User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
Socioeconomic status, race found to impact CPAP compliance
SAN DIEGO –
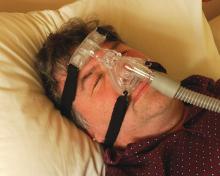
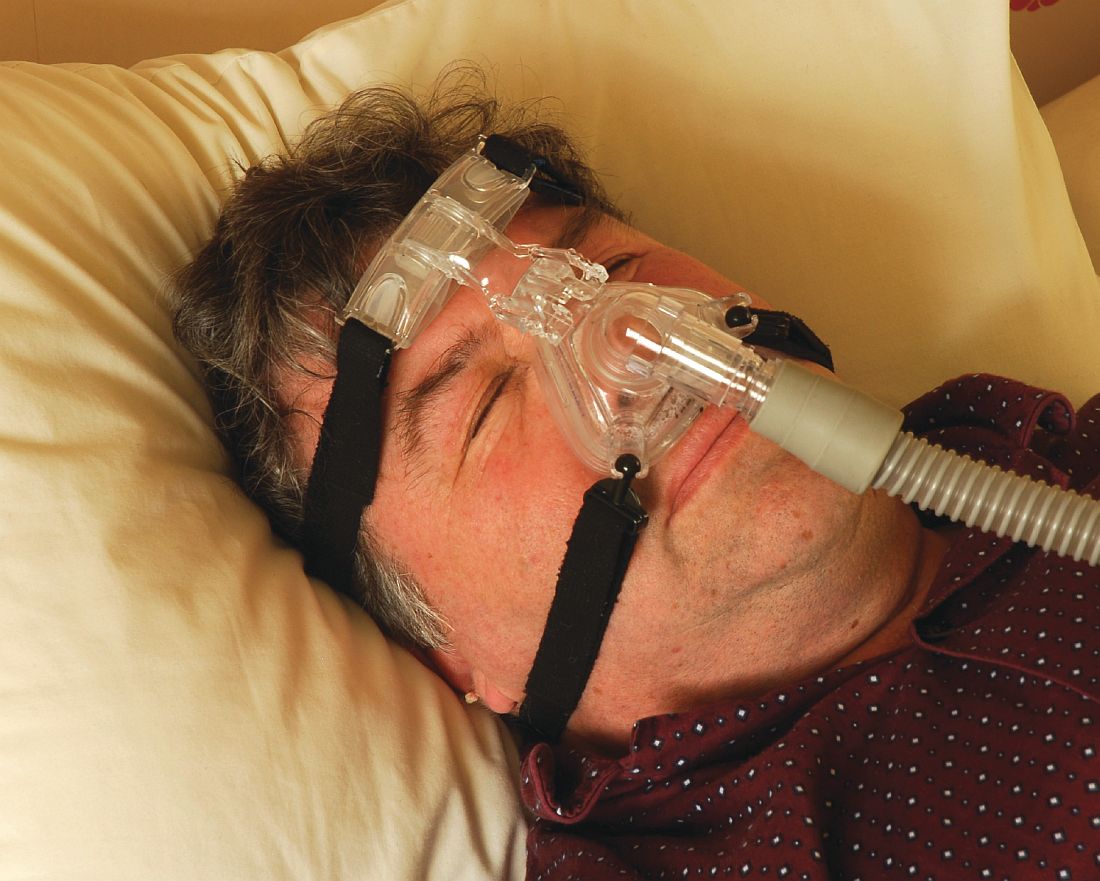
“CPAP is the gold standard treatment for OSA [obstructive sleep apnea] and is very effective, especially for those with severe disease,” researchers led by Philip S. LoSavio, MD, wrote in an abstract presented at the Triological Society’s Combined Sections Meeting. “However, CPAP is a significant challenge for patients for various reasons, with reports of only 46%-80% of OSA patients using CPAP for more than 4 consecutive hours on two out of three nights.”
In an effort to identify and define different factors associated with CPAP compliance, Dr. LoSavio and his colleagues collected data on 578 patients with OSA on CPAP who were treated at Rush University Medical Center, Chicago. The mean patient age was 58 years, 52% were female, 43% were African American, 40% were white, their mean body mass index was 36.91 kg/m2, and their mean apnea-hypopnea index was 37.25 events per hour. The researchers recorded CPAP use at office visits via CPAP module or card, and patients were considered CPAP compliant if their machines logged 4 consecutive hours of use for 70% or more of nights. During the office visits, patients completed a questionnaire asking if they were suffering from different otolaryngology-related diseases, including sinus headaches, gastroesophageal reflex, and enlarged tonsils. Dr. LoSavio, who heads the section of sleep surgery in the department of otorhinolaryngology at Rush University Medical Center, and his colleagues performed logistic regression to ascertain the effects of race and socioeconomic status on CPAP compliance while adjusting for OSA severity. They also analyzed the adjusted association of median income and self-reported symptoms of sinus headaches, GERD, and enlarged tonsils, on CPAP compliance.
They found that African American patients were less compliant with CPAP, compared with their white counterparts (OR 0.42; P less than .01). In addition, patients with mild OSA were less likely to be compliant compared with those who had severe disease (OR 0.57; P less than .03). Self-reported symptoms of sinus headaches, GERD, and enlarged tonsils were associated with significantly lower levels of compliance, while higher median income was positively associated with higher levels of compliance. When the researchers grouped incomes based on the 2018 federal tax classification brackets, they observed a significant association between compliance and median income (P less than .001), with a likelihood ratio of 20.4.
“Previous studies have shown that with increases in OSA disease severity, defined by higher [apnea-hypopnea index], comes increases in CPAP compliance, while other studies have alluded to the fact that lower socioeconomic status can affect CPAP compliance,” Dr. LoSavio and his associates wrote in their abstract. “A novel aspect of our study hoped to shed light on different otolaryngology-related diseases and how they might affect compliance. The patients with comorbid GERD, sinus headaches, and enlarged tonsils were less CPAP compliant in our study. These conditions are relatively easily treated and could therefore provide an avenue to increase CPAP compliance if addressed.” They acknowledged certain limitations of the study, including its single-center design and the self-reported nature of the patient questionnaire.
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: LoSavio P et al. Triological CSM 2019, Abstracts.
SAN DIEGO –
“CPAP is the gold standard treatment for OSA [obstructive sleep apnea] and is very effective, especially for those with severe disease,” researchers led by Philip S. LoSavio, MD, wrote in an abstract presented at the Triological Society’s Combined Sections Meeting. “However, CPAP is a significant challenge for patients for various reasons, with reports of only 46%-80% of OSA patients using CPAP for more than 4 consecutive hours on two out of three nights.”
In an effort to identify and define different factors associated with CPAP compliance, Dr. LoSavio and his colleagues collected data on 578 patients with OSA on CPAP who were treated at Rush University Medical Center, Chicago. The mean patient age was 58 years, 52% were female, 43% were African American, 40% were white, their mean body mass index was 36.91 kg/m2, and their mean apnea-hypopnea index was 37.25 events per hour. The researchers recorded CPAP use at office visits via CPAP module or card, and patients were considered CPAP compliant if their machines logged 4 consecutive hours of use for 70% or more of nights. During the office visits, patients completed a questionnaire asking if they were suffering from different otolaryngology-related diseases, including sinus headaches, gastroesophageal reflex, and enlarged tonsils. Dr. LoSavio, who heads the section of sleep surgery in the department of otorhinolaryngology at Rush University Medical Center, and his colleagues performed logistic regression to ascertain the effects of race and socioeconomic status on CPAP compliance while adjusting for OSA severity. They also analyzed the adjusted association of median income and self-reported symptoms of sinus headaches, GERD, and enlarged tonsils, on CPAP compliance.
