User login
Bronchiolitis Diagnosis and Treatment Still Difficult
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
EXPERT ANALYSIS FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
What Have We Learned From European Birth Cohort Studies?
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
What Have We Learned From European Birth Cohort Studies?
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
LONDON – Food allergy is most commonly linked to hen’s eggs in Berlin, breastfeeding protects against the development of asthma, and both asthma and atopic disease are not one but several related conditions.
These are just a few of the recent findings obtained from European birth cohort studies, and reported at the Excellence in Paediatrics annual meeting.
“Birth cohort studies provide an opportunity to examine the effects of environmental influences on child health and development,” said Dr. Giorgio Tamburlini, research director at the Institute of Child Health (IRCCS) Burlo Garofolo in Trieste, Italy. Such studies also allow complex interactions between genes and the environment to be explored.
Over the past 2 decades, interest has grown in the performance of large, longitudinal studies of pregnant women and their newborn babies. This stems from “mounting evidence that many diseases and conditions have causes that start shortly after conception,” Dr. Tamburlini observed. “Factors that influence early organ and system development may have profound effects on health during childhood, as well as during later life.”
Food allergy is an increasingly common problem among young children, and data from EuroPrevall have started to provide much needed information on its prevalence and causes. The project started in 2005 and ended in December 2009. Early findings obtained at the Charité University Medical Center Berlin – one of the many centers contributing to the EuroPrevall birth cohort – showed that 402 (26%) of 1,568 children aged 2.5 years or younger had a possible food allergy.
The results of double-blind, placebo-controlled food challenge tests showed that hen’s egg, peanut, cow’s milk, and wheat were the most common causes of food allergy. Estimating the overall prevalence of food allergy showed that about 2% of children had developed clinically relevant food allergy, accounting for “a tenth of those with suspected reactions,” said study investigator Dr. Thomas Keil of Charité.
“We are excited to see the results from other centers,” Dr. Keil added, noting that there may well be some differences from the Berlin findings, not only in prevalence but also in the allergens responsible. “EuroPrevall will hopefully provide good data on the prevalence patterns, risk factors, quality of life, and costs of food allergies in European children.”
Importantly, the EuroPrevall data have been collected via standardized methods, meaning that the natural course of food allergies among the participating European centers can be compared. This will help researchers examine possible risk factors for food allergy, Dr. Keil said.
Other recent data from the BAMSE (Barn Allergi Milieu Stockholm Epidemiologi) birth cohort have shown a protective role of breastfeeding on the development of asthma. Children who were breastfed for at least 4 months were significantly less likely to develop asthma by the age of 8 years than were those breastfed for fewer than 4 months (J. Allergy Clin. Immunol. 2010;125:1013-9).
The BAMSE birth cohort was established between 1994 and 1996, said Dr. Anna Bergström of the Institute of Environmental Medicine at the Karolinska Institutet in Stockholm. Starting out with more than 4,000 children, the cohort has been reevaluated multiple times – at 1, 2, 4, 8, and 12 years – with the 16-year follow-up begun in November 2010 and clinical examinations scheduled for January 2011.
“Several of the studies in the BAMSE cohort have suggested that it is important to consider disease-related modification of exposure when you study allergic disease in children,” Dr. Bergström observed.
For instance, recent findings of one unpublished study showed that the consumption of certain fruits and vegetables may temper the chances of developing allergic disease. “Consumption of total fruit, apples and pears, carrots, and legumes was inversely associated with allergic disease,” Dr. Bergström explained. However, after excluding children with food-related allergic symptoms, the associations mostly disappeared, suggesting that the avoidance of certain foods by affected children had influenced the associations.
Recent findings from the MAAS (Manchester Asthma and Allergy Study) cohort have shown that asthma and atopic disease are not single but most likely multiple diseases. MAAS started in 1995 and was designed to identify risk factors for the development of asthma and allergies in early life.
“In the 19th century, in textbooks of pediatrics, we had a disease that was called fever,” said Dr. Adnan Custovic, professor of allergy and head of the respiratory research group at University Hospital of South Manchester (England), which runs the MAAS.
“We have learned better; nobody would call a disease ‘fever’ nowadays,” Dr. Custovic said. “I certainly hope than in 10 years’ time that asthma will be confined to history just as much as fever has been confined to the history of diseases.”
