User login
Quality Improvement Project Helps Hospital Patients Get Needed Prescriptions
A quality-improvement (QI) project to give high-risk patients ready access to prescribed medications at the time of hospital discharge achieved an 86% success rate, according to an abstract poster presented at HM12 in San Diego last April.1
Lead author Elizabeth Le, MD, then a resident at the University of California at San Francisco Medical Center (UCSF) and now a practicing hospitalist at the Veterans Administration Medical Center in Palo Alto, Calif., says the multidisciplinary “brown bag medications” project involved training house staff to recognize patients at risk. Staff meetings and rounds were used to identify appropriate candidates—those with limited mobility or cognitive issues, lacking insurance coverage or financial resources, a history of medication noncompliance, or leaving the hospital against medical advice—as well as those prescribed medications with a greater urgency for administration on schedule, such as anticoagulants or antibiotics.
About one-quarter of patients on the unit where this approach was first tested were found to need the service, which involved faxing prescriptions to an outpatient pharmacy across the street from the hospital for either pick-up by the family or delivery to the patient’s hospital room. For those with financial impediments, hospital social workers and case managers explored other options, including the social work department’s discretionary use fund, to pay for the drugs.
Dr. Le believes the project could be replicated in other facilities that lack access to in-house pharmacy services at discharge. She recommends involving social workers and case managers in the planning.
At UCSF, recent EHR implementation has automated the ordering of medications, but the challenge of recognizing who could benefit from extra help in obtaining their discharge medications remains a critical issue for hospitals trying to bring readmissions under control.
For more information about the brown bag medications program, contact Dr. Le at Elizabeth.Le@va.gov.
References
A quality-improvement (QI) project to give high-risk patients ready access to prescribed medications at the time of hospital discharge achieved an 86% success rate, according to an abstract poster presented at HM12 in San Diego last April.1
Lead author Elizabeth Le, MD, then a resident at the University of California at San Francisco Medical Center (UCSF) and now a practicing hospitalist at the Veterans Administration Medical Center in Palo Alto, Calif., says the multidisciplinary “brown bag medications” project involved training house staff to recognize patients at risk. Staff meetings and rounds were used to identify appropriate candidates—those with limited mobility or cognitive issues, lacking insurance coverage or financial resources, a history of medication noncompliance, or leaving the hospital against medical advice—as well as those prescribed medications with a greater urgency for administration on schedule, such as anticoagulants or antibiotics.
About one-quarter of patients on the unit where this approach was first tested were found to need the service, which involved faxing prescriptions to an outpatient pharmacy across the street from the hospital for either pick-up by the family or delivery to the patient’s hospital room. For those with financial impediments, hospital social workers and case managers explored other options, including the social work department’s discretionary use fund, to pay for the drugs.
Dr. Le believes the project could be replicated in other facilities that lack access to in-house pharmacy services at discharge. She recommends involving social workers and case managers in the planning.
At UCSF, recent EHR implementation has automated the ordering of medications, but the challenge of recognizing who could benefit from extra help in obtaining their discharge medications remains a critical issue for hospitals trying to bring readmissions under control.
For more information about the brown bag medications program, contact Dr. Le at Elizabeth.Le@va.gov.
References
A quality-improvement (QI) project to give high-risk patients ready access to prescribed medications at the time of hospital discharge achieved an 86% success rate, according to an abstract poster presented at HM12 in San Diego last April.1
Lead author Elizabeth Le, MD, then a resident at the University of California at San Francisco Medical Center (UCSF) and now a practicing hospitalist at the Veterans Administration Medical Center in Palo Alto, Calif., says the multidisciplinary “brown bag medications” project involved training house staff to recognize patients at risk. Staff meetings and rounds were used to identify appropriate candidates—those with limited mobility or cognitive issues, lacking insurance coverage or financial resources, a history of medication noncompliance, or leaving the hospital against medical advice—as well as those prescribed medications with a greater urgency for administration on schedule, such as anticoagulants or antibiotics.
About one-quarter of patients on the unit where this approach was first tested were found to need the service, which involved faxing prescriptions to an outpatient pharmacy across the street from the hospital for either pick-up by the family or delivery to the patient’s hospital room. For those with financial impediments, hospital social workers and case managers explored other options, including the social work department’s discretionary use fund, to pay for the drugs.
Dr. Le believes the project could be replicated in other facilities that lack access to in-house pharmacy services at discharge. She recommends involving social workers and case managers in the planning.
At UCSF, recent EHR implementation has automated the ordering of medications, but the challenge of recognizing who could benefit from extra help in obtaining their discharge medications remains a critical issue for hospitals trying to bring readmissions under control.
For more information about the brown bag medications program, contact Dr. Le at Elizabeth.Le@va.gov.
References
Bloodsteam Infections in ICU Patients Plummet
Reduction in bloodstream infection rates resulting from a simple intervention: bathing all ICU patients daily with antimicrobial chlorhexidine soap rather than the widely mandated practice of screening ICU patients to determine which ones harbor methicillin-resistant Staphylococcus aureus (MRSA) and then implementing an MRSA treatment protocol for them.
According to data on 75,000 patients at hospitals in 16 states presented in October at the Infectious Diseases Society of America annual meeting, there also was a 37% reduction in patients with MRSA.
Lead researcher Susan Huang, MD, an infectious-disease specialist at the University of California at Irvine, says the results show the benefits of this preventive approach, which included applying an antibiotic ointment to the patient’s nasal passage, and could make ICU screening for drug-resistant organisms, such as MRSA, unnecessary.
Reduction in bloodstream infection rates resulting from a simple intervention: bathing all ICU patients daily with antimicrobial chlorhexidine soap rather than the widely mandated practice of screening ICU patients to determine which ones harbor methicillin-resistant Staphylococcus aureus (MRSA) and then implementing an MRSA treatment protocol for them.
According to data on 75,000 patients at hospitals in 16 states presented in October at the Infectious Diseases Society of America annual meeting, there also was a 37% reduction in patients with MRSA.
Lead researcher Susan Huang, MD, an infectious-disease specialist at the University of California at Irvine, says the results show the benefits of this preventive approach, which included applying an antibiotic ointment to the patient’s nasal passage, and could make ICU screening for drug-resistant organisms, such as MRSA, unnecessary.
Reduction in bloodstream infection rates resulting from a simple intervention: bathing all ICU patients daily with antimicrobial chlorhexidine soap rather than the widely mandated practice of screening ICU patients to determine which ones harbor methicillin-resistant Staphylococcus aureus (MRSA) and then implementing an MRSA treatment protocol for them.
According to data on 75,000 patients at hospitals in 16 states presented in October at the Infectious Diseases Society of America annual meeting, there also was a 37% reduction in patients with MRSA.
Lead researcher Susan Huang, MD, an infectious-disease specialist at the University of California at Irvine, says the results show the benefits of this preventive approach, which included applying an antibiotic ointment to the patient’s nasal passage, and could make ICU screening for drug-resistant organisms, such as MRSA, unnecessary.
Accountability Hits Home for Hospitalists
Russell Cowles III, MD, lead hospitalist at Bergan Mercy Medical Center in Omaha, Neb., recalls the shock on the faces of hospitalists who attended his presentation to SHM’s Nebraska Area chapter meeting last spring. Dr. Cowles and co-presenter Eric Rice, MD, MMM, SFHM, chapter president and assistant medical director of Alegent Creighton Hospital Medicine Services, were introducing their fellow hospitalists to a forthcoming Medicare initiative called the Physician Feedback/Value-Based Payment Modifier (VBPM) program.
“And everyone in the audience was completely stunned,” Dr. Cowles says. “They had never even dreamed that any of this would come down to the physician level.”
They’re not alone.
“Unless you work in administration or you’re leading a group, I don’t think very many people know this exists,” Dr. Cowles says. “Your average practicing physician, I think, has no clue that this measurement is going on behind the scenes.”
Authorized by the Affordable Care Act, the budget-neutral scheme ties future Medicare reimbursements to measures of quality and efficiency, and grades physicians on a curve. The Physician Quality Reporting System (PQRS), in place since 2007, forms the foundation of the new program, with feedback arriving in the form of a Quality and Resource Use Report (QRUR), a confidential report card sent to providers. The VBPM program then uses those reports as the basis for a financial reward or penalty.
In principle, SHM and hospitalist leaders have supported the concept of quality measurements as a way to hold doctors more accountable and to help the Centers for Medicare & Medicaid Services (CMS) take a more proactive role in improving quality of care while containing costs. And, in theory, HM leaders say hospitalists might be better able to adapt to the added responsibility of performance measurement and reporting due to their central role in the like-minded hospital value-based purchasing (VBP) program that began Oct. 1.
“If the expectation is that we will be involved in some of these initiatives and help the hospitals gain revenue, now we can actually see some dollars for those efforts,” says Julia Wright, MD, SFHM, FACP, president of the MidAtlantic Business Unit for Brentwood, Tenn.-based Cogent HMG. But the inverse is also true: If hospitals are going to have dollars at risk for performance, she says, CMS believes physicians should share in that risk as the providers of healthcare.
On that score, Dr. Rice says, hospitalists might have an advantage due to their focus on teamwork and their role in transitioning patients between inpatient and outpatient settings. In fact, he sees the VBPM as an “enormous opportunity” for hospitalists to demonstrate their leadership in helping to shape how organizations and institutions adapt to a quickly evolving healthcare environment.
But first, hospitalists will need to fully engage. In 2010, CMS found that only about 1 in 4 eligible physicians were participating in the voluntary PQRS and earning a reporting bonus of what is now 0.5% of allowable Medicare charges (roughly $800 for the average hospitalist). The stakes will grow when the PQRS transforms into a negative incentive program in 2015, with a 1.5% penalty for doctors who do not meet its reporting requirements. In 2016 and thereafter, the assessed penalty grows to 2% (about $3,200 for the average hospitalist).
“I think the unfolding timeline has really provided the potential for lulling us into complacency and procrastination,” says Patrick Torcson, MD, MMM, FACP, SFHM, director of hospital medicine at St. Tammany Parish Hospital in Covington, La., and chair of SHM’s Performance Measurement and Reporting Committee.
According to CMS, “physician groups can avoid all negative adjustments simply by participating in the PQRS.” Nonparticipants, however, could get hit with a double whammy. With no quality data, CMS would have no way to assess groups’ performances and would automatically deduct an extra 1% of Medicare reimbursements under the VBPM program. For groups of 100 eligible providers or more, that combined PQRS-VBPM penalty could amount to 2.5% in 2015.
PQRS participants have more leeway and a smaller downside. Starting January 2015, eligible provider groups who meet the reporting requirements can choose either to have no adjustments at all or to compete in the VBPM program for a performance-based bonus or a penalty of 1%, based on cost and quality scores. In January 2017, the program is expected to expand to include all providers, whether in individual or group practice.
A Measure of Relevance
Based on the first QRURs, sent out in March 2012 to providers in four pilot states, SHM wrote a letter to CMS that offered a detailed analysis of several additional concerns. The society followed up with a second letter that provided a more expansive critique of the proposed 2013 Physician Fee Schedule.
One worry is whether the physician feedback/VBPM program has included enough performance measures that are relevant to hospitalists. A Public Policy column in The Hospitalist (“Metric Accountability,” November 2012, p. 18) counted only 10 PQRS measures that apply routinely to HM providers out of a list of more than 200. Even those 10 aren’t always applicable.
