User login
MDedge latest news is breaking news from medical conferences, journals, guidelines, the FDA and CDC.
Cell-Free DNA Blood Test Shows Strong Performance in Detecting Early-Stage CRC
Cell-Free DNA Blood Test Shows Strong Performance in Detecting Early-Stage CRC
TOPLINE:
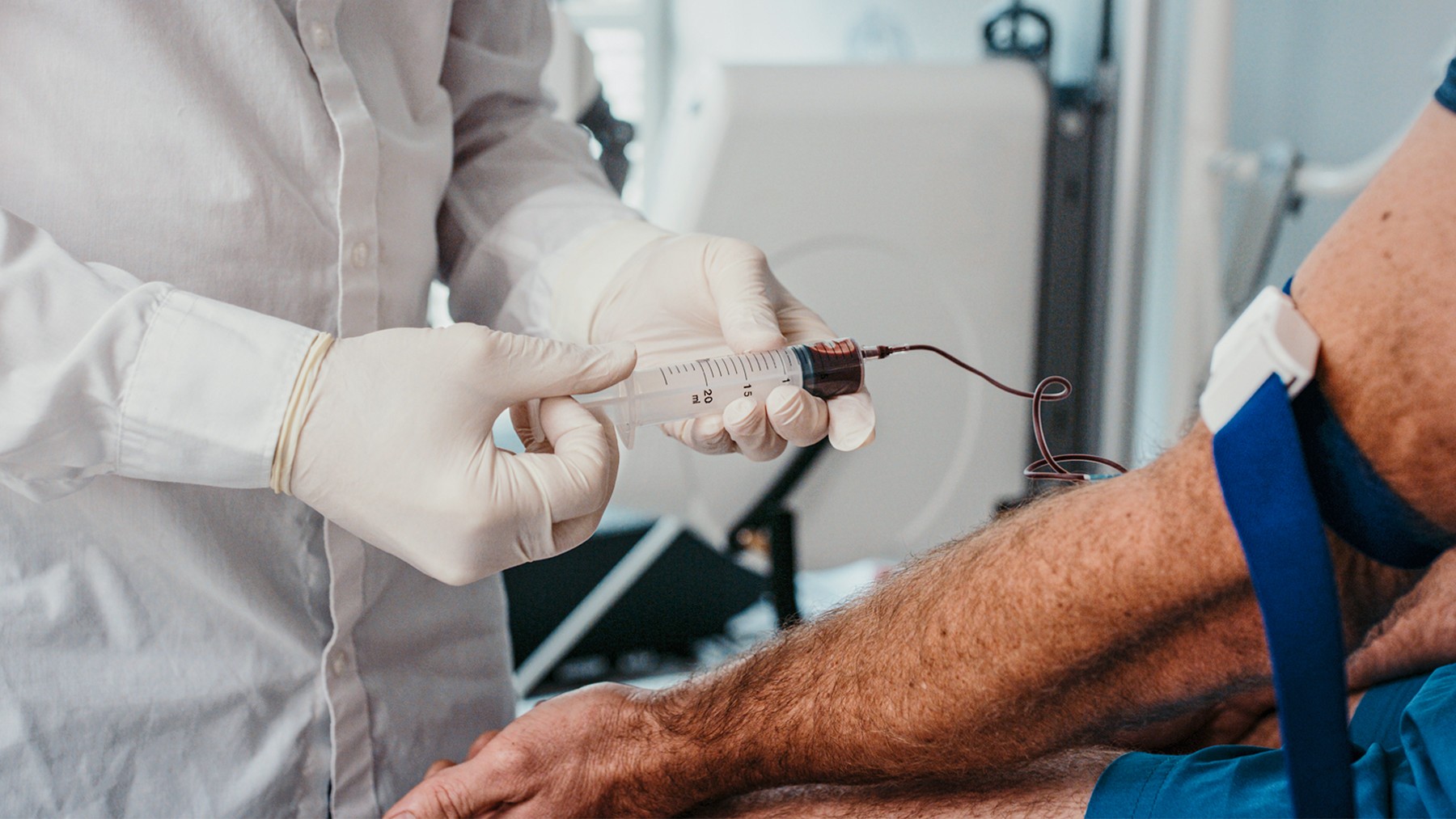
A novel, blood-based test developed using fragmentomic features of cell-free DNA (cfDNA) detects colorectal cancer (CRC) with a 90.4% sensitivity and shows consistent performance across stages and tumor locations.
METHODOLOGY:
- Researchers conducted a prospective case-control study to develop and validate a noninvasive cfDNA-based screening test for CRC.
- Adults aged 40-89 years with CRC or advanced adenomas were enrolled at a tertiary center in South Korea between 2021 and 2024.
- Blood samples were drawn after colonoscopy, but prior to treatment, in patients with CRC, advanced adenomas, and asymptomatic controls with normal colonoscopy results.
- A model was trained on fragmentonic features derived from whole genome sequencing of cfDNA from 1250 participants and validated for its diagnostic performance in the remaining 427 participants, including all with advanced adenomas.
- The primary endpoint was the sensitivity of the cfDNA test for detecting CRC. The area under the receiver operating characteristic curve (AUROC) was also calculated.
TAKEAWAY:
- The cfDNA test detected CRC with 90.4% sensitivity and an AUROC of 0.978.
- Sensitivity by CRC stage was 84.2% for stage I, 85.0% for stage II, 94.4% for stage III, 100% for stage IV.
- Advanced adenomas were detected with 58.3% sensitivity and an AUROC of 0.862.
- Among individuals with normal colonoscopy findings, the test was correctly negative 94.7% of the time.
- Diagnostic sensitivities were consistent between left- and right-sided CRC tumors, among participants aged < 60 years and ≥ 60 years, and across left- and right-sided advanced adenomas.
IN PRACTICE:
"This highlights the potential clinical utility of the test in identifying candidates for minimally invasive therapeutic approaches tool for CRC," the authors wrote. "Notably, the high sensitivity observed for early-stage CRC and the favorable sensitivity for [advanced adenoma] suggest that this cfDNA test may offer benefits not only in diagnosis but also in prognosis and ultimately in CRC prevention."
SOURCE:
This study was led by Seung Wook Hong, MD, Asan Medical Center in Seoul, South Korea. It was published online on November 19, 2025, in the American Journal of Gastroenterology.
LIMITATIONS:
The case-control design introduced spectrum bias by comparing clearly defined CRC and advanced adenomas cases with individuals who had normal colonoscopy results. The CRC prevalence of 17% to 18% was higher than that observed in true screening populations, limiting generalizability. The exclusively Korean cohort limited extrapolation to non-Asian populations.
DISCLOSURES:
The study received support from GC Genome, Yongin, South Korea. The authors reported no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
A novel, blood-based test developed using fragmentomic features of cell-free DNA (cfDNA) detects colorectal cancer (CRC) with a 90.4% sensitivity and shows consistent performance across stages and tumor locations.
METHODOLOGY:
- Researchers conducted a prospective case-control study to develop and validate a noninvasive cfDNA-based screening test for CRC.
- Adults aged 40-89 years with CRC or advanced adenomas were enrolled at a tertiary center in South Korea between 2021 and 2024.
- Blood samples were drawn after colonoscopy, but prior to treatment, in patients with CRC, advanced adenomas, and asymptomatic controls with normal colonoscopy results.
- A model was trained on fragmentonic features derived from whole genome sequencing of cfDNA from 1250 participants and validated for its diagnostic performance in the remaining 427 participants, including all with advanced adenomas.
- The primary endpoint was the sensitivity of the cfDNA test for detecting CRC. The area under the receiver operating characteristic curve (AUROC) was also calculated.
TAKEAWAY:
- The cfDNA test detected CRC with 90.4% sensitivity and an AUROC of 0.978.
- Sensitivity by CRC stage was 84.2% for stage I, 85.0% for stage II, 94.4% for stage III, 100% for stage IV.
- Advanced adenomas were detected with 58.3% sensitivity and an AUROC of 0.862.
- Among individuals with normal colonoscopy findings, the test was correctly negative 94.7% of the time.
- Diagnostic sensitivities were consistent between left- and right-sided CRC tumors, among participants aged < 60 years and ≥ 60 years, and across left- and right-sided advanced adenomas.
IN PRACTICE:
"This highlights the potential clinical utility of the test in identifying candidates for minimally invasive therapeutic approaches tool for CRC," the authors wrote. "Notably, the high sensitivity observed for early-stage CRC and the favorable sensitivity for [advanced adenoma] suggest that this cfDNA test may offer benefits not only in diagnosis but also in prognosis and ultimately in CRC prevention."
SOURCE:
This study was led by Seung Wook Hong, MD, Asan Medical Center in Seoul, South Korea. It was published online on November 19, 2025, in the American Journal of Gastroenterology.
LIMITATIONS:
The case-control design introduced spectrum bias by comparing clearly defined CRC and advanced adenomas cases with individuals who had normal colonoscopy results. The CRC prevalence of 17% to 18% was higher than that observed in true screening populations, limiting generalizability. The exclusively Korean cohort limited extrapolation to non-Asian populations.
DISCLOSURES:
The study received support from GC Genome, Yongin, South Korea. The authors reported no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
A novel, blood-based test developed using fragmentomic features of cell-free DNA (cfDNA) detects colorectal cancer (CRC) with a 90.4% sensitivity and shows consistent performance across stages and tumor locations.
METHODOLOGY:
- Researchers conducted a prospective case-control study to develop and validate a noninvasive cfDNA-based screening test for CRC.
- Adults aged 40-89 years with CRC or advanced adenomas were enrolled at a tertiary center in South Korea between 2021 and 2024.
- Blood samples were drawn after colonoscopy, but prior to treatment, in patients with CRC, advanced adenomas, and asymptomatic controls with normal colonoscopy results.
- A model was trained on fragmentonic features derived from whole genome sequencing of cfDNA from 1250 participants and validated for its diagnostic performance in the remaining 427 participants, including all with advanced adenomas.
- The primary endpoint was the sensitivity of the cfDNA test for detecting CRC. The area under the receiver operating characteristic curve (AUROC) was also calculated.
TAKEAWAY:
- The cfDNA test detected CRC with 90.4% sensitivity and an AUROC of 0.978.
- Sensitivity by CRC stage was 84.2% for stage I, 85.0% for stage II, 94.4% for stage III, 100% for stage IV.
- Advanced adenomas were detected with 58.3% sensitivity and an AUROC of 0.862.
- Among individuals with normal colonoscopy findings, the test was correctly negative 94.7% of the time.
- Diagnostic sensitivities were consistent between left- and right-sided CRC tumors, among participants aged < 60 years and ≥ 60 years, and across left- and right-sided advanced adenomas.
IN PRACTICE:
"This highlights the potential clinical utility of the test in identifying candidates for minimally invasive therapeutic approaches tool for CRC," the authors wrote. "Notably, the high sensitivity observed for early-stage CRC and the favorable sensitivity for [advanced adenoma] suggest that this cfDNA test may offer benefits not only in diagnosis but also in prognosis and ultimately in CRC prevention."
SOURCE:
This study was led by Seung Wook Hong, MD, Asan Medical Center in Seoul, South Korea. It was published online on November 19, 2025, in the American Journal of Gastroenterology.
LIMITATIONS:
The case-control design introduced spectrum bias by comparing clearly defined CRC and advanced adenomas cases with individuals who had normal colonoscopy results. The CRC prevalence of 17% to 18% was higher than that observed in true screening populations, limiting generalizability. The exclusively Korean cohort limited extrapolation to non-Asian populations.
DISCLOSURES:
The study received support from GC Genome, Yongin, South Korea. The authors reported no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
Cell-Free DNA Blood Test Shows Strong Performance in Detecting Early-Stage CRC
Cell-Free DNA Blood Test Shows Strong Performance in Detecting Early-Stage CRC
Balancing the Challenge of Research with the Joys of Clinical Care
Andrew Ofosu, MD, MPH, loves the variety that GI medicine offers on a day-to-day basis.
Some days are spent in the endoscopy suite, performing endoscopic retrograde cholangiopancreatography in patients with cholangitis, “which is usually a high-stakes situation,” he said. Other days he might be in clinic, helping to manage a patient with chronic pancreatitis.
“The contrast of the immediate impact of a procedure combined with the continuity of long-term relationships, is special to me,” said Dr. Ofosu, an associate professor of medicine at Cincinnati College of Medicine, in Cincinnati, Ohio. He’s also a member of AGA’s Future Leaders program, which provides early career GI physicians with opportunities to network and develop leadership skills.
In an interview, he discussed his research pursuits in the areas of pancreatic cancer and artificial intelligence (AI), and his unique methods for connecting with patients. The art of listening to patient concerns is crucial, he says, especially following a difficult diagnosis.
What’s it like to be part of the AGA Future Leaders Class of 2025-2026? How has the experience enriched your career?
Dr. Ofosu: My time being part of this group has been very transformative. It’s provided mentorship from national leaders. It’s enabled me to collaborate with peers across different institutions and given me opportunities to refine my leadership skills. It’s changed my perspective and created a network that has equipped me to contribute meaningfully to the gastroenterology community and to my institution.
What is the most challenging clinical case you’ve encountered?
Dr. Ofosu: One case that stands out was a young patient with recurrent idiopathic pancreatitis. We went through all the potential differential etiologies that includes genetics, autoimmune disease and structural etiologies. It became a long, diagnostic journey. The challenge wasn’t just the medical aspect of it, but the emotional aspect of it…when you don’t have all the answers available. We were eventually able to figure out what the cause of the pancreatitis was. It was genetic, and the patient is doing great now.
One of your research interests has been developing innovative ways to use AI in endoscopic ultrasound to identify and characterize lesions. Can you discuss some of those innovations?
Dr. Ofosu: It’s definitely an area that I’m looking to explore at this time; to leverage AI to improve diagnostic capability of endoscopic ultrasound. The whole idea is to be able to use AI to analyze images in real time that can help highlight features, which can ultimately help in distinguishing both benign and malignant tumors, and allowing AI to provide real time diagnostic support, improving accuracy of diagnosis and reducing unnecessary treatment.
In 2021, you conducted a study to investigate the demographics, clinical outcomes and survival outcomes of patients diagnosed with early and late onset pancreatic adenocarcinoma. What did your study reveal and what are the next steps?
Dr. Ofosu: Our study looked at over 136,000 patients with pancreatic adenocarcinoma and compared those diagnosed under age 40 to older patients. We found that although pancreatic cancer is rare in the young, both groups are presenting more often with advanced disease, and incidence is rising. Younger patients tend to have tumors in the head of the pancreas, while older patients more often show growth in the body and tail. Survival overall remains very poor—about 6 to 7 months—but slightly better in younger patients.
I think the next step is to better understand the biological drivers of early onset PAC to look at integrating molecular profiling to see if there are distinct genetic patterns that can guide therapy. Ultimately the goal is to improve early detection and tailor management strategy for this subset of patients.
What is your approach to patient communication and education?
Dr. Ofosu: I aim for clarity and empathy. Some GI diagnoses can be intimidating, with all the terminologies, and so I use a lot of analogies and visuals to simplify complex conditions. I also ensure that patients understand what we are discussing because I found that what a patient hears isn’t always what they think I explained.
I believe being honest and compassionate should go hand in hand. I don’t shy away from delivering difficult news, but I always take time to pause, listen, and acknowledge emotions. I found that patients and families appreciate transparency even when the prognosis is tough, as long as they know I’m fully present with them.
Can you share a memorable patient interaction that impacted you?
Dr. Ofosu: There was one patient with chronic pancreatitis due to alcohol who had limited economic and social support. Beyond the medical management, what made a difference was sitting and listening to the patient, helping them connect to resources and social support – a social network. I think this reinforces that medicine isn’t just about lab values. It’s all about restoring dignity and focus with the patient.
What do you think is the biggest misconception about your specialty?
Dr. Ofosu: That gastroenterology is all about procedures, that all we do is scope. In reality, it’s a combination of technical expertise as well as the cognitive aspect of providing long-term management of complex diseases that affect patients, which takes a diverse skillset beyond endoscopy.
Lightning Round
What’s your favorite season of the year?
Fall. I like the colors of changing leaves
What’s your favorite way to spend a weekend?
Watching soccer with family and friends
If you could have dinner with any historical figure, who would it be?
Nelson Mandela
What’s your go-to karaoke song?Don’t Stop Believin’ by Journey
What’s one thing on your bucket list?
Travel to Europe, experience different cultures
What’s your favorite childhood memory?
When I learned how to fly a kite
If you could instantly learn any skill, what would it be?
Playing piano
Are you a planner or more spontaneous?
Planner
What’s your favorite holiday tradition?
Sharing Christmas dinner with family.
Andrew Ofosu, MD, MPH, loves the variety that GI medicine offers on a day-to-day basis.
Some days are spent in the endoscopy suite, performing endoscopic retrograde cholangiopancreatography in patients with cholangitis, “which is usually a high-stakes situation,” he said. Other days he might be in clinic, helping to manage a patient with chronic pancreatitis.
“The contrast of the immediate impact of a procedure combined with the continuity of long-term relationships, is special to me,” said Dr. Ofosu, an associate professor of medicine at Cincinnati College of Medicine, in Cincinnati, Ohio. He’s also a member of AGA’s Future Leaders program, which provides early career GI physicians with opportunities to network and develop leadership skills.
In an interview, he discussed his research pursuits in the areas of pancreatic cancer and artificial intelligence (AI), and his unique methods for connecting with patients. The art of listening to patient concerns is crucial, he says, especially following a difficult diagnosis.
