User login
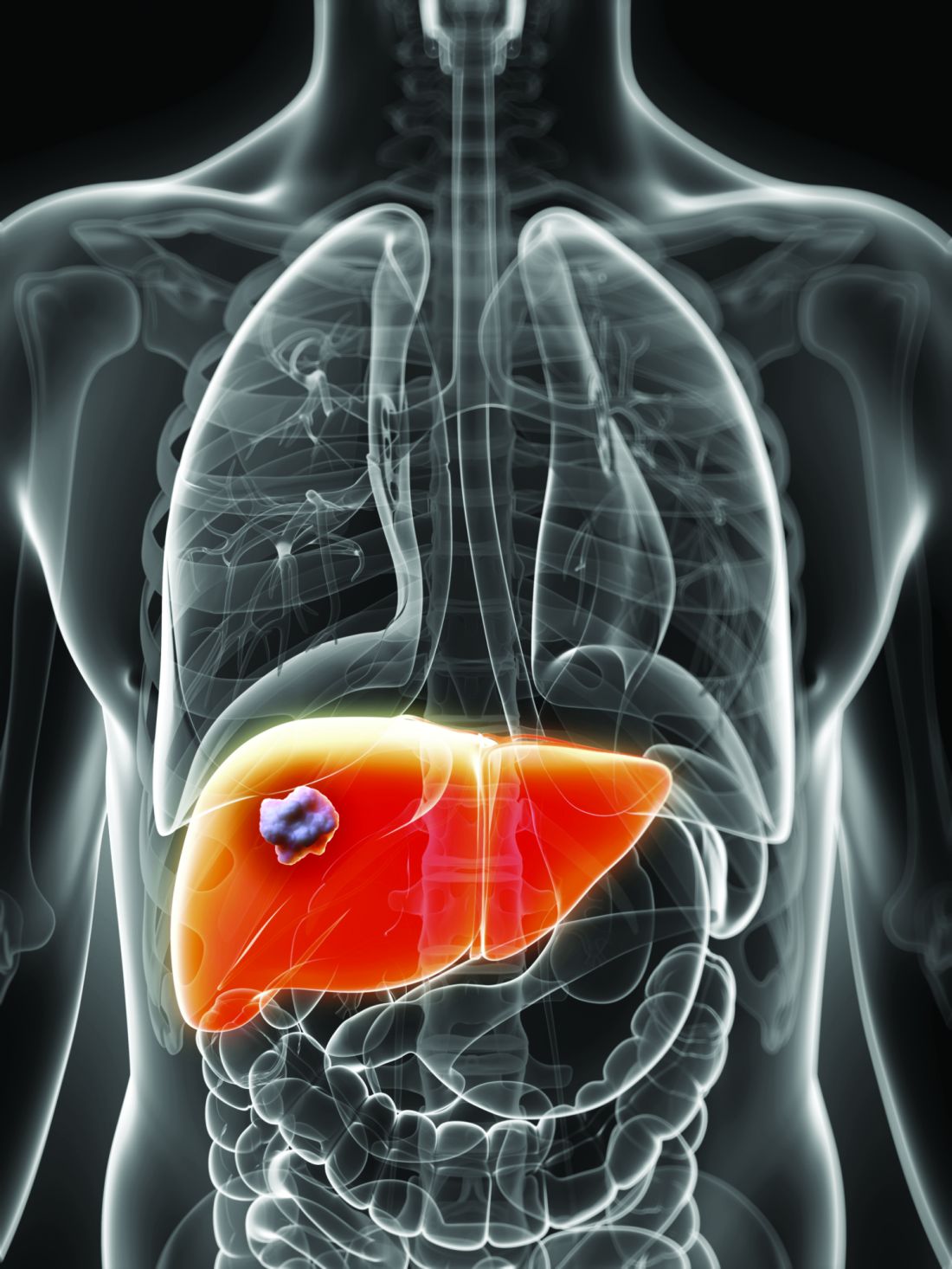
Prealbumin level predicts outcomes for HCC resection
Preoperative prealbumin levels independently predicted survival after curative liver resection for hepatocellular carcinoma (HCC) in a recent multicenter, retrospective study.
By contrast, preoperative albumin levels did not predict long-term overall or relapse-free survival in the analysis, which was reported by Tian Yang, MD, and Feng Shen, MD, along with their coinvestigators, in the journal HPB.
Those findings suggest that serum prealbumin is superior to the widely used serum albumin level as a marker of nutritional status and liver function in this setting, according to Dr. Yang and Dr. Shen, who are with the department of hepatobiliary surgery at Eastern Hepatobiliary Surgery Hospital, Shanghai, China.
“The importance of preoperative prealbumin level in predicting long-term prognosis after liver resection for HCC should be given adequate attention by hepatic surgeons,” they wrote in their report.
The retrospective analysis included a total of 1,483 patients with HCC newly diagnosed at one of six medical institutions in China during 2001-2014. Of those patients, 1,046 (71%) had normal prealbumin levels (above 170 mg/L) measured within a week before surgery, while the remaining 437 (29%) had low prealbumin levels.
Overall survival was a mean of 72 months for the low prealbumin group versus 99 months for the normal prealbumin group (P less than .001), with a corresponding 5-year overall survival of 31% versus 43%, respectively, investigators reported
Likewise, relapse-free survival was a mean of 56 months for the low prealbumin group versus 77 months for the normal prealbumin groups (P less than .001), with 5-year relapse-free survival rates of 20% and 28%, respectively.
In multivariable Cox-regression analyses, the hazard ratios of low preoperative prealbumin level for risk of decreased overall survival and for risk of decreased relapse-free survival were 1.45 (95% confidence interval, 1.24-1.70) and 1.28 (95% CI, 1.10-1.48), respectively.
By contrast, preoperative albumin level was not an independent predictor of either overall or relapse-free survival in multivariate analyses, according to investigators.
Despite these findings, it remains controversial as to which marker is more accurate as a measure of nutritional status, investigators wrote in their report.
While albumin is more commonly used in clinical practice, they explained, multiple studies have shown prealbumin is more specific and sensitive in evaluating protein malnutrition and liver function.
The present study, although retrospective, is multicenter, has a large sample size, and includes adequately long follow-up. Nevertheless, further studies will be required to determine whether prealbumin could replace albumin for assessments of nutritional status and liver function after curative liver resection for HCC, investigators concluded.
The research was supported in part by the National Natural Science Foundation of China and the Shanghai Pujiang Program. Dr. Yang, Dr. Shen, and their coauthors had no conflicts of interest to disclose.
SOURCE: Li J-D et al. HPB (Oxford). 2018 Aug 3. doi: 10.1016/j.hpb.2018.06.1803.
Preoperative prealbumin levels independently predicted survival after curative liver resection for hepatocellular carcinoma (HCC) in a recent multicenter, retrospective study.
By contrast, preoperative albumin levels did not predict long-term overall or relapse-free survival in the analysis, which was reported by Tian Yang, MD, and Feng Shen, MD, along with their coinvestigators, in the journal HPB.
Those findings suggest that serum prealbumin is superior to the widely used serum albumin level as a marker of nutritional status and liver function in this setting, according to Dr. Yang and Dr. Shen, who are with the department of hepatobiliary surgery at Eastern Hepatobiliary Surgery Hospital, Shanghai, China.
“The importance of preoperative prealbumin level in predicting long-term prognosis after liver resection for HCC should be given adequate attention by hepatic surgeons,” they wrote in their report.
The retrospective analysis included a total of 1,483 patients with HCC newly diagnosed at one of six medical institutions in China during 2001-2014. Of those patients, 1,046 (71%) had normal prealbumin levels (above 170 mg/L) measured within a week before surgery, while the remaining 437 (29%) had low prealbumin levels.
Overall survival was a mean of 72 months for the low prealbumin group versus 99 months for the normal prealbumin group (P less than .001), with a corresponding 5-year overall survival of 31% versus 43%, respectively, investigators reported
Likewise, relapse-free survival was a mean of 56 months for the low prealbumin group versus 77 months for the normal prealbumin groups (P less than .001), with 5-year relapse-free survival rates of 20% and 28%, respectively.
In multivariable Cox-regression analyses, the hazard ratios of low preoperative prealbumin level for risk of decreased overall survival and for risk of decreased relapse-free survival were 1.45 (95% confidence interval, 1.24-1.70) and 1.28 (95% CI, 1.10-1.48), respectively.
By contrast, preoperative albumin level was not an independent predictor of either overall or relapse-free survival in multivariate analyses, according to investigators.
Despite these findings, it remains controversial as to which marker is more accurate as a measure of nutritional status, investigators wrote in their report.
While albumin is more commonly used in clinical practice, they explained, multiple studies have shown prealbumin is more specific and sensitive in evaluating protein malnutrition and liver function.
The present study, although retrospective, is multicenter, has a large sample size, and includes adequately long follow-up. Nevertheless, further studies will be required to determine whether prealbumin could replace albumin for assessments of nutritional status and liver function after curative liver resection for HCC, investigators concluded.
The research was supported in part by the National Natural Science Foundation of China and the Shanghai Pujiang Program. Dr. Yang, Dr. Shen, and their coauthors had no conflicts of interest to disclose.
SOURCE: Li J-D et al. HPB (Oxford). 2018 Aug 3. doi: 10.1016/j.hpb.2018.06.1803.
Preoperative prealbumin levels independently predicted survival after curative liver resection for hepatocellular carcinoma (HCC) in a recent multicenter, retrospective study.
By contrast, preoperative albumin levels did not predict long-term overall or relapse-free survival in the analysis, which was reported by Tian Yang, MD, and Feng Shen, MD, along with their coinvestigators, in the journal HPB.
Those findings suggest that serum prealbumin is superior to the widely used serum albumin level as a marker of nutritional status and liver function in this setting, according to Dr. Yang and Dr. Shen, who are with the department of hepatobiliary surgery at Eastern Hepatobiliary Surgery Hospital, Shanghai, China.
“The importance of preoperative prealbumin level in predicting long-term prognosis after liver resection for HCC should be given adequate attention by hepatic surgeons,” they wrote in their report.
The retrospective analysis included a total of 1,483 patients with HCC newly diagnosed at one of six medical institutions in China during 2001-2014. Of those patients, 1,046 (71%) had normal prealbumin levels (above 170 mg/L) measured within a week before surgery, while the remaining 437 (29%) had low prealbumin levels.
Overall survival was a mean of 72 months for the low prealbumin group versus 99 months for the normal prealbumin group (P less than .001), with a corresponding 5-year overall survival of 31% versus 43%, respectively, investigators reported
Likewise, relapse-free survival was a mean of 56 months for the low prealbumin group versus 77 months for the normal prealbumin groups (P less than .001), with 5-year relapse-free survival rates of 20% and 28%, respectively.
In multivariable Cox-regression analyses, the hazard ratios of low preoperative prealbumin level for risk of decreased overall survival and for risk of decreased relapse-free survival were 1.45 (95% confidence interval, 1.24-1.70) and 1.28 (95% CI, 1.10-1.48), respectively.
By contrast, preoperative albumin level was not an independent predictor of either overall or relapse-free survival in multivariate analyses, according to investigators.