“I work at a teaching hospital that’s large enough to have a neurology program, so most acute-stroke patients are admitted by the neurologists,” says Gregory Seymann, MD, SFHM, chief of the division of hospital medicine at the University of California at San Diego and a member of SHM’s Performance Measurement and Reporting Committee. “Five of the 10 measures are related to stroke patients, but my group rarely admits stroke patients.” That means only five PQRS measures remain relevant to him.
On paper, the issue might be readily resolved by expanding the number of measures to better reflect HM responsibilities—such as four measures proposed by SHM that relate to transitions of care and medication reconciliation.

—Patrick Torcson, MD, MMM, FACP, SFHM, director, hospital medicine, St. Tammany Parish Hospital, Covington, La., chair, SHM’s Performance Measurement and Reporting Committee
Other groups, though, have their own ideas. A letter to CMS signed by 28 patient and healthcare payor groups calls for the elimination of almost two dozen PQRS measures deemed unnecessary, duplicative, or uninformative, and for the addition of nine others that might better assess patient outcomes and quality of care. Jennifer Eames Huff, director of the Consumer-Purchaser Disclosure Project at San Francisco-based Pacific Business Group on Health, one of the letter’s signatories, says some of those potential measures might be more applicable to hospitalists as well.
But therein lies the rub. Although process measures might not always be strong indicators of quality of care, the introduction of outcome measures often makes providers nervous, says Gary Young, JD, PhD, director of the Center for Health Policy and Healthcare Research at Northeastern University in Boston. “Most providers feel that their patients are sicker and more vulnerable to poorer outcomes, and they don’t want to be judged poorly because they have sicker patients,” he says. Reaching an agreement on the best collection of measures may require some intense negotiations, he says.

–Win Whitcomb, MD, MHM, medical director of healthcare quality, Baystate Medical Center, Springfield, Mass.
Fairer Comparisons
Dr. Cowles cites two de-identified QRURs received by Alegent Creighton Health back in March—one for a hospitalist and one for an office-based general internist—to illustrate another major concern shared by many HM providers. The reports broke down each doctor’s relative healthcare contributions, using predetermined percentages of the total care and costs to conclude whether that doctor directed, influenced, or contributed to a patient’s care.
Hospitalists, by the nature of their jobs, seldom direct the care of any patient. But because their influence or contribution is almost always within the inpatient environment, HM providers account for proportionately higher costs than office-based physicians. The result can be a rather ugly curve: For healthcare costs incurred, the general internist was at the 65th percentile, while the hospitalist was at the 96th percentile.
The point, Dr. Cowles says, is that hospitalists and clinic-based physicians see patients with remarkably different acuities. “We just need to make sure that we’re comparing apples to apples, that you’re going to compare someone who sees a high-acuity patient with someone else who sees a high-acuity patient,” he says.
One silver lining could be increased momentum toward establishing HM as its own Medicare-recognized specialty. Hospitalist leaders who say the process is likely to be difficult but not impossible cite the successful effort to win recognition of HM as a focused practice by the American Board of Internal Medicine.
“We’re going to have to think outside the box in terms of working toward an identifier for hospitalists,” says Win Whitcomb, MD, MHM, medical director of healthcare quality at Baystate Medical Center in Springfield, Mass., and a member of SHM’s Performance and Measurement Reporting Committee. “But that’s going to happen—it’s not a matter of if, it’s a matter of when and how.”
As one potential interim solution, SHM has suggested a self-identification designation by which hospitalists would distinguish themselves from the larger, general internal-medicine category and thereby avoid unfair comparisons.
A Question of Attribution
Of the concerns raised by SHM, the question of attribution might be among the thorniest. Dr. Young says the “big-time issue” is pitting many consumer groups, payors, and employers against healthcare providers. The consumer groups want accountability at the individual provider level, while the providers strongly prefer group accountability, setting up a major clash over how responsibility will be parceled out.
Hospitalists have been taught to embrace responsibility while viewing healthcare delivery as a team sport. And the contributions of individual HM providers aren’t easily untangled. “If somebody has a bad outcome and they’ve been under the care of three different hospitalists, it’s virtually impossible to attribute that outcome to one of those three hospitalists,” Dr. Whitcomb says. “We really need to think about attribution differently, and it’s going to need to be across groups of hospitalists.”
SHM has suggested that CMS include an option for group rather than individual evaluation. “You’re just making it explicit that you can’t assign some of these measures to individual physicians. We can assign some of these measures to groups,” Dr. Whitcomb says.

—Julia Wright, MD, SFHM, FACP, president, MidAtlantic Business Unit, Cogent HMG, Brentwood, Tenn.
In its 2013 Medicare Physician Fee Schedule final rule, CMS opted to alter the doctor comparison methodology used for upcoming QRURs and the 2015 application of the VBPM. The agency also agreed to consider hospitalists’ concerns about fair attribution, relevant measures, and proper designation as it develops future proposals. Regardless of how those issues are ironed out, Dr. Torcson says, it’s clear to him that sitting on the sidelines is no longer an option for any physician group. Nor is it acceptable “to say this won’t work for me. We’re having to come up with proactive proposals for what will work to be part of the CMS quality agenda.”
SHM’s thorough analysis and realistic feedback, he says, has been well received by Medicare officials, raising hopes that many of the remaining differences can be resolved. “I am very confident that self-reporting or self-nomination as a hospitalist is going to be in place by the time those negative incentives kick in,” Dr. Torcson says. “And I’m also very confident that we’re going to have other, very creative options for quality measurement and performance reporting.”
One idea under consideration by CMS would allow hospitalists or other doctors to designate their hospitals’ quality data as a surrogate measure of their own performance. “I think that’s going to be a really great option for hospitalists who self-nominate,” Dr. Torcson says.
For many hospitalists, the option would effectively get around the issue of individual versus group attribution and instead align doctors’ fates with that of their institutions. SHM, Dr. Torcson says, has endorsed the proposal and offered to work with CMS to help institute it. He’s also confident that the reporting requirements for multiple, overlapping CMS programs will be more streamlined over time.
Some health professionals believe that hospitals and doctors already are devoting too much time and energy to measuring and recording the proliferating set of mandatory metrics. But Dr. Whitcomb says payors and patients are unlikely to have much sympathy.
“We as a profession are accountable to society at large. And that argument, that there are too many measurements and that we shouldn’t be held accountable as physicians for our performance, is a nonstarter when you’re trying to explain that to consumers,” he says. “The status quo is not tenable, and so it’s going to be a long journey and we need to be able to move in that direction.”
Bryn Nelson is a freelance medical writer in Seattle.
Russell Cowles III, MD, lead hospitalist at Bergan Mercy Medical Center in Omaha, Neb., recalls the shock on the faces of hospitalists who attended his presentation to SHM’s Nebraska Area chapter meeting last spring. Dr. Cowles and co-presenter Eric Rice, MD, MMM, SFHM, chapter president and assistant medical director of Alegent Creighton Hospital Medicine Services, were introducing their fellow hospitalists to a forthcoming Medicare initiative called the Physician Feedback/Value-Based Payment Modifier (VBPM) program.
“And everyone in the audience was completely stunned,” Dr. Cowles says. “They had never even dreamed that any of this would come down to the physician level.”
They’re not alone.
“Unless you work in administration or you’re leading a group, I don’t think very many people know this exists,” Dr. Cowles says. “Your average practicing physician, I think, has no clue that this measurement is going on behind the scenes.”
Authorized by the Affordable Care Act, the budget-neutral scheme ties future Medicare reimbursements to measures of quality and efficiency, and grades physicians on a curve. The Physician Quality Reporting System (PQRS), in place since 2007, forms the foundation of the new program, with feedback arriving in the form of a Quality and Resource Use Report (QRUR), a confidential report card sent to providers. The VBPM program then uses those reports as the basis for a financial reward or penalty.
In principle, SHM and hospitalist leaders have supported the concept of quality measurements as a way to hold doctors more accountable and to help the Centers for Medicare & Medicaid Services (CMS) take a more proactive role in improving quality of care while containing costs. And, in theory, HM leaders say hospitalists might be better able to adapt to the added responsibility of performance measurement and reporting due to their central role in the like-minded hospital value-based purchasing (VBP) program that began Oct. 1.
“If the expectation is that we will be involved in some of these initiatives and help the hospitals gain revenue, now we can actually see some dollars for those efforts,” says Julia Wright, MD, SFHM, FACP, president of the MidAtlantic Business Unit for Brentwood, Tenn.-based Cogent HMG. But the inverse is also true: If hospitals are going to have dollars at risk for performance, she says, CMS believes physicians should share in that risk as the providers of healthcare.
On that score, Dr. Rice says, hospitalists might have an advantage due to their focus on teamwork and their role in transitioning patients between inpatient and outpatient settings. In fact, he sees the VBPM as an “enormous opportunity” for hospitalists to demonstrate their leadership in helping to shape how organizations and institutions adapt to a quickly evolving healthcare environment.
But first, hospitalists will need to fully engage. In 2010, CMS found that only about 1 in 4 eligible physicians were participating in the voluntary PQRS and earning a reporting bonus of what is now 0.5% of allowable Medicare charges (roughly $800 for the average hospitalist). The stakes will grow when the PQRS transforms into a negative incentive program in 2015, with a 1.5% penalty for doctors who do not meet its reporting requirements. In 2016 and thereafter, the assessed penalty grows to 2% (about $3,200 for the average hospitalist).
“I think the unfolding timeline has really provided the potential for lulling us into complacency and procrastination,” says Patrick Torcson, MD, MMM, FACP, SFHM, director of hospital medicine at St. Tammany Parish Hospital in Covington, La., and chair of SHM’s Performance Measurement and Reporting Committee.
According to CMS, “physician groups can avoid all negative adjustments simply by participating in the PQRS.” Nonparticipants, however, could get hit with a double whammy. With no quality data, CMS would have no way to assess groups’ performances and would automatically deduct an extra 1% of Medicare reimbursements under the VBPM program. For groups of 100 eligible providers or more, that combined PQRS-VBPM penalty could amount to 2.5% in 2015.
PQRS participants have more leeway and a smaller downside. Starting January 2015, eligible provider groups who meet the reporting requirements can choose either to have no adjustments at all or to compete in the VBPM program for a performance-based bonus or a penalty of 1%, based on cost and quality scores. In January 2017, the program is expected to expand to include all providers, whether in individual or group practice.
A Measure of Relevance
Based on the first QRURs, sent out in March 2012 to providers in four pilot states, SHM wrote a letter to CMS that offered a detailed analysis of several additional concerns. The society followed up with a second letter that provided a more expansive critique of the proposed 2013 Physician Fee Schedule.
One worry is whether the physician feedback/VBPM program has included enough performance measures that are relevant to hospitalists. A Public Policy column in The Hospitalist (“Metric Accountability,” November 2012, p. 18) counted only 10 PQRS measures that apply routinely to HM providers out of a list of more than 200. Even those 10 aren’t always applicable.
