User login
Researchers Confirm Psoriatic Arthritis Risk Allele
European researchers have confirmed a new independent susceptibility allele for psoriatic arthritis that could possibly represent a new candidate pharmacogenetic marker for the disease.
"In this collaborative work, we replicated the association of TNF*-857T as a susceptibility allele for [psoriatic arthritis (PsA)] independent of the main PSORS1 risk allele," wrote Emiliano Giardina, Ph.D., of the University of Rome, and his colleagues in an article published online in Arthritis & Rheumatism (doi:10.1002/art.30591).
It’s long been known that the strongest and most replicated susceptibility region for psoriatic vulgaris – and by extension PsA – is within the major histocompatibility complex (MHC) region (PSORS1-psoriasis susceptibility region). "This locus maps to chromosome 6p21.3, comprising many different class I antigens associated with disease expression. Human leukocyte antigen (HLA)-C was repetitively reported as the PSORS1 gene and HLA-Cw*06:02 as the susceptibility allele," they noted.
In this study, the researchers attempted to confirm this finding by assessing allele and genotype frequencies of TNF*-857 in three independent cohorts. They included a German cohort (374 cases and 561 controls), an Italian cohort (400 cases and 400 controls), and a British cohort (135 cases and 354 controls.
The overall cohort of 2,224 individuals of European ancestry was assessed for distribution of HLA-Cw*06:02/PSORS1 risk allele and also was typed for TNF*-857T. The overall allele frequency of TNF*-857T was significantly higher in individuals with PsA (27%) than in control individuals (20%).
The researchers calculated the genotype frequencies of TNF*-857T in samples that were positive and negative for the PSORS1 risk allele, in order to verify the existence of an association independent of the PSORS1 risk allele.
"Overall, the frequency of heterozygous or homozygous carriers of TNF*-857T (TT/CT) in individuals negative for the PSORS1/HLA-C risk allele was significantly higher in PsA patients (30%) than in control subjects (21%)," they reported. This yielded an odds ratio of 1.35
"As expected, the haplotype analysis confirmed TNF*-857T as a susceptibility factor independent of the PSORS1/HLA-C risk allele," they wrote. Association of PsA to TNF*-857T was significant in individuals not carrying the PSORS1/HLA-C risk allele, with an odds ratio of 1.27.
"Although the functional role of TNF*-857T remains to be determined, previous data could show that the allele T increases the transcription of TNF-alpha." In addition, tumor necrosis factor–alpha is known to play a pivotal role in both the activation and extravasation of T-cells in the highly vascularized synovium, as well as in subchondral osteoclastogenesis promoting bone erosions." Genes encoding for TNF-alpha, along with other cytokines, could be candidate pharmacogenetic markers.
The study was supported by a research grant from the Italian Association for the Defense of Psoriatic Patients; the Interdisciplinary Centre for Clinical Research at the University of Erlangen-Nuremberg, Germany; and the Bath Institute for Rheumatic Diseases. Two researchers were received grants from Wyeth-Pharm GmbH (Germany).
A most intriguing aspect of psoriasis epidemiology is that about a quarter of these patients will develop psoriatic arthritis, and this disease clusters in families with remarkably high heritability. Despite evidence for genetic factors in this disease, the search for genes associated with arthritis and not psoriasis has been challenging because almost all PsA patients also have psoriasis. PSORS-1, the MHC region that contains Cw6, the allele with the strongest association with psoriasis, is characterized by long linkage disequilibrium. One report noted an association of PsA with the TNF*-857T allele that was independent of PSORS1. In this multinational study of 909 patients and 1,315 healthy controls, the TNF*-857T allele was found at significantly higher frequency in PsA patients negative for the PSORS1 allele (30%), compared with controls (21%). This study replicates findings in the previous study and is also of note because the TNF*-867T allele increases the transcription of TNF, a pivotal cytokine in the pathogenesis of PsA. Also of possible relevance is that this allele is associated with response to etanercept in RA. The replication of this important association should catalyze additional genetic and pharmacogenetic studies to better understand the diagnostic and functional significance of this allele in psoriatic disease.
Christopher T. Ritchlin, M.D., is professor of medicine, allergy/immunology, and rheumatology at the University of Rochester (N.Y.) He reported having no conflicts of interest that are relevant to this piece.
A most intriguing aspect of psoriasis epidemiology is that about a quarter of these patients will develop psoriatic arthritis, and this disease clusters in families with remarkably high heritability. Despite evidence for genetic factors in this disease, the search for genes associated with arthritis and not psoriasis has been challenging because almost all PsA patients also have psoriasis. PSORS-1, the MHC region that contains Cw6, the allele with the strongest association with psoriasis, is characterized by long linkage disequilibrium. One report noted an association of PsA with the TNF*-857T allele that was independent of PSORS1. In this multinational study of 909 patients and 1,315 healthy controls, the TNF*-857T allele was found at significantly higher frequency in PsA patients negative for the PSORS1 allele (30%), compared with controls (21%). This study replicates findings in the previous study and is also of note because the TNF*-867T allele increases the transcription of TNF, a pivotal cytokine in the pathogenesis of PsA. Also of possible relevance is that this allele is associated with response to etanercept in RA. The replication of this important association should catalyze additional genetic and pharmacogenetic studies to better understand the diagnostic and functional significance of this allele in psoriatic disease.
Christopher T. Ritchlin, M.D., is professor of medicine, allergy/immunology, and rheumatology at the University of Rochester (N.Y.) He reported having no conflicts of interest that are relevant to this piece.
A most intriguing aspect of psoriasis epidemiology is that about a quarter of these patients will develop psoriatic arthritis, and this disease clusters in families with remarkably high heritability. Despite evidence for genetic factors in this disease, the search for genes associated with arthritis and not psoriasis has been challenging because almost all PsA patients also have psoriasis. PSORS-1, the MHC region that contains Cw6, the allele with the strongest association with psoriasis, is characterized by long linkage disequilibrium. One report noted an association of PsA with the TNF*-857T allele that was independent of PSORS1. In this multinational study of 909 patients and 1,315 healthy controls, the TNF*-857T allele was found at significantly higher frequency in PsA patients negative for the PSORS1 allele (30%), compared with controls (21%). This study replicates findings in the previous study and is also of note because the TNF*-867T allele increases the transcription of TNF, a pivotal cytokine in the pathogenesis of PsA. Also of possible relevance is that this allele is associated with response to etanercept in RA. The replication of this important association should catalyze additional genetic and pharmacogenetic studies to better understand the diagnostic and functional significance of this allele in psoriatic disease.