Although much useful data can be obtained from a birth cohort study, there are several challenges to be faced when conducting such a study. One of these is the cost. Performing “open-ended” studies that may proceed for many years can be financially draining, said Dr. Tamburlini, who noted that sponsors often like to see results much faster than they can be obtained.
“One of the clear lessons is that the potential of birth cohort studies for scientific output can be maximized by collaboration between studies,” Dr. Tamburlini said. Not only does this mean shared costs, but also that data could be compared to achieve results faster.
The sharing of data may just be an ideal at the current time, as it depends on data being collected and documented in a similar, standardized way in all studies, but initiatives to improve data sharing are underway.
One such initiative is Birthcohorts.net, which aims to act as an inventory of all birth cohort studies performed around the globe. For inclusion in the database, studies need to include at least 250 children, involve the collection of biological specimens from the child and/or parents, and obtain information on parental exposures during pregnancy. Data from the cohort also need to be accessible for research collaboration, at least in theory.
Through collaborations and “more uniform data collection,” the results of birth cohort studies open up the possibility of pooling data, Dr. Tamburlini said. This means much greater power to detect how childhood diseases develop and “the impact of early exposures on children at risk.”
Dr. Tamburlini, Dr. Keil, Dr. Bergström, and Dr. Custovic did not report any conflicts of interest.
FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Scan Neonatal Brain Early to Optimize Results
LONDON – Magnetic resonance imaging should be used as early as possible to scan the neonatal brain if there are any unexplained symptoms, or if hemorrhagic or thrombotic lesions are suspected.
In the case of thrombosis, it’s important to scan early to decide whether anticoagulation is required, neonatal imaging expert Dr. Mary A. Rutherford of Imperial College London said at the Excellence in Paediatrics annual meeting.
However, Dr. Rutherford, who trained as a pediatrician, noted that for acquired injuries, the use of conventional MRI should be delayed 1-4 weeks, as hypoxic-ischemic brain injury is easier to detect 7 days after the insult.
MRI can be used for a variety of diagnostic and prognostic reasons in full-term neonates; it can help to establish the cause of symptoms, identify brain abnormalities, and determine the likely timing of any injury to the developing brain, she said. Neonatal MRI can also help predict outcomes, provide information for risk management and, in these days of increased medicolegal vigilance, perhaps help clinicians avoid the threat of litigation.
Today, most clinical departments will have an MRI scanner that uses field strengths of 1.5-3 Tesla, which are fine for neonatal imaging, Dr. Rutherford said. "What you really need," she noted, "is an interested radiologist or radiographer." Myelination occurs during the first 2 years of life, so an experienced pediatric or radiology image interpreter is also required.
As access to MRI scanners may be limited, it’s important to be ready as soon as a scanner is free, Dr. Rutherford advised. This means that the neonate must be suitably prepared prior to the scan. Choral hydrate, given 15 minutes before the scan, may be used to keep the neonate sedated temporarily, and ear protection must be worn. The neonate’s head and body should then be "wrapped and fixed" as carefully as possibly into position inside the scanner, so there is little chance of any waking or movement during the scan.
Ventilation may be needed during the scan, and a pediatric staff member needs to be with the baby at all times. Pulse oximetry can be used to monitor the neonate while the scan is in progress.
"MRI is an expensive technology, and you really want to make sure that you get the best possible results from all the effort that is put in by trying to put a baby into an MRI scanner," Dr. Rutherford said.
A key element to successful scanning is ensuring that the MRI coil used fits as closely as possibly to the neonate’s head. "Poor coil choice or head positioning results in poor image quality," she warned.
Motion is another common reason for poor quality images, so motion-resistant sequences need to be considered. T1-weighted (transverse/sagittal), T2-weighted (transverse), and diffusion-weighted imaging may all be appropriate sequences to use. Magnetic resonance venography and angiography can provide useful information about thrombosis or stroke, respectively.
"In this day and age, all infants with a neonatal encephalopathy require – and deserve to have – the benefit of an MR scan," Dr. Rutherford said. Other candidates for MRI include neonates with seizures, severe jaundice, abnormal cranial ultrasound findings, unexplained neurologic signs, dysmorphic features, and where a co-twin has died in utero.
Neonates with unexplained symptoms or who are at risk of hemorrhagic/thrombotic lesions require prompt MRI, as soon as access to a scanner can be arranged.