They found that African American patients were less compliant with CPAP, compared with their white counterparts (OR 0.42; P less than .01). In addition, patients with mild OSA were less likely to be compliant compared with those who had severe disease (OR 0.57; P less than .03). Self-reported symptoms of sinus headaches, GERD, and enlarged tonsils were associated with significantly lower levels of compliance, while higher median income was positively associated with higher levels of compliance. When the researchers grouped incomes based on the 2018 federal tax classification brackets, they observed a significant association between compliance and median income (P less than .001), with a likelihood ratio of 20.4.
“Previous studies have shown that with increases in OSA disease severity, defined by higher [apnea-hypopnea index], comes increases in CPAP compliance, while other studies have alluded to the fact that lower socioeconomic status can affect CPAP compliance,” Dr. LoSavio and his associates wrote in their abstract. “A novel aspect of our study hoped to shed light on different otolaryngology-related diseases and how they might affect compliance. The patients with comorbid GERD, sinus headaches, and enlarged tonsils were less CPAP compliant in our study. These conditions are relatively easily treated and could therefore provide an avenue to increase CPAP compliance if addressed.” They acknowledged certain limitations of the study, including its single-center design and the self-reported nature of the patient questionnaire.
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: LoSavio P et al. Triological CSM 2019, Abstracts.
SAN DIEGO –
“CPAP is the gold standard treatment for OSA [obstructive sleep apnea] and is very effective, especially for those with severe disease,” researchers led by Philip S. LoSavio, MD, wrote in an abstract presented at the Triological Society’s Combined Sections Meeting. “However, CPAP is a significant challenge for patients for various reasons, with reports of only 46%-80% of OSA patients using CPAP for more than 4 consecutive hours on two out of three nights.”
In an effort to identify and define different factors associated with CPAP compliance, Dr. LoSavio and his colleagues collected data on 578 patients with OSA on CPAP who were treated at Rush University Medical Center, Chicago. The mean patient age was 58 years, 52% were female, 43% were African American, 40% were white, their mean body mass index was 36.91 kg/m2, and their mean apnea-hypopnea index was 37.25 events per hour. The researchers recorded CPAP use at office visits via CPAP module or card, and patients were considered CPAP compliant if their machines logged 4 consecutive hours of use for 70% or more of nights. During the office visits, patients completed a questionnaire asking if they were suffering from different otolaryngology-related diseases, including sinus headaches, gastroesophageal reflex, and enlarged tonsils. Dr. LoSavio, who heads the section of sleep surgery in the department of otorhinolaryngology at Rush University Medical Center, and his colleagues performed logistic regression to ascertain the effects of race and socioeconomic status on CPAP compliance while adjusting for OSA severity. They also analyzed the adjusted association of median income and self-reported symptoms of sinus headaches, GERD, and enlarged tonsils, on CPAP compliance.
They found that African American patients were less compliant with CPAP, compared with their white counterparts (OR 0.42; P less than .01). In addition, patients with mild OSA were less likely to be compliant compared with those who had severe disease (OR 0.57; P less than .03). Self-reported symptoms of sinus headaches, GERD, and enlarged tonsils were associated with significantly lower levels of compliance, while higher median income was positively associated with higher levels of compliance. When the researchers grouped incomes based on the 2018 federal tax classification brackets, they observed a significant association between compliance and median income (P less than .001), with a likelihood ratio of 20.4.
“Previous studies have shown that with increases in OSA disease severity, defined by higher [apnea-hypopnea index], comes increases in CPAP compliance, while other studies have alluded to the fact that lower socioeconomic status can affect CPAP compliance,” Dr. LoSavio and his associates wrote in their abstract. “A novel aspect of our study hoped to shed light on different otolaryngology-related diseases and how they might affect compliance. The patients with comorbid GERD, sinus headaches, and enlarged tonsils were less CPAP compliant in our study. These conditions are relatively easily treated and could therefore provide an avenue to increase CPAP compliance if addressed.” They acknowledged certain limitations of the study, including its single-center design and the self-reported nature of the patient questionnaire.
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: LoSavio P et al. Triological CSM 2019, Abstracts.
REPORTING FROM THE TRIOLOGICAL CSM
Key clinical point: Compliance with continuous positive airway pressure is affected by patient socioeconomic status and race.
Major finding: African American patients were less compliant with CPAP, compared with their white counterparts (OR 0.42; P less than .01).
Study details: A retrospective study of 578 obstructive sleep apnea patients on CPAP.
Disclosures: The researchers reported having no financial disclosures.
Source: LoSavio P et al. Triological CSM 2019, Abstracts.
Trump administration salutes parade of generic drug approvals, but hundreds aren’t for sale
The Trump administration has been trumpeting a huge increase in Food and Drug Administration generic drug approvals during the past 2 years, the result of its actions to streamline a cumbersome process and combat anticompetitive practices. But nearly half of those newly approved drugs aren’t being sold in the United States, Kaiser Health News has found, meaning that many patients are deriving little practical benefit from the administration’s efforts.
The administration’s aggressive push to approve more generics is designed to spur more competition with expensive brand-name drugs, and drive prices lower, President Trump noted at a White House event in January 2019. The FDA has approved more than 1,600 generic drug applications since January 2017 – about a third more than it did during the last 2 years of the Obama administration.
But more than 700 generics, or about 43%, still weren’t on the market as of early January, a KHN data analysis of FDA and drug list price records shows. Even more noteworthy: 36% of generics that would be the first to compete against a branded drug are not yet for sale. That means thousands or even millions of patients have no option beyond buying branded drugs that can cost thousands of dollars per month.
“That’s shockingly high,” said former congressman Henry Waxman, who cosponsored the 1984 law that paved the way for the generic approval process as we know it today. He said he’d like to know more but suspects anticompetitive behavior is at least partly to blame and that revisions to the so-called Hatch-Waxman Act might be needed.
The approved generics that haven’t made it to American medicine cabinets include generic versions of expensive medicines like the blood thinner ticagrelor (Brilinta) and HIV medication emtricitabine/tenofovir disoproxil fumarate (Truvada). They also include six different generic versions of sodium nitroprusside (Nitropress), a heart failure drug, whose price spiked 310% in 2015.
Experts say a variety of factors are to blame. Generics sellers have fought for years against patent litigation and other delay tactics that protect brand-name drugs from competition. In recent years, vast industry consolidation has reduced the ranks of companies willing to purchase and distribute generics. And, in some cases, makers of generics obtain approvals and ultimately make a business decision to sit on them.
“It’s a real problem because we’re not getting all the expected competition,” FDA Commissioner Scott Gottlieb, MD, said in an interview, adding that it will be difficult to solve because it has so many causes. It takes five generics on the market to drive prices down to 33% of the original brand-name price, according to an FDA analysis.
Without generics to lower drug costs, branded manufacturers can continue to increase their prices, at a rate of roughly 10% a year, said Scott Knoer, PharmD, chief pharmacy officer at the Cleveland Clinic. “It makes health care costs go up across the board.”
Even if hospital patients don’t directly see high drug prices in their bills, the higher costs get passed to insurers, who pass them on as higher premiums, Dr. Knoer said. They also get passed to taxpayers, who pay for drugs covered by Medicare and Medicaid.
Consolidation on multiple tiers of the drug supply chain have changed the face of the generic drug market, warping supply and demand.
In some cases, key pharmaceutical ingredients are unavailable or a manufacturer doesn’t have the capacity to launch a product because it’s having difficulty meeting demand for existing products.
Manufacturing consolidation has dramatically reduced the production of injectable drugs, which are typically administered in a doctor’s office. This may be why 157 injectable generics that were approved in the past 2 years haven’t been brought to market.
Erin Fox, PharmD, a pharmacist at the University of Utah, Salt Lake City, who tracks drug shortages, said the KHN analysis of stalled generics “highlights that companies often have a lot of products ‘on the books’ but aren’t really making them.” A few generics on the list – like a 10% dextrose injection, to treat patients with low blood sugar – would have been helpful to combat shortages the past few years. “This comes up with shortages a lot – it looks like there are more suppliers than there really are,” Dr. Fox said.