“I work at a teaching hospital that’s large enough to have a neurology program, so most acute-stroke patients are admitted by the neurologists,” says Gregory Seymann, MD, SFHM, chief of the division of hospital medicine at the University of California at San Diego and a member of SHM’s Performance Measurement and Reporting Committee. “Five of the 10 measures are related to stroke patients, but my group rarely admits stroke patients.” That means only five PQRS measures remain relevant to him.
On paper, the issue might be readily resolved by expanding the number of measures to better reflect HM responsibilities—such as four measures proposed by SHM that relate to transitions of care and medication reconciliation.

—Patrick Torcson, MD, MMM, FACP, SFHM, director, hospital medicine, St. Tammany Parish Hospital, Covington, La., chair, SHM’s Performance Measurement and Reporting Committee
Other groups, though, have their own ideas. A letter to CMS signed by 28 patient and healthcare payor groups calls for the elimination of almost two dozen PQRS measures deemed unnecessary, duplicative, or uninformative, and for the addition of nine others that might better assess patient outcomes and quality of care. Jennifer Eames Huff, director of the Consumer-Purchaser Disclosure Project at San Francisco-based Pacific Business Group on Health, one of the letter’s signatories, says some of those potential measures might be more applicable to hospitalists as well.
But therein lies the rub. Although process measures might not always be strong indicators of quality of care, the introduction of outcome measures often makes providers nervous, says Gary Young, JD, PhD, director of the Center for Health Policy and Healthcare Research at Northeastern University in Boston. “Most providers feel that their patients are sicker and more vulnerable to poorer outcomes, and they don’t want to be judged poorly because they have sicker patients,” he says. Reaching an agreement on the best collection of measures may require some intense negotiations, he says.

–Win Whitcomb, MD, MHM, medical director of healthcare quality, Baystate Medical Center, Springfield, Mass.
Fairer Comparisons
Dr. Cowles cites two de-identified QRURs received by Alegent Creighton Health back in March—one for a hospitalist and one for an office-based general internist—to illustrate another major concern shared by many HM providers. The reports broke down each doctor’s relative healthcare contributions, using predetermined percentages of the total care and costs to conclude whether that doctor directed, influenced, or contributed to a patient’s care.
Hospitalists, by the nature of their jobs, seldom direct the care of any patient. But because their influence or contribution is almost always within the inpatient environment, HM providers account for proportionately higher costs than office-based physicians. The result can be a rather ugly curve: For healthcare costs incurred, the general internist was at the 65th percentile, while the hospitalist was at the 96th percentile.
The point, Dr. Cowles says, is that hospitalists and clinic-based physicians see patients with remarkably different acuities. “We just need to make sure that we’re comparing apples to apples, that you’re going to compare someone who sees a high-acuity patient with someone else who sees a high-acuity patient,” he says.
One silver lining could be increased momentum toward establishing HM as its own Medicare-recognized specialty. Hospitalist leaders who say the process is likely to be difficult but not impossible cite the successful effort to win recognition of HM as a focused practice by the American Board of Internal Medicine.
“We’re going to have to think outside the box in terms of working toward an identifier for hospitalists,” says Win Whitcomb, MD, MHM, medical director of healthcare quality at Baystate Medical Center in Springfield, Mass., and a member of SHM’s Performance and Measurement Reporting Committee. “But that’s going to happen—it’s not a matter of if, it’s a matter of when and how.”
As one potential interim solution, SHM has suggested a self-identification designation by which hospitalists would distinguish themselves from the larger, general internal-medicine category and thereby avoid unfair comparisons.
A Question of Attribution
Of the concerns raised by SHM, the question of attribution might be among the thorniest. Dr. Young says the “big-time issue” is pitting many consumer groups, payors, and employers against healthcare providers. The consumer groups want accountability at the individual provider level, while the providers strongly prefer group accountability, setting up a major clash over how responsibility will be parceled out.
Hospitalists have been taught to embrace responsibility while viewing healthcare delivery as a team sport. And the contributions of individual HM providers aren’t easily untangled. “If somebody has a bad outcome and they’ve been under the care of three different hospitalists, it’s virtually impossible to attribute that outcome to one of those three hospitalists,” Dr. Whitcomb says. “We really need to think about attribution differently, and it’s going to need to be across groups of hospitalists.”
SHM has suggested that CMS include an option for group rather than individual evaluation. “You’re just making it explicit that you can’t assign some of these measures to individual physicians. We can assign some of these measures to groups,” Dr. Whitcomb says.

—Julia Wright, MD, SFHM, FACP, president, MidAtlantic Business Unit, Cogent HMG, Brentwood, Tenn.
In its 2013 Medicare Physician Fee Schedule final rule, CMS opted to alter the doctor comparison methodology used for upcoming QRURs and the 2015 application of the VBPM. The agency also agreed to consider hospitalists’ concerns about fair attribution, relevant measures, and proper designation as it develops future proposals. Regardless of how those issues are ironed out, Dr. Torcson says, it’s clear to him that sitting on the sidelines is no longer an option for any physician group. Nor is it acceptable “to say this won’t work for me. We’re having to come up with proactive proposals for what will work to be part of the CMS quality agenda.”
SHM’s thorough analysis and realistic feedback, he says, has been well received by Medicare officials, raising hopes that many of the remaining differences can be resolved. “I am very confident that self-reporting or self-nomination as a hospitalist is going to be in place by the time those negative incentives kick in,” Dr. Torcson says. “And I’m also very confident that we’re going to have other, very creative options for quality measurement and performance reporting.”
One idea under consideration by CMS would allow hospitalists or other doctors to designate their hospitals’ quality data as a surrogate measure of their own performance. “I think that’s going to be a really great option for hospitalists who self-nominate,” Dr. Torcson says.
For many hospitalists, the option would effectively get around the issue of individual versus group attribution and instead align doctors’ fates with that of their institutions. SHM, Dr. Torcson says, has endorsed the proposal and offered to work with CMS to help institute it. He’s also confident that the reporting requirements for multiple, overlapping CMS programs will be more streamlined over time.
Some health professionals believe that hospitals and doctors already are devoting too much time and energy to measuring and recording the proliferating set of mandatory metrics. But Dr. Whitcomb says payors and patients are unlikely to have much sympathy.
“We as a profession are accountable to society at large. And that argument, that there are too many measurements and that we shouldn’t be held accountable as physicians for our performance, is a nonstarter when you’re trying to explain that to consumers,” he says. “The status quo is not tenable, and so it’s going to be a long journey and we need to be able to move in that direction.”
Bryn Nelson is a freelance medical writer in Seattle.
Russell Cowles III, MD, lead hospitalist at Bergan Mercy Medical Center in Omaha, Neb., recalls the shock on the faces of hospitalists who attended his presentation to SHM’s Nebraska Area chapter meeting last spring. Dr. Cowles and co-presenter Eric Rice, MD, MMM, SFHM, chapter president and assistant medical director of Alegent Creighton Hospital Medicine Services, were introducing their fellow hospitalists to a forthcoming Medicare initiative called the Physician Feedback/Value-Based Payment Modifier (VBPM) program.
“And everyone in the audience was completely stunned,” Dr. Cowles says. “They had never even dreamed that any of this would come down to the physician level.”
They’re not alone.
“Unless you work in administration or you’re leading a group, I don’t think very many people know this exists,” Dr. Cowles says. “Your average practicing physician, I think, has no clue that this measurement is going on behind the scenes.”
Authorized by the Affordable Care Act, the budget-neutral scheme ties future Medicare reimbursements to measures of quality and efficiency, and grades physicians on a curve. The Physician Quality Reporting System (PQRS), in place since 2007, forms the foundation of the new program, with feedback arriving in the form of a Quality and Resource Use Report (QRUR), a confidential report card sent to providers. The VBPM program then uses those reports as the basis for a financial reward or penalty.
In principle, SHM and hospitalist leaders have supported the concept of quality measurements as a way to hold doctors more accountable and to help the Centers for Medicare & Medicaid Services (CMS) take a more proactive role in improving quality of care while containing costs. And, in theory, HM leaders say hospitalists might be better able to adapt to the added responsibility of performance measurement and reporting due to their central role in the like-minded hospital value-based purchasing (VBP) program that began Oct. 1.
“If the expectation is that we will be involved in some of these initiatives and help the hospitals gain revenue, now we can actually see some dollars for those efforts,” says Julia Wright, MD, SFHM, FACP, president of the MidAtlantic Business Unit for Brentwood, Tenn.-based Cogent HMG. But the inverse is also true: If hospitals are going to have dollars at risk for performance, she says, CMS believes physicians should share in that risk as the providers of healthcare.
On that score, Dr. Rice says, hospitalists might have an advantage due to their focus on teamwork and their role in transitioning patients between inpatient and outpatient settings. In fact, he sees the VBPM as an “enormous opportunity” for hospitalists to demonstrate their leadership in helping to shape how organizations and institutions adapt to a quickly evolving healthcare environment.
But first, hospitalists will need to fully engage. In 2010, CMS found that only about 1 in 4 eligible physicians were participating in the voluntary PQRS and earning a reporting bonus of what is now 0.5% of allowable Medicare charges (roughly $800 for the average hospitalist). The stakes will grow when the PQRS transforms into a negative incentive program in 2015, with a 1.5% penalty for doctors who do not meet its reporting requirements. In 2016 and thereafter, the assessed penalty grows to 2% (about $3,200 for the average hospitalist).
“I think the unfolding timeline has really provided the potential for lulling us into complacency and procrastination,” says Patrick Torcson, MD, MMM, FACP, SFHM, director of hospital medicine at St. Tammany Parish Hospital in Covington, La., and chair of SHM’s Performance Measurement and Reporting Committee.
According to CMS, “physician groups can avoid all negative adjustments simply by participating in the PQRS.” Nonparticipants, however, could get hit with a double whammy. With no quality data, CMS would have no way to assess groups’ performances and would automatically deduct an extra 1% of Medicare reimbursements under the VBPM program. For groups of 100 eligible providers or more, that combined PQRS-VBPM penalty could amount to 2.5% in 2015.
PQRS participants have more leeway and a smaller downside. Starting January 2015, eligible provider groups who meet the reporting requirements can choose either to have no adjustments at all or to compete in the VBPM program for a performance-based bonus or a penalty of 1%, based on cost and quality scores. In January 2017, the program is expected to expand to include all providers, whether in individual or group practice.
A Measure of Relevance
Based on the first QRURs, sent out in March 2012 to providers in four pilot states, SHM wrote a letter to CMS that offered a detailed analysis of several additional concerns. The society followed up with a second letter that provided a more expansive critique of the proposed 2013 Physician Fee Schedule.
One worry is whether the physician feedback/VBPM program has included enough performance measures that are relevant to hospitalists. A Public Policy column in The Hospitalist (“Metric Accountability,” November 2012, p. 18) counted only 10 PQRS measures that apply routinely to HM providers out of a list of more than 200. Even those 10 aren’t always applicable.
“I work at a teaching hospital that’s large enough to have a neurology program, so most acute-stroke patients are admitted by the neurologists,” says Gregory Seymann, MD, SFHM, chief of the division of hospital medicine at the University of California at San Diego and a member of SHM’s Performance Measurement and Reporting Committee. “Five of the 10 measures are related to stroke patients, but my group rarely admits stroke patients.” That means only five PQRS measures remain relevant to him.
