User login
CAR T-cell therapy seems feasible for NHL, MM

©ASCO/Rodney White
CHICAGO—The CD19-directed chimeric antigen receptor (CAR) T-cell therapy CTL019 has shown promise for treating non-Hodgkin lymphoma (NHL) and may be a feasible treatment option for multiple myeloma (MM) as well, according to researchers.
In an ongoing phase 2 trial, CTL019 has produced durable responses in patients with relapsed or refractory NHL.
And early results of a phase 1 trial suggest CTL019 can provide clinical benefit in heavily pretreated patients with MM.
Both studies were presented at the 2015 ASCO Annual Meeting. The University of Pennsylvania and Novartis have an exclusive global collaboration to research, develop, and commercialize CTL019.
CTL019 in NHL
Stephen Schuster, MD, of the Abramson Cancer Center of the University of Pennsylvania in Philadelphia, presented results of the phase 2 NHL trial (abstract 8516*).
The trial included 20 evaluable patients, 13 with diffuse large B-cell lymphoma (DLBCL) and 7 with follicular lymphoma (FL). At the time of presentation, the median follow-up was 274 days for the patients with DLBCL and 290 days for those with FL.
The overall response rate was 100% in patients with FL and 50% in those with DLBCL. Thirteen patients responded to the therapy, including 11 who achieved a complete response and 2 who experienced a partial response.
Six patients with a partial response to treatment at 3 months achieved a complete response by 6 months. Two patients with a partial response experienced disease progression at 6 and 12 months after treatment.
The researchers said toxicity appeared to be acceptable, with primarily grade 2 cytokine release syndrome (CRS). Two patients developed CRS of grade 3 or higher at peak T-cell expansion. There were no deaths from CRS.
“The results from this ongoing study of CTL019 are encouraging, as we now have data through 6 months showing that patients may have achieved durable overall response rates,” Dr Schuster said. “These data support our ongoing efforts to determine the potential role of CTL019 in improving outcomes for patients with certain types of B-cell lymphomas.”
CTL019 in MM
Alfred Garfall, MD, of the Abramson Cancer Center, presented preliminary results of an ongoing phase 1 study investigating CTL019 in patients with MM (abstract 8517*).
Dr Garfall and his colleagues hypothesized that CTL019 would exhibit efficacy in MM due to low-level CD19 expression on MM plasma cells or CD19 expression in drug-resistant, disease-propagating subsets of the MM clone.
The study included 5 patients who experienced disease progression within a year of a prior autologous stem cell transplant and were medically fit to undergo a second autologous transplant. The patients had received a median of 7.5 prior lines of therapy.
“We found potential evidence of clinical benefit in 3 of 4 patients with more than 100 days of follow-up,” Dr Garfall said.
Two patients experienced longer, deeper responses, and 1 patient experienced CRS.
The data suggest “it is safe and feasible to manufacture and administered CTL019 to refractory multiple myeloma patients,” Dr Garfall said.
*Information in the abstract differs from that presented at the meeting.

©ASCO/Rodney White
CHICAGO—The CD19-directed chimeric antigen receptor (CAR) T-cell therapy CTL019 has shown promise for treating non-Hodgkin lymphoma (NHL) and may be a feasible treatment option for multiple myeloma (MM) as well, according to researchers.
In an ongoing phase 2 trial, CTL019 has produced durable responses in patients with relapsed or refractory NHL.
And early results of a phase 1 trial suggest CTL019 can provide clinical benefit in heavily pretreated patients with MM.
Both studies were presented at the 2015 ASCO Annual Meeting. The University of Pennsylvania and Novartis have an exclusive global collaboration to research, develop, and commercialize CTL019.
CTL019 in NHL
Stephen Schuster, MD, of the Abramson Cancer Center of the University of Pennsylvania in Philadelphia, presented results of the phase 2 NHL trial (abstract 8516*).
The trial included 20 evaluable patients, 13 with diffuse large B-cell lymphoma (DLBCL) and 7 with follicular lymphoma (FL). At the time of presentation, the median follow-up was 274 days for the patients with DLBCL and 290 days for those with FL.
The overall response rate was 100% in patients with FL and 50% in those with DLBCL. Thirteen patients responded to the therapy, including 11 who achieved a complete response and 2 who experienced a partial response.
Six patients with a partial response to treatment at 3 months achieved a complete response by 6 months. Two patients with a partial response experienced disease progression at 6 and 12 months after treatment.
The researchers said toxicity appeared to be acceptable, with primarily grade 2 cytokine release syndrome (CRS). Two patients developed CRS of grade 3 or higher at peak T-cell expansion. There were no deaths from CRS.
“The results from this ongoing study of CTL019 are encouraging, as we now have data through 6 months showing that patients may have achieved durable overall response rates,” Dr Schuster said. “These data support our ongoing efforts to determine the potential role of CTL019 in improving outcomes for patients with certain types of B-cell lymphomas.”
CTL019 in MM
Alfred Garfall, MD, of the Abramson Cancer Center, presented preliminary results of an ongoing phase 1 study investigating CTL019 in patients with MM (abstract 8517*).
Dr Garfall and his colleagues hypothesized that CTL019 would exhibit efficacy in MM due to low-level CD19 expression on MM plasma cells or CD19 expression in drug-resistant, disease-propagating subsets of the MM clone.
The study included 5 patients who experienced disease progression within a year of a prior autologous stem cell transplant and were medically fit to undergo a second autologous transplant. The patients had received a median of 7.5 prior lines of therapy.
“We found potential evidence of clinical benefit in 3 of 4 patients with more than 100 days of follow-up,” Dr Garfall said.
Two patients experienced longer, deeper responses, and 1 patient experienced CRS.
The data suggest “it is safe and feasible to manufacture and administered CTL019 to refractory multiple myeloma patients,” Dr Garfall said.
*Information in the abstract differs from that presented at the meeting.

©ASCO/Rodney White
CHICAGO—The CD19-directed chimeric antigen receptor (CAR) T-cell therapy CTL019 has shown promise for treating non-Hodgkin lymphoma (NHL) and may be a feasible treatment option for multiple myeloma (MM) as well, according to researchers.
In an ongoing phase 2 trial, CTL019 has produced durable responses in patients with relapsed or refractory NHL.
And early results of a phase 1 trial suggest CTL019 can provide clinical benefit in heavily pretreated patients with MM.
Both studies were presented at the 2015 ASCO Annual Meeting. The University of Pennsylvania and Novartis have an exclusive global collaboration to research, develop, and commercialize CTL019.
CTL019 in NHL
Stephen Schuster, MD, of the Abramson Cancer Center of the University of Pennsylvania in Philadelphia, presented results of the phase 2 NHL trial (abstract 8516*).
The trial included 20 evaluable patients, 13 with diffuse large B-cell lymphoma (DLBCL) and 7 with follicular lymphoma (FL). At the time of presentation, the median follow-up was 274 days for the patients with DLBCL and 290 days for those with FL.
The overall response rate was 100% in patients with FL and 50% in those with DLBCL. Thirteen patients responded to the therapy, including 11 who achieved a complete response and 2 who experienced a partial response.
Six patients with a partial response to treatment at 3 months achieved a complete response by 6 months. Two patients with a partial response experienced disease progression at 6 and 12 months after treatment.
The researchers said toxicity appeared to be acceptable, with primarily grade 2 cytokine release syndrome (CRS). Two patients developed CRS of grade 3 or higher at peak T-cell expansion. There were no deaths from CRS.
“The results from this ongoing study of CTL019 are encouraging, as we now have data through 6 months showing that patients may have achieved durable overall response rates,” Dr Schuster said. “These data support our ongoing efforts to determine the potential role of CTL019 in improving outcomes for patients with certain types of B-cell lymphomas.”
CTL019 in MM
Alfred Garfall, MD, of the Abramson Cancer Center, presented preliminary results of an ongoing phase 1 study investigating CTL019 in patients with MM (abstract 8517*).
Dr Garfall and his colleagues hypothesized that CTL019 would exhibit efficacy in MM due to low-level CD19 expression on MM plasma cells or CD19 expression in drug-resistant, disease-propagating subsets of the MM clone.
The study included 5 patients who experienced disease progression within a year of a prior autologous stem cell transplant and were medically fit to undergo a second autologous transplant. The patients had received a median of 7.5 prior lines of therapy.
“We found potential evidence of clinical benefit in 3 of 4 patients with more than 100 days of follow-up,” Dr Garfall said.
Two patients experienced longer, deeper responses, and 1 patient experienced CRS.
The data suggest “it is safe and feasible to manufacture and administered CTL019 to refractory multiple myeloma patients,” Dr Garfall said.
*Information in the abstract differs from that presented at the meeting.
Follow-up PET/CT has ‘clinical value’ in NHL
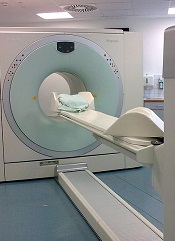
BALTIMORE—Post-treatment PET/CT scans may be necessary for some patients with non-Hodgkin lymphoma (NHL), according to a presentation at the 2015 SNMMI Annual Meeting.
“[T]he role of post-treatment PET/CT has been controversial,” said Mehdi Taghipour, MD, of Johns Hopkins University in Baltimore, Maryland.
“Our study proves that 39% of follow-up PET/CT scans added clinical value, which represents a significant improvement in NHL patient care.”
Dr Taghipour presented the details of this study at the meeting as abstract 599.
He and his colleagues had examined 560 PET/CT scans from 204 patients. Imaging was performed 6 months or more after the patient completed primary therapy.
The researchers assessed the value of follow-up PET/CT by conducting statistical analyses to determine changes in patient management and evaluated the accuracy of these scans compared to either histopathology or an additional 6-month follow-up.
Results showed that the sensitivity of PET/CT for detecting relapsed NHL was 95.1%, and the specificity was 90.5%. Positive and negative predictive values were 84.5% and 97.1%, respectively.
The overall accuracy of follow-up PET/CT with the common imaging agent fluorodeoxyglucose (FDG) was 92.1%.
Follow-up PET/CT led to changes in patient management in 17% of cases, and new treatments were initiated after 15.7% of scans. More than 69% of scans were performed without prior clinical suspicion of recurrence, and 30.7% of scans were ordered because of suspected disease.
More than 22% of follow-up scans showed suspected disease when there was no clinical suspicion for disease recurrence, and the presence of disease was ruled out in 17.4% of scans where the treating physician had suspected recurrence prior to the scan. ![]()

BALTIMORE—Post-treatment PET/CT scans may be necessary for some patients with non-Hodgkin lymphoma (NHL), according to a presentation at the 2015 SNMMI Annual Meeting.
“[T]he role of post-treatment PET/CT has been controversial,” said Mehdi Taghipour, MD, of Johns Hopkins University in Baltimore, Maryland.
“Our study proves that 39% of follow-up PET/CT scans added clinical value, which represents a significant improvement in NHL patient care.”
Dr Taghipour presented the details of this study at the meeting as abstract 599.
He and his colleagues had examined 560 PET/CT scans from 204 patients. Imaging was performed 6 months or more after the patient completed primary therapy.
The researchers assessed the value of follow-up PET/CT by conducting statistical analyses to determine changes in patient management and evaluated the accuracy of these scans compared to either histopathology or an additional 6-month follow-up.
Results showed that the sensitivity of PET/CT for detecting relapsed NHL was 95.1%, and the specificity was 90.5%. Positive and negative predictive values were 84.5% and 97.1%, respectively.
The overall accuracy of follow-up PET/CT with the common imaging agent fluorodeoxyglucose (FDG) was 92.1%.
Follow-up PET/CT led to changes in patient management in 17% of cases, and new treatments were initiated after 15.7% of scans. More than 69% of scans were performed without prior clinical suspicion of recurrence, and 30.7% of scans were ordered because of suspected disease.
More than 22% of follow-up scans showed suspected disease when there was no clinical suspicion for disease recurrence, and the presence of disease was ruled out in 17.4% of scans where the treating physician had suspected recurrence prior to the scan. ![]()