Despite these findings, it remains controversial as to which marker is more accurate as a measure of nutritional status, investigators wrote in their report.
While albumin is more commonly used in clinical practice, they explained, multiple studies have shown prealbumin is more specific and sensitive in evaluating protein malnutrition and liver function.
The present study, although retrospective, is multicenter, has a large sample size, and includes adequately long follow-up. Nevertheless, further studies will be required to determine whether prealbumin could replace albumin for assessments of nutritional status and liver function after curative liver resection for HCC, investigators concluded.
The research was supported in part by the National Natural Science Foundation of China and the Shanghai Pujiang Program. Dr. Yang, Dr. Shen, and their coauthors had no conflicts of interest to disclose.
SOURCE: Li J-D et al. HPB (Oxford). 2018 Aug 3. doi: 10.1016/j.hpb.2018.06.1803.
FROM HPB
Key clinical point: Preoperative prealbumin levels independently predicted survival after curative liver resection for HCC, while preoperative albumin levels did not.
Major finding: The hazard ratios of low preoperative prealbumin level for risk of decreased overall survival and for risk of decreased relapse-free survival were 1.45 (95% confidence interval, 1.24-1.70) and 1.28 (95% CI, 1.10-1.48), respectively.
Study details: Retrospective analysis that included 1,483 patients with HCC newly diagnosed at one of six institutions in China during 2001-2014.
Disclosures: The research was supported in part by the National Natural Science Foundation of China and the Shanghai Pujiang Program. The study authors had no conflicts of interest to disclose.
Source: Li J-D et al. HPB (Oxford). 2018 Aug 3. doi: 10.1016/j.hpb.2018.06.1803.
Percutaneous drainage upped morbidity risk in hepatobiliary cancer patients
ORLANDO – In patients with was associated with an increased risk of death or serious morbidity versus endoscopic drainage, results of a recent retrospective study show.
Patients undergoing percutaneous transhepatic biliary drainage did have more preoperative comorbidities, compared with those undergoing endoscopic biliary stenting, according researcher Q. Lina Hu, MD, an American College of Surgeons Clinical Scholar-in-Residence.
“Nevertheless, compared to endoscopic drainage, percutaneous drainage was associated with a significantly increased morbidity and mortality, even after adjustment for measured confounders,” Dr. Hu said a presentation at the American College of Surgeons Quality and Safety Conference.
Patients with resectable hepatobiliary malignancies often present with biliary obstruction, which may increase risk of perioperative morbidity and mortality, said Dr. Hu, a general surgery resident at University of California, Los Angeles.
“Preoperative biliary drainage is thought to reduce this risk by resolving cholestasis and preserving liver function,” she said.
However, the preferred drainage technique is not established, she added.
The endoscopic approach approximates normal physiologic drainage, she said, but is associated with complications including pancreatitis and cholangitis. By contrast, percutaneous drainage has a lower contamination risk and higher rate of success, but involves external catheters and has catheter-related complications.
To evaluate associations between preoperative drainage technique and postoperative outcomes, Dr. Hu and her colleagues queried the ACS National Surgical Quality Improvement Program (NSQIP) Procedure-Targeted Hepatectomy Database. They identified 527 patients who underwent preoperative biliary drainage prior to resection between 2014 and 2017, of whom about 80% underwent endoscopic drainage and 20% underwent percutaneous drainage. The primary outcome of their analysis was 30-day death or serious morbidity.
Patients who were selected for percutaneous drainage had significantly more preoperative comorbidities, including higher American Society of Anesthesiologists class, recent weight loss, and lower albumin levels, Dr. Hu said.
Death or serious morbidity occurred in 250 of the patients, or approximately 48% of the cohort.
In unadjusted analysis, the incidence of death or serious morbidity was significantly more frequent in the percutaneous group, compared with endoscopic group. The percutaneous group also had greater odds of surgical site infection, liver failure, bile leakage, and prolonged length of stay.
Those associations remained significant for death or serious morbidity and surgical site infection in both multivariable– and propensity score–adjusted models, Dr. Hu said.
In a propensity score–matched model, 93 patients who received percutaneous drainage were matched one-to-one to 93 patients who received endoscopic drainage based on relevant baseline characteristics. In that rigorous analysis, the odds ratio for death or serious morbidity was 2.17 (95% confidence interval, 1.16-4.09), according to the report.
“Death and serious morbidity was significantly associated with percutaneous drainage across all models, suggesting that patients receiving percutaneous drainage were more likely to experience an adverse event, compared to patients receiving endoscopic drainage,” Dr. Hu said.
However, Dr. Hu acknowledged the limitations of the retrospective study, noting that propensity score adjustment and matching accounts for measured confounders. “It obviously cannot account for any unmeasured confounders,” she said.
Dr. Hu reported funding from the Agency for Healthcare Research and Quality related to her position. She had no disclosures related to her presentation.
ORLANDO – In patients with was associated with an increased risk of death or serious morbidity versus endoscopic drainage, results of a recent retrospective study show.
Patients undergoing percutaneous transhepatic biliary drainage did have more preoperative comorbidities, compared with those undergoing endoscopic biliary stenting, according researcher Q. Lina Hu, MD, an American College of Surgeons Clinical Scholar-in-Residence.
“Nevertheless, compared to endoscopic drainage, percutaneous drainage was associated with a significantly increased morbidity and mortality, even after adjustment for measured confounders,” Dr. Hu said a presentation at the American College of Surgeons Quality and Safety Conference.
Patients with resectable hepatobiliary malignancies often present with biliary obstruction, which may increase risk of perioperative morbidity and mortality, said Dr. Hu, a general surgery resident at University of California, Los Angeles.
“Preoperative biliary drainage is thought to reduce this risk by resolving cholestasis and preserving liver function,” she said.
However, the preferred drainage technique is not established, she added.
The endoscopic approach approximates normal physiologic drainage, she said, but is associated with complications including pancreatitis and cholangitis. By contrast, percutaneous drainage has a lower contamination risk and higher rate of success, but involves external catheters and has catheter-related complications.
To evaluate associations between preoperative drainage technique and postoperative outcomes, Dr. Hu and her colleagues queried the ACS National Surgical Quality Improvement Program (NSQIP) Procedure-Targeted Hepatectomy Database. They identified 527 patients who underwent preoperative biliary drainage prior to resection between 2014 and 2017, of whom about 80% underwent endoscopic drainage and 20% underwent percutaneous drainage. The primary outcome of their analysis was 30-day death or serious morbidity.
Patients who were selected for percutaneous drainage had significantly more preoperative comorbidities, including higher American Society of Anesthesiologists class, recent weight loss, and lower albumin levels, Dr. Hu said.
Death or serious morbidity occurred in 250 of the patients, or approximately 48% of the cohort.
In unadjusted analysis, the incidence of death or serious morbidity was significantly more frequent in the percutaneous group, compared with endoscopic group. The percutaneous group also had greater odds of surgical site infection, liver failure, bile leakage, and prolonged length of stay.
Those associations remained significant for death or serious morbidity and surgical site infection in both multivariable– and propensity score–adjusted models, Dr. Hu said.
In a propensity score–matched model, 93 patients who received percutaneous drainage were matched one-to-one to 93 patients who received endoscopic drainage based on relevant baseline characteristics. In that rigorous analysis, the odds ratio for death or serious morbidity was 2.17 (95% confidence interval, 1.16-4.09), according to the report.
“Death and serious morbidity was significantly associated with percutaneous drainage across all models, suggesting that patients receiving percutaneous drainage were more likely to experience an adverse event, compared to patients receiving endoscopic drainage,” Dr. Hu said.
However, Dr. Hu acknowledged the limitations of the retrospective study, noting that propensity score adjustment and matching accounts for measured confounders. “It obviously cannot account for any unmeasured confounders,” she said.
Dr. Hu reported funding from the Agency for Healthcare Research and Quality related to her position. She had no disclosures related to her presentation.
ORLANDO – In patients with was associated with an increased risk of death or serious morbidity versus endoscopic drainage, results of a recent retrospective study show.
Patients undergoing percutaneous transhepatic biliary drainage did have more preoperative comorbidities, compared with those undergoing endoscopic biliary stenting, according researcher Q. Lina Hu, MD, an American College of Surgeons Clinical Scholar-in-Residence.
“Nevertheless, compared to endoscopic drainage, percutaneous drainage was associated with a significantly increased morbidity and mortality, even after adjustment for measured confounders,” Dr. Hu said a presentation at the American College of Surgeons Quality and Safety Conference.
Patients with resectable hepatobiliary malignancies often present with biliary obstruction, which may increase risk of perioperative morbidity and mortality, said Dr. Hu, a general surgery resident at University of California, Los Angeles.
“Preoperative biliary drainage is thought to reduce this risk by resolving cholestasis and preserving liver function,” she said.
However, the preferred drainage technique is not established, she added.
The endoscopic approach approximates normal physiologic drainage, she said, but is associated with complications including pancreatitis and cholangitis. By contrast, percutaneous drainage has a lower contamination risk and higher rate of success, but involves external catheters and has catheter-related complications.
To evaluate associations between preoperative drainage technique and postoperative outcomes, Dr. Hu and her colleagues queried the ACS National Surgical Quality Improvement Program (NSQIP) Procedure-Targeted Hepatectomy Database. They identified 527 patients who underwent preoperative biliary drainage prior to resection between 2014 and 2017, of whom about 80% underwent endoscopic drainage and 20% underwent percutaneous drainage. The primary outcome of their analysis was 30-day death or serious morbidity.
Patients who were selected for percutaneous drainage had significantly more preoperative comorbidities, including higher American Society of Anesthesiologists class, recent weight loss, and lower albumin levels, Dr. Hu said.
Death or serious morbidity occurred in 250 of the patients, or approximately 48% of the cohort.
In unadjusted analysis, the incidence of death or serious morbidity was significantly more frequent in the percutaneous group, compared with endoscopic group. The percutaneous group also had greater odds of surgical site infection, liver failure, bile leakage, and prolonged length of stay.
Those associations remained significant for death or serious morbidity and surgical site infection in both multivariable– and propensity score–adjusted models, Dr. Hu said.
In a propensity score–matched model, 93 patients who received percutaneous drainage were matched one-to-one to 93 patients who received endoscopic drainage based on relevant baseline characteristics. In that rigorous analysis, the odds ratio for death or serious morbidity was 2.17 (95% confidence interval, 1.16-4.09), according to the report.
“Death and serious morbidity was significantly associated with percutaneous drainage across all models, suggesting that patients receiving percutaneous drainage were more likely to experience an adverse event, compared to patients receiving endoscopic drainage,” Dr. Hu said.
However, Dr. Hu acknowledged the limitations of the retrospective study, noting that propensity score adjustment and matching accounts for measured confounders. “It obviously cannot account for any unmeasured confounders,” she said.
Dr. Hu reported funding from the Agency for Healthcare Research and Quality related to her position. She had no disclosures related to her presentation.
REPORTING FROM ACSQSC 2018
Key clinical point: Percutaneous biliary drainage for resectable hepatobiliary cancer was associated with an increased risk of death or serious morbidity, compared with endoscopic drainage.