"You will also want to image fairly quickly in cases of severe neonatal encephalopathy, especially if you are considering withdrawing active treatment," Dr. Rutherford said.
By contrast, for acquired injuries, she noted, "If we want to get the best possible detection of any acquired injury, then we should think about imaging probably between 1 and 4 weeks post insult." Diffusion-weighted imaging is best for identifying early ischemic lesions.
With regards to preterm neonates, routine MRI scanning is not recommended, but early scanning is perhaps advisable if there are unexplained symptoms or withdrawal of care is being considered.
Dr. Rutherford is the editor of "MRI of the Neonatal Brain," (Philadelphia: Saunders, Ltd., 2001). More information: MRI of the Neonatal Brain.
LONDON – Magnetic resonance imaging should be used as early as possible to scan the neonatal brain if there are any unexplained symptoms, or if hemorrhagic or thrombotic lesions are suspected.
In the case of thrombosis, it’s important to scan early to decide whether anticoagulation is required, neonatal imaging expert Dr. Mary A. Rutherford of Imperial College London said at the Excellence in Paediatrics annual meeting.
However, Dr. Rutherford, who trained as a pediatrician, noted that for acquired injuries, the use of conventional MRI should be delayed 1-4 weeks, as hypoxic-ischemic brain injury is easier to detect 7 days after the insult.
MRI can be used for a variety of diagnostic and prognostic reasons in full-term neonates; it can help to establish the cause of symptoms, identify brain abnormalities, and determine the likely timing of any injury to the developing brain, she said. Neonatal MRI can also help predict outcomes, provide information for risk management and, in these days of increased medicolegal vigilance, perhaps help clinicians avoid the threat of litigation.
Today, most clinical departments will have an MRI scanner that uses field strengths of 1.5-3 Tesla, which are fine for neonatal imaging, Dr. Rutherford said. "What you really need," she noted, "is an interested radiologist or radiographer." Myelination occurs during the first 2 years of life, so an experienced pediatric or radiology image interpreter is also required.
As access to MRI scanners may be limited, it’s important to be ready as soon as a scanner is free, Dr. Rutherford advised. This means that the neonate must be suitably prepared prior to the scan. Choral hydrate, given 15 minutes before the scan, may be used to keep the neonate sedated temporarily, and ear protection must be worn. The neonate’s head and body should then be "wrapped and fixed" as carefully as possibly into position inside the scanner, so there is little chance of any waking or movement during the scan.
Ventilation may be needed during the scan, and a pediatric staff member needs to be with the baby at all times. Pulse oximetry can be used to monitor the neonate while the scan is in progress.
"MRI is an expensive technology, and you really want to make sure that you get the best possible results from all the effort that is put in by trying to put a baby into an MRI scanner," Dr. Rutherford said.
A key element to successful scanning is ensuring that the MRI coil used fits as closely as possibly to the neonate’s head. "Poor coil choice or head positioning results in poor image quality," she warned.
Motion is another common reason for poor quality images, so motion-resistant sequences need to be considered. T1-weighted (transverse/sagittal), T2-weighted (transverse), and diffusion-weighted imaging may all be appropriate sequences to use. Magnetic resonance venography and angiography can provide useful information about thrombosis or stroke, respectively.
"In this day and age, all infants with a neonatal encephalopathy require – and deserve to have – the benefit of an MR scan," Dr. Rutherford said. Other candidates for MRI include neonates with seizures, severe jaundice, abnormal cranial ultrasound findings, unexplained neurologic signs, dysmorphic features, and where a co-twin has died in utero.
Neonates with unexplained symptoms or who are at risk of hemorrhagic/thrombotic lesions require prompt MRI, as soon as access to a scanner can be arranged.
"You will also want to image fairly quickly in cases of severe neonatal encephalopathy, especially if you are considering withdrawing active treatment," Dr. Rutherford said.
By contrast, for acquired injuries, she noted, "If we want to get the best possible detection of any acquired injury, then we should think about imaging probably between 1 and 4 weeks post insult." Diffusion-weighted imaging is best for identifying early ischemic lesions.
With regards to preterm neonates, routine MRI scanning is not recommended, but early scanning is perhaps advisable if there are unexplained symptoms or withdrawal of care is being considered.
Dr. Rutherford is the editor of "MRI of the Neonatal Brain," (Philadelphia: Saunders, Ltd., 2001). More information: MRI of the Neonatal Brain.