BALTIMORE—Post-treatment PET/CT scans may be necessary for some patients with non-Hodgkin lymphoma (NHL), according to a presentation at the 2015 SNMMI Annual Meeting.
“[T]he role of post-treatment PET/CT has been controversial,” said Mehdi Taghipour, MD, of Johns Hopkins University in Baltimore, Maryland.
“Our study proves that 39% of follow-up PET/CT scans added clinical value, which represents a significant improvement in NHL patient care.”
Dr Taghipour presented the details of this study at the meeting as abstract 599.
He and his colleagues had examined 560 PET/CT scans from 204 patients. Imaging was performed 6 months or more after the patient completed primary therapy.
The researchers assessed the value of follow-up PET/CT by conducting statistical analyses to determine changes in patient management and evaluated the accuracy of these scans compared to either histopathology or an additional 6-month follow-up.
Results showed that the sensitivity of PET/CT for detecting relapsed NHL was 95.1%, and the specificity was 90.5%. Positive and negative predictive values were 84.5% and 97.1%, respectively.
The overall accuracy of follow-up PET/CT with the common imaging agent fluorodeoxyglucose (FDG) was 92.1%.
Follow-up PET/CT led to changes in patient management in 17% of cases, and new treatments were initiated after 15.7% of scans. More than 69% of scans were performed without prior clinical suspicion of recurrence, and 30.7% of scans were ordered because of suspected disease.
More than 22% of follow-up scans showed suspected disease when there was no clinical suspicion for disease recurrence, and the presence of disease was ruled out in 17.4% of scans where the treating physician had suspected recurrence prior to the scan. ![]()
No survival difference with allo- or auto-SCT in PTCL

© ASCO/Max Gersh
CHICAGO—Allogeneic and autologous transplants produce similar survival rates when used as first-line therapy in younger patients with peripheral
T-cell lymphoma (PTCL), according to interim results of the AATT trial.
The study also showed that deaths among patients who received autologous stem cell transplants (auto-SCTs) were a result of relapse and salvage treatment, while deaths among allogeneic SCT (allo-SCT) recipients were transplant-related.
Norbert Schmitz, MD, PhD, of Asklepios Hospital St. Georg in Hamburg, Germany, presented these findings at the 2015 ASCO Annual Meeting (abstract 8507*).
Dr Schmitz noted that only previous study comparing auto-SCT with allo-SCT as first-line therapy in PTCL was not designed or powered to evaluate the differences between the transplant types.
So he and his colleagues conducted the AATT trial to determine the differences. The team hypothesized that allo-SCT would improve 3-year event-free survival from 35% to 60%, given an α of 5% and a power of 80%. They needed 140 patients to prove or disprove this theory.
Ultimately, the investigators enrolled 104 patients and performed an interim analysis when 58 patients were evaluable for response.
Of the 58 patients, 30 were randomized to the auto-SCT arm and 28 to the allo-SCT arm. Baseline characteristics were similar between the arms, including patients’ median ages (49 and 50, respectively), the proportion of patients with stage III/IV disease (87% and 93%), and the proportion with ECOG status greater than 1 (23% and 18%).
Most patients in both arms had PTCL not otherwise specified (36% in the auto-SCT arm and 50% in the allo-SCT arm). Other subtypes included angioimmunoblastic T-cell lymphoma (23% and 32%, respectively), ALK-negative anaplastic large-cell lymphoma (20% and 4%), and “other” PTCLs (20% and 8%). The other PTCLs were NK/T-cell lymphoma, intestinal T/NK-cell lymphoma, hepatosplenic γδ lymphoma, and subcutaneous panniculitis-like PTCL.
Treatment characteristics
Before undergoing transplant, patients in both arms received treatment with CHOEP (cyclophosphamide, doxorubicin, etoposide, vincristine, and prednisone) on days 1, 15, 29, and 43. If they experienced a complete response (CR), partial response, or no change, patients received DHAP (dexamethasone, cytarabine, and cisplatin) on day 64.
Patients in the auto-SCT arm received BEAM (carmustine, etoposide, cytarabine, and melphalan) prior to transplant. And patients in the allo-SCT arm received FBC (fludarabine, busulfan, and cyclophosphamide).
Overall, 36 patients (62%) completed treatment per protocol, 19 in the auto-SCT arm and 17 in the allo-SCT arm. Thirty-eight percent of all patients could not proceed to transplant per protocol, mostly because of early lymphoma progression.
Response and survival
The researchers observed CRs/unconfirmed CRs (CRus) in 33% (n=10) of patients in the auto-SCT arm and 39% (n=11) in the allo-SCT arm. CR/CRus and progressive disease within 2 months occurred in 3% (n=1) and 4% (n=1) of patients, respectively.
Partial responses were seen in 17% (n=5) of patients in the auto-SCT arm and 7% (n=2) in the allo-SCT arm. There was no change in 7% (n=2) and 0% of patients, respectively. And responses were unknown in 7% (n=2) of patients in the auto-SCT arm.
Progressive disease occurred in 33% (n=10) of patients in the auto-SCT arm and 36% (n=10) in the allo-SCT arm. And treatment-related death occurred in 0% (n=0) and 14% (n=4), respectively.
At the interim analysis, there was no significant difference between the treatment arms with regard to event-free survival (P=0.963) or overall survival (P=0.174).
“At that time, the decision was made to stop the study,” Dr Schmitz said.
He explained that a conditional power analysis showed a low probability that the primary endpoint—a 25% improvement in event-free survival with allo-SCT—could still be met. So the data safety monitoring board decided to stop enrollment.
An updated analysis, performed at a median observation time of 26 months, showed there was still no significant difference in overall survival between the treatment arms (P=0.362).
Cause of death
In the intent-to-treat population—30 patients in the auto-SCT arm and 28 in the allo-SCT arm—there were 16 lymphoma-related deaths, 10 in the auto-SCT arm and 6 in the allo-SCT arm.
There were 6 deaths related to study treatment (4 early and 2 late), all in the allo-SCT arm. One patient in the allo-SCT arm died of post-transplant lymphoproliferative disorder, and 1 patient in the same arm died of hemorrhage after salvage. One patient in each arm died as a result of salvage treatment.
Dr Schmitz and his colleagues also looked at the cause of death among patients who received a transplant—19 in the auto-SCT arm and 17 in the allo-SCT arm.
After SCT, there were 7 deaths in each arm. In the auto-SCT arm, there were 6 lymphoma-related deaths and 1 death related to salvage treatment. In the allo-SCT arm, there were 7 cases of non-relapse-related mortality, including 1 patient with post-transplant lymphoproliferative disorder.
“There certainly seems to be a [graft-vs-lymphoma] effect of allo-transplant in T-cell lymphoma that is, unfortunately, in some way, counterbalanced by high transplant-related mortality,” Dr Schmitz said.
He added that results of a final analysis of the 104 patients enrolled on this study should be available in 2017. ![]()
*Information in the abstract differs from that presented at the meeting.

© ASCO/Max Gersh
CHICAGO—Allogeneic and autologous transplants produce similar survival rates when used as first-line therapy in younger patients with peripheral
T-cell lymphoma (PTCL), according to interim results of the AATT trial.
The study also showed that deaths among patients who received autologous stem cell transplants (auto-SCTs) were a result of relapse and salvage treatment, while deaths among allogeneic SCT (allo-SCT) recipients were transplant-related.
Norbert Schmitz, MD, PhD, of Asklepios Hospital St. Georg in Hamburg, Germany, presented these findings at the 2015 ASCO Annual Meeting (abstract 8507*).
Dr Schmitz noted that only previous study comparing auto-SCT with allo-SCT as first-line therapy in PTCL was not designed or powered to evaluate the differences between the transplant types.
So he and his colleagues conducted the AATT trial to determine the differences. The team hypothesized that allo-SCT would improve 3-year event-free survival from 35% to 60%, given an α of 5% and a power of 80%. They needed 140 patients to prove or disprove this theory.
Ultimately, the investigators enrolled 104 patients and performed an interim analysis when 58 patients were evaluable for response.
Of the 58 patients, 30 were randomized to the auto-SCT arm and 28 to the allo-SCT arm. Baseline characteristics were similar between the arms, including patients’ median ages (49 and 50, respectively), the proportion of patients with stage III/IV disease (87% and 93%), and the proportion with ECOG status greater than 1 (23% and 18%).
Most patients in both arms had PTCL not otherwise specified (36% in the auto-SCT arm and 50% in the allo-SCT arm). Other subtypes included angioimmunoblastic T-cell lymphoma (23% and 32%, respectively), ALK-negative anaplastic large-cell lymphoma (20% and 4%), and “other” PTCLs (20% and 8%). The other PTCLs were NK/T-cell lymphoma, intestinal T/NK-cell lymphoma, hepatosplenic γδ lymphoma, and subcutaneous panniculitis-like PTCL.
Treatment characteristics
Before undergoing transplant, patients in both arms received treatment with CHOEP (cyclophosphamide, doxorubicin, etoposide, vincristine, and prednisone) on days 1, 15, 29, and 43. If they experienced a complete response (CR), partial response, or no change, patients received DHAP (dexamethasone, cytarabine, and cisplatin) on day 64.
Patients in the auto-SCT arm received BEAM (carmustine, etoposide, cytarabine, and melphalan) prior to transplant. And patients in the allo-SCT arm received FBC (fludarabine, busulfan, and cyclophosphamide).
Overall, 36 patients (62%) completed treatment per protocol, 19 in the auto-SCT arm and 17 in the allo-SCT arm. Thirty-eight percent of all patients could not proceed to transplant per protocol, mostly because of early lymphoma progression.
Response and survival
The researchers observed CRs/unconfirmed CRs (CRus) in 33% (n=10) of patients in the auto-SCT arm and 39% (n=11) in the allo-SCT arm. CR/CRus and progressive disease within 2 months occurred in 3% (n=1) and 4% (n=1) of patients, respectively.
Partial responses were seen in 17% (n=5) of patients in the auto-SCT arm and 7% (n=2) in the allo-SCT arm. There was no change in 7% (n=2) and 0% of patients, respectively. And responses were unknown in 7% (n=2) of patients in the auto-SCT arm.
Progressive disease occurred in 33% (n=10) of patients in the auto-SCT arm and 36% (n=10) in the allo-SCT arm. And treatment-related death occurred in 0% (n=0) and 14% (n=4), respectively.
At the interim analysis, there was no significant difference between the treatment arms with regard to event-free survival (P=0.963) or overall survival (P=0.174).
“At that time, the decision was made to stop the study,” Dr Schmitz said.
He explained that a conditional power analysis showed a low probability that the primary endpoint—a 25% improvement in event-free survival with allo-SCT—could still be met. So the data safety monitoring board decided to stop enrollment.
An updated analysis, performed at a median observation time of 26 months, showed there was still no significant difference in overall survival between the treatment arms (P=0.362).
Cause of death
In the intent-to-treat population—30 patients in the auto-SCT arm and 28 in the allo-SCT arm—there were 16 lymphoma-related deaths, 10 in the auto-SCT arm and 6 in the allo-SCT arm.
There were 6 deaths related to study treatment (4 early and 2 late), all in the allo-SCT arm. One patient in the allo-SCT arm died of post-transplant lymphoproliferative disorder, and 1 patient in the same arm died of hemorrhage after salvage. One patient in each arm died as a result of salvage treatment.
Dr Schmitz and his colleagues also looked at the cause of death among patients who received a transplant—19 in the auto-SCT arm and 17 in the allo-SCT arm.
After SCT, there were 7 deaths in each arm. In the auto-SCT arm, there were 6 lymphoma-related deaths and 1 death related to salvage treatment. In the allo-SCT arm, there were 7 cases of non-relapse-related mortality, including 1 patient with post-transplant lymphoproliferative disorder.
“There certainly seems to be a [graft-vs-lymphoma] effect of allo-transplant in T-cell lymphoma that is, unfortunately, in some way, counterbalanced by high transplant-related mortality,” Dr Schmitz said.
He added that results of a final analysis of the 104 patients enrolled on this study should be available in 2017. ![]()
*Information in the abstract differs from that presented at the meeting.