What’s it like to be part of the AGA Future Leaders Class of 2025-2026? How has the experience enriched your career?
Dr. Ofosu: My time being part of this group has been very transformative. It’s provided mentorship from national leaders. It’s enabled me to collaborate with peers across different institutions and given me opportunities to refine my leadership skills. It’s changed my perspective and created a network that has equipped me to contribute meaningfully to the gastroenterology community and to my institution.
What is the most challenging clinical case you’ve encountered?
Dr. Ofosu: One case that stands out was a young patient with recurrent idiopathic pancreatitis. We went through all the potential differential etiologies that includes genetics, autoimmune disease and structural etiologies. It became a long, diagnostic journey. The challenge wasn’t just the medical aspect of it, but the emotional aspect of it…when you don’t have all the answers available. We were eventually able to figure out what the cause of the pancreatitis was. It was genetic, and the patient is doing great now.
One of your research interests has been developing innovative ways to use AI in endoscopic ultrasound to identify and characterize lesions. Can you discuss some of those innovations?
Dr. Ofosu: It’s definitely an area that I’m looking to explore at this time; to leverage AI to improve diagnostic capability of endoscopic ultrasound. The whole idea is to be able to use AI to analyze images in real time that can help highlight features, which can ultimately help in distinguishing both benign and malignant tumors, and allowing AI to provide real time diagnostic support, improving accuracy of diagnosis and reducing unnecessary treatment.
In 2021, you conducted a study to investigate the demographics, clinical outcomes and survival outcomes of patients diagnosed with early and late onset pancreatic adenocarcinoma. What did your study reveal and what are the next steps?
Dr. Ofosu: Our study looked at over 136,000 patients with pancreatic adenocarcinoma and compared those diagnosed under age 40 to older patients. We found that although pancreatic cancer is rare in the young, both groups are presenting more often with advanced disease, and incidence is rising. Younger patients tend to have tumors in the head of the pancreas, while older patients more often show growth in the body and tail. Survival overall remains very poor—about 6 to 7 months—but slightly better in younger patients.
I think the next step is to better understand the biological drivers of early onset PAC to look at integrating molecular profiling to see if there are distinct genetic patterns that can guide therapy. Ultimately the goal is to improve early detection and tailor management strategy for this subset of patients.
What is your approach to patient communication and education?
Dr. Ofosu: I aim for clarity and empathy. Some GI diagnoses can be intimidating, with all the terminologies, and so I use a lot of analogies and visuals to simplify complex conditions. I also ensure that patients understand what we are discussing because I found that what a patient hears isn’t always what they think I explained.
I believe being honest and compassionate should go hand in hand. I don’t shy away from delivering difficult news, but I always take time to pause, listen, and acknowledge emotions. I found that patients and families appreciate transparency even when the prognosis is tough, as long as they know I’m fully present with them.
Can you share a memorable patient interaction that impacted you?
Dr. Ofosu: There was one patient with chronic pancreatitis due to alcohol who had limited economic and social support. Beyond the medical management, what made a difference was sitting and listening to the patient, helping them connect to resources and social support – a social network. I think this reinforces that medicine isn’t just about lab values. It’s all about restoring dignity and focus with the patient.
What do you think is the biggest misconception about your specialty?
Dr. Ofosu: That gastroenterology is all about procedures, that all we do is scope. In reality, it’s a combination of technical expertise as well as the cognitive aspect of providing long-term management of complex diseases that affect patients, which takes a diverse skillset beyond endoscopy.
Lightning Round
What’s your favorite season of the year?
Fall. I like the colors of changing leaves
What’s your favorite way to spend a weekend?
Watching soccer with family and friends
If you could have dinner with any historical figure, who would it be?
Nelson Mandela
What’s your go-to karaoke song?Don’t Stop Believin’ by Journey
What’s one thing on your bucket list?
Travel to Europe, experience different cultures
What’s your favorite childhood memory?
When I learned how to fly a kite
If you could instantly learn any skill, what would it be?
Playing piano
Are you a planner or more spontaneous?
Planner
What’s your favorite holiday tradition?
Sharing Christmas dinner with family.
Andrew Ofosu, MD, MPH, loves the variety that GI medicine offers on a day-to-day basis.
Some days are spent in the endoscopy suite, performing endoscopic retrograde cholangiopancreatography in patients with cholangitis, “which is usually a high-stakes situation,” he said. Other days he might be in clinic, helping to manage a patient with chronic pancreatitis.
“The contrast of the immediate impact of a procedure combined with the continuity of long-term relationships, is special to me,” said Dr. Ofosu, an associate professor of medicine at Cincinnati College of Medicine, in Cincinnati, Ohio. He’s also a member of AGA’s Future Leaders program, which provides early career GI physicians with opportunities to network and develop leadership skills.
In an interview, he discussed his research pursuits in the areas of pancreatic cancer and artificial intelligence (AI), and his unique methods for connecting with patients. The art of listening to patient concerns is crucial, he says, especially following a difficult diagnosis.
What’s it like to be part of the AGA Future Leaders Class of 2025-2026? How has the experience enriched your career?
Dr. Ofosu: My time being part of this group has been very transformative. It’s provided mentorship from national leaders. It’s enabled me to collaborate with peers across different institutions and given me opportunities to refine my leadership skills. It’s changed my perspective and created a network that has equipped me to contribute meaningfully to the gastroenterology community and to my institution.
What is the most challenging clinical case you’ve encountered?
Dr. Ofosu: One case that stands out was a young patient with recurrent idiopathic pancreatitis. We went through all the potential differential etiologies that includes genetics, autoimmune disease and structural etiologies. It became a long, diagnostic journey. The challenge wasn’t just the medical aspect of it, but the emotional aspect of it…when you don’t have all the answers available. We were eventually able to figure out what the cause of the pancreatitis was. It was genetic, and the patient is doing great now.
One of your research interests has been developing innovative ways to use AI in endoscopic ultrasound to identify and characterize lesions. Can you discuss some of those innovations?
Dr. Ofosu: It’s definitely an area that I’m looking to explore at this time; to leverage AI to improve diagnostic capability of endoscopic ultrasound. The whole idea is to be able to use AI to analyze images in real time that can help highlight features, which can ultimately help in distinguishing both benign and malignant tumors, and allowing AI to provide real time diagnostic support, improving accuracy of diagnosis and reducing unnecessary treatment.
In 2021, you conducted a study to investigate the demographics, clinical outcomes and survival outcomes of patients diagnosed with early and late onset pancreatic adenocarcinoma. What did your study reveal and what are the next steps?
Dr. Ofosu: Our study looked at over 136,000 patients with pancreatic adenocarcinoma and compared those diagnosed under age 40 to older patients. We found that although pancreatic cancer is rare in the young, both groups are presenting more often with advanced disease, and incidence is rising. Younger patients tend to have tumors in the head of the pancreas, while older patients more often show growth in the body and tail. Survival overall remains very poor—about 6 to 7 months—but slightly better in younger patients.
I think the next step is to better understand the biological drivers of early onset PAC to look at integrating molecular profiling to see if there are distinct genetic patterns that can guide therapy. Ultimately the goal is to improve early detection and tailor management strategy for this subset of patients.
What is your approach to patient communication and education?
Dr. Ofosu: I aim for clarity and empathy. Some GI diagnoses can be intimidating, with all the terminologies, and so I use a lot of analogies and visuals to simplify complex conditions. I also ensure that patients understand what we are discussing because I found that what a patient hears isn’t always what they think I explained.
I believe being honest and compassionate should go hand in hand. I don’t shy away from delivering difficult news, but I always take time to pause, listen, and acknowledge emotions. I found that patients and families appreciate transparency even when the prognosis is tough, as long as they know I’m fully present with them.
Can you share a memorable patient interaction that impacted you?
Dr. Ofosu: There was one patient with chronic pancreatitis due to alcohol who had limited economic and social support. Beyond the medical management, what made a difference was sitting and listening to the patient, helping them connect to resources and social support – a social network. I think this reinforces that medicine isn’t just about lab values. It’s all about restoring dignity and focus with the patient.
What do you think is the biggest misconception about your specialty?
Dr. Ofosu: That gastroenterology is all about procedures, that all we do is scope. In reality, it’s a combination of technical expertise as well as the cognitive aspect of providing long-term management of complex diseases that affect patients, which takes a diverse skillset beyond endoscopy.
Lightning Round
What’s your favorite season of the year?
Fall. I like the colors of changing leaves
What’s your favorite way to spend a weekend?
Watching soccer with family and friends
If you could have dinner with any historical figure, who would it be?
Nelson Mandela
What’s your go-to karaoke song?Don’t Stop Believin’ by Journey
What’s one thing on your bucket list?
Travel to Europe, experience different cultures
What’s your favorite childhood memory?
When I learned how to fly a kite
If you could instantly learn any skill, what would it be?
Playing piano
Are you a planner or more spontaneous?
Planner
What’s your favorite holiday tradition?
Sharing Christmas dinner with family.

“Don’t Take Shortcuts,” Endoscopy Researcher Advises
But the work he’s most proud of took place when he was a graduate student at Harvard, working on a master’s degree in epidemiology and biostatistics.
Jovani compared two different types of needles for tissue acquisition with endoscopic ultrasound. His finding that fine needle biopsy is better than fine needle aspiration for lesions isn’t groundbreaking, yet “the reason why I feel proud of that one is because it’s the first paper I did completely by myself,” said Jovani, medical director for advanced therapeutic endoscopy with Gastro Health Florida, in Miami, Florida.
Dr. Jovani has since contributed to countless peer-reviewed articles and book chapters and has presented research findings at meetings across the globe. He will be program director of the upcoming gastroenterology fellowship program at Florida International University School of Medicine, Miami, and participates in several endoscopy panels in the U.S. and in Europe to set guidelines and improve the quality of endoscopic procedures.
Therapeutic endoscopy is a clinical interest of his, specifically in the areas of third space, biliopancreatic and bariatric endoscopy. In an interview, he discussed how he used third space endoscopy to save a patient and improve her quality of life
Indeed, helping patients feel better is the most satisfying part of his career.
“A lot of people may have acute pain or an early cancer or many other problems that they need solving. As a physician, you can be the one who solves it,” said Jovani.
But training in medicine involves hard work, he advised. In the interview, he explained why young doctors should never rely on shortcuts to solve problems.
Therapeutic endoscopy is a specific interest of yours. How has this field advanced since you’ve been practicing gastroenterology?
Dr. Jovani: In the last 10 to 15 years, significant improvements have come along. As an example, lumen-apposing metal stents have revolutionized the way we do therapeutic endoscopy. A lot of procedures were not possible beforehand and we would have to send patients to surgery. Now, these can be done with endoscopy.
Examples include drainage of pancreatic collections, gallbladder drainage, or gastrojejunostomy (a connection between the stomach and the intestine) or reversal of Roux-en-Y gastric bypass to reach and drain the bile duct. Many of these procedures can be done with these metal stents that were not possible beforehand. Bariatric endoscopy is a relatively new field, and that has significantly changed the management of obesity.
There’s also third space endoscopy for the treatment of gastroparesis, achalasia, and early cancer.
What is third space endoscopy and how are you applying it in your practice?
Dr. Jovani: Third space endoscopy refers to a new space that’s created between the mucosa and the muscularis propria into the submucosa. We go in the submucosa, we inject some fluid there, and we cut the submucosa and we separate the mucosa from the muscle.
This allows us to do a lot of procedures. For patients with achalasia, we can tunnel through the submucosa, get into the muscle and perform myotomy, meaning that we can cut the muscle. By doing so, we can treat achalasia with a minimally invasive method. Patients can either go home the next day or even on the same day. The same thing applies for gastroparesis. With early cancer, we can go through in the submucosa, and if the cancer is in the mucosa only, or if it is in the very superficial submucosa, we can treat it without a need for surgery. Sometimes the procedure is simple, but other times it can be very challenging.
Can you discuss a challenging case where you applied third space endoscopy?
Dr. Jovani: It was a gastric cancer case. I did an endoscopic ultrasound for staging purposes. When I saw the lesion, it looked very superficial, like an early cancer of the stomach. I called the surgeon and said I could take it out with endoscopy. And it was in a very difficult location, so it was a very challenging procedure. It took about 12 hours to do it, but I was able to completely take it out. More than a year later, the patient was cancer free and more importantly, we preserved the stomach. Before I did this, she was prepared to undergo total gastrectomy, which meant I would have taken out her entire stomach.
Instead, with this minimally invasive procedure, I was able to take the cancer away and keep the stomach, which preserved her quality of life as well.
When you don’t have the stomach, obviously you adapt, but the quality of life is never the same. The type of food you eat, the frequency of eating, the quality of food you eat is not the same. The fact that we could avoid that in this patient feels very good.
What advice would you give to aspiring medical students?
Dr. Jovani: Do the hard work that’s required to be a doctor. Being a physician is a hard job, but it’s very rewarding. It’s like going to the gym—there really are no shortcuts. You have to do the work, you have to get tired, you have to study hard. You may study things you might not think will be useful to you necessarily in the future field that you choose. If it is GI, you still need to study all the other fields because sometimes patients may have GI diseases that are connecting with other diseases and you won’t know that if you haven’t studied the other diseases.
Patients are not only one disease, but they are also complex patients. Sometimes if you try to correct one disease, you create a complication with the other disease and you might not be aware of that.
Don’t create shortcuts like ChatGPT, things that are becoming fashionable with younger people today. Do the hard work the old way in which you have to memorize things. Knowledge is the only thing that really can help the patient.
Go to GI meetings. Offer to meet people, collaborate, network. Don’t be shy about it. Even if it is not natural to you, just do it. It’ll become more natural as you do it. GI, like any other field, any other endeavor in human society, is something that also depends on interactions. Therefore, it’s good to learn how to interact, how to network, how to do research projects. Even with people from far away, communication is very easy. You don’t really need to do research projects only with people in your local environment. You can do research projects with people who are on the other side of the state or even on the other side of the world.
You place an emphasis on individualized patient care. Can you discuss what that means to you?
Dr. Jovani: It basically means that there isn’t one size fits all in the management of diseases. Obviously there are some general principles that are applicable to everybody, but sometimes for the single specific patient, what works for one patient might not necessarily work for the next patient.
With Endoscopic Retrograde Cholangiopancreatography (ERCP) for example, there are so many things that go into that. Most papilla are in a certain position and it’s relatively easy to cannulate. But there are others that are in very different positions or in different angulations and they might require specific techniques that are not applicable in the majority of cases. You have to adapt to the single patient.How you speak to the patient is also important. Some may prefer a certain type of communication and other patients may prefer another type of communication involving patients or family. You have to adapt to the single patient. You have to understand the different types of personalities and adapt how you explain things or how you communicate disease, or management of disease or even complications to the specific patient. Different approaches are more appropriate for different patients with different needs. At the end of the day, patients are single individuals after all.
Where do you see the field of GI medicine advancing internationally over the next 5 years?
Dr. Jovani: Artificial intelligence or AI is a big player. It will help with diagnostics primarily, at least over the short term. Potentially it can help with therapeutics as well. There’s a lot of investment and excitement and interest in artificial intelligence.
Therapeutic endoscopy robotics, especially in interventional endoscopy, third space endoscopy, is also gaining attention.
With regards to bariatric endoscopy, we should have a CPT code for it in January 2027. This will increase volume because it’ll be covered more by insurance. These are things that will help advance GI in the next five or 10 years.
Lightning Round
What’s one hobby you’d like to pick up?
Kite surfing
What’s your favorite season of the year?
Summer
What’s your favorite way to spend a weekend?
Traveling or going to the beach
If you could have dinner with any historical figure, who would it be?
Jesus Christ
What’s your favorite holiday tradition?
New Year’s Eve
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
You can do it!
What’s your comfort food?
Lasagna
But the work he’s most proud of took place when he was a graduate student at Harvard, working on a master’s degree in epidemiology and biostatistics.
Jovani compared two different types of needles for tissue acquisition with endoscopic ultrasound. His finding that fine needle biopsy is better than fine needle aspiration for lesions isn’t groundbreaking, yet “the reason why I feel proud of that one is because it’s the first paper I did completely by myself,” said Jovani, medical director for advanced therapeutic endoscopy with Gastro Health Florida, in Miami, Florida.
Dr. Jovani has since contributed to countless peer-reviewed articles and book chapters and has presented research findings at meetings across the globe. He will be program director of the upcoming gastroenterology fellowship program at Florida International University School of Medicine, Miami, and participates in several endoscopy panels in the U.S. and in Europe to set guidelines and improve the quality of endoscopic procedures.
Therapeutic endoscopy is a clinical interest of his, specifically in the areas of third space, biliopancreatic and bariatric endoscopy. In an interview, he discussed how he used third space endoscopy to save a patient and improve her quality of life
Indeed, helping patients feel better is the most satisfying part of his career.
“A lot of people may have acute pain or an early cancer or many other problems that they need solving. As a physician, you can be the one who solves it,” said Jovani.
But training in medicine involves hard work, he advised. In the interview, he explained why young doctors should never rely on shortcuts to solve problems.
Therapeutic endoscopy is a specific interest of yours. How has this field advanced since you’ve been practicing gastroenterology?
Dr. Jovani: In the last 10 to 15 years, significant improvements have come along. As an example, lumen-apposing metal stents have revolutionized the way we do therapeutic endoscopy. A lot of procedures were not possible beforehand and we would have to send patients to surgery. Now, these can be done with endoscopy.
