have breast-conserving surgery, compared with 20% of patients who had received adjuvant chemotherapy.
Data source: Retrospective review of data on 132,976 patients with invasive ER–/PR– breast cancer.
Disclosures: Dr. Puig and Dr. Morrow had no relevant disclosures.
Hold rectal surgery decision until neoadjuvant chemo is done
BOSTON – Good results come to those who wait, suggest the findings of a study of optimal timing of surgical decisions in patients with advanced stage cancers in the distal rectum.
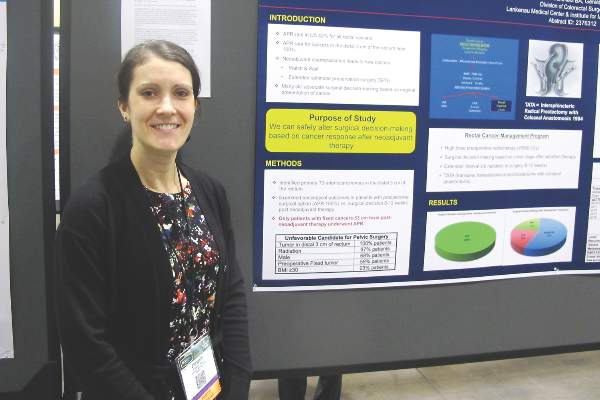
When surgeons waited 8 to 12 weeks after the completion of neoadjuvant chemoradiation to decide whether to proceed with radical sphincter preservation surgery (SPS) or abdominoperineal resection (APR) in patients with T3 cancers of the distal third of the rectum, they were able to avoid creating a colostomy with no adverse oncologic outcomes in 79% of patients, reported Dr. Elizabeth A. Myers and her colleagues from the Lankenau Medical Center and Institute for Medical Research in Wynnewood, Pennsylvania.
“An interesting thing, but still quite controversial, is the timing of when you do surgery,” Dr. Myers said in an interview during a poster session at the annual Society of Surgical Oncology Cancer Symposium.
“There is a large school of thought that still believes you should base your surgical plan on the tumor at its presentation, versus making the decision once the patient has undergone neoadjuvant chemoradiation treatment. The purpose of our study is to show with our data that you can safely alter your decision making based on what the cancer presents as following neoadjuvant chemoradiation,” she said.
The investigators looked at 192 consecutive patients with T3 cancers of the distal third of the rectum who were included in a prospectively maintained database. At the time of presentation, all of the patients would have met criteria for requiring APR and colostomy, due to unfavorable factors for pelvic surgery such as prior radiation (97%), male sex (68%), preoperative fixed tumor (59%), or obesity (23%).
The patients underwent neoadjuvant radiation given at a mean of dose of 5,580 cGy, consisting of a 4,500 cGy standard dose and a 1,080 cGy boost to the area of tumor. Most (87%) also received concurrent 5-fluorauracil-based chemotherapy.
“We have found that this helps to downgrade the tumor quite well,” Dr. Myers said.
Following the completion of therapy, they waited for 8 to 12 additional weeks before planning surgery to allow for the maximum benefit of radiation.
All patients, except those who at the end of neoadjuvant chemotherapy still had a fixed cancer at the 3 cm level or below, were offered SPS. The mean time from completion of chemotherapy to surgery was 11 weeks.
Of the 192 patients, 41 underwent APR, 109 had radical SPS, including 107 receiving transanal transabdominal proctocolectomy with coloanal anastomosis (TATA), and 2 receiving low anterior resection. The remaining patients had local excision with either a transanal technique (TAE; 15 patients) or transanal endoscopic microsurgery (TEM, 27 patients).
After a mean follow-up of 55.4 months (range, 1-242 months) the 5-year stoma-free survival rate was 79%. Kaplan-Meier 5-year actuarial survival rates were 98% for all patients who underwent radical SPS, 100% for those who had local excision with TEM, 82% for those who had local excision with TAE (combined SPS procedures, 95%), and 72% for patients who underwent APR.
Local recurrences occurred in 6.6% of all patients who underwent SPS, compared with 7.3% of those who underwent APR. Distant metastases occurred in 22.5% and 24.4%, respectively.
“Holding surgical decision-making until after completion of neoadjuvant therapy allows for increased sphincter preservation with good oncologic outcomes in rectal cancer patients,” the investigators concluded.
BOSTON – Good results come to those who wait, suggest the findings of a study of optimal timing of surgical decisions in patients with advanced stage cancers in the distal rectum.
When surgeons waited 8 to 12 weeks after the completion of neoadjuvant chemoradiation to decide whether to proceed with radical sphincter preservation surgery (SPS) or abdominoperineal resection (APR) in patients with T3 cancers of the distal third of the rectum, they were able to avoid creating a colostomy with no adverse oncologic outcomes in 79% of patients, reported Dr. Elizabeth A. Myers and her colleagues from the Lankenau Medical Center and Institute for Medical Research in Wynnewood, Pennsylvania.
“An interesting thing, but still quite controversial, is the timing of when you do surgery,” Dr. Myers said in an interview during a poster session at the annual Society of Surgical Oncology Cancer Symposium.
“There is a large school of thought that still believes you should base your surgical plan on the tumor at its presentation, versus making the decision once the patient has undergone neoadjuvant chemoradiation treatment. The purpose of our study is to show with our data that you can safely alter your decision making based on what the cancer presents as following neoadjuvant chemoradiation,” she said.
The investigators looked at 192 consecutive patients with T3 cancers of the distal third of the rectum who were included in a prospectively maintained database. At the time of presentation, all of the patients would have met criteria for requiring APR and colostomy, due to unfavorable factors for pelvic surgery such as prior radiation (97%), male sex (68%), preoperative fixed tumor (59%), or obesity (23%).
The patients underwent neoadjuvant radiation given at a mean of dose of 5,580 cGy, consisting of a 4,500 cGy standard dose and a 1,080 cGy boost to the area of tumor. Most (87%) also received concurrent 5-fluorauracil-based chemotherapy.
“We have found that this helps to downgrade the tumor quite well,” Dr. Myers said.
Following the completion of therapy, they waited for 8 to 12 additional weeks before planning surgery to allow for the maximum benefit of radiation.
All patients, except those who at the end of neoadjuvant chemotherapy still had a fixed cancer at the 3 cm level or below, were offered SPS. The mean time from completion of chemotherapy to surgery was 11 weeks.
Of the 192 patients, 41 underwent APR, 109 had radical SPS, including 107 receiving transanal transabdominal proctocolectomy with coloanal anastomosis (TATA), and 2 receiving low anterior resection. The remaining patients had local excision with either a transanal technique (TAE; 15 patients) or transanal endoscopic microsurgery (TEM, 27 patients).
After a mean follow-up of 55.4 months (range, 1-242 months) the 5-year stoma-free survival rate was 79%. Kaplan-Meier 5-year actuarial survival rates were 98% for all patients who underwent radical SPS, 100% for those who had local excision with TEM, 82% for those who had local excision with TAE (combined SPS procedures, 95%), and 72% for patients who underwent APR.
Local recurrences occurred in 6.6% of all patients who underwent SPS, compared with 7.3% of those who underwent APR. Distant metastases occurred in 22.5% and 24.4%, respectively.
“Holding surgical decision-making until after completion of neoadjuvant therapy allows for increased sphincter preservation with good oncologic outcomes in rectal cancer patients,” the investigators concluded.
BOSTON – Good results come to those who wait, suggest the findings of a study of optimal timing of surgical decisions in patients with advanced stage cancers in the distal rectum.
When surgeons waited 8 to 12 weeks after the completion of neoadjuvant chemoradiation to decide whether to proceed with radical sphincter preservation surgery (SPS) or abdominoperineal resection (APR) in patients with T3 cancers of the distal third of the rectum, they were able to avoid creating a colostomy with no adverse oncologic outcomes in 79% of patients, reported Dr. Elizabeth A. Myers and her colleagues from the Lankenau Medical Center and Institute for Medical Research in Wynnewood, Pennsylvania.
“An interesting thing, but still quite controversial, is the timing of when you do surgery,” Dr. Myers said in an interview during a poster session at the annual Society of Surgical Oncology Cancer Symposium.
“There is a large school of thought that still believes you should base your surgical plan on the tumor at its presentation, versus making the decision once the patient has undergone neoadjuvant chemoradiation treatment. The purpose of our study is to show with our data that you can safely alter your decision making based on what the cancer presents as following neoadjuvant chemoradiation,” she said.
The investigators looked at 192 consecutive patients with T3 cancers of the distal third of the rectum who were included in a prospectively maintained database. At the time of presentation, all of the patients would have met criteria for requiring APR and colostomy, due to unfavorable factors for pelvic surgery such as prior radiation (97%), male sex (68%), preoperative fixed tumor (59%), or obesity (23%).
The patients underwent neoadjuvant radiation given at a mean of dose of 5,580 cGy, consisting of a 4,500 cGy standard dose and a 1,080 cGy boost to the area of tumor. Most (87%) also received concurrent 5-fluorauracil-based chemotherapy.
“We have found that this helps to downgrade the tumor quite well,” Dr. Myers said.
Following the completion of therapy, they waited for 8 to 12 additional weeks before planning surgery to allow for the maximum benefit of radiation.
All patients, except those who at the end of neoadjuvant chemotherapy still had a fixed cancer at the 3 cm level or below, were offered SPS. The mean time from completion of chemotherapy to surgery was 11 weeks.
Of the 192 patients, 41 underwent APR, 109 had radical SPS, including 107 receiving transanal transabdominal proctocolectomy with coloanal anastomosis (TATA), and 2 receiving low anterior resection. The remaining patients had local excision with either a transanal technique (TAE; 15 patients) or transanal endoscopic microsurgery (TEM, 27 patients).
After a mean follow-up of 55.4 months (range, 1-242 months) the 5-year stoma-free survival rate was 79%. Kaplan-Meier 5-year actuarial survival rates were 98% for all patients who underwent radical SPS, 100% for those who had local excision with TEM, 82% for those who had local excision with TAE (combined SPS procedures, 95%), and 72% for patients who underwent APR.
Local recurrences occurred in 6.6% of all patients who underwent SPS, compared with 7.3% of those who underwent APR. Distant metastases occurred in 22.5% and 24.4%, respectively.
“Holding surgical decision-making until after completion of neoadjuvant therapy allows for increased sphincter preservation with good oncologic outcomes in rectal cancer patients,” the investigators concluded.
FROM SSO 2016
Key clinical point: Waiting 8-12 weeks following neoadjuvant chemoradiation in patients with T3 distal rectal cancers improves chances for sphincter preservation.
Major finding: The 5-year stoma-free survival rate was 79% in patients initially considered candidates for APR and colostomy.
Data source: Retrospective review of 192 patients in a prospectively maintained database.
Disclosures: The study was internally supported. Dr. Myers reported having no conflicts of interest.
Elective CRC resections increase with universal insurance
BOSTON – Expanding access to health insurance for low- and moderate-income families has apparently improved colorectal cancer care in Massachusetts, and may do the same for other states that participate in Medicaid expansion under the Affordable Care Act.
That assertion comes from investigators at Massachusetts General Hospital in Boston. They found that following the introduction in 2006 of a universal health insurance law in the Bay State – the law that would serve as a model for the Affordable Care Act – the rate of elective colorectal resections increased while the rate of emergent resections decreased.
In contrast, in three states used as controls, the opposite occurred.
“This could be due to a variety of different factors, including earlier diagnosis, presenting with disease more amenable to surgical resection. It could also be due to increased referrals from primary care providers or GI doctors,” said Dr. Andrew P. Loehrer from the Massachusetts General Hospital Department of Surgery, at the annual Society of Surgical Oncology Cancer Symposium.
He acknowledged, however, that the administrative dataset he and his colleagues used in the study lacks information about clinical staging or use of neoadjuvant therapy, making it difficult to determine whether insured patients actually present at an earlier, more readily treatable disease stage.
Nonetheless, “from a cancer standpoint, my study provides early, hopeful evidence. In order to definitively say that this improves care, we need to have some more of the cancer-specific variables, but with this study, combined with some other work that we and other groups have done, we see that patients in Massachusetts are presenting with earlier stage disease, whether it’s acute disease or cancer, and they’re getting more appropriate care in a more timely fashion,” he said in an interview.