Christopher T. Ritchlin, M.D., is professor of medicine, allergy/immunology, and rheumatology at the University of Rochester (N.Y.) He reported having no conflicts of interest that are relevant to this piece.
European researchers have confirmed a new independent susceptibility allele for psoriatic arthritis that could possibly represent a new candidate pharmacogenetic marker for the disease.
"In this collaborative work, we replicated the association of TNF*-857T as a susceptibility allele for [psoriatic arthritis (PsA)] independent of the main PSORS1 risk allele," wrote Emiliano Giardina, Ph.D., of the University of Rome, and his colleagues in an article published online in Arthritis & Rheumatism (doi:10.1002/art.30591).
It’s long been known that the strongest and most replicated susceptibility region for psoriatic vulgaris – and by extension PsA – is within the major histocompatibility complex (MHC) region (PSORS1-psoriasis susceptibility region). "This locus maps to chromosome 6p21.3, comprising many different class I antigens associated with disease expression. Human leukocyte antigen (HLA)-C was repetitively reported as the PSORS1 gene and HLA-Cw*06:02 as the susceptibility allele," they noted.
In this study, the researchers attempted to confirm this finding by assessing allele and genotype frequencies of TNF*-857 in three independent cohorts. They included a German cohort (374 cases and 561 controls), an Italian cohort (400 cases and 400 controls), and a British cohort (135 cases and 354 controls.
The overall cohort of 2,224 individuals of European ancestry was assessed for distribution of HLA-Cw*06:02/PSORS1 risk allele and also was typed for TNF*-857T. The overall allele frequency of TNF*-857T was significantly higher in individuals with PsA (27%) than in control individuals (20%).
The researchers calculated the genotype frequencies of TNF*-857T in samples that were positive and negative for the PSORS1 risk allele, in order to verify the existence of an association independent of the PSORS1 risk allele.
"Overall, the frequency of heterozygous or homozygous carriers of TNF*-857T (TT/CT) in individuals negative for the PSORS1/HLA-C risk allele was significantly higher in PsA patients (30%) than in control subjects (21%)," they reported. This yielded an odds ratio of 1.35
"As expected, the haplotype analysis confirmed TNF*-857T as a susceptibility factor independent of the PSORS1/HLA-C risk allele," they wrote. Association of PsA to TNF*-857T was significant in individuals not carrying the PSORS1/HLA-C risk allele, with an odds ratio of 1.27.
"Although the functional role of TNF*-857T remains to be determined, previous data could show that the allele T increases the transcription of TNF-alpha." In addition, tumor necrosis factor–alpha is known to play a pivotal role in both the activation and extravasation of T-cells in the highly vascularized synovium, as well as in subchondral osteoclastogenesis promoting bone erosions." Genes encoding for TNF-alpha, along with other cytokines, could be candidate pharmacogenetic markers.
The study was supported by a research grant from the Italian Association for the Defense of Psoriatic Patients; the Interdisciplinary Centre for Clinical Research at the University of Erlangen-Nuremberg, Germany; and the Bath Institute for Rheumatic Diseases. Two researchers were received grants from Wyeth-Pharm GmbH (Germany).
European researchers have confirmed a new independent susceptibility allele for psoriatic arthritis that could possibly represent a new candidate pharmacogenetic marker for the disease.
"In this collaborative work, we replicated the association of TNF*-857T as a susceptibility allele for [psoriatic arthritis (PsA)] independent of the main PSORS1 risk allele," wrote Emiliano Giardina, Ph.D., of the University of Rome, and his colleagues in an article published online in Arthritis & Rheumatism (doi:10.1002/art.30591).
It’s long been known that the strongest and most replicated susceptibility region for psoriatic vulgaris – and by extension PsA – is within the major histocompatibility complex (MHC) region (PSORS1-psoriasis susceptibility region). "This locus maps to chromosome 6p21.3, comprising many different class I antigens associated with disease expression. Human leukocyte antigen (HLA)-C was repetitively reported as the PSORS1 gene and HLA-Cw*06:02 as the susceptibility allele," they noted.
In this study, the researchers attempted to confirm this finding by assessing allele and genotype frequencies of TNF*-857 in three independent cohorts. They included a German cohort (374 cases and 561 controls), an Italian cohort (400 cases and 400 controls), and a British cohort (135 cases and 354 controls.
The overall cohort of 2,224 individuals of European ancestry was assessed for distribution of HLA-Cw*06:02/PSORS1 risk allele and also was typed for TNF*-857T. The overall allele frequency of TNF*-857T was significantly higher in individuals with PsA (27%) than in control individuals (20%).
The researchers calculated the genotype frequencies of TNF*-857T in samples that were positive and negative for the PSORS1 risk allele, in order to verify the existence of an association independent of the PSORS1 risk allele.
"Overall, the frequency of heterozygous or homozygous carriers of TNF*-857T (TT/CT) in individuals negative for the PSORS1/HLA-C risk allele was significantly higher in PsA patients (30%) than in control subjects (21%)," they reported. This yielded an odds ratio of 1.35
"As expected, the haplotype analysis confirmed TNF*-857T as a susceptibility factor independent of the PSORS1/HLA-C risk allele," they wrote. Association of PsA to TNF*-857T was significant in individuals not carrying the PSORS1/HLA-C risk allele, with an odds ratio of 1.27.
"Although the functional role of TNF*-857T remains to be determined, previous data could show that the allele T increases the transcription of TNF-alpha." In addition, tumor necrosis factor–alpha is known to play a pivotal role in both the activation and extravasation of T-cells in the highly vascularized synovium, as well as in subchondral osteoclastogenesis promoting bone erosions." Genes encoding for TNF-alpha, along with other cytokines, could be candidate pharmacogenetic markers.
The study was supported by a research grant from the Italian Association for the Defense of Psoriatic Patients; the Interdisciplinary Centre for Clinical Research at the University of Erlangen-Nuremberg, Germany; and the Bath Institute for Rheumatic Diseases. Two researchers were received grants from Wyeth-Pharm GmbH (Germany).