LONDON – Magnetic resonance imaging should be used as early as possible to scan the neonatal brain if there are any unexplained symptoms, or if hemorrhagic or thrombotic lesions are suspected.
In the case of thrombosis, it’s important to scan early to decide whether anticoagulation is required, neonatal imaging expert Dr. Mary A. Rutherford of Imperial College London said at the Excellence in Paediatrics annual meeting.
However, Dr. Rutherford, who trained as a pediatrician, noted that for acquired injuries, the use of conventional MRI should be delayed 1-4 weeks, as hypoxic-ischemic brain injury is easier to detect 7 days after the insult.
MRI can be used for a variety of diagnostic and prognostic reasons in full-term neonates; it can help to establish the cause of symptoms, identify brain abnormalities, and determine the likely timing of any injury to the developing brain, she said. Neonatal MRI can also help predict outcomes, provide information for risk management and, in these days of increased medicolegal vigilance, perhaps help clinicians avoid the threat of litigation.
Today, most clinical departments will have an MRI scanner that uses field strengths of 1.5-3 Tesla, which are fine for neonatal imaging, Dr. Rutherford said. "What you really need," she noted, "is an interested radiologist or radiographer." Myelination occurs during the first 2 years of life, so an experienced pediatric or radiology image interpreter is also required.
As access to MRI scanners may be limited, it’s important to be ready as soon as a scanner is free, Dr. Rutherford advised. This means that the neonate must be suitably prepared prior to the scan. Choral hydrate, given 15 minutes before the scan, may be used to keep the neonate sedated temporarily, and ear protection must be worn. The neonate’s head and body should then be "wrapped and fixed" as carefully as possibly into position inside the scanner, so there is little chance of any waking or movement during the scan.
Ventilation may be needed during the scan, and a pediatric staff member needs to be with the baby at all times. Pulse oximetry can be used to monitor the neonate while the scan is in progress.
"MRI is an expensive technology, and you really want to make sure that you get the best possible results from all the effort that is put in by trying to put a baby into an MRI scanner," Dr. Rutherford said.
A key element to successful scanning is ensuring that the MRI coil used fits as closely as possibly to the neonate’s head. "Poor coil choice or head positioning results in poor image quality," she warned.
Motion is another common reason for poor quality images, so motion-resistant sequences need to be considered. T1-weighted (transverse/sagittal), T2-weighted (transverse), and diffusion-weighted imaging may all be appropriate sequences to use. Magnetic resonance venography and angiography can provide useful information about thrombosis or stroke, respectively.
"In this day and age, all infants with a neonatal encephalopathy require – and deserve to have – the benefit of an MR scan," Dr. Rutherford said. Other candidates for MRI include neonates with seizures, severe jaundice, abnormal cranial ultrasound findings, unexplained neurologic signs, dysmorphic features, and where a co-twin has died in utero.
Neonates with unexplained symptoms or who are at risk of hemorrhagic/thrombotic lesions require prompt MRI, as soon as access to a scanner can be arranged.
"You will also want to image fairly quickly in cases of severe neonatal encephalopathy, especially if you are considering withdrawing active treatment," Dr. Rutherford said.
By contrast, for acquired injuries, she noted, "If we want to get the best possible detection of any acquired injury, then we should think about imaging probably between 1 and 4 weeks post insult." Diffusion-weighted imaging is best for identifying early ischemic lesions.
With regards to preterm neonates, routine MRI scanning is not recommended, but early scanning is perhaps advisable if there are unexplained symptoms or withdrawal of care is being considered.
Dr. Rutherford is the editor of "MRI of the Neonatal Brain," (Philadelphia: Saunders, Ltd., 2001). More information: MRI of the Neonatal Brain.
EXPERT ANALYSIS FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Propranolol Plus Laser Equals New Option for Infantile Hemangiomas
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
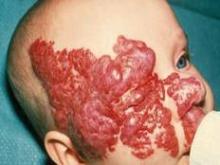
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Major Finding: Of 14 infants given propranolol in combination with laser therapy, only 1 child experienced a rebound of their hemangioma.
Data Source: Prospective, observational study of 23 infants with large facial hemangiomas that were causing severe functional impairment.
Disclosures: Dr. Poetke said she had no relevant financial disclosures.