Major finding: For patients having percutaneous biliary drainage, the odds ratio for death or serious morbidity was 2.17 (95% confidence interval, 1.16-4.09).
Study details: Cohort of 327 patients in the ACS NSQIP database who underwent preoperative biliary drainage.
Disclosures: The investigators had no disclosures.
Neoadjuvant-treated N2 rectal cancer linked to PCR failure
Orlando – Clinical an analysis of a large, multicenter database has suggested.
In multivariate regression, pretreatment N2 stage was the only variable significantly associated with failure of achieving pathologic complete response, according to Ebram Salama, MD, of Sir Mortimer B. Davis Jewish General Hospital at McGill University, Montreal.
“We should be reconsidering putting these patients in watch-and-wait protocols,” Dr. Salama said in an oral abstract presentation at the American College of Surgeons Quality and Safety Conference.
The analysis included 369 elective cases of cT2-4 N0-2 rectal cancer that were treated with neoadjuvant chemoradiotherapy during 2016 from the American College of Surgeons National Surgical Quality Improvement Program (NSQIP) proctectomy-specific database.
Of those cases, 53 (14.4%) achieved PCR, a proportion consistent with what has been reported previously in medical literature, Dr. Salama noted during his presentation.
The multivariate analysis revealed that pretreatment N2 stage was a negative predictor of PCR with an odds ratio of 0.18 (95% confidence interval, 0.04-0.82; P = .026), according to presented data.
By contrast, Dr. Salama said, there were no significant associations between response and other variables, including pretreatment N1 stage, pretreatment T stage, tumor location, gender, or body mass index.
Dr. Salama acknowledged limitations of this retrospective study, including a lack of data on other variables of interest, such as carcinoembryonic antigen, tumor size, imaging characteristics, molecular markers, and the time interval between chemoradiotherapy and surgery.
“We obviously need more data to evaluate other predictive factors in achieving a complete pathological response,” he said, adding that it’s also unclear whether the results of the present study could be generalized to institutions not participating in ACS NSQIP.
Dr. Salama presented the research on behalf of Nathalie Wong-Chong, MD, also of McGill University. He had no conflicts of interest to report for his presentation.
Orlando – Clinical an analysis of a large, multicenter database has suggested.
In multivariate regression, pretreatment N2 stage was the only variable significantly associated with failure of achieving pathologic complete response, according to Ebram Salama, MD, of Sir Mortimer B. Davis Jewish General Hospital at McGill University, Montreal.
“We should be reconsidering putting these patients in watch-and-wait protocols,” Dr. Salama said in an oral abstract presentation at the American College of Surgeons Quality and Safety Conference.
The analysis included 369 elective cases of cT2-4 N0-2 rectal cancer that were treated with neoadjuvant chemoradiotherapy during 2016 from the American College of Surgeons National Surgical Quality Improvement Program (NSQIP) proctectomy-specific database.
Of those cases, 53 (14.4%) achieved PCR, a proportion consistent with what has been reported previously in medical literature, Dr. Salama noted during his presentation.
The multivariate analysis revealed that pretreatment N2 stage was a negative predictor of PCR with an odds ratio of 0.18 (95% confidence interval, 0.04-0.82; P = .026), according to presented data.
By contrast, Dr. Salama said, there were no significant associations between response and other variables, including pretreatment N1 stage, pretreatment T stage, tumor location, gender, or body mass index.
Dr. Salama acknowledged limitations of this retrospective study, including a lack of data on other variables of interest, such as carcinoembryonic antigen, tumor size, imaging characteristics, molecular markers, and the time interval between chemoradiotherapy and surgery.
“We obviously need more data to evaluate other predictive factors in achieving a complete pathological response,” he said, adding that it’s also unclear whether the results of the present study could be generalized to institutions not participating in ACS NSQIP.
Dr. Salama presented the research on behalf of Nathalie Wong-Chong, MD, also of McGill University. He had no conflicts of interest to report for his presentation.
Orlando – Clinical an analysis of a large, multicenter database has suggested.
In multivariate regression, pretreatment N2 stage was the only variable significantly associated with failure of achieving pathologic complete response, according to Ebram Salama, MD, of Sir Mortimer B. Davis Jewish General Hospital at McGill University, Montreal.
“We should be reconsidering putting these patients in watch-and-wait protocols,” Dr. Salama said in an oral abstract presentation at the American College of Surgeons Quality and Safety Conference.
The analysis included 369 elective cases of cT2-4 N0-2 rectal cancer that were treated with neoadjuvant chemoradiotherapy during 2016 from the American College of Surgeons National Surgical Quality Improvement Program (NSQIP) proctectomy-specific database.
Of those cases, 53 (14.4%) achieved PCR, a proportion consistent with what has been reported previously in medical literature, Dr. Salama noted during his presentation.
The multivariate analysis revealed that pretreatment N2 stage was a negative predictor of PCR with an odds ratio of 0.18 (95% confidence interval, 0.04-0.82; P = .026), according to presented data.
By contrast, Dr. Salama said, there were no significant associations between response and other variables, including pretreatment N1 stage, pretreatment T stage, tumor location, gender, or body mass index.
Dr. Salama acknowledged limitations of this retrospective study, including a lack of data on other variables of interest, such as carcinoembryonic antigen, tumor size, imaging characteristics, molecular markers, and the time interval between chemoradiotherapy and surgery.
“We obviously need more data to evaluate other predictive factors in achieving a complete pathological response,” he said, adding that it’s also unclear whether the results of the present study could be generalized to institutions not participating in ACS NSQIP.
Dr. Salama presented the research on behalf of Nathalie Wong-Chong, MD, also of McGill University. He had no conflicts of interest to report for his presentation.
REPORTING FROM ACSQSC 2018
Key clinical point: N2 disease may be a negative predictor of pathological complete response after neoadjuvant chemoradiotherapy for rectal cancer.
Major finding: Pretreatment N2 stage was a negative predictor of complete pathological response, with an odds ratio of 0.18 (95% confidence interval, 0.04-0.82; P = .026).
Study details: A study of 369 elective cases of cT2-4 N0-2 rectal cancer treated with neoadjuvant chemoradiotherapy from 2016 in the ACS NSQIP proctectomy-specific database.
Disclosures: Dr. Salama had no conflicts of interest to report for his presentation.
Breast cancer patients don’t get the financial counseling they want from their clinicians
About half of medical oncologists – and even fewer surgeons and radiation oncologists – have someone in their practice to discuss the financial implications of treating breast cancer, a physician-patient survey has found.
Patients are feeling that lack of service, too; 73% of women in the survey said their providers didn’t offer much, or even any, help in tackling the potentially devastating financial impact of their cancer. Women reported a variety of these issues, including increased debt, lost time at work, skimping on their food budget, and even losing their homes as the medical bills added up.
“The privations observed in the current study are sobering and consistent with studies published before the widespread awareness of the potential for financial toxicity after the diagnosis and treatment of cancer,” wrote Reshma Jagsi, MD, and coauthors. The report was published in Cancer.
“… Unfortunately, unmet needs for discussion persist, as does unresolved worry. The percentage of patients who perceive meaningful clinician engagement is low, with far fewer than one-quarter of respondents reporting more than a little discussion of these issues, which is strikingly lower than the percentage of providers who perceive routinely making services available,” they wrote.
Dr. Jagsi, of the University of Michigan, Ann Arbor, and her colleagues used the Surveillance, Epidemiology, and End Results (SEER) database to identify 2,502 women in Georgia and Los Angeles County who were diagnosed with early-stage breast cancer from 2013 to 2015. They contacted these women, who were at least 1 year out from diagnosis, and their oncology providers with a survey designed to determine how both groups communicated about financial issues, and how those issues affected patients’ day-to-day lives.
Most of the clinicians were surgeons (370); the rest were medical oncologists (306) or radiation oncologists (169). About a quarter of each group was in a teaching practice.
Among the medical oncologists, 50.9% reported that someone in their practice often or always discussed financial burden with patients, as did 15.6% of surgeons and 43.2% of radiation oncologists. Medical oncologists were also more likely to respond that they were very aware of out-of-pocket costs for patients, as did 27.3% of surgeons and 34.3% of radiation oncologists.
About 57% of medical oncologists thought it was quite or extremely important to save their patients money; 35.3% of surgeons and 55.8% of radiation oncologists also responded so.
Many women reported at least some measure of financial toxicity related to their cancer and its treatment, and this varied widely by ethnicity and race. Debt was common, noted by 58.9% of black patients, 33.5% of Latina patients, and about 28% of both white and Asian patients.
“Many patients also had substantial lost income and out-of-pocket expenses that they attributed to breast cancer,” the authors wrote. “Overall, 14% of patients reported lost income that was [at least] 10% of their household income, 17% of patients reported spending [at least] 10% of household income on out-of-pocket medical expenses, and 7% of patients reported spending [at least] 10% of household income on out-of-pocket nonmedical expenses.
Housing loss attributed to breast cancer was most common among blacks (6%) and Latinas (4.7%), and less so among whites and Asians (about 1% each).
Blacks and Latinas also were more likely to report a utility disconnection due to unpaid bills (5.9% and 3.2%, respectively) compared with whites and Asians (1.7% and 0.5%).
One way women financially coped, the survey found, was to cut the food budget. “One in five whites [21.5%] and Asians [22.5%] cut down spending on food, as did nearly one-half of black individuals [45.2%] and greater than one-third of Latinas [35.8%].”
Worry about finances was most common among blacks and Latinas (about 50%), but about a third of white and Asian women also reported worry. Survey results suggested that clinicians were not addressing these issues.
Women – especially nonwhite women – wanted to have these talks, with 15.2% of whites, 31.1% of blacks, 30.3% of Latinas, and 25.4% of Asians reporting this desire.
“Unmet patient needs for engagement with physicians regarding financial concerns were common. Of the 945 women who expressed worrying at least somewhat, 679 (72.8%) indicated that cancer physicians and their staff did not help at least somewhat,” the authors said.
More than half of the 523 women who expressed a desire to talk to health care providers regarding the impact of breast cancer on employment or finances (55.4%) reported that this discussion never took place, either with the oncologist, primary care provider, social worker, or any other professional involved in their care.
A multivariate analysis examined patient characteristics associated with the desire to discuss financial toxicity with a health care provider. Younger age, nonwhite race, lower income, being employed, receiving chemotherapy, and living in Georgia all showed significant, independent interaction.
“Given these findings, it is clear that thoughtfully designed, prospective interventions are necessary to address the remarkably common experiences of financial burden that patients report even in the modern era,” the investigators wrote. “These interventions might include training for physicians and their staff regarding how to have effective conversations in this context, in ways that are sensitive to cultural differences and needs. Other promising approaches might include the use of advanced technology to engage patients in interactive exercises that elicit their financial concerns and experiences and alert providers to their needs.”
The study was largely funded by a grant from the National Cancer Institute and the University of Michigan. Dr. Jagsi disclosed that she has been a consultant for Amgen but not relative to this study.
SOURCE: Jagsi R et al. Cancer 2018 Jul 23. doi: 10.1002/cncr.31532.