FROM ARTHRITIS & RHEUMATISM
Major Finding: TNF*-857T is a susceptibility allele for PsA independent of the main PSORS1 risk allele.
Data Source: A study of 2,224 individuals.
Disclosures: The study was supported by a research grant from the Italian Association for the Defense of Psoriatic Patients, the Interdisciplinary Centre for Clinical Research at the University of Erlangen-Nuremberg, and the Bath Institute for Rheumatic Diseases. Two researchers were received grants from Wyeth-Pharm GmbH (Germany).
Itchy and Pregnant? Consider Range of Skin Conditions
SAN FRANCISCO – When a pregnant woman presents with a complaint of itching, consider a range of causes, not just those triggered by pregnancy, Dr. Bethanee J. Schlosser advised.
Although some dermatoses of pregnancy are common, a pregnant woman’s itching may have nothing to do with her pregnancy and could be the result of contact dermatitis, drug eruption, scabies, folliculitis, or another cause, Dr. Schlosser said at SDEF Women’s & Pediatric Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"Just because they’re pregnant doesn’t mean they only have to fit in the pregnancy dermatoses box," Dr. Schlosser of the department of dermatology, and director of the women’s skin health program, at Northwestern University in Chicago said in an interview.
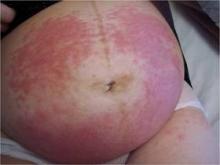
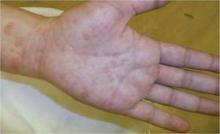
With that said, the two most prominent dermatoses of pregnancy are pruritic urticarial papules and plaques of pregnancy, a condition now known under the umbrella term polymorphic eruption of pregnancy, and pemphigoid gestationis, previously called herpes gestationis.
Polymorphic eruption of pregnancy occurs in about 1 in 300 pregnancies and is generally associated with multiple gestations and increased maternal weight gain. It is also more common in women having their first child. The mean onset is at about 35 weeks, but in about 15% of cases, the onset can be post partum, according to Dr. Schlosser.
Pemphigoid gestationis is a rare acquired autoimmune blistering disease unique to pregnancy. It occurs in 1 in 50,000 pregnancies and is probably the least common dermatosis of pregnancy. The onset is usually in the second or third trimester, but in about 14% of cases, the onset can occur post partum. With pemphigoid gestationis, there is no change in maternal outcome, but there are risks to the fetus including being small for gestational age, preterm delivery, and neonatal pemphigoid disease.
Typically, patients with the polymorphic eruption present with "hivelike" or urticarial papules and plaques, but no blisters, while women with pemphigoid gestationis often have more blistering. However, the clinical presentations and the routine histopathology can be identical, Dr. Schlosser explained.
"I’ve seen patients with both entities, with both kinds of clinical features," she noted. "If it’s in your differential diagnosis and you can’t distinguish 100% clinically, then that’s where the utility of biopsy comes in."
Cutaneous biopsy is a common procedure and is low risk, she reported, even in the context of pregnancy. Routine histopathology and direct immunofluorescence are essential in terms of differentiating between pemphigoid gestationis and polymorphic eruption.
The first-line treatment for both conditions is topical corticosteroids and oral antihistamines when the condition is mild or localized and systemic corticosteroids in severe cases. Although the treatments are generally the same, the difference between the two conditions is not academic, Dr. Schlosser said, because the potential sequelae and considerations for mother and child are different.
Dr. Schlosser also recommended that dermatologists make it a priority to communicate with the referring physician, specifically to review the risks to both the mother and child that may be associated with a particular skin condition or its treatments.
For example, polymorphic eruption of pregnancy is generally nonthreatening to the mother and child. But Dr. Schlosser said she has seen patients with widespread, severe polymorphic eruptions who have needed treatment with systemic corticosteroids. That’s essential information for the ob.gyn.; if the patient has a cesarean delivery, the patient will likely require stress-dose corticosteroids. Similarly, the newborn would need to be monitored for hypoglycemia during the immediate after-birth period.
"That doesn’t mean that dermatologists shouldn’t treat pregnant women aggressively, when appropriate," Dr. Schlosser said. "But the entire multidisciplinary care team needs to be kept informed so that the risks can be managed."
Dr. Schlosser said she had no relevant financial disclosures. SDEF and this news organization are owned by Elsevier.
SAN FRANCISCO – When a pregnant woman presents with a complaint of itching, consider a range of causes, not just those triggered by pregnancy, Dr. Bethanee J. Schlosser advised.
Although some dermatoses of pregnancy are common, a pregnant woman’s itching may have nothing to do with her pregnancy and could be the result of contact dermatitis, drug eruption, scabies, folliculitis, or another cause, Dr. Schlosser said at SDEF Women’s & Pediatric Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"Just because they’re pregnant doesn’t mean they only have to fit in the pregnancy dermatoses box," Dr. Schlosser of the department of dermatology, and director of the women’s skin health program, at Northwestern University in Chicago said in an interview.
With that said, the two most prominent dermatoses of pregnancy are pruritic urticarial papules and plaques of pregnancy, a condition now known under the umbrella term polymorphic eruption of pregnancy, and pemphigoid gestationis, previously called herpes gestationis.
Polymorphic eruption of pregnancy occurs in about 1 in 300 pregnancies and is generally associated with multiple gestations and increased maternal weight gain. It is also more common in women having their first child. The mean onset is at about 35 weeks, but in about 15% of cases, the onset can be post partum, according to Dr. Schlosser.
Pemphigoid gestationis is a rare acquired autoimmune blistering disease unique to pregnancy. It occurs in 1 in 50,000 pregnancies and is probably the least common dermatosis of pregnancy. The onset is usually in the second or third trimester, but in about 14% of cases, the onset can occur post partum. With pemphigoid gestationis, there is no change in maternal outcome, but there are risks to the fetus including being small for gestational age, preterm delivery, and neonatal pemphigoid disease.
Typically, patients with the polymorphic eruption present with "hivelike" or urticarial papules and plaques, but no blisters, while women with pemphigoid gestationis often have more blistering. However, the clinical presentations and the routine histopathology can be identical, Dr. Schlosser explained.