On paper, the issue might be readily resolved by expanding the number of measures to better reflect HM responsibilities—such as four measures proposed by SHM that relate to transitions of care and medication reconciliation.

—Patrick Torcson, MD, MMM, FACP, SFHM, director, hospital medicine, St. Tammany Parish Hospital, Covington, La., chair, SHM’s Performance Measurement and Reporting Committee
Other groups, though, have their own ideas. A letter to CMS signed by 28 patient and healthcare payor groups calls for the elimination of almost two dozen PQRS measures deemed unnecessary, duplicative, or uninformative, and for the addition of nine others that might better assess patient outcomes and quality of care. Jennifer Eames Huff, director of the Consumer-Purchaser Disclosure Project at San Francisco-based Pacific Business Group on Health, one of the letter’s signatories, says some of those potential measures might be more applicable to hospitalists as well.
But therein lies the rub. Although process measures might not always be strong indicators of quality of care, the introduction of outcome measures often makes providers nervous, says Gary Young, JD, PhD, director of the Center for Health Policy and Healthcare Research at Northeastern University in Boston. “Most providers feel that their patients are sicker and more vulnerable to poorer outcomes, and they don’t want to be judged poorly because they have sicker patients,” he says. Reaching an agreement on the best collection of measures may require some intense negotiations, he says.

–Win Whitcomb, MD, MHM, medical director of healthcare quality, Baystate Medical Center, Springfield, Mass.
Fairer Comparisons
Dr. Cowles cites two de-identified QRURs received by Alegent Creighton Health back in March—one for a hospitalist and one for an office-based general internist—to illustrate another major concern shared by many HM providers. The reports broke down each doctor’s relative healthcare contributions, using predetermined percentages of the total care and costs to conclude whether that doctor directed, influenced, or contributed to a patient’s care.
Hospitalists, by the nature of their jobs, seldom direct the care of any patient. But because their influence or contribution is almost always within the inpatient environment, HM providers account for proportionately higher costs than office-based physicians. The result can be a rather ugly curve: For healthcare costs incurred, the general internist was at the 65th percentile, while the hospitalist was at the 96th percentile.
The point, Dr. Cowles says, is that hospitalists and clinic-based physicians see patients with remarkably different acuities. “We just need to make sure that we’re comparing apples to apples, that you’re going to compare someone who sees a high-acuity patient with someone else who sees a high-acuity patient,” he says.
One silver lining could be increased momentum toward establishing HM as its own Medicare-recognized specialty. Hospitalist leaders who say the process is likely to be difficult but not impossible cite the successful effort to win recognition of HM as a focused practice by the American Board of Internal Medicine.
“We’re going to have to think outside the box in terms of working toward an identifier for hospitalists,” says Win Whitcomb, MD, MHM, medical director of healthcare quality at Baystate Medical Center in Springfield, Mass., and a member of SHM’s Performance and Measurement Reporting Committee. “But that’s going to happen—it’s not a matter of if, it’s a matter of when and how.”
As one potential interim solution, SHM has suggested a self-identification designation by which hospitalists would distinguish themselves from the larger, general internal-medicine category and thereby avoid unfair comparisons.
A Question of Attribution
Of the concerns raised by SHM, the question of attribution might be among the thorniest. Dr. Young says the “big-time issue” is pitting many consumer groups, payors, and employers against healthcare providers. The consumer groups want accountability at the individual provider level, while the providers strongly prefer group accountability, setting up a major clash over how responsibility will be parceled out.
Hospitalists have been taught to embrace responsibility while viewing healthcare delivery as a team sport. And the contributions of individual HM providers aren’t easily untangled. “If somebody has a bad outcome and they’ve been under the care of three different hospitalists, it’s virtually impossible to attribute that outcome to one of those three hospitalists,” Dr. Whitcomb says. “We really need to think about attribution differently, and it’s going to need to be across groups of hospitalists.”
SHM has suggested that CMS include an option for group rather than individual evaluation. “You’re just making it explicit that you can’t assign some of these measures to individual physicians. We can assign some of these measures to groups,” Dr. Whitcomb says.

—Julia Wright, MD, SFHM, FACP, president, MidAtlantic Business Unit, Cogent HMG, Brentwood, Tenn.
In its 2013 Medicare Physician Fee Schedule final rule, CMS opted to alter the doctor comparison methodology used for upcoming QRURs and the 2015 application of the VBPM. The agency also agreed to consider hospitalists’ concerns about fair attribution, relevant measures, and proper designation as it develops future proposals. Regardless of how those issues are ironed out, Dr. Torcson says, it’s clear to him that sitting on the sidelines is no longer an option for any physician group. Nor is it acceptable “to say this won’t work for me. We’re having to come up with proactive proposals for what will work to be part of the CMS quality agenda.”
SHM’s thorough analysis and realistic feedback, he says, has been well received by Medicare officials, raising hopes that many of the remaining differences can be resolved. “I am very confident that self-reporting or self-nomination as a hospitalist is going to be in place by the time those negative incentives kick in,” Dr. Torcson says. “And I’m also very confident that we’re going to have other, very creative options for quality measurement and performance reporting.”
One idea under consideration by CMS would allow hospitalists or other doctors to designate their hospitals’ quality data as a surrogate measure of their own performance. “I think that’s going to be a really great option for hospitalists who self-nominate,” Dr. Torcson says.
For many hospitalists, the option would effectively get around the issue of individual versus group attribution and instead align doctors’ fates with that of their institutions. SHM, Dr. Torcson says, has endorsed the proposal and offered to work with CMS to help institute it. He’s also confident that the reporting requirements for multiple, overlapping CMS programs will be more streamlined over time.
Some health professionals believe that hospitals and doctors already are devoting too much time and energy to measuring and recording the proliferating set of mandatory metrics. But Dr. Whitcomb says payors and patients are unlikely to have much sympathy.
“We as a profession are accountable to society at large. And that argument, that there are too many measurements and that we shouldn’t be held accountable as physicians for our performance, is a nonstarter when you’re trying to explain that to consumers,” he says. “The status quo is not tenable, and so it’s going to be a long journey and we need to be able to move in that direction.”
Bryn Nelson is a freelance medical writer in Seattle.
Hospitalists Should Consider Fall Risks with Sleep Agent
An author of a new study associating the hypnotic zolpidem (Ambien) with higher rates of patient falls says hospitalists should keep the popular drug’s risks front of mind.
The retrospective cohort study in the Journal of Hospital Medicine, “Zolpidem is Independently Associated with Increased Risk of Inpatient Falls,” found that the rate of falls increased nearly six times among patients taking the sleep agent.1 The research team at the Center for Sleep Medicine at the Mayo Clinic in Rochester, N.Y., calculated one additional fall for every 55 admitted patients who were administered the treatment.
“What this says to me is if one is going to use zolpidem, you have to be aware you’re increasing the risk of fall,” says sleep specialist Timothy Morgenthaler, MD, the Mayo Clinic’s chief patient officer. “Knowledgeable of that, one ought to consider whether there are alternatives or whether the risks outweigh the goal in that setting.”
Dr. Morgenthaler says zolpidem is the most commonly prescribed hypnotic at his hospital, and believes it to be the most common treatment in the U.S. He began studying the issue after nurses reported that it appeared patients were falling after taking the agent. In response to the study, Mayo Clinic removed zolpidem from many of its admission order sets and attempted to help improve patient sleep via other methods, including noise reduction.
“We haven’t removed it from our formulary, and I’m not saying it doesn’t have a role in some points,” he says, “but rather than encouraging it as an option in patients being admitted into the patient, we’re choosing instead now to encourage nonpharmacologic sleep enhancements.”
Visit the-hospitalist.org for more information about HM’s approach to patient falls.
Reference
An author of a new study associating the hypnotic zolpidem (Ambien) with higher rates of patient falls says hospitalists should keep the popular drug’s risks front of mind.
The retrospective cohort study in the Journal of Hospital Medicine, “Zolpidem is Independently Associated with Increased Risk of Inpatient Falls,” found that the rate of falls increased nearly six times among patients taking the sleep agent.1 The research team at the Center for Sleep Medicine at the Mayo Clinic in Rochester, N.Y., calculated one additional fall for every 55 admitted patients who were administered the treatment.
“What this says to me is if one is going to use zolpidem, you have to be aware you’re increasing the risk of fall,” says sleep specialist Timothy Morgenthaler, MD, the Mayo Clinic’s chief patient officer. “Knowledgeable of that, one ought to consider whether there are alternatives or whether the risks outweigh the goal in that setting.”
Dr. Morgenthaler says zolpidem is the most commonly prescribed hypnotic at his hospital, and believes it to be the most common treatment in the U.S. He began studying the issue after nurses reported that it appeared patients were falling after taking the agent. In response to the study, Mayo Clinic removed zolpidem from many of its admission order sets and attempted to help improve patient sleep via other methods, including noise reduction.
“We haven’t removed it from our formulary, and I’m not saying it doesn’t have a role in some points,” he says, “but rather than encouraging it as an option in patients being admitted into the patient, we’re choosing instead now to encourage nonpharmacologic sleep enhancements.”
Visit the-hospitalist.org for more information about HM’s approach to patient falls.
Reference
An author of a new study associating the hypnotic zolpidem (Ambien) with higher rates of patient falls says hospitalists should keep the popular drug’s risks front of mind.
The retrospective cohort study in the Journal of Hospital Medicine, “Zolpidem is Independently Associated with Increased Risk of Inpatient Falls,” found that the rate of falls increased nearly six times among patients taking the sleep agent.1 The research team at the Center for Sleep Medicine at the Mayo Clinic in Rochester, N.Y., calculated one additional fall for every 55 admitted patients who were administered the treatment.
“What this says to me is if one is going to use zolpidem, you have to be aware you’re increasing the risk of fall,” says sleep specialist Timothy Morgenthaler, MD, the Mayo Clinic’s chief patient officer. “Knowledgeable of that, one ought to consider whether there are alternatives or whether the risks outweigh the goal in that setting.”
Dr. Morgenthaler says zolpidem is the most commonly prescribed hypnotic at his hospital, and believes it to be the most common treatment in the U.S. He began studying the issue after nurses reported that it appeared patients were falling after taking the agent. In response to the study, Mayo Clinic removed zolpidem from many of its admission order sets and attempted to help improve patient sleep via other methods, including noise reduction.
“We haven’t removed it from our formulary, and I’m not saying it doesn’t have a role in some points,” he says, “but rather than encouraging it as an option in patients being admitted into the patient, we’re choosing instead now to encourage nonpharmacologic sleep enhancements.”
Visit the-hospitalist.org for more information about HM’s approach to patient falls.
Reference
Smartphones Distract Hospital Staff on Rounds
Smartphone use by hospitalists and other hospital staff is becoming ubiquitous, with a recent survey showing 72% of physicians using these devices at work.1 At the same time, concerns are being raised about clinical distractions and threats to patient privacy, even while such benefits as rapid access to colleagues, medical references, and patient records are touted.
In a study published in the Journal of Hospital Medicine, Rachel Katz-Sidlow, MD, of the department of pediatrics at Jacobi Medical Center in Bronx, N.Y., and colleagues surveyed residents’ and attendings’ perceptions of the use of smartphones during inpatient rounds, both their own and observed behaviors of colleagues.2 Fifty-seven percent of residents and 28% of faculty reported using smartphones during inpatient rounds, while significantly higher percentages observed other team members doing so.