About half of medical oncologists – and even fewer surgeons and radiation oncologists – have someone in their practice to discuss the financial implications of treating breast cancer, a physician-patient survey has found.
Patients are feeling that lack of service, too; 73% of women in the survey said their providers didn’t offer much, or even any, help in tackling the potentially devastating financial impact of their cancer. Women reported a variety of these issues, including increased debt, lost time at work, skimping on their food budget, and even losing their homes as the medical bills added up.
“The privations observed in the current study are sobering and consistent with studies published before the widespread awareness of the potential for financial toxicity after the diagnosis and treatment of cancer,” wrote Reshma Jagsi, MD, and coauthors. The report was published in Cancer.
“… Unfortunately, unmet needs for discussion persist, as does unresolved worry. The percentage of patients who perceive meaningful clinician engagement is low, with far fewer than one-quarter of respondents reporting more than a little discussion of these issues, which is strikingly lower than the percentage of providers who perceive routinely making services available,” they wrote.
Dr. Jagsi, of the University of Michigan, Ann Arbor, and her colleagues used the Surveillance, Epidemiology, and End Results (SEER) database to identify 2,502 women in Georgia and Los Angeles County who were diagnosed with early-stage breast cancer from 2013 to 2015. They contacted these women, who were at least 1 year out from diagnosis, and their oncology providers with a survey designed to determine how both groups communicated about financial issues, and how those issues affected patients’ day-to-day lives.
Most of the clinicians were surgeons (370); the rest were medical oncologists (306) or radiation oncologists (169). About a quarter of each group was in a teaching practice.
Among the medical oncologists, 50.9% reported that someone in their practice often or always discussed financial burden with patients, as did 15.6% of surgeons and 43.2% of radiation oncologists. Medical oncologists were also more likely to respond that they were very aware of out-of-pocket costs for patients, as did 27.3% of surgeons and 34.3% of radiation oncologists.
About 57% of medical oncologists thought it was quite or extremely important to save their patients money; 35.3% of surgeons and 55.8% of radiation oncologists also responded so.
Many women reported at least some measure of financial toxicity related to their cancer and its treatment, and this varied widely by ethnicity and race. Debt was common, noted by 58.9% of black patients, 33.5% of Latina patients, and about 28% of both white and Asian patients.
“Many patients also had substantial lost income and out-of-pocket expenses that they attributed to breast cancer,” the authors wrote. “Overall, 14% of patients reported lost income that was [at least] 10% of their household income, 17% of patients reported spending [at least] 10% of household income on out-of-pocket medical expenses, and 7% of patients reported spending [at least] 10% of household income on out-of-pocket nonmedical expenses.
Housing loss attributed to breast cancer was most common among blacks (6%) and Latinas (4.7%), and less so among whites and Asians (about 1% each).
Blacks and Latinas also were more likely to report a utility disconnection due to unpaid bills (5.9% and 3.2%, respectively) compared with whites and Asians (1.7% and 0.5%).
One way women financially coped, the survey found, was to cut the food budget. “One in five whites [21.5%] and Asians [22.5%] cut down spending on food, as did nearly one-half of black individuals [45.2%] and greater than one-third of Latinas [35.8%].”
Worry about finances was most common among blacks and Latinas (about 50%), but about a third of white and Asian women also reported worry. Survey results suggested that clinicians were not addressing these issues.
Women – especially nonwhite women – wanted to have these talks, with 15.2% of whites, 31.1% of blacks, 30.3% of Latinas, and 25.4% of Asians reporting this desire.
“Unmet patient needs for engagement with physicians regarding financial concerns were common. Of the 945 women who expressed worrying at least somewhat, 679 (72.8%) indicated that cancer physicians and their staff did not help at least somewhat,” the authors said.
More than half of the 523 women who expressed a desire to talk to health care providers regarding the impact of breast cancer on employment or finances (55.4%) reported that this discussion never took place, either with the oncologist, primary care provider, social worker, or any other professional involved in their care.
A multivariate analysis examined patient characteristics associated with the desire to discuss financial toxicity with a health care provider. Younger age, nonwhite race, lower income, being employed, receiving chemotherapy, and living in Georgia all showed significant, independent interaction.
“Given these findings, it is clear that thoughtfully designed, prospective interventions are necessary to address the remarkably common experiences of financial burden that patients report even in the modern era,” the investigators wrote. “These interventions might include training for physicians and their staff regarding how to have effective conversations in this context, in ways that are sensitive to cultural differences and needs. Other promising approaches might include the use of advanced technology to engage patients in interactive exercises that elicit their financial concerns and experiences and alert providers to their needs.”
The study was largely funded by a grant from the National Cancer Institute and the University of Michigan. Dr. Jagsi disclosed that she has been a consultant for Amgen but not relative to this study.
SOURCE: Jagsi R et al. Cancer 2018 Jul 23. doi: 10.1002/cncr.31532.
About half of medical oncologists – and even fewer surgeons and radiation oncologists – have someone in their practice to discuss the financial implications of treating breast cancer, a physician-patient survey has found.
Patients are feeling that lack of service, too; 73% of women in the survey said their providers didn’t offer much, or even any, help in tackling the potentially devastating financial impact of their cancer. Women reported a variety of these issues, including increased debt, lost time at work, skimping on their food budget, and even losing their homes as the medical bills added up.
“The privations observed in the current study are sobering and consistent with studies published before the widespread awareness of the potential for financial toxicity after the diagnosis and treatment of cancer,” wrote Reshma Jagsi, MD, and coauthors. The report was published in Cancer.
“… Unfortunately, unmet needs for discussion persist, as does unresolved worry. The percentage of patients who perceive meaningful clinician engagement is low, with far fewer than one-quarter of respondents reporting more than a little discussion of these issues, which is strikingly lower than the percentage of providers who perceive routinely making services available,” they wrote.
Dr. Jagsi, of the University of Michigan, Ann Arbor, and her colleagues used the Surveillance, Epidemiology, and End Results (SEER) database to identify 2,502 women in Georgia and Los Angeles County who were diagnosed with early-stage breast cancer from 2013 to 2015. They contacted these women, who were at least 1 year out from diagnosis, and their oncology providers with a survey designed to determine how both groups communicated about financial issues, and how those issues affected patients’ day-to-day lives.
Most of the clinicians were surgeons (370); the rest were medical oncologists (306) or radiation oncologists (169). About a quarter of each group was in a teaching practice.
Among the medical oncologists, 50.9% reported that someone in their practice often or always discussed financial burden with patients, as did 15.6% of surgeons and 43.2% of radiation oncologists. Medical oncologists were also more likely to respond that they were very aware of out-of-pocket costs for patients, as did 27.3% of surgeons and 34.3% of radiation oncologists.
About 57% of medical oncologists thought it was quite or extremely important to save their patients money; 35.3% of surgeons and 55.8% of radiation oncologists also responded so.
Many women reported at least some measure of financial toxicity related to their cancer and its treatment, and this varied widely by ethnicity and race. Debt was common, noted by 58.9% of black patients, 33.5% of Latina patients, and about 28% of both white and Asian patients.
“Many patients also had substantial lost income and out-of-pocket expenses that they attributed to breast cancer,” the authors wrote. “Overall, 14% of patients reported lost income that was [at least] 10% of their household income, 17% of patients reported spending [at least] 10% of household income on out-of-pocket medical expenses, and 7% of patients reported spending [at least] 10% of household income on out-of-pocket nonmedical expenses.
Housing loss attributed to breast cancer was most common among blacks (6%) and Latinas (4.7%), and less so among whites and Asians (about 1% each).
Blacks and Latinas also were more likely to report a utility disconnection due to unpaid bills (5.9% and 3.2%, respectively) compared with whites and Asians (1.7% and 0.5%).
One way women financially coped, the survey found, was to cut the food budget. “One in five whites [21.5%] and Asians [22.5%] cut down spending on food, as did nearly one-half of black individuals [45.2%] and greater than one-third of Latinas [35.8%].”
Worry about finances was most common among blacks and Latinas (about 50%), but about a third of white and Asian women also reported worry. Survey results suggested that clinicians were not addressing these issues.
Women – especially nonwhite women – wanted to have these talks, with 15.2% of whites, 31.1% of blacks, 30.3% of Latinas, and 25.4% of Asians reporting this desire.
“Unmet patient needs for engagement with physicians regarding financial concerns were common. Of the 945 women who expressed worrying at least somewhat, 679 (72.8%) indicated that cancer physicians and their staff did not help at least somewhat,” the authors said.
More than half of the 523 women who expressed a desire to talk to health care providers regarding the impact of breast cancer on employment or finances (55.4%) reported that this discussion never took place, either with the oncologist, primary care provider, social worker, or any other professional involved in their care.
A multivariate analysis examined patient characteristics associated with the desire to discuss financial toxicity with a health care provider. Younger age, nonwhite race, lower income, being employed, receiving chemotherapy, and living in Georgia all showed significant, independent interaction.
“Given these findings, it is clear that thoughtfully designed, prospective interventions are necessary to address the remarkably common experiences of financial burden that patients report even in the modern era,” the investigators wrote. “These interventions might include training for physicians and their staff regarding how to have effective conversations in this context, in ways that are sensitive to cultural differences and needs. Other promising approaches might include the use of advanced technology to engage patients in interactive exercises that elicit their financial concerns and experiences and alert providers to their needs.”
The study was largely funded by a grant from the National Cancer Institute and the University of Michigan. Dr. Jagsi disclosed that she has been a consultant for Amgen but not relative to this study.
SOURCE: Jagsi R et al. Cancer 2018 Jul 23. doi: 10.1002/cncr.31532.
FROM CANCER
Key clinical point: Oncology care providers aren’t providing adequate financial counseling for patients with breast cancer.
Major finding: Half of medical oncologists say they don’t have a staff member routinely discuss the financial impact of breast cancer, and 73% of patients say they’ve never had this discussion with their doctor.
Study details: The survey comprised 2,502 patients and 845 physicians.
Disclosures: The study was largely funded by a grant from the National Cancer Institute and the University of Michigan. Dr. Jagsi disclosed that she has been a consultant for Amgen but not relative to this study.
Source: Jagsi R et al. Cancer 2018 Jul 23. doi: 10.1002/cncr.31532.
PREOPANC-1: Early findings suggest benefit with preop chemo in pancreatic cancer
CHICAGO – Preoperative chemotherapy improves outcomes in patients with resectable or borderline resectable pancreatic cancer, preliminary findings from the phase 3 PREOPANC-1 trial suggest.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Overall survival in 127 patients randomized to immediate surgery followed by adjuvant chemotherapy was 13.7 months vs. 17.1 months in 119 patients randomized to receive preoperative chemoradiotherapy and postoperative adjuvant chemotherapy, Geertjan van Tienhoven, MD, PhD, reported at the annual meeting of the American Society of Clinical Oncology.
The difference did not quite reach statistical significance, but final analysis requires an additional 26 events, Dr. van Tienhoven of Academic Medical Center, Amsterdam explained in a video interview at the meeting.
Other differences between the groups, which included disease-free survival, local control, and metastasis-free survival, did differ significantly in favor of preoperative chemotherapy, he said.