"I’ve seen patients with both entities, with both kinds of clinical features," she noted. "If it’s in your differential diagnosis and you can’t distinguish 100% clinically, then that’s where the utility of biopsy comes in."
Cutaneous biopsy is a common procedure and is low risk, she reported, even in the context of pregnancy. Routine histopathology and direct immunofluorescence are essential in terms of differentiating between pemphigoid gestationis and polymorphic eruption.
The first-line treatment for both conditions is topical corticosteroids and oral antihistamines when the condition is mild or localized and systemic corticosteroids in severe cases. Although the treatments are generally the same, the difference between the two conditions is not academic, Dr. Schlosser said, because the potential sequelae and considerations for mother and child are different.
Dr. Schlosser also recommended that dermatologists make it a priority to communicate with the referring physician, specifically to review the risks to both the mother and child that may be associated with a particular skin condition or its treatments.
For example, polymorphic eruption of pregnancy is generally nonthreatening to the mother and child. But Dr. Schlosser said she has seen patients with widespread, severe polymorphic eruptions who have needed treatment with systemic corticosteroids. That’s essential information for the ob.gyn.; if the patient has a cesarean delivery, the patient will likely require stress-dose corticosteroids. Similarly, the newborn would need to be monitored for hypoglycemia during the immediate after-birth period.
"That doesn’t mean that dermatologists shouldn’t treat pregnant women aggressively, when appropriate," Dr. Schlosser said. "But the entire multidisciplinary care team needs to be kept informed so that the risks can be managed."
Dr. Schlosser said she had no relevant financial disclosures. SDEF and this news organization are owned by Elsevier.
SAN FRANCISCO – When a pregnant woman presents with a complaint of itching, consider a range of causes, not just those triggered by pregnancy, Dr. Bethanee J. Schlosser advised.
Although some dermatoses of pregnancy are common, a pregnant woman’s itching may have nothing to do with her pregnancy and could be the result of contact dermatitis, drug eruption, scabies, folliculitis, or another cause, Dr. Schlosser said at SDEF Women’s & Pediatric Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"Just because they’re pregnant doesn’t mean they only have to fit in the pregnancy dermatoses box," Dr. Schlosser of the department of dermatology, and director of the women’s skin health program, at Northwestern University in Chicago said in an interview.
With that said, the two most prominent dermatoses of pregnancy are pruritic urticarial papules and plaques of pregnancy, a condition now known under the umbrella term polymorphic eruption of pregnancy, and pemphigoid gestationis, previously called herpes gestationis.
Polymorphic eruption of pregnancy occurs in about 1 in 300 pregnancies and is generally associated with multiple gestations and increased maternal weight gain. It is also more common in women having their first child. The mean onset is at about 35 weeks, but in about 15% of cases, the onset can be post partum, according to Dr. Schlosser.
Pemphigoid gestationis is a rare acquired autoimmune blistering disease unique to pregnancy. It occurs in 1 in 50,000 pregnancies and is probably the least common dermatosis of pregnancy. The onset is usually in the second or third trimester, but in about 14% of cases, the onset can occur post partum. With pemphigoid gestationis, there is no change in maternal outcome, but there are risks to the fetus including being small for gestational age, preterm delivery, and neonatal pemphigoid disease.
Typically, patients with the polymorphic eruption present with "hivelike" or urticarial papules and plaques, but no blisters, while women with pemphigoid gestationis often have more blistering. However, the clinical presentations and the routine histopathology can be identical, Dr. Schlosser explained.
"I’ve seen patients with both entities, with both kinds of clinical features," she noted. "If it’s in your differential diagnosis and you can’t distinguish 100% clinically, then that’s where the utility of biopsy comes in."
Cutaneous biopsy is a common procedure and is low risk, she reported, even in the context of pregnancy. Routine histopathology and direct immunofluorescence are essential in terms of differentiating between pemphigoid gestationis and polymorphic eruption.
The first-line treatment for both conditions is topical corticosteroids and oral antihistamines when the condition is mild or localized and systemic corticosteroids in severe cases. Although the treatments are generally the same, the difference between the two conditions is not academic, Dr. Schlosser said, because the potential sequelae and considerations for mother and child are different.
Dr. Schlosser also recommended that dermatologists make it a priority to communicate with the referring physician, specifically to review the risks to both the mother and child that may be associated with a particular skin condition or its treatments.
For example, polymorphic eruption of pregnancy is generally nonthreatening to the mother and child. But Dr. Schlosser said she has seen patients with widespread, severe polymorphic eruptions who have needed treatment with systemic corticosteroids. That’s essential information for the ob.gyn.; if the patient has a cesarean delivery, the patient will likely require stress-dose corticosteroids. Similarly, the newborn would need to be monitored for hypoglycemia during the immediate after-birth period.
"That doesn’t mean that dermatologists shouldn’t treat pregnant women aggressively, when appropriate," Dr. Schlosser said. "But the entire multidisciplinary care team needs to be kept informed so that the risks can be managed."
Dr. Schlosser said she had no relevant financial disclosures. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF WOMEN'S & PEDIATRIC DERMATOLOGY SEMINAR
FDA: TNF Blockers Up Risk of Legionella, Listeria Infection
The Food and Drug Administration has updated the boxed warning label of all tumor necrosis factor–alpha blockers to include information on the risk of infection from Legionella and Listeria.
The warnings and precautions sections of the drug labels also have been revised to include information on the risk for serious infections that could lead to death from multiple disease-causing pathogens.
The TNF blockers that will receive the warnings include Remicade (infliximab), Enbrel (etanercept), Humira (adalimumab), Cimzia (certolizumab pegol), and Simponi (golimumab), according to the FDA announcement.
The FDA advised that risks and benefits should be weighed before initiating TNF blocker therapy in patients with chronic or reoccurring infections, or in patients with conditions that may put them at higher risk for infection.
Reports of serious adverse events associated with these and other drugs should be reported to MedWatch at 800-332-1088.
The Food and Drug Administration has updated the boxed warning label of all tumor necrosis factor–alpha blockers to include information on the risk of infection from Legionella and Listeria.
The warnings and precautions sections of the drug labels also have been revised to include information on the risk for serious infections that could lead to death from multiple disease-causing pathogens.