The most common smartphone uses were for patient care, but doctors also use them to read and reply to personal texts and emails, as well as for non-patient-care-related Web searches. The authors observe that smartphones “introduce another source of interruption, multitasking, and distraction into the hospital environment,” with potential negative consequences.
Nineteen percent of residents believed they had missed important clinical information because of smartphone distraction during rounds. After seeing the survey results, Jacobi Medical Center instituted a smartphone policy in February 2012, essentially requiring personal mobile communication devices to be silenced at the start of rounds, except for patient care communication or urgent family matters, Dr. Katz-Sidlow wrote in an email to the The Hospitalist.
Confirmation of the spread of communication technology in the hospital toward smartphones and away from traditional pagers comes from data presented at the American Academy of Pediatrics conference in New Orleans in October by Stephanie Kuhlmann, MD, pediatric hospitalist at the University of Kansas at Wichita.3 Dr. Kuhlmann conducted an electronic survey of pediatric hospitalists, with 60% reporting that they receive work-related text messages. Twelve percent sent more than 10 text messages per shift, while 40% expressed concern about HIPAA violations. Most text messages are not encrypted, and many hospitals have yet to implement appropriately secure programs and policies, Dr. Kuhlmann says.
“Hospitals need to be aware of this trend and need to find a way to secure these text messages,” she adds.
Another recent survey by the Orem, Utah-based firm KLAS Research found that while 70% of clinicians report using smartphones or tablets to look up electronic patient records, they are less likely to input information into the EHR on these devices because of the difficulty of entering data on their small screens.4
References
- Dolan B. 72 percent of US physicians use smartphones. Mobi Health News website. Available at: http://mobihealthnews.com/7505/72-percent-of-us-physicians-use-smartphones/. Accessed Dec. 8, 2012.
- Katz-Sidlow RJ, Ludwig A, Millers S, Sidlow R. Smartphone use during inpatient attending rounds: prevalence, patterns and potential for distraction. J Hosp Med. 2012;7(8):595-599.
- Miller NS. Text messages are a growing trend among pediatric hospitalists. Pediatric News Digital Network website. Available at: http://www.pediatricnews.com/news/top-news/single-article/text-messages-are-a-growing-trend-among-pediatric-hospitalists/3dabf7208c75c44d36f368a83221d320.html. Accessed Nov. 1, 2012.
- Westerlind E. Mobile healthcare applications: can enterprise vendors keep up? KLAS website. Available at: http://www.klasresearch.com/KLASreports. Accessed Dec. 8, 2012.
Smartphone use by hospitalists and other hospital staff is becoming ubiquitous, with a recent survey showing 72% of physicians using these devices at work.1 At the same time, concerns are being raised about clinical distractions and threats to patient privacy, even while such benefits as rapid access to colleagues, medical references, and patient records are touted.
In a study published in the Journal of Hospital Medicine, Rachel Katz-Sidlow, MD, of the department of pediatrics at Jacobi Medical Center in Bronx, N.Y., and colleagues surveyed residents’ and attendings’ perceptions of the use of smartphones during inpatient rounds, both their own and observed behaviors of colleagues.2 Fifty-seven percent of residents and 28% of faculty reported using smartphones during inpatient rounds, while significantly higher percentages observed other team members doing so.
The most common smartphone uses were for patient care, but doctors also use them to read and reply to personal texts and emails, as well as for non-patient-care-related Web searches. The authors observe that smartphones “introduce another source of interruption, multitasking, and distraction into the hospital environment,” with potential negative consequences.
Nineteen percent of residents believed they had missed important clinical information because of smartphone distraction during rounds. After seeing the survey results, Jacobi Medical Center instituted a smartphone policy in February 2012, essentially requiring personal mobile communication devices to be silenced at the start of rounds, except for patient care communication or urgent family matters, Dr. Katz-Sidlow wrote in an email to the The Hospitalist.
Confirmation of the spread of communication technology in the hospital toward smartphones and away from traditional pagers comes from data presented at the American Academy of Pediatrics conference in New Orleans in October by Stephanie Kuhlmann, MD, pediatric hospitalist at the University of Kansas at Wichita.3 Dr. Kuhlmann conducted an electronic survey of pediatric hospitalists, with 60% reporting that they receive work-related text messages. Twelve percent sent more than 10 text messages per shift, while 40% expressed concern about HIPAA violations. Most text messages are not encrypted, and many hospitals have yet to implement appropriately secure programs and policies, Dr. Kuhlmann says.
“Hospitals need to be aware of this trend and need to find a way to secure these text messages,” she adds.
Another recent survey by the Orem, Utah-based firm KLAS Research found that while 70% of clinicians report using smartphones or tablets to look up electronic patient records, they are less likely to input information into the EHR on these devices because of the difficulty of entering data on their small screens.4
References
- Dolan B. 72 percent of US physicians use smartphones. Mobi Health News website. Available at: http://mobihealthnews.com/7505/72-percent-of-us-physicians-use-smartphones/. Accessed Dec. 8, 2012.
- Katz-Sidlow RJ, Ludwig A, Millers S, Sidlow R. Smartphone use during inpatient attending rounds: prevalence, patterns and potential for distraction. J Hosp Med. 2012;7(8):595-599.
- Miller NS. Text messages are a growing trend among pediatric hospitalists. Pediatric News Digital Network website. Available at: http://www.pediatricnews.com/news/top-news/single-article/text-messages-are-a-growing-trend-among-pediatric-hospitalists/3dabf7208c75c44d36f368a83221d320.html. Accessed Nov. 1, 2012.
- Westerlind E. Mobile healthcare applications: can enterprise vendors keep up? KLAS website. Available at: http://www.klasresearch.com/KLASreports. Accessed Dec. 8, 2012.
Smartphone use by hospitalists and other hospital staff is becoming ubiquitous, with a recent survey showing 72% of physicians using these devices at work.1 At the same time, concerns are being raised about clinical distractions and threats to patient privacy, even while such benefits as rapid access to colleagues, medical references, and patient records are touted.
In a study published in the Journal of Hospital Medicine, Rachel Katz-Sidlow, MD, of the department of pediatrics at Jacobi Medical Center in Bronx, N.Y., and colleagues surveyed residents’ and attendings’ perceptions of the use of smartphones during inpatient rounds, both their own and observed behaviors of colleagues.2 Fifty-seven percent of residents and 28% of faculty reported using smartphones during inpatient rounds, while significantly higher percentages observed other team members doing so.
The most common smartphone uses were for patient care, but doctors also use them to read and reply to personal texts and emails, as well as for non-patient-care-related Web searches. The authors observe that smartphones “introduce another source of interruption, multitasking, and distraction into the hospital environment,” with potential negative consequences.
Nineteen percent of residents believed they had missed important clinical information because of smartphone distraction during rounds. After seeing the survey results, Jacobi Medical Center instituted a smartphone policy in February 2012, essentially requiring personal mobile communication devices to be silenced at the start of rounds, except for patient care communication or urgent family matters, Dr. Katz-Sidlow wrote in an email to the The Hospitalist.
Confirmation of the spread of communication technology in the hospital toward smartphones and away from traditional pagers comes from data presented at the American Academy of Pediatrics conference in New Orleans in October by Stephanie Kuhlmann, MD, pediatric hospitalist at the University of Kansas at Wichita.3 Dr. Kuhlmann conducted an electronic survey of pediatric hospitalists, with 60% reporting that they receive work-related text messages. Twelve percent sent more than 10 text messages per shift, while 40% expressed concern about HIPAA violations. Most text messages are not encrypted, and many hospitals have yet to implement appropriately secure programs and policies, Dr. Kuhlmann says.
“Hospitals need to be aware of this trend and need to find a way to secure these text messages,” she adds.
Another recent survey by the Orem, Utah-based firm KLAS Research found that while 70% of clinicians report using smartphones or tablets to look up electronic patient records, they are less likely to input information into the EHR on these devices because of the difficulty of entering data on their small screens.4
References
- Dolan B. 72 percent of US physicians use smartphones. Mobi Health News website. Available at: http://mobihealthnews.com/7505/72-percent-of-us-physicians-use-smartphones/. Accessed Dec. 8, 2012.
- Katz-Sidlow RJ, Ludwig A, Millers S, Sidlow R. Smartphone use during inpatient attending rounds: prevalence, patterns and potential for distraction. J Hosp Med. 2012;7(8):595-599.
- Miller NS. Text messages are a growing trend among pediatric hospitalists. Pediatric News Digital Network website. Available at: http://www.pediatricnews.com/news/top-news/single-article/text-messages-are-a-growing-trend-among-pediatric-hospitalists/3dabf7208c75c44d36f368a83221d320.html. Accessed Nov. 1, 2012.
- Westerlind E. Mobile healthcare applications: can enterprise vendors keep up? KLAS website. Available at: http://www.klasresearch.com/KLASreports. Accessed Dec. 8, 2012.
Adherence to CHF Measures Doesn’t Improve Hospital Readmission Rates
A study of the relationship between hospital adherence to congestive heart failure (CHF) quality performance measures and 30-day readmission rates found little association, except for the assessment of left ventricular function, which, if not performed according to guidelines, was associated with higher readmissions.1
Lead author Sula Mazimba, MD, MPH, and colleagues at Kettering Medical Center in Kettering, Ohio, looked at adherence to the performance measures, which in recent years have been adopted by quality organizations and third-party payors as surrogate markers for quality of care. These include documented ordering of angiotensin-converting enzyme (ACE) inhibitors, providing discharge instructions to patients, and counseling on smoking cessation.
The study looked retrospectively at 6,000 CHF patients within a four-hospital healthcare system between 2001 and 2009, at a time when adherence to the performance measures rose to 99.9% from 95.8%. The hospital readmission rate for these patients averaged 19.6%.
Larry Beresford is a freelance writer in Oakland, Calif.
References
A study of the relationship between hospital adherence to congestive heart failure (CHF) quality performance measures and 30-day readmission rates found little association, except for the assessment of left ventricular function, which, if not performed according to guidelines, was associated with higher readmissions.1
Lead author Sula Mazimba, MD, MPH, and colleagues at Kettering Medical Center in Kettering, Ohio, looked at adherence to the performance measures, which in recent years have been adopted by quality organizations and third-party payors as surrogate markers for quality of care. These include documented ordering of angiotensin-converting enzyme (ACE) inhibitors, providing discharge instructions to patients, and counseling on smoking cessation.
The study looked retrospectively at 6,000 CHF patients within a four-hospital healthcare system between 2001 and 2009, at a time when adherence to the performance measures rose to 99.9% from 95.8%. The hospital readmission rate for these patients averaged 19.6%.
Larry Beresford is a freelance writer in Oakland, Calif.
References
A study of the relationship between hospital adherence to congestive heart failure (CHF) quality performance measures and 30-day readmission rates found little association, except for the assessment of left ventricular function, which, if not performed according to guidelines, was associated with higher readmissions.1
Lead author Sula Mazimba, MD, MPH, and colleagues at Kettering Medical Center in Kettering, Ohio, looked at adherence to the performance measures, which in recent years have been adopted by quality organizations and third-party payors as surrogate markers for quality of care. These include documented ordering of angiotensin-converting enzyme (ACE) inhibitors, providing discharge instructions to patients, and counseling on smoking cessation.