Of note, 72% and 62% of patients in the immediate surgery and preoperative chemoradiotherapy groups, respectively, underwent resection and a greater proportion of patients in the latter group achieved microscopically complete resection, he said (63% vs. 31%).
Should these results hold up in the final analysis, particularly if the difference in overall survival reaches statistical significance, “then this is a proof of principle and practice-changing trial,” Dr. van Tienhoven said.
Dr. van Tienhoven reported having no disclosures.
SOURCE: van Tienhoven et al. ASCO 2108, Abstract LBA4002.
CHICAGO – Preoperative chemotherapy improves outcomes in patients with resectable or borderline resectable pancreatic cancer, preliminary findings from the phase 3 PREOPANC-1 trial suggest.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Overall survival in 127 patients randomized to immediate surgery followed by adjuvant chemotherapy was 13.7 months vs. 17.1 months in 119 patients randomized to receive preoperative chemoradiotherapy and postoperative adjuvant chemotherapy, Geertjan van Tienhoven, MD, PhD, reported at the annual meeting of the American Society of Clinical Oncology.
The difference did not quite reach statistical significance, but final analysis requires an additional 26 events, Dr. van Tienhoven of Academic Medical Center, Amsterdam explained in a video interview at the meeting.
Other differences between the groups, which included disease-free survival, local control, and metastasis-free survival, did differ significantly in favor of preoperative chemotherapy, he said.
Of note, 72% and 62% of patients in the immediate surgery and preoperative chemoradiotherapy groups, respectively, underwent resection and a greater proportion of patients in the latter group achieved microscopically complete resection, he said (63% vs. 31%).
Should these results hold up in the final analysis, particularly if the difference in overall survival reaches statistical significance, “then this is a proof of principle and practice-changing trial,” Dr. van Tienhoven said.
Dr. van Tienhoven reported having no disclosures.
SOURCE: van Tienhoven et al. ASCO 2108, Abstract LBA4002.
CHICAGO – Preoperative chemotherapy improves outcomes in patients with resectable or borderline resectable pancreatic cancer, preliminary findings from the phase 3 PREOPANC-1 trial suggest.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Overall survival in 127 patients randomized to immediate surgery followed by adjuvant chemotherapy was 13.7 months vs. 17.1 months in 119 patients randomized to receive preoperative chemoradiotherapy and postoperative adjuvant chemotherapy, Geertjan van Tienhoven, MD, PhD, reported at the annual meeting of the American Society of Clinical Oncology.
The difference did not quite reach statistical significance, but final analysis requires an additional 26 events, Dr. van Tienhoven of Academic Medical Center, Amsterdam explained in a video interview at the meeting.
Other differences between the groups, which included disease-free survival, local control, and metastasis-free survival, did differ significantly in favor of preoperative chemotherapy, he said.
Of note, 72% and 62% of patients in the immediate surgery and preoperative chemoradiotherapy groups, respectively, underwent resection and a greater proportion of patients in the latter group achieved microscopically complete resection, he said (63% vs. 31%).
Should these results hold up in the final analysis, particularly if the difference in overall survival reaches statistical significance, “then this is a proof of principle and practice-changing trial,” Dr. van Tienhoven said.
Dr. van Tienhoven reported having no disclosures.
SOURCE: van Tienhoven et al. ASCO 2108, Abstract LBA4002.
REPORTING FROM ASCO 2018
Study eyes liver transplantation after Region 5 UNOS downstaging
Liver transplantation led to “excellent outcomes” when performed after downstaging hepatocellular carcinoma using the UNOS (United Network for Organ Sharing) Region 5 protocol, investigators reported.
Downstaging succeeded for 58% of patients, and an estimated 87% of transplantation recipients were alive and recurrence free at 5 years, said Neil Mehta, MD, of the University of California, San Francisco, and his associates. The findings support expanding priority access to liver transplantation to include patients whose hepatocellular carcinoma (HCC) has been successfully downstaged, they said. “In the meantime, UNOS has recently approved the Region 5 downstaging protocol for receiving automatic HCC-MELD exception listing,” they wrote. The report was published in the June issue of Clinical Gastroenterology and Hepatology (doi: 10.1016/j.cgh.2017.11.037).
This is the first multicenter study of HCC downstaging according to a uniform protocol, the researchers noted. In multivariable analyses, downstaging was significantly more likely to fail in the setting of moderate to severe (Child Pugh B or C) hepatic impairment (hazard ratio, 3.3; 95% confidence interval, 3.0 to 3.6; P less than .001) or baseline alpha-fetoprotein level above 1,000 ng/mL (HR, 1.6; 95% CI, 1.4 to 1.9; P less than .001).
The incidence of HCC in the United States is expected to keep rising for at least another decade because of epidemic levels of fatty liver disease and chronic hepatitis C, the investigators noted. Downstaging HCC with local-regional therapy is a common bridge to transplantation, and successful treatment tends to reflect favorable tumor biology, which bodes well for transplantation. However, no multicenter study had evaluated these associations. Therefore, the investigators retrospectively studied 187 patients with HCC from three centers in California who underwent downstaging according to the UNOS Region 5 protocol between 2002 and 2012.
A total of 156 patients (83%) were successfully downstaged to within Milan criteria after a median of 2.7 months (interquartile range, 1.4 to 4.9 months), said the researchers. Among patients who were successfully downstaged but did not undergo transplantation, 37 patients had tumor progression or died from liver-related causes after a median of 6 months, while 10 patients remained on the transplant list. Among the 109 patients who underwent transplantation after a median of 13 months (interquartile range 6 to 19 months), median follow-up time was 4.3 years and estimated 5-year survival was 80%, and estimated recurrence-free survival was 87%.
Fully 68% of successfully downstaged patients required only one local-regional treatment, the researchers said. The Region 5 protocol considers patients eligible for downstaging if they have a single HCC lesion measuring up to 8 cm or multiple lesions whose combined diameters do not exceed 8 cm, and no evidence of extrahepatic disease or vascular invasion on multiphase computed tomography or magnetic resonance imaging.
The protocol considers downstaging successful if it results in one lesion measuring up to 5 cm or no more than three lesions of up to 3 cm each. Thus, patients who start out with four or five lesions must have complete necrosis of at least one to two tumors. Successfully downstaged patients must remain free of acute hepatic decompensation for at least 3 consecutive months before undergoing transplantation, according to the protocol.
“Slight refinements in the inclusion criteria for downstaging seem warranted [given] that all Child’s B/C patients with pretreatment alpha-fetoprotein greater than 1000 ng/mL suffered poor outcomes when downstaging was attempted,” the investigators noted. They reported that the 1-year risk of failed downstaging was 70% among patients with both Child’s B/C cirrhosis and alpha-fetoprotein level at or above 1000 ng/mL, 32% among patients with one risk factor, and 14% among patients with no risk factors (P less than .001).
The National Institutes of Health provided partial funding. The investigators reported having no conflicts of interest.
SOURCE: Mehta N, et al. Clin Gastroenterol Hepatol. 2017 Nov 23. doi: 10.1016/j.cgh.2017.11.037.
Liver transplantation of selected patients with hepatocellular carcinoma (HCC) is an accepted indication and associated with excellent outcomes. Until recently, criteria for liver transplantation were based on the Milan criteria that only took size and number of tumors under consideration. In this multicenter study, patients who were outside of Milan criteria were successfully downstaged to within Milan criteria with locoregional therapy and subsequently transplanted with excellent outcomes. Salient features included the following. 1) Six months waiting after the first treatment and 3 months after downstaging was required to ensure that the tumor stage remained within Milan criteria. 2) Any specific type of locoregional therapy was allowed. 3) Downstaging was possible in a majority of patients after a single treatment. 4) Patients with alpha-fetoprotein greater than 1000 ng/mL (approximately 10%) as well as presence of substantial decompensated liver disease (approximately 40%) did not have favorable outcomes. 4) On multivariable analysis, tumor biology was a stronger predictor of poor outcomes than was stage of liver disease.
Sumeet K. Asrani, MD, MSc, is associate professor in medicine and hepatologist at Baylor University Medical Center, and medical director of the Center for Advanced Liver Disease, Dallas. He has no conflicts of interest.
Liver transplantation of selected patients with hepatocellular carcinoma (HCC) is an accepted indication and associated with excellent outcomes. Until recently, criteria for liver transplantation were based on the Milan criteria that only took size and number of tumors under consideration. In this multicenter study, patients who were outside of Milan criteria were successfully downstaged to within Milan criteria with locoregional therapy and subsequently transplanted with excellent outcomes. Salient features included the following. 1) Six months waiting after the first treatment and 3 months after downstaging was required to ensure that the tumor stage remained within Milan criteria. 2) Any specific type of locoregional therapy was allowed. 3) Downstaging was possible in a majority of patients after a single treatment. 4) Patients with alpha-fetoprotein greater than 1000 ng/mL (approximately 10%) as well as presence of substantial decompensated liver disease (approximately 40%) did not have favorable outcomes. 4) On multivariable analysis, tumor biology was a stronger predictor of poor outcomes than was stage of liver disease.
Sumeet K. Asrani, MD, MSc, is associate professor in medicine and hepatologist at Baylor University Medical Center, and medical director of the Center for Advanced Liver Disease, Dallas. He has no conflicts of interest.
Liver transplantation of selected patients with hepatocellular carcinoma (HCC) is an accepted indication and associated with excellent outcomes. Until recently, criteria for liver transplantation were based on the Milan criteria that only took size and number of tumors under consideration. In this multicenter study, patients who were outside of Milan criteria were successfully downstaged to within Milan criteria with locoregional therapy and subsequently transplanted with excellent outcomes. Salient features included the following. 1) Six months waiting after the first treatment and 3 months after downstaging was required to ensure that the tumor stage remained within Milan criteria. 2) Any specific type of locoregional therapy was allowed. 3) Downstaging was possible in a majority of patients after a single treatment. 4) Patients with alpha-fetoprotein greater than 1000 ng/mL (approximately 10%) as well as presence of substantial decompensated liver disease (approximately 40%) did not have favorable outcomes. 4) On multivariable analysis, tumor biology was a stronger predictor of poor outcomes than was stage of liver disease.
Sumeet K. Asrani, MD, MSc, is associate professor in medicine and hepatologist at Baylor University Medical Center, and medical director of the Center for Advanced Liver Disease, Dallas. He has no conflicts of interest.
Liver transplantation led to “excellent outcomes” when performed after downstaging hepatocellular carcinoma using the UNOS (United Network for Organ Sharing) Region 5 protocol, investigators reported.
Downstaging succeeded for 58% of patients, and an estimated 87% of transplantation recipients were alive and recurrence free at 5 years, said Neil Mehta, MD, of the University of California, San Francisco, and his associates. The findings support expanding priority access to liver transplantation to include patients whose hepatocellular carcinoma (HCC) has been successfully downstaged, they said. “In the meantime, UNOS has recently approved the Region 5 downstaging protocol for receiving automatic HCC-MELD exception listing,” they wrote. The report was published in the June issue of Clinical Gastroenterology and Hepatology (doi: 10.1016/j.cgh.2017.11.037).