© ASCO/Max Gersh
CHICAGO—Allogeneic and autologous transplants produce similar survival rates when used as first-line therapy in younger patients with peripheral
T-cell lymphoma (PTCL), according to interim results of the AATT trial.
The study also showed that deaths among patients who received autologous stem cell transplants (auto-SCTs) were a result of relapse and salvage treatment, while deaths among allogeneic SCT (allo-SCT) recipients were transplant-related.
Norbert Schmitz, MD, PhD, of Asklepios Hospital St. Georg in Hamburg, Germany, presented these findings at the 2015 ASCO Annual Meeting (abstract 8507*).
Dr Schmitz noted that only previous study comparing auto-SCT with allo-SCT as first-line therapy in PTCL was not designed or powered to evaluate the differences between the transplant types.
So he and his colleagues conducted the AATT trial to determine the differences. The team hypothesized that allo-SCT would improve 3-year event-free survival from 35% to 60%, given an α of 5% and a power of 80%. They needed 140 patients to prove or disprove this theory.
Ultimately, the investigators enrolled 104 patients and performed an interim analysis when 58 patients were evaluable for response.
Of the 58 patients, 30 were randomized to the auto-SCT arm and 28 to the allo-SCT arm. Baseline characteristics were similar between the arms, including patients’ median ages (49 and 50, respectively), the proportion of patients with stage III/IV disease (87% and 93%), and the proportion with ECOG status greater than 1 (23% and 18%).
Most patients in both arms had PTCL not otherwise specified (36% in the auto-SCT arm and 50% in the allo-SCT arm). Other subtypes included angioimmunoblastic T-cell lymphoma (23% and 32%, respectively), ALK-negative anaplastic large-cell lymphoma (20% and 4%), and “other” PTCLs (20% and 8%). The other PTCLs were NK/T-cell lymphoma, intestinal T/NK-cell lymphoma, hepatosplenic γδ lymphoma, and subcutaneous panniculitis-like PTCL.
Treatment characteristics
Before undergoing transplant, patients in both arms received treatment with CHOEP (cyclophosphamide, doxorubicin, etoposide, vincristine, and prednisone) on days 1, 15, 29, and 43. If they experienced a complete response (CR), partial response, or no change, patients received DHAP (dexamethasone, cytarabine, and cisplatin) on day 64.
Patients in the auto-SCT arm received BEAM (carmustine, etoposide, cytarabine, and melphalan) prior to transplant. And patients in the allo-SCT arm received FBC (fludarabine, busulfan, and cyclophosphamide).
Overall, 36 patients (62%) completed treatment per protocol, 19 in the auto-SCT arm and 17 in the allo-SCT arm. Thirty-eight percent of all patients could not proceed to transplant per protocol, mostly because of early lymphoma progression.
Response and survival
The researchers observed CRs/unconfirmed CRs (CRus) in 33% (n=10) of patients in the auto-SCT arm and 39% (n=11) in the allo-SCT arm. CR/CRus and progressive disease within 2 months occurred in 3% (n=1) and 4% (n=1) of patients, respectively.
Partial responses were seen in 17% (n=5) of patients in the auto-SCT arm and 7% (n=2) in the allo-SCT arm. There was no change in 7% (n=2) and 0% of patients, respectively. And responses were unknown in 7% (n=2) of patients in the auto-SCT arm.
Progressive disease occurred in 33% (n=10) of patients in the auto-SCT arm and 36% (n=10) in the allo-SCT arm. And treatment-related death occurred in 0% (n=0) and 14% (n=4), respectively.
At the interim analysis, there was no significant difference between the treatment arms with regard to event-free survival (P=0.963) or overall survival (P=0.174).
“At that time, the decision was made to stop the study,” Dr Schmitz said.
He explained that a conditional power analysis showed a low probability that the primary endpoint—a 25% improvement in event-free survival with allo-SCT—could still be met. So the data safety monitoring board decided to stop enrollment.
An updated analysis, performed at a median observation time of 26 months, showed there was still no significant difference in overall survival between the treatment arms (P=0.362).
Cause of death
In the intent-to-treat population—30 patients in the auto-SCT arm and 28 in the allo-SCT arm—there were 16 lymphoma-related deaths, 10 in the auto-SCT arm and 6 in the allo-SCT arm.
There were 6 deaths related to study treatment (4 early and 2 late), all in the allo-SCT arm. One patient in the allo-SCT arm died of post-transplant lymphoproliferative disorder, and 1 patient in the same arm died of hemorrhage after salvage. One patient in each arm died as a result of salvage treatment.
Dr Schmitz and his colleagues also looked at the cause of death among patients who received a transplant—19 in the auto-SCT arm and 17 in the allo-SCT arm.
After SCT, there were 7 deaths in each arm. In the auto-SCT arm, there were 6 lymphoma-related deaths and 1 death related to salvage treatment. In the allo-SCT arm, there were 7 cases of non-relapse-related mortality, including 1 patient with post-transplant lymphoproliferative disorder.
“There certainly seems to be a [graft-vs-lymphoma] effect of allo-transplant in T-cell lymphoma that is, unfortunately, in some way, counterbalanced by high transplant-related mortality,” Dr Schmitz said.
He added that results of a final analysis of the 104 patients enrolled on this study should be available in 2017. ![]()
*Information in the abstract differs from that presented at the meeting.
Triplet shows early promise for relapsed CLL, NHL

©ASCO/Rodney White
CHICAGO—A 3-drug combination is safe and highly active in certain patients with relapsed B-cell malignancies, according to a speaker at the 2015 ASCO Annual Meeting.
The combination consists of the anti-CD20 monoclonal antibody ublituximab, the PI3Kδ inhibitor TGR-1202, and the BTK inhibitor ibrutinib.
In a small, phase 1 study, the triplet produced an overall response rate of 62%. It was particularly active in patients with chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) and those with mantle cell lymphoma (MCL).
The most common adverse events were infusion reactions, gastrointestinal events, rash, and fatigue. Grade 3 neutropenia and leukopenia occurred in 1 patient each.
Nathan Fowler, MD, of MD Anderson Cancer Center in Houston, Texas, presented these results at the meeting as abstract 8501.*
The trial enrolled 16 patients with CLL/SLL or non-Hodgkin lymphoma (NHL). Four had CLL, 1 had SLL, and 1 had Richter’s transformation. Four patients had follicular lymphoma (FL), 3 had diffuse large B-cell lymphoma (DLBCL), 2 had mantle cell lymphoma (MCL), and 1 had marginal zone lymphoma (MZL).
The patients’ median age was 63, and their median number of prior treatment regimens was 4 (range, 1-5). Fifty percent of patients (n=8) were refractory to prior therapy.
Treatment consisted of 900 mg of ublituximab, ibrutinib at either 420 mg (CLL/SLL) or 560 mg (NHL), and TGR-1202 at 3 different doses: 400 mg, 600 mg, or 800 mg. Ibrutinib and TGR-1202 were given once-daily beginning on day 1 of each cycle. Ublituximab was given on days 1, 8, and 15 of cycles 1 and 2, then on day 1 of cycles 4, 6, 9, and 12.
Safety and efficacy
Sixteen patients were evaluable for safety and 13 for efficacy. One of the patients was removed from the efficacy analysis at the discretion of the investigators, and it was too early to evaluate the other 2 patients.
The median time on study was 4 months (range, 1-9 months). The 5 CLL/SLL patients received TGR-1202 at 400 mg. One of these patients had a dose-limiting toxicity—reactivation of varicella zoster.
Of the NHL patients, 3 received TGR-1202 at 400 mg, 4 received 600 mg, and 4 received 800 mg. There were no dose-limiting toxicities in any of these patients.
Adverse events that were considered possibly related to treatment included infusion reactions (25%), diarrhea (19%), nausea (19%), fatigue (19%), rash (19%), anemia (13%), neutropenia (13%), leukopenia (13%), and insomnia (13%). Grade 3 events included neutropenia and leukopenia (6% each), and there were no grade 4 events.
“The majority of patients have demonstrated a response to the therapy,” Dr Fowler said. “All of the patients that have responded continue on treatment, and the longest [treatment duration] is about 10 months.”
The only complete response occurred in a patient with MCL. Partial responses occurred in all 3 CLL patients, 2 FL patients, the SLL patient, the MZL patient, and 1 MCL patient. One patient with FL, 2 with DLBCL, and 1 with Richter’s transformation did not respond to treatment.
In closing, Dr Fowler said this treatment was well-tolerated and showed significant early activity in this heavily pretreated patient population. Dose-escalation with TGR-1202 continues at 800 mg, and phase 2 studies of the triplet are planned. ![]()
*Information in the abstract differs from that presented at the meeting.

©ASCO/Rodney White
CHICAGO—A 3-drug combination is safe and highly active in certain patients with relapsed B-cell malignancies, according to a speaker at the 2015 ASCO Annual Meeting.
The combination consists of the anti-CD20 monoclonal antibody ublituximab, the PI3Kδ inhibitor TGR-1202, and the BTK inhibitor ibrutinib.
In a small, phase 1 study, the triplet produced an overall response rate of 62%. It was particularly active in patients with chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) and those with mantle cell lymphoma (MCL).
The most common adverse events were infusion reactions, gastrointestinal events, rash, and fatigue. Grade 3 neutropenia and leukopenia occurred in 1 patient each.
Nathan Fowler, MD, of MD Anderson Cancer Center in Houston, Texas, presented these results at the meeting as abstract 8501.*
The trial enrolled 16 patients with CLL/SLL or non-Hodgkin lymphoma (NHL). Four had CLL, 1 had SLL, and 1 had Richter’s transformation. Four patients had follicular lymphoma (FL), 3 had diffuse large B-cell lymphoma (DLBCL), 2 had mantle cell lymphoma (MCL), and 1 had marginal zone lymphoma (MZL).
The patients’ median age was 63, and their median number of prior treatment regimens was 4 (range, 1-5). Fifty percent of patients (n=8) were refractory to prior therapy.
Treatment consisted of 900 mg of ublituximab, ibrutinib at either 420 mg (CLL/SLL) or 560 mg (NHL), and TGR-1202 at 3 different doses: 400 mg, 600 mg, or 800 mg. Ibrutinib and TGR-1202 were given once-daily beginning on day 1 of each cycle. Ublituximab was given on days 1, 8, and 15 of cycles 1 and 2, then on day 1 of cycles 4, 6, 9, and 12.
Safety and efficacy
Sixteen patients were evaluable for safety and 13 for efficacy. One of the patients was removed from the efficacy analysis at the discretion of the investigators, and it was too early to evaluate the other 2 patients.
The median time on study was 4 months (range, 1-9 months). The 5 CLL/SLL patients received TGR-1202 at 400 mg. One of these patients had a dose-limiting toxicity—reactivation of varicella zoster.
Of the NHL patients, 3 received TGR-1202 at 400 mg, 4 received 600 mg, and 4 received 800 mg. There were no dose-limiting toxicities in any of these patients.
Adverse events that were considered possibly related to treatment included infusion reactions (25%), diarrhea (19%), nausea (19%), fatigue (19%), rash (19%), anemia (13%), neutropenia (13%), leukopenia (13%), and insomnia (13%). Grade 3 events included neutropenia and leukopenia (6% each), and there were no grade 4 events.
“The majority of patients have demonstrated a response to the therapy,” Dr Fowler said. “All of the patients that have responded continue on treatment, and the longest [treatment duration] is about 10 months.”
The only complete response occurred in a patient with MCL. Partial responses occurred in all 3 CLL patients, 2 FL patients, the SLL patient, the MZL patient, and 1 MCL patient. One patient with FL, 2 with DLBCL, and 1 with Richter’s transformation did not respond to treatment.
In closing, Dr Fowler said this treatment was well-tolerated and showed significant early activity in this heavily pretreated patient population. Dose-escalation with TGR-1202 continues at 800 mg, and phase 2 studies of the triplet are planned. ![]()
*Information in the abstract differs from that presented at the meeting.