The study looked retrospectively at 6,000 CHF patients within a four-hospital healthcare system between 2001 and 2009, at a time when adherence to the performance measures rose to 99.9% from 95.8%. The hospital readmission rate for these patients averaged 19.6%.
Larry Beresford is a freelance writer in Oakland, Calif.
References
Win Whitcomb: Hospitalists Central to Helping Hospitals Meet Performance Goals, Avoid Financial Penalities
After a long wait, the time where quality really matters to the finance department has arrived. Why? Because now a lot of money is on the line based on hospitals’ ability to demonstrate performance on quality, patient safety, and patient satisfaction measures. And there is no physician group more central to the hospital’s performance on these measures than hospitalists.
To make this point, I will discuss the financial implications of three programs that are part of the Affordable Care Act: hospital value-based purchasing (HVBP), readmission penalties, and hospital-acquired conditions (HACs). Although many have found fault with these programs, especially the ones that only penalize hospitals (HACs and readmissions*), the dollars at risk can represent a new business case for hospitalist programs. High-performing hospitalist programs can positively impact their institution’s income statement.
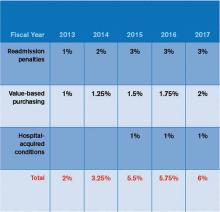
In October 2012, readmissions penalties and VBP payments/penalties went into effect. In October 2014, a 1% penalty for groups in the worst-performing quartile in the HACs will be in force. Taken together, as Table 1 demonstrates, the total payments at risk will grow such that by fiscal-year 2017, 6% of a hospital’s inpatient payments from Medicare will be at risk. To put this in perspective, Table 2 models the dollars at risk for each of the five years beginning in 2013 for the three programs in a hypothetical, 327-bed hospital. While the risk in 2013 is a modest $1.7 million, by 2017, this hospital has more than $5 million at risk.
So where should hospitalists be focusing their efforts with these three programs and the monies that accompany them? First, for those designing incentive compensation for hospitalists, the incentives should address the applicable elements of these programs. Second, the components of VBP will evolve. For example, 2013 VPB payments are based on 70% process measures (a subset of the core measure set for heart failure, myocardial infarction, pneumonia, and surgery) and 30% patient satisfaction measures. In 2015, VBP will add such outcomes measures as central-line-associated bloodstream infections, catheter UTIs, mortality rates, and the new efficiency measure, Medicare spending per beneficiary. Third, readmissions penalties, while encompassing heart failure, myocardial infarction, and pneumonia for fiscal-year 2013 payments, will expand in fiscal-year 2015 to include chronic obstructive pulmonary disease, coronary artery bypass grafting, percutaneous coronary intervention, and other vascular conditions.
While all this can be hard to keep track of, not to mention address in the course of daily patient care, I suggest hospitalists set the following priorities to enable high performance for their hospitals under these programs:
- Catheter UTIs. Work with nursing, the ED, and other areas to ensure that catheters are indicated, insertion is sterile, there is a mechanism for their prompt removal, specimens are collected and handled appropriately, and that “present on admission” is documented if appropriate.
- Central-line-associated bloodstream infections. Ensure your hospital has the systems in place to support the central-line insertion bundle, and that the bundle elements are followed and documented.
- Readmissions. Focus on heart failure, pneumonia, myocardial infarction, and COPD; work with nursing and case management to identify those at high risk for readmission; perform targeted interventions based on that risk (e.g. palliative care or clinical pharmacy consultation); prioritize medication reconciliation; provide timely communication of discharge summary to the next provider of care; and contact the patient soon after discharge to ensure they are following their plan of care.
- Patient satisfaction. Have a system for high performance on the questions comprising the “doctor communication” domain. These are “How often did doctors treat you with courtesy and respect/listen carefully to you/explain things in a way you could understand?”
Medicare’s Message
Clearly, the financial impacts of hospital quality, satisfaction, and safety are growing, conveying the message from the Centers for Medicare & Medicaid Services (CMS) that quality matters, making a business case for quality. Our focus as leaders in hospital systems improvement will only sharpen as we see hospital payments increasingly affected as a direct consequence of our efforts. If that doesn’t get the attention of the finance department, what will?
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at wfwhit@comcast.net.
After a long wait, the time where quality really matters to the finance department has arrived. Why? Because now a lot of money is on the line based on hospitals’ ability to demonstrate performance on quality, patient safety, and patient satisfaction measures. And there is no physician group more central to the hospital’s performance on these measures than hospitalists.
To make this point, I will discuss the financial implications of three programs that are part of the Affordable Care Act: hospital value-based purchasing (HVBP), readmission penalties, and hospital-acquired conditions (HACs). Although many have found fault with these programs, especially the ones that only penalize hospitals (HACs and readmissions*), the dollars at risk can represent a new business case for hospitalist programs. High-performing hospitalist programs can positively impact their institution’s income statement.
In October 2012, readmissions penalties and VBP payments/penalties went into effect. In October 2014, a 1% penalty for groups in the worst-performing quartile in the HACs will be in force. Taken together, as Table 1 demonstrates, the total payments at risk will grow such that by fiscal-year 2017, 6% of a hospital’s inpatient payments from Medicare will be at risk. To put this in perspective, Table 2 models the dollars at risk for each of the five years beginning in 2013 for the three programs in a hypothetical, 327-bed hospital. While the risk in 2013 is a modest $1.7 million, by 2017, this hospital has more than $5 million at risk.
So where should hospitalists be focusing their efforts with these three programs and the monies that accompany them? First, for those designing incentive compensation for hospitalists, the incentives should address the applicable elements of these programs. Second, the components of VBP will evolve. For example, 2013 VPB payments are based on 70% process measures (a subset of the core measure set for heart failure, myocardial infarction, pneumonia, and surgery) and 30% patient satisfaction measures. In 2015, VBP will add such outcomes measures as central-line-associated bloodstream infections, catheter UTIs, mortality rates, and the new efficiency measure, Medicare spending per beneficiary. Third, readmissions penalties, while encompassing heart failure, myocardial infarction, and pneumonia for fiscal-year 2013 payments, will expand in fiscal-year 2015 to include chronic obstructive pulmonary disease, coronary artery bypass grafting, percutaneous coronary intervention, and other vascular conditions.
While all this can be hard to keep track of, not to mention address in the course of daily patient care, I suggest hospitalists set the following priorities to enable high performance for their hospitals under these programs:
- Catheter UTIs. Work with nursing, the ED, and other areas to ensure that catheters are indicated, insertion is sterile, there is a mechanism for their prompt removal, specimens are collected and handled appropriately, and that “present on admission” is documented if appropriate.
- Central-line-associated bloodstream infections. Ensure your hospital has the systems in place to support the central-line insertion bundle, and that the bundle elements are followed and documented.
- Readmissions. Focus on heart failure, pneumonia, myocardial infarction, and COPD; work with nursing and case management to identify those at high risk for readmission; perform targeted interventions based on that risk (e.g. palliative care or clinical pharmacy consultation); prioritize medication reconciliation; provide timely communication of discharge summary to the next provider of care; and contact the patient soon after discharge to ensure they are following their plan of care.
- Patient satisfaction. Have a system for high performance on the questions comprising the “doctor communication” domain. These are “How often did doctors treat you with courtesy and respect/listen carefully to you/explain things in a way you could understand?”
Medicare’s Message
Clearly, the financial impacts of hospital quality, satisfaction, and safety are growing, conveying the message from the Centers for Medicare & Medicaid Services (CMS) that quality matters, making a business case for quality. Our focus as leaders in hospital systems improvement will only sharpen as we see hospital payments increasingly affected as a direct consequence of our efforts. If that doesn’t get the attention of the finance department, what will?
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at wfwhit@comcast.net.
After a long wait, the time where quality really matters to the finance department has arrived. Why? Because now a lot of money is on the line based on hospitals’ ability to demonstrate performance on quality, patient safety, and patient satisfaction measures. And there is no physician group more central to the hospital’s performance on these measures than hospitalists.
To make this point, I will discuss the financial implications of three programs that are part of the Affordable Care Act: hospital value-based purchasing (HVBP), readmission penalties, and hospital-acquired conditions (HACs). Although many have found fault with these programs, especially the ones that only penalize hospitals (HACs and readmissions*), the dollars at risk can represent a new business case for hospitalist programs. High-performing hospitalist programs can positively impact their institution’s income statement.
In October 2012, readmissions penalties and VBP payments/penalties went into effect. In October 2014, a 1% penalty for groups in the worst-performing quartile in the HACs will be in force. Taken together, as Table 1 demonstrates, the total payments at risk will grow such that by fiscal-year 2017, 6% of a hospital’s inpatient payments from Medicare will be at risk. To put this in perspective, Table 2 models the dollars at risk for each of the five years beginning in 2013 for the three programs in a hypothetical, 327-bed hospital. While the risk in 2013 is a modest $1.7 million, by 2017, this hospital has more than $5 million at risk.
So where should hospitalists be focusing their efforts with these three programs and the monies that accompany them? First, for those designing incentive compensation for hospitalists, the incentives should address the applicable elements of these programs. Second, the components of VBP will evolve. For example, 2013 VPB payments are based on 70% process measures (a subset of the core measure set for heart failure, myocardial infarction, pneumonia, and surgery) and 30% patient satisfaction measures. In 2015, VBP will add such outcomes measures as central-line-associated bloodstream infections, catheter UTIs, mortality rates, and the new efficiency measure, Medicare spending per beneficiary. Third, readmissions penalties, while encompassing heart failure, myocardial infarction, and pneumonia for fiscal-year 2013 payments, will expand in fiscal-year 2015 to include chronic obstructive pulmonary disease, coronary artery bypass grafting, percutaneous coronary intervention, and other vascular conditions.
While all this can be hard to keep track of, not to mention address in the course of daily patient care, I suggest hospitalists set the following priorities to enable high performance for their hospitals under these programs:
- Catheter UTIs. Work with nursing, the ED, and other areas to ensure that catheters are indicated, insertion is sterile, there is a mechanism for their prompt removal, specimens are collected and handled appropriately, and that “present on admission” is documented if appropriate.
- Central-line-associated bloodstream infections. Ensure your hospital has the systems in place to support the central-line insertion bundle, and that the bundle elements are followed and documented.
- Readmissions. Focus on heart failure, pneumonia, myocardial infarction, and COPD; work with nursing and case management to identify those at high risk for readmission; perform targeted interventions based on that risk (e.g. palliative care or clinical pharmacy consultation); prioritize medication reconciliation; provide timely communication of discharge summary to the next provider of care; and contact the patient soon after discharge to ensure they are following their plan of care.
- Patient satisfaction. Have a system for high performance on the questions comprising the “doctor communication” domain. These are “How often did doctors treat you with courtesy and respect/listen carefully to you/explain things in a way you could understand?”
Medicare’s Message
Clearly, the financial impacts of hospital quality, satisfaction, and safety are growing, conveying the message from the Centers for Medicare & Medicaid Services (CMS) that quality matters, making a business case for quality. Our focus as leaders in hospital systems improvement will only sharpen as we see hospital payments increasingly affected as a direct consequence of our efforts. If that doesn’t get the attention of the finance department, what will?