Examples include drainage of pancreatic collections, gallbladder drainage, or gastrojejunostomy (a connection between the stomach and the intestine) or reversal of Roux-en-Y gastric bypass to reach and drain the bile duct. Many of these procedures can be done with these metal stents that were not possible beforehand. Bariatric endoscopy is a relatively new field, and that has significantly changed the management of obesity.
There’s also third space endoscopy for the treatment of gastroparesis, achalasia, and early cancer.
What is third space endoscopy and how are you applying it in your practice?
Dr. Jovani: Third space endoscopy refers to a new space that’s created between the mucosa and the muscularis propria into the submucosa. We go in the submucosa, we inject some fluid there, and we cut the submucosa and we separate the mucosa from the muscle.
This allows us to do a lot of procedures. For patients with achalasia, we can tunnel through the submucosa, get into the muscle and perform myotomy, meaning that we can cut the muscle. By doing so, we can treat achalasia with a minimally invasive method. Patients can either go home the next day or even on the same day. The same thing applies for gastroparesis. With early cancer, we can go through in the submucosa, and if the cancer is in the mucosa only, or if it is in the very superficial submucosa, we can treat it without a need for surgery. Sometimes the procedure is simple, but other times it can be very challenging.
Can you discuss a challenging case where you applied third space endoscopy?
Dr. Jovani: It was a gastric cancer case. I did an endoscopic ultrasound for staging purposes. When I saw the lesion, it looked very superficial, like an early cancer of the stomach. I called the surgeon and said I could take it out with endoscopy. And it was in a very difficult location, so it was a very challenging procedure. It took about 12 hours to do it, but I was able to completely take it out. More than a year later, the patient was cancer free and more importantly, we preserved the stomach. Before I did this, she was prepared to undergo total gastrectomy, which meant I would have taken out her entire stomach.
Instead, with this minimally invasive procedure, I was able to take the cancer away and keep the stomach, which preserved her quality of life as well.
When you don’t have the stomach, obviously you adapt, but the quality of life is never the same. The type of food you eat, the frequency of eating, the quality of food you eat is not the same. The fact that we could avoid that in this patient feels very good.
What advice would you give to aspiring medical students?
Dr. Jovani: Do the hard work that’s required to be a doctor. Being a physician is a hard job, but it’s very rewarding. It’s like going to the gym—there really are no shortcuts. You have to do the work, you have to get tired, you have to study hard. You may study things you might not think will be useful to you necessarily in the future field that you choose. If it is GI, you still need to study all the other fields because sometimes patients may have GI diseases that are connecting with other diseases and you won’t know that if you haven’t studied the other diseases.
Patients are not only one disease, but they are also complex patients. Sometimes if you try to correct one disease, you create a complication with the other disease and you might not be aware of that.
Don’t create shortcuts like ChatGPT, things that are becoming fashionable with younger people today. Do the hard work the old way in which you have to memorize things. Knowledge is the only thing that really can help the patient.
Go to GI meetings. Offer to meet people, collaborate, network. Don’t be shy about it. Even if it is not natural to you, just do it. It’ll become more natural as you do it. GI, like any other field, any other endeavor in human society, is something that also depends on interactions. Therefore, it’s good to learn how to interact, how to network, how to do research projects. Even with people from far away, communication is very easy. You don’t really need to do research projects only with people in your local environment. You can do research projects with people who are on the other side of the state or even on the other side of the world.
You place an emphasis on individualized patient care. Can you discuss what that means to you?
Dr. Jovani: It basically means that there isn’t one size fits all in the management of diseases. Obviously there are some general principles that are applicable to everybody, but sometimes for the single specific patient, what works for one patient might not necessarily work for the next patient.
With Endoscopic Retrograde Cholangiopancreatography (ERCP) for example, there are so many things that go into that. Most papilla are in a certain position and it’s relatively easy to cannulate. But there are others that are in very different positions or in different angulations and they might require specific techniques that are not applicable in the majority of cases. You have to adapt to the single patient.How you speak to the patient is also important. Some may prefer a certain type of communication and other patients may prefer another type of communication involving patients or family. You have to adapt to the single patient. You have to understand the different types of personalities and adapt how you explain things or how you communicate disease, or management of disease or even complications to the specific patient. Different approaches are more appropriate for different patients with different needs. At the end of the day, patients are single individuals after all.
Where do you see the field of GI medicine advancing internationally over the next 5 years?
Dr. Jovani: Artificial intelligence or AI is a big player. It will help with diagnostics primarily, at least over the short term. Potentially it can help with therapeutics as well. There’s a lot of investment and excitement and interest in artificial intelligence.
Therapeutic endoscopy robotics, especially in interventional endoscopy, third space endoscopy, is also gaining attention.
With regards to bariatric endoscopy, we should have a CPT code for it in January 2027. This will increase volume because it’ll be covered more by insurance. These are things that will help advance GI in the next five or 10 years.
Lightning Round
What’s one hobby you’d like to pick up?
Kite surfing
What’s your favorite season of the year?
Summer
What’s your favorite way to spend a weekend?
Traveling or going to the beach
If you could have dinner with any historical figure, who would it be?
Jesus Christ
What’s your favorite holiday tradition?
New Year’s Eve
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
You can do it!
What’s your comfort food?
Lasagna
But the work he’s most proud of took place when he was a graduate student at Harvard, working on a master’s degree in epidemiology and biostatistics.
Jovani compared two different types of needles for tissue acquisition with endoscopic ultrasound. His finding that fine needle biopsy is better than fine needle aspiration for lesions isn’t groundbreaking, yet “the reason why I feel proud of that one is because it’s the first paper I did completely by myself,” said Jovani, medical director for advanced therapeutic endoscopy with Gastro Health Florida, in Miami, Florida.
Dr. Jovani has since contributed to countless peer-reviewed articles and book chapters and has presented research findings at meetings across the globe. He will be program director of the upcoming gastroenterology fellowship program at Florida International University School of Medicine, Miami, and participates in several endoscopy panels in the U.S. and in Europe to set guidelines and improve the quality of endoscopic procedures.
Therapeutic endoscopy is a clinical interest of his, specifically in the areas of third space, biliopancreatic and bariatric endoscopy. In an interview, he discussed how he used third space endoscopy to save a patient and improve her quality of life
Indeed, helping patients feel better is the most satisfying part of his career.
“A lot of people may have acute pain or an early cancer or many other problems that they need solving. As a physician, you can be the one who solves it,” said Jovani.
But training in medicine involves hard work, he advised. In the interview, he explained why young doctors should never rely on shortcuts to solve problems.
Therapeutic endoscopy is a specific interest of yours. How has this field advanced since you’ve been practicing gastroenterology?
Dr. Jovani: In the last 10 to 15 years, significant improvements have come along. As an example, lumen-apposing metal stents have revolutionized the way we do therapeutic endoscopy. A lot of procedures were not possible beforehand and we would have to send patients to surgery. Now, these can be done with endoscopy.
Examples include drainage of pancreatic collections, gallbladder drainage, or gastrojejunostomy (a connection between the stomach and the intestine) or reversal of Roux-en-Y gastric bypass to reach and drain the bile duct. Many of these procedures can be done with these metal stents that were not possible beforehand. Bariatric endoscopy is a relatively new field, and that has significantly changed the management of obesity.
There’s also third space endoscopy for the treatment of gastroparesis, achalasia, and early cancer.
What is third space endoscopy and how are you applying it in your practice?
Dr. Jovani: Third space endoscopy refers to a new space that’s created between the mucosa and the muscularis propria into the submucosa. We go in the submucosa, we inject some fluid there, and we cut the submucosa and we separate the mucosa from the muscle.
This allows us to do a lot of procedures. For patients with achalasia, we can tunnel through the submucosa, get into the muscle and perform myotomy, meaning that we can cut the muscle. By doing so, we can treat achalasia with a minimally invasive method. Patients can either go home the next day or even on the same day. The same thing applies for gastroparesis. With early cancer, we can go through in the submucosa, and if the cancer is in the mucosa only, or if it is in the very superficial submucosa, we can treat it without a need for surgery. Sometimes the procedure is simple, but other times it can be very challenging.
Can you discuss a challenging case where you applied third space endoscopy?
Dr. Jovani: It was a gastric cancer case. I did an endoscopic ultrasound for staging purposes. When I saw the lesion, it looked very superficial, like an early cancer of the stomach. I called the surgeon and said I could take it out with endoscopy. And it was in a very difficult location, so it was a very challenging procedure. It took about 12 hours to do it, but I was able to completely take it out. More than a year later, the patient was cancer free and more importantly, we preserved the stomach. Before I did this, she was prepared to undergo total gastrectomy, which meant I would have taken out her entire stomach.
Instead, with this minimally invasive procedure, I was able to take the cancer away and keep the stomach, which preserved her quality of life as well.
When you don’t have the stomach, obviously you adapt, but the quality of life is never the same. The type of food you eat, the frequency of eating, the quality of food you eat is not the same. The fact that we could avoid that in this patient feels very good.
What advice would you give to aspiring medical students?
Dr. Jovani: Do the hard work that’s required to be a doctor. Being a physician is a hard job, but it’s very rewarding. It’s like going to the gym—there really are no shortcuts. You have to do the work, you have to get tired, you have to study hard. You may study things you might not think will be useful to you necessarily in the future field that you choose. If it is GI, you still need to study all the other fields because sometimes patients may have GI diseases that are connecting with other diseases and you won’t know that if you haven’t studied the other diseases.
Patients are not only one disease, but they are also complex patients. Sometimes if you try to correct one disease, you create a complication with the other disease and you might not be aware of that.
Don’t create shortcuts like ChatGPT, things that are becoming fashionable with younger people today. Do the hard work the old way in which you have to memorize things. Knowledge is the only thing that really can help the patient.
Go to GI meetings. Offer to meet people, collaborate, network. Don’t be shy about it. Even if it is not natural to you, just do it. It’ll become more natural as you do it. GI, like any other field, any other endeavor in human society, is something that also depends on interactions. Therefore, it’s good to learn how to interact, how to network, how to do research projects. Even with people from far away, communication is very easy. You don’t really need to do research projects only with people in your local environment. You can do research projects with people who are on the other side of the state or even on the other side of the world.
You place an emphasis on individualized patient care. Can you discuss what that means to you?
Dr. Jovani: It basically means that there isn’t one size fits all in the management of diseases. Obviously there are some general principles that are applicable to everybody, but sometimes for the single specific patient, what works for one patient might not necessarily work for the next patient.
With Endoscopic Retrograde Cholangiopancreatography (ERCP) for example, there are so many things that go into that. Most papilla are in a certain position and it’s relatively easy to cannulate. But there are others that are in very different positions or in different angulations and they might require specific techniques that are not applicable in the majority of cases. You have to adapt to the single patient.How you speak to the patient is also important. Some may prefer a certain type of communication and other patients may prefer another type of communication involving patients or family. You have to adapt to the single patient. You have to understand the different types of personalities and adapt how you explain things or how you communicate disease, or management of disease or even complications to the specific patient. Different approaches are more appropriate for different patients with different needs. At the end of the day, patients are single individuals after all.
Where do you see the field of GI medicine advancing internationally over the next 5 years?
Dr. Jovani: Artificial intelligence or AI is a big player. It will help with diagnostics primarily, at least over the short term. Potentially it can help with therapeutics as well. There’s a lot of investment and excitement and interest in artificial intelligence.
Therapeutic endoscopy robotics, especially in interventional endoscopy, third space endoscopy, is also gaining attention.
With regards to bariatric endoscopy, we should have a CPT code for it in January 2027. This will increase volume because it’ll be covered more by insurance. These are things that will help advance GI in the next five or 10 years.
Lightning Round
What’s one hobby you’d like to pick up?
Kite surfing
What’s your favorite season of the year?
Summer
What’s your favorite way to spend a weekend?
Traveling or going to the beach
If you could have dinner with any historical figure, who would it be?
Jesus Christ
What’s your favorite holiday tradition?
New Year’s Eve
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
You can do it!
What’s your comfort food?
Lasagna

Geographic Clusters Show Uneven Cancer Screening in the US
Geographic Clusters Show Uneven Cancer Screening in the US
TOPLINE:
An analysis of 3142 US counties revealed that county-level screening for breast, cervical, and colorectal cancer increased overall between 1997 and 2019; however, despite the reduced geographic variation, persistently high-screening clusters remained in the Northeast, whereas persistently low-screening clusters remained in the Southwest.
METHODOLOGY:
- Cancer screening reduces mortality. Despite guideline recommendation, the uptake of breast, cervical, and colorectal cancer screening in the US falls short of national goals and varies across sociodemographic groups. To date, only a few studies have examined geographic and temporal patterns of screening.
- To address this gap, researchers conducted a cross-sectional study using an ecological panel design to analyze county-level screening prevalence across 3142 US mainland counties from 1997 to 2019, deriving prevalence estimates from Behavioral Risk Factor Surveillance System (BRFSS) and National Health Interview Survey (NHIS) data over 3- to 5-year periods.
- Spatial autocorrelation analyses, including Global Moran I and the bivariate local indicator of spatial autocorrelation, were performed to assess geographic clusters of cancer screening within each period. Four types of local geographic clusters of county-level cancer screening were identified: counties with persistently high screening rates, counties with persistently low screening rates, counties in which screening rates decreased from high to low, and counties in which screening rates increased from low to high.
- Screening prevalence was compared across multiple time windows for different modalities (mammography, a Papanicolaou test, colonoscopy, colorectal cancer test, endoscopy, and a fecal occult blood test [FOBT]). Overall, 3101 counties were analyzed for mammography and the Papanicolaou test, 3107 counties for colonoscopy, 3100 counties for colorectal cancer test, 3089 counties for endoscopy, and 3090 counties for the FOBT.
TAKEAWAY:
- Overall screening prevalence increased from 1997 to 2019, and global spatial autocorrelation declined over time. For instance, the distribution of mammography screening became 83% more uniform in more recent years (Moran I, 0.57 in 1997-1999 vs 0.10 in 2017-2019). Similarly, Papanicolaou test screening became more uniform in more recent years (Moran I, 0.44 vs. 0.07). These changes indicate reduced geographic heterogeneity.
- Colonoscopy and endoscopy use increased, surpassing a 50% prevalence in many counties for 2010; however, FOBT use declined. Spatial clustering also attenuated, with a 23.4% declined in Moran I for colonoscopy from 2011-2016 to 2017-2019, a 12.3% decline in the colorectal cancer test from 2004-2007 to 2008-2010, and a 14.0% decline for endoscopy from 2004-2007 to 2008-2010.
- Persistently high-/high-screening clusters were concentrated in the Northeast for mammography and colorectal cancer screening and in the East for Papanicolaou test screening, whereas persistently low-/low-screening clusters were concentrated in the Southwest for the same modalities.
- Clusters of low- and high-screening counties were more disadvantaged -- with lower socioeconomic status and a higher proportion of non-White residents -- than other cluster types, suggesting some improvement in screening uptake in more disadvantaged areas. Counties with persistently low screening exhibited greater socioeconomic disadvantages -- lower media household income, higher poverty, lower home values, and lower educational attainment -- than those with persistently high screening.
IN PRACTICE:
"This cross-sectional study found that despite secular increases that reduced geographic variation in screening, local clusters of high and low screening persisted in the Northeast and Southwest US, respectively. Future studies could incorporate health care access characteristics to explain why areas of low screening did not catch up to optimize cancer screening practice," the authors wrote.
SOURCE:
The study, led by Pranoti Pradhan, PhD, Harvard T.H. Chan School of Public Health, Boston, was published online in JAMA Network Open.
LIMITATIONS:
The county-level estimates were modeled using BRFSS, NHIS, and US Census data, which might be susceptible to sampling biases despite corrections for nonresponse and noncoverage. Researchers lacked data on specific health systems characteristics that may have directly driven changes in prevalence and were restricted to using screening time intervals available from the Small Area Estimates for Cancer-Relates Measures from the National Cancer Institute, rather than those according to US Preventive Services Task Force guidelines. Additionally, the spatial cluster method was sensitive to county size and arrangement, which may have influenced local cluster detection.
DISCLOSURES:
This research was supported by the T32 Cancer Prevention and Control Funding Fellowship and T32 Cancer Epidemiology Fellowship at the Harvard T.H. Chan School of Public Health. The authors declared having no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
An analysis of 3142 US counties revealed that county-level screening for breast, cervical, and colorectal cancer increased overall between 1997 and 2019; however, despite the reduced geographic variation, persistently high-screening clusters remained in the Northeast, whereas persistently low-screening clusters remained in the Southwest.
METHODOLOGY:
- Cancer screening reduces mortality. Despite guideline recommendation, the uptake of breast, cervical, and colorectal cancer screening in the US falls short of national goals and varies across sociodemographic groups. To date, only a few studies have examined geographic and temporal patterns of screening.
- To address this gap, researchers conducted a cross-sectional study using an ecological panel design to analyze county-level screening prevalence across 3142 US mainland counties from 1997 to 2019, deriving prevalence estimates from Behavioral Risk Factor Surveillance System (BRFSS) and National Health Interview Survey (NHIS) data over 3- to 5-year periods.
- Spatial autocorrelation analyses, including Global Moran I and the bivariate local indicator of spatial autocorrelation, were performed to assess geographic clusters of cancer screening within each period. Four types of local geographic clusters of county-level cancer screening were identified: counties with persistently high screening rates, counties with persistently low screening rates, counties in which screening rates decreased from high to low, and counties in which screening rates increased from low to high.