The TNF blockers that will receive the warnings include Remicade (infliximab), Enbrel (etanercept), Humira (adalimumab), Cimzia (certolizumab pegol), and Simponi (golimumab), according to the FDA announcement.
The FDA advised that risks and benefits should be weighed before initiating TNF blocker therapy in patients with chronic or reoccurring infections, or in patients with conditions that may put them at higher risk for infection.
Reports of serious adverse events associated with these and other drugs should be reported to MedWatch at 800-332-1088.
The Food and Drug Administration has updated the boxed warning label of all tumor necrosis factor–alpha blockers to include information on the risk of infection from Legionella and Listeria.
The warnings and precautions sections of the drug labels also have been revised to include information on the risk for serious infections that could lead to death from multiple disease-causing pathogens.
The TNF blockers that will receive the warnings include Remicade (infliximab), Enbrel (etanercept), Humira (adalimumab), Cimzia (certolizumab pegol), and Simponi (golimumab), according to the FDA announcement.
The FDA advised that risks and benefits should be weighed before initiating TNF blocker therapy in patients with chronic or reoccurring infections, or in patients with conditions that may put them at higher risk for infection.
Reports of serious adverse events associated with these and other drugs should be reported to MedWatch at 800-332-1088.
Rights and Wrongs [editorial]
Evaluating the Efficacy and Safety of Calcipotriene/Betamethasone Ointment Occluded With a Hydrogel Patch: A 6-Week Bilaterally Controlled, Investigator-Blinded Trial
Psoriasis Rupioides: A Rare Variant of a Common Disease
Generalized Cryptococcus albidus in an Immunosuppressed Patient With Palmopustular Psoriasis
Abatacept-Induced Psoriasis [letter]
FDA Guidance on Biosimilars Expected by End of Year
The Food and Drug Administration expects to issue its guidance on biosimilars by the end of 2011, more than a year after legislation designed to make cheaper generic versions of therapeutic biologics available was incorporated into the Patient Protection and Affordable Care Act of 2010.
A year earlier, the Biologics Price Competition and Innovation Act of 2009 (BPCI) established an abbreviated approval pathway for biological products that are shown to be "highly similar" or "biosimilar" to, or "interchangeable" with, an FDA-approved biological product, according to the FDA's summary of the legislation.
The complex issues related to its implementation are still being worked out by a special committee at the agency, which met in November 2010 to discuss the issues and challenges of implementing the BPCI Act. Manufacturers of biologic therapeutics, generic pharmaceutical companies, patient groups, and other interested parties provided their input at that meeting.
An FDA spokesperson said that the agency "continues to carefully review and consider all comments from the November 2010 hearing and from the docket as we move forward in our implementation" of the statute. Biosimilars are also referred to as "follow-on biologics."
Of the major biologics, etanercept (Enbrel) will be the first to lose its patent, in 2012.
Dr. Steven Kozlowski, director of the FDA's Office of Biotechnology Products, and other FDA officials noted that access to expensive biologic therapies "may be limited, not infrequently because of their cost" and emphasized the challenges the agency faced in implementing the act in a "Perspective" article published online on Aug. 4 in the New England Journal of Medicine (2011;365:385-8).
The coauthors of the article, "Developing the Nation's Biosimilar Program," were Dr. Janet Woodcock, director of the FDA's Center for Drug Evaluation and Research; Dr. Karen Midthun, director of the Center for Biologics Evaluation and Research; and Dr. Rachel Behrman Sherman, director of the Office of Medical Policy.
"Reconciling the science of biosimilar development with the new regulatory framework required by the BPCI Act presents the FDA with numerous challenges," primarily, establishing scientific criteria "that address the key question: how similar is similar enough when it comes to the substitution of complex biologic drug products in clinical practice?" They cited immunogenicity as "a critical factor" when evaluating biosimilars, and noted that product-specific safety monitoring should be included in the process.
For now, it remains difficult to predict when these more affordable generic formulations of the expensive biologic treatments for inflammatory diseases will become available.
A spokesperson for the Generic Pharmaceutical Association (GPhA) said that the legislation left a lot to the FDA's discretion. FDA's regulations must not be burdensome and should not create barriers to making these products available, he said. "Ultimately, we want patients to have access to these drugs at affordable prices." A representative of the GPhA made a presentation at the November 2010 meeting and submitted formal comments to the docket in December.
In the dermatology arena, biosimilars would be welcomed primarily because of cost savings for patients and increased access to these effective treatments, said Dr. Mark G. Lebwohl, professor and chairman of the department of dermatology at Mount Sinai School of Medicine, N.Y.
Biosimilars will not be identical to the drugs they replace, "and when tested, they will have to come into a certain narrow window of similarity in terms of both safety and side effects," he said in an interview. The dilemma with the side effect profile is that it may not be fully characterized for years and, in terms of effectiveness, "the dilemma is that they have to be approximately equal to the drug that it is replacing."
For example, a biosimilar for etanercept that is 10% less effective than the original product could make a difference clinically. A biosimilar could conceivably work better than the biologic drug it is replacing, but "if it is too much more effective, it’s not a biosimilar and will have to through a new drug application." Moreover, if it is more effective, it might be more immunosuppressive, raising concerns about more side effects, Dr. Lebwohl pointed out.
Dr. Lebwohl disclosed that he has been an investigator for and the department of dermatology at Mount Sinai has received funds from most of the manufacturers of biologics for psoriasis.
More on the BPCI Act is available on the FDA website.
The Food and Drug Administration expects to issue its guidance on biosimilars by the end of 2011, more than a year after legislation designed to make cheaper generic versions of therapeutic biologics available was incorporated into the Patient Protection and Affordable Care Act of 2010.
A year earlier, the Biologics Price Competition and Innovation Act of 2009 (BPCI) established an abbreviated approval pathway for biological products that are shown to be "highly similar" or "biosimilar" to, or "interchangeable" with, an FDA-approved biological product, according to the FDA's summary of the legislation.
The complex issues related to its implementation are still being worked out by a special committee at the agency, which met in November 2010 to discuss the issues and challenges of implementing the BPCI Act. Manufacturers of biologic therapeutics, generic pharmaceutical companies, patient groups, and other interested parties provided their input at that meeting.
An FDA spokesperson said that the agency "continues to carefully review and consider all comments from the November 2010 hearing and from the docket as we move forward in our implementation" of the statute. Biosimilars are also referred to as "follow-on biologics."