©ASCO/Rodney White
CHICAGO—A 3-drug combination is safe and highly active in certain patients with relapsed B-cell malignancies, according to a speaker at the 2015 ASCO Annual Meeting.
The combination consists of the anti-CD20 monoclonal antibody ublituximab, the PI3Kδ inhibitor TGR-1202, and the BTK inhibitor ibrutinib.
In a small, phase 1 study, the triplet produced an overall response rate of 62%. It was particularly active in patients with chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) and those with mantle cell lymphoma (MCL).
The most common adverse events were infusion reactions, gastrointestinal events, rash, and fatigue. Grade 3 neutropenia and leukopenia occurred in 1 patient each.
Nathan Fowler, MD, of MD Anderson Cancer Center in Houston, Texas, presented these results at the meeting as abstract 8501.*
The trial enrolled 16 patients with CLL/SLL or non-Hodgkin lymphoma (NHL). Four had CLL, 1 had SLL, and 1 had Richter’s transformation. Four patients had follicular lymphoma (FL), 3 had diffuse large B-cell lymphoma (DLBCL), 2 had mantle cell lymphoma (MCL), and 1 had marginal zone lymphoma (MZL).
The patients’ median age was 63, and their median number of prior treatment regimens was 4 (range, 1-5). Fifty percent of patients (n=8) were refractory to prior therapy.
Treatment consisted of 900 mg of ublituximab, ibrutinib at either 420 mg (CLL/SLL) or 560 mg (NHL), and TGR-1202 at 3 different doses: 400 mg, 600 mg, or 800 mg. Ibrutinib and TGR-1202 were given once-daily beginning on day 1 of each cycle. Ublituximab was given on days 1, 8, and 15 of cycles 1 and 2, then on day 1 of cycles 4, 6, 9, and 12.
Safety and efficacy
Sixteen patients were evaluable for safety and 13 for efficacy. One of the patients was removed from the efficacy analysis at the discretion of the investigators, and it was too early to evaluate the other 2 patients.
The median time on study was 4 months (range, 1-9 months). The 5 CLL/SLL patients received TGR-1202 at 400 mg. One of these patients had a dose-limiting toxicity—reactivation of varicella zoster.
Of the NHL patients, 3 received TGR-1202 at 400 mg, 4 received 600 mg, and 4 received 800 mg. There were no dose-limiting toxicities in any of these patients.
Adverse events that were considered possibly related to treatment included infusion reactions (25%), diarrhea (19%), nausea (19%), fatigue (19%), rash (19%), anemia (13%), neutropenia (13%), leukopenia (13%), and insomnia (13%). Grade 3 events included neutropenia and leukopenia (6% each), and there were no grade 4 events.
“The majority of patients have demonstrated a response to the therapy,” Dr Fowler said. “All of the patients that have responded continue on treatment, and the longest [treatment duration] is about 10 months.”
The only complete response occurred in a patient with MCL. Partial responses occurred in all 3 CLL patients, 2 FL patients, the SLL patient, the MZL patient, and 1 MCL patient. One patient with FL, 2 with DLBCL, and 1 with Richter’s transformation did not respond to treatment.
In closing, Dr Fowler said this treatment was well-tolerated and showed significant early activity in this heavily pretreated patient population. Dose-escalation with TGR-1202 continues at 800 mg, and phase 2 studies of the triplet are planned. ![]()
*Information in the abstract differs from that presented at the meeting.
Drug prolongs PFS in indolent, refractory NHL

the 2015 ASCO Annual Meeting
CHICAGO—Adding obinutuzumab to treatment with bendamustine improves progression-free survival (PFS) in patients with rituximab-refractory, indolent non-Hodgkin lymphoma (NHL), interim results of the phase 3 GADOLIN trial suggest.
Study investigators said patients who received obinutuzumab and bendamustine followed by obinutuzumab maintenance had roughly double the PFS of patients who received bendamustine alone.
There was no significant difference between the treatment groups with regard to response rates or overall survival (OS), but the investigators said longer follow-up is needed to determine if obinutuzumab confers a benefit in OS.
This trial was stopped before its protocol-specified final analysis because of the PFS benefit observed in the obinutuzumab arm.
Laurie Sehn, MD, of the BC Cancer Agency in Vancouver, Canada, presented these results at the 2015 ASCO Annual Meeting (abstract LBA8502). Genentech Inc. and F. Hoffmann-La Roche Ltd. funded this research.
The trial included 413 patients with rituximab-refractory NHL, including follicular lymphoma (FL), marginal zone lymphoma (MZL), small lymphocytic lymphoma (SLL), and Waldenstrom’s macroglobulinemia (WM).
The patients were randomized to receive bendamustine alone (120 mg/m2/day on days 1 and 2 for up to six 28-day cycles) or a combination of bendamustine (90 mg/m2/day on days 1 and 2 for up to six 28-day cycles) plus obinutuzumab (1000 mg on days 1, 8, and 15 for cycle 1, followed by 1 dose for up to six 28-day cycles), followed by obinutuzumab maintenance (1000 mg every 2 months for 2 years or until progression).
Dr Sehn said there were no significant differences in baseline characteristics between the treatment arms. Patients in both arms had received a median of 2 prior treatments, and the median time from last treatment was about 4 months.
Of the 194 patients randomized to treatment in the obinutuzumab-bendamustine (OB) arm, 79.9% had FL, 13.9% had MZL, and 6.2% had SLL. Of the 202 patients randomized to the bendamustine-alone (control) arm, 82.2% had FL, 9.4% had MZL, 7.9% had SLL, and 0.5% had WM.
Ultimately, 156 patients completed induction in the OB arm, as did 129 patients in the control arm. Thirty-six patients completed maintenance with obinutuzumab, and 46 were still receiving maintenance at the time of analysis.
Safety results
Dr Sehn said there were no unexpected safety signals among patients in the OB arm.
About 99% of patients in the OB arm experienced at least 1 adverse event (AE), as did 98% of patients in the control arm. Severe AEs occurred in 38.1% and 32.8% of patients, respectively, and grade 3/4 AEs occurred in 67% and 62.1%, respectively.
AEs leading to treatment withdrawal occurred in 18% and 15.7% of patients, respectively. And AEs leading to death occurred in 6.2% and 6.1%, respectively.
Grade 3/4 AEs that occurred in at least 2% of patients in the OB and control arms, respectively, were neutropenia (33% vs 26.3%), thrombocytopenia (10.8% vs 16.2%), infusion-related reactions (10.8% vs 5.6%), anemia (7.7% vs 10.1%), febrile neutropenia (4.6% vs 3.5%), nausea (1% vs 3%), fatigue (1.5% vs 2.5%), diarrhea (1% vs 2.5%), and vomiting (2.1% vs 1%).
Response and survival
According to an independent radiology facility, 69.2% of patients in the OB arm had responded to treatment at the end of induction, as had 63% of the control arm. The best overall response by the 12-month mark was 78.7% and 76.6%, respectively.
The median follow-up was 21 months. At that point, the median PFS had not been reached in the OB arm but was 14.9 months in the control arm (P<0.0001), according to the independent radiology facility.
According to investigators, the median PFS was 29.2 months and 14 months, respectively (P<0.0001).
The median OS has not been reached in either arm (P=0.4017). Thirty-four patients (18%) in the OB arm died, as did 41 (20%) in the control arm.
Dr Sehn said longer follow-up is needed to determine the potential OS benefit associated with obinutuzumab, but the PFS benefit of OB is clinically meaningful.
“The fact that this new approach doubled average remission time marks a major step forward for our patients,” she said. “Obinutuzumab may offer patients the chance to stay well for a significantly longer period of time, putting off the need for additional chemotherapy.” ![]()

the 2015 ASCO Annual Meeting
CHICAGO—Adding obinutuzumab to treatment with bendamustine improves progression-free survival (PFS) in patients with rituximab-refractory, indolent non-Hodgkin lymphoma (NHL), interim results of the phase 3 GADOLIN trial suggest.
Study investigators said patients who received obinutuzumab and bendamustine followed by obinutuzumab maintenance had roughly double the PFS of patients who received bendamustine alone.
There was no significant difference between the treatment groups with regard to response rates or overall survival (OS), but the investigators said longer follow-up is needed to determine if obinutuzumab confers a benefit in OS.
This trial was stopped before its protocol-specified final analysis because of the PFS benefit observed in the obinutuzumab arm.
Laurie Sehn, MD, of the BC Cancer Agency in Vancouver, Canada, presented these results at the 2015 ASCO Annual Meeting (abstract LBA8502). Genentech Inc. and F. Hoffmann-La Roche Ltd. funded this research.
The trial included 413 patients with rituximab-refractory NHL, including follicular lymphoma (FL), marginal zone lymphoma (MZL), small lymphocytic lymphoma (SLL), and Waldenstrom’s macroglobulinemia (WM).
The patients were randomized to receive bendamustine alone (120 mg/m2/day on days 1 and 2 for up to six 28-day cycles) or a combination of bendamustine (90 mg/m2/day on days 1 and 2 for up to six 28-day cycles) plus obinutuzumab (1000 mg on days 1, 8, and 15 for cycle 1, followed by 1 dose for up to six 28-day cycles), followed by obinutuzumab maintenance (1000 mg every 2 months for 2 years or until progression).
Dr Sehn said there were no significant differences in baseline characteristics between the treatment arms. Patients in both arms had received a median of 2 prior treatments, and the median time from last treatment was about 4 months.
Of the 194 patients randomized to treatment in the obinutuzumab-bendamustine (OB) arm, 79.9% had FL, 13.9% had MZL, and 6.2% had SLL. Of the 202 patients randomized to the bendamustine-alone (control) arm, 82.2% had FL, 9.4% had MZL, 7.9% had SLL, and 0.5% had WM.
Ultimately, 156 patients completed induction in the OB arm, as did 129 patients in the control arm. Thirty-six patients completed maintenance with obinutuzumab, and 46 were still receiving maintenance at the time of analysis.
Safety results
Dr Sehn said there were no unexpected safety signals among patients in the OB arm.
About 99% of patients in the OB arm experienced at least 1 adverse event (AE), as did 98% of patients in the control arm. Severe AEs occurred in 38.1% and 32.8% of patients, respectively, and grade 3/4 AEs occurred in 67% and 62.1%, respectively.
AEs leading to treatment withdrawal occurred in 18% and 15.7% of patients, respectively. And AEs leading to death occurred in 6.2% and 6.1%, respectively.
Grade 3/4 AEs that occurred in at least 2% of patients in the OB and control arms, respectively, were neutropenia (33% vs 26.3%), thrombocytopenia (10.8% vs 16.2%), infusion-related reactions (10.8% vs 5.6%), anemia (7.7% vs 10.1%), febrile neutropenia (4.6% vs 3.5%), nausea (1% vs 3%), fatigue (1.5% vs 2.5%), diarrhea (1% vs 2.5%), and vomiting (2.1% vs 1%).
Response and survival
According to an independent radiology facility, 69.2% of patients in the OB arm had responded to treatment at the end of induction, as had 63% of the control arm. The best overall response by the 12-month mark was 78.7% and 76.6%, respectively.
The median follow-up was 21 months. At that point, the median PFS had not been reached in the OB arm but was 14.9 months in the control arm (P<0.0001), according to the independent radiology facility.
According to investigators, the median PFS was 29.2 months and 14 months, respectively (P<0.0001).
The median OS has not been reached in either arm (P=0.4017). Thirty-four patients (18%) in the OB arm died, as did 41 (20%) in the control arm.
Dr Sehn said longer follow-up is needed to determine the potential OS benefit associated with obinutuzumab, but the PFS benefit of OB is clinically meaningful.
“The fact that this new approach doubled average remission time marks a major step forward for our patients,” she said. “Obinutuzumab may offer patients the chance to stay well for a significantly longer period of time, putting off the need for additional chemotherapy.” ![]()