Role model
Dr. Loehrer noted that disparities in access to health care have been shown in previous studies to be associated with the likelihood of unfavorable outcomes for patients with colorectal cancer. For example, a 2008 study (Lancet Oncol. 2008 Mar;9:222-31) showed that uninsured patients with colorectal cancer had a twofold greater risk for presenting with advanced disease than privately insured patients. Additionally, a 2004 study (Br J Surg. 91:605-9) showed that patients who presented with colorectal cancer requiring emergent resection had significantly lower 5-year overall survival than patients who underwent elective resection.
Massachusetts implemented its pioneering health insurance reform law in 2006. The law increased eligibility for persons with incomes up to 150% of the Federal Poverty Level, created government-subsidized insurance for those with incomes from 150% to 300% of the poverty line, mandated that all Bay State residents have some form of health insurance, and allowed young adults up to the age of 26 to remain on their parents’ plans.
To see whether insurance reform could have a salutary effect on cancer care, the investigators drew on Agency for Health Research and Quality (AHRQ) State Inpatient Databases for Massachusetts and for Florida, New Jersey, and New York as control states. They used ICD-9 diagnosis codes to identify patients with colorectal cancer, including those who underwent resection.
To establish procedure rates, they used U.S. Census Bureau data to establish the population of denominators, which included all adults 18-54 years of age who were insured either through Medicaid, Commonwealth Care (in Massachusetts), or were listed as uninsured or self-pay. Medicare-insured patients were not included, as they were not directly affected by the reform law.
They identified 18,598 patients admitted to Massachusetts hospitals for colorectal cancer from 2001 through 2011, and 147,482 admitted during the same period to hospitals in the control states.
The authors created Poisson difference-in-differences models which compare changes in the selected outcomes in Massachusetts with changes in the control states. The models were adjusted for age, sex, race, hospital type, and secular trends.
They found that admission rates for colorectal cancer increased over time in Massachusetts by 13.3 per 100,000 residents per quarter, compared with 8.3/100,000 in the control states, translating into an adjusted rate ratio (ARR) of 1.13. Resection rates for cancer, the primary study outcome, also grew by a significantly larger margin in Massachusetts, by 5.5/100,000, compared with 0.5/100,000 in control states, with an ARR of 1.37 (P less than .001 for both comparisons).
For the secondary outcome of changes in emergent and elective resections after admission, they found that emergent surgeries in Massachusetts declined by 2.7/100,000, but increased by 4.4/100,000 in the states without insurance reform. Similarly, elective resections after admission increased in the Bay State by 7.4/100,000, but decreased by 1.8/100,000 in control states.
Relative to controls, the adjusted probability that a patient with colorectal cancer in Massachusetts would have emergent surgery after admission declined by 6.1% (P = .014) and the probability that he or she would have elective resection increased by 7.8% (P = .005).
An analysis of the odds ratio of resection during admission, adjusted for age, race, presentation with metastatic disease, hospital type, and secular trends, showed that prior to reform uninsured patients in both Massachusetts and control states were significantly less likely than privately insured patients to have resections (odds ratio, 0.42 in Mass.; 0.45 in control states).
However, after the implementation of reform the gap between previously uninsured and privately insured in Massachusetts narrowed (OR, 0.63) but remained the same in control states (OR, 0.44).
Dr. Loehrer acknowledged in an interview that Massachusetts differs from other states in some regards, including in concentrations of health providers and in requirements for insurance coverage that were in place even before the 2006 reforms, but is optimistic that improvements in colorectal cancer care can occur in states that have embraced the Affordable Care Act.
“There are a lot of services that were available and we had high colonoscopy rates prior to all of this, but that said, the mechanism is exactly the same, there are still vulnerable populations, and at this point I think it’s hopeful and promising that we will see similar results in other states,” he said.
BOSTON – Expanding access to health insurance for low- and moderate-income families has apparently improved colorectal cancer care in Massachusetts, and may do the same for other states that participate in Medicaid expansion under the Affordable Care Act.
That assertion comes from investigators at Massachusetts General Hospital in Boston. They found that following the introduction in 2006 of a universal health insurance law in the Bay State – the law that would serve as a model for the Affordable Care Act – the rate of elective colorectal resections increased while the rate of emergent resections decreased.
In contrast, in three states used as controls, the opposite occurred.
“This could be due to a variety of different factors, including earlier diagnosis, presenting with disease more amenable to surgical resection. It could also be due to increased referrals from primary care providers or GI doctors,” said Dr. Andrew P. Loehrer from the Massachusetts General Hospital Department of Surgery, at the annual Society of Surgical Oncology Cancer Symposium.
He acknowledged, however, that the administrative dataset he and his colleagues used in the study lacks information about clinical staging or use of neoadjuvant therapy, making it difficult to determine whether insured patients actually present at an earlier, more readily treatable disease stage.
Nonetheless, “from a cancer standpoint, my study provides early, hopeful evidence. In order to definitively say that this improves care, we need to have some more of the cancer-specific variables, but with this study, combined with some other work that we and other groups have done, we see that patients in Massachusetts are presenting with earlier stage disease, whether it’s acute disease or cancer, and they’re getting more appropriate care in a more timely fashion,” he said in an interview.
Role model
Dr. Loehrer noted that disparities in access to health care have been shown in previous studies to be associated with the likelihood of unfavorable outcomes for patients with colorectal cancer. For example, a 2008 study (Lancet Oncol. 2008 Mar;9:222-31) showed that uninsured patients with colorectal cancer had a twofold greater risk for presenting with advanced disease than privately insured patients. Additionally, a 2004 study (Br J Surg. 91:605-9) showed that patients who presented with colorectal cancer requiring emergent resection had significantly lower 5-year overall survival than patients who underwent elective resection.
Massachusetts implemented its pioneering health insurance reform law in 2006. The law increased eligibility for persons with incomes up to 150% of the Federal Poverty Level, created government-subsidized insurance for those with incomes from 150% to 300% of the poverty line, mandated that all Bay State residents have some form of health insurance, and allowed young adults up to the age of 26 to remain on their parents’ plans.
To see whether insurance reform could have a salutary effect on cancer care, the investigators drew on Agency for Health Research and Quality (AHRQ) State Inpatient Databases for Massachusetts and for Florida, New Jersey, and New York as control states. They used ICD-9 diagnosis codes to identify patients with colorectal cancer, including those who underwent resection.
To establish procedure rates, they used U.S. Census Bureau data to establish the population of denominators, which included all adults 18-54 years of age who were insured either through Medicaid, Commonwealth Care (in Massachusetts), or were listed as uninsured or self-pay. Medicare-insured patients were not included, as they were not directly affected by the reform law.
They identified 18,598 patients admitted to Massachusetts hospitals for colorectal cancer from 2001 through 2011, and 147,482 admitted during the same period to hospitals in the control states.
The authors created Poisson difference-in-differences models which compare changes in the selected outcomes in Massachusetts with changes in the control states. The models were adjusted for age, sex, race, hospital type, and secular trends.
They found that admission rates for colorectal cancer increased over time in Massachusetts by 13.3 per 100,000 residents per quarter, compared with 8.3/100,000 in the control states, translating into an adjusted rate ratio (ARR) of 1.13. Resection rates for cancer, the primary study outcome, also grew by a significantly larger margin in Massachusetts, by 5.5/100,000, compared with 0.5/100,000 in control states, with an ARR of 1.37 (P less than .001 for both comparisons).
For the secondary outcome of changes in emergent and elective resections after admission, they found that emergent surgeries in Massachusetts declined by 2.7/100,000, but increased by 4.4/100,000 in the states without insurance reform. Similarly, elective resections after admission increased in the Bay State by 7.4/100,000, but decreased by 1.8/100,000 in control states.
Relative to controls, the adjusted probability that a patient with colorectal cancer in Massachusetts would have emergent surgery after admission declined by 6.1% (P = .014) and the probability that he or she would have elective resection increased by 7.8% (P = .005).
An analysis of the odds ratio of resection during admission, adjusted for age, race, presentation with metastatic disease, hospital type, and secular trends, showed that prior to reform uninsured patients in both Massachusetts and control states were significantly less likely than privately insured patients to have resections (odds ratio, 0.42 in Mass.; 0.45 in control states).
However, after the implementation of reform the gap between previously uninsured and privately insured in Massachusetts narrowed (OR, 0.63) but remained the same in control states (OR, 0.44).
Dr. Loehrer acknowledged in an interview that Massachusetts differs from other states in some regards, including in concentrations of health providers and in requirements for insurance coverage that were in place even before the 2006 reforms, but is optimistic that improvements in colorectal cancer care can occur in states that have embraced the Affordable Care Act.
“There are a lot of services that were available and we had high colonoscopy rates prior to all of this, but that said, the mechanism is exactly the same, there are still vulnerable populations, and at this point I think it’s hopeful and promising that we will see similar results in other states,” he said.
BOSTON – Expanding access to health insurance for low- and moderate-income families has apparently improved colorectal cancer care in Massachusetts, and may do the same for other states that participate in Medicaid expansion under the Affordable Care Act.
That assertion comes from investigators at Massachusetts General Hospital in Boston. They found that following the introduction in 2006 of a universal health insurance law in the Bay State – the law that would serve as a model for the Affordable Care Act – the rate of elective colorectal resections increased while the rate of emergent resections decreased.
In contrast, in three states used as controls, the opposite occurred.
“This could be due to a variety of different factors, including earlier diagnosis, presenting with disease more amenable to surgical resection. It could also be due to increased referrals from primary care providers or GI doctors,” said Dr. Andrew P. Loehrer from the Massachusetts General Hospital Department of Surgery, at the annual Society of Surgical Oncology Cancer Symposium.
He acknowledged, however, that the administrative dataset he and his colleagues used in the study lacks information about clinical staging or use of neoadjuvant therapy, making it difficult to determine whether insured patients actually present at an earlier, more readily treatable disease stage.
Nonetheless, “from a cancer standpoint, my study provides early, hopeful evidence. In order to definitively say that this improves care, we need to have some more of the cancer-specific variables, but with this study, combined with some other work that we and other groups have done, we see that patients in Massachusetts are presenting with earlier stage disease, whether it’s acute disease or cancer, and they’re getting more appropriate care in a more timely fashion,” he said in an interview.
Role model
Dr. Loehrer noted that disparities in access to health care have been shown in previous studies to be associated with the likelihood of unfavorable outcomes for patients with colorectal cancer. For example, a 2008 study (Lancet Oncol. 2008 Mar;9:222-31) showed that uninsured patients with colorectal cancer had a twofold greater risk for presenting with advanced disease than privately insured patients. Additionally, a 2004 study (Br J Surg. 91:605-9) showed that patients who presented with colorectal cancer requiring emergent resection had significantly lower 5-year overall survival than patients who underwent elective resection.
Massachusetts implemented its pioneering health insurance reform law in 2006. The law increased eligibility for persons with incomes up to 150% of the Federal Poverty Level, created government-subsidized insurance for those with incomes from 150% to 300% of the poverty line, mandated that all Bay State residents have some form of health insurance, and allowed young adults up to the age of 26 to remain on their parents’ plans.
To see whether insurance reform could have a salutary effect on cancer care, the investigators drew on Agency for Health Research and Quality (AHRQ) State Inpatient Databases for Massachusetts and for Florida, New Jersey, and New York as control states. They used ICD-9 diagnosis codes to identify patients with colorectal cancer, including those who underwent resection.
To establish procedure rates, they used U.S. Census Bureau data to establish the population of denominators, which included all adults 18-54 years of age who were insured either through Medicaid, Commonwealth Care (in Massachusetts), or were listed as uninsured or self-pay. Medicare-insured patients were not included, as they were not directly affected by the reform law.
They identified 18,598 patients admitted to Massachusetts hospitals for colorectal cancer from 2001 through 2011, and 147,482 admitted during the same period to hospitals in the control states.
The authors created Poisson difference-in-differences models which compare changes in the selected outcomes in Massachusetts with changes in the control states. The models were adjusted for age, sex, race, hospital type, and secular trends.