Of the major biologics, etanercept (Enbrel) will be the first to lose its patent, in 2012.
Dr. Steven Kozlowski, director of the FDA's Office of Biotechnology Products, and other FDA officials noted that access to expensive biologic therapies "may be limited, not infrequently because of their cost" and emphasized the challenges the agency faced in implementing the act in a "Perspective" article published online on Aug. 4 in the New England Journal of Medicine (2011;365:385-8).
The coauthors of the article, "Developing the Nation's Biosimilar Program," were Dr. Janet Woodcock, director of the FDA's Center for Drug Evaluation and Research; Dr. Karen Midthun, director of the Center for Biologics Evaluation and Research; and Dr. Rachel Behrman Sherman, director of the Office of Medical Policy.
"Reconciling the science of biosimilar development with the new regulatory framework required by the BPCI Act presents the FDA with numerous challenges," primarily, establishing scientific criteria "that address the key question: how similar is similar enough when it comes to the substitution of complex biologic drug products in clinical practice?" They cited immunogenicity as "a critical factor" when evaluating biosimilars, and noted that product-specific safety monitoring should be included in the process.
For now, it remains difficult to predict when these more affordable generic formulations of the expensive biologic treatments for inflammatory diseases will become available.
A spokesperson for the Generic Pharmaceutical Association (GPhA) said that the legislation left a lot to the FDA's discretion. FDA's regulations must not be burdensome and should not create barriers to making these products available, he said. "Ultimately, we want patients to have access to these drugs at affordable prices." A representative of the GPhA made a presentation at the November 2010 meeting and submitted formal comments to the docket in December.
In the dermatology arena, biosimilars would be welcomed primarily because of cost savings for patients and increased access to these effective treatments, said Dr. Mark G. Lebwohl, professor and chairman of the department of dermatology at Mount Sinai School of Medicine, N.Y.
Biosimilars will not be identical to the drugs they replace, "and when tested, they will have to come into a certain narrow window of similarity in terms of both safety and side effects," he said in an interview. The dilemma with the side effect profile is that it may not be fully characterized for years and, in terms of effectiveness, "the dilemma is that they have to be approximately equal to the drug that it is replacing."
For example, a biosimilar for etanercept that is 10% less effective than the original product could make a difference clinically. A biosimilar could conceivably work better than the biologic drug it is replacing, but "if it is too much more effective, it’s not a biosimilar and will have to through a new drug application." Moreover, if it is more effective, it might be more immunosuppressive, raising concerns about more side effects, Dr. Lebwohl pointed out.
Dr. Lebwohl disclosed that he has been an investigator for and the department of dermatology at Mount Sinai has received funds from most of the manufacturers of biologics for psoriasis.
More on the BPCI Act is available on the FDA website.
The Food and Drug Administration expects to issue its guidance on biosimilars by the end of 2011, more than a year after legislation designed to make cheaper generic versions of therapeutic biologics available was incorporated into the Patient Protection and Affordable Care Act of 2010.
A year earlier, the Biologics Price Competition and Innovation Act of 2009 (BPCI) established an abbreviated approval pathway for biological products that are shown to be "highly similar" or "biosimilar" to, or "interchangeable" with, an FDA-approved biological product, according to the FDA's summary of the legislation.
The complex issues related to its implementation are still being worked out by a special committee at the agency, which met in November 2010 to discuss the issues and challenges of implementing the BPCI Act. Manufacturers of biologic therapeutics, generic pharmaceutical companies, patient groups, and other interested parties provided their input at that meeting.
An FDA spokesperson said that the agency "continues to carefully review and consider all comments from the November 2010 hearing and from the docket as we move forward in our implementation" of the statute. Biosimilars are also referred to as "follow-on biologics."
Of the major biologics, etanercept (Enbrel) will be the first to lose its patent, in 2012.
Dr. Steven Kozlowski, director of the FDA's Office of Biotechnology Products, and other FDA officials noted that access to expensive biologic therapies "may be limited, not infrequently because of their cost" and emphasized the challenges the agency faced in implementing the act in a "Perspective" article published online on Aug. 4 in the New England Journal of Medicine (2011;365:385-8).
The coauthors of the article, "Developing the Nation's Biosimilar Program," were Dr. Janet Woodcock, director of the FDA's Center for Drug Evaluation and Research; Dr. Karen Midthun, director of the Center for Biologics Evaluation and Research; and Dr. Rachel Behrman Sherman, director of the Office of Medical Policy.
"Reconciling the science of biosimilar development with the new regulatory framework required by the BPCI Act presents the FDA with numerous challenges," primarily, establishing scientific criteria "that address the key question: how similar is similar enough when it comes to the substitution of complex biologic drug products in clinical practice?" They cited immunogenicity as "a critical factor" when evaluating biosimilars, and noted that product-specific safety monitoring should be included in the process.
For now, it remains difficult to predict when these more affordable generic formulations of the expensive biologic treatments for inflammatory diseases will become available.
A spokesperson for the Generic Pharmaceutical Association (GPhA) said that the legislation left a lot to the FDA's discretion. FDA's regulations must not be burdensome and should not create barriers to making these products available, he said. "Ultimately, we want patients to have access to these drugs at affordable prices." A representative of the GPhA made a presentation at the November 2010 meeting and submitted formal comments to the docket in December.
In the dermatology arena, biosimilars would be welcomed primarily because of cost savings for patients and increased access to these effective treatments, said Dr. Mark G. Lebwohl, professor and chairman of the department of dermatology at Mount Sinai School of Medicine, N.Y.
Biosimilars will not be identical to the drugs they replace, "and when tested, they will have to come into a certain narrow window of similarity in terms of both safety and side effects," he said in an interview. The dilemma with the side effect profile is that it may not be fully characterized for years and, in terms of effectiveness, "the dilemma is that they have to be approximately equal to the drug that it is replacing."
For example, a biosimilar for etanercept that is 10% less effective than the original product could make a difference clinically. A biosimilar could conceivably work better than the biologic drug it is replacing, but "if it is too much more effective, it’s not a biosimilar and will have to through a new drug application." Moreover, if it is more effective, it might be more immunosuppressive, raising concerns about more side effects, Dr. Lebwohl pointed out.