- Screening prevalence was compared across multiple time windows for different modalities (mammography, a Papanicolaou test, colonoscopy, colorectal cancer test, endoscopy, and a fecal occult blood test [FOBT]). Overall, 3101 counties were analyzed for mammography and the Papanicolaou test, 3107 counties for colonoscopy, 3100 counties for colorectal cancer test, 3089 counties for endoscopy, and 3090 counties for the FOBT.
TAKEAWAY:
- Overall screening prevalence increased from 1997 to 2019, and global spatial autocorrelation declined over time. For instance, the distribution of mammography screening became 83% more uniform in more recent years (Moran I, 0.57 in 1997-1999 vs 0.10 in 2017-2019). Similarly, Papanicolaou test screening became more uniform in more recent years (Moran I, 0.44 vs. 0.07). These changes indicate reduced geographic heterogeneity.
- Colonoscopy and endoscopy use increased, surpassing a 50% prevalence in many counties for 2010; however, FOBT use declined. Spatial clustering also attenuated, with a 23.4% declined in Moran I for colonoscopy from 2011-2016 to 2017-2019, a 12.3% decline in the colorectal cancer test from 2004-2007 to 2008-2010, and a 14.0% decline for endoscopy from 2004-2007 to 2008-2010.
- Persistently high-/high-screening clusters were concentrated in the Northeast for mammography and colorectal cancer screening and in the East for Papanicolaou test screening, whereas persistently low-/low-screening clusters were concentrated in the Southwest for the same modalities.
- Clusters of low- and high-screening counties were more disadvantaged -- with lower socioeconomic status and a higher proportion of non-White residents -- than other cluster types, suggesting some improvement in screening uptake in more disadvantaged areas. Counties with persistently low screening exhibited greater socioeconomic disadvantages -- lower media household income, higher poverty, lower home values, and lower educational attainment -- than those with persistently high screening.
IN PRACTICE:
"This cross-sectional study found that despite secular increases that reduced geographic variation in screening, local clusters of high and low screening persisted in the Northeast and Southwest US, respectively. Future studies could incorporate health care access characteristics to explain why areas of low screening did not catch up to optimize cancer screening practice," the authors wrote.
SOURCE:
The study, led by Pranoti Pradhan, PhD, Harvard T.H. Chan School of Public Health, Boston, was published online in JAMA Network Open.
LIMITATIONS:
The county-level estimates were modeled using BRFSS, NHIS, and US Census data, which might be susceptible to sampling biases despite corrections for nonresponse and noncoverage. Researchers lacked data on specific health systems characteristics that may have directly driven changes in prevalence and were restricted to using screening time intervals available from the Small Area Estimates for Cancer-Relates Measures from the National Cancer Institute, rather than those according to US Preventive Services Task Force guidelines. Additionally, the spatial cluster method was sensitive to county size and arrangement, which may have influenced local cluster detection.
DISCLOSURES:
This research was supported by the T32 Cancer Prevention and Control Funding Fellowship and T32 Cancer Epidemiology Fellowship at the Harvard T.H. Chan School of Public Health. The authors declared having no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
An analysis of 3142 US counties revealed that county-level screening for breast, cervical, and colorectal cancer increased overall between 1997 and 2019; however, despite the reduced geographic variation, persistently high-screening clusters remained in the Northeast, whereas persistently low-screening clusters remained in the Southwest.
METHODOLOGY:
- Cancer screening reduces mortality. Despite guideline recommendation, the uptake of breast, cervical, and colorectal cancer screening in the US falls short of national goals and varies across sociodemographic groups. To date, only a few studies have examined geographic and temporal patterns of screening.
- To address this gap, researchers conducted a cross-sectional study using an ecological panel design to analyze county-level screening prevalence across 3142 US mainland counties from 1997 to 2019, deriving prevalence estimates from Behavioral Risk Factor Surveillance System (BRFSS) and National Health Interview Survey (NHIS) data over 3- to 5-year periods.
- Spatial autocorrelation analyses, including Global Moran I and the bivariate local indicator of spatial autocorrelation, were performed to assess geographic clusters of cancer screening within each period. Four types of local geographic clusters of county-level cancer screening were identified: counties with persistently high screening rates, counties with persistently low screening rates, counties in which screening rates decreased from high to low, and counties in which screening rates increased from low to high.
- Screening prevalence was compared across multiple time windows for different modalities (mammography, a Papanicolaou test, colonoscopy, colorectal cancer test, endoscopy, and a fecal occult blood test [FOBT]). Overall, 3101 counties were analyzed for mammography and the Papanicolaou test, 3107 counties for colonoscopy, 3100 counties for colorectal cancer test, 3089 counties for endoscopy, and 3090 counties for the FOBT.
TAKEAWAY:
- Overall screening prevalence increased from 1997 to 2019, and global spatial autocorrelation declined over time. For instance, the distribution of mammography screening became 83% more uniform in more recent years (Moran I, 0.57 in 1997-1999 vs 0.10 in 2017-2019). Similarly, Papanicolaou test screening became more uniform in more recent years (Moran I, 0.44 vs. 0.07). These changes indicate reduced geographic heterogeneity.
- Colonoscopy and endoscopy use increased, surpassing a 50% prevalence in many counties for 2010; however, FOBT use declined. Spatial clustering also attenuated, with a 23.4% declined in Moran I for colonoscopy from 2011-2016 to 2017-2019, a 12.3% decline in the colorectal cancer test from 2004-2007 to 2008-2010, and a 14.0% decline for endoscopy from 2004-2007 to 2008-2010.
- Persistently high-/high-screening clusters were concentrated in the Northeast for mammography and colorectal cancer screening and in the East for Papanicolaou test screening, whereas persistently low-/low-screening clusters were concentrated in the Southwest for the same modalities.
- Clusters of low- and high-screening counties were more disadvantaged -- with lower socioeconomic status and a higher proportion of non-White residents -- than other cluster types, suggesting some improvement in screening uptake in more disadvantaged areas. Counties with persistently low screening exhibited greater socioeconomic disadvantages -- lower media household income, higher poverty, lower home values, and lower educational attainment -- than those with persistently high screening.
IN PRACTICE:
"This cross-sectional study found that despite secular increases that reduced geographic variation in screening, local clusters of high and low screening persisted in the Northeast and Southwest US, respectively. Future studies could incorporate health care access characteristics to explain why areas of low screening did not catch up to optimize cancer screening practice," the authors wrote.
SOURCE:
The study, led by Pranoti Pradhan, PhD, Harvard T.H. Chan School of Public Health, Boston, was published online in JAMA Network Open.
LIMITATIONS:
The county-level estimates were modeled using BRFSS, NHIS, and US Census data, which might be susceptible to sampling biases despite corrections for nonresponse and noncoverage. Researchers lacked data on specific health systems characteristics that may have directly driven changes in prevalence and were restricted to using screening time intervals available from the Small Area Estimates for Cancer-Relates Measures from the National Cancer Institute, rather than those according to US Preventive Services Task Force guidelines. Additionally, the spatial cluster method was sensitive to county size and arrangement, which may have influenced local cluster detection.
DISCLOSURES:
This research was supported by the T32 Cancer Prevention and Control Funding Fellowship and T32 Cancer Epidemiology Fellowship at the Harvard T.H. Chan School of Public Health. The authors declared having no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
Geographic Clusters Show Uneven Cancer Screening in the US
Geographic Clusters Show Uneven Cancer Screening in the US
Latest COVID-19 Shot May Cut Severe Outcomes in Veterans
TOPLINE:
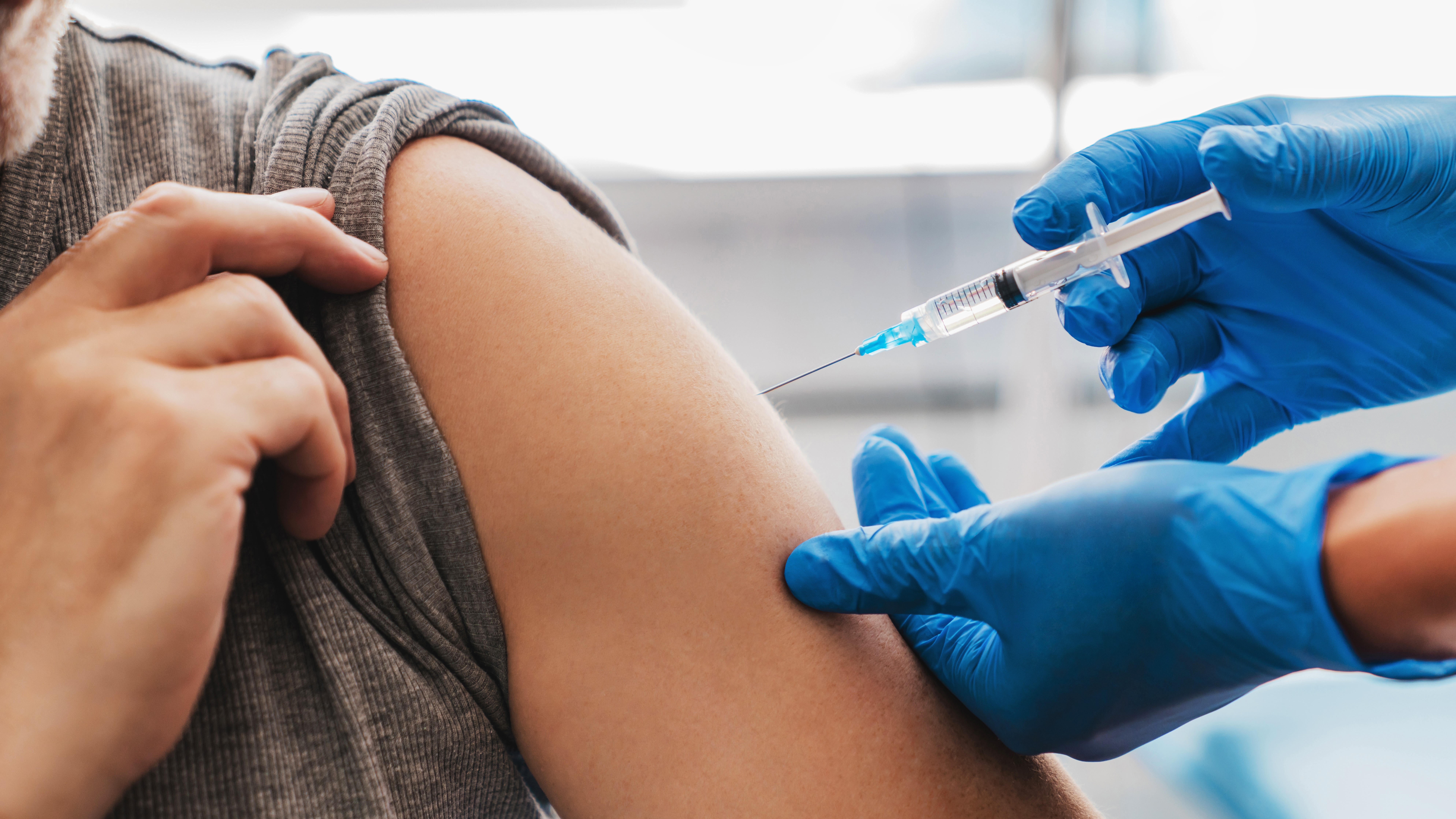
Among US veterans, same-day receipt of both the 2024-2025 COVID19 vaccine and the influenza vaccine was associated with lower risks for emergency department visits, hospitalizations, and deaths compared with receipt of the influenza vaccine alone.
METHODOLOGY:
- Researchers conducted an observational study to assess the effectiveness of the 2024-2025 COVID-19 vaccine by comparing veterans who received both the COVID-19 and influenza vaccines on the same day with those who received only the influenza vaccine between September 3 and December 31, 2024.
- Data on participants (mean age, approximately 71.5 years; approximately 92% men) were sourced from electronic health records of the Department of Veterans Affairs and included 164,132 veterans who received both vaccines vs 131,839 who received only the seasonal influenza vaccine, with a follow-up duration of 180 days.
- The vaccines used were mainly the 2024-2025 mRNA COVID19 vaccines: Moderna mRNA1273, Pfizer BNT162b2, and the highdose trivalent 2024-2025 seasonal influenza vaccine.
- Primary outcomes were COVID-19-associated emergency department visits, hospitalizations, and deaths.
TAKEAWAY:
- Receipt of both the COVID-19 and influenza vaccines was associated with a lower risk for COVID-19-associated emergency department visits compared with receipt of the influenza vaccine alone, resulting in a vaccine effectiveness of 29.3% and a risk difference of 18.3 per 10,000 persons (95% CI, 10.8-27.6).
- Similarly, COVID-19 vaccine effectiveness was 39.2% (95% CI, 21.6-54.5) against COVID-19-associated hospitalizations, with a risk difference of 7.5 per 10,000 persons (95% CI, 3.4-13.0).
- For COVID-19-associated deaths, vaccine effectiveness was 64% (95% CI, 23.0-85.8), with a risk difference of 2.2 per 10,000 persons (95% CI, 0.5-6.9).
- Benefits were consistent across age groups (< 65, 65-75, and > 75 years) and among people with various comorbidities, including cardiovascular disease and immunocompromised status.
IN PRACTICE:
“The evidence may help inform ongoing discussions about the value of COVID-19 vaccines in the current epidemiologic landscape,” the authors wrote.
SOURCE:
The study was led by Miao Cai, PhD , Research and Development Service, Veterans Affairs St. Louis Health Care System, and the Veterans Research and Education Foundation of St. Louis, Missouri. It was published online in The New England Journal of Medicine .
LIMITATIONS:
The demographic composition of the cohort — predominantly older, White, male veterans — may limit the generalizability of the study. Although numerous covariates were adjusted for, residual confounding could not be fully ruled out. Safety and variantspecific effectiveness were not assessed.
DISCLOSURES:
The study was supported by a grant from the Department of Veterans Affairs. Two authors disclosed consulting for Pfizer.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Among US veterans, same-day receipt of both the 2024-2025 COVID19 vaccine and the influenza vaccine was associated with lower risks for emergency department visits, hospitalizations, and deaths compared with receipt of the influenza vaccine alone.
METHODOLOGY:
- Researchers conducted an observational study to assess the effectiveness of the 2024-2025 COVID-19 vaccine by comparing veterans who received both the COVID-19 and influenza vaccines on the same day with those who received only the influenza vaccine between September 3 and December 31, 2024.
- Data on participants (mean age, approximately 71.5 years; approximately 92% men) were sourced from electronic health records of the Department of Veterans Affairs and included 164,132 veterans who received both vaccines vs 131,839 who received only the seasonal influenza vaccine, with a follow-up duration of 180 days.
- The vaccines used were mainly the 2024-2025 mRNA COVID19 vaccines: Moderna mRNA1273, Pfizer BNT162b2, and the highdose trivalent 2024-2025 seasonal influenza vaccine.
- Primary outcomes were COVID-19-associated emergency department visits, hospitalizations, and deaths.
TAKEAWAY:
- Receipt of both the COVID-19 and influenza vaccines was associated with a lower risk for COVID-19-associated emergency department visits compared with receipt of the influenza vaccine alone, resulting in a vaccine effectiveness of 29.3% and a risk difference of 18.3 per 10,000 persons (95% CI, 10.8-27.6).
- Similarly, COVID-19 vaccine effectiveness was 39.2% (95% CI, 21.6-54.5) against COVID-19-associated hospitalizations, with a risk difference of 7.5 per 10,000 persons (95% CI, 3.4-13.0).
- For COVID-19-associated deaths, vaccine effectiveness was 64% (95% CI, 23.0-85.8), with a risk difference of 2.2 per 10,000 persons (95% CI, 0.5-6.9).
- Benefits were consistent across age groups (< 65, 65-75, and > 75 years) and among people with various comorbidities, including cardiovascular disease and immunocompromised status.
IN PRACTICE:
“The evidence may help inform ongoing discussions about the value of COVID-19 vaccines in the current epidemiologic landscape,” the authors wrote.
SOURCE:
The study was led by Miao Cai, PhD , Research and Development Service, Veterans Affairs St. Louis Health Care System, and the Veterans Research and Education Foundation of St. Louis, Missouri. It was published online in The New England Journal of Medicine .
LIMITATIONS:
The demographic composition of the cohort — predominantly older, White, male veterans — may limit the generalizability of the study. Although numerous covariates were adjusted for, residual confounding could not be fully ruled out. Safety and variantspecific effectiveness were not assessed.
DISCLOSURES:
The study was supported by a grant from the Department of Veterans Affairs. Two authors disclosed consulting for Pfizer.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Among US veterans, same-day receipt of both the 2024-2025 COVID19 vaccine and the influenza vaccine was associated with lower risks for emergency department visits, hospitalizations, and deaths compared with receipt of the influenza vaccine alone.
METHODOLOGY:
- Researchers conducted an observational study to assess the effectiveness of the 2024-2025 COVID-19 vaccine by comparing veterans who received both the COVID-19 and influenza vaccines on the same day with those who received only the influenza vaccine between September 3 and December 31, 2024.
- Data on participants (mean age, approximately 71.5 years; approximately 92% men) were sourced from electronic health records of the Department of Veterans Affairs and included 164,132 veterans who received both vaccines vs 131,839 who received only the seasonal influenza vaccine, with a follow-up duration of 180 days.
- The vaccines used were mainly the 2024-2025 mRNA COVID19 vaccines: Moderna mRNA1273, Pfizer BNT162b2, and the highdose trivalent 2024-2025 seasonal influenza vaccine.