Propranolol/Laser Therapy Offers New Option for Infantile Hemangioma
LONDON – The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON – The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON – The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Bronchiolitis Diagnosis and Treatment Still Difficult
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
EXPERT ANALYSIS FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Bronchiolitis Diagnosis and Treatment Still Difficult
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
LONDON – Primary care and emergency physicians face significant difficulties in the diagnosis and treatment of bronchiolitis, particularly during the winter months when the prevalence of the condition rises.
Part of the problem is making a differential diagnosis, compounded by the lack of available evidence-based treatments, experts said at the Excellence in Paediatrics annual meeting in London.
Primary care physicians and general practitioners (GPs) are often not comfortable making a diagnosis of bronchiolitis, said Dr. Mike Thomas, an Asthma UK senior research fellow at the University of Aberdeen (Scotland). "There isn’t a simple, gold-standard diagnostic test, which makes things rather difficult," he observed.
Bronchiolitis typically occurs in infants aged 3-6 months, and a diagnosis is often based on the presenting symptoms, which may include difficulty in breathing, wheeze, crackles on auscultation, cough, and even apnea in very young babies. General irritability and poor feeding may also be apparent.
These symptoms are shared with several other respiratory conditions, such as asthma, viral-induced wheeze, bacterial lower respiratory tract infection, pneumonia, and some rarer lung diseases such as cystic fibrosis.
Investigations – chest x-ray, hematology, and virology – are not routinely recommended, and even when a diagnosis is made, "we’re not 100% sure what to do," Dr. Thomas said.
Evidence-based treatments for the condition are lacking, Dr. Thomas said, with current practice guidelines set in 2006 in both the United Kingdom and United States tending to give advice on what not to do rather than what treatment to give.
"The bottom line is that there is no evidence-based specific treatment in prehospitalized infants ... and we’re left giving standard advice to children with viral illness on the use of fluids and antipyretics."
Dr. Joan L. Robinson, professor of pediatrics at Stollery Children’s Hospital in Edmonton, Alberta, noted that problems in diagnosing and treating bronchiolitis also exist in the ED.
Indeed, evidence shows that ED physicians and radiologists may interpret chest X-rays very differently, often misdiagnosing bronchiolitis as bacterial pneumonia (J. Pediatr. 2007;150:429-33; Pediatr. Pulmonol. 2009;44:122-7).
"Chest x-ray in a typical case of bronchiolitis leads to overdiagnosis of pneumonia and therefore overuse of antibiotics," Dr. Robinson cautioned.
Viral testing has its pros and cons, but it is probably not cost effective in the majority of non–high-risk outpatient cases, she added. "There is no clear correct answer as to whether hospitals should encourage routine testing for inpatients," Dr. Robinson observed.
Dr. Steve Cunningham, a consultant respiratory pediatrician at the Royal Hospital for Sick Children in Edinburgh, commented that treatments for bronchiolitis range from those that aim to improve airflow to those that reduce mucosal inflammation, lessen edema, or improve mucous movement.
Of all available treatments, however, only continuous positive airway pressure and nasal hypertonic saline had any, although still questionable, effect.
With the difficulties in diagnosis and treatment, it becomes all the more important for parents and other caregivers to be well informed about bronchiolitis and how to recognize the signs of a child’s possible deterioration.
"Most infants with bronchiolitis will have a mild illness that can be managed at home," Dr. Thomas said. Caregivers need to know, however, that there is "no cure," and that while symptoms may disappear at around 2 weeks in half of all affected infants, prolonged illness can result in others. It is unclear if there is a higher risk of developing asthma later in life.
Together with general advice on hygiene and regular hand-washing, physicians should remind caregivers that other factors, such as breast-feeding and passive smoking, can have an effect on the child’s health.
"There is also need for better education for GPs and a better evidence base for management," Dr. Thomas suggested. Primary care and general practitioners are uniquely placed to help monitor infants and young children, possibly preventing the need for emergency hospital admission.
Dr. Thomas, Dr. Robinson, and Dr. Cunningham said that they had no conflicts of interest.
EXPERT ANALYSIS FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Hib-MenC-TT Vaccine Works When Given With Pneumococcal Vaccines
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).
Major Finding: At 2 years post vaccination, 82% of children who received HibMenC-TT concomitantly with a pneumococcal conjugate vaccine still had antibodies against Neisseria meningitidis serogroup C, and 100% had antibodies against Haemophilus influenzae type B.