the 2015 ASCO Annual Meeting
CHICAGO—Adding obinutuzumab to treatment with bendamustine improves progression-free survival (PFS) in patients with rituximab-refractory, indolent non-Hodgkin lymphoma (NHL), interim results of the phase 3 GADOLIN trial suggest.
Study investigators said patients who received obinutuzumab and bendamustine followed by obinutuzumab maintenance had roughly double the PFS of patients who received bendamustine alone.
There was no significant difference between the treatment groups with regard to response rates or overall survival (OS), but the investigators said longer follow-up is needed to determine if obinutuzumab confers a benefit in OS.
This trial was stopped before its protocol-specified final analysis because of the PFS benefit observed in the obinutuzumab arm.
Laurie Sehn, MD, of the BC Cancer Agency in Vancouver, Canada, presented these results at the 2015 ASCO Annual Meeting (abstract LBA8502). Genentech Inc. and F. Hoffmann-La Roche Ltd. funded this research.
The trial included 413 patients with rituximab-refractory NHL, including follicular lymphoma (FL), marginal zone lymphoma (MZL), small lymphocytic lymphoma (SLL), and Waldenstrom’s macroglobulinemia (WM).
The patients were randomized to receive bendamustine alone (120 mg/m2/day on days 1 and 2 for up to six 28-day cycles) or a combination of bendamustine (90 mg/m2/day on days 1 and 2 for up to six 28-day cycles) plus obinutuzumab (1000 mg on days 1, 8, and 15 for cycle 1, followed by 1 dose for up to six 28-day cycles), followed by obinutuzumab maintenance (1000 mg every 2 months for 2 years or until progression).
Dr Sehn said there were no significant differences in baseline characteristics between the treatment arms. Patients in both arms had received a median of 2 prior treatments, and the median time from last treatment was about 4 months.
Of the 194 patients randomized to treatment in the obinutuzumab-bendamustine (OB) arm, 79.9% had FL, 13.9% had MZL, and 6.2% had SLL. Of the 202 patients randomized to the bendamustine-alone (control) arm, 82.2% had FL, 9.4% had MZL, 7.9% had SLL, and 0.5% had WM.
Ultimately, 156 patients completed induction in the OB arm, as did 129 patients in the control arm. Thirty-six patients completed maintenance with obinutuzumab, and 46 were still receiving maintenance at the time of analysis.
Safety results
Dr Sehn said there were no unexpected safety signals among patients in the OB arm.
About 99% of patients in the OB arm experienced at least 1 adverse event (AE), as did 98% of patients in the control arm. Severe AEs occurred in 38.1% and 32.8% of patients, respectively, and grade 3/4 AEs occurred in 67% and 62.1%, respectively.
AEs leading to treatment withdrawal occurred in 18% and 15.7% of patients, respectively. And AEs leading to death occurred in 6.2% and 6.1%, respectively.
Grade 3/4 AEs that occurred in at least 2% of patients in the OB and control arms, respectively, were neutropenia (33% vs 26.3%), thrombocytopenia (10.8% vs 16.2%), infusion-related reactions (10.8% vs 5.6%), anemia (7.7% vs 10.1%), febrile neutropenia (4.6% vs 3.5%), nausea (1% vs 3%), fatigue (1.5% vs 2.5%), diarrhea (1% vs 2.5%), and vomiting (2.1% vs 1%).
Response and survival
According to an independent radiology facility, 69.2% of patients in the OB arm had responded to treatment at the end of induction, as had 63% of the control arm. The best overall response by the 12-month mark was 78.7% and 76.6%, respectively.
The median follow-up was 21 months. At that point, the median PFS had not been reached in the OB arm but was 14.9 months in the control arm (P<0.0001), according to the independent radiology facility.
According to investigators, the median PFS was 29.2 months and 14 months, respectively (P<0.0001).
The median OS has not been reached in either arm (P=0.4017). Thirty-four patients (18%) in the OB arm died, as did 41 (20%) in the control arm.
Dr Sehn said longer follow-up is needed to determine the potential OS benefit associated with obinutuzumab, but the PFS benefit of OB is clinically meaningful.
“The fact that this new approach doubled average remission time marks a major step forward for our patients,” she said. “Obinutuzumab may offer patients the chance to stay well for a significantly longer period of time, putting off the need for additional chemotherapy.” ![]()
Drug improves upon standard therapy for relapsed CLL/SLL, speaker says

Chanan-Khan, MD
© ASCO/Zach Boyden-Holmes
CHICAGO—Interim results of the phase 3 HELIOS trial suggest that adding ibrutinib to treatment with bendamustine and rituximab (BR) improves outcomes for patients with relapsed chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL).
Patients who received ibrutinib and BR had significantly higher response rates and a significantly longer progression-free survival than patients who received BR with placebo.
There was no significant difference between the arms with regard to overall survival, but the researchers said these results were confounded by the fact that 31% of patients in the placebo arm crossed over to the ibrutinib arm after they progressed.
“We found that ibrutinib can be safely paired with existing therapy to powerfully prolong remissions and improve patients’ well-being,” said study investigator Asher Alban Akmal Chanan-Khan, MD, of the Mayo Clinic in Jacksonville, Florida.
Dr Chanan-Khan presented these findings at the 2015 ASCO Annual Meeting (abstract LBA7005). The research was funded by Janssen Research & Development, LLC, the company co-developing ibrutinib with Pharmacyclics.
The study included 578 patients with previously treated CLL/SLL, excluding those with del(17p). The patients were randomized to receive 6 cycles of BR plus once-daily ibrutinib (n=289) or 6 cycles of BR plus placebo (n=289). Ibrutinib and placebo were given until disease progression or unacceptable toxicity.
Dr Chanan-Khan said baseline characteristics were comparable between the treatment arms. For each arm, the median number of prior treatments was 2, more than 50% of patients had bulky disease, and about 80% of patients had unmutated IGVH.
“[However,] advanced Rai-stage disease was observed in a slightly [greater] proportion of patients in the control arm versus the ibrutinib arm,” Dr Chanan-Khan noted. “Conversely, a higher proportion of patients with del(11q) was noted in the ibrutinib-containing arm.”
Ultimately, 81.9% (n=235) of patients in the ibrutinib arm and 77.4% (n=222) of those in the placebo arm received their assigned 6 cycles of BR. At the time of analysis, the rate of treatment discontinuation was 29.1% (n=84) in the ibrutinib arm and 64.7% in the placebo arm (n=187).
Those patients who progressed on placebo were allowed to cross over to the ibrutinib arm, and 90 patients had crossed over at the time of the interim analysis.
Response and survival
The study’s primary endpoint was progression-free survival, as assessed by an independent review committee (IRC), in the intent-to-treat population (n=289 in each arm).
At a median follow-up of 17 months, progression-free survival was 13.3 months in the placebo arm and was not reached in the ibrutinib arm (P<0.0001).
“The hazard ratio on this particular survival curve is 0.20, which translates into a reduced risk of progression or death by 80%,” Dr Chanan-Khan said. “This is remarkable. You cannot get a better hazard ratio than this.”
Dr Chanan-Khan also noted that the overall response rate was significantly higher in the ibrutinib arm than the placebo arm. The rates were 82.7% and 67.8%, respectively (P<0.0001), according to the IRC, and 86.2% and 68.9%, respectively (P<0.0001), according to investigator assessment.
The rate of complete response plus complete response with incomplete blood count recovery was 10.4% in the ibrutinib arm and 2.8% in the placebo arm, according to the IRC. According to investigator assessment, the rates were 21.4% and 5.9%, respectively.
The median overall survival was not reached in either arm, and the hazard ratio was 0.628 (P=0.0598).
Adverse events
Dr Chanan-Kahn said the safety profile of the ibrutinib-BR combination was consistent with the safety profiles of each individual drug.
The incidence of adverse events was 70.7% in the ibrutinib-BR arm and 70% in the placebo-BR arm. The most common events were neutropenia (58.2% and 54.7%, respectively), nausea (36.9% vs 35.2%), diarrhea (35.5% vs 23.7%), thrombocytopenia (30.7% vs 24.4%), pyrexia (24.7% vs 22%), anemia (22.6% vs 28.9%), and fatigue (21.6% vs 22.6%).
The incidence of grade 3/4 adverse events was 28.9% in the ibrutinib arm and 25% in the placebo arm. The most common of these were neutropenia (53.7% vs 50.5%) and thrombocytopenia (15% in both arms).
Atrial fibrillation was seen in 7.3% of patients in the ibrutinib arm and 2.8% in the placebo arm. Grade 3/4 atrial fibrillation occurred in 2.8% and 0.7% of patients, respectively. The incidence of tumor lysis syndrome was 3.5% in both arms.
The rate of bleeding was 31% in the ibrutinib arm and 14.6% in the placebo arm. And the rates of major hemorrhage were 3.8% and 1.7%, respectively.
Adverse events were the primary reason for discontinuation in patients who received ibrutinib—14.2%, compared to 11.8% of patients who received placebo. The primary reason for discontinuation in the placebo arm was progressive disease or relapse—45%, compared to 4.8% in the ibrutinib arm.
Taken together, the results of this trial suggest treatment with ibrutinib and BR is superior to standard BR therapy in patients with relapsed CLL/SLL, Dr Chanan-Kahn said.
“This was one of the most rigorous clinical trials ever conducted in CLL,” he said, “and it truly validates ibrutinib as an important drug for this cancer.” ![]()