A lot can change between the time a drugmaker files a generic application with the FDA and the time it’s approved.
Some drugmakers that applied for generic approval years ago switched their attention to more profitable products. Novartis, for instance, recently sold a generics division run by Sandoz so Sandoz could focus on other drugs, including biosimilars, which compete with expensive biologic drugs made from living organisms.
“Some of these [generic] drug applications have been sitting 6, 7, 8 years,” said Robert W. Pollock, a former acting deputy director of the FDA’s Office of Generic Drugs who now works for Lachman Consultants. By the time it’s approved, a generic can fall out of favor because patients taking the branded version reported new side effects or because a more-effective branded drug was approved.
For some generic manufacturers, there’s money to be made by waiting. Brand-name drugmakers will pay them to keep their products off the market as part of a tactic sometimes called “pay for delay.” The Federal Trade Commission estimates that such deals cost consumers and taxpayers $3.5 billion a year.
The number of these potentially anticompetitive settlements decreased from fiscal 2014 to fiscal 2015, according to the latest FTC report. Still, Dr. Gottlieb said he hopes to crack down on such tactics. The first generic to take on a branded drug is granted 180 days of exclusivity before the second and third generics can be approved, giving those products a clear advantage.
“We don’t like that companies are able to just park [a generic for] 180 days while they cut a deal not to come to market,” Dr. Gottlieb said, adding that with help from Congress he hopes to force companies to forfeit exclusivity if they don’t launch on time.
In some cases, according to Dr. Gottlieb, generic drugmakers wait until they’ve stockpiled a number of newly approved generics and have landed a contract with a purchaser before bringing their medicines to market.
These bundled contracts are secretive, so not much is known about them, but it means companies are filing generic applications just for the option of introducing generics, said health care economist Rena Conti of the Questrom School of Business at Boston University. They’ll wait until the most strategic time to launch, which could be after the competition shakes out, leaving them as “the last man standing,” Ms. Conti said. Then they can launch and hike the price.
To be sure, the FDA under Dr. Gottlieb’s leadership has taken steps to increase generic competition, from shaming brand-name drugmakers for blocking generics to publishing documents to help manufacturers win approval more easily. But approval doesn’t necessarily spur competition.
“We used to say it was all about getting in – once you got approval from the FDA, then you could go to market,” said Chip Davis, CEO of the Association for Accessible Medicines, the trade group for makers of generic drugs. The biggest challenges his members face is that there aren’t enough companies purchasing drugs, Mr. Davis said. Consolidation has led to three large buying groups covering 90% of the market, according to a Drug Channels Institute report. So, if you’re the fourth or fifth generic, you may have no one left to sell to.
Yet another barrier relates to how drug middlemen select the drugs they’ll cover under industry formularies, which determine what products insurance plans will cover. In some cases, middlemen known as “pharmacy benefit managers” have made it clear they don’t have room on their formularies for another generic. Or they do, but they give branded drugs preferential treatment with lower copays, hurting the generic’s market share.
Barriers to entry are lower under Gottlieb’s FDA than they’ve been in years past, Conti said, and regulations can help foster competition. But, she said, “they can only do so much.”
Methodology
To identify approved drugs that have not reached the market, Kaiser Health News used the FDA’s Orange Book database – as of Jan. 2 – to identify drug applications approved in 2017 or 2018. We then searched the FDA’s online National Drug Code directory for billing codes for the drugs associated with each application as of the same date. To account for a possible lag, we supplemented this list with a more complete billing code directory that we obtained via a Freedom of Information Act request. It includes codes with expected future launch dates that don’t appear in the online version.
According to experts, a billing code doesn’t necessarily mean a drug is on the market. However, every drug on the market needs a list price for reimbursement. We provided a list of application numbers and billing codes to information technology firm Connecture, which then told us whether each one was active, inactive, or had no list price as of Jan. 17.
If an application had at least one billing code with a list price attached, we counted it as on the market, even if other billing codes did not have list prices.
Sometimes, a single generic application can have multiple approval dates. If one of these approval dates occurred in the past 2 years, we included it in our analysis.
To determine whether a drug was a first generic, KHN used the FDA’s 2017 and 2018 lists of first generics as of Jan 2.
Kaiser Health News is a nonprofit national health policy news service. It is an editorially independent program of the Henry J. Kaiser Family Foundation that is not affiliated with Kaiser Permanente.
The Trump administration has been trumpeting a huge increase in Food and Drug Administration generic drug approvals during the past 2 years, the result of its actions to streamline a cumbersome process and combat anticompetitive practices. But nearly half of those newly approved drugs aren’t being sold in the United States, Kaiser Health News has found, meaning that many patients are deriving little practical benefit from the administration’s efforts.
The administration’s aggressive push to approve more generics is designed to spur more competition with expensive brand-name drugs, and drive prices lower, President Trump noted at a White House event in January 2019. The FDA has approved more than 1,600 generic drug applications since January 2017 – about a third more than it did during the last 2 years of the Obama administration.
But more than 700 generics, or about 43%, still weren’t on the market as of early January, a KHN data analysis of FDA and drug list price records shows. Even more noteworthy: 36% of generics that would be the first to compete against a branded drug are not yet for sale. That means thousands or even millions of patients have no option beyond buying branded drugs that can cost thousands of dollars per month.
“That’s shockingly high,” said former congressman Henry Waxman, who cosponsored the 1984 law that paved the way for the generic approval process as we know it today. He said he’d like to know more but suspects anticompetitive behavior is at least partly to blame and that revisions to the so-called Hatch-Waxman Act might be needed.
The approved generics that haven’t made it to American medicine cabinets include generic versions of expensive medicines like the blood thinner ticagrelor (Brilinta) and HIV medication emtricitabine/tenofovir disoproxil fumarate (Truvada). They also include six different generic versions of sodium nitroprusside (Nitropress), a heart failure drug, whose price spiked 310% in 2015.
Experts say a variety of factors are to blame. Generics sellers have fought for years against patent litigation and other delay tactics that protect brand-name drugs from competition. In recent years, vast industry consolidation has reduced the ranks of companies willing to purchase and distribute generics. And, in some cases, makers of generics obtain approvals and ultimately make a business decision to sit on them.
“It’s a real problem because we’re not getting all the expected competition,” FDA Commissioner Scott Gottlieb, MD, said in an interview, adding that it will be difficult to solve because it has so many causes. It takes five generics on the market to drive prices down to 33% of the original brand-name price, according to an FDA analysis.
Without generics to lower drug costs, branded manufacturers can continue to increase their prices, at a rate of roughly 10% a year, said Scott Knoer, PharmD, chief pharmacy officer at the Cleveland Clinic. “It makes health care costs go up across the board.”
Even if hospital patients don’t directly see high drug prices in their bills, the higher costs get passed to insurers, who pass them on as higher premiums, Dr. Knoer said. They also get passed to taxpayers, who pay for drugs covered by Medicare and Medicaid.
Consolidation on multiple tiers of the drug supply chain have changed the face of the generic drug market, warping supply and demand.
In some cases, key pharmaceutical ingredients are unavailable or a manufacturer doesn’t have the capacity to launch a product because it’s having difficulty meeting demand for existing products.
Manufacturing consolidation has dramatically reduced the production of injectable drugs, which are typically administered in a doctor’s office. This may be why 157 injectable generics that were approved in the past 2 years haven’t been brought to market.
Erin Fox, PharmD, a pharmacist at the University of Utah, Salt Lake City, who tracks drug shortages, said the KHN analysis of stalled generics “highlights that companies often have a lot of products ‘on the books’ but aren’t really making them.” A few generics on the list – like a 10% dextrose injection, to treat patients with low blood sugar – would have been helpful to combat shortages the past few years. “This comes up with shortages a lot – it looks like there are more suppliers than there really are,” Dr. Fox said.