They found that admission rates for colorectal cancer increased over time in Massachusetts by 13.3 per 100,000 residents per quarter, compared with 8.3/100,000 in the control states, translating into an adjusted rate ratio (ARR) of 1.13. Resection rates for cancer, the primary study outcome, also grew by a significantly larger margin in Massachusetts, by 5.5/100,000, compared with 0.5/100,000 in control states, with an ARR of 1.37 (P less than .001 for both comparisons).
For the secondary outcome of changes in emergent and elective resections after admission, they found that emergent surgeries in Massachusetts declined by 2.7/100,000, but increased by 4.4/100,000 in the states without insurance reform. Similarly, elective resections after admission increased in the Bay State by 7.4/100,000, but decreased by 1.8/100,000 in control states.
Relative to controls, the adjusted probability that a patient with colorectal cancer in Massachusetts would have emergent surgery after admission declined by 6.1% (P = .014) and the probability that he or she would have elective resection increased by 7.8% (P = .005).
An analysis of the odds ratio of resection during admission, adjusted for age, race, presentation with metastatic disease, hospital type, and secular trends, showed that prior to reform uninsured patients in both Massachusetts and control states were significantly less likely than privately insured patients to have resections (odds ratio, 0.42 in Mass.; 0.45 in control states).
However, after the implementation of reform the gap between previously uninsured and privately insured in Massachusetts narrowed (OR, 0.63) but remained the same in control states (OR, 0.44).
Dr. Loehrer acknowledged in an interview that Massachusetts differs from other states in some regards, including in concentrations of health providers and in requirements for insurance coverage that were in place even before the 2006 reforms, but is optimistic that improvements in colorectal cancer care can occur in states that have embraced the Affordable Care Act.
“There are a lot of services that were available and we had high colonoscopy rates prior to all of this, but that said, the mechanism is exactly the same, there are still vulnerable populations, and at this point I think it’s hopeful and promising that we will see similar results in other states,” he said.
FROM SSO 2016
Key clinical point: Outcomes for patients with colorectal cancer (CRC) who undergo elective resection are better than for those who require emergent resections.
Major finding: Elective CRC resection rates increased and emergent resections decreased after universal insurance was instituted in Massachusetts in 2006.
Data source: Retrospective study comparing differences over time between CRC resection rates in Massachusetts vs. those in Florida, New Jersey, and New York.
Disclosures: The study was supported in part by a grant from the National Institute on Aging. Dr. Loehrer and his coauthors reported no conflicts of interest.
HIV-positive life expectancy improves, but gap remains
BOSTON – Optimally treated patients with HIV are living longer than ever, and have narrowed but not completely closed the gap in life expectancy with their uninfected peers, investigators in a large cohort study reported.
In 1996, a 20-year-old infected with HIV could expect to live only 19 more years, to age 39. In 2011, the additional life expectancy for a 20-year-old HIV-positive subject was 53 years, meaning that given survival to age 20, he or she could expect to live to age 73, said Julia L. Marcus, Ph.D., from Kaiser Permanente Northern California in Oakland.
She and her colleagues studied life expectancy in a cohort of nearly 25,000 Kaiser Permanente California members who were HIV-positive and more than 250,000 HIV-negative members in an effort to better delineate differences in survival by HIV status than in earlier comparisons.
“This is the first study to our knowledge to directly compare life expectancy by HIV status, accounting for individual-level factors and access to health care. We have complete ascertainment of deaths, and therefore no loss to follow-up, and our results are generalizable to the broader insured population,” Dr. Marcus said at the Conference on Retroviruses and Opportunistic Infections.
The study results reflect the remarkable improvement in care of insured HIV-positive patients with the introduction of antiretroviral therapy (ART), which has allowed more than half of all HIV-positive individuals to live to age 50 or older, she said.
Previous studies suggesting that there is still a gap in life expectancy between HIV-positive and HIV-negative people had compared HIV-positive individuals with the general population, limiting their ability to account for differences in life expectancy by HIV status because of differences in sociodemographic factors, access to care, and risk factors that may affect survival, Dr. Marcus said.
To overcome these limitations, the investigators compared life expectancies for 24,768 HIV-positive people who were members of Kaiser Permanente California at any time from 1996 through 2011 with those of 257,600 HIV-negative members.
They conducted estimates by year of study follow-up, sex, race/ethnicity, HIV risk group, CD4 counts at ART initiation, and by key modifiable risk factors including viral hepatitis, drug and alcohol abuse, and smoking.
They found that over the course of the study, mortality rates among HIV-negative members remained relatively stable, at 439 per 100,000 person-years (py) in 1996, to 381/100,000 in 2011. In contrast, there was a steep decline among HIV-positive members, from 7,077/100,000 py in 1996, to 1,054/100,000 py in 2011.
Among women, remaining life expectancy at age 20 among those who were HIV-negative was 65 years in 1996, and 64 in 2011. In contrast, HIV-positive women saw an increase from 37 years in 1996 to 51 in 2011. Yet at the latest time point, there was still a 13-year gap in expectancy between HIV-negative and HIV-positive women.
Among HIV-negative men at age 20, additional life expectancy remained at 62 years throughout the study period, whereas among HIV-positive men it improved from 38 years in 1996 to 49 years in 2011. But here, too, there remained a 13-year gap in expectancy between HIV-positive and HIV-negative subjects.
An analysis of life expectancies at age 20 by race/ethnicity showed similar significant gains throughout the study period for whites, blacks, and Hispanics (P less than .0010), although HIV-positive whites and Hispanics did slightly but significantly better than blacks (P = .007 and .001, respectively),
There were also significant gains in life expectancy among men having sex with men, from 40 years in 1996 to 51 years in 2011, heterosexuals, from 38 years to 51 years, and among injectable drug users, from 36 to 46 years.
To see whether they could account for the 13-year gap that remained between HIV-positive and HIV-negative members, the authors looked at various care- and disease-related factors. When they considered those patients who received optimal therapy, with ART initiated when their CD4 counts were 500 or above, the expectancy gap narrowed to 7.9 years.
When they controlled for patients without hepatitis B or C infections, the gap narrowed to 7.2 years. HIV-positive patients with no drug or alcohol abuse had only 6.8 years less life expectancy than their HIV-negative counterparts, and those who did not smoke had only a 5.4 year life-expectancy decrement.
In the question-and-answer session following Dr. Marcus’ talk, an attendee suggested that some of the remaining gap may be explained by mental health differences between HIV-positive and HIV-negative patients.
“I would urge that you start looking at mental health issues and depression in particular, which is both vastly more common in people with HIV, and also has a demonstrable impact on mortality. That may explain some of the gap,” he said.
Dr. Marcus agreed about the importance of looking at this question, and noted that it is being actively explored in ongoing studies.
Dr. Marcus disclosed that she has been supported by a research grant to her institution from Merck.
BOSTON – Optimally treated patients with HIV are living longer than ever, and have narrowed but not completely closed the gap in life expectancy with their uninfected peers, investigators in a large cohort study reported.
In 1996, a 20-year-old infected with HIV could expect to live only 19 more years, to age 39. In 2011, the additional life expectancy for a 20-year-old HIV-positive subject was 53 years, meaning that given survival to age 20, he or she could expect to live to age 73, said Julia L. Marcus, Ph.D., from Kaiser Permanente Northern California in Oakland.
She and her colleagues studied life expectancy in a cohort of nearly 25,000 Kaiser Permanente California members who were HIV-positive and more than 250,000 HIV-negative members in an effort to better delineate differences in survival by HIV status than in earlier comparisons.
“This is the first study to our knowledge to directly compare life expectancy by HIV status, accounting for individual-level factors and access to health care. We have complete ascertainment of deaths, and therefore no loss to follow-up, and our results are generalizable to the broader insured population,” Dr. Marcus said at the Conference on Retroviruses and Opportunistic Infections.
The study results reflect the remarkable improvement in care of insured HIV-positive patients with the introduction of antiretroviral therapy (ART), which has allowed more than half of all HIV-positive individuals to live to age 50 or older, she said.
Previous studies suggesting that there is still a gap in life expectancy between HIV-positive and HIV-negative people had compared HIV-positive individuals with the general population, limiting their ability to account for differences in life expectancy by HIV status because of differences in sociodemographic factors, access to care, and risk factors that may affect survival, Dr. Marcus said.
To overcome these limitations, the investigators compared life expectancies for 24,768 HIV-positive people who were members of Kaiser Permanente California at any time from 1996 through 2011 with those of 257,600 HIV-negative members.
They conducted estimates by year of study follow-up, sex, race/ethnicity, HIV risk group, CD4 counts at ART initiation, and by key modifiable risk factors including viral hepatitis, drug and alcohol abuse, and smoking.
They found that over the course of the study, mortality rates among HIV-negative members remained relatively stable, at 439 per 100,000 person-years (py) in 1996, to 381/100,000 in 2011. In contrast, there was a steep decline among HIV-positive members, from 7,077/100,000 py in 1996, to 1,054/100,000 py in 2011.
Among women, remaining life expectancy at age 20 among those who were HIV-negative was 65 years in 1996, and 64 in 2011. In contrast, HIV-positive women saw an increase from 37 years in 1996 to 51 in 2011. Yet at the latest time point, there was still a 13-year gap in expectancy between HIV-negative and HIV-positive women.
Among HIV-negative men at age 20, additional life expectancy remained at 62 years throughout the study period, whereas among HIV-positive men it improved from 38 years in 1996 to 49 years in 2011. But here, too, there remained a 13-year gap in expectancy between HIV-positive and HIV-negative subjects.
An analysis of life expectancies at age 20 by race/ethnicity showed similar significant gains throughout the study period for whites, blacks, and Hispanics (P less than .0010), although HIV-positive whites and Hispanics did slightly but significantly better than blacks (P = .007 and .001, respectively),
There were also significant gains in life expectancy among men having sex with men, from 40 years in 1996 to 51 years in 2011, heterosexuals, from 38 years to 51 years, and among injectable drug users, from 36 to 46 years.
To see whether they could account for the 13-year gap that remained between HIV-positive and HIV-negative members, the authors looked at various care- and disease-related factors. When they considered those patients who received optimal therapy, with ART initiated when their CD4 counts were 500 or above, the expectancy gap narrowed to 7.9 years.
When they controlled for patients without hepatitis B or C infections, the gap narrowed to 7.2 years. HIV-positive patients with no drug or alcohol abuse had only 6.8 years less life expectancy than their HIV-negative counterparts, and those who did not smoke had only a 5.4 year life-expectancy decrement.
In the question-and-answer session following Dr. Marcus’ talk, an attendee suggested that some of the remaining gap may be explained by mental health differences between HIV-positive and HIV-negative patients.
“I would urge that you start looking at mental health issues and depression in particular, which is both vastly more common in people with HIV, and also has a demonstrable impact on mortality. That may explain some of the gap,” he said.
Dr. Marcus agreed about the importance of looking at this question, and noted that it is being actively explored in ongoing studies.
Dr. Marcus disclosed that she has been supported by a research grant to her institution from Merck.
BOSTON – Optimally treated patients with HIV are living longer than ever, and have narrowed but not completely closed the gap in life expectancy with their uninfected peers, investigators in a large cohort study reported.
In 1996, a 20-year-old infected with HIV could expect to live only 19 more years, to age 39. In 2011, the additional life expectancy for a 20-year-old HIV-positive subject was 53 years, meaning that given survival to age 20, he or she could expect to live to age 73, said Julia L. Marcus, Ph.D., from Kaiser Permanente Northern California in Oakland.
She and her colleagues studied life expectancy in a cohort of nearly 25,000 Kaiser Permanente California members who were HIV-positive and more than 250,000 HIV-negative members in an effort to better delineate differences in survival by HIV status than in earlier comparisons.
“This is the first study to our knowledge to directly compare life expectancy by HIV status, accounting for individual-level factors and access to health care. We have complete ascertainment of deaths, and therefore no loss to follow-up, and our results are generalizable to the broader insured population,” Dr. Marcus said at the Conference on Retroviruses and Opportunistic Infections.
The study results reflect the remarkable improvement in care of insured HIV-positive patients with the introduction of antiretroviral therapy (ART), which has allowed more than half of all HIV-positive individuals to live to age 50 or older, she said.