Chanan-Khan, MD
© ASCO/Zach Boyden-Holmes
CHICAGO—Interim results of the phase 3 HELIOS trial suggest that adding ibrutinib to treatment with bendamustine and rituximab (BR) improves outcomes for patients with relapsed chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL).
Patients who received ibrutinib and BR had significantly higher response rates and a significantly longer progression-free survival than patients who received BR with placebo.
There was no significant difference between the arms with regard to overall survival, but the researchers said these results were confounded by the fact that 31% of patients in the placebo arm crossed over to the ibrutinib arm after they progressed.
“We found that ibrutinib can be safely paired with existing therapy to powerfully prolong remissions and improve patients’ well-being,” said study investigator Asher Alban Akmal Chanan-Khan, MD, of the Mayo Clinic in Jacksonville, Florida.
Dr Chanan-Khan presented these findings at the 2015 ASCO Annual Meeting (abstract LBA7005). The research was funded by Janssen Research & Development, LLC, the company co-developing ibrutinib with Pharmacyclics.
The study included 578 patients with previously treated CLL/SLL, excluding those with del(17p). The patients were randomized to receive 6 cycles of BR plus once-daily ibrutinib (n=289) or 6 cycles of BR plus placebo (n=289). Ibrutinib and placebo were given until disease progression or unacceptable toxicity.
Dr Chanan-Khan said baseline characteristics were comparable between the treatment arms. For each arm, the median number of prior treatments was 2, more than 50% of patients had bulky disease, and about 80% of patients had unmutated IGVH.
“[However,] advanced Rai-stage disease was observed in a slightly [greater] proportion of patients in the control arm versus the ibrutinib arm,” Dr Chanan-Khan noted. “Conversely, a higher proportion of patients with del(11q) was noted in the ibrutinib-containing arm.”
Ultimately, 81.9% (n=235) of patients in the ibrutinib arm and 77.4% (n=222) of those in the placebo arm received their assigned 6 cycles of BR. At the time of analysis, the rate of treatment discontinuation was 29.1% (n=84) in the ibrutinib arm and 64.7% in the placebo arm (n=187).
Those patients who progressed on placebo were allowed to cross over to the ibrutinib arm, and 90 patients had crossed over at the time of the interim analysis.
Response and survival
The study’s primary endpoint was progression-free survival, as assessed by an independent review committee (IRC), in the intent-to-treat population (n=289 in each arm).
At a median follow-up of 17 months, progression-free survival was 13.3 months in the placebo arm and was not reached in the ibrutinib arm (P<0.0001).
“The hazard ratio on this particular survival curve is 0.20, which translates into a reduced risk of progression or death by 80%,” Dr Chanan-Khan said. “This is remarkable. You cannot get a better hazard ratio than this.”
Dr Chanan-Khan also noted that the overall response rate was significantly higher in the ibrutinib arm than the placebo arm. The rates were 82.7% and 67.8%, respectively (P<0.0001), according to the IRC, and 86.2% and 68.9%, respectively (P<0.0001), according to investigator assessment.
The rate of complete response plus complete response with incomplete blood count recovery was 10.4% in the ibrutinib arm and 2.8% in the placebo arm, according to the IRC. According to investigator assessment, the rates were 21.4% and 5.9%, respectively.
The median overall survival was not reached in either arm, and the hazard ratio was 0.628 (P=0.0598).
Adverse events
Dr Chanan-Kahn said the safety profile of the ibrutinib-BR combination was consistent with the safety profiles of each individual drug.
The incidence of adverse events was 70.7% in the ibrutinib-BR arm and 70% in the placebo-BR arm. The most common events were neutropenia (58.2% and 54.7%, respectively), nausea (36.9% vs 35.2%), diarrhea (35.5% vs 23.7%), thrombocytopenia (30.7% vs 24.4%), pyrexia (24.7% vs 22%), anemia (22.6% vs 28.9%), and fatigue (21.6% vs 22.6%).
The incidence of grade 3/4 adverse events was 28.9% in the ibrutinib arm and 25% in the placebo arm. The most common of these were neutropenia (53.7% vs 50.5%) and thrombocytopenia (15% in both arms).
Atrial fibrillation was seen in 7.3% of patients in the ibrutinib arm and 2.8% in the placebo arm. Grade 3/4 atrial fibrillation occurred in 2.8% and 0.7% of patients, respectively. The incidence of tumor lysis syndrome was 3.5% in both arms.
The rate of bleeding was 31% in the ibrutinib arm and 14.6% in the placebo arm. And the rates of major hemorrhage were 3.8% and 1.7%, respectively.
Adverse events were the primary reason for discontinuation in patients who received ibrutinib—14.2%, compared to 11.8% of patients who received placebo. The primary reason for discontinuation in the placebo arm was progressive disease or relapse—45%, compared to 4.8% in the ibrutinib arm.
Taken together, the results of this trial suggest treatment with ibrutinib and BR is superior to standard BR therapy in patients with relapsed CLL/SLL, Dr Chanan-Kahn said.
“This was one of the most rigorous clinical trials ever conducted in CLL,” he said, “and it truly validates ibrutinib as an important drug for this cancer.” ![]()

Chanan-Khan, MD
© ASCO/Zach Boyden-Holmes
CHICAGO—Interim results of the phase 3 HELIOS trial suggest that adding ibrutinib to treatment with bendamustine and rituximab (BR) improves outcomes for patients with relapsed chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL).
Patients who received ibrutinib and BR had significantly higher response rates and a significantly longer progression-free survival than patients who received BR with placebo.
There was no significant difference between the arms with regard to overall survival, but the researchers said these results were confounded by the fact that 31% of patients in the placebo arm crossed over to the ibrutinib arm after they progressed.
“We found that ibrutinib can be safely paired with existing therapy to powerfully prolong remissions and improve patients’ well-being,” said study investigator Asher Alban Akmal Chanan-Khan, MD, of the Mayo Clinic in Jacksonville, Florida.
Dr Chanan-Khan presented these findings at the 2015 ASCO Annual Meeting (abstract LBA7005). The research was funded by Janssen Research & Development, LLC, the company co-developing ibrutinib with Pharmacyclics.
The study included 578 patients with previously treated CLL/SLL, excluding those with del(17p). The patients were randomized to receive 6 cycles of BR plus once-daily ibrutinib (n=289) or 6 cycles of BR plus placebo (n=289). Ibrutinib and placebo were given until disease progression or unacceptable toxicity.
Dr Chanan-Khan said baseline characteristics were comparable between the treatment arms. For each arm, the median number of prior treatments was 2, more than 50% of patients had bulky disease, and about 80% of patients had unmutated IGVH.
“[However,] advanced Rai-stage disease was observed in a slightly [greater] proportion of patients in the control arm versus the ibrutinib arm,” Dr Chanan-Khan noted. “Conversely, a higher proportion of patients with del(11q) was noted in the ibrutinib-containing arm.”
Ultimately, 81.9% (n=235) of patients in the ibrutinib arm and 77.4% (n=222) of those in the placebo arm received their assigned 6 cycles of BR. At the time of analysis, the rate of treatment discontinuation was 29.1% (n=84) in the ibrutinib arm and 64.7% in the placebo arm (n=187).
Those patients who progressed on placebo were allowed to cross over to the ibrutinib arm, and 90 patients had crossed over at the time of the interim analysis.
Response and survival
The study’s primary endpoint was progression-free survival, as assessed by an independent review committee (IRC), in the intent-to-treat population (n=289 in each arm).
At a median follow-up of 17 months, progression-free survival was 13.3 months in the placebo arm and was not reached in the ibrutinib arm (P<0.0001).
“The hazard ratio on this particular survival curve is 0.20, which translates into a reduced risk of progression or death by 80%,” Dr Chanan-Khan said. “This is remarkable. You cannot get a better hazard ratio than this.”
Dr Chanan-Khan also noted that the overall response rate was significantly higher in the ibrutinib arm than the placebo arm. The rates were 82.7% and 67.8%, respectively (P<0.0001), according to the IRC, and 86.2% and 68.9%, respectively (P<0.0001), according to investigator assessment.
The rate of complete response plus complete response with incomplete blood count recovery was 10.4% in the ibrutinib arm and 2.8% in the placebo arm, according to the IRC. According to investigator assessment, the rates were 21.4% and 5.9%, respectively.
The median overall survival was not reached in either arm, and the hazard ratio was 0.628 (P=0.0598).
Adverse events
Dr Chanan-Kahn said the safety profile of the ibrutinib-BR combination was consistent with the safety profiles of each individual drug.
The incidence of adverse events was 70.7% in the ibrutinib-BR arm and 70% in the placebo-BR arm. The most common events were neutropenia (58.2% and 54.7%, respectively), nausea (36.9% vs 35.2%), diarrhea (35.5% vs 23.7%), thrombocytopenia (30.7% vs 24.4%), pyrexia (24.7% vs 22%), anemia (22.6% vs 28.9%), and fatigue (21.6% vs 22.6%).
The incidence of grade 3/4 adverse events was 28.9% in the ibrutinib arm and 25% in the placebo arm. The most common of these were neutropenia (53.7% vs 50.5%) and thrombocytopenia (15% in both arms).
Atrial fibrillation was seen in 7.3% of patients in the ibrutinib arm and 2.8% in the placebo arm. Grade 3/4 atrial fibrillation occurred in 2.8% and 0.7% of patients, respectively. The incidence of tumor lysis syndrome was 3.5% in both arms.
The rate of bleeding was 31% in the ibrutinib arm and 14.6% in the placebo arm. And the rates of major hemorrhage were 3.8% and 1.7%, respectively.
Adverse events were the primary reason for discontinuation in patients who received ibrutinib—14.2%, compared to 11.8% of patients who received placebo. The primary reason for discontinuation in the placebo arm was progressive disease or relapse—45%, compared to 4.8% in the ibrutinib arm.
Taken together, the results of this trial suggest treatment with ibrutinib and BR is superior to standard BR therapy in patients with relapsed CLL/SLL, Dr Chanan-Kahn said.
“This was one of the most rigorous clinical trials ever conducted in CLL,” he said, “and it truly validates ibrutinib as an important drug for this cancer.” ![]()
Hodgkin lymphoma incidence on the decline worldwide

Photo courtesy of NIH
In trying to estimate the global cancer burden, researchers found that cases of Hodgkin lymphoma (HL) have decreased worldwide over the last 2 decades.
The team studied 28 cancer types in 188 countries, and HL was the only malignancy whose incidence decreased from 1990 to 2013.
And the number of HL deaths in 2013 was comparatively low. When the researchers ranked cancers according to the number of global deaths, HL was 26th on the list of 28.
The researchers disclosed these results in JAMA Oncology.
The team collected data from cancer registries, vital records, verbal autopsy reports, and other sources to estimate the global cancer burden.
The data suggested that, in 2013, there were 14.9 million new cancer cases and 8.2 million cancer deaths worldwide. The proportion of cancer deaths as part of all deaths increased from 12% in 1990 to 15% in 2013.
The most common malignancy in men was prostate cancer, with 1.4 million cases in 2013. For women, it was breast cancer, with 1.8 million cases in 2013.
Tracheal, bronchus, and lung cancers were the leading cause of cancer death in men and women, with 1.6 million deaths in 2013.
Hematologic malignancies
Globally, the age-standardized incidence of HL per 100,000 people decreased by 34% during the time period studied. Cases of HL fell from about 103,000 in 1990 to 93,000 in 2013.
When the researchers ranked cancer types according to the number of global deaths in 2013, HL came in 26th. There were about 24,000 HL deaths in 2013—14,000 among men and 10,000 among women.
Non-Hodgkin lymphoma (NHL) came in 11th for global cancer deaths in 2013. There were about 226,000 NHL deaths—133,000 among men and 92,000 among women.
In addition, the incidence of NHL more than doubled from 1990 to 2013, rising from about 227,000 to 465,000. According to 2013 data, 1 in 103 men and 1 in 151 women developed NHL between birth and 79 years of age.
The researchers observed an increase in cases of multiple myeloma (MM) as well, from about 63,000 in 1990 to 117,000 in 2013.
In 2013, there were about 79,000 MM deaths—42,000 among men and 37,000 among women. MM ranked 19th on the list of global cancer deaths in 2013.
Leukemia ranked 9th on the list. There were about 265,000 leukemia deaths in 2013—149,000 among men and 116,000 among women.
Cases of leukemia increased from 297,000 in 1990 to 414,000 in 2013. According to 2013 data, 1 in 127 men and 1 in 203 women developed leukemia between birth and 79 years of age.
This research shows that cancer remains a major threat to people’s health around the world, said study author Christina Fitzmaurice, MD, of the University of Washington in Seattle.
“Cancer prevention, screening, and treatment programs are costly,” she noted, “and it is very important for countries to know which cancers cause the highest disease burden in order to allocate scarce resources appropriately.” ![]()