A lot can change between the time a drugmaker files a generic application with the FDA and the time it’s approved.
Some drugmakers that applied for generic approval years ago switched their attention to more profitable products. Novartis, for instance, recently sold a generics division run by Sandoz so Sandoz could focus on other drugs, including biosimilars, which compete with expensive biologic drugs made from living organisms.
“Some of these [generic] drug applications have been sitting 6, 7, 8 years,” said Robert W. Pollock, a former acting deputy director of the FDA’s Office of Generic Drugs who now works for Lachman Consultants. By the time it’s approved, a generic can fall out of favor because patients taking the branded version reported new side effects or because a more-effective branded drug was approved.
For some generic manufacturers, there’s money to be made by waiting. Brand-name drugmakers will pay them to keep their products off the market as part of a tactic sometimes called “pay for delay.” The Federal Trade Commission estimates that such deals cost consumers and taxpayers $3.5 billion a year.
The number of these potentially anticompetitive settlements decreased from fiscal 2014 to fiscal 2015, according to the latest FTC report. Still, Dr. Gottlieb said he hopes to crack down on such tactics. The first generic to take on a branded drug is granted 180 days of exclusivity before the second and third generics can be approved, giving those products a clear advantage.
“We don’t like that companies are able to just park [a generic for] 180 days while they cut a deal not to come to market,” Dr. Gottlieb said, adding that with help from Congress he hopes to force companies to forfeit exclusivity if they don’t launch on time.
In some cases, according to Dr. Gottlieb, generic drugmakers wait until they’ve stockpiled a number of newly approved generics and have landed a contract with a purchaser before bringing their medicines to market.
These bundled contracts are secretive, so not much is known about them, but it means companies are filing generic applications just for the option of introducing generics, said health care economist Rena Conti of the Questrom School of Business at Boston University. They’ll wait until the most strategic time to launch, which could be after the competition shakes out, leaving them as “the last man standing,” Ms. Conti said. Then they can launch and hike the price.
To be sure, the FDA under Dr. Gottlieb’s leadership has taken steps to increase generic competition, from shaming brand-name drugmakers for blocking generics to publishing documents to help manufacturers win approval more easily. But approval doesn’t necessarily spur competition.
“We used to say it was all about getting in – once you got approval from the FDA, then you could go to market,” said Chip Davis, CEO of the Association for Accessible Medicines, the trade group for makers of generic drugs. The biggest challenges his members face is that there aren’t enough companies purchasing drugs, Mr. Davis said. Consolidation has led to three large buying groups covering 90% of the market, according to a Drug Channels Institute report. So, if you’re the fourth or fifth generic, you may have no one left to sell to.
Yet another barrier relates to how drug middlemen select the drugs they’ll cover under industry formularies, which determine what products insurance plans will cover. In some cases, middlemen known as “pharmacy benefit managers” have made it clear they don’t have room on their formularies for another generic. Or they do, but they give branded drugs preferential treatment with lower copays, hurting the generic’s market share.
Barriers to entry are lower under Gottlieb’s FDA than they’ve been in years past, Conti said, and regulations can help foster competition. But, she said, “they can only do so much.”
Methodology
To identify approved drugs that have not reached the market, Kaiser Health News used the FDA’s Orange Book database – as of Jan. 2 – to identify drug applications approved in 2017 or 2018. We then searched the FDA’s online National Drug Code directory for billing codes for the drugs associated with each application as of the same date. To account for a possible lag, we supplemented this list with a more complete billing code directory that we obtained via a Freedom of Information Act request. It includes codes with expected future launch dates that don’t appear in the online version.
According to experts, a billing code doesn’t necessarily mean a drug is on the market. However, every drug on the market needs a list price for reimbursement. We provided a list of application numbers and billing codes to information technology firm Connecture, which then told us whether each one was active, inactive, or had no list price as of Jan. 17.
If an application had at least one billing code with a list price attached, we counted it as on the market, even if other billing codes did not have list prices.
Sometimes, a single generic application can have multiple approval dates. If one of these approval dates occurred in the past 2 years, we included it in our analysis.
To determine whether a drug was a first generic, KHN used the FDA’s 2017 and 2018 lists of first generics as of Jan 2.
Kaiser Health News is a nonprofit national health policy news service. It is an editorially independent program of the Henry J. Kaiser Family Foundation that is not affiliated with Kaiser Permanente.
The Trump administration has been trumpeting a huge increase in Food and Drug Administration generic drug approvals during the past 2 years, the result of its actions to streamline a cumbersome process and combat anticompetitive practices. But nearly half of those newly approved drugs aren’t being sold in the United States, Kaiser Health News has found, meaning that many patients are deriving little practical benefit from the administration’s efforts.
The administration’s aggressive push to approve more generics is designed to spur more competition with expensive brand-name drugs, and drive prices lower, President Trump noted at a White House event in January 2019. The FDA has approved more than 1,600 generic drug applications since January 2017 – about a third more than it did during the last 2 years of the Obama administration.
But more than 700 generics, or about 43%, still weren’t on the market as of early January, a KHN data analysis of FDA and drug list price records shows. Even more noteworthy: 36% of generics that would be the first to compete against a branded drug are not yet for sale. That means thousands or even millions of patients have no option beyond buying branded drugs that can cost thousands of dollars per month.
“That’s shockingly high,” said former congressman Henry Waxman, who cosponsored the 1984 law that paved the way for the generic approval process as we know it today. He said he’d like to know more but suspects anticompetitive behavior is at least partly to blame and that revisions to the so-called Hatch-Waxman Act might be needed.
The approved generics that haven’t made it to American medicine cabinets include generic versions of expensive medicines like the blood thinner ticagrelor (Brilinta) and HIV medication emtricitabine/tenofovir disoproxil fumarate (Truvada). They also include six different generic versions of sodium nitroprusside (Nitropress), a heart failure drug, whose price spiked 310% in 2015.
Experts say a variety of factors are to blame. Generics sellers have fought for years against patent litigation and other delay tactics that protect brand-name drugs from competition. In recent years, vast industry consolidation has reduced the ranks of companies willing to purchase and distribute generics. And, in some cases, makers of generics obtain approvals and ultimately make a business decision to sit on them.
“It’s a real problem because we’re not getting all the expected competition,” FDA Commissioner Scott Gottlieb, MD, said in an interview, adding that it will be difficult to solve because it has so many causes. It takes five generics on the market to drive prices down to 33% of the original brand-name price, according to an FDA analysis.
Without generics to lower drug costs, branded manufacturers can continue to increase their prices, at a rate of roughly 10% a year, said Scott Knoer, PharmD, chief pharmacy officer at the Cleveland Clinic. “It makes health care costs go up across the board.”
Even if hospital patients don’t directly see high drug prices in their bills, the higher costs get passed to insurers, who pass them on as higher premiums, Dr. Knoer said. They also get passed to taxpayers, who pay for drugs covered by Medicare and Medicaid.
Consolidation on multiple tiers of the drug supply chain have changed the face of the generic drug market, warping supply and demand.
In some cases, key pharmaceutical ingredients are unavailable or a manufacturer doesn’t have the capacity to launch a product because it’s having difficulty meeting demand for existing products.
Manufacturing consolidation has dramatically reduced the production of injectable drugs, which are typically administered in a doctor’s office. This may be why 157 injectable generics that were approved in the past 2 years haven’t been brought to market.
Erin Fox, PharmD, a pharmacist at the University of Utah, Salt Lake City, who tracks drug shortages, said the KHN analysis of stalled generics “highlights that companies often have a lot of products ‘on the books’ but aren’t really making them.” A few generics on the list – like a 10% dextrose injection, to treat patients with low blood sugar – would have been helpful to combat shortages the past few years. “This comes up with shortages a lot – it looks like there are more suppliers than there really are,” Dr. Fox said.