Previous studies suggesting that there is still a gap in life expectancy between HIV-positive and HIV-negative people had compared HIV-positive individuals with the general population, limiting their ability to account for differences in life expectancy by HIV status because of differences in sociodemographic factors, access to care, and risk factors that may affect survival, Dr. Marcus said.
To overcome these limitations, the investigators compared life expectancies for 24,768 HIV-positive people who were members of Kaiser Permanente California at any time from 1996 through 2011 with those of 257,600 HIV-negative members.
They conducted estimates by year of study follow-up, sex, race/ethnicity, HIV risk group, CD4 counts at ART initiation, and by key modifiable risk factors including viral hepatitis, drug and alcohol abuse, and smoking.
They found that over the course of the study, mortality rates among HIV-negative members remained relatively stable, at 439 per 100,000 person-years (py) in 1996, to 381/100,000 in 2011. In contrast, there was a steep decline among HIV-positive members, from 7,077/100,000 py in 1996, to 1,054/100,000 py in 2011.
Among women, remaining life expectancy at age 20 among those who were HIV-negative was 65 years in 1996, and 64 in 2011. In contrast, HIV-positive women saw an increase from 37 years in 1996 to 51 in 2011. Yet at the latest time point, there was still a 13-year gap in expectancy between HIV-negative and HIV-positive women.
Among HIV-negative men at age 20, additional life expectancy remained at 62 years throughout the study period, whereas among HIV-positive men it improved from 38 years in 1996 to 49 years in 2011. But here, too, there remained a 13-year gap in expectancy between HIV-positive and HIV-negative subjects.
An analysis of life expectancies at age 20 by race/ethnicity showed similar significant gains throughout the study period for whites, blacks, and Hispanics (P less than .0010), although HIV-positive whites and Hispanics did slightly but significantly better than blacks (P = .007 and .001, respectively),
There were also significant gains in life expectancy among men having sex with men, from 40 years in 1996 to 51 years in 2011, heterosexuals, from 38 years to 51 years, and among injectable drug users, from 36 to 46 years.
To see whether they could account for the 13-year gap that remained between HIV-positive and HIV-negative members, the authors looked at various care- and disease-related factors. When they considered those patients who received optimal therapy, with ART initiated when their CD4 counts were 500 or above, the expectancy gap narrowed to 7.9 years.
When they controlled for patients without hepatitis B or C infections, the gap narrowed to 7.2 years. HIV-positive patients with no drug or alcohol abuse had only 6.8 years less life expectancy than their HIV-negative counterparts, and those who did not smoke had only a 5.4 year life-expectancy decrement.
In the question-and-answer session following Dr. Marcus’ talk, an attendee suggested that some of the remaining gap may be explained by mental health differences between HIV-positive and HIV-negative patients.
“I would urge that you start looking at mental health issues and depression in particular, which is both vastly more common in people with HIV, and also has a demonstrable impact on mortality. That may explain some of the gap,” he said.
Dr. Marcus agreed about the importance of looking at this question, and noted that it is being actively explored in ongoing studies.
Dr. Marcus disclosed that she has been supported by a research grant to her institution from Merck.
AT CROI 2016
Key clinical point: As of 2011, there was a 13-year gap in life expectancy between HIV-positive and HIV-negative members of the same health plan.
Major finding: Life expectancy for a 20-year-old with HIV improved from 19 years in 1996 to 53 years in 2011.
Data source: Cohort study of 24,768 HIV-positive and 257,600 HIV-negative members of Kaiser Permanente California.
Disclosures: Dr. Marcus disclosed that she has been supported by a research grant to her institution from Merck.
Lessons from the Indiana HIV/HCV outbreak
BOSTON – Nearly 1 year after 11 new HIV infections were diagnosed in Scott County, Ind., a region that had an incidence of fewer than 1 HIV infection per year over the previous decade, 188 new HIV infections have now been diagnosed, and more than 90% of the cases were coinfected with hepatitis C (HCV), according to Dr. John T. Brooks of the Centers for Disease Control and Prevention.
Lessons from the outbreak, he said, include the inescapable fact that the United States is experiencing an expanding epidemic of heroin use that is driving an increase in injection drug use, putting many more U.S. residents at risk for the spread of HIV and HCV infection.
The response to the outbreak “required a large and extremely intensive collaboration of local, state, and federal public health resources in close partnership with community members, and like all outbreak investigations, there are two goals: First, establish the extent of the outbreak, and then institute prevention and control measures,” Dr. Brooks reported at a plenary session at the Conference on Retroviruses and Opportunistic Infections.
Once the cases were detected and confirmed, the health authorities went into action, deploying emergency command at the state level, similar to that deployed during a weather disaster, with a team of 35 disease intervention specialists and other public health workers from 14 states and the District of Columbia who went door to door, testing as many people as possible to find HIV infections, and tracing contacts to determine where additional, undiagnosed cases might be.
“The pattern of how we approached this outbreak is very much how you might approach tuberculosis, where you first detect that there’s a disease and confirm the diagnosis, you deploy an intervention to treat – sort of induction therapy – and once it’s under control you switch to consolidation therapy to keep the disease at bay, and then over time you might scan the person or follow up to see if the disease is recurring. The difference here is that we’re doing it on a population level,” said Dr. Brooks of the CDC’s division of HIV/AIDS prevention.
Astute observer spotted trend
The outbreak came to the attention of public health authorities when a “very, very astute” disease intervention specialist working in the county health department recognized that there were 11 new infections related to one another in Scott County, with the epicenter in the town of Austin.
Early in the outbreak, investigators determined that the HIV and HCV transmissions were occurring in a dense network of persons who inject drugs, mostly the opioid analgesic oxymorphone, but also heroin, methamphetamine, and cocaine. “During interviews, it was evident that 96% of the people had injected in the past 12 months, and that oxymorphone was the preferred drug used by 92%,” Dr. Brooks said.
Oxymorphone is available in generic and branded formulations. Although the brand name version (Opana and Opana ER) has a coating intended to prevent crushing the pills and dissolving the drug for the purpose of injection, “addiction can make you very creative, and the residents of this town had figured how to get around that,” Dr. Brooks said.
The outbreak was multigenerational, and it was not uncommon to find a household with three generations of drug abusers – grandparent, parents, and children – who injected drugs between 4 and 15 times each day, with one to as many as six needle-sharing partners per injection event, and sharing of injection equipment. Information was available on 181 of the 188 HIV-infected cases. The median age was 34 years (interquartile range, 28-42), 58% were male, 99% were non-Hispanic whites, and 96% had injected drugs within the past 12 months.
Jailhouse testing
The investigators established HIV testing both in the Scott County jail and in detention centers in surrounding counties in a sentinel system to determine whether the outbreak might have spread beyond the county line. The disease intervention specialists collected intravenous blood samples and performed point-of-care rapid testing for later confirmation, and for testing for acute HIV and HCV infection.
The workers also provided county residents with disease prevention educational materials and directed them to services as required, including treatment and antiretroviral therapy, and/or addition and harm reduction services and preexposure prophylaxis, if appropriate.
Major logistical challenges for responders included the fact that very few affected individuals were either employed or insured, and most lacked the necessary documents to enroll in state-supported care Medicaid expansion, recently adopted by Indiana as part of the Affordable Care Act.
In addition, residents in this impoverished, remote community in Southeastern Indiana – which ranks last among Indiana’s 92 counties in many health statistic categories – were aware of HIV or had correct information about transmission risks or treatment benefits.
Efforts were further hampered by the atmosphere of distrust between drug injectors and law enforcement; the lack of outpatient HIV or HCV care in the community; meager addiction services, including medication-assisted therapy; and a statewide ban on needle-exchange programs. In May of 2015, Indiana Gov. Mike Pence signed into law a bill allowing syringe exchange in areas where there was an urgent need because of disease outbreak.
In November of 2015, there was a retesting “blitz” in which disease intervention teams returned to the community and attempted to locate all persons who had previously tested negative, or had not been located on the first go-round and tested again to determine whether any of the residents had developed new infections.
“If there’s one message I’d like you to take away today,” Dr. Brooks told attendees, “it’s this: We all know now that this could happen again, but with your help and commitment, it doesn’t have to.”
BOSTON – Nearly 1 year after 11 new HIV infections were diagnosed in Scott County, Ind., a region that had an incidence of fewer than 1 HIV infection per year over the previous decade, 188 new HIV infections have now been diagnosed, and more than 90% of the cases were coinfected with hepatitis C (HCV), according to Dr. John T. Brooks of the Centers for Disease Control and Prevention.
Lessons from the outbreak, he said, include the inescapable fact that the United States is experiencing an expanding epidemic of heroin use that is driving an increase in injection drug use, putting many more U.S. residents at risk for the spread of HIV and HCV infection.
The response to the outbreak “required a large and extremely intensive collaboration of local, state, and federal public health resources in close partnership with community members, and like all outbreak investigations, there are two goals: First, establish the extent of the outbreak, and then institute prevention and control measures,” Dr. Brooks reported at a plenary session at the Conference on Retroviruses and Opportunistic Infections.
Once the cases were detected and confirmed, the health authorities went into action, deploying emergency command at the state level, similar to that deployed during a weather disaster, with a team of 35 disease intervention specialists and other public health workers from 14 states and the District of Columbia who went door to door, testing as many people as possible to find HIV infections, and tracing contacts to determine where additional, undiagnosed cases might be.
“The pattern of how we approached this outbreak is very much how you might approach tuberculosis, where you first detect that there’s a disease and confirm the diagnosis, you deploy an intervention to treat – sort of induction therapy – and once it’s under control you switch to consolidation therapy to keep the disease at bay, and then over time you might scan the person or follow up to see if the disease is recurring. The difference here is that we’re doing it on a population level,” said Dr. Brooks of the CDC’s division of HIV/AIDS prevention.
Astute observer spotted trend
The outbreak came to the attention of public health authorities when a “very, very astute” disease intervention specialist working in the county health department recognized that there were 11 new infections related to one another in Scott County, with the epicenter in the town of Austin.
Early in the outbreak, investigators determined that the HIV and HCV transmissions were occurring in a dense network of persons who inject drugs, mostly the opioid analgesic oxymorphone, but also heroin, methamphetamine, and cocaine. “During interviews, it was evident that 96% of the people had injected in the past 12 months, and that oxymorphone was the preferred drug used by 92%,” Dr. Brooks said.
Oxymorphone is available in generic and branded formulations. Although the brand name version (Opana and Opana ER) has a coating intended to prevent crushing the pills and dissolving the drug for the purpose of injection, “addiction can make you very creative, and the residents of this town had figured how to get around that,” Dr. Brooks said.
The outbreak was multigenerational, and it was not uncommon to find a household with three generations of drug abusers – grandparent, parents, and children – who injected drugs between 4 and 15 times each day, with one to as many as six needle-sharing partners per injection event, and sharing of injection equipment. Information was available on 181 of the 188 HIV-infected cases. The median age was 34 years (interquartile range, 28-42), 58% were male, 99% were non-Hispanic whites, and 96% had injected drugs within the past 12 months.
Jailhouse testing
The investigators established HIV testing both in the Scott County jail and in detention centers in surrounding counties in a sentinel system to determine whether the outbreak might have spread beyond the county line. The disease intervention specialists collected intravenous blood samples and performed point-of-care rapid testing for later confirmation, and for testing for acute HIV and HCV infection.
The workers also provided county residents with disease prevention educational materials and directed them to services as required, including treatment and antiretroviral therapy, and/or addition and harm reduction services and preexposure prophylaxis, if appropriate.
Major logistical challenges for responders included the fact that very few affected individuals were either employed or insured, and most lacked the necessary documents to enroll in state-supported care Medicaid expansion, recently adopted by Indiana as part of the Affordable Care Act.
In addition, residents in this impoverished, remote community in Southeastern Indiana – which ranks last among Indiana’s 92 counties in many health statistic categories – were aware of HIV or had correct information about transmission risks or treatment benefits.
Efforts were further hampered by the atmosphere of distrust between drug injectors and law enforcement; the lack of outpatient HIV or HCV care in the community; meager addiction services, including medication-assisted therapy; and a statewide ban on needle-exchange programs. In May of 2015, Indiana Gov. Mike Pence signed into law a bill allowing syringe exchange in areas where there was an urgent need because of disease outbreak.