- Primary outcomes were COVID-19-associated emergency department visits, hospitalizations, and deaths.
TAKEAWAY:
- Receipt of both the COVID-19 and influenza vaccines was associated with a lower risk for COVID-19-associated emergency department visits compared with receipt of the influenza vaccine alone, resulting in a vaccine effectiveness of 29.3% and a risk difference of 18.3 per 10,000 persons (95% CI, 10.8-27.6).
- Similarly, COVID-19 vaccine effectiveness was 39.2% (95% CI, 21.6-54.5) against COVID-19-associated hospitalizations, with a risk difference of 7.5 per 10,000 persons (95% CI, 3.4-13.0).
- For COVID-19-associated deaths, vaccine effectiveness was 64% (95% CI, 23.0-85.8), with a risk difference of 2.2 per 10,000 persons (95% CI, 0.5-6.9).
- Benefits were consistent across age groups (< 65, 65-75, and > 75 years) and among people with various comorbidities, including cardiovascular disease and immunocompromised status.
IN PRACTICE:
“The evidence may help inform ongoing discussions about the value of COVID-19 vaccines in the current epidemiologic landscape,” the authors wrote.
SOURCE:
The study was led by Miao Cai, PhD , Research and Development Service, Veterans Affairs St. Louis Health Care System, and the Veterans Research and Education Foundation of St. Louis, Missouri. It was published online in The New England Journal of Medicine .
LIMITATIONS:
The demographic composition of the cohort — predominantly older, White, male veterans — may limit the generalizability of the study. Although numerous covariates were adjusted for, residual confounding could not be fully ruled out. Safety and variantspecific effectiveness were not assessed.
DISCLOSURES:
The study was supported by a grant from the Department of Veterans Affairs. Two authors disclosed consulting for Pfizer.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
COVID Linked to Eye Issues, But Vaccine Offers Protection
TOPLINE:
Patients with COVID had a higher risk of developing diplopia and cranial nerve VI palsy than those with influenza. Compared with unvaccinated patients, recipients of mRNA vaccines against SARS-CoV-2 had a more than 30% reduced risk of developing posterior-segment complications including retinal edema, vitreous hemorrhage, and optic neuritis.
METHODOLOGY:
- Researchers conducted a retrospective cohort analysis of US electronic health records from March 2020 to April 2021 to assess eye complications after COVID and the effect of mRNA vaccination on them.
- They analyzed matched cohorts of 73,654 vaccinated patients with COVID (mean age, 60.6 years; 61.6% women) and 73,654 unvaccinated patients with the condition (mean age, 61.2 years; 62.8% women); vaccination status was determined based on recorded receipt of an mRNA vaccine.
- In a separate matched analysis, 77,809 patients with COVID (mean age, 39.3 years; 58.8% women) were compared with a historic cohort of 77,809 patients with influenza (mean age, 39.7 years; 58.9% women).
- The incidence of ophthalmic conditions — retinal artery occlusion, retinal vein occlusion, retinal edema, vitreous hemorrhage, and neuro-ophthalmic manifestations — was assessed within 4 months of infection.
TAKEAWAY:
- Vaccinated patients with COVID had 32% lower odds of retinal edema (odds ratio [OR], 0.68; 99.5% CI, 0.54-0.85), 45% lower odds of vitreous hemorrhage (OR, 0.55; 99.5% CI, 0.44-0.68), and 40% lower odds of optic neuritis (OR, 0.60; 99.5% CI, 0.43-0.85) than unvaccinated patients with the disease.
- No significant differences were found in the incidence of retinal artery occlusion, retinal vein occlusion, or retinal hemorrhage between the vaccinated and unvaccinated cohorts.
- Patients with COVID had markedly higher odds of diplopia (OR, 1.89; 99.5% CI, 1.53-2.32) and cranial nerve VI palsy (OR, 3.19; 99.5% CI, 1.82-5.59) than those with influenza.
- The incidence of other neuro-ophthalmic manifestations and retinal complications was similar between patients with COVID and those with influenza.
IN PRACTICE:
“The complications we assessed were rare, though our results showed an increased incidence of retinal edema, vitreous hemorrhage, and optic neuritis in the nonvaccinated COVID-19 cohort,” the researchers reported.
“The increased incidence of retinal edema and vitreous hemorrhage in the nonvaccinated cohort suggests a potential for COVID-19 to affect posterior segment structures,” they added.
SOURCE:
This study was led by Alexander E. Azar, Case Western Reserve University School of Medicine, Cleveland. It was published online in Eye.
LIMITATIONS:
This study could not determine if vaccination against COVID could prevent ophthalmic manifestations. Vaccination status may have been underreported since many participants received COVID vaccines at pharmacies or community centers not directly documented in the electronic health records. The study’s timeframe only reflected data from early strains of SARS-CoV-2 between March 2020 and April 2021, potentially limiting generalizability to newer variants or later vaccination phases.
DISCLOSURES:
This study received support from the Clinical and Translational Science Collaborative of Cleveland, funded by the National Institutes of Health, National Center for Advancing Translational Science, and other sources. Some authors reported serving as consultants, participating in speakers’ bureaus, receiving personal fees, and having other ties with multiple pharmaceutical companies.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
Patients with COVID had a higher risk of developing diplopia and cranial nerve VI palsy than those with influenza. Compared with unvaccinated patients, recipients of mRNA vaccines against SARS-CoV-2 had a more than 30% reduced risk of developing posterior-segment complications including retinal edema, vitreous hemorrhage, and optic neuritis.
METHODOLOGY:
- Researchers conducted a retrospective cohort analysis of US electronic health records from March 2020 to April 2021 to assess eye complications after COVID and the effect of mRNA vaccination on them.
- They analyzed matched cohorts of 73,654 vaccinated patients with COVID (mean age, 60.6 years; 61.6% women) and 73,654 unvaccinated patients with the condition (mean age, 61.2 years; 62.8% women); vaccination status was determined based on recorded receipt of an mRNA vaccine.
- In a separate matched analysis, 77,809 patients with COVID (mean age, 39.3 years; 58.8% women) were compared with a historic cohort of 77,809 patients with influenza (mean age, 39.7 years; 58.9% women).
- The incidence of ophthalmic conditions — retinal artery occlusion, retinal vein occlusion, retinal edema, vitreous hemorrhage, and neuro-ophthalmic manifestations — was assessed within 4 months of infection.
TAKEAWAY:
- Vaccinated patients with COVID had 32% lower odds of retinal edema (odds ratio [OR], 0.68; 99.5% CI, 0.54-0.85), 45% lower odds of vitreous hemorrhage (OR, 0.55; 99.5% CI, 0.44-0.68), and 40% lower odds of optic neuritis (OR, 0.60; 99.5% CI, 0.43-0.85) than unvaccinated patients with the disease.
- No significant differences were found in the incidence of retinal artery occlusion, retinal vein occlusion, or retinal hemorrhage between the vaccinated and unvaccinated cohorts.
- Patients with COVID had markedly higher odds of diplopia (OR, 1.89; 99.5% CI, 1.53-2.32) and cranial nerve VI palsy (OR, 3.19; 99.5% CI, 1.82-5.59) than those with influenza.
- The incidence of other neuro-ophthalmic manifestations and retinal complications was similar between patients with COVID and those with influenza.
IN PRACTICE:
“The complications we assessed were rare, though our results showed an increased incidence of retinal edema, vitreous hemorrhage, and optic neuritis in the nonvaccinated COVID-19 cohort,” the researchers reported.
“The increased incidence of retinal edema and vitreous hemorrhage in the nonvaccinated cohort suggests a potential for COVID-19 to affect posterior segment structures,” they added.
SOURCE:
This study was led by Alexander E. Azar, Case Western Reserve University School of Medicine, Cleveland. It was published online in Eye.
LIMITATIONS:
This study could not determine if vaccination against COVID could prevent ophthalmic manifestations. Vaccination status may have been underreported since many participants received COVID vaccines at pharmacies or community centers not directly documented in the electronic health records. The study’s timeframe only reflected data from early strains of SARS-CoV-2 between March 2020 and April 2021, potentially limiting generalizability to newer variants or later vaccination phases.
DISCLOSURES:
This study received support from the Clinical and Translational Science Collaborative of Cleveland, funded by the National Institutes of Health, National Center for Advancing Translational Science, and other sources. Some authors reported serving as consultants, participating in speakers’ bureaus, receiving personal fees, and having other ties with multiple pharmaceutical companies.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
Patients with COVID had a higher risk of developing diplopia and cranial nerve VI palsy than those with influenza. Compared with unvaccinated patients, recipients of mRNA vaccines against SARS-CoV-2 had a more than 30% reduced risk of developing posterior-segment complications including retinal edema, vitreous hemorrhage, and optic neuritis.
METHODOLOGY:
- Researchers conducted a retrospective cohort analysis of US electronic health records from March 2020 to April 2021 to assess eye complications after COVID and the effect of mRNA vaccination on them.
- They analyzed matched cohorts of 73,654 vaccinated patients with COVID (mean age, 60.6 years; 61.6% women) and 73,654 unvaccinated patients with the condition (mean age, 61.2 years; 62.8% women); vaccination status was determined based on recorded receipt of an mRNA vaccine.
- In a separate matched analysis, 77,809 patients with COVID (mean age, 39.3 years; 58.8% women) were compared with a historic cohort of 77,809 patients with influenza (mean age, 39.7 years; 58.9% women).
- The incidence of ophthalmic conditions — retinal artery occlusion, retinal vein occlusion, retinal edema, vitreous hemorrhage, and neuro-ophthalmic manifestations — was assessed within 4 months of infection.
TAKEAWAY:
- Vaccinated patients with COVID had 32% lower odds of retinal edema (odds ratio [OR], 0.68; 99.5% CI, 0.54-0.85), 45% lower odds of vitreous hemorrhage (OR, 0.55; 99.5% CI, 0.44-0.68), and 40% lower odds of optic neuritis (OR, 0.60; 99.5% CI, 0.43-0.85) than unvaccinated patients with the disease.
- No significant differences were found in the incidence of retinal artery occlusion, retinal vein occlusion, or retinal hemorrhage between the vaccinated and unvaccinated cohorts.
- Patients with COVID had markedly higher odds of diplopia (OR, 1.89; 99.5% CI, 1.53-2.32) and cranial nerve VI palsy (OR, 3.19; 99.5% CI, 1.82-5.59) than those with influenza.
- The incidence of other neuro-ophthalmic manifestations and retinal complications was similar between patients with COVID and those with influenza.
IN PRACTICE:
“The complications we assessed were rare, though our results showed an increased incidence of retinal edema, vitreous hemorrhage, and optic neuritis in the nonvaccinated COVID-19 cohort,” the researchers reported.
“The increased incidence of retinal edema and vitreous hemorrhage in the nonvaccinated cohort suggests a potential for COVID-19 to affect posterior segment structures,” they added.
SOURCE:
This study was led by Alexander E. Azar, Case Western Reserve University School of Medicine, Cleveland. It was published online in Eye.
LIMITATIONS:
This study could not determine if vaccination against COVID could prevent ophthalmic manifestations. Vaccination status may have been underreported since many participants received COVID vaccines at pharmacies or community centers not directly documented in the electronic health records. The study’s timeframe only reflected data from early strains of SARS-CoV-2 between March 2020 and April 2021, potentially limiting generalizability to newer variants or later vaccination phases.
DISCLOSURES:
This study received support from the Clinical and Translational Science Collaborative of Cleveland, funded by the National Institutes of Health, National Center for Advancing Translational Science, and other sources. Some authors reported serving as consultants, participating in speakers’ bureaus, receiving personal fees, and having other ties with multiple pharmaceutical companies.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
Targeted Osteoporosis Program May Benefit At-Risk Older Men
Efforts to identify older men at risk for osteoporosis and treat those who are eligible received a boost from results reported from a Veterans Affairs (VA) study that showed a significant increase in screening, treatment, and medication adherence.
The cluster randomized trial used a centralized nurse-led intervention to assess men for traditional osteoporosis risk factors, offer bone density testing, and recommend treatment for eligible men. Over 2 years, the intervention group had a higher average femoral neck bone density than patients who underwent usual care.
“We designed this study to see if a risk factor-based approach, which is what most of the guidelines use, made sense and was feasible — that men would be accepting of screening and [the approach] would yield a similar proportion of people who need osteoporosis treatment as screening in women, which is widely recommended and implemented. And sure enough, we found that about 85% of the men in the VA primary care practices in our target age range of between 65 and 85 actually met criteria for screening, and over half of them had low bone mass. They were very accepting of screening, very accepting of treatment, and had excellent compliance rates. So, our study, we believe, supports the idea of identifying men with at least one risk factor for fracture and offering them osteoporosis screening starting at age 65, similar to what we do for women,” Cathleen S. Colón-Emeric, MD, MHS, said in an interview. She is the lead author of the study, a physician in the Durham VA Health Care System, and professor of medicine at Duke University School of Medicine, Durham, North Carolina.
“We were able to see a positive effect on bone density in the bone health group, compared with the usual care group, which suggests that if we followed these folks longer and had enough of them, we would be able to show a fracture reduction benefit,” Colón-Emeric said.
There have been few randomized trials of screening interventions in men, leading to inconsistencies in guidelines, according to the authors of the new study, published online in JAMA Internal Medicine . Both the US Preventive Services Task Force and the Veterans Health Administration National Center for Health Promotion and Disease Prevention consider there to be insufficient evidence to recommend for or against screening in men who have not experienced a fracture. Some professional societies recommend such screening, but there are inconsistencies in the recommended criteria, such as age range or risk factors.
Beyond the age of 50 years, one in five men will experience an osteoporosis-related fracture at some point in their life, according to a 2009 study. Treatment is inexpensive and effective in both men and women, and economic models suggest that screening using dual-energy x-ray absorptiometry (DXA) would be cost-effective. Still, screening is rare among men, with fewer than 10% of men getting screened before having an osteoporosis-related fracture.
“It’s important to screen men at risk for osteoporosis due to the dramatically increased mortality men suffer after a fragility fracture compared with women. Within 1 year of a hip fracture, mortality is as high as 36%. Studies have also shown that osteoporosis in men is undertreated, with only 10%-50% being prescribed antifracture treatment within 1 year of a hip fracture. Most individuals do not regain their prior level of function after a hip fracture,” said Joe C. Huang, MD, who was asked for comment. He is a clinical assistant professor of gerontology and geriatric medicine at Harborview Medical Center Senior Care Clinic and Healthy Bones Clinic in Seattle.
Details of the Intervention
The bone health service (BHS) intervention employed an electronic health record case-finding tool and a nurse care manager who undertook screening and treatment monitoring. They identified potential risk factors that included hyperthyroidism, hyperparathyroidism, rheumatoid arthritis, alcohol dependence, chronic lung disease, chronic liver disease, stroke, parkinsonism, prostate cancer, smoking, diabetes, pernicious anemia, gastrectomy, or high-risk medication use in at least 3 months of the prior 2 years. These medications included traditional antiepileptics, glucocorticoids, and androgen deprivation therapy.
The BHS nurse invited eligible men to be screened using an initial letter, followed by up to three phone calls. After DXA screening, the nurse scheduled an electronic consult with an osteoporosis expert, and patients with a T-score between -1 and -2.4 and an elevated 10-year fracture risk as measured by the Fracture Risk Assessment Tool were recommended for osteoporosis medication, vitamin D, and dietary or supplemental calcium. Following the prescription, the nurse provided patient education over the phone and mailed out written instructions. The nurse also made phone calls at 1 month, 6 months, and 12 months to encourage adherence and address common treatment barriers such as forgetting to take medication or dealing with gastrointestinal effects. The researchers recruited 38 primary care physicians from two VA health systems. The study included 3112 male veterans between the ages of 65 and 85 years (40.4% Black and 56% White). Nearly all participants (85.5%) had at least one indication for screening according to VA undersecretary guidelines, and almost a third (32.1%) had been prescribed androgen deprivation therapy, traditional antiepileptic drugs, or glucocorticoids.
Over a mean follow-up of 1.5 years, there was a much higher screening rate in the BHS group (49.2% vs 2.3%; P < .001), with a similar overall yield of DXA results recommending osteoporosis treatment (22.4% vs 27.2%). In the BHS group, 84.4% of patients who had treatment recommended followed through with treatment initiation. The mean persistence over follow-up was 657 days (SD, 366 days), and adherence was high with a mean proportion of days covered of 91.7%.
It was not possible to statistically compare adherence with the usual-care group because there were too few screened patients found to be eligible for treatment in that group, but the historic mean proportion of days covered at the two participating facilities was 52%.
After 2 years, the mean femoral neck T-score tested randomly in a subset of patients was better in the BHS arm, although it did not meet statistical significance according to the Bonferroni corrected criterion of P < .025 (-0.55 vs -0.70; P = .04). Fracture rates were similar between the two groups (1.8% vs 2.0%; P = .69).
Can the Findings Be Translated Across Clinics?
It remains to be seen how well the model could translate to other healthcare settings, according to Kenny Lin, MD, MPH, who was asked for comment on the study. “Outside of the VA health system and perhaps integrated HMOs [health maintenance organizations] such as Kaiser, Geisinger, etc., it seems unlikely that most primary care docs will have access to a centralized bone health service. Who’s going to pay for it? It leaves unanswered the question of whether it’s more efficient to address [osteoporosis] screening on a practice or population level. I suspect the latter is probably superior, but this study doesn’t provide any empiric evidence that this is so,” said Lin, associate director of the Penn Medicine Lancaster General Hospital’s Family Medicine Residency Program, Lancaster, Pennsylvania. The findings could help sway recommendations to screen men for osteoporosis, according to Susan Ott, MD, who was also asked for comment. Guideline committees “have been trying to be very scientific [about it]. I think they overdo it because they only look at one or two kinds of studies, and there are more kinds of science than just a randomized clinical trial. But they’re kind of stuck on that. The fact that this study was a randomized trial maybe they will finally change their recommendation, because there really shouldn’t be any difference in screening for men and for women. The men are actually discriminated against,” said Ott, emeritus professor of medicine at the University of Washington, Seattle.