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at wfwhit@comcast.net.
2013: The Year of Quality Improvement
Years ago, hospitalists were introduced as new, efficient options for staffing hospitals. Today, they are known as the quarterbacks for patient care and quality improvement (QI) within the hospital.
This year, hospitalists everywhere can help their hospitals resolve to make 2013 a landmark year for QI. And making time for quality improvement need not be a major investment, nor do you have to “reinvent the wheel” and create your own programs.
SHM’s full menu of QI options gives hospitalists and other caregivers the confidence that their program is field-tested as well as the ability to choose the level of involvement that’s right for them.
For more information, visit www.hospitalmedicine.org/qi.
Years ago, hospitalists were introduced as new, efficient options for staffing hospitals. Today, they are known as the quarterbacks for patient care and quality improvement (QI) within the hospital.
This year, hospitalists everywhere can help their hospitals resolve to make 2013 a landmark year for QI. And making time for quality improvement need not be a major investment, nor do you have to “reinvent the wheel” and create your own programs.
SHM’s full menu of QI options gives hospitalists and other caregivers the confidence that their program is field-tested as well as the ability to choose the level of involvement that’s right for them.
For more information, visit www.hospitalmedicine.org/qi.
Years ago, hospitalists were introduced as new, efficient options for staffing hospitals. Today, they are known as the quarterbacks for patient care and quality improvement (QI) within the hospital.
This year, hospitalists everywhere can help their hospitals resolve to make 2013 a landmark year for QI. And making time for quality improvement need not be a major investment, nor do you have to “reinvent the wheel” and create your own programs.
SHM’s full menu of QI options gives hospitalists and other caregivers the confidence that their program is field-tested as well as the ability to choose the level of involvement that’s right for them.
For more information, visit www.hospitalmedicine.org/qi.
Society for Hospital Medicine Compiles List of Don'ts for Hospitalists
In hospital medicine, what a hospitalist doesn’t do can be just as important as what he or she does do.
That’s why SHM and hospitalist experts from across the country collaborated with the American Board of Internal Medicine Foundation on its groundbreaking Choosing Wisely campaign to publish 10 procedures that hospitalists should think twice about before conducting. Together, with more than a dozen medical specialties, SHM will announce the list of procedures in Washington, D.C., on Feb. 21.
Of the medical specialties contributing lists to Choosing Wisely, SHM is unique in that it will publish two lists (each with five recommendations): one for adult HM and another for pediatric HM.
Once the recommendations have been made public, hospitalists will have multiple ways of learning about them. SHM will publish the recommendations online, via email, and in The Hospitalist. Details about the unique process of developing the Choosing Wisely lists—and the impact they will have on everyday hospitalist practice—will be published in the Journal of Hospital Medicine.
Others in healthcare, including patients and family members, will have a chance to learn about Choosing Wisely through a partnership with Consumer Reports and the public dialogue that the campaign hopes to generate.
SHM President Shaun Frost, MD, SFHM, has been unequivocal in his support for the campaign and has urged all hospitalists to support it as well. “Attention to care affordability and experience are essential to reforming our broken healthcare system, so let’s lead the charge in these areas and help others who are doing the same,” Dr. Frost wrote in the November 2012 issue of The Hospitalist.
To get more involved with this industry-changing campaign, visit www.choosingwisely.org and check out the upcoming Choosing Wisely pre-course at SHM’s annual meeting at www.hospitalmedicine2013.org.
In hospital medicine, what a hospitalist doesn’t do can be just as important as what he or she does do.
That’s why SHM and hospitalist experts from across the country collaborated with the American Board of Internal Medicine Foundation on its groundbreaking Choosing Wisely campaign to publish 10 procedures that hospitalists should think twice about before conducting. Together, with more than a dozen medical specialties, SHM will announce the list of procedures in Washington, D.C., on Feb. 21.
Of the medical specialties contributing lists to Choosing Wisely, SHM is unique in that it will publish two lists (each with five recommendations): one for adult HM and another for pediatric HM.
Once the recommendations have been made public, hospitalists will have multiple ways of learning about them. SHM will publish the recommendations online, via email, and in The Hospitalist. Details about the unique process of developing the Choosing Wisely lists—and the impact they will have on everyday hospitalist practice—will be published in the Journal of Hospital Medicine.
Others in healthcare, including patients and family members, will have a chance to learn about Choosing Wisely through a partnership with Consumer Reports and the public dialogue that the campaign hopes to generate.
SHM President Shaun Frost, MD, SFHM, has been unequivocal in his support for the campaign and has urged all hospitalists to support it as well. “Attention to care affordability and experience are essential to reforming our broken healthcare system, so let’s lead the charge in these areas and help others who are doing the same,” Dr. Frost wrote in the November 2012 issue of The Hospitalist.
To get more involved with this industry-changing campaign, visit www.choosingwisely.org and check out the upcoming Choosing Wisely pre-course at SHM’s annual meeting at www.hospitalmedicine2013.org.
In hospital medicine, what a hospitalist doesn’t do can be just as important as what he or she does do.
That’s why SHM and hospitalist experts from across the country collaborated with the American Board of Internal Medicine Foundation on its groundbreaking Choosing Wisely campaign to publish 10 procedures that hospitalists should think twice about before conducting. Together, with more than a dozen medical specialties, SHM will announce the list of procedures in Washington, D.C., on Feb. 21.
Of the medical specialties contributing lists to Choosing Wisely, SHM is unique in that it will publish two lists (each with five recommendations): one for adult HM and another for pediatric HM.
Once the recommendations have been made public, hospitalists will have multiple ways of learning about them. SHM will publish the recommendations online, via email, and in The Hospitalist. Details about the unique process of developing the Choosing Wisely lists—and the impact they will have on everyday hospitalist practice—will be published in the Journal of Hospital Medicine.
Others in healthcare, including patients and family members, will have a chance to learn about Choosing Wisely through a partnership with Consumer Reports and the public dialogue that the campaign hopes to generate.
SHM President Shaun Frost, MD, SFHM, has been unequivocal in his support for the campaign and has urged all hospitalists to support it as well. “Attention to care affordability and experience are essential to reforming our broken healthcare system, so let’s lead the charge in these areas and help others who are doing the same,” Dr. Frost wrote in the November 2012 issue of The Hospitalist.
To get more involved with this industry-changing campaign, visit www.choosingwisely.org and check out the upcoming Choosing Wisely pre-course at SHM’s annual meeting at www.hospitalmedicine2013.org.
Shaun Frost: Call for Transparency in Healthcare Performance Results to Impact Hospitalists
Policymakers believe that publicly reporting healthcare performance results is essential to improving care delivery. In order to achieve a healthcare system that is consistently reliable, the Institute of Medicine (IOM) recently recommended that performance transparency be considered a foundational feature of healthcare systems that seek to constantly, systematically, and seamlessly improve.1 The IOM has suggested strategies (see Table 1, right) for producing readily available information on safety, quality, prices and cost, and health outcomes. As these strategies are being deployed, it is essential that hospitalists consider the impact they will have on their personal practice, key stakeholders, and the patients that they serve.
Performance Data Sources
The accessibility of publicly reported healthcare performance information is increasing rapidly. Among HM practitioners, perhaps the most widely recognized data source is the Centers for Medicare & Medicaid Services’ (CMS) Hospital Compare website (www.hospitalcompare.hhs.gov). According to CMS, its performance information on more than 4,000 hospitals is intended to help patients make decisions about where to seek healthcare, as well as encourage hospitals to improve the quality of care they provide.
The information currently reported is extensive and comprehensive (see Table 2, right). Furthermore, CMS continually adds data as new performance measures are created and validated.
Beyond the federal government, private health insurance companies, consortiums of employer purchasers of healthcare (e.g. the Leapfrog Group), and community collaboratives (e.g. Minnesota Community Measurement in the state of Minnesota) are reporting care provider performance information.
In addition, consumer advocacy groups have entered the picture. Earlier this year, Consumer Reports magazine launched an initiative to rate the quality of hospitals (and cardiac surgery groups) through the publication of patient outcomes (central-line-associated bloodstream infections, surgical site infections, readmissions, complications, mortality), patient experience (communications about medications and discharge, and other markers of satisfaction), and hospital best practices (use of EHR, and the appropriate use of abdominal and chest CT scanning). Consumer Reports also provides a composite hospital safety score, and a 36-page technical manual explaining the strategy and methodology behind their ratings.
Public performance reporting is furthermore becoming big business for healthcare entrepreneurs. Castlight Health, with its $181 million in private capital backing, is viewed by some as the “Travelocity of healthcare.” Castlight calls its searchable databases “transparency portals” that allow consumers to understand, before they visit a care provider, what they will be paying and how the care provider ranks on quality and outcomes.
Finally, numerous unregulated Internet sites that employ methodologically questionable practices are reporting on healthcare performance. Many of these sources collect and publish subjective reports of care experiences, with little or no requirement that the reporter confirm the nature of the relationship that they have with the care provider.
Transparency and Key Stakeholders
The hospital that you work in expects you to know how it performs, and to help it improve in the areas over which you have influence. Hospitals monitor publicly reported data because their futures depend on strong performance. As of October 2012, hospital Medicare reimbursement is linked to publicly reported performance measures that were incorporated into CMS’ value-based purchasing (VBP) initiative. Furthermore, hospital market share will be increasingly dependent on performance transparency as consumers and patients utilize these data to make informed decisions about where to seek high-value healthcare.
Patients have a vested interest in knowing how their care providers perform. A recent study by PricewaterhouseCoopers reported that 72% of consumers ranked provider reputation and personal experience as the top drivers of provider choice.2 Furthermore, employers and patients increasingly are demanding access to care affordability information—an interest driven in large part by the increasing popularity of consumer-directed health insurance plans (CDHPs). Under CDHPs, patients save money on premiums in exchange for higher deductibles that are typically paired with healthcare spending accounts. The intent is to increase consumer engagement and awareness of the cost of routine healthcare expenses while protecting against the cost of catastrophic events. It is estimated that 15% to 20% of people with employer-sponsored health insurance are in high-deductible plans, and many believe CDHPs will soon make up the majority of employer-provided coverage.
Patients interested in knowing how individual doctors perform will soon have increased access to this type of information as well. For example, CMS also produces a Physician Compare website (www.medicare.gov/find-a-doctor) that offers performance information on individual doctors. Currently, Physician Compare has little detailed information. Expect this to change, however, as Medicare moves forward with developing valid and reliable individual physician performance metrics for its Physician Value-Based Payment Modifier (VBPM) program (see “A New Measuring Stick,”).
Under VBPM, doctors will have payment modifiers assigned to their Medicare professional fee claims that will adjust payments based on the value of care that they have delivered historically. For example, it is possible in the future that physicians failing to prescribe ace inhibitors to heart failure patients will be paid less than physicians who universally provide evidence-based, best-practice heart failure care. The measurement period for the calculation of these modifiers begins this year, and hospitalists need to be aware that their performance after this time period might affect the amount of Medicare professional fee reimbursement they receive in the future.
Conclusions
Public performance reporting is a keystone healthcare reform strategy that will influence the behavior and practice patterns of hospitals and hospitalists. Hospitalists should regularly review publicly reported healthcare performance data, and commit to working collaboratively with colleagues to capitalize on improvement opportunities suggested by these data.