In November of 2015, there was a retesting “blitz” in which disease intervention teams returned to the community and attempted to locate all persons who had previously tested negative, or had not been located on the first go-round and tested again to determine whether any of the residents had developed new infections.
“If there’s one message I’d like you to take away today,” Dr. Brooks told attendees, “it’s this: We all know now that this could happen again, but with your help and commitment, it doesn’t have to.”
BOSTON – Nearly 1 year after 11 new HIV infections were diagnosed in Scott County, Ind., a region that had an incidence of fewer than 1 HIV infection per year over the previous decade, 188 new HIV infections have now been diagnosed, and more than 90% of the cases were coinfected with hepatitis C (HCV), according to Dr. John T. Brooks of the Centers for Disease Control and Prevention.
Lessons from the outbreak, he said, include the inescapable fact that the United States is experiencing an expanding epidemic of heroin use that is driving an increase in injection drug use, putting many more U.S. residents at risk for the spread of HIV and HCV infection.
The response to the outbreak “required a large and extremely intensive collaboration of local, state, and federal public health resources in close partnership with community members, and like all outbreak investigations, there are two goals: First, establish the extent of the outbreak, and then institute prevention and control measures,” Dr. Brooks reported at a plenary session at the Conference on Retroviruses and Opportunistic Infections.
Once the cases were detected and confirmed, the health authorities went into action, deploying emergency command at the state level, similar to that deployed during a weather disaster, with a team of 35 disease intervention specialists and other public health workers from 14 states and the District of Columbia who went door to door, testing as many people as possible to find HIV infections, and tracing contacts to determine where additional, undiagnosed cases might be.
“The pattern of how we approached this outbreak is very much how you might approach tuberculosis, where you first detect that there’s a disease and confirm the diagnosis, you deploy an intervention to treat – sort of induction therapy – and once it’s under control you switch to consolidation therapy to keep the disease at bay, and then over time you might scan the person or follow up to see if the disease is recurring. The difference here is that we’re doing it on a population level,” said Dr. Brooks of the CDC’s division of HIV/AIDS prevention.
Astute observer spotted trend
The outbreak came to the attention of public health authorities when a “very, very astute” disease intervention specialist working in the county health department recognized that there were 11 new infections related to one another in Scott County, with the epicenter in the town of Austin.
Early in the outbreak, investigators determined that the HIV and HCV transmissions were occurring in a dense network of persons who inject drugs, mostly the opioid analgesic oxymorphone, but also heroin, methamphetamine, and cocaine. “During interviews, it was evident that 96% of the people had injected in the past 12 months, and that oxymorphone was the preferred drug used by 92%,” Dr. Brooks said.
Oxymorphone is available in generic and branded formulations. Although the brand name version (Opana and Opana ER) has a coating intended to prevent crushing the pills and dissolving the drug for the purpose of injection, “addiction can make you very creative, and the residents of this town had figured how to get around that,” Dr. Brooks said.
The outbreak was multigenerational, and it was not uncommon to find a household with three generations of drug abusers – grandparent, parents, and children – who injected drugs between 4 and 15 times each day, with one to as many as six needle-sharing partners per injection event, and sharing of injection equipment. Information was available on 181 of the 188 HIV-infected cases. The median age was 34 years (interquartile range, 28-42), 58% were male, 99% were non-Hispanic whites, and 96% had injected drugs within the past 12 months.
Jailhouse testing
The investigators established HIV testing both in the Scott County jail and in detention centers in surrounding counties in a sentinel system to determine whether the outbreak might have spread beyond the county line. The disease intervention specialists collected intravenous blood samples and performed point-of-care rapid testing for later confirmation, and for testing for acute HIV and HCV infection.
The workers also provided county residents with disease prevention educational materials and directed them to services as required, including treatment and antiretroviral therapy, and/or addition and harm reduction services and preexposure prophylaxis, if appropriate.
Major logistical challenges for responders included the fact that very few affected individuals were either employed or insured, and most lacked the necessary documents to enroll in state-supported care Medicaid expansion, recently adopted by Indiana as part of the Affordable Care Act.
In addition, residents in this impoverished, remote community in Southeastern Indiana – which ranks last among Indiana’s 92 counties in many health statistic categories – were aware of HIV or had correct information about transmission risks or treatment benefits.
Efforts were further hampered by the atmosphere of distrust between drug injectors and law enforcement; the lack of outpatient HIV or HCV care in the community; meager addiction services, including medication-assisted therapy; and a statewide ban on needle-exchange programs. In May of 2015, Indiana Gov. Mike Pence signed into law a bill allowing syringe exchange in areas where there was an urgent need because of disease outbreak.
In November of 2015, there was a retesting “blitz” in which disease intervention teams returned to the community and attempted to locate all persons who had previously tested negative, or had not been located on the first go-round and tested again to determine whether any of the residents had developed new infections.
“If there’s one message I’d like you to take away today,” Dr. Brooks told attendees, “it’s this: We all know now that this could happen again, but with your help and commitment, it doesn’t have to.”
AT CROI 2016
WHO: Zika epidemic requires ‘research-guided’ public health interventions
The link between Zika virus infections in pregnant women and microcephaly in neonates is strong, and there is good if somewhat less robust evidence for the virus causing severe neurological sequelae, especially Guillain-Barré syndrome, world health experts say.
Zika virus outbreaks have been reported in 31 countries and territories in the Americas, totaling more than 135,000 reported cases, and about 3,000 laboratory-confirmed cases, Dr. Marcos Espinal, director of the department of communicable diseases and health analysis at the Pan American Health Organization/World Health Organization, said at a joint PAHO/WHO meeting announcing key findings from an international meeting on the global challenge from Zika virus.
“The reports of these cases do not reflect the real situation, as in 80% of the cases globally there have been no signs and symptoms of Zika disease,” Dr. Espinal said.
Although the epidemic has garnered worldwide attention, there are many more unknowns than knowns about Zika virus and its sequelae, and recent findings from the outbreak are of particular concern, noted Dr. Lyle Petersen of the Centers for Disease Control and Prevention in Atlanta.
“It’s the first vector-borne disease we’ve seen that’s caused infections in fetuses and abnormal birth outcomes, and it’s also the first vector-borne disease that is also readily spread via sexual means,” he said.
To date, cases of microcephaly in the fetuses of Zika-infected women have been reported only in Brazil and in French Polynesia. As of Feb. 23, 2016, 5,640 cases of microcephaly had been reported in Brazil. In French Polynesia, as reported in The Lancet, following an epidemic of Zika from September 2013 through March 2014 affecting an estimated 28,000 individuals (about 11.5% of the population), clinicians noted an increase in cerebral congenital abnormalities, including microcephaly, ventriculomegaly, severe abnormalities of midline structures and the cerebellum, and abnormal gyration.
In addition, an increase in the incidence of Guillain-Barré syndrome cases coinciding with Zika virus outbreaks has been reported in Brazil, Colombia, El Salvador, Suriname, and Venezuela.
Resistant mosquitoes
Dr. Paulo Buss, director of the Global Health Center at the Oswaldo Cruz Foundation in Brazil, acknowledged that his country was the epicenter of the current epidemic, but noted that Brazil’s surveillance system was quick to identify the onset of the epidemic and make connections between Zika infection and its affect on congenital malformations and neurological disease. He pointed out that the epidemic is taking an especially hard toll on Brazilians with low incomes, who often live in overcrowded, unsanitary conditions, with no running water and no window screens to protect against mosquitoes.
One of the greatest challenges to public health authorities is the hardiness and adaptability of the vector, the Aedes aegypti and Aedes albopictus mosquitoes that are also prime vectors for dengue, chikungunya, and yellow fever infections, Dr. Buss said.
That point was reinforced in a recent report in The Lancet by Brazilian researchers who said that although their government has recently intensified efforts to eliminate Aedes aegypti using insecticides to kill adult mosquitoes and larvicides to eradicate breeding pools, “the results have been very disappointing.”
Despite mosquito eradication efforts, there has been an increase in the incidence of registered dengue cases in Brazil, with 1.6 million cases and 863 deaths reported in 2015. In addition, growing resistance by the vector to pesticides has forced health authorities to try a succession of different agents, further increasing the likelihood of resistance.
Areas of need
World health authorities broadly agreed, Dr. Espinal said, on the need for improved laboratory detection of infections, particularly a rapid and accurate test for pregnant women. Research questions must focus on both clinical research into prevention and treatment of infection, but also public health issues such as more effective vector control.
“This is a unique situation,” said the CDC’s Dr. Petersen. “I’ve been studying vector-borne diseases spread by mosquitoes for more than 20 years, and I’ve never seen anything like this.”
The situation calls for a research-guided response, he said, with collaboration and support from government and nongovernment organizations, WHO, PAHO, and academic institutions. The response must also be very rapid, as thousands of new infections are occurring in the Americas daily, he added.
“I think this outbreak reminds us that we all must be prepared. Over the last decade, we have let our responsibilities for vector-borne disease deteriorate. Mosquito control programs have gone away, and we’ve not developed any new pesticides in 50 years,” Petersen said. “This is a very good reminder that new things happen, and unexpected things happen, and we must be prepared.”
He said that there is a special need for prevention efforts aimed at pregnant women, including means of protecting them from mosquito bites with the use of insect repellents, window screens, and bed nets, and also the use of condoms to protect them from the possibility of infection from sex with an infected partner.
The link between Zika virus infections in pregnant women and microcephaly in neonates is strong, and there is good if somewhat less robust evidence for the virus causing severe neurological sequelae, especially Guillain-Barré syndrome, world health experts say.
Zika virus outbreaks have been reported in 31 countries and territories in the Americas, totaling more than 135,000 reported cases, and about 3,000 laboratory-confirmed cases, Dr. Marcos Espinal, director of the department of communicable diseases and health analysis at the Pan American Health Organization/World Health Organization, said at a joint PAHO/WHO meeting announcing key findings from an international meeting on the global challenge from Zika virus.
“The reports of these cases do not reflect the real situation, as in 80% of the cases globally there have been no signs and symptoms of Zika disease,” Dr. Espinal said.
Although the epidemic has garnered worldwide attention, there are many more unknowns than knowns about Zika virus and its sequelae, and recent findings from the outbreak are of particular concern, noted Dr. Lyle Petersen of the Centers for Disease Control and Prevention in Atlanta.
“It’s the first vector-borne disease we’ve seen that’s caused infections in fetuses and abnormal birth outcomes, and it’s also the first vector-borne disease that is also readily spread via sexual means,” he said.
To date, cases of microcephaly in the fetuses of Zika-infected women have been reported only in Brazil and in French Polynesia. As of Feb. 23, 2016, 5,640 cases of microcephaly had been reported in Brazil. In French Polynesia, as reported in The Lancet, following an epidemic of Zika from September 2013 through March 2014 affecting an estimated 28,000 individuals (about 11.5% of the population), clinicians noted an increase in cerebral congenital abnormalities, including microcephaly, ventriculomegaly, severe abnormalities of midline structures and the cerebellum, and abnormal gyration.
In addition, an increase in the incidence of Guillain-Barré syndrome cases coinciding with Zika virus outbreaks has been reported in Brazil, Colombia, El Salvador, Suriname, and Venezuela.
Resistant mosquitoes
Dr. Paulo Buss, director of the Global Health Center at the Oswaldo Cruz Foundation in Brazil, acknowledged that his country was the epicenter of the current epidemic, but noted that Brazil’s surveillance system was quick to identify the onset of the epidemic and make connections between Zika infection and its affect on congenital malformations and neurological disease. He pointed out that the epidemic is taking an especially hard toll on Brazilians with low incomes, who often live in overcrowded, unsanitary conditions, with no running water and no window screens to protect against mosquitoes.
One of the greatest challenges to public health authorities is the hardiness and adaptability of the vector, the Aedes aegypti and Aedes albopictus mosquitoes that are also prime vectors for dengue, chikungunya, and yellow fever infections, Dr. Buss said.