A lot can change between the time a drugmaker files a generic application with the FDA and the time it’s approved.
Some drugmakers that applied for generic approval years ago switched their attention to more profitable products. Novartis, for instance, recently sold a generics division run by Sandoz so Sandoz could focus on other drugs, including biosimilars, which compete with expensive biologic drugs made from living organisms.
“Some of these [generic] drug applications have been sitting 6, 7, 8 years,” said Robert W. Pollock, a former acting deputy director of the FDA’s Office of Generic Drugs who now works for Lachman Consultants. By the time it’s approved, a generic can fall out of favor because patients taking the branded version reported new side effects or because a more-effective branded drug was approved.
For some generic manufacturers, there’s money to be made by waiting. Brand-name drugmakers will pay them to keep their products off the market as part of a tactic sometimes called “pay for delay.” The Federal Trade Commission estimates that such deals cost consumers and taxpayers $3.5 billion a year.
The number of these potentially anticompetitive settlements decreased from fiscal 2014 to fiscal 2015, according to the latest FTC report. Still, Dr. Gottlieb said he hopes to crack down on such tactics. The first generic to take on a branded drug is granted 180 days of exclusivity before the second and third generics can be approved, giving those products a clear advantage.
“We don’t like that companies are able to just park [a generic for] 180 days while they cut a deal not to come to market,” Dr. Gottlieb said, adding that with help from Congress he hopes to force companies to forfeit exclusivity if they don’t launch on time.
In some cases, according to Dr. Gottlieb, generic drugmakers wait until they’ve stockpiled a number of newly approved generics and have landed a contract with a purchaser before bringing their medicines to market.
These bundled contracts are secretive, so not much is known about them, but it means companies are filing generic applications just for the option of introducing generics, said health care economist Rena Conti of the Questrom School of Business at Boston University. They’ll wait until the most strategic time to launch, which could be after the competition shakes out, leaving them as “the last man standing,” Ms. Conti said. Then they can launch and hike the price.
To be sure, the FDA under Dr. Gottlieb’s leadership has taken steps to increase generic competition, from shaming brand-name drugmakers for blocking generics to publishing documents to help manufacturers win approval more easily. But approval doesn’t necessarily spur competition.
“We used to say it was all about getting in – once you got approval from the FDA, then you could go to market,” said Chip Davis, CEO of the Association for Accessible Medicines, the trade group for makers of generic drugs. The biggest challenges his members face is that there aren’t enough companies purchasing drugs, Mr. Davis said. Consolidation has led to three large buying groups covering 90% of the market, according to a Drug Channels Institute report. So, if you’re the fourth or fifth generic, you may have no one left to sell to.
Yet another barrier relates to how drug middlemen select the drugs they’ll cover under industry formularies, which determine what products insurance plans will cover. In some cases, middlemen known as “pharmacy benefit managers” have made it clear they don’t have room on their formularies for another generic. Or they do, but they give branded drugs preferential treatment with lower copays, hurting the generic’s market share.
Barriers to entry are lower under Gottlieb’s FDA than they’ve been in years past, Conti said, and regulations can help foster competition. But, she said, “they can only do so much.”
Methodology
To identify approved drugs that have not reached the market, Kaiser Health News used the FDA’s Orange Book database – as of Jan. 2 – to identify drug applications approved in 2017 or 2018. We then searched the FDA’s online National Drug Code directory for billing codes for the drugs associated with each application as of the same date. To account for a possible lag, we supplemented this list with a more complete billing code directory that we obtained via a Freedom of Information Act request. It includes codes with expected future launch dates that don’t appear in the online version.
According to experts, a billing code doesn’t necessarily mean a drug is on the market. However, every drug on the market needs a list price for reimbursement. We provided a list of application numbers and billing codes to information technology firm Connecture, which then told us whether each one was active, inactive, or had no list price as of Jan. 17.
If an application had at least one billing code with a list price attached, we counted it as on the market, even if other billing codes did not have list prices.
Sometimes, a single generic application can have multiple approval dates. If one of these approval dates occurred in the past 2 years, we included it in our analysis.
To determine whether a drug was a first generic, KHN used the FDA’s 2017 and 2018 lists of first generics as of Jan 2.
Kaiser Health News is a nonprofit national health policy news service. It is an editorially independent program of the Henry J. Kaiser Family Foundation that is not affiliated with Kaiser Permanente.
500 Women in Medicine: Part I
Ms. Gerull and Ms. Loe are third-year medical students at Washington University School of Medicine in St. Louis.
Their aim is to create a network of support and advancement for women in medicine. 500 Women in Medicine is a pod of the organization 500 Women Scientists.
In this episode, Nick Andrews speaks with the two innovators about their motivation to found this organization.
Correction, 3/12/19: An earlier version of this article misstated Kate Gerull's name.
Ms. Gerull and Ms. Loe are third-year medical students at Washington University School of Medicine in St. Louis.
Their aim is to create a network of support and advancement for women in medicine. 500 Women in Medicine is a pod of the organization 500 Women Scientists.
In this episode, Nick Andrews speaks with the two innovators about their motivation to found this organization.
Correction, 3/12/19: An earlier version of this article misstated Kate Gerull's name.
Ms. Gerull and Ms. Loe are third-year medical students at Washington University School of Medicine in St. Louis.
Their aim is to create a network of support and advancement for women in medicine. 500 Women in Medicine is a pod of the organization 500 Women Scientists.
In this episode, Nick Andrews speaks with the two innovators about their motivation to found this organization.
Correction, 3/12/19: An earlier version of this article misstated Kate Gerull's name.
Novel plasma biomarkers for Alzheimer’s
Also today, biomarkers predict VTE risk with menopausal oral hormone therapy, there is a cloud of inconsistency hanging over cannabis data, and compounded pain creams are no better than placebo for chronic localized pain.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, biomarkers predict VTE risk with menopausal oral hormone therapy, there is a cloud of inconsistency hanging over cannabis data, and compounded pain creams are no better than placebo for chronic localized pain.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, biomarkers predict VTE risk with menopausal oral hormone therapy, there is a cloud of inconsistency hanging over cannabis data, and compounded pain creams are no better than placebo for chronic localized pain.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Hearing drills into patient impact of ACA legal challenge
If Republican state attorneys general prevail in their legal bid to overturn the Affordable Care Act, patients with preexisting conditions will lose their coverage protections, and an additional 24 million Americans could become uninsured, according to testimony presented at a Feb. 6 hearing of the House Energy and Commerce Health Subcommittee.
A ruling for the plaintiffs in Texas v. United States also would mean the ACA’s consumer protections for employer-based coverage would be eliminated, affecting more than 150 million Americans, said Christen Linke Young, an attorney and fellow for the liberal-leaning USC-Brookings Schaeffer Initiative on Health Policy.
“The ACA’s changes to Medicare would be undone, reinstating copays on preventive services and reopening the prescription drug ‘donut hole,’ ” Ms. Young testified at the hearing. “It would also create major confusion in Medicare payment, as the ACA policies that are today fully integrated into the Medicare payment rules would suddenly lack a legislative basis.”
Ms. Linke Young was one of five witnesses who testified before lawmakers about the implications of Texas v. United States, an ongoing legal case that centers on whether a part of the health care law should be severed and if so, whether the entire law should then fall.
A group of Republican state attorneys general sued over the law in 2018, arguing that, because budget legislation in 2017 zeroed out the penalties associated with the ACA’s individual mandate, the mandate is invalid. The attorneys general also argue that, if the mandate is severed, the entire ACA should be struck down.