This is the first multicenter study of HCC downstaging according to a uniform protocol, the researchers noted. In multivariable analyses, downstaging was significantly more likely to fail in the setting of moderate to severe (Child Pugh B or C) hepatic impairment (hazard ratio, 3.3; 95% confidence interval, 3.0 to 3.6; P less than .001) or baseline alpha-fetoprotein level above 1,000 ng/mL (HR, 1.6; 95% CI, 1.4 to 1.9; P less than .001).
The incidence of HCC in the United States is expected to keep rising for at least another decade because of epidemic levels of fatty liver disease and chronic hepatitis C, the investigators noted. Downstaging HCC with local-regional therapy is a common bridge to transplantation, and successful treatment tends to reflect favorable tumor biology, which bodes well for transplantation. However, no multicenter study had evaluated these associations. Therefore, the investigators retrospectively studied 187 patients with HCC from three centers in California who underwent downstaging according to the UNOS Region 5 protocol between 2002 and 2012.
A total of 156 patients (83%) were successfully downstaged to within Milan criteria after a median of 2.7 months (interquartile range, 1.4 to 4.9 months), said the researchers. Among patients who were successfully downstaged but did not undergo transplantation, 37 patients had tumor progression or died from liver-related causes after a median of 6 months, while 10 patients remained on the transplant list. Among the 109 patients who underwent transplantation after a median of 13 months (interquartile range 6 to 19 months), median follow-up time was 4.3 years and estimated 5-year survival was 80%, and estimated recurrence-free survival was 87%.
Fully 68% of successfully downstaged patients required only one local-regional treatment, the researchers said. The Region 5 protocol considers patients eligible for downstaging if they have a single HCC lesion measuring up to 8 cm or multiple lesions whose combined diameters do not exceed 8 cm, and no evidence of extrahepatic disease or vascular invasion on multiphase computed tomography or magnetic resonance imaging.
The protocol considers downstaging successful if it results in one lesion measuring up to 5 cm or no more than three lesions of up to 3 cm each. Thus, patients who start out with four or five lesions must have complete necrosis of at least one to two tumors. Successfully downstaged patients must remain free of acute hepatic decompensation for at least 3 consecutive months before undergoing transplantation, according to the protocol.
“Slight refinements in the inclusion criteria for downstaging seem warranted [given] that all Child’s B/C patients with pretreatment alpha-fetoprotein greater than 1000 ng/mL suffered poor outcomes when downstaging was attempted,” the investigators noted. They reported that the 1-year risk of failed downstaging was 70% among patients with both Child’s B/C cirrhosis and alpha-fetoprotein level at or above 1000 ng/mL, 32% among patients with one risk factor, and 14% among patients with no risk factors (P less than .001).
The National Institutes of Health provided partial funding. The investigators reported having no conflicts of interest.
SOURCE: Mehta N, et al. Clin Gastroenterol Hepatol. 2017 Nov 23. doi: 10.1016/j.cgh.2017.11.037.
Liver transplantation led to “excellent outcomes” when performed after downstaging hepatocellular carcinoma using the UNOS (United Network for Organ Sharing) Region 5 protocol, investigators reported.
Downstaging succeeded for 58% of patients, and an estimated 87% of transplantation recipients were alive and recurrence free at 5 years, said Neil Mehta, MD, of the University of California, San Francisco, and his associates. The findings support expanding priority access to liver transplantation to include patients whose hepatocellular carcinoma (HCC) has been successfully downstaged, they said. “In the meantime, UNOS has recently approved the Region 5 downstaging protocol for receiving automatic HCC-MELD exception listing,” they wrote. The report was published in the June issue of Clinical Gastroenterology and Hepatology (doi: 10.1016/j.cgh.2017.11.037).
This is the first multicenter study of HCC downstaging according to a uniform protocol, the researchers noted. In multivariable analyses, downstaging was significantly more likely to fail in the setting of moderate to severe (Child Pugh B or C) hepatic impairment (hazard ratio, 3.3; 95% confidence interval, 3.0 to 3.6; P less than .001) or baseline alpha-fetoprotein level above 1,000 ng/mL (HR, 1.6; 95% CI, 1.4 to 1.9; P less than .001).
The incidence of HCC in the United States is expected to keep rising for at least another decade because of epidemic levels of fatty liver disease and chronic hepatitis C, the investigators noted. Downstaging HCC with local-regional therapy is a common bridge to transplantation, and successful treatment tends to reflect favorable tumor biology, which bodes well for transplantation. However, no multicenter study had evaluated these associations. Therefore, the investigators retrospectively studied 187 patients with HCC from three centers in California who underwent downstaging according to the UNOS Region 5 protocol between 2002 and 2012.
A total of 156 patients (83%) were successfully downstaged to within Milan criteria after a median of 2.7 months (interquartile range, 1.4 to 4.9 months), said the researchers. Among patients who were successfully downstaged but did not undergo transplantation, 37 patients had tumor progression or died from liver-related causes after a median of 6 months, while 10 patients remained on the transplant list. Among the 109 patients who underwent transplantation after a median of 13 months (interquartile range 6 to 19 months), median follow-up time was 4.3 years and estimated 5-year survival was 80%, and estimated recurrence-free survival was 87%.
Fully 68% of successfully downstaged patients required only one local-regional treatment, the researchers said. The Region 5 protocol considers patients eligible for downstaging if they have a single HCC lesion measuring up to 8 cm or multiple lesions whose combined diameters do not exceed 8 cm, and no evidence of extrahepatic disease or vascular invasion on multiphase computed tomography or magnetic resonance imaging.
The protocol considers downstaging successful if it results in one lesion measuring up to 5 cm or no more than three lesions of up to 3 cm each. Thus, patients who start out with four or five lesions must have complete necrosis of at least one to two tumors. Successfully downstaged patients must remain free of acute hepatic decompensation for at least 3 consecutive months before undergoing transplantation, according to the protocol.
“Slight refinements in the inclusion criteria for downstaging seem warranted [given] that all Child’s B/C patients with pretreatment alpha-fetoprotein greater than 1000 ng/mL suffered poor outcomes when downstaging was attempted,” the investigators noted. They reported that the 1-year risk of failed downstaging was 70% among patients with both Child’s B/C cirrhosis and alpha-fetoprotein level at or above 1000 ng/mL, 32% among patients with one risk factor, and 14% among patients with no risk factors (P less than .001).
The National Institutes of Health provided partial funding. The investigators reported having no conflicts of interest.
SOURCE: Mehta N, et al. Clin Gastroenterol Hepatol. 2017 Nov 23. doi: 10.1016/j.cgh.2017.11.037.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Key clinical point: Liver transplantation led to excellent outcomes when performed after downstaging hepatocellular carcinoma according to the UNOS (United Network for Organ Sharing) Region 5 protocol.
Major finding: Downstaging succeeded in 58% of patients. Estimated 5-year posttransplantation recurrence-free survival was 87%.
Study details: Retrospective multicenter study of 187 patients with hepatocellular carcinoma.
Disclosures: The National Institutes of Health provided partial funding. The investigators reported having no conflicts of interest.
Source: Mehta N et al. Clin Gastroenterol Hepatol. 2017 Nov 23. doi: 10.1016/j.cgh.2017.11.037.
Palliative care may reduce suicide among lung cancer patients
according to new research that will be presented at an international conference of the American Thoracic Society.
“Suicide is a significant national public health problem, especially among lung cancer patients and among veterans,” said lead author, Donald R. Sullivan, MD, of the division of pulmonary and critical care medicine at Oregon Health & Science University and a member of the OHSU Knight Cancer Institute, in a statement.
The investigators found that veterans who experienced at least one “palliative care encounter” after learning they had lung cancer were 82% less likely to die by suicide (odds ratio, 0.18; 95% confidence interval, 0.07-0.46; P less than .001), when compared with veterans who were diagnosed with lung cancer but did not receive palliative care.
The suicide rate for the advanced-stage lung cancer patients was 200/100,000 patient-years, which was more than five times higher than the suicide rate – adjusted for age, sex, and year – for all veterans using VA health care (37.5/100,000), according to the study abstract.
Of the 20,900 lung cancer patients analyzed, 30 committed suicide. Only six (20%) of the patients who died by suicide had received palliative care. Overall, most patients (18,192 or 87%) in the registry died of lung cancer. Other cancers, heart disease, and chronic obstructive pulmonary disease were some of the other common causes of death for the lung cancer patients, according to the abstract.
While several medical societies recommend palliative care for all patients with advanced-stage lung cancer, there is a gap between those recommendations and practice, noted Dr. Sullivan. “There are many barriers to palliative care, and unfortunately, some are related to clinician referrals. Not all doctors are aware of the benefits of palliative care,” he said in the statement.
Dr. Sullivan added that palliative care should be offered to all patients shortly after receiving a diagnosis of advanced-stage lung cancer.
More details on this study will be presented at the conference on Monday, May 21, at 2:30 p.m. in Room 14 A-B (Mezzanine Level) of the San Diego Convention Center.
according to new research that will be presented at an international conference of the American Thoracic Society.
“Suicide is a significant national public health problem, especially among lung cancer patients and among veterans,” said lead author, Donald R. Sullivan, MD, of the division of pulmonary and critical care medicine at Oregon Health & Science University and a member of the OHSU Knight Cancer Institute, in a statement.
The investigators found that veterans who experienced at least one “palliative care encounter” after learning they had lung cancer were 82% less likely to die by suicide (odds ratio, 0.18; 95% confidence interval, 0.07-0.46; P less than .001), when compared with veterans who were diagnosed with lung cancer but did not receive palliative care.
The suicide rate for the advanced-stage lung cancer patients was 200/100,000 patient-years, which was more than five times higher than the suicide rate – adjusted for age, sex, and year – for all veterans using VA health care (37.5/100,000), according to the study abstract.
Of the 20,900 lung cancer patients analyzed, 30 committed suicide. Only six (20%) of the patients who died by suicide had received palliative care. Overall, most patients (18,192 or 87%) in the registry died of lung cancer. Other cancers, heart disease, and chronic obstructive pulmonary disease were some of the other common causes of death for the lung cancer patients, according to the abstract.
While several medical societies recommend palliative care for all patients with advanced-stage lung cancer, there is a gap between those recommendations and practice, noted Dr. Sullivan. “There are many barriers to palliative care, and unfortunately, some are related to clinician referrals. Not all doctors are aware of the benefits of palliative care,” he said in the statement.
Dr. Sullivan added that palliative care should be offered to all patients shortly after receiving a diagnosis of advanced-stage lung cancer.
More details on this study will be presented at the conference on Monday, May 21, at 2:30 p.m. in Room 14 A-B (Mezzanine Level) of the San Diego Convention Center.
according to new research that will be presented at an international conference of the American Thoracic Society.
“Suicide is a significant national public health problem, especially among lung cancer patients and among veterans,” said lead author, Donald R. Sullivan, MD, of the division of pulmonary and critical care medicine at Oregon Health & Science University and a member of the OHSU Knight Cancer Institute, in a statement.