That point was reinforced in a recent report in The Lancet by Brazilian researchers who said that although their government has recently intensified efforts to eliminate Aedes aegypti using insecticides to kill adult mosquitoes and larvicides to eradicate breeding pools, “the results have been very disappointing.”
Despite mosquito eradication efforts, there has been an increase in the incidence of registered dengue cases in Brazil, with 1.6 million cases and 863 deaths reported in 2015. In addition, growing resistance by the vector to pesticides has forced health authorities to try a succession of different agents, further increasing the likelihood of resistance.
Areas of need
World health authorities broadly agreed, Dr. Espinal said, on the need for improved laboratory detection of infections, particularly a rapid and accurate test for pregnant women. Research questions must focus on both clinical research into prevention and treatment of infection, but also public health issues such as more effective vector control.
“This is a unique situation,” said the CDC’s Dr. Petersen. “I’ve been studying vector-borne diseases spread by mosquitoes for more than 20 years, and I’ve never seen anything like this.”
The situation calls for a research-guided response, he said, with collaboration and support from government and nongovernment organizations, WHO, PAHO, and academic institutions. The response must also be very rapid, as thousands of new infections are occurring in the Americas daily, he added.
“I think this outbreak reminds us that we all must be prepared. Over the last decade, we have let our responsibilities for vector-borne disease deteriorate. Mosquito control programs have gone away, and we’ve not developed any new pesticides in 50 years,” Petersen said. “This is a very good reminder that new things happen, and unexpected things happen, and we must be prepared.”
He said that there is a special need for prevention efforts aimed at pregnant women, including means of protecting them from mosquito bites with the use of insect repellents, window screens, and bed nets, and also the use of condoms to protect them from the possibility of infection from sex with an infected partner.
The link between Zika virus infections in pregnant women and microcephaly in neonates is strong, and there is good if somewhat less robust evidence for the virus causing severe neurological sequelae, especially Guillain-Barré syndrome, world health experts say.
Zika virus outbreaks have been reported in 31 countries and territories in the Americas, totaling more than 135,000 reported cases, and about 3,000 laboratory-confirmed cases, Dr. Marcos Espinal, director of the department of communicable diseases and health analysis at the Pan American Health Organization/World Health Organization, said at a joint PAHO/WHO meeting announcing key findings from an international meeting on the global challenge from Zika virus.
“The reports of these cases do not reflect the real situation, as in 80% of the cases globally there have been no signs and symptoms of Zika disease,” Dr. Espinal said.
Although the epidemic has garnered worldwide attention, there are many more unknowns than knowns about Zika virus and its sequelae, and recent findings from the outbreak are of particular concern, noted Dr. Lyle Petersen of the Centers for Disease Control and Prevention in Atlanta.
“It’s the first vector-borne disease we’ve seen that’s caused infections in fetuses and abnormal birth outcomes, and it’s also the first vector-borne disease that is also readily spread via sexual means,” he said.
To date, cases of microcephaly in the fetuses of Zika-infected women have been reported only in Brazil and in French Polynesia. As of Feb. 23, 2016, 5,640 cases of microcephaly had been reported in Brazil. In French Polynesia, as reported in The Lancet, following an epidemic of Zika from September 2013 through March 2014 affecting an estimated 28,000 individuals (about 11.5% of the population), clinicians noted an increase in cerebral congenital abnormalities, including microcephaly, ventriculomegaly, severe abnormalities of midline structures and the cerebellum, and abnormal gyration.
In addition, an increase in the incidence of Guillain-Barré syndrome cases coinciding with Zika virus outbreaks has been reported in Brazil, Colombia, El Salvador, Suriname, and Venezuela.
Resistant mosquitoes
Dr. Paulo Buss, director of the Global Health Center at the Oswaldo Cruz Foundation in Brazil, acknowledged that his country was the epicenter of the current epidemic, but noted that Brazil’s surveillance system was quick to identify the onset of the epidemic and make connections between Zika infection and its affect on congenital malformations and neurological disease. He pointed out that the epidemic is taking an especially hard toll on Brazilians with low incomes, who often live in overcrowded, unsanitary conditions, with no running water and no window screens to protect against mosquitoes.
One of the greatest challenges to public health authorities is the hardiness and adaptability of the vector, the Aedes aegypti and Aedes albopictus mosquitoes that are also prime vectors for dengue, chikungunya, and yellow fever infections, Dr. Buss said.
That point was reinforced in a recent report in The Lancet by Brazilian researchers who said that although their government has recently intensified efforts to eliminate Aedes aegypti using insecticides to kill adult mosquitoes and larvicides to eradicate breeding pools, “the results have been very disappointing.”
Despite mosquito eradication efforts, there has been an increase in the incidence of registered dengue cases in Brazil, with 1.6 million cases and 863 deaths reported in 2015. In addition, growing resistance by the vector to pesticides has forced health authorities to try a succession of different agents, further increasing the likelihood of resistance.
Areas of need
World health authorities broadly agreed, Dr. Espinal said, on the need for improved laboratory detection of infections, particularly a rapid and accurate test for pregnant women. Research questions must focus on both clinical research into prevention and treatment of infection, but also public health issues such as more effective vector control.
“This is a unique situation,” said the CDC’s Dr. Petersen. “I’ve been studying vector-borne diseases spread by mosquitoes for more than 20 years, and I’ve never seen anything like this.”
The situation calls for a research-guided response, he said, with collaboration and support from government and nongovernment organizations, WHO, PAHO, and academic institutions. The response must also be very rapid, as thousands of new infections are occurring in the Americas daily, he added.
“I think this outbreak reminds us that we all must be prepared. Over the last decade, we have let our responsibilities for vector-borne disease deteriorate. Mosquito control programs have gone away, and we’ve not developed any new pesticides in 50 years,” Petersen said. “This is a very good reminder that new things happen, and unexpected things happen, and we must be prepared.”
He said that there is a special need for prevention efforts aimed at pregnant women, including means of protecting them from mosquito bites with the use of insect repellents, window screens, and bed nets, and also the use of condoms to protect them from the possibility of infection from sex with an infected partner.
FROM A JOINT PAHO/WHO MEETING
CROI: The future of HIV is here: mAbs in prevention, treatment
BOSTON – There is a long history of the use of antibodies for prevention and treatment of many different infectious diseases, and now it’s HIV’s turn, a vaccine investigator said.
Data from animal models and early human trials suggest that recently isolated, broadly neutralizing monoclonal antibodies (mAbs) against HIV-1 may be effective for prevention of infection and for viral suppression in infected individuals, according to Dr. John R. Mascola from the Vaccine Research Center at the National Institute of Allergy and Infectious Diseases in Bethesda, Md.
“Antibodies are biologically active; even a single antibody can reduce plasma virus by 1-2 logs with a single infusion. However, selection for resistant strains can occur and does occur rapidly in the setting of incomplete viral suppression. So this strongly suggests the combination of antibodies, or antibodies plus antiretroviral drugs are likely to be required for viral suppression,” he said in a plenary talk at the Conference on Retroviruses and Opportunistic Infections.
The effect of antibodies on reduction or elimination of viral reservoirs, however, is still unclear, and will require additional research, he said.
There is a long history of passive immunization with antibodies, he said, beginning with “serum therapy” for diphtheria, tetanus, and streptococcal infections, and progressing to the use of immune globulins for the prevention of common viral diseases such as measles, poliomyelitis, cytomegalovirus, hepatitis A, and respiratory syncytial virus (in high-risk infants) and for postexposure prophylaxis of hepatitis B, rabies, and varicella-zoster virus, he said.
“In the infectious disease world, the concept of using antibodies for HIV has been around for a long time, really, based on our knowledge of all these other viral diseases. But what has changed and really invigorated the field is the discovery of many potent neutralizing antibodies since 2009,” he said.
More than 20 antibodies directed against several different viral binding sites have been described in the last 6 years alone.
Two important considerations for successful prevention of binding of HIV and entry into cells is the breadth (percentage of all HIV strains that are neutralized) and potency of mAbs, Dr. Mascola said.
More recently discovered mAbs are up to 500-fold more potent than older anti-HIV antibodies, the first of which were described in the early 1990s, but the perfect antibody with the right combination of breadth and potency has not been identified to date, he said.
Prevention
Preclinical studies conducted over the last 2 decades using ape and monkey models and simian HIV (SHIV) has shown that neutralizing antibodies can prevent infection, and that more recently discovered mAbs are especially effective when given before a viral challenge. However, there are few if any data on protection against viral challenge in humans, Dr. Mascola pointed out.
“What’s encouraging is that within the next couple of years, rather than where we are now where I can tell you about antibodies to only one site, there are very likely to be antibodies to four major sites on the virus,” he added.
Several phase I trials of an antibody labeled VRC01, directed against the CD4 binding site, are currently in the recruiting or planning stages.
Questions that remain about antibodies for HIV transmission prevention in humans included what level of mAbs is required for protections, where and how mAbs work (for example, in the lumen, epithelial surface, mucosal tissue, or lymphoid tissue), and whether Fc-mediated effector functions are required for protection.
Treatment
Whereas antibodies for prevention are aimed at blocking transmission and acquisition of infection, antibodies for treatment of HIV have a different clinical use, as complements to antiretroviral therapy, with a different mechanism of action. Therapeutic antibodies have the potential to eliminate infected cells, and could help to deplete cell-associated viral reservoirs, Dr. Mascola said.
During acute infection, they could be used in tandem with antiretroviral therapy for quick reduction of viremia and to limit seeding of a viral reservoir. Some long-lasting antibodies could help with maintenance of viral suppression.
As noted before, antibodies directed against HIV-1 are biologically active and can markedly reduce plasma viremia, but are subject to rapid development of resistance in the setting of incomplete viral suppression. Thus, mAbs will likely be used in combination with other mAbs or antiretroviral drugs to achieve effective viral suppression, and antibodies with long half-lives will likely be needed to achieve depletion of viral reservoirs, Dr. Mascola said.
Dr. Mascola is an employee of the National Institutes of Health. He reported no other conflicts.
BOSTON – There is a long history of the use of antibodies for prevention and treatment of many different infectious diseases, and now it’s HIV’s turn, a vaccine investigator said.
Data from animal models and early human trials suggest that recently isolated, broadly neutralizing monoclonal antibodies (mAbs) against HIV-1 may be effective for prevention of infection and for viral suppression in infected individuals, according to Dr. John R. Mascola from the Vaccine Research Center at the National Institute of Allergy and Infectious Diseases in Bethesda, Md.
“Antibodies are biologically active; even a single antibody can reduce plasma virus by 1-2 logs with a single infusion. However, selection for resistant strains can occur and does occur rapidly in the setting of incomplete viral suppression. So this strongly suggests the combination of antibodies, or antibodies plus antiretroviral drugs are likely to be required for viral suppression,” he said in a plenary talk at the Conference on Retroviruses and Opportunistic Infections.
The effect of antibodies on reduction or elimination of viral reservoirs, however, is still unclear, and will require additional research, he said.
There is a long history of passive immunization with antibodies, he said, beginning with “serum therapy” for diphtheria, tetanus, and streptococcal infections, and progressing to the use of immune globulins for the prevention of common viral diseases such as measles, poliomyelitis, cytomegalovirus, hepatitis A, and respiratory syncytial virus (in high-risk infants) and for postexposure prophylaxis of hepatitis B, rabies, and varicella-zoster virus, he said.
“In the infectious disease world, the concept of using antibodies for HIV has been around for a long time, really, based on our knowledge of all these other viral diseases. But what has changed and really invigorated the field is the discovery of many potent neutralizing antibodies since 2009,” he said.
More than 20 antibodies directed against several different viral binding sites have been described in the last 6 years alone.
Two important considerations for successful prevention of binding of HIV and entry into cells is the breadth (percentage of all HIV strains that are neutralized) and potency of mAbs, Dr. Mascola said.
More recently discovered mAbs are up to 500-fold more potent than older anti-HIV antibodies, the first of which were described in the early 1990s, but the perfect antibody with the right combination of breadth and potency has not been identified to date, he said.
Prevention
Preclinical studies conducted over the last 2 decades using ape and monkey models and simian HIV (SHIV) has shown that neutralizing antibodies can prevent infection, and that more recently discovered mAbs are especially effective when given before a viral challenge. However, there are few if any data on protection against viral challenge in humans, Dr. Mascola pointed out.