In response to the suit, the Trump administration agreed that the mandate is unconstitutional and should be parsed. Attorneys for the administration wrote that, if the mandate is found unconstitutional, the court should also consider finding two other provisions – the guaranteed issue and community rating requirements – of the ACA invalid. Guaranteed issue refers to insurers in the individual market offering coverage to all citizens, regardless of preexisting conditions, while community rating refers to charging equal premiums to every patient, no matter their past health status. The remainder of the ACA can stand without the three linked provisions, according to the Trump administration, which refused to defend the case.
A coalition of 17 Democratic attorneys general have stepped in to defend the case.
In December, a district court declared the entire ACA to be invalid, a decision immediately appealed to the 5th Circuit by the Democratic attorneys general. In January, the circuit court froze the case in light of the federal government’s partial shutdown. The case remains on hold.
At the hearing, Thomas P. Miller, a resident fellow at the conservative-leaning American Enterprise Institute, testified that a 5th Circuit decision would not likely come before summer 2019, followed by a potential U.S. Supreme Court reading in 2020 – if the case gets that far.
“The probability of a Supreme Court ruling that would overturn the entire ACA remains very low, despite last December’s decision at the federal district court level reaching exactly that legal conclusion,” Mr. Miller testified. “Given the murkiness of divining legislative intent in harder cases like the ACA, challenges to the individual mandate, past and present, it’s better to conclude that, although several different severability settings are hypothetically conceivable, it remains all but certain that an ultimate Supreme Court ruling in this case will, at a minimum, follow its previous inclinations revealed in the 2012 and 2015 ACA challenges and try to save as much of the law as possible.”
If the individual mandate is ultimately severed from the ACA, the decision would have little impact on beneficiaries or function of the health care law, according to Simon Lazarus, a lawyer and writer on constitutional and legal issues.
“Such a result will have virtually no impact on the operation of the ACA, nor on the millions of Americans – in reality, substantially all Americans – who depend on the ACA and its guarantees for people with preexisting conditions and myriad other protections that now are ‘baked into’ the national health care system,” Mr. Lazarus testified at the hearing. “To declare invalid the law’s shared responsibility payment provision, when that provision has no financial penalty behind it, will, by itself, have little if any depressive effect on the number of enrollees in health insurance plans.”
However, Mr. Lazarus noted that the guaranteed issue and community rating provisions of the law are “critical protections” for people with preexisting conditions.
Avik Roy, president for the Foundation for Research on Equal Opportunity, a nonpartisan organization that supports universal health care, testified that the Trump administration’s position about the mandate being tied to the guaranteed issue and community rating provisions is being mischaracterized as implying the administration opposes protecting people with preexisting conditions. President Trump has repeatedly expressed that any reforms or replacements of the ACA cover those with preexisting conditions, he said.
Mr. Roy recommended that Congress pass a bill reiterating the guaranteed issue and community rating requirements in the individual market to ensure protection for patients with preexisting conditions in light of Texas v. United States.
“I understand that a motion to produce such legislation was proposed by House Republicans during floor debate at the beginning of this Congress, [a bill] that would guarantee that no American could be denied coverage, or be charged higher premiums or cost sharing, as a result of a previous or current illness – and that the motion was defeated by the majority,” Mr. Roy testified. To me, this is a shame, as such legislation would ensure that Americans with preexisting conditions would be protected whatever the courts decide. I hope that Congress will reconsider its position.”
A number of subcommittee members pledged their support for protecting people with preexisting conditions and encouraged discussion of further legislation proposals.
“Let me speak on behalf of Republicans; we fully support protecting Americans with preexisting conditions,” said Rep. Greg Walden (R-Ore.), ranking member of the full committee. “We’ve said this repeatedly, we’ve acted accordingly, and we mean it completely. We could and should inject certainly into the system by passing legislation to protect those with preexisting conditions.”
Rep. Michael Burgess, MD, (R-Texas) questioned why the subcommittee was having a hearing on Texas v. United States, rather than focusing on making specific health policy improvements.
“It’s unfortunate we’re having a hearing that doesn’t move toward the development of any policies that will actually improve health care for Americans,” Rep. Burgess said during the hearing. “To that effect, there are numerous options that you could bring before us that could moot [Texas v. United States], but the subcommittee apparently has chosen not to do so.”
Committee Chairman Frank Pallone Jr. (D-N.J.), who called for the hearing, took offense at Rep. Burgess’ statements, expressing the importance of the hearing and the case at large.
“I saw no effort at all in the time that you were the chairman [of the health subcommittee] to try to work toward solutions in improving the ACA,” Rep. Pallone said. “What I saw were constant efforts to join with President Trump to sabotage it. ... and the reason that this hearing is so important is because the ultimate sabotage would be to have the courts rule that the ACA was unconstitutional, which is totally bogus.”
The Subcommittee on Health will hold another hearing on Feb. 13 to discuss ACA legislation and protections for patients with preexisting conditions.
If Republican state attorneys general prevail in their legal bid to overturn the Affordable Care Act, patients with preexisting conditions will lose their coverage protections, and an additional 24 million Americans could become uninsured, according to testimony presented at a Feb. 6 hearing of the House Energy and Commerce Health Subcommittee.
A ruling for the plaintiffs in Texas v. United States also would mean the ACA’s consumer protections for employer-based coverage would be eliminated, affecting more than 150 million Americans, said Christen Linke Young, an attorney and fellow for the liberal-leaning USC-Brookings Schaeffer Initiative on Health Policy.
“The ACA’s changes to Medicare would be undone, reinstating copays on preventive services and reopening the prescription drug ‘donut hole,’ ” Ms. Young testified at the hearing. “It would also create major confusion in Medicare payment, as the ACA policies that are today fully integrated into the Medicare payment rules would suddenly lack a legislative basis.”
Ms. Linke Young was one of five witnesses who testified before lawmakers about the implications of Texas v. United States, an ongoing legal case that centers on whether a part of the health care law should be severed and if so, whether the entire law should then fall.
A group of Republican state attorneys general sued over the law in 2018, arguing that, because budget legislation in 2017 zeroed out the penalties associated with the ACA’s individual mandate, the mandate is invalid. The attorneys general also argue that, if the mandate is severed, the entire ACA should be struck down.
In response to the suit, the Trump administration agreed that the mandate is unconstitutional and should be parsed. Attorneys for the administration wrote that, if the mandate is found unconstitutional, the court should also consider finding two other provisions – the guaranteed issue and community rating requirements – of the ACA invalid. Guaranteed issue refers to insurers in the individual market offering coverage to all citizens, regardless of preexisting conditions, while community rating refers to charging equal premiums to every patient, no matter their past health status. The remainder of the ACA can stand without the three linked provisions, according to the Trump administration, which refused to defend the case.
A coalition of 17 Democratic attorneys general have stepped in to defend the case.
In December, a district court declared the entire ACA to be invalid, a decision immediately appealed to the 5th Circuit by the Democratic attorneys general. In January, the circuit court froze the case in light of the federal government’s partial shutdown. The case remains on hold.
At the hearing, Thomas P. Miller, a resident fellow at the conservative-leaning American Enterprise Institute, testified that a 5th Circuit decision would not likely come before summer 2019, followed by a potential U.S. Supreme Court reading in 2020 – if the case gets that far.
“The probability of a Supreme Court ruling that would overturn the entire ACA remains very low, despite last December’s decision at the federal district court level reaching exactly that legal conclusion,” Mr. Miller testified. “Given the murkiness of divining legislative intent in harder cases like the ACA, challenges to the individual mandate, past and present, it’s better to conclude that, although several different severability settings are hypothetically conceivable, it remains all but certain that an ultimate Supreme Court ruling in this case will, at a minimum, follow its previous inclinations revealed in the 2012 and 2015 ACA challenges and try to save as much of the law as possible.”
If the individual mandate is ultimately severed from the ACA, the decision would have little impact on beneficiaries or function of the health care law, according to Simon Lazarus, a lawyer and writer on constitutional and legal issues.