The investigators found that veterans who experienced at least one “palliative care encounter” after learning they had lung cancer were 82% less likely to die by suicide (odds ratio, 0.18; 95% confidence interval, 0.07-0.46; P less than .001), when compared with veterans who were diagnosed with lung cancer but did not receive palliative care.
The suicide rate for the advanced-stage lung cancer patients was 200/100,000 patient-years, which was more than five times higher than the suicide rate – adjusted for age, sex, and year – for all veterans using VA health care (37.5/100,000), according to the study abstract.
Of the 20,900 lung cancer patients analyzed, 30 committed suicide. Only six (20%) of the patients who died by suicide had received palliative care. Overall, most patients (18,192 or 87%) in the registry died of lung cancer. Other cancers, heart disease, and chronic obstructive pulmonary disease were some of the other common causes of death for the lung cancer patients, according to the abstract.
While several medical societies recommend palliative care for all patients with advanced-stage lung cancer, there is a gap between those recommendations and practice, noted Dr. Sullivan. “There are many barriers to palliative care, and unfortunately, some are related to clinician referrals. Not all doctors are aware of the benefits of palliative care,” he said in the statement.
Dr. Sullivan added that palliative care should be offered to all patients shortly after receiving a diagnosis of advanced-stage lung cancer.
More details on this study will be presented at the conference on Monday, May 21, at 2:30 p.m. in Room 14 A-B (Mezzanine Level) of the San Diego Convention Center.
FROM ATS 2018
Delay of NSCLC surgery can lead to worse prognosis
SAN DIEGO – Delaying
“There is significant upstaging with time from completion of clinical staging to surgical resection, with a 4% increase of upstaging per week for the overall study population,” said study coauthor Harmik J. Soukiasian, MD, FACS, of Cedars-Sinai Medical Center, Los Angeles, in an interview. “Upstaging impacts lung cancer prognosis as more advanced stages portend to a poorer prognosis.”
An estimated 80%-85% of lung cancer patients have NSCLC, according to the American Cancer Society, and Dr. Soukiasian said surgery offers a chance at a cure for those diagnosed at stage I.
“National Cancer Comprehensive Network (NCCN) Guidelines recommend surgery within 8 weeks of completed clinical staging for NSCLC to limit cancer progression or upstaging,” Dr. Soukiasian said. “Although these guidelines are well established and widely adopted, our study performs a more granular analysis, studying time as a predictor of upstaging for those patients diagnosed with stage I NSCLC.”
For the new study, Dr. Soukiasian and colleagues tracked 52,406 patients in a cancer database who had stage I NSCLC but had not undergone preoperative chemotherapy. The researchers tracked their clinical stages for up to 12 weeks from initial staging.
Researchers found that, while staging levels rose with each successive week, just 25% of patients underwent surgery by 1 week, and only 79% had surgery in accordance with NSCLC guidelines by week 8. At 12 weeks, 9% had still not undergone surgery.
Upstaging was common: 22% at 1 week, 32% after 8 weeks, and 33% after 12 weeks.
“We demonstrate that patients diagnosed with stage I NSCLC benefit from surgery sooner than the 8-week window recommended by the NCCN guidelines,” Dr. Soukiasian said. “Exclusive of the rate of progression and in addition to time to surgery, our study also demonstrated academic centers, higher lymph node yield during surgery, and left-sided tumors to be independent predictors of upstaging.”
The study design doesn’t provide insight into why surgery is often delayed. However, “we can theorize factors associated with delays to surgery may be due to patient factors (personal scheduling, availability of support systems, etc.), delays in follow up, operating room availability or scheduling, and issues with insurance approval,” Dr. Soukiasian said.
In his presentation, Dr. Soukiasian emphasized the role of the mediastinum. “Given the clinical impact of stage III disease, we analyzed upstaging rates of stage I NSCLC to stage IIIA and revealed a 1.3% increase per week of upstaging specifically to stage IIIA. Additionally, almost 5% of patients initially diagnosed with stage I NSCLC upstaged to IIIA disease. The significant rate of upstaging to IIIA disease makes the case for more accurate and aggressive mediastinal staging prior to surgical resection.”
No disclosures and no study funding are reported.
SOURCE: Soukiasian HJ et al. AATS 2018, Abstract 67.
SAN DIEGO – Delaying
“There is significant upstaging with time from completion of clinical staging to surgical resection, with a 4% increase of upstaging per week for the overall study population,” said study coauthor Harmik J. Soukiasian, MD, FACS, of Cedars-Sinai Medical Center, Los Angeles, in an interview. “Upstaging impacts lung cancer prognosis as more advanced stages portend to a poorer prognosis.”
An estimated 80%-85% of lung cancer patients have NSCLC, according to the American Cancer Society, and Dr. Soukiasian said surgery offers a chance at a cure for those diagnosed at stage I.
“National Cancer Comprehensive Network (NCCN) Guidelines recommend surgery within 8 weeks of completed clinical staging for NSCLC to limit cancer progression or upstaging,” Dr. Soukiasian said. “Although these guidelines are well established and widely adopted, our study performs a more granular analysis, studying time as a predictor of upstaging for those patients diagnosed with stage I NSCLC.”
For the new study, Dr. Soukiasian and colleagues tracked 52,406 patients in a cancer database who had stage I NSCLC but had not undergone preoperative chemotherapy. The researchers tracked their clinical stages for up to 12 weeks from initial staging.
Researchers found that, while staging levels rose with each successive week, just 25% of patients underwent surgery by 1 week, and only 79% had surgery in accordance with NSCLC guidelines by week 8. At 12 weeks, 9% had still not undergone surgery.
Upstaging was common: 22% at 1 week, 32% after 8 weeks, and 33% after 12 weeks.
“We demonstrate that patients diagnosed with stage I NSCLC benefit from surgery sooner than the 8-week window recommended by the NCCN guidelines,” Dr. Soukiasian said. “Exclusive of the rate of progression and in addition to time to surgery, our study also demonstrated academic centers, higher lymph node yield during surgery, and left-sided tumors to be independent predictors of upstaging.”
The study design doesn’t provide insight into why surgery is often delayed. However, “we can theorize factors associated with delays to surgery may be due to patient factors (personal scheduling, availability of support systems, etc.), delays in follow up, operating room availability or scheduling, and issues with insurance approval,” Dr. Soukiasian said.
In his presentation, Dr. Soukiasian emphasized the role of the mediastinum. “Given the clinical impact of stage III disease, we analyzed upstaging rates of stage I NSCLC to stage IIIA and revealed a 1.3% increase per week of upstaging specifically to stage IIIA. Additionally, almost 5% of patients initially diagnosed with stage I NSCLC upstaged to IIIA disease. The significant rate of upstaging to IIIA disease makes the case for more accurate and aggressive mediastinal staging prior to surgical resection.”
No disclosures and no study funding are reported.
SOURCE: Soukiasian HJ et al. AATS 2018, Abstract 67.
SAN DIEGO – Delaying
“There is significant upstaging with time from completion of clinical staging to surgical resection, with a 4% increase of upstaging per week for the overall study population,” said study coauthor Harmik J. Soukiasian, MD, FACS, of Cedars-Sinai Medical Center, Los Angeles, in an interview. “Upstaging impacts lung cancer prognosis as more advanced stages portend to a poorer prognosis.”
An estimated 80%-85% of lung cancer patients have NSCLC, according to the American Cancer Society, and Dr. Soukiasian said surgery offers a chance at a cure for those diagnosed at stage I.
“National Cancer Comprehensive Network (NCCN) Guidelines recommend surgery within 8 weeks of completed clinical staging for NSCLC to limit cancer progression or upstaging,” Dr. Soukiasian said. “Although these guidelines are well established and widely adopted, our study performs a more granular analysis, studying time as a predictor of upstaging for those patients diagnosed with stage I NSCLC.”
For the new study, Dr. Soukiasian and colleagues tracked 52,406 patients in a cancer database who had stage I NSCLC but had not undergone preoperative chemotherapy. The researchers tracked their clinical stages for up to 12 weeks from initial staging.
Researchers found that, while staging levels rose with each successive week, just 25% of patients underwent surgery by 1 week, and only 79% had surgery in accordance with NSCLC guidelines by week 8. At 12 weeks, 9% had still not undergone surgery.
Upstaging was common: 22% at 1 week, 32% after 8 weeks, and 33% after 12 weeks.
“We demonstrate that patients diagnosed with stage I NSCLC benefit from surgery sooner than the 8-week window recommended by the NCCN guidelines,” Dr. Soukiasian said. “Exclusive of the rate of progression and in addition to time to surgery, our study also demonstrated academic centers, higher lymph node yield during surgery, and left-sided tumors to be independent predictors of upstaging.”
The study design doesn’t provide insight into why surgery is often delayed. However, “we can theorize factors associated with delays to surgery may be due to patient factors (personal scheduling, availability of support systems, etc.), delays in follow up, operating room availability or scheduling, and issues with insurance approval,” Dr. Soukiasian said.
In his presentation, Dr. Soukiasian emphasized the role of the mediastinum. “Given the clinical impact of stage III disease, we analyzed upstaging rates of stage I NSCLC to stage IIIA and revealed a 1.3% increase per week of upstaging specifically to stage IIIA. Additionally, almost 5% of patients initially diagnosed with stage I NSCLC upstaged to IIIA disease. The significant rate of upstaging to IIIA disease makes the case for more accurate and aggressive mediastinal staging prior to surgical resection.”
No disclosures and no study funding are reported.
SOURCE: Soukiasian HJ et al. AATS 2018, Abstract 67.
AT THE AATS ANNUAL MEETING
Key clinical point: Clinical staging levels worsen in each successive surgery-free week after initial staging in certain NSCLC patients.
Major finding: There was a 1.3% increase per week of upstaging to stage IIIA.
Study details: Analysis of 52,406 patients with stage I NSCLC who were tracked for up to 12 weeks.
Disclosures: No disclosures and no funding were reported.
Source: Soukiasian HJ et al. AATS 2018, Abstract 67.
FDA approves marketing of device to control GI bleeding
The Food and Drug Administration announced May 7 that it has permitted marketing of .
Hemospray is an aerosolized spray device that delivers a mineral blend to the bleeding site in the GI tract and is applied during endoscopic procedures and can cover large ulcers or tumors.
The FDA evaluated data from clinical studies consisting of 228 patients with upper and lower GI bleeding, supplemented with evidence from medical literature, including an additional 522 patients. The studies found that Hemospray stopped GI bleeding in 95% of patients within 5 minutes of device usage. Results also found that bleeding recurred, usually within 72 hours, and up to 30 days following device usage, in 20% of patients. Bowel perforation was observed as a serious side effect in approximately 1% of patients.
“The device provides an additional, nonsurgical option for treating upper and lower GI bleeding in certain patients, and may help reduce the risk of death from a GI bleed for many patients,” said Binita Ashar, MD, director, division of surgical devices, in the FDA’s Center for Devices and Radiological Health in a press release.
Hemospray is not intended for patients who have a gastrointestinal fistula or are at high risk for GI perforation. The device is not intended for use in patients with variceal bleeding. The FDA permitted the marketing of the Hemospray device to Wilson-Cook Medical.*
Read the full press release here.