In fact, she noted that the risks for men are similar to those for women, except that men tend to develop issues 5-10 years later in life. To screen and treat men, healthcare systems can “do the same thing they do with women. Just change the age range,” Ott said.
Lin sounded a different note, suggesting that the focus should remain on improvement of screening and treatment adherence in women. “We know that up to two thirds of women discontinue osteoporosis drugs within a year, and if we can’t figure out how to improve abysmal adherence in women, it’s unlikely we will persuade enough men to take these drugs to make a difference,” he said.
The study was funded by a grant from the VA Health Systems Research. Colón-Emeric, Lin, Ott, and Huang reported having no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Efforts to identify older men at risk for osteoporosis and treat those who are eligible received a boost from results reported from a Veterans Affairs (VA) study that showed a significant increase in screening, treatment, and medication adherence.
The cluster randomized trial used a centralized nurse-led intervention to assess men for traditional osteoporosis risk factors, offer bone density testing, and recommend treatment for eligible men. Over 2 years, the intervention group had a higher average femoral neck bone density than patients who underwent usual care.
“We designed this study to see if a risk factor-based approach, which is what most of the guidelines use, made sense and was feasible — that men would be accepting of screening and [the approach] would yield a similar proportion of people who need osteoporosis treatment as screening in women, which is widely recommended and implemented. And sure enough, we found that about 85% of the men in the VA primary care practices in our target age range of between 65 and 85 actually met criteria for screening, and over half of them had low bone mass. They were very accepting of screening, very accepting of treatment, and had excellent compliance rates. So, our study, we believe, supports the idea of identifying men with at least one risk factor for fracture and offering them osteoporosis screening starting at age 65, similar to what we do for women,” Cathleen S. Colón-Emeric, MD, MHS, said in an interview. She is the lead author of the study, a physician in the Durham VA Health Care System, and professor of medicine at Duke University School of Medicine, Durham, North Carolina.
“We were able to see a positive effect on bone density in the bone health group, compared with the usual care group, which suggests that if we followed these folks longer and had enough of them, we would be able to show a fracture reduction benefit,” Colón-Emeric said.
There have been few randomized trials of screening interventions in men, leading to inconsistencies in guidelines, according to the authors of the new study, published online in JAMA Internal Medicine . Both the US Preventive Services Task Force and the Veterans Health Administration National Center for Health Promotion and Disease Prevention consider there to be insufficient evidence to recommend for or against screening in men who have not experienced a fracture. Some professional societies recommend such screening, but there are inconsistencies in the recommended criteria, such as age range or risk factors.
Beyond the age of 50 years, one in five men will experience an osteoporosis-related fracture at some point in their life, according to a 2009 study. Treatment is inexpensive and effective in both men and women, and economic models suggest that screening using dual-energy x-ray absorptiometry (DXA) would be cost-effective. Still, screening is rare among men, with fewer than 10% of men getting screened before having an osteoporosis-related fracture.
“It’s important to screen men at risk for osteoporosis due to the dramatically increased mortality men suffer after a fragility fracture compared with women. Within 1 year of a hip fracture, mortality is as high as 36%. Studies have also shown that osteoporosis in men is undertreated, with only 10%-50% being prescribed antifracture treatment within 1 year of a hip fracture. Most individuals do not regain their prior level of function after a hip fracture,” said Joe C. Huang, MD, who was asked for comment. He is a clinical assistant professor of gerontology and geriatric medicine at Harborview Medical Center Senior Care Clinic and Healthy Bones Clinic in Seattle.
Details of the Intervention
The bone health service (BHS) intervention employed an electronic health record case-finding tool and a nurse care manager who undertook screening and treatment monitoring. They identified potential risk factors that included hyperthyroidism, hyperparathyroidism, rheumatoid arthritis, alcohol dependence, chronic lung disease, chronic liver disease, stroke, parkinsonism, prostate cancer, smoking, diabetes, pernicious anemia, gastrectomy, or high-risk medication use in at least 3 months of the prior 2 years. These medications included traditional antiepileptics, glucocorticoids, and androgen deprivation therapy.
The BHS nurse invited eligible men to be screened using an initial letter, followed by up to three phone calls. After DXA screening, the nurse scheduled an electronic consult with an osteoporosis expert, and patients with a T-score between -1 and -2.4 and an elevated 10-year fracture risk as measured by the Fracture Risk Assessment Tool were recommended for osteoporosis medication, vitamin D, and dietary or supplemental calcium. Following the prescription, the nurse provided patient education over the phone and mailed out written instructions. The nurse also made phone calls at 1 month, 6 months, and 12 months to encourage adherence and address common treatment barriers such as forgetting to take medication or dealing with gastrointestinal effects. The researchers recruited 38 primary care physicians from two VA health systems. The study included 3112 male veterans between the ages of 65 and 85 years (40.4% Black and 56% White). Nearly all participants (85.5%) had at least one indication for screening according to VA undersecretary guidelines, and almost a third (32.1%) had been prescribed androgen deprivation therapy, traditional antiepileptic drugs, or glucocorticoids.
Over a mean follow-up of 1.5 years, there was a much higher screening rate in the BHS group (49.2% vs 2.3%; P < .001), with a similar overall yield of DXA results recommending osteoporosis treatment (22.4% vs 27.2%). In the BHS group, 84.4% of patients who had treatment recommended followed through with treatment initiation. The mean persistence over follow-up was 657 days (SD, 366 days), and adherence was high with a mean proportion of days covered of 91.7%.
It was not possible to statistically compare adherence with the usual-care group because there were too few screened patients found to be eligible for treatment in that group, but the historic mean proportion of days covered at the two participating facilities was 52%.
After 2 years, the mean femoral neck T-score tested randomly in a subset of patients was better in the BHS arm, although it did not meet statistical significance according to the Bonferroni corrected criterion of P < .025 (-0.55 vs -0.70; P = .04). Fracture rates were similar between the two groups (1.8% vs 2.0%; P = .69).
Can the Findings Be Translated Across Clinics?
It remains to be seen how well the model could translate to other healthcare settings, according to Kenny Lin, MD, MPH, who was asked for comment on the study. “Outside of the VA health system and perhaps integrated HMOs [health maintenance organizations] such as Kaiser, Geisinger, etc., it seems unlikely that most primary care docs will have access to a centralized bone health service. Who’s going to pay for it? It leaves unanswered the question of whether it’s more efficient to address [osteoporosis] screening on a practice or population level. I suspect the latter is probably superior, but this study doesn’t provide any empiric evidence that this is so,” said Lin, associate director of the Penn Medicine Lancaster General Hospital’s Family Medicine Residency Program, Lancaster, Pennsylvania. The findings could help sway recommendations to screen men for osteoporosis, according to Susan Ott, MD, who was also asked for comment. Guideline committees “have been trying to be very scientific [about it]. I think they overdo it because they only look at one or two kinds of studies, and there are more kinds of science than just a randomized clinical trial. But they’re kind of stuck on that. The fact that this study was a randomized trial maybe they will finally change their recommendation, because there really shouldn’t be any difference in screening for men and for women. The men are actually discriminated against,” said Ott, emeritus professor of medicine at the University of Washington, Seattle.
In fact, she noted that the risks for men are similar to those for women, except that men tend to develop issues 5-10 years later in life. To screen and treat men, healthcare systems can “do the same thing they do with women. Just change the age range,” Ott said.
Lin sounded a different note, suggesting that the focus should remain on improvement of screening and treatment adherence in women. “We know that up to two thirds of women discontinue osteoporosis drugs within a year, and if we can’t figure out how to improve abysmal adherence in women, it’s unlikely we will persuade enough men to take these drugs to make a difference,” he said.
The study was funded by a grant from the VA Health Systems Research. Colón-Emeric, Lin, Ott, and Huang reported having no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Efforts to identify older men at risk for osteoporosis and treat those who are eligible received a boost from results reported from a Veterans Affairs (VA) study that showed a significant increase in screening, treatment, and medication adherence.
The cluster randomized trial used a centralized nurse-led intervention to assess men for traditional osteoporosis risk factors, offer bone density testing, and recommend treatment for eligible men. Over 2 years, the intervention group had a higher average femoral neck bone density than patients who underwent usual care.
“We designed this study to see if a risk factor-based approach, which is what most of the guidelines use, made sense and was feasible — that men would be accepting of screening and [the approach] would yield a similar proportion of people who need osteoporosis treatment as screening in women, which is widely recommended and implemented. And sure enough, we found that about 85% of the men in the VA primary care practices in our target age range of between 65 and 85 actually met criteria for screening, and over half of them had low bone mass. They were very accepting of screening, very accepting of treatment, and had excellent compliance rates. So, our study, we believe, supports the idea of identifying men with at least one risk factor for fracture and offering them osteoporosis screening starting at age 65, similar to what we do for women,” Cathleen S. Colón-Emeric, MD, MHS, said in an interview. She is the lead author of the study, a physician in the Durham VA Health Care System, and professor of medicine at Duke University School of Medicine, Durham, North Carolina.
“We were able to see a positive effect on bone density in the bone health group, compared with the usual care group, which suggests that if we followed these folks longer and had enough of them, we would be able to show a fracture reduction benefit,” Colón-Emeric said.
There have been few randomized trials of screening interventions in men, leading to inconsistencies in guidelines, according to the authors of the new study, published online in JAMA Internal Medicine . Both the US Preventive Services Task Force and the Veterans Health Administration National Center for Health Promotion and Disease Prevention consider there to be insufficient evidence to recommend for or against screening in men who have not experienced a fracture. Some professional societies recommend such screening, but there are inconsistencies in the recommended criteria, such as age range or risk factors.
Beyond the age of 50 years, one in five men will experience an osteoporosis-related fracture at some point in their life, according to a 2009 study. Treatment is inexpensive and effective in both men and women, and economic models suggest that screening using dual-energy x-ray absorptiometry (DXA) would be cost-effective. Still, screening is rare among men, with fewer than 10% of men getting screened before having an osteoporosis-related fracture.
“It’s important to screen men at risk for osteoporosis due to the dramatically increased mortality men suffer after a fragility fracture compared with women. Within 1 year of a hip fracture, mortality is as high as 36%. Studies have also shown that osteoporosis in men is undertreated, with only 10%-50% being prescribed antifracture treatment within 1 year of a hip fracture. Most individuals do not regain their prior level of function after a hip fracture,” said Joe C. Huang, MD, who was asked for comment. He is a clinical assistant professor of gerontology and geriatric medicine at Harborview Medical Center Senior Care Clinic and Healthy Bones Clinic in Seattle.
Details of the Intervention
The bone health service (BHS) intervention employed an electronic health record case-finding tool and a nurse care manager who undertook screening and treatment monitoring. They identified potential risk factors that included hyperthyroidism, hyperparathyroidism, rheumatoid arthritis, alcohol dependence, chronic lung disease, chronic liver disease, stroke, parkinsonism, prostate cancer, smoking, diabetes, pernicious anemia, gastrectomy, or high-risk medication use in at least 3 months of the prior 2 years. These medications included traditional antiepileptics, glucocorticoids, and androgen deprivation therapy.
The BHS nurse invited eligible men to be screened using an initial letter, followed by up to three phone calls. After DXA screening, the nurse scheduled an electronic consult with an osteoporosis expert, and patients with a T-score between -1 and -2.4 and an elevated 10-year fracture risk as measured by the Fracture Risk Assessment Tool were recommended for osteoporosis medication, vitamin D, and dietary or supplemental calcium. Following the prescription, the nurse provided patient education over the phone and mailed out written instructions. The nurse also made phone calls at 1 month, 6 months, and 12 months to encourage adherence and address common treatment barriers such as forgetting to take medication or dealing with gastrointestinal effects. The researchers recruited 38 primary care physicians from two VA health systems. The study included 3112 male veterans between the ages of 65 and 85 years (40.4% Black and 56% White). Nearly all participants (85.5%) had at least one indication for screening according to VA undersecretary guidelines, and almost a third (32.1%) had been prescribed androgen deprivation therapy, traditional antiepileptic drugs, or glucocorticoids.
Over a mean follow-up of 1.5 years, there was a much higher screening rate in the BHS group (49.2% vs 2.3%; P < .001), with a similar overall yield of DXA results recommending osteoporosis treatment (22.4% vs 27.2%). In the BHS group, 84.4% of patients who had treatment recommended followed through with treatment initiation. The mean persistence over follow-up was 657 days (SD, 366 days), and adherence was high with a mean proportion of days covered of 91.7%.
It was not possible to statistically compare adherence with the usual-care group because there were too few screened patients found to be eligible for treatment in that group, but the historic mean proportion of days covered at the two participating facilities was 52%.
After 2 years, the mean femoral neck T-score tested randomly in a subset of patients was better in the BHS arm, although it did not meet statistical significance according to the Bonferroni corrected criterion of P < .025 (-0.55 vs -0.70; P = .04). Fracture rates were similar between the two groups (1.8% vs 2.0%; P = .69).
Can the Findings Be Translated Across Clinics?
It remains to be seen how well the model could translate to other healthcare settings, according to Kenny Lin, MD, MPH, who was asked for comment on the study. “Outside of the VA health system and perhaps integrated HMOs [health maintenance organizations] such as Kaiser, Geisinger, etc., it seems unlikely that most primary care docs will have access to a centralized bone health service. Who’s going to pay for it? It leaves unanswered the question of whether it’s more efficient to address [osteoporosis] screening on a practice or population level. I suspect the latter is probably superior, but this study doesn’t provide any empiric evidence that this is so,” said Lin, associate director of the Penn Medicine Lancaster General Hospital’s Family Medicine Residency Program, Lancaster, Pennsylvania. The findings could help sway recommendations to screen men for osteoporosis, according to Susan Ott, MD, who was also asked for comment. Guideline committees “have been trying to be very scientific [about it]. I think they overdo it because they only look at one or two kinds of studies, and there are more kinds of science than just a randomized clinical trial. But they’re kind of stuck on that. The fact that this study was a randomized trial maybe they will finally change their recommendation, because there really shouldn’t be any difference in screening for men and for women. The men are actually discriminated against,” said Ott, emeritus professor of medicine at the University of Washington, Seattle.
In fact, she noted that the risks for men are similar to those for women, except that men tend to develop issues 5-10 years later in life. To screen and treat men, healthcare systems can “do the same thing they do with women. Just change the age range,” Ott said.
Lin sounded a different note, suggesting that the focus should remain on improvement of screening and treatment adherence in women. “We know that up to two thirds of women discontinue osteoporosis drugs within a year, and if we can’t figure out how to improve abysmal adherence in women, it’s unlikely we will persuade enough men to take these drugs to make a difference,” he said.
The study was funded by a grant from the VA Health Systems Research. Colón-Emeric, Lin, Ott, and Huang reported having no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
New York GI Links Health Equity and CRC Screening
Pascale M. White, MD, MBA, MS never tires of excising precancerous polyps.
“To know that I have removed something that could have been potentially dangerous to this patient in years to come, that wasn’t causing any symptoms but silently lurking there” is a great feeling, said Dr. White, an associate professor with dual appointments in the divisions of gastroenterology and liver diseases at the Icahn School of Medicine at Mount Sinai, New York.
“When I do procedures, I always go in with the mindset that this could be a lifesaving procedure for this patient. And that definitely keeps me excited about the field,” she said.
Colorectal cancer is preventable, but when it comes to screening, there are large health disparities. African Americans are 20% more likely to get diagnosed with colorectal cancer and 40% more likely to die from the disease. “Knowing that there are low screening rates among this population, there’s a lot of work to be done with mitigating those disparities,” said Dr. White, who has made it her life’s work to expand access to care and address health inequities.
Dr. White is an inaugural director of Health Equity in Action for Liver and Digestive Diseases (HEALD) and an inaugural fellow of the United Hospital Fund’s Health Equity Fellowship. In 2025, she received the AGA-Pfizer Beacon of Hope Award, which celebrates three women in the GI field who have played a key role in advancing gender and health equity in medicine.
“Through the United Hospital Fund’s Health Equity Fellowship, I have partnered with an East Harlem community health center to conduct seminars and tailor a one-page shared decision tool for colorectal cancer screening to jumpstart discussions on screening choices between patients and providers,” said Dr. White.
In an interview, she offered more details about her mission to connect with communities to improve screening rates for colorectal cancer.
Can you discuss your work with HEALD?
Dr. White: HEALD is a growing initiative to identify and address any access barriers to our screening programs. At this time, I’m working to identify how patients are getting referred to us in our division for colorectal cancer screening and how we can create a more streamlined and robust pathway for patients in the community, namely at federally qualified health centers in East Harlem.
You co-founded the Association of Black Gastroenterologists and Hepatologists (ABGH) in 2021. What are you hoping to accomplish with this organization?
Dr. White: ABGH was co-founded by eleven of us from across the country for the purpose of addressing health care disparities in GI and liver diseases that disproportionately affect Black patient populations. Our mission is to promote health equity, advance science and develop the careers of Black gastroenterologists, hepatologists, and scientists.