“Such a result will have virtually no impact on the operation of the ACA, nor on the millions of Americans – in reality, substantially all Americans – who depend on the ACA and its guarantees for people with preexisting conditions and myriad other protections that now are ‘baked into’ the national health care system,” Mr. Lazarus testified at the hearing. “To declare invalid the law’s shared responsibility payment provision, when that provision has no financial penalty behind it, will, by itself, have little if any depressive effect on the number of enrollees in health insurance plans.”
However, Mr. Lazarus noted that the guaranteed issue and community rating provisions of the law are “critical protections” for people with preexisting conditions.
Avik Roy, president for the Foundation for Research on Equal Opportunity, a nonpartisan organization that supports universal health care, testified that the Trump administration’s position about the mandate being tied to the guaranteed issue and community rating provisions is being mischaracterized as implying the administration opposes protecting people with preexisting conditions. President Trump has repeatedly expressed that any reforms or replacements of the ACA cover those with preexisting conditions, he said.
Mr. Roy recommended that Congress pass a bill reiterating the guaranteed issue and community rating requirements in the individual market to ensure protection for patients with preexisting conditions in light of Texas v. United States.
“I understand that a motion to produce such legislation was proposed by House Republicans during floor debate at the beginning of this Congress, [a bill] that would guarantee that no American could be denied coverage, or be charged higher premiums or cost sharing, as a result of a previous or current illness – and that the motion was defeated by the majority,” Mr. Roy testified. To me, this is a shame, as such legislation would ensure that Americans with preexisting conditions would be protected whatever the courts decide. I hope that Congress will reconsider its position.”
A number of subcommittee members pledged their support for protecting people with preexisting conditions and encouraged discussion of further legislation proposals.
“Let me speak on behalf of Republicans; we fully support protecting Americans with preexisting conditions,” said Rep. Greg Walden (R-Ore.), ranking member of the full committee. “We’ve said this repeatedly, we’ve acted accordingly, and we mean it completely. We could and should inject certainly into the system by passing legislation to protect those with preexisting conditions.”
Rep. Michael Burgess, MD, (R-Texas) questioned why the subcommittee was having a hearing on Texas v. United States, rather than focusing on making specific health policy improvements.
“It’s unfortunate we’re having a hearing that doesn’t move toward the development of any policies that will actually improve health care for Americans,” Rep. Burgess said during the hearing. “To that effect, there are numerous options that you could bring before us that could moot [Texas v. United States], but the subcommittee apparently has chosen not to do so.”
Committee Chairman Frank Pallone Jr. (D-N.J.), who called for the hearing, took offense at Rep. Burgess’ statements, expressing the importance of the hearing and the case at large.
“I saw no effort at all in the time that you were the chairman [of the health subcommittee] to try to work toward solutions in improving the ACA,” Rep. Pallone said. “What I saw were constant efforts to join with President Trump to sabotage it. ... and the reason that this hearing is so important is because the ultimate sabotage would be to have the courts rule that the ACA was unconstitutional, which is totally bogus.”
The Subcommittee on Health will hold another hearing on Feb. 13 to discuss ACA legislation and protections for patients with preexisting conditions.
If Republican state attorneys general prevail in their legal bid to overturn the Affordable Care Act, patients with preexisting conditions will lose their coverage protections, and an additional 24 million Americans could become uninsured, according to testimony presented at a Feb. 6 hearing of the House Energy and Commerce Health Subcommittee.
A ruling for the plaintiffs in Texas v. United States also would mean the ACA’s consumer protections for employer-based coverage would be eliminated, affecting more than 150 million Americans, said Christen Linke Young, an attorney and fellow for the liberal-leaning USC-Brookings Schaeffer Initiative on Health Policy.
“The ACA’s changes to Medicare would be undone, reinstating copays on preventive services and reopening the prescription drug ‘donut hole,’ ” Ms. Young testified at the hearing. “It would also create major confusion in Medicare payment, as the ACA policies that are today fully integrated into the Medicare payment rules would suddenly lack a legislative basis.”
Ms. Linke Young was one of five witnesses who testified before lawmakers about the implications of Texas v. United States, an ongoing legal case that centers on whether a part of the health care law should be severed and if so, whether the entire law should then fall.
A group of Republican state attorneys general sued over the law in 2018, arguing that, because budget legislation in 2017 zeroed out the penalties associated with the ACA’s individual mandate, the mandate is invalid. The attorneys general also argue that, if the mandate is severed, the entire ACA should be struck down.
In response to the suit, the Trump administration agreed that the mandate is unconstitutional and should be parsed. Attorneys for the administration wrote that, if the mandate is found unconstitutional, the court should also consider finding two other provisions – the guaranteed issue and community rating requirements – of the ACA invalid. Guaranteed issue refers to insurers in the individual market offering coverage to all citizens, regardless of preexisting conditions, while community rating refers to charging equal premiums to every patient, no matter their past health status. The remainder of the ACA can stand without the three linked provisions, according to the Trump administration, which refused to defend the case.
A coalition of 17 Democratic attorneys general have stepped in to defend the case.
In December, a district court declared the entire ACA to be invalid, a decision immediately appealed to the 5th Circuit by the Democratic attorneys general. In January, the circuit court froze the case in light of the federal government’s partial shutdown. The case remains on hold.
At the hearing, Thomas P. Miller, a resident fellow at the conservative-leaning American Enterprise Institute, testified that a 5th Circuit decision would not likely come before summer 2019, followed by a potential U.S. Supreme Court reading in 2020 – if the case gets that far.
“The probability of a Supreme Court ruling that would overturn the entire ACA remains very low, despite last December’s decision at the federal district court level reaching exactly that legal conclusion,” Mr. Miller testified. “Given the murkiness of divining legislative intent in harder cases like the ACA, challenges to the individual mandate, past and present, it’s better to conclude that, although several different severability settings are hypothetically conceivable, it remains all but certain that an ultimate Supreme Court ruling in this case will, at a minimum, follow its previous inclinations revealed in the 2012 and 2015 ACA challenges and try to save as much of the law as possible.”
If the individual mandate is ultimately severed from the ACA, the decision would have little impact on beneficiaries or function of the health care law, according to Simon Lazarus, a lawyer and writer on constitutional and legal issues.
“Such a result will have virtually no impact on the operation of the ACA, nor on the millions of Americans – in reality, substantially all Americans – who depend on the ACA and its guarantees for people with preexisting conditions and myriad other protections that now are ‘baked into’ the national health care system,” Mr. Lazarus testified at the hearing. “To declare invalid the law’s shared responsibility payment provision, when that provision has no financial penalty behind it, will, by itself, have little if any depressive effect on the number of enrollees in health insurance plans.”
However, Mr. Lazarus noted that the guaranteed issue and community rating provisions of the law are “critical protections” for people with preexisting conditions.
Avik Roy, president for the Foundation for Research on Equal Opportunity, a nonpartisan organization that supports universal health care, testified that the Trump administration’s position about the mandate being tied to the guaranteed issue and community rating provisions is being mischaracterized as implying the administration opposes protecting people with preexisting conditions. President Trump has repeatedly expressed that any reforms or replacements of the ACA cover those with preexisting conditions, he said.
Mr. Roy recommended that Congress pass a bill reiterating the guaranteed issue and community rating requirements in the individual market to ensure protection for patients with preexisting conditions in light of Texas v. United States.
“I understand that a motion to produce such legislation was proposed by House Republicans during floor debate at the beginning of this Congress, [a bill] that would guarantee that no American could be denied coverage, or be charged higher premiums or cost sharing, as a result of a previous or current illness – and that the motion was defeated by the majority,” Mr. Roy testified. To me, this is a shame, as such legislation would ensure that Americans with preexisting conditions would be protected whatever the courts decide. I hope that Congress will reconsider its position.”