“What’s encouraging is that within the next couple of years, rather than where we are now where I can tell you about antibodies to only one site, there are very likely to be antibodies to four major sites on the virus,” he added.
Several phase I trials of an antibody labeled VRC01, directed against the CD4 binding site, are currently in the recruiting or planning stages.
Questions that remain about antibodies for HIV transmission prevention in humans included what level of mAbs is required for protections, where and how mAbs work (for example, in the lumen, epithelial surface, mucosal tissue, or lymphoid tissue), and whether Fc-mediated effector functions are required for protection.
Treatment
Whereas antibodies for prevention are aimed at blocking transmission and acquisition of infection, antibodies for treatment of HIV have a different clinical use, as complements to antiretroviral therapy, with a different mechanism of action. Therapeutic antibodies have the potential to eliminate infected cells, and could help to deplete cell-associated viral reservoirs, Dr. Mascola said.
During acute infection, they could be used in tandem with antiretroviral therapy for quick reduction of viremia and to limit seeding of a viral reservoir. Some long-lasting antibodies could help with maintenance of viral suppression.
As noted before, antibodies directed against HIV-1 are biologically active and can markedly reduce plasma viremia, but are subject to rapid development of resistance in the setting of incomplete viral suppression. Thus, mAbs will likely be used in combination with other mAbs or antiretroviral drugs to achieve effective viral suppression, and antibodies with long half-lives will likely be needed to achieve depletion of viral reservoirs, Dr. Mascola said.
Dr. Mascola is an employee of the National Institutes of Health. He reported no other conflicts.
BOSTON – There is a long history of the use of antibodies for prevention and treatment of many different infectious diseases, and now it’s HIV’s turn, a vaccine investigator said.
Data from animal models and early human trials suggest that recently isolated, broadly neutralizing monoclonal antibodies (mAbs) against HIV-1 may be effective for prevention of infection and for viral suppression in infected individuals, according to Dr. John R. Mascola from the Vaccine Research Center at the National Institute of Allergy and Infectious Diseases in Bethesda, Md.
“Antibodies are biologically active; even a single antibody can reduce plasma virus by 1-2 logs with a single infusion. However, selection for resistant strains can occur and does occur rapidly in the setting of incomplete viral suppression. So this strongly suggests the combination of antibodies, or antibodies plus antiretroviral drugs are likely to be required for viral suppression,” he said in a plenary talk at the Conference on Retroviruses and Opportunistic Infections.
The effect of antibodies on reduction or elimination of viral reservoirs, however, is still unclear, and will require additional research, he said.
There is a long history of passive immunization with antibodies, he said, beginning with “serum therapy” for diphtheria, tetanus, and streptococcal infections, and progressing to the use of immune globulins for the prevention of common viral diseases such as measles, poliomyelitis, cytomegalovirus, hepatitis A, and respiratory syncytial virus (in high-risk infants) and for postexposure prophylaxis of hepatitis B, rabies, and varicella-zoster virus, he said.
“In the infectious disease world, the concept of using antibodies for HIV has been around for a long time, really, based on our knowledge of all these other viral diseases. But what has changed and really invigorated the field is the discovery of many potent neutralizing antibodies since 2009,” he said.
More than 20 antibodies directed against several different viral binding sites have been described in the last 6 years alone.
Two important considerations for successful prevention of binding of HIV and entry into cells is the breadth (percentage of all HIV strains that are neutralized) and potency of mAbs, Dr. Mascola said.
More recently discovered mAbs are up to 500-fold more potent than older anti-HIV antibodies, the first of which were described in the early 1990s, but the perfect antibody with the right combination of breadth and potency has not been identified to date, he said.
Prevention
Preclinical studies conducted over the last 2 decades using ape and monkey models and simian HIV (SHIV) has shown that neutralizing antibodies can prevent infection, and that more recently discovered mAbs are especially effective when given before a viral challenge. However, there are few if any data on protection against viral challenge in humans, Dr. Mascola pointed out.
“What’s encouraging is that within the next couple of years, rather than where we are now where I can tell you about antibodies to only one site, there are very likely to be antibodies to four major sites on the virus,” he added.
Several phase I trials of an antibody labeled VRC01, directed against the CD4 binding site, are currently in the recruiting or planning stages.
Questions that remain about antibodies for HIV transmission prevention in humans included what level of mAbs is required for protections, where and how mAbs work (for example, in the lumen, epithelial surface, mucosal tissue, or lymphoid tissue), and whether Fc-mediated effector functions are required for protection.
Treatment
Whereas antibodies for prevention are aimed at blocking transmission and acquisition of infection, antibodies for treatment of HIV have a different clinical use, as complements to antiretroviral therapy, with a different mechanism of action. Therapeutic antibodies have the potential to eliminate infected cells, and could help to deplete cell-associated viral reservoirs, Dr. Mascola said.
During acute infection, they could be used in tandem with antiretroviral therapy for quick reduction of viremia and to limit seeding of a viral reservoir. Some long-lasting antibodies could help with maintenance of viral suppression.
As noted before, antibodies directed against HIV-1 are biologically active and can markedly reduce plasma viremia, but are subject to rapid development of resistance in the setting of incomplete viral suppression. Thus, mAbs will likely be used in combination with other mAbs or antiretroviral drugs to achieve effective viral suppression, and antibodies with long half-lives will likely be needed to achieve depletion of viral reservoirs, Dr. Mascola said.
Dr. Mascola is an employee of the National Institutes of Health. He reported no other conflicts.
AT CROI 2016
Key clinical point:. Preclinical and early human studies suggest that anti-HIV-1 neutralizing antibodies may be effective in prevention and treatment.
Major finding: One antibody type is capable of reducing HIV-1 plasma viremia by 1-2 log10.
Data source: Review of current understanding and research into HIV-1 neutralizing monoclonal antibodies.
Disclosures: Dr. Mascola is an employee of the National Institutes of Health.
More patients are achieving HIV suppression, CDC says
BOSTON – People with HIV who get proper medical care stand a better chance than ever of achieving durable viral suppression, said investigators from the Centers for Disease Control and Prevention at the Conference on Retroviruses and Opportunistic Infections.
Data from a nationwide surveillance sample of patients receiving medical care for HIV in the United States shows that the proportion of all HIV-infected persons whose viral levels were suppressed below 200 copies/mL at their most recent visit increased from 72% in 2009 to 80% in 2013 (P for trend less than .01), reported Heather Bradley, Ph.D., of the CDC.
“These findings are really encouraging in terms of progress toward the National HIV/AIDS strategy goals of both improving the health of persons living with HIV and reducing infections,” she said at a media briefing following her presentation of data at in a CROI 2016 oral session.
The CDC investigators drew on the Medical Monitoring Project, a surveillance system that provides nationally representative data on HIV medical care to estimate the proportion of persons receiving care who achieve viral suppression at both their last tests and at all tests during the previous 12 months.
They collected data on a total of 23,125 HIV-infected persons from interviews and medical records, and looked at trends over time in viral suppression in the population as a whole and by categories of sex, age, race/ethnicity, sexual behavior, and sexual orientation.
“Encouragingly, the largest increases that we observed were seen among populations with the lowest level of viral suppression in 2009, including young people and non-Hispanic blacks,” Dr. Bradley said.
Among 18- to 29-year-olds, suppression rates improved from 56% in 2009 to 68% in 2013 (P for trend less than .001), and among non-Hispanic blacks the rates improved from 64% to 76%, respectively (P for trend less than .01).
The trend toward improved viral suppression was in fact seen in both men and in women, among all age groups, in non-Hispanic whites and Hispanics, and in men who have sex with men; men who have sex with women; and women who have sex with men.
In addition, there was significant improvement in the proportion of persons with viral suppression at all tests during the previous year, with rates growing from 58% in 2009 to 68% in 2013.
Dr. Bradley said that the improvement in viral control may be attributable to public health efforts to improve access to medical care for persons with HIV, and to promotion of early initiation of antiretroviral therapies.
The study was funded by the CDC. Dr. Bradley is a CDC employee.
BOSTON – People with HIV who get proper medical care stand a better chance than ever of achieving durable viral suppression, said investigators from the Centers for Disease Control and Prevention at the Conference on Retroviruses and Opportunistic Infections.
Data from a nationwide surveillance sample of patients receiving medical care for HIV in the United States shows that the proportion of all HIV-infected persons whose viral levels were suppressed below 200 copies/mL at their most recent visit increased from 72% in 2009 to 80% in 2013 (P for trend less than .01), reported Heather Bradley, Ph.D., of the CDC.
“These findings are really encouraging in terms of progress toward the National HIV/AIDS strategy goals of both improving the health of persons living with HIV and reducing infections,” she said at a media briefing following her presentation of data at in a CROI 2016 oral session.
The CDC investigators drew on the Medical Monitoring Project, a surveillance system that provides nationally representative data on HIV medical care to estimate the proportion of persons receiving care who achieve viral suppression at both their last tests and at all tests during the previous 12 months.
They collected data on a total of 23,125 HIV-infected persons from interviews and medical records, and looked at trends over time in viral suppression in the population as a whole and by categories of sex, age, race/ethnicity, sexual behavior, and sexual orientation.
“Encouragingly, the largest increases that we observed were seen among populations with the lowest level of viral suppression in 2009, including young people and non-Hispanic blacks,” Dr. Bradley said.
Among 18- to 29-year-olds, suppression rates improved from 56% in 2009 to 68% in 2013 (P for trend less than .001), and among non-Hispanic blacks the rates improved from 64% to 76%, respectively (P for trend less than .01).
The trend toward improved viral suppression was in fact seen in both men and in women, among all age groups, in non-Hispanic whites and Hispanics, and in men who have sex with men; men who have sex with women; and women who have sex with men.
In addition, there was significant improvement in the proportion of persons with viral suppression at all tests during the previous year, with rates growing from 58% in 2009 to 68% in 2013.
Dr. Bradley said that the improvement in viral control may be attributable to public health efforts to improve access to medical care for persons with HIV, and to promotion of early initiation of antiretroviral therapies.
The study was funded by the CDC. Dr. Bradley is a CDC employee.
BOSTON – People with HIV who get proper medical care stand a better chance than ever of achieving durable viral suppression, said investigators from the Centers for Disease Control and Prevention at the Conference on Retroviruses and Opportunistic Infections.
Data from a nationwide surveillance sample of patients receiving medical care for HIV in the United States shows that the proportion of all HIV-infected persons whose viral levels were suppressed below 200 copies/mL at their most recent visit increased from 72% in 2009 to 80% in 2013 (P for trend less than .01), reported Heather Bradley, Ph.D., of the CDC.
“These findings are really encouraging in terms of progress toward the National HIV/AIDS strategy goals of both improving the health of persons living with HIV and reducing infections,” she said at a media briefing following her presentation of data at in a CROI 2016 oral session.
The CDC investigators drew on the Medical Monitoring Project, a surveillance system that provides nationally representative data on HIV medical care to estimate the proportion of persons receiving care who achieve viral suppression at both their last tests and at all tests during the previous 12 months.
They collected data on a total of 23,125 HIV-infected persons from interviews and medical records, and looked at trends over time in viral suppression in the population as a whole and by categories of sex, age, race/ethnicity, sexual behavior, and sexual orientation.
“Encouragingly, the largest increases that we observed were seen among populations with the lowest level of viral suppression in 2009, including young people and non-Hispanic blacks,” Dr. Bradley said.
Among 18- to 29-year-olds, suppression rates improved from 56% in 2009 to 68% in 2013 (P for trend less than .001), and among non-Hispanic blacks the rates improved from 64% to 76%, respectively (P for trend less than .01).
The trend toward improved viral suppression was in fact seen in both men and in women, among all age groups, in non-Hispanic whites and Hispanics, and in men who have sex with men; men who have sex with women; and women who have sex with men.
In addition, there was significant improvement in the proportion of persons with viral suppression at all tests during the previous year, with rates growing from 58% in 2009 to 68% in 2013.
Dr. Bradley said that the improvement in viral control may be attributable to public health efforts to improve access to medical care for persons with HIV, and to promotion of early initiation of antiretroviral therapies.