Dr. Frost is president of SHM.
References
- Institute of Medicine. Best care at lower cost: The path to continuously learning health care in America. Institute of Medicine website. Available at: http://www.iom.edu/bestcare. Accessed Nov. 24, 2012.
- PricewaterhouseCoopers’ Health Research Institute. Customer experience in healthcare: the moment of truth. PricewaterhouseCoopers website. Available at: http://www.pwc.com/es_MX/mx/publicaciones/archivo/2012-09-customer-experience-healthcare.pdf. Accessed Nov. 25, 2012.
Policymakers believe that publicly reporting healthcare performance results is essential to improving care delivery. In order to achieve a healthcare system that is consistently reliable, the Institute of Medicine (IOM) recently recommended that performance transparency be considered a foundational feature of healthcare systems that seek to constantly, systematically, and seamlessly improve.1 The IOM has suggested strategies (see Table 1, right) for producing readily available information on safety, quality, prices and cost, and health outcomes. As these strategies are being deployed, it is essential that hospitalists consider the impact they will have on their personal practice, key stakeholders, and the patients that they serve.
Performance Data Sources
The accessibility of publicly reported healthcare performance information is increasing rapidly. Among HM practitioners, perhaps the most widely recognized data source is the Centers for Medicare & Medicaid Services’ (CMS) Hospital Compare website (www.hospitalcompare.hhs.gov). According to CMS, its performance information on more than 4,000 hospitals is intended to help patients make decisions about where to seek healthcare, as well as encourage hospitals to improve the quality of care they provide.
The information currently reported is extensive and comprehensive (see Table 2, right). Furthermore, CMS continually adds data as new performance measures are created and validated.
Beyond the federal government, private health insurance companies, consortiums of employer purchasers of healthcare (e.g. the Leapfrog Group), and community collaboratives (e.g. Minnesota Community Measurement in the state of Minnesota) are reporting care provider performance information.
In addition, consumer advocacy groups have entered the picture. Earlier this year, Consumer Reports magazine launched an initiative to rate the quality of hospitals (and cardiac surgery groups) through the publication of patient outcomes (central-line-associated bloodstream infections, surgical site infections, readmissions, complications, mortality), patient experience (communications about medications and discharge, and other markers of satisfaction), and hospital best practices (use of EHR, and the appropriate use of abdominal and chest CT scanning). Consumer Reports also provides a composite hospital safety score, and a 36-page technical manual explaining the strategy and methodology behind their ratings.
Public performance reporting is furthermore becoming big business for healthcare entrepreneurs. Castlight Health, with its $181 million in private capital backing, is viewed by some as the “Travelocity of healthcare.” Castlight calls its searchable databases “transparency portals” that allow consumers to understand, before they visit a care provider, what they will be paying and how the care provider ranks on quality and outcomes.
Finally, numerous unregulated Internet sites that employ methodologically questionable practices are reporting on healthcare performance. Many of these sources collect and publish subjective reports of care experiences, with little or no requirement that the reporter confirm the nature of the relationship that they have with the care provider.
Transparency and Key Stakeholders
The hospital that you work in expects you to know how it performs, and to help it improve in the areas over which you have influence. Hospitals monitor publicly reported data because their futures depend on strong performance. As of October 2012, hospital Medicare reimbursement is linked to publicly reported performance measures that were incorporated into CMS’ value-based purchasing (VBP) initiative. Furthermore, hospital market share will be increasingly dependent on performance transparency as consumers and patients utilize these data to make informed decisions about where to seek high-value healthcare.
Patients have a vested interest in knowing how their care providers perform. A recent study by PricewaterhouseCoopers reported that 72% of consumers ranked provider reputation and personal experience as the top drivers of provider choice.2 Furthermore, employers and patients increasingly are demanding access to care affordability information—an interest driven in large part by the increasing popularity of consumer-directed health insurance plans (CDHPs). Under CDHPs, patients save money on premiums in exchange for higher deductibles that are typically paired with healthcare spending accounts. The intent is to increase consumer engagement and awareness of the cost of routine healthcare expenses while protecting against the cost of catastrophic events. It is estimated that 15% to 20% of people with employer-sponsored health insurance are in high-deductible plans, and many believe CDHPs will soon make up the majority of employer-provided coverage.
Patients interested in knowing how individual doctors perform will soon have increased access to this type of information as well. For example, CMS also produces a Physician Compare website (www.medicare.gov/find-a-doctor) that offers performance information on individual doctors. Currently, Physician Compare has little detailed information. Expect this to change, however, as Medicare moves forward with developing valid and reliable individual physician performance metrics for its Physician Value-Based Payment Modifier (VBPM) program (see “A New Measuring Stick,”).
Under VBPM, doctors will have payment modifiers assigned to their Medicare professional fee claims that will adjust payments based on the value of care that they have delivered historically. For example, it is possible in the future that physicians failing to prescribe ace inhibitors to heart failure patients will be paid less than physicians who universally provide evidence-based, best-practice heart failure care. The measurement period for the calculation of these modifiers begins this year, and hospitalists need to be aware that their performance after this time period might affect the amount of Medicare professional fee reimbursement they receive in the future.
Conclusions
Public performance reporting is a keystone healthcare reform strategy that will influence the behavior and practice patterns of hospitals and hospitalists. Hospitalists should regularly review publicly reported healthcare performance data, and commit to working collaboratively with colleagues to capitalize on improvement opportunities suggested by these data.
Dr. Frost is president of SHM.
References
- Institute of Medicine. Best care at lower cost: The path to continuously learning health care in America. Institute of Medicine website. Available at: http://www.iom.edu/bestcare. Accessed Nov. 24, 2012.
- PricewaterhouseCoopers’ Health Research Institute. Customer experience in healthcare: the moment of truth. PricewaterhouseCoopers website. Available at: http://www.pwc.com/es_MX/mx/publicaciones/archivo/2012-09-customer-experience-healthcare.pdf. Accessed Nov. 25, 2012.
Policymakers believe that publicly reporting healthcare performance results is essential to improving care delivery. In order to achieve a healthcare system that is consistently reliable, the Institute of Medicine (IOM) recently recommended that performance transparency be considered a foundational feature of healthcare systems that seek to constantly, systematically, and seamlessly improve.1 The IOM has suggested strategies (see Table 1, right) for producing readily available information on safety, quality, prices and cost, and health outcomes. As these strategies are being deployed, it is essential that hospitalists consider the impact they will have on their personal practice, key stakeholders, and the patients that they serve.
Performance Data Sources
The accessibility of publicly reported healthcare performance information is increasing rapidly. Among HM practitioners, perhaps the most widely recognized data source is the Centers for Medicare & Medicaid Services’ (CMS) Hospital Compare website (www.hospitalcompare.hhs.gov). According to CMS, its performance information on more than 4,000 hospitals is intended to help patients make decisions about where to seek healthcare, as well as encourage hospitals to improve the quality of care they provide.
The information currently reported is extensive and comprehensive (see Table 2, right). Furthermore, CMS continually adds data as new performance measures are created and validated.
Beyond the federal government, private health insurance companies, consortiums of employer purchasers of healthcare (e.g. the Leapfrog Group), and community collaboratives (e.g. Minnesota Community Measurement in the state of Minnesota) are reporting care provider performance information.
In addition, consumer advocacy groups have entered the picture. Earlier this year, Consumer Reports magazine launched an initiative to rate the quality of hospitals (and cardiac surgery groups) through the publication of patient outcomes (central-line-associated bloodstream infections, surgical site infections, readmissions, complications, mortality), patient experience (communications about medications and discharge, and other markers of satisfaction), and hospital best practices (use of EHR, and the appropriate use of abdominal and chest CT scanning). Consumer Reports also provides a composite hospital safety score, and a 36-page technical manual explaining the strategy and methodology behind their ratings.
Public performance reporting is furthermore becoming big business for healthcare entrepreneurs. Castlight Health, with its $181 million in private capital backing, is viewed by some as the “Travelocity of healthcare.” Castlight calls its searchable databases “transparency portals” that allow consumers to understand, before they visit a care provider, what they will be paying and how the care provider ranks on quality and outcomes.
Finally, numerous unregulated Internet sites that employ methodologically questionable practices are reporting on healthcare performance. Many of these sources collect and publish subjective reports of care experiences, with little or no requirement that the reporter confirm the nature of the relationship that they have with the care provider.
Transparency and Key Stakeholders
The hospital that you work in expects you to know how it performs, and to help it improve in the areas over which you have influence. Hospitals monitor publicly reported data because their futures depend on strong performance. As of October 2012, hospital Medicare reimbursement is linked to publicly reported performance measures that were incorporated into CMS’ value-based purchasing (VBP) initiative. Furthermore, hospital market share will be increasingly dependent on performance transparency as consumers and patients utilize these data to make informed decisions about where to seek high-value healthcare.
Patients have a vested interest in knowing how their care providers perform. A recent study by PricewaterhouseCoopers reported that 72% of consumers ranked provider reputation and personal experience as the top drivers of provider choice.2 Furthermore, employers and patients increasingly are demanding access to care affordability information—an interest driven in large part by the increasing popularity of consumer-directed health insurance plans (CDHPs). Under CDHPs, patients save money on premiums in exchange for higher deductibles that are typically paired with healthcare spending accounts. The intent is to increase consumer engagement and awareness of the cost of routine healthcare expenses while protecting against the cost of catastrophic events. It is estimated that 15% to 20% of people with employer-sponsored health insurance are in high-deductible plans, and many believe CDHPs will soon make up the majority of employer-provided coverage.
Patients interested in knowing how individual doctors perform will soon have increased access to this type of information as well. For example, CMS also produces a Physician Compare website (www.medicare.gov/find-a-doctor) that offers performance information on individual doctors. Currently, Physician Compare has little detailed information. Expect this to change, however, as Medicare moves forward with developing valid and reliable individual physician performance metrics for its Physician Value-Based Payment Modifier (VBPM) program (see “A New Measuring Stick,”).
Under VBPM, doctors will have payment modifiers assigned to their Medicare professional fee claims that will adjust payments based on the value of care that they have delivered historically. For example, it is possible in the future that physicians failing to prescribe ace inhibitors to heart failure patients will be paid less than physicians who universally provide evidence-based, best-practice heart failure care. The measurement period for the calculation of these modifiers begins this year, and hospitalists need to be aware that their performance after this time period might affect the amount of Medicare professional fee reimbursement they receive in the future.
Conclusions
Public performance reporting is a keystone healthcare reform strategy that will influence the behavior and practice patterns of hospitals and hospitalists. Hospitalists should regularly review publicly reported healthcare performance data, and commit to working collaboratively with colleagues to capitalize on improvement opportunities suggested by these data.
Dr. Frost is president of SHM.
References
- Institute of Medicine. Best care at lower cost: The path to continuously learning health care in America. Institute of Medicine website. Available at: http://www.iom.edu/bestcare. Accessed Nov. 24, 2012.
- PricewaterhouseCoopers’ Health Research Institute. Customer experience in healthcare: the moment of truth. PricewaterhouseCoopers website. Available at: http://www.pwc.com/es_MX/mx/publicaciones/archivo/2012-09-customer-experience-healthcare.pdf. Accessed Nov. 25, 2012.