Dr. Lebwohl disclosed that he has been an investigator for and the department of dermatology at Mount Sinai has received funds from most of the manufacturers of biologics for psoriasis.
More on the BPCI Act is available on the FDA website.
Psoriasis, Biologics: Concern Remains About CV Risks
The use of biologic agents for chronic plaque psoriasis was not associated with a significant increase in the risk of major adverse cardiovascular events in a meta-analysis of 22 randomized clinical trials reported in the Aug. 24/31 issue of JAMA.
However, the study had several limitations that prevented the investigators from definitively establishing whether anti-interleukin-12 and anti-interleukin 23 (anti-IL12/23) agents such as usetekinumab and briakinumab or anti-TNFa agents such as adalimumab, etanercept, and infliximab expose psoriasis patients to excess cardiovascular risk.
"Access to patient-level data for these studies was not granted by any of the study sponsors, which precluded the use of a more statistically robust time-to-event analysis. [In addition,] the small number of major adverse CV events in placebo-controlled phases of these studies and the limited duration of the placebo-controlled phases reduce the power of this meta-analysis to detect a change in risk," said Caitriona Ryan, MB, BAO, BCh, of the department of dermatology, Baylor Research Institute, Dallas, and her associates.
"Until more definitive data become available, we believe that dermatologists should exercise heightened vigilance for CV risk factors when initiating anti-Il12/23 agents in psoriasis patients," they noted.
Initially, it was thought that these biologic agents, which help control inflammation in RA and psoriasis patients, might also exert a cardioprotective effect. So there was surprise and concern when preliminary reports showed a numerical excess of major adverse CV events (MACE) in industry-sponsored trials of ustekinumab (Centocor Ortho) and briakinumab (Abbott). "A total of 53 MACEs have occurred to date across all phases of these studies; 26 MACES, including 1 CV death, in studies of ustekinumab and 27 MACEs, including 4 CV deaths, in studies of briakinumab," the investigators said.
To clarify a possible link, they performed a meta-analysis of all randomized clinical trials (RCTs) in which these two agents as well as anti-TNFa agents were compared with placebo in subjects who had chronic plaque psoriasis but no psoriatic arthritis. A total of 10,183 patients comprised the study population. "The primary outcome measure was the number of MACEs during the placebo-controlled phase of treatment," the researchers said.
Although they found no significant rise in risk of MACEs, the investigators said they were limited in their ability to do so by small numbers of subjects, small numbers of MACEs, short duration of drug exposure, and flaws in the RCTs. For example, two myocardial infarctions were not reported in the "adverse event" sections of one prominent industry-sponsored study.
Even though meta-analysis is intended to increase the power to detect rare events by pooling data from several studies, it "cannot correct for limitations in quality of the original clinical trials, most notably the absence of a systematic strategy to screen for, capture, and adjudicate CV events," they noted (JAMA 2011;306:864-71).
"We remain concerned about the MACE rate of 1.33 per 100 patient-years in the placebo-controlled phase of the phase III briakinumab study, with an overall rate of 0.60 events per 100 patient-years across all treatment periods. Indeed, after identification of these cases," patients with two or more CV risk factors were withdrawn from the study. "Subsequently, in July 2011, all clinical trials of briakinumab were discontinued by Abbott, pending further investigations particularly relating to possible mechanistic links to MACEs," the investigators said.
"With numerous therapeutics agents inhibiting IL-17 and IL-23 currently in development, it is essential that the effect of these cytokines on vascular inflammation be fully explored," they stressed.
Their results highlight "the inherent limitations of placebo-controlled clinical trials to reliably interpret the significance of rare events given their current design." RCTs often are underpowered and too brief to detect rare or long-term adverse events, the researchers added.
The investigators reported receiving no external funding for this study. Dr. Ryan reported ties to Janssen-Cilag, Pfizer (a maker of etanercept), Galderma, and Abbott (maker of briakinumab and adalimumab), and his associates reported ties to numerous pharmaceutical companies including the above and Centocor (maker of ustekinumab and infliximab), Amgen (comaker of etanercept), and Schering-Plough (a maker of infliximab).
The use of biologic agents for chronic plaque psoriasis was not associated with a significant increase in the risk of major adverse cardiovascular events in a meta-analysis of 22 randomized clinical trials reported in the Aug. 24/31 issue of JAMA.
However, the study had several limitations that prevented the investigators from definitively establishing whether anti-interleukin-12 and anti-interleukin 23 (anti-IL12/23) agents such as usetekinumab and briakinumab or anti-TNFa agents such as adalimumab, etanercept, and infliximab expose psoriasis patients to excess cardiovascular risk.
"Access to patient-level data for these studies was not granted by any of the study sponsors, which precluded the use of a more statistically robust time-to-event analysis. [In addition,] the small number of major adverse CV events in placebo-controlled phases of these studies and the limited duration of the placebo-controlled phases reduce the power of this meta-analysis to detect a change in risk," said Caitriona Ryan, MB, BAO, BCh, of the department of dermatology, Baylor Research Institute, Dallas, and her associates.
"Until more definitive data become available, we believe that dermatologists should exercise heightened vigilance for CV risk factors when initiating anti-Il12/23 agents in psoriasis patients," they noted.
Initially, it was thought that these biologic agents, which help control inflammation in RA and psoriasis patients, might also exert a cardioprotective effect. So there was surprise and concern when preliminary reports showed a numerical excess of major adverse CV events (MACE) in industry-sponsored trials of ustekinumab (Centocor Ortho) and briakinumab (Abbott). "A total of 53 MACEs have occurred to date across all phases of these studies; 26 MACES, including 1 CV death, in studies of ustekinumab and 27 MACEs, including 4 CV deaths, in studies of briakinumab," the investigators said.
To clarify a possible link, they performed a meta-analysis of all randomized clinical trials (RCTs) in which these two agents as well as anti-TNFa agents were compared with placebo in subjects who had chronic plaque psoriasis but no psoriatic arthritis. A total of 10,183 patients comprised the study population. "The primary outcome measure was the number of MACEs during the placebo-controlled phase of treatment," the researchers said.