Photo courtesy of NIH
In trying to estimate the global cancer burden, researchers found that cases of Hodgkin lymphoma (HL) have decreased worldwide over the last 2 decades.
The team studied 28 cancer types in 188 countries, and HL was the only malignancy whose incidence decreased from 1990 to 2013.
And the number of HL deaths in 2013 was comparatively low. When the researchers ranked cancers according to the number of global deaths, HL was 26th on the list of 28.
The researchers disclosed these results in JAMA Oncology.
The team collected data from cancer registries, vital records, verbal autopsy reports, and other sources to estimate the global cancer burden.
The data suggested that, in 2013, there were 14.9 million new cancer cases and 8.2 million cancer deaths worldwide. The proportion of cancer deaths as part of all deaths increased from 12% in 1990 to 15% in 2013.
The most common malignancy in men was prostate cancer, with 1.4 million cases in 2013. For women, it was breast cancer, with 1.8 million cases in 2013.
Tracheal, bronchus, and lung cancers were the leading cause of cancer death in men and women, with 1.6 million deaths in 2013.
Hematologic malignancies
Globally, the age-standardized incidence of HL per 100,000 people decreased by 34% during the time period studied. Cases of HL fell from about 103,000 in 1990 to 93,000 in 2013.
When the researchers ranked cancer types according to the number of global deaths in 2013, HL came in 26th. There were about 24,000 HL deaths in 2013—14,000 among men and 10,000 among women.
Non-Hodgkin lymphoma (NHL) came in 11th for global cancer deaths in 2013. There were about 226,000 NHL deaths—133,000 among men and 92,000 among women.
In addition, the incidence of NHL more than doubled from 1990 to 2013, rising from about 227,000 to 465,000. According to 2013 data, 1 in 103 men and 1 in 151 women developed NHL between birth and 79 years of age.
The researchers observed an increase in cases of multiple myeloma (MM) as well, from about 63,000 in 1990 to 117,000 in 2013.
In 2013, there were about 79,000 MM deaths—42,000 among men and 37,000 among women. MM ranked 19th on the list of global cancer deaths in 2013.
Leukemia ranked 9th on the list. There were about 265,000 leukemia deaths in 2013—149,000 among men and 116,000 among women.
Cases of leukemia increased from 297,000 in 1990 to 414,000 in 2013. According to 2013 data, 1 in 127 men and 1 in 203 women developed leukemia between birth and 79 years of age.
This research shows that cancer remains a major threat to people’s health around the world, said study author Christina Fitzmaurice, MD, of the University of Washington in Seattle.
“Cancer prevention, screening, and treatment programs are costly,” she noted, “and it is very important for countries to know which cancers cause the highest disease burden in order to allocate scarce resources appropriately.” ![]()

Photo courtesy of NIH
In trying to estimate the global cancer burden, researchers found that cases of Hodgkin lymphoma (HL) have decreased worldwide over the last 2 decades.
The team studied 28 cancer types in 188 countries, and HL was the only malignancy whose incidence decreased from 1990 to 2013.
And the number of HL deaths in 2013 was comparatively low. When the researchers ranked cancers according to the number of global deaths, HL was 26th on the list of 28.
The researchers disclosed these results in JAMA Oncology.
The team collected data from cancer registries, vital records, verbal autopsy reports, and other sources to estimate the global cancer burden.
The data suggested that, in 2013, there were 14.9 million new cancer cases and 8.2 million cancer deaths worldwide. The proportion of cancer deaths as part of all deaths increased from 12% in 1990 to 15% in 2013.
The most common malignancy in men was prostate cancer, with 1.4 million cases in 2013. For women, it was breast cancer, with 1.8 million cases in 2013.
Tracheal, bronchus, and lung cancers were the leading cause of cancer death in men and women, with 1.6 million deaths in 2013.
Hematologic malignancies
Globally, the age-standardized incidence of HL per 100,000 people decreased by 34% during the time period studied. Cases of HL fell from about 103,000 in 1990 to 93,000 in 2013.
When the researchers ranked cancer types according to the number of global deaths in 2013, HL came in 26th. There were about 24,000 HL deaths in 2013—14,000 among men and 10,000 among women.
Non-Hodgkin lymphoma (NHL) came in 11th for global cancer deaths in 2013. There were about 226,000 NHL deaths—133,000 among men and 92,000 among women.
In addition, the incidence of NHL more than doubled from 1990 to 2013, rising from about 227,000 to 465,000. According to 2013 data, 1 in 103 men and 1 in 151 women developed NHL between birth and 79 years of age.
The researchers observed an increase in cases of multiple myeloma (MM) as well, from about 63,000 in 1990 to 117,000 in 2013.
In 2013, there were about 79,000 MM deaths—42,000 among men and 37,000 among women. MM ranked 19th on the list of global cancer deaths in 2013.
Leukemia ranked 9th on the list. There were about 265,000 leukemia deaths in 2013—149,000 among men and 116,000 among women.
Cases of leukemia increased from 297,000 in 1990 to 414,000 in 2013. According to 2013 data, 1 in 127 men and 1 in 203 women developed leukemia between birth and 79 years of age.
This research shows that cancer remains a major threat to people’s health around the world, said study author Christina Fitzmaurice, MD, of the University of Washington in Seattle.
“Cancer prevention, screening, and treatment programs are costly,” she noted, “and it is very important for countries to know which cancers cause the highest disease burden in order to allocate scarce resources appropriately.” ![]()
Inhibitor promotes chemosensitization in CLL

PHILADELPHIA—A DNA-dependent protein kinase (DNA-PK) inhibitor can sensitize chronic lymphocytic leukemia (CLL) cells to chemotherapy, according to
preclinical research.
The inhibitor, NDD0004, sensitized CLL cells—even those from patients with high-risk cytogenetics—to treatment with mitoxantrone.
However, not all CLL samples were sensitive to treatment, so researchers are now trying to determine which patients might derive benefit from DNA-PK inhibitors.
Gesa Junge, a PhD student at Newcastle University in the UK, and her colleagues conducted this research and presented the results at the AACR Annual Meeting 2015 (abstract 3624*). The work was supported by AstraZeneca.
The researchers’ goal was to validate that DNA-PK inhibition is a valid approach to chemosensitization in CLL. So the team tested NU7441—a compound that inhibits DNA-PK and PI3 kinase—and NDD0004—a more selective DNA-PK inhibitor.
The team isolated CLL cells from patients’ peripheral blood, cultured the cells, and treated them with mitoxantrone and/or 1μM of NDD0004 or 1μM of NU7441.
Junge and her colleagues found that NDD0004 sensitized cells to mitoxantrone more effectively than NU7441. Sensitization was 202-fold higher with NDD004 plus mitoxantrone than with mitoxantrone alone and 69-fold higher with NU7441 plus mitoxantrone than with mitoxantrone alone (P=0.02).
However, sensitization varied between CLL samples, and the researchers have yet to determine why. Their experiments showed that variability was not a result of DNA-PK levels.
Still, the team found that CLL cells from patients with poor prognostic markers were sensitive to DNA-PK inhibition.
Sensitization with NU7441 plus mitoxantrone was 69-fold higher than mitoxantrone alone in CLL samples with del(13q), 25-fold higher in samples with del(11q), 12-fold higher in samples with TP53 mutation, and 16-fold higher in samples with ATM dysfunction.
Sensitization with NDD0004 plus mitoxantrone was 201-fold higher than mitoxantrone alone in CLL samples with del(13q), 314-fold higher in samples with del(11q), 27-fold higher in samples with TP53 mutation, and 18-fold higher in samples with ATM dysfunction.
To confirm that sensitization was a result of DNA-PK inhibition, Junge and her colleagues tested NDD0004 in an isogenic pair of DNA-PK-deficient and DNA-PK-proficient HCT116 cells. They found that HCT116 cells lacking DNA-PK were not sensitive to NDD0004, but cells with DNA-PK were sensitive.
The researchers also investigated the mechanism of NDD0004. Their results suggest the drug works by inhibiting the repair of DNA double-strand breaks.
“What we think is happening is that we are inducing DNA damage with mitoxantrone, and that gets repaired by 24 hours,” Junge said. “But if the DNA-PK inhibitor is there, the damage persists, and that seems to translate quite nicely into an apoptosis response.”
To further this research, Junge and her colleagues are hoping to identify biomarkers that can help them determine which CLL patients are likely to respond to DNA-PK inhibitors. ![]()
*Information in the abstract differs from that presented at the meeting.

PHILADELPHIA—A DNA-dependent protein kinase (DNA-PK) inhibitor can sensitize chronic lymphocytic leukemia (CLL) cells to chemotherapy, according to
preclinical research.
The inhibitor, NDD0004, sensitized CLL cells—even those from patients with high-risk cytogenetics—to treatment with mitoxantrone.
However, not all CLL samples were sensitive to treatment, so researchers are now trying to determine which patients might derive benefit from DNA-PK inhibitors.
Gesa Junge, a PhD student at Newcastle University in the UK, and her colleagues conducted this research and presented the results at the AACR Annual Meeting 2015 (abstract 3624*). The work was supported by AstraZeneca.
The researchers’ goal was to validate that DNA-PK inhibition is a valid approach to chemosensitization in CLL. So the team tested NU7441—a compound that inhibits DNA-PK and PI3 kinase—and NDD0004—a more selective DNA-PK inhibitor.
The team isolated CLL cells from patients’ peripheral blood, cultured the cells, and treated them with mitoxantrone and/or 1μM of NDD0004 or 1μM of NU7441.
Junge and her colleagues found that NDD0004 sensitized cells to mitoxantrone more effectively than NU7441. Sensitization was 202-fold higher with NDD004 plus mitoxantrone than with mitoxantrone alone and 69-fold higher with NU7441 plus mitoxantrone than with mitoxantrone alone (P=0.02).
However, sensitization varied between CLL samples, and the researchers have yet to determine why. Their experiments showed that variability was not a result of DNA-PK levels.
Still, the team found that CLL cells from patients with poor prognostic markers were sensitive to DNA-PK inhibition.
Sensitization with NU7441 plus mitoxantrone was 69-fold higher than mitoxantrone alone in CLL samples with del(13q), 25-fold higher in samples with del(11q), 12-fold higher in samples with TP53 mutation, and 16-fold higher in samples with ATM dysfunction.
Sensitization with NDD0004 plus mitoxantrone was 201-fold higher than mitoxantrone alone in CLL samples with del(13q), 314-fold higher in samples with del(11q), 27-fold higher in samples with TP53 mutation, and 18-fold higher in samples with ATM dysfunction.
To confirm that sensitization was a result of DNA-PK inhibition, Junge and her colleagues tested NDD0004 in an isogenic pair of DNA-PK-deficient and DNA-PK-proficient HCT116 cells. They found that HCT116 cells lacking DNA-PK were not sensitive to NDD0004, but cells with DNA-PK were sensitive.
The researchers also investigated the mechanism of NDD0004. Their results suggest the drug works by inhibiting the repair of DNA double-strand breaks.
“What we think is happening is that we are inducing DNA damage with mitoxantrone, and that gets repaired by 24 hours,” Junge said. “But if the DNA-PK inhibitor is there, the damage persists, and that seems to translate quite nicely into an apoptosis response.”
To further this research, Junge and her colleagues are hoping to identify biomarkers that can help them determine which CLL patients are likely to respond to DNA-PK inhibitors. ![]()
*Information in the abstract differs from that presented at the meeting.