Our mentorship program is one way we give back to incoming residents who are interested in pursuing a career in GI. The Nurturing, Excelling, and Unifying Sisters in Medicine (NEXUS) conference centers the perspectives of Black women in medicine from all specialties. The ABGH Summit is an educational conference that features renowned experts in the health equity space.
But at the center of it all is our community outreach. When we started the organization after Chadwick Boseman’s death during the height of the COVID pandemic, all our community events were held over Zoom. Now with our in-person events you can feel the energy in the room. Our main community facing event is called Bustin’ A Gut. It’s a genius combination of comedy and medical education. We have a panel of physicians and comedians. The physicians talk about a range of GI topics such as colorectal cancer screening choices, alarm signs or symptoms of colon cancer, nutrition, and general gut health. The community members feel comfortable asking their questions and the comedians help keep the conversation entertaining and lighthearted. It’s a true laugh and learn event.
How did you become interested in health equity? Was there a specific event or circumstance you could share?
Dr. White: It was my residency training at New York University and my experiences at Bellevue Hospital that really introduced me to a place where everyone could get care. Whether you are coming from another country or right up the street, Bellevue saw everyone who walked through its doors. This is in deep contrast to the vast majority of hospitals where if you do not have insurance, you cannot be seen. Then there are people who have access to care but are overwhelmed by the complexities of the medical system.
Consider colorectal cancer, for example. It is a preventable disease, yet most people aren’t getting screened because they either don’t know they should, they are fearful of the process, or they don’t know how to go about getting the tests done. These are namely knowledge barriers that we can address. I thought: If there’s something I could do to help patients learn about colorectal cancer screening and how they can take steps to prevent this disease, then that’s how I want to spend my career.
You created the Direct Access GI Clinic (DAGIC), one of the projects that led to the AGA-Pfizer Beacon of Hope Award for Gender and Health Equity. How does DAGIC reduce wait times and improve endoscopic care coordination for underserved, high-risk patients?
Dr. White: I developed and implemented a clinic workflow that identified high-risk patients who were sent for direct access procedures but who needed office consultations prior to their procedures. These were the sickest of the sickest patients that needed to be prioritized. Working with my nurse practitioner and office ncurse, we triaged these patients and carved out dedicated time in the week where only DAGIC patients were scheduled.
Creating this direct workflow meant that these patients no longer had to wait three months. They were waiting at most, two to three weeks to be seen. I don’t take for granted that one change in a system can lead to impactful outcomes in patient care and access.
You also co-authored an update to the American College of Gastroenterology’s colorectal cancer screening guidelines for African Americans. Is there anything unique and important that’s worth noting?
Dr. White: We updated those guidelines to include physician recommendation as a potential barrier to screening. We know that patients are more likely to be screened if they are recommended to do so by their physician. Yet, some patients are less likely to receive a physician recommendation for screening. We need to dive deeper into the reasons why this is happening. And if there are any gaps, for example in physician knowledge, that’s something we should readily address.
One of your interests is guiding students, residents, and fellows. What advice would you give to aspiring medical students?
Dr. White: Keep an open mind and explore all your options before committing to a specialty. If you find the field exciting and you are motivated to spend time learning more about it, seek opportunities to conduct research and find a mentor that can further guide you on your journey.
Lightning Round
What’s your favorite season of the year?
Fall
What’s your favorite way to spend a weekend?
Playing golf
If you could have dinner with any historical figure, who would it be?
Barack Obama
What’s your go-to karaoke song?
Livin’ on a Prayer by Bon Jovi
What’s one thing on your bucket list?
Travel to Rome
If you could instantly learn any skill, what would it be?
Speak Mandarin
What’s your favorite holiday tradition?
Watching Hallmark movies with my daughter
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
Progress, not perfection
Expand Your GI Community with AGA Membership
Renew your AGA membership by Dec. 31 to continue getting to know your AGA Gastro Squad through our monthly column. AGA member spotlights introduce members to one another while recognizing their accomplishments.
Want to recognize a colleague? Submit a nomination to GINews@gastro.org.
Pascale M. White, MD, MBA, MS never tires of excising precancerous polyps.
“To know that I have removed something that could have been potentially dangerous to this patient in years to come, that wasn’t causing any symptoms but silently lurking there” is a great feeling, said Dr. White, an associate professor with dual appointments in the divisions of gastroenterology and liver diseases at the Icahn School of Medicine at Mount Sinai, New York.
“When I do procedures, I always go in with the mindset that this could be a lifesaving procedure for this patient. And that definitely keeps me excited about the field,” she said.
Colorectal cancer is preventable, but when it comes to screening, there are large health disparities. African Americans are 20% more likely to get diagnosed with colorectal cancer and 40% more likely to die from the disease. “Knowing that there are low screening rates among this population, there’s a lot of work to be done with mitigating those disparities,” said Dr. White, who has made it her life’s work to expand access to care and address health inequities.
Dr. White is an inaugural director of Health Equity in Action for Liver and Digestive Diseases (HEALD) and an inaugural fellow of the United Hospital Fund’s Health Equity Fellowship. In 2025, she received the AGA-Pfizer Beacon of Hope Award, which celebrates three women in the GI field who have played a key role in advancing gender and health equity in medicine.
“Through the United Hospital Fund’s Health Equity Fellowship, I have partnered with an East Harlem community health center to conduct seminars and tailor a one-page shared decision tool for colorectal cancer screening to jumpstart discussions on screening choices between patients and providers,” said Dr. White.
In an interview, she offered more details about her mission to connect with communities to improve screening rates for colorectal cancer.
Can you discuss your work with HEALD?
Dr. White: HEALD is a growing initiative to identify and address any access barriers to our screening programs. At this time, I’m working to identify how patients are getting referred to us in our division for colorectal cancer screening and how we can create a more streamlined and robust pathway for patients in the community, namely at federally qualified health centers in East Harlem.
You co-founded the Association of Black Gastroenterologists and Hepatologists (ABGH) in 2021. What are you hoping to accomplish with this organization?
Dr. White: ABGH was co-founded by eleven of us from across the country for the purpose of addressing health care disparities in GI and liver diseases that disproportionately affect Black patient populations. Our mission is to promote health equity, advance science and develop the careers of Black gastroenterologists, hepatologists, and scientists.
Our mentorship program is one way we give back to incoming residents who are interested in pursuing a career in GI. The Nurturing, Excelling, and Unifying Sisters in Medicine (NEXUS) conference centers the perspectives of Black women in medicine from all specialties. The ABGH Summit is an educational conference that features renowned experts in the health equity space.
But at the center of it all is our community outreach. When we started the organization after Chadwick Boseman’s death during the height of the COVID pandemic, all our community events were held over Zoom. Now with our in-person events you can feel the energy in the room. Our main community facing event is called Bustin’ A Gut. It’s a genius combination of comedy and medical education. We have a panel of physicians and comedians. The physicians talk about a range of GI topics such as colorectal cancer screening choices, alarm signs or symptoms of colon cancer, nutrition, and general gut health. The community members feel comfortable asking their questions and the comedians help keep the conversation entertaining and lighthearted. It’s a true laugh and learn event.
How did you become interested in health equity? Was there a specific event or circumstance you could share?
Dr. White: It was my residency training at New York University and my experiences at Bellevue Hospital that really introduced me to a place where everyone could get care. Whether you are coming from another country or right up the street, Bellevue saw everyone who walked through its doors. This is in deep contrast to the vast majority of hospitals where if you do not have insurance, you cannot be seen. Then there are people who have access to care but are overwhelmed by the complexities of the medical system.
Consider colorectal cancer, for example. It is a preventable disease, yet most people aren’t getting screened because they either don’t know they should, they are fearful of the process, or they don’t know how to go about getting the tests done. These are namely knowledge barriers that we can address. I thought: If there’s something I could do to help patients learn about colorectal cancer screening and how they can take steps to prevent this disease, then that’s how I want to spend my career.
You created the Direct Access GI Clinic (DAGIC), one of the projects that led to the AGA-Pfizer Beacon of Hope Award for Gender and Health Equity. How does DAGIC reduce wait times and improve endoscopic care coordination for underserved, high-risk patients?
Dr. White: I developed and implemented a clinic workflow that identified high-risk patients who were sent for direct access procedures but who needed office consultations prior to their procedures. These were the sickest of the sickest patients that needed to be prioritized. Working with my nurse practitioner and office ncurse, we triaged these patients and carved out dedicated time in the week where only DAGIC patients were scheduled.
Creating this direct workflow meant that these patients no longer had to wait three months. They were waiting at most, two to three weeks to be seen. I don’t take for granted that one change in a system can lead to impactful outcomes in patient care and access.
You also co-authored an update to the American College of Gastroenterology’s colorectal cancer screening guidelines for African Americans. Is there anything unique and important that’s worth noting?
Dr. White: We updated those guidelines to include physician recommendation as a potential barrier to screening. We know that patients are more likely to be screened if they are recommended to do so by their physician. Yet, some patients are less likely to receive a physician recommendation for screening. We need to dive deeper into the reasons why this is happening. And if there are any gaps, for example in physician knowledge, that’s something we should readily address.
One of your interests is guiding students, residents, and fellows. What advice would you give to aspiring medical students?
Dr. White: Keep an open mind and explore all your options before committing to a specialty. If you find the field exciting and you are motivated to spend time learning more about it, seek opportunities to conduct research and find a mentor that can further guide you on your journey.
Lightning Round
What’s your favorite season of the year?
Fall
What’s your favorite way to spend a weekend?
Playing golf
If you could have dinner with any historical figure, who would it be?
Barack Obama
What’s your go-to karaoke song?
Livin’ on a Prayer by Bon Jovi
What’s one thing on your bucket list?
Travel to Rome
If you could instantly learn any skill, what would it be?
Speak Mandarin
What’s your favorite holiday tradition?
Watching Hallmark movies with my daughter
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
Progress, not perfection
Expand Your GI Community with AGA Membership
Renew your AGA membership by Dec. 31 to continue getting to know your AGA Gastro Squad through our monthly column. AGA member spotlights introduce members to one another while recognizing their accomplishments.
Want to recognize a colleague? Submit a nomination to GINews@gastro.org.
Pascale M. White, MD, MBA, MS never tires of excising precancerous polyps.
“To know that I have removed something that could have been potentially dangerous to this patient in years to come, that wasn’t causing any symptoms but silently lurking there” is a great feeling, said Dr. White, an associate professor with dual appointments in the divisions of gastroenterology and liver diseases at the Icahn School of Medicine at Mount Sinai, New York.
“When I do procedures, I always go in with the mindset that this could be a lifesaving procedure for this patient. And that definitely keeps me excited about the field,” she said.
Colorectal cancer is preventable, but when it comes to screening, there are large health disparities. African Americans are 20% more likely to get diagnosed with colorectal cancer and 40% more likely to die from the disease. “Knowing that there are low screening rates among this population, there’s a lot of work to be done with mitigating those disparities,” said Dr. White, who has made it her life’s work to expand access to care and address health inequities.
Dr. White is an inaugural director of Health Equity in Action for Liver and Digestive Diseases (HEALD) and an inaugural fellow of the United Hospital Fund’s Health Equity Fellowship. In 2025, she received the AGA-Pfizer Beacon of Hope Award, which celebrates three women in the GI field who have played a key role in advancing gender and health equity in medicine.
“Through the United Hospital Fund’s Health Equity Fellowship, I have partnered with an East Harlem community health center to conduct seminars and tailor a one-page shared decision tool for colorectal cancer screening to jumpstart discussions on screening choices between patients and providers,” said Dr. White.
In an interview, she offered more details about her mission to connect with communities to improve screening rates for colorectal cancer.
Can you discuss your work with HEALD?
Dr. White: HEALD is a growing initiative to identify and address any access barriers to our screening programs. At this time, I’m working to identify how patients are getting referred to us in our division for colorectal cancer screening and how we can create a more streamlined and robust pathway for patients in the community, namely at federally qualified health centers in East Harlem.
You co-founded the Association of Black Gastroenterologists and Hepatologists (ABGH) in 2021. What are you hoping to accomplish with this organization?
Dr. White: ABGH was co-founded by eleven of us from across the country for the purpose of addressing health care disparities in GI and liver diseases that disproportionately affect Black patient populations. Our mission is to promote health equity, advance science and develop the careers of Black gastroenterologists, hepatologists, and scientists.
Our mentorship program is one way we give back to incoming residents who are interested in pursuing a career in GI. The Nurturing, Excelling, and Unifying Sisters in Medicine (NEXUS) conference centers the perspectives of Black women in medicine from all specialties. The ABGH Summit is an educational conference that features renowned experts in the health equity space.
But at the center of it all is our community outreach. When we started the organization after Chadwick Boseman’s death during the height of the COVID pandemic, all our community events were held over Zoom. Now with our in-person events you can feel the energy in the room. Our main community facing event is called Bustin’ A Gut. It’s a genius combination of comedy and medical education. We have a panel of physicians and comedians. The physicians talk about a range of GI topics such as colorectal cancer screening choices, alarm signs or symptoms of colon cancer, nutrition, and general gut health. The community members feel comfortable asking their questions and the comedians help keep the conversation entertaining and lighthearted. It’s a true laugh and learn event.
How did you become interested in health equity? Was there a specific event or circumstance you could share?
Dr. White: It was my residency training at New York University and my experiences at Bellevue Hospital that really introduced me to a place where everyone could get care. Whether you are coming from another country or right up the street, Bellevue saw everyone who walked through its doors. This is in deep contrast to the vast majority of hospitals where if you do not have insurance, you cannot be seen. Then there are people who have access to care but are overwhelmed by the complexities of the medical system.
Consider colorectal cancer, for example. It is a preventable disease, yet most people aren’t getting screened because they either don’t know they should, they are fearful of the process, or they don’t know how to go about getting the tests done. These are namely knowledge barriers that we can address. I thought: If there’s something I could do to help patients learn about colorectal cancer screening and how they can take steps to prevent this disease, then that’s how I want to spend my career.
You created the Direct Access GI Clinic (DAGIC), one of the projects that led to the AGA-Pfizer Beacon of Hope Award for Gender and Health Equity. How does DAGIC reduce wait times and improve endoscopic care coordination for underserved, high-risk patients?
Dr. White: I developed and implemented a clinic workflow that identified high-risk patients who were sent for direct access procedures but who needed office consultations prior to their procedures. These were the sickest of the sickest patients that needed to be prioritized. Working with my nurse practitioner and office ncurse, we triaged these patients and carved out dedicated time in the week where only DAGIC patients were scheduled.
Creating this direct workflow meant that these patients no longer had to wait three months. They were waiting at most, two to three weeks to be seen. I don’t take for granted that one change in a system can lead to impactful outcomes in patient care and access.
You also co-authored an update to the American College of Gastroenterology’s colorectal cancer screening guidelines for African Americans. Is there anything unique and important that’s worth noting?
Dr. White: We updated those guidelines to include physician recommendation as a potential barrier to screening. We know that patients are more likely to be screened if they are recommended to do so by their physician. Yet, some patients are less likely to receive a physician recommendation for screening. We need to dive deeper into the reasons why this is happening. And if there are any gaps, for example in physician knowledge, that’s something we should readily address.
One of your interests is guiding students, residents, and fellows. What advice would you give to aspiring medical students?
Dr. White: Keep an open mind and explore all your options before committing to a specialty. If you find the field exciting and you are motivated to spend time learning more about it, seek opportunities to conduct research and find a mentor that can further guide you on your journey.
Lightning Round
What’s your favorite season of the year?
Fall
What’s your favorite way to spend a weekend?
Playing golf
If you could have dinner with any historical figure, who would it be?
Barack Obama
What’s your go-to karaoke song?
Livin’ on a Prayer by Bon Jovi
What’s one thing on your bucket list?
Travel to Rome
If you could instantly learn any skill, what would it be?
Speak Mandarin
What’s your favorite holiday tradition?
Watching Hallmark movies with my daughter
Are you a planner or more spontaneous?
Planner
What’s the best piece of advice you’ve ever received?
Progress, not perfection
Expand Your GI Community with AGA Membership
Renew your AGA membership by Dec. 31 to continue getting to know your AGA Gastro Squad through our monthly column. AGA member spotlights introduce members to one another while recognizing their accomplishments.
Want to recognize a colleague? Submit a nomination to GINews@gastro.org.

Team-Based Care is Crucial for Head-and-Neck Cancer Cases
Team-Based Care is Crucial for Head-and-Neck Cancer Cases
PHOENIX – A 70-year-old Vietnam veteran with oropharyngeal cancer presented challenges beyond his disease.
He couldn’t afford transportation for daily radiation treatments and had lost > 10% of his body weight due to pain and eating difficulties, recalled radiation oncologist Vinita Takiar, MD, PhD, in a presentation at the annual meeting of the Association of VA Hematology/Oncology.
To make matters more difficult, his wife held medical power of attorney despite his apparent competence to make decisions, said Takiar, who formerly worked with the US Department of Veterans Affairs (VA) Cincinnati Healthcare System and is now chair of radiation oncology at Penn State University.
All these factors would likely have derailed his treatment if not for a coordinated team intervention, Takiar said. Fortunately, the clinic launched a multifaceted effort involving representatives from the social work, dentistry, ethics, nutrition, and chaplaincy departments.
When surgery became impossible because the patient couldn’t lie on the operating table for adequate tumor exposure, she said, the existing team framework enabled a seamless and rapid transition to radiation with concurrent chemotherapy.