Correction, 5/10/18: An earlier version of this article incorrectly described the patient population that should not be treated with Hemospray.
The Food and Drug Administration announced May 7 that it has permitted marketing of .
Hemospray is an aerosolized spray device that delivers a mineral blend to the bleeding site in the GI tract and is applied during endoscopic procedures and can cover large ulcers or tumors.
The FDA evaluated data from clinical studies consisting of 228 patients with upper and lower GI bleeding, supplemented with evidence from medical literature, including an additional 522 patients. The studies found that Hemospray stopped GI bleeding in 95% of patients within 5 minutes of device usage. Results also found that bleeding recurred, usually within 72 hours, and up to 30 days following device usage, in 20% of patients. Bowel perforation was observed as a serious side effect in approximately 1% of patients.
“The device provides an additional, nonsurgical option for treating upper and lower GI bleeding in certain patients, and may help reduce the risk of death from a GI bleed for many patients,” said Binita Ashar, MD, director, division of surgical devices, in the FDA’s Center for Devices and Radiological Health in a press release.
Hemospray is not intended for patients who have a gastrointestinal fistula or are at high risk for GI perforation. The device is not intended for use in patients with variceal bleeding. The FDA permitted the marketing of the Hemospray device to Wilson-Cook Medical.*
Read the full press release here.
Correction, 5/10/18: An earlier version of this article incorrectly described the patient population that should not be treated with Hemospray.
The Food and Drug Administration announced May 7 that it has permitted marketing of .
Hemospray is an aerosolized spray device that delivers a mineral blend to the bleeding site in the GI tract and is applied during endoscopic procedures and can cover large ulcers or tumors.
The FDA evaluated data from clinical studies consisting of 228 patients with upper and lower GI bleeding, supplemented with evidence from medical literature, including an additional 522 patients. The studies found that Hemospray stopped GI bleeding in 95% of patients within 5 minutes of device usage. Results also found that bleeding recurred, usually within 72 hours, and up to 30 days following device usage, in 20% of patients. Bowel perforation was observed as a serious side effect in approximately 1% of patients.
“The device provides an additional, nonsurgical option for treating upper and lower GI bleeding in certain patients, and may help reduce the risk of death from a GI bleed for many patients,” said Binita Ashar, MD, director, division of surgical devices, in the FDA’s Center for Devices and Radiological Health in a press release.
Hemospray is not intended for patients who have a gastrointestinal fistula or are at high risk for GI perforation. The device is not intended for use in patients with variceal bleeding. The FDA permitted the marketing of the Hemospray device to Wilson-Cook Medical.*
Read the full press release here.
Correction, 5/10/18: An earlier version of this article incorrectly described the patient population that should not be treated with Hemospray.
Leg lymphedema after gynecologic lymphadenectomy exceeds expectations
NEW ORLEANS – Leg lymphedema occurred in 19%-40% of women with a gynecologic cancer who underwent surgery with lymphadenectomy in a prospective study of 821 U.S. patients.
The incidence of lymphedema of the lower extremity (LLE) during 2 years of follow-up was 18% among 672 endometrial cancer patients, 25% among 124 cervical cancer patients, and 40% among 24 vulvar cancer patients, Jay W. Carlson, DO, said at the annual meeting of the Society of Gynecologic Oncology.
Although the study followed patients for 2 years after surgery, 84% of the LLE events occurred within the first 6 months after surgery, and 95% within the first 12 months. The robust incidence rates documented in this study contrasted with a general perception that LLE is relatively uncommon, leading Dr. Carlson to note that the new data show “the incidence of LLE is under recognized.” The findings also bucked conventional wisdom by showing no link between the incidence of LLE and number of lymph nodes dissected or with use of radiation treatment, said Dr. Carlson, a gynecologic oncologist at Mercy Clinic Women’s Oncology in Springfield, Mo.
To better define the incidence of LLE after lymphadenectomy for gynecologic cancers, the Gynecologic Oncology Group organized the Lymphedema and Gynecologic Cancer (LEG) study, run at more than 70 U.S. centers during June 2012–November 2014. The study enrolled patients scheduled for surgery to treat endometrial, cervical, or vulvar cancer, and applied systematic leg measurement to patients just before and at several prespecified times following surgery through 2 years of follow-up.
The study began with a total of 1,054 patients, but the final analysis that Dr. Carlson presented excluded patients who did not actually undergo lymphadenectomy during their surgery, did not have leg volume data available both before and after their surgery, or had a comorbidity or change in body mass that could have caused the change in leg size. The researchers also required patients identified with LLE to have completed the Gynecologic Cancer Lymphedema Questionnaire (Gynecol Oncol. 2010 May;117[2]:317-23) and tallied a score of at least 4, and to have at least a 10% increase in leg volume at the time of diagnosis, compared with the presurgical volume.
The exclusions yielded a total of 672 patients with endometrial cancer, including 127 who developed LLE (19%); 124 patients with cervical cancer, including 31 who developed LLE (25%); and 25 patients with vulvar cancer, including 10 who developed LLE (40%), Dr. Carlson reported.
Analysis of the patients who developed LLE showed no significant association with type of surgery (open, robotic, or laparoscopic), and no significant associations with several patient-specific factors including age, race, cancer stage, surgical blood loss, or serum albumin, he said.
mzoler@MDedge.com
On Twitter @mitchelzoler
SOURCE: Carlson J et al. SGO 2018, Abstract 11.
NEW ORLEANS – Leg lymphedema occurred in 19%-40% of women with a gynecologic cancer who underwent surgery with lymphadenectomy in a prospective study of 821 U.S. patients.
The incidence of lymphedema of the lower extremity (LLE) during 2 years of follow-up was 18% among 672 endometrial cancer patients, 25% among 124 cervical cancer patients, and 40% among 24 vulvar cancer patients, Jay W. Carlson, DO, said at the annual meeting of the Society of Gynecologic Oncology.
Although the study followed patients for 2 years after surgery, 84% of the LLE events occurred within the first 6 months after surgery, and 95% within the first 12 months. The robust incidence rates documented in this study contrasted with a general perception that LLE is relatively uncommon, leading Dr. Carlson to note that the new data show “the incidence of LLE is under recognized.” The findings also bucked conventional wisdom by showing no link between the incidence of LLE and number of lymph nodes dissected or with use of radiation treatment, said Dr. Carlson, a gynecologic oncologist at Mercy Clinic Women’s Oncology in Springfield, Mo.
To better define the incidence of LLE after lymphadenectomy for gynecologic cancers, the Gynecologic Oncology Group organized the Lymphedema and Gynecologic Cancer (LEG) study, run at more than 70 U.S. centers during June 2012–November 2014. The study enrolled patients scheduled for surgery to treat endometrial, cervical, or vulvar cancer, and applied systematic leg measurement to patients just before and at several prespecified times following surgery through 2 years of follow-up.
The study began with a total of 1,054 patients, but the final analysis that Dr. Carlson presented excluded patients who did not actually undergo lymphadenectomy during their surgery, did not have leg volume data available both before and after their surgery, or had a comorbidity or change in body mass that could have caused the change in leg size. The researchers also required patients identified with LLE to have completed the Gynecologic Cancer Lymphedema Questionnaire (Gynecol Oncol. 2010 May;117[2]:317-23) and tallied a score of at least 4, and to have at least a 10% increase in leg volume at the time of diagnosis, compared with the presurgical volume.
The exclusions yielded a total of 672 patients with endometrial cancer, including 127 who developed LLE (19%); 124 patients with cervical cancer, including 31 who developed LLE (25%); and 25 patients with vulvar cancer, including 10 who developed LLE (40%), Dr. Carlson reported.
Analysis of the patients who developed LLE showed no significant association with type of surgery (open, robotic, or laparoscopic), and no significant associations with several patient-specific factors including age, race, cancer stage, surgical blood loss, or serum albumin, he said.
mzoler@MDedge.com
On Twitter @mitchelzoler
SOURCE: Carlson J et al. SGO 2018, Abstract 11.
NEW ORLEANS – Leg lymphedema occurred in 19%-40% of women with a gynecologic cancer who underwent surgery with lymphadenectomy in a prospective study of 821 U.S. patients.
The incidence of lymphedema of the lower extremity (LLE) during 2 years of follow-up was 18% among 672 endometrial cancer patients, 25% among 124 cervical cancer patients, and 40% among 24 vulvar cancer patients, Jay W. Carlson, DO, said at the annual meeting of the Society of Gynecologic Oncology.
Although the study followed patients for 2 years after surgery, 84% of the LLE events occurred within the first 6 months after surgery, and 95% within the first 12 months. The robust incidence rates documented in this study contrasted with a general perception that LLE is relatively uncommon, leading Dr. Carlson to note that the new data show “the incidence of LLE is under recognized.” The findings also bucked conventional wisdom by showing no link between the incidence of LLE and number of lymph nodes dissected or with use of radiation treatment, said Dr. Carlson, a gynecologic oncologist at Mercy Clinic Women’s Oncology in Springfield, Mo.
To better define the incidence of LLE after lymphadenectomy for gynecologic cancers, the Gynecologic Oncology Group organized the Lymphedema and Gynecologic Cancer (LEG) study, run at more than 70 U.S. centers during June 2012–November 2014. The study enrolled patients scheduled for surgery to treat endometrial, cervical, or vulvar cancer, and applied systematic leg measurement to patients just before and at several prespecified times following surgery through 2 years of follow-up.
The study began with a total of 1,054 patients, but the final analysis that Dr. Carlson presented excluded patients who did not actually undergo lymphadenectomy during their surgery, did not have leg volume data available both before and after their surgery, or had a comorbidity or change in body mass that could have caused the change in leg size. The researchers also required patients identified with LLE to have completed the Gynecologic Cancer Lymphedema Questionnaire (Gynecol Oncol. 2010 May;117[2]:317-23) and tallied a score of at least 4, and to have at least a 10% increase in leg volume at the time of diagnosis, compared with the presurgical volume.
The exclusions yielded a total of 672 patients with endometrial cancer, including 127 who developed LLE (19%); 124 patients with cervical cancer, including 31 who developed LLE (25%); and 25 patients with vulvar cancer, including 10 who developed LLE (40%), Dr. Carlson reported.
Analysis of the patients who developed LLE showed no significant association with type of surgery (open, robotic, or laparoscopic), and no significant associations with several patient-specific factors including age, race, cancer stage, surgical blood loss, or serum albumin, he said.
mzoler@MDedge.com
On Twitter @mitchelzoler
SOURCE: Carlson J et al. SGO 2018, Abstract 11.
REPORTING FROM SGO 2018
Key clinical point: Leg lymphedema is common following lymphadenectomy for a gynecologic cancer.
Major finding: Leg lymphedema incidence was 19%-40% during 2-year follow-up after lymphadenectomy during gynecologic cancer surgery.
Study details: LEG, a multicenter, U.S. prospective study with 821 gynecologic cancer patients in the final analysis.
Disclosures: LEG had no commercial funding. Dr. Carlson had no disclosures.
Source: Carlson J et al. SGO 2018, Abstract 11.