PHILADELPHIA—A DNA-dependent protein kinase (DNA-PK) inhibitor can sensitize chronic lymphocytic leukemia (CLL) cells to chemotherapy, according to
preclinical research.
The inhibitor, NDD0004, sensitized CLL cells—even those from patients with high-risk cytogenetics—to treatment with mitoxantrone.
However, not all CLL samples were sensitive to treatment, so researchers are now trying to determine which patients might derive benefit from DNA-PK inhibitors.
Gesa Junge, a PhD student at Newcastle University in the UK, and her colleagues conducted this research and presented the results at the AACR Annual Meeting 2015 (abstract 3624*). The work was supported by AstraZeneca.
The researchers’ goal was to validate that DNA-PK inhibition is a valid approach to chemosensitization in CLL. So the team tested NU7441—a compound that inhibits DNA-PK and PI3 kinase—and NDD0004—a more selective DNA-PK inhibitor.
The team isolated CLL cells from patients’ peripheral blood, cultured the cells, and treated them with mitoxantrone and/or 1μM of NDD0004 or 1μM of NU7441.
Junge and her colleagues found that NDD0004 sensitized cells to mitoxantrone more effectively than NU7441. Sensitization was 202-fold higher with NDD004 plus mitoxantrone than with mitoxantrone alone and 69-fold higher with NU7441 plus mitoxantrone than with mitoxantrone alone (P=0.02).
However, sensitization varied between CLL samples, and the researchers have yet to determine why. Their experiments showed that variability was not a result of DNA-PK levels.
Still, the team found that CLL cells from patients with poor prognostic markers were sensitive to DNA-PK inhibition.
Sensitization with NU7441 plus mitoxantrone was 69-fold higher than mitoxantrone alone in CLL samples with del(13q), 25-fold higher in samples with del(11q), 12-fold higher in samples with TP53 mutation, and 16-fold higher in samples with ATM dysfunction.
Sensitization with NDD0004 plus mitoxantrone was 201-fold higher than mitoxantrone alone in CLL samples with del(13q), 314-fold higher in samples with del(11q), 27-fold higher in samples with TP53 mutation, and 18-fold higher in samples with ATM dysfunction.
To confirm that sensitization was a result of DNA-PK inhibition, Junge and her colleagues tested NDD0004 in an isogenic pair of DNA-PK-deficient and DNA-PK-proficient HCT116 cells. They found that HCT116 cells lacking DNA-PK were not sensitive to NDD0004, but cells with DNA-PK were sensitive.
The researchers also investigated the mechanism of NDD0004. Their results suggest the drug works by inhibiting the repair of DNA double-strand breaks.
“What we think is happening is that we are inducing DNA damage with mitoxantrone, and that gets repaired by 24 hours,” Junge said. “But if the DNA-PK inhibitor is there, the damage persists, and that seems to translate quite nicely into an apoptosis response.”
To further this research, Junge and her colleagues are hoping to identify biomarkers that can help them determine which CLL patients are likely to respond to DNA-PK inhibitors.
*Information in the abstract differs from that presented at the meeting.
Combo targets AML, BL in the same way

Image by Ed Uthman
Combining a cholesterol-lowering drug and a contraceptive steroid could be a safe, effective treatment for leukemias, lymphomas, and other malignancies, according to researchers.
Their work helps explain how this combination treatment, bezafibrate and medroxyprogesterone acetate (BaP), kills cancer cells.
The team discovered that BaP’s mechanism of action is the same in acute myeloid leukemia (AML) and Burkitt lymphoma (BL) cells.
The findings have been published in Cancer Research.
BaP has been shown to prolong survival in early stage trials of elderly AML patients, when compared to standard palliative care. BaP has also been used alongside chemotherapy to successfully treat children with BL.
However, it was unclear whether BaP’s activity against these 2 very different malignancies was mediated by a common mechanism or by different effects in each cancer.
To gain some insight, Andrew Southam, PhD, of the University of Birmingham in the UK, and his colleagues investigated the drugs’ effects on the metabolism and chemical make-up of AML and BL cells.
They found that, in both cell types, BaP blocks stearoyl CoA desaturase, an enzyme crucial to the production of fatty acids, which cancer cells need to grow and multiply. The team also showed that BaP’s ability to deactivate stearoyl CoA desaturase was what prompted the cancer cells to die.
“Developing drugs to target the fatty-acid building blocks of cancer cells has been a promising area of research in recent years,” Dr Southam said. “It is very exciting we have identified these non-toxic drugs already sitting on pharmacy shelves.”
He and his colleagues believe these findings also open up the possibility that BaP could be used to treat other cancers that rely on high levels of stearoyl CoA desaturase to grow, including chronic lymphocytic leukemia and some types of non-Hodgkin lymphoma, as well as prostate, colon, and esophageal cancers.
“This drug combination shows real promise,” said Chris Bunce, PhD, also of the University of Birmingham.
“Affordable, effective, non-toxic treatments that extend survival, while offering a good quality of life, are in demand for almost all types of cancer.”

Image by Ed Uthman
Combining a cholesterol-lowering drug and a contraceptive steroid could be a safe, effective treatment for leukemias, lymphomas, and other malignancies, according to researchers.
Their work helps explain how this combination treatment, bezafibrate and medroxyprogesterone acetate (BaP), kills cancer cells.
The team discovered that BaP’s mechanism of action is the same in acute myeloid leukemia (AML) and Burkitt lymphoma (BL) cells.
The findings have been published in Cancer Research.
BaP has been shown to prolong survival in early stage trials of elderly AML patients, when compared to standard palliative care. BaP has also been used alongside chemotherapy to successfully treat children with BL.
However, it was unclear whether BaP’s activity against these 2 very different malignancies was mediated by a common mechanism or by different effects in each cancer.
To gain some insight, Andrew Southam, PhD, of the University of Birmingham in the UK, and his colleagues investigated the drugs’ effects on the metabolism and chemical make-up of AML and BL cells.
They found that, in both cell types, BaP blocks stearoyl CoA desaturase, an enzyme crucial to the production of fatty acids, which cancer cells need to grow and multiply. The team also showed that BaP’s ability to deactivate stearoyl CoA desaturase was what prompted the cancer cells to die.
“Developing drugs to target the fatty-acid building blocks of cancer cells has been a promising area of research in recent years,” Dr Southam said. “It is very exciting we have identified these non-toxic drugs already sitting on pharmacy shelves.”
He and his colleagues believe these findings also open up the possibility that BaP could be used to treat other cancers that rely on high levels of stearoyl CoA desaturase to grow, including chronic lymphocytic leukemia and some types of non-Hodgkin lymphoma, as well as prostate, colon, and esophageal cancers.
“This drug combination shows real promise,” said Chris Bunce, PhD, also of the University of Birmingham.
“Affordable, effective, non-toxic treatments that extend survival, while offering a good quality of life, are in demand for almost all types of cancer.”

Image by Ed Uthman
Combining a cholesterol-lowering drug and a contraceptive steroid could be a safe, effective treatment for leukemias, lymphomas, and other malignancies, according to researchers.
Their work helps explain how this combination treatment, bezafibrate and medroxyprogesterone acetate (BaP), kills cancer cells.
The team discovered that BaP’s mechanism of action is the same in acute myeloid leukemia (AML) and Burkitt lymphoma (BL) cells.
The findings have been published in Cancer Research.
BaP has been shown to prolong survival in early stage trials of elderly AML patients, when compared to standard palliative care. BaP has also been used alongside chemotherapy to successfully treat children with BL.
However, it was unclear whether BaP’s activity against these 2 very different malignancies was mediated by a common mechanism or by different effects in each cancer.
To gain some insight, Andrew Southam, PhD, of the University of Birmingham in the UK, and his colleagues investigated the drugs’ effects on the metabolism and chemical make-up of AML and BL cells.
They found that, in both cell types, BaP blocks stearoyl CoA desaturase, an enzyme crucial to the production of fatty acids, which cancer cells need to grow and multiply. The team also showed that BaP’s ability to deactivate stearoyl CoA desaturase was what prompted the cancer cells to die.
“Developing drugs to target the fatty-acid building blocks of cancer cells has been a promising area of research in recent years,” Dr Southam said. “It is very exciting we have identified these non-toxic drugs already sitting on pharmacy shelves.”
He and his colleagues believe these findings also open up the possibility that BaP could be used to treat other cancers that rely on high levels of stearoyl CoA desaturase to grow, including chronic lymphocytic leukemia and some types of non-Hodgkin lymphoma, as well as prostate, colon, and esophageal cancers.
“This drug combination shows real promise,” said Chris Bunce, PhD, also of the University of Birmingham.
“Affordable, effective, non-toxic treatments that extend survival, while offering a good quality of life, are in demand for almost all types of cancer.”
Company stops phase 3 PTCL trial

for use in a clinical trial
Photo by Esther Dyson
Takeda Pharmaceutical Company Limited has announced its decision to discontinue its phase 3 trial of the aurora A kinase inhibitor alisertib (MLN8237) in patients with relapsed or refractory peripheral T-cell lymphoma (PTCL).
Results of a pre-specified interim analysis indicated that alisertib was unlikely to meet the study’s primary endpoint: providing superior progression-free survival over the standard of care for PTCL.
Takeda said patients enrolled in the trial may continue to receive alisertib if they are thought to be benefitting from it and no safety concerns are present.
The company is encouraging patients to consult their study investigators to address any questions and before making any changes to their medication.
Takeda is working with trial investigators and local regulatory authorities to ensure that PTCL patients who participated in the study receive appropriate care.
The company is still investigating alisertib for use in small-cell lung cancer.
“While we are disappointed that alisertib will not be further investigated for relapsed or refractory peripheral T-cell lymphoma, we are optimistic about alisertib’s clinical development program in small-cell lung cancer,” said Michael Vasconcelles, MD, global head of the Takeda Oncology Therapeutic Unit.
“The randomized, phase 2 study of alisertib in small-cell lung cancer will continue as planned and is currently underway. Takeda also continues to support investigator-initiated research with alisertib and will evaluate its potential use in other oncology indications going forward.”

for use in a clinical trial
Photo by Esther Dyson
Takeda Pharmaceutical Company Limited has announced its decision to discontinue its phase 3 trial of the aurora A kinase inhibitor alisertib (MLN8237) in patients with relapsed or refractory peripheral T-cell lymphoma (PTCL).
Results of a pre-specified interim analysis indicated that alisertib was unlikely to meet the study’s primary endpoint: providing superior progression-free survival over the standard of care for PTCL.
Takeda said patients enrolled in the trial may continue to receive alisertib if they are thought to be benefitting from it and no safety concerns are present.
The company is encouraging patients to consult their study investigators to address any questions and before making any changes to their medication.
Takeda is working with trial investigators and local regulatory authorities to ensure that PTCL patients who participated in the study receive appropriate care.
The company is still investigating alisertib for use in small-cell lung cancer.
“While we are disappointed that alisertib will not be further investigated for relapsed or refractory peripheral T-cell lymphoma, we are optimistic about alisertib’s clinical development program in small-cell lung cancer,” said Michael Vasconcelles, MD, global head of the Takeda Oncology Therapeutic Unit.
“The randomized, phase 2 study of alisertib in small-cell lung cancer will continue as planned and is currently underway. Takeda also continues to support investigator-initiated research with alisertib and will evaluate its potential use in other oncology indications going forward.”

for use in a clinical trial
Photo by Esther Dyson
Takeda Pharmaceutical Company Limited has announced its decision to discontinue its phase 3 trial of the aurora A kinase inhibitor alisertib (MLN8237) in patients with relapsed or refractory peripheral T-cell lymphoma (PTCL).
Results of a pre-specified interim analysis indicated that alisertib was unlikely to meet the study’s primary endpoint: providing superior progression-free survival over the standard of care for PTCL.
Takeda said patients enrolled in the trial may continue to receive alisertib if they are thought to be benefitting from it and no safety concerns are present.
The company is encouraging patients to consult their study investigators to address any questions and before making any changes to their medication.
Takeda is working with trial investigators and local regulatory authorities to ensure that PTCL patients who participated in the study receive appropriate care.
The company is still investigating alisertib for use in small-cell lung cancer.
“While we are disappointed that alisertib will not be further investigated for relapsed or refractory peripheral T-cell lymphoma, we are optimistic about alisertib’s clinical development program in small-cell lung cancer,” said Michael Vasconcelles, MD, global head of the Takeda Oncology Therapeutic Unit.
“The randomized, phase 2 study of alisertib in small-cell lung cancer will continue as planned and is currently underway. Takeda also continues to support investigator-initiated research with alisertib and will evaluate its potential use in other oncology indications going forward.”