The patient completed treatment with an excellent response, offering a lesson in the importance of multidisciplinary care in head-and-neck cancers, she said.
In fact, when it comes to these forms of cancer, coordinated care “is probably more impactful than any treatment that we’re going to come up with,” she said. “The data show that when we do multidisciplinary care and we do it well, it actually improves the patient experience and outcomes.”
As Takiar noted, teamwork matters in many ways. It leads to better logistics and can address disparities, reduce financial burden and stigma, and even increase clinical trial involvement.
She pointed to studies linking teamwork to better outcomes, support for patients, and overall survival.
Takiar highlighted different parts of teams headed by radiation oncologists who act as “a node to improve multimodal care delivery.”
Speech and swallowing specialists, for example, are helpful in head-and-neck cancer because “there’s an impact on speech, swallowing, and appearance. Our patients don’t want to go out to dinner with friends because they can’t do it.”
Dentists and prosthodontists are key team members too: “I have dentists who have my cell phone number. They just call me: ‘Can I do this extraction? Was this in your radiation field? What was the dose?’”
Other team members include ear, nose, and throat specialists, palliative and supportive care specialists, medical oncologists, nurses, pathologists, transportation workers, and service connection specialists. She noted that previous military experience can affect radiation therapy. For example, the physical restraints required during treatment present particular challenges for veterans who’ve had wartime trauma. These patients may require therapy adjustments.
What’s next on the horizon? Takiar highlighted precision oncology and molecular profiling, artificial intelligence in care decisions and in radiation planning, telemedicine and virtual tumor boards, and expanded survivorship programs.
As for now, she urged colleagues to not be afraid to chat with radiation oncologists. “Please talk to us. We prioritize open communication and shared decision-making with the entire team,” she said. “If you see something and think your radiation oncologist should know about it, you think it was caused by the radiation, you should reach out to us.”
Takiar reported no disclosures.
PHOENIX – A 70-year-old Vietnam veteran with oropharyngeal cancer presented challenges beyond his disease.
He couldn’t afford transportation for daily radiation treatments and had lost > 10% of his body weight due to pain and eating difficulties, recalled radiation oncologist Vinita Takiar, MD, PhD, in a presentation at the annual meeting of the Association of VA Hematology/Oncology.
To make matters more difficult, his wife held medical power of attorney despite his apparent competence to make decisions, said Takiar, who formerly worked with the US Department of Veterans Affairs (VA) Cincinnati Healthcare System and is now chair of radiation oncology at Penn State University.
All these factors would likely have derailed his treatment if not for a coordinated team intervention, Takiar said. Fortunately, the clinic launched a multifaceted effort involving representatives from the social work, dentistry, ethics, nutrition, and chaplaincy departments.
When surgery became impossible because the patient couldn’t lie on the operating table for adequate tumor exposure, she said, the existing team framework enabled a seamless and rapid transition to radiation with concurrent chemotherapy.
The patient completed treatment with an excellent response, offering a lesson in the importance of multidisciplinary care in head-and-neck cancers, she said.
In fact, when it comes to these forms of cancer, coordinated care “is probably more impactful than any treatment that we’re going to come up with,” she said. “The data show that when we do multidisciplinary care and we do it well, it actually improves the patient experience and outcomes.”
As Takiar noted, teamwork matters in many ways. It leads to better logistics and can address disparities, reduce financial burden and stigma, and even increase clinical trial involvement.
She pointed to studies linking teamwork to better outcomes, support for patients, and overall survival.
Takiar highlighted different parts of teams headed by radiation oncologists who act as “a node to improve multimodal care delivery.”
Speech and swallowing specialists, for example, are helpful in head-and-neck cancer because “there’s an impact on speech, swallowing, and appearance. Our patients don’t want to go out to dinner with friends because they can’t do it.”
Dentists and prosthodontists are key team members too: “I have dentists who have my cell phone number. They just call me: ‘Can I do this extraction? Was this in your radiation field? What was the dose?’”
Other team members include ear, nose, and throat specialists, palliative and supportive care specialists, medical oncologists, nurses, pathologists, transportation workers, and service connection specialists. She noted that previous military experience can affect radiation therapy. For example, the physical restraints required during treatment present particular challenges for veterans who’ve had wartime trauma. These patients may require therapy adjustments.
What’s next on the horizon? Takiar highlighted precision oncology and molecular profiling, artificial intelligence in care decisions and in radiation planning, telemedicine and virtual tumor boards, and expanded survivorship programs.
As for now, she urged colleagues to not be afraid to chat with radiation oncologists. “Please talk to us. We prioritize open communication and shared decision-making with the entire team,” she said. “If you see something and think your radiation oncologist should know about it, you think it was caused by the radiation, you should reach out to us.”
Takiar reported no disclosures.
PHOENIX – A 70-year-old Vietnam veteran with oropharyngeal cancer presented challenges beyond his disease.
He couldn’t afford transportation for daily radiation treatments and had lost > 10% of his body weight due to pain and eating difficulties, recalled radiation oncologist Vinita Takiar, MD, PhD, in a presentation at the annual meeting of the Association of VA Hematology/Oncology.
To make matters more difficult, his wife held medical power of attorney despite his apparent competence to make decisions, said Takiar, who formerly worked with the US Department of Veterans Affairs (VA) Cincinnati Healthcare System and is now chair of radiation oncology at Penn State University.
All these factors would likely have derailed his treatment if not for a coordinated team intervention, Takiar said. Fortunately, the clinic launched a multifaceted effort involving representatives from the social work, dentistry, ethics, nutrition, and chaplaincy departments.
When surgery became impossible because the patient couldn’t lie on the operating table for adequate tumor exposure, she said, the existing team framework enabled a seamless and rapid transition to radiation with concurrent chemotherapy.
The patient completed treatment with an excellent response, offering a lesson in the importance of multidisciplinary care in head-and-neck cancers, she said.
In fact, when it comes to these forms of cancer, coordinated care “is probably more impactful than any treatment that we’re going to come up with,” she said. “The data show that when we do multidisciplinary care and we do it well, it actually improves the patient experience and outcomes.”
As Takiar noted, teamwork matters in many ways. It leads to better logistics and can address disparities, reduce financial burden and stigma, and even increase clinical trial involvement.
She pointed to studies linking teamwork to better outcomes, support for patients, and overall survival.
Takiar highlighted different parts of teams headed by radiation oncologists who act as “a node to improve multimodal care delivery.”
Speech and swallowing specialists, for example, are helpful in head-and-neck cancer because “there’s an impact on speech, swallowing, and appearance. Our patients don’t want to go out to dinner with friends because they can’t do it.”
Dentists and prosthodontists are key team members too: “I have dentists who have my cell phone number. They just call me: ‘Can I do this extraction? Was this in your radiation field? What was the dose?’”
Other team members include ear, nose, and throat specialists, palliative and supportive care specialists, medical oncologists, nurses, pathologists, transportation workers, and service connection specialists. She noted that previous military experience can affect radiation therapy. For example, the physical restraints required during treatment present particular challenges for veterans who’ve had wartime trauma. These patients may require therapy adjustments.
What’s next on the horizon? Takiar highlighted precision oncology and molecular profiling, artificial intelligence in care decisions and in radiation planning, telemedicine and virtual tumor boards, and expanded survivorship programs.
As for now, she urged colleagues to not be afraid to chat with radiation oncologists. “Please talk to us. We prioritize open communication and shared decision-making with the entire team,” she said. “If you see something and think your radiation oncologist should know about it, you think it was caused by the radiation, you should reach out to us.”
Takiar reported no disclosures.
Team-Based Care is Crucial for Head-and-Neck Cancer Cases
Team-Based Care is Crucial for Head-and-Neck Cancer Cases
Trauma, Military Fitness, and Eating Disorders
Military culture may hold 2 salient risk factors for eating disorders: exposure to trauma and body condition standards. A recent study from the US Department of Veteran Affairs (VA) Salisbury Health Care System (VASHCS) found that veterans with posttraumatic stress disorder (PTSD) are more likely to report eating disturbances—particularly issues related to body dissatisfaction and dissatisfaction with eating habits. A 2019 study found that one-third of veterans who were overweight or obese screened positive for engaging in “making weight” behaviors during military service, or unhealthy weight control strategies. Frequently reported weight management behavior was excessive exercise, fasting/skipping meals, sitting in a sauna/wearing a latex suit, laxatives, diuretics, and vomiting.
Service members who are “normal” weight by civilian standards may be labeled “overweight” by the military. In a March 12 memo, Secretary of Defense Pete Hegseth ordered a US Department of Defense review of existing standards for physical fitness, body composition, and grooming. “Our troops will be fit — not fat. Our troops will look sharp — not sloppy. We seek only quality — not quotas. BOTTOM LINE: our @DeptofDefense will make standards HIGH & GREAT again — across the entire force,” he posted on X.
The desire to control weight to fit military standards, however, isn’t the only risk factor. Researchers at VASHCS surveyed 527 post-9/11 veterans (80.7% male) who typically deployed 1 or 2 times. All participants completed the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; the Neuro-Quality of Life in Neurological Disorders Positive Affect and Well-Being Scale (PAWB); and the Eating Disturbances Scale.
Nearly half (46%) of the sample met diagnostic criteria for a lifetime PTSD diagnosis. The study also reported significantly greater eating disturbances in veterans with a lifetime PTSD diagnosis than those without. Women reported significantly greater eating disturbances than men.
Most participants (80%) reported some level of dissatisfaction with their eating disturbances and 74% of participants reported feeling as if they were too fat.
Eating disturbances include refusing food, overexercising, overeating, and misusing laxatives or diuretic pills. Previous research that suggest that 10% to 15% of female veterans and 4% to 8% of male veterans report clinically significant disordered eating behaviors, especially binge eating. One study found that 78% of 45,477 overweight or obese veterans receiving care in VA facilities reported clinically significant binge eating. In a 2021 study, 254 veterans presenting for routine clinical care completed self‐report questionnaires assessing eating disorders, PTSD, depression, and shame, and 31% met probable criteria for bulimia nervosa, binge‐eating disorder, or purging disorder.
According to a 2023 study, eating disturbances that do not meet diagnostic criteria for a formal disorder can be problematic and may function as coping strategies for some facets of military life. The VASHCS researchers found that interventions focused on PAWB, such as acceptance and commitment therapy or compassion-focused therapy, may have potential as a protective factor. Including components that foster hope, optimism, and personal strength may positively mitigate the relationship between PTSD and eating disturbances. PAWB was significantly correlated with eating disturbances; individuals with a lifetime PTSD diagnosis reported significantly lower PAWB than those without.
Interventions grounded in positive psychology have shown promise. A group-based program found “noticeable” (although nonsignificant) improvements in optimistic thinking and treatment engagement. The study also cites that clinicians are beginning to incorporate positive psychology strategies (eg, gratitude journaling, goal setting, and “best possible self” visualization) as adjuncts to traditional treatments. Positive psychology, they write, holds “significant promise as a complementary approach to enhance recovery outcomes in both PTSD and eating disorders.”
Military culture may hold 2 salient risk factors for eating disorders: exposure to trauma and body condition standards. A recent study from the US Department of Veteran Affairs (VA) Salisbury Health Care System (VASHCS) found that veterans with posttraumatic stress disorder (PTSD) are more likely to report eating disturbances—particularly issues related to body dissatisfaction and dissatisfaction with eating habits. A 2019 study found that one-third of veterans who were overweight or obese screened positive for engaging in “making weight” behaviors during military service, or unhealthy weight control strategies. Frequently reported weight management behavior was excessive exercise, fasting/skipping meals, sitting in a sauna/wearing a latex suit, laxatives, diuretics, and vomiting.
Service members who are “normal” weight by civilian standards may be labeled “overweight” by the military. In a March 12 memo, Secretary of Defense Pete Hegseth ordered a US Department of Defense review of existing standards for physical fitness, body composition, and grooming. “Our troops will be fit — not fat. Our troops will look sharp — not sloppy. We seek only quality — not quotas. BOTTOM LINE: our @DeptofDefense will make standards HIGH & GREAT again — across the entire force,” he posted on X.
The desire to control weight to fit military standards, however, isn’t the only risk factor. Researchers at VASHCS surveyed 527 post-9/11 veterans (80.7% male) who typically deployed 1 or 2 times. All participants completed the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; the Neuro-Quality of Life in Neurological Disorders Positive Affect and Well-Being Scale (PAWB); and the Eating Disturbances Scale.
Nearly half (46%) of the sample met diagnostic criteria for a lifetime PTSD diagnosis. The study also reported significantly greater eating disturbances in veterans with a lifetime PTSD diagnosis than those without. Women reported significantly greater eating disturbances than men.
Most participants (80%) reported some level of dissatisfaction with their eating disturbances and 74% of participants reported feeling as if they were too fat.
Eating disturbances include refusing food, overexercising, overeating, and misusing laxatives or diuretic pills. Previous research that suggest that 10% to 15% of female veterans and 4% to 8% of male veterans report clinically significant disordered eating behaviors, especially binge eating. One study found that 78% of 45,477 overweight or obese veterans receiving care in VA facilities reported clinically significant binge eating. In a 2021 study, 254 veterans presenting for routine clinical care completed self‐report questionnaires assessing eating disorders, PTSD, depression, and shame, and 31% met probable criteria for bulimia nervosa, binge‐eating disorder, or purging disorder.
According to a 2023 study, eating disturbances that do not meet diagnostic criteria for a formal disorder can be problematic and may function as coping strategies for some facets of military life. The VASHCS researchers found that interventions focused on PAWB, such as acceptance and commitment therapy or compassion-focused therapy, may have potential as a protective factor. Including components that foster hope, optimism, and personal strength may positively mitigate the relationship between PTSD and eating disturbances. PAWB was significantly correlated with eating disturbances; individuals with a lifetime PTSD diagnosis reported significantly lower PAWB than those without.
Interventions grounded in positive psychology have shown promise. A group-based program found “noticeable” (although nonsignificant) improvements in optimistic thinking and treatment engagement. The study also cites that clinicians are beginning to incorporate positive psychology strategies (eg, gratitude journaling, goal setting, and “best possible self” visualization) as adjuncts to traditional treatments. Positive psychology, they write, holds “significant promise as a complementary approach to enhance recovery outcomes in both PTSD and eating disorders.”
Military culture may hold 2 salient risk factors for eating disorders: exposure to trauma and body condition standards. A recent study from the US Department of Veteran Affairs (VA) Salisbury Health Care System (VASHCS) found that veterans with posttraumatic stress disorder (PTSD) are more likely to report eating disturbances—particularly issues related to body dissatisfaction and dissatisfaction with eating habits. A 2019 study found that one-third of veterans who were overweight or obese screened positive for engaging in “making weight” behaviors during military service, or unhealthy weight control strategies. Frequently reported weight management behavior was excessive exercise, fasting/skipping meals, sitting in a sauna/wearing a latex suit, laxatives, diuretics, and vomiting.
Service members who are “normal” weight by civilian standards may be labeled “overweight” by the military. In a March 12 memo, Secretary of Defense Pete Hegseth ordered a US Department of Defense review of existing standards for physical fitness, body composition, and grooming. “Our troops will be fit — not fat. Our troops will look sharp — not sloppy. We seek only quality — not quotas. BOTTOM LINE: our @DeptofDefense will make standards HIGH & GREAT again — across the entire force,” he posted on X.
The desire to control weight to fit military standards, however, isn’t the only risk factor. Researchers at VASHCS surveyed 527 post-9/11 veterans (80.7% male) who typically deployed 1 or 2 times. All participants completed the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; the Neuro-Quality of Life in Neurological Disorders Positive Affect and Well-Being Scale (PAWB); and the Eating Disturbances Scale.
Nearly half (46%) of the sample met diagnostic criteria for a lifetime PTSD diagnosis. The study also reported significantly greater eating disturbances in veterans with a lifetime PTSD diagnosis than those without. Women reported significantly greater eating disturbances than men.
Most participants (80%) reported some level of dissatisfaction with their eating disturbances and 74% of participants reported feeling as if they were too fat.
Eating disturbances include refusing food, overexercising, overeating, and misusing laxatives or diuretic pills. Previous research that suggest that 10% to 15% of female veterans and 4% to 8% of male veterans report clinically significant disordered eating behaviors, especially binge eating. One study found that 78% of 45,477 overweight or obese veterans receiving care in VA facilities reported clinically significant binge eating. In a 2021 study, 254 veterans presenting for routine clinical care completed self‐report questionnaires assessing eating disorders, PTSD, depression, and shame, and 31% met probable criteria for bulimia nervosa, binge‐eating disorder, or purging disorder.
According to a 2023 study, eating disturbances that do not meet diagnostic criteria for a formal disorder can be problematic and may function as coping strategies for some facets of military life. The VASHCS researchers found that interventions focused on PAWB, such as acceptance and commitment therapy or compassion-focused therapy, may have potential as a protective factor. Including components that foster hope, optimism, and personal strength may positively mitigate the relationship between PTSD and eating disturbances. PAWB was significantly correlated with eating disturbances; individuals with a lifetime PTSD diagnosis reported significantly lower PAWB than those without.
Interventions grounded in positive psychology have shown promise. A group-based program found “noticeable” (although nonsignificant) improvements in optimistic thinking and treatment engagement. The study also cites that clinicians are beginning to incorporate positive psychology strategies (eg, gratitude journaling, goal setting, and “best possible self” visualization) as adjuncts to traditional treatments. Positive psychology, they write, holds “significant promise as a complementary approach to enhance recovery outcomes in both PTSD and eating disorders.”