Although they found no significant rise in risk of MACEs, the investigators said they were limited in their ability to do so by small numbers of subjects, small numbers of MACEs, short duration of drug exposure, and flaws in the RCTs. For example, two myocardial infarctions were not reported in the "adverse event" sections of one prominent industry-sponsored study.
Even though meta-analysis is intended to increase the power to detect rare events by pooling data from several studies, it "cannot correct for limitations in quality of the original clinical trials, most notably the absence of a systematic strategy to screen for, capture, and adjudicate CV events," they noted (JAMA 2011;306:864-71).
"We remain concerned about the MACE rate of 1.33 per 100 patient-years in the placebo-controlled phase of the phase III briakinumab study, with an overall rate of 0.60 events per 100 patient-years across all treatment periods. Indeed, after identification of these cases," patients with two or more CV risk factors were withdrawn from the study. "Subsequently, in July 2011, all clinical trials of briakinumab were discontinued by Abbott, pending further investigations particularly relating to possible mechanistic links to MACEs," the investigators said.
"With numerous therapeutics agents inhibiting IL-17 and IL-23 currently in development, it is essential that the effect of these cytokines on vascular inflammation be fully explored," they stressed.
Their results highlight "the inherent limitations of placebo-controlled clinical trials to reliably interpret the significance of rare events given their current design." RCTs often are underpowered and too brief to detect rare or long-term adverse events, the researchers added.
The investigators reported receiving no external funding for this study. Dr. Ryan reported ties to Janssen-Cilag, Pfizer (a maker of etanercept), Galderma, and Abbott (maker of briakinumab and adalimumab), and his associates reported ties to numerous pharmaceutical companies including the above and Centocor (maker of ustekinumab and infliximab), Amgen (comaker of etanercept), and Schering-Plough (a maker of infliximab).
The use of biologic agents for chronic plaque psoriasis was not associated with a significant increase in the risk of major adverse cardiovascular events in a meta-analysis of 22 randomized clinical trials reported in the Aug. 24/31 issue of JAMA.
However, the study had several limitations that prevented the investigators from definitively establishing whether anti-interleukin-12 and anti-interleukin 23 (anti-IL12/23) agents such as usetekinumab and briakinumab or anti-TNFa agents such as adalimumab, etanercept, and infliximab expose psoriasis patients to excess cardiovascular risk.
"Access to patient-level data for these studies was not granted by any of the study sponsors, which precluded the use of a more statistically robust time-to-event analysis. [In addition,] the small number of major adverse CV events in placebo-controlled phases of these studies and the limited duration of the placebo-controlled phases reduce the power of this meta-analysis to detect a change in risk," said Caitriona Ryan, MB, BAO, BCh, of the department of dermatology, Baylor Research Institute, Dallas, and her associates.
"Until more definitive data become available, we believe that dermatologists should exercise heightened vigilance for CV risk factors when initiating anti-Il12/23 agents in psoriasis patients," they noted.
Initially, it was thought that these biologic agents, which help control inflammation in RA and psoriasis patients, might also exert a cardioprotective effect. So there was surprise and concern when preliminary reports showed a numerical excess of major adverse CV events (MACE) in industry-sponsored trials of ustekinumab (Centocor Ortho) and briakinumab (Abbott). "A total of 53 MACEs have occurred to date across all phases of these studies; 26 MACES, including 1 CV death, in studies of ustekinumab and 27 MACEs, including 4 CV deaths, in studies of briakinumab," the investigators said.
To clarify a possible link, they performed a meta-analysis of all randomized clinical trials (RCTs) in which these two agents as well as anti-TNFa agents were compared with placebo in subjects who had chronic plaque psoriasis but no psoriatic arthritis. A total of 10,183 patients comprised the study population. "The primary outcome measure was the number of MACEs during the placebo-controlled phase of treatment," the researchers said.
Although they found no significant rise in risk of MACEs, the investigators said they were limited in their ability to do so by small numbers of subjects, small numbers of MACEs, short duration of drug exposure, and flaws in the RCTs. For example, two myocardial infarctions were not reported in the "adverse event" sections of one prominent industry-sponsored study.
Even though meta-analysis is intended to increase the power to detect rare events by pooling data from several studies, it "cannot correct for limitations in quality of the original clinical trials, most notably the absence of a systematic strategy to screen for, capture, and adjudicate CV events," they noted (JAMA 2011;306:864-71).
"We remain concerned about the MACE rate of 1.33 per 100 patient-years in the placebo-controlled phase of the phase III briakinumab study, with an overall rate of 0.60 events per 100 patient-years across all treatment periods. Indeed, after identification of these cases," patients with two or more CV risk factors were withdrawn from the study. "Subsequently, in July 2011, all clinical trials of briakinumab were discontinued by Abbott, pending further investigations particularly relating to possible mechanistic links to MACEs," the investigators said.
"With numerous therapeutics agents inhibiting IL-17 and IL-23 currently in development, it is essential that the effect of these cytokines on vascular inflammation be fully explored," they stressed.
Their results highlight "the inherent limitations of placebo-controlled clinical trials to reliably interpret the significance of rare events given their current design." RCTs often are underpowered and too brief to detect rare or long-term adverse events, the researchers added.
The investigators reported receiving no external funding for this study. Dr. Ryan reported ties to Janssen-Cilag, Pfizer (a maker of etanercept), Galderma, and Abbott (maker of briakinumab and adalimumab), and his associates reported ties to numerous pharmaceutical companies including the above and Centocor (maker of ustekinumab and infliximab), Amgen (comaker of etanercept), and Schering-Plough (a maker of infliximab).
FROM JAMA
Major Finding: Treatment of plaque psoriasis with biologic agents did not appear to raise the risk of major adverse cardiovascular events in a meta-analysis, but low numbers and flaws in the studies’ methodologies don't allow definitive conclusions to be drawn.
Data Source: A meta-analysis of CV outcomes in 22 randomized clinical trials of anti-IL 12/23 agents and anti-TNFa agents used to treat psoriasis.
Disclosures: This study received no external funding. Dr. Ryan reported ties to Janssen-Cilag, Pfizer (a maker of etanercept), Galderma, and Abbott (maker of briakinumab and adalimumab), and his associates reported ties to numerous pharmaceutical companies including the above and Centocor (maker of ustekinumab and infliximab), Amgen (comaker of etanercept), and Schering-Plough (a maker of infliximab).