The study was funded by the CDC. Dr. Bradley is a CDC employee.
AT CROI 2016
Key clinical point: HIV viral suppression rates (less than 200 copies/mL) improved significantly during 2009-2013.
Major finding: The proportion of all HIV-infected persons whose viral levels were suppressed below 200 copies/mL at their most recent visit increased from 72% in 2009, to 80% in 2013.
Data source: Surveillance data on 23,125 HIV-infected persons in the United States.
Disclosures: The study was funded by the CDC. Dr. Bradley is a CDC employee.
Perceptions of HIV infectiousness may influence sexual behavior
BOSTON – Although antiretroviral therapy (ART) has been shown to reduce risk of HIV transmission, particularly among heterosexuals, there is a gap between patient perception of infectiousness and actual risk of HIV transmission, suggesting that clinicians need to do better at discussing implications with patients on treatment.
Among patients participating in a randomized clinical trial comparing three ART regimens, nearly half reported a decline in their perception of their own infectiousness (POI) at 48 weeks compared with study entry, but few participants thought themselves to be noninfectious at any time point, reported Dr. Raphael Landovitz of the David Geffen School of Medicine at the University of California, Los Angeles.
“We think this highlights some important opportunities for finding populations who need more education about what it means for their sexual partners in terms of their infectiousness by a sexual route as they achieve therapy, and I think as providers we can do a better job about contextualizing the benefits of antiretroviral therapy, not only for individuals, but for populations,” he said at a media briefing following his presentation of the data in an oral abstract session at the Conference on Retroviruses and Opportunistic Infections.
Dr. Landovitz and colleagues conducted a secondary analysis of data from the AIDS Clinical Trials Group (ACTG) A5257 Trial, which compared tenofovir/emtricitabine in combination with either atazanavir, raltegravir, or darunavir.
Patients in the trial were asked at baseline and every 48 weeks to rate on a visual analog scale from 0 to 100 their response to the question, “How likely would you be to give someone HIV if you had unprotected sex with them today?” – with 0 being not at all infectious, and 100 being highly infectious.
At baseline, 6% had a POI of not at all infectious, 10% thought themselves to be at low risk for HIV transmission. 26% considered themselves at medium risk, and 58% had a POI of highly infectious.
At week 48, 10% rated themselves as not infectious, 32% as low risk, 20% as medium risk, and 38% as highly at risk of transmission from unprotected sex.
These POI scores were at odds with the actual risk of infectiousness, however: At week 48, 91% of participants had HIV RNA levels of less than 50 copies per mL, the investigators found.
In multivariate analysis controlling for sociodemographic factors, sexual partner preferences and any stimulant drug use, factors associated with a greater probability of decline in POI included higher baseline POI, younger age, and higher level of education. In contrast, non-Hispanic blacks and patients with CD4 levels lower than 50 cells at the start of ART were less likely to have a decline in POI.
In all, 99 patients had a decline to a POI of not infectious. Factors associated with this change were baseline POI, female sex, and no stimulant drug use. Of those who thought of themselves as not infectious at week 48, 8 had HIV RNA levels about 50 copies/mL.
Interestingly, actual viral suppression was not associated with POI, Dr. Landovitz said.
In the briefing, he said that it’s incumbent on caregivers not to present patients with either/or choices, but instead to have a nuanced discussion about relative transmission risks. For example, if the patient has undetectable viral levels and is on treatment, is tested and treated for other sexually transmitted infections and has a known sexual dynamic, he or she probably has a very low risk of transmitting HIV to his/her sexual partner, he said.
However, “the challenge lies in messaging to patients that there are a lot of assumptions in that statement. What if the HIV-infected person has not been consistent with [his or her] antiretroviral therapy for whatever reason? ... What if there’s been something traumatic going on in their lives, or what if there has been a new substance abuse overlay that’s compromised their ability to adhere, and they’re no longer virologically suppressed as they thought they were at their last measurement? Then that’s not a guarantee [of low risk],” he said.
“I try and couch it to patients that based on what we know, if someone really is on treatment and undetectable, the risk of sexual transmission is very low. It’s probably not zero, but it’s very, very low,” he added.
Primary funding for ACGT A5257 came from the National Institute of Allergy and Infectious Diseases. Dr. Landovitz disclosed receiving research grants to his institution and consulting fees from Gilead Sciences.
BOSTON – Although antiretroviral therapy (ART) has been shown to reduce risk of HIV transmission, particularly among heterosexuals, there is a gap between patient perception of infectiousness and actual risk of HIV transmission, suggesting that clinicians need to do better at discussing implications with patients on treatment.
Among patients participating in a randomized clinical trial comparing three ART regimens, nearly half reported a decline in their perception of their own infectiousness (POI) at 48 weeks compared with study entry, but few participants thought themselves to be noninfectious at any time point, reported Dr. Raphael Landovitz of the David Geffen School of Medicine at the University of California, Los Angeles.
“We think this highlights some important opportunities for finding populations who need more education about what it means for their sexual partners in terms of their infectiousness by a sexual route as they achieve therapy, and I think as providers we can do a better job about contextualizing the benefits of antiretroviral therapy, not only for individuals, but for populations,” he said at a media briefing following his presentation of the data in an oral abstract session at the Conference on Retroviruses and Opportunistic Infections.
Dr. Landovitz and colleagues conducted a secondary analysis of data from the AIDS Clinical Trials Group (ACTG) A5257 Trial, which compared tenofovir/emtricitabine in combination with either atazanavir, raltegravir, or darunavir.
Patients in the trial were asked at baseline and every 48 weeks to rate on a visual analog scale from 0 to 100 their response to the question, “How likely would you be to give someone HIV if you had unprotected sex with them today?” – with 0 being not at all infectious, and 100 being highly infectious.
At baseline, 6% had a POI of not at all infectious, 10% thought themselves to be at low risk for HIV transmission. 26% considered themselves at medium risk, and 58% had a POI of highly infectious.
At week 48, 10% rated themselves as not infectious, 32% as low risk, 20% as medium risk, and 38% as highly at risk of transmission from unprotected sex.
These POI scores were at odds with the actual risk of infectiousness, however: At week 48, 91% of participants had HIV RNA levels of less than 50 copies per mL, the investigators found.
In multivariate analysis controlling for sociodemographic factors, sexual partner preferences and any stimulant drug use, factors associated with a greater probability of decline in POI included higher baseline POI, younger age, and higher level of education. In contrast, non-Hispanic blacks and patients with CD4 levels lower than 50 cells at the start of ART were less likely to have a decline in POI.
In all, 99 patients had a decline to a POI of not infectious. Factors associated with this change were baseline POI, female sex, and no stimulant drug use. Of those who thought of themselves as not infectious at week 48, 8 had HIV RNA levels about 50 copies/mL.
Interestingly, actual viral suppression was not associated with POI, Dr. Landovitz said.
In the briefing, he said that it’s incumbent on caregivers not to present patients with either/or choices, but instead to have a nuanced discussion about relative transmission risks. For example, if the patient has undetectable viral levels and is on treatment, is tested and treated for other sexually transmitted infections and has a known sexual dynamic, he or she probably has a very low risk of transmitting HIV to his/her sexual partner, he said.
However, “the challenge lies in messaging to patients that there are a lot of assumptions in that statement. What if the HIV-infected person has not been consistent with [his or her] antiretroviral therapy for whatever reason? ... What if there’s been something traumatic going on in their lives, or what if there has been a new substance abuse overlay that’s compromised their ability to adhere, and they’re no longer virologically suppressed as they thought they were at their last measurement? Then that’s not a guarantee [of low risk],” he said.
“I try and couch it to patients that based on what we know, if someone really is on treatment and undetectable, the risk of sexual transmission is very low. It’s probably not zero, but it’s very, very low,” he added.
Primary funding for ACGT A5257 came from the National Institute of Allergy and Infectious Diseases. Dr. Landovitz disclosed receiving research grants to his institution and consulting fees from Gilead Sciences.
BOSTON – Although antiretroviral therapy (ART) has been shown to reduce risk of HIV transmission, particularly among heterosexuals, there is a gap between patient perception of infectiousness and actual risk of HIV transmission, suggesting that clinicians need to do better at discussing implications with patients on treatment.
Among patients participating in a randomized clinical trial comparing three ART regimens, nearly half reported a decline in their perception of their own infectiousness (POI) at 48 weeks compared with study entry, but few participants thought themselves to be noninfectious at any time point, reported Dr. Raphael Landovitz of the David Geffen School of Medicine at the University of California, Los Angeles.
“We think this highlights some important opportunities for finding populations who need more education about what it means for their sexual partners in terms of their infectiousness by a sexual route as they achieve therapy, and I think as providers we can do a better job about contextualizing the benefits of antiretroviral therapy, not only for individuals, but for populations,” he said at a media briefing following his presentation of the data in an oral abstract session at the Conference on Retroviruses and Opportunistic Infections.
Dr. Landovitz and colleagues conducted a secondary analysis of data from the AIDS Clinical Trials Group (ACTG) A5257 Trial, which compared tenofovir/emtricitabine in combination with either atazanavir, raltegravir, or darunavir.
Patients in the trial were asked at baseline and every 48 weeks to rate on a visual analog scale from 0 to 100 their response to the question, “How likely would you be to give someone HIV if you had unprotected sex with them today?” – with 0 being not at all infectious, and 100 being highly infectious.
At baseline, 6% had a POI of not at all infectious, 10% thought themselves to be at low risk for HIV transmission. 26% considered themselves at medium risk, and 58% had a POI of highly infectious.
At week 48, 10% rated themselves as not infectious, 32% as low risk, 20% as medium risk, and 38% as highly at risk of transmission from unprotected sex.
These POI scores were at odds with the actual risk of infectiousness, however: At week 48, 91% of participants had HIV RNA levels of less than 50 copies per mL, the investigators found.
In multivariate analysis controlling for sociodemographic factors, sexual partner preferences and any stimulant drug use, factors associated with a greater probability of decline in POI included higher baseline POI, younger age, and higher level of education. In contrast, non-Hispanic blacks and patients with CD4 levels lower than 50 cells at the start of ART were less likely to have a decline in POI.
In all, 99 patients had a decline to a POI of not infectious. Factors associated with this change were baseline POI, female sex, and no stimulant drug use. Of those who thought of themselves as not infectious at week 48, 8 had HIV RNA levels about 50 copies/mL.
Interestingly, actual viral suppression was not associated with POI, Dr. Landovitz said.
In the briefing, he said that it’s incumbent on caregivers not to present patients with either/or choices, but instead to have a nuanced discussion about relative transmission risks. For example, if the patient has undetectable viral levels and is on treatment, is tested and treated for other sexually transmitted infections and has a known sexual dynamic, he or she probably has a very low risk of transmitting HIV to his/her sexual partner, he said.
However, “the challenge lies in messaging to patients that there are a lot of assumptions in that statement. What if the HIV-infected person has not been consistent with [his or her] antiretroviral therapy for whatever reason? ... What if there’s been something traumatic going on in their lives, or what if there has been a new substance abuse overlay that’s compromised their ability to adhere, and they’re no longer virologically suppressed as they thought they were at their last measurement? Then that’s not a guarantee [of low risk],” he said.
“I try and couch it to patients that based on what we know, if someone really is on treatment and undetectable, the risk of sexual transmission is very low. It’s probably not zero, but it’s very, very low,” he added.
Primary funding for ACGT A5257 came from the National Institute of Allergy and Infectious Diseases. Dr. Landovitz disclosed receiving research grants to his institution and consulting fees from Gilead Sciences.
AT CROI 2016
Key clinical point:. HIV-infected persons’ perceptions of infectiousness may affect their sexual behaviors and risk of HIV transmission.
Major finding: Only a few participants in a trial of antiretroviral therapy thought of themselves as noninfectious after 48 weeks of therapy.
Data source: Secondary analysis of a randomized clinical trial comparing three antiretroviral regimens in 1809 ART-naive persons infected with HIV.
Disclosures: Primary funding for ACGT A5257 came from the National Institute of Allergy and Infectious Diseases. Dr. Landovitz disclosed receiving research grants to his institution and consulting fees from Gilead Sciences.