Data Source: Phase IIIB, open, long-term, multicenter, follow-up study of 581 children who were vaccinated with the Hib-MenC-TT conjugate vaccine (Menitorix) or one of two meningococcal vaccines (Meningitec or NeisVac-C) in combination with one of two conjugate pneumococcal vaccines (Synflorix or Prevnar).
Disclosures: GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth.
Hib-MenC-TT Vaccine Works When Given With Pneumococcal Vaccines
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).
LONDON – Children remain protected against common influenza- and meningitis-causing bacteria for up to 2 years when they were vaccinated using the Hib-MenC-TT (Haemophilus influenzae type b/meningitis C/tetanus toxoid) vaccine in conjunction with one of two conjugate pneumococcal vaccines, according to phase IIIB study results.
More than 80% of children retained antibodies against Neisseria meningitidis serogroup C, and 100% retained antibodies against H. influenzae type b after completion of a full vaccination course.
"This study assessed the long-term persistence of MenC and Hib antibodies approximately 2 years after completion of a full vaccination course with HibMenC-TT, or the control vaccines MenC-CRM197 or MenC-TT, when coadministered with DTPa-containing (or DTPa/Hib-containing) and pneumococcal vaccines," explained study investigator Dr. Ryszard Konior.
Dr. Konior of John Paul II Hospital in Krakow, Poland, reported the findings at the Excellence in Paediatrics annual meeting.
In all, 581 children were evaluated during the study. All received a primary vaccination course at 2, 4, and 6 months of age, a booster vaccination at 11-18 months, and reassessment at 36-40 months.
Children were randomized to one of the following four groups and received various combinations of vaccines for the primary and booster vaccinations:
• Children in the Pn-Men group (n = 144) received a meningitis C conjugate vaccine (MenC-CRM197 [Wyeth’s Meningitec]); a diphtheria, tetanus toxoid, acellular pertussis–hepatitis B virus–polio virus inactivated/H. influenzae type b vaccine (DTPa-HBV-IPV/Hib [GlaxoSmithKline’s Infanrix hexa]); and a pneumococcal conjugate vaccine (nontypeable H. influenzae [NTHi], protein D, diphtheria or tetanus toxoid conjugates) adsorbed (10Pn-PD-DiT [GSK’s Synflorix]) for primary vaccination, followed by MenC-CRM197, a DTPa/Hib-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pn-Neis group (n = 147) received the same vaccines as did the Pn-Men group, with the exception being the use of MenC-TT (Baxter’s NeisVac-C) in place of MenC-CRM197.
• Children in the Pn-HibC group (n = 149) were given Hib-MenC-TT (GSK’s Menitorix), DTPa-HBV-IPV/Hib, and 10Pn-PD-DiT for primary vaccination and vaccination, followed by Hib-MenC-TT, a DTPa-containing vaccine, and 10Pn-PD-DiT for booster vaccination.
• Children in the Pr-HibC group (n = 141) were given the same vaccines as was the Pn-HibC group, with the exception being that 10Pn-PD-DiT was replaced with a seven valent pneumococcal conjugate vaccine (7vCRM [Pfizer’s Prevnar]).
"More than 82% of subjects retained rSBA [rabbit serum bactericidal antibodies] titers [greater than or equal to] 1:8 at 2 years post booster vaccination," said Dr. Konior, which showed sustained protection against the meningitis-causing bacteria. The percentage of children with antibody titers above this threshold was similar in the Pn-Men, Pn-HibC, and Pr-HibC groups, albeit lower than the percentage in the Pn-Neis group.
In addition, all children had anti-PRP (polyribosylribitol phosphate) greater than or equal to 0.15 mcg/mL, indicating that they remained protected against H. influenzae infection. The best results were achieved in the Pn-HibC group, with the lowest antibody titers observed in the groups with a DTPa/Hib-containing vaccine (that is, Pn-Neis and Pn-Men).
Dr. Konior reported that there were no safety concerns. He concluded that these results suggest that seropositivity and seroprotection against both N. meningitidis serogroup C and H. influenzae type B persists in most children up to 3 years of age or older, and that the results favor the use of Hib-MenC-TT (Menitorix) in conjunction with conjugate pneumococcal vaccines.
GlaxoSmithKline Biologicals in Rixensart, Belgium, supported the study. Dr. Konior has participated in clinical vaccine studies sponsored by GSK, Baxter, Novartis Vaccines, and Wyeth (now part of Pfizer).