A number of subcommittee members pledged their support for protecting people with preexisting conditions and encouraged discussion of further legislation proposals.
“Let me speak on behalf of Republicans; we fully support protecting Americans with preexisting conditions,” said Rep. Greg Walden (R-Ore.), ranking member of the full committee. “We’ve said this repeatedly, we’ve acted accordingly, and we mean it completely. We could and should inject certainly into the system by passing legislation to protect those with preexisting conditions.”
Rep. Michael Burgess, MD, (R-Texas) questioned why the subcommittee was having a hearing on Texas v. United States, rather than focusing on making specific health policy improvements.
“It’s unfortunate we’re having a hearing that doesn’t move toward the development of any policies that will actually improve health care for Americans,” Rep. Burgess said during the hearing. “To that effect, there are numerous options that you could bring before us that could moot [Texas v. United States], but the subcommittee apparently has chosen not to do so.”
Committee Chairman Frank Pallone Jr. (D-N.J.), who called for the hearing, took offense at Rep. Burgess’ statements, expressing the importance of the hearing and the case at large.
“I saw no effort at all in the time that you were the chairman [of the health subcommittee] to try to work toward solutions in improving the ACA,” Rep. Pallone said. “What I saw were constant efforts to join with President Trump to sabotage it. ... and the reason that this hearing is so important is because the ultimate sabotage would be to have the courts rule that the ACA was unconstitutional, which is totally bogus.”
The Subcommittee on Health will hold another hearing on Feb. 13 to discuss ACA legislation and protections for patients with preexisting conditions.
REPORTING FROM A HEALTH SUBCOMMITTEE HEARING
Nonsurgical OSA treatment ineffective in children with Down syndrome
CORONADO, CALIF. – Resolution of who were treated nonsurgically with either medication, observation, or supplemental oxygen was low, results from a small cohort study showed.
“This suggests that we should consider early treatment options, including multimodal approaches, for children with mild OSA and Down syndrome,” one of the study authors, Javier J.M. Howard, MPH, said at the Triological Society’s Combined Sections Meeting. “Prospective studies with longer follow-up are needed to better understand treatment outcomes in children with Down syndrome and mild OSA.”
An estimated 1%-6% of otherwise healthy children have obstructive sleep apnea, but the prevalence in children with Down syndrome is estimated to be between 30% and 70%, said Mr. Howard, a medical student at the University of Cincinnati. Additionally, those with Down syndrome tend to have more severe phenotypes, including significant hypoxemia and hypoventilation, compared with children without Down syndrome. “Nasal steroids, oral antileukotrienes, and supplemental oxygen have shown efficacy in the treatment of mild OSA in otherwise healthy children,” he said. “Observation is also employed in children with mild OSA, as a proportion of them will resolve spontaneously. The efficacy of these approaches in children with Down syndrome is unknown.”
In a study led by senior author Stacey L. Ishman, MD, MPH, researchers set out to examine the efficacy of single-medication therapy with either montelukast or intransal steroids versus observation versus oxygen on polysomnographic (PSG) outcomes in children with Down syndrome. They conducted a retrospective chart review of 24 children diagnosed with Down syndrome and mild OSA. The children were surgically naive and were treated between 2012 and 2017 with either supplemental oxygen, a single medication, or were observed. They had a follow-up PSG 3-12 months after initiation of treatment. The primary outcome was obstructive apnea hypopnea index (AHI), while secondary outcomes were oxygen saturation nadir, percent of total sleep time in rapid eye movement, and percentage of total sleep time with end-tidal carbon dioxide of greater than 50 mm Hg.
Of the 24 children, 58% were female, 67% were white, 13 were treated with observation, one was treated with oxygen, and 10 were treated with medication. Their baseline obstructive AHIs were 2.9, 3.5, and 3.3 events per hour, respectively. The follow-up PSGs revealed no statistically significant changes in obstructive AHI, oxygen saturation nadir, percentage of total sleep time in rapid eye movement, or percentage of total sleep time with end-tidal carbon dioxide greater than 50 mm Hg for any treatment group. OSA resolved in one patient in the observation group and in two patients in the medication group. At the same time, OSA worsened in two patients each in the medication and observation groups. Resolution of OSA was observed in 20% of patients in the medication group, compared with 7.1% of those in the observation or oxygen group (P = .82).
Mr. Howard acknowledged certain limitations of the study, including the potential for selection bias, its retrospective design, and its small sample size. “Resolution of mild OSA was low for all of our treatment groups after 3-12 months of treatment,” he said. “Resolution with medication was lower in our study, compared to published studies in otherwise healthy children.”
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: Howard J et al .Triological CSM, Abstracts.
CORONADO, CALIF. – Resolution of who were treated nonsurgically with either medication, observation, or supplemental oxygen was low, results from a small cohort study showed.
“This suggests that we should consider early treatment options, including multimodal approaches, for children with mild OSA and Down syndrome,” one of the study authors, Javier J.M. Howard, MPH, said at the Triological Society’s Combined Sections Meeting. “Prospective studies with longer follow-up are needed to better understand treatment outcomes in children with Down syndrome and mild OSA.”
An estimated 1%-6% of otherwise healthy children have obstructive sleep apnea, but the prevalence in children with Down syndrome is estimated to be between 30% and 70%, said Mr. Howard, a medical student at the University of Cincinnati. Additionally, those with Down syndrome tend to have more severe phenotypes, including significant hypoxemia and hypoventilation, compared with children without Down syndrome. “Nasal steroids, oral antileukotrienes, and supplemental oxygen have shown efficacy in the treatment of mild OSA in otherwise healthy children,” he said. “Observation is also employed in children with mild OSA, as a proportion of them will resolve spontaneously. The efficacy of these approaches in children with Down syndrome is unknown.”
In a study led by senior author Stacey L. Ishman, MD, MPH, researchers set out to examine the efficacy of single-medication therapy with either montelukast or intransal steroids versus observation versus oxygen on polysomnographic (PSG) outcomes in children with Down syndrome. They conducted a retrospective chart review of 24 children diagnosed with Down syndrome and mild OSA. The children were surgically naive and were treated between 2012 and 2017 with either supplemental oxygen, a single medication, or were observed. They had a follow-up PSG 3-12 months after initiation of treatment. The primary outcome was obstructive apnea hypopnea index (AHI), while secondary outcomes were oxygen saturation nadir, percent of total sleep time in rapid eye movement, and percentage of total sleep time with end-tidal carbon dioxide of greater than 50 mm Hg.
Of the 24 children, 58% were female, 67% were white, 13 were treated with observation, one was treated with oxygen, and 10 were treated with medication. Their baseline obstructive AHIs were 2.9, 3.5, and 3.3 events per hour, respectively. The follow-up PSGs revealed no statistically significant changes in obstructive AHI, oxygen saturation nadir, percentage of total sleep time in rapid eye movement, or percentage of total sleep time with end-tidal carbon dioxide greater than 50 mm Hg for any treatment group. OSA resolved in one patient in the observation group and in two patients in the medication group. At the same time, OSA worsened in two patients each in the medication and observation groups. Resolution of OSA was observed in 20% of patients in the medication group, compared with 7.1% of those in the observation or oxygen group (P = .82).
Mr. Howard acknowledged certain limitations of the study, including the potential for selection bias, its retrospective design, and its small sample size. “Resolution of mild OSA was low for all of our treatment groups after 3-12 months of treatment,” he said. “Resolution with medication was lower in our study, compared to published studies in otherwise healthy children.”
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: Howard J et al .Triological CSM, Abstracts.
CORONADO, CALIF. – Resolution of who were treated nonsurgically with either medication, observation, or supplemental oxygen was low, results from a small cohort study showed.
“This suggests that we should consider early treatment options, including multimodal approaches, for children with mild OSA and Down syndrome,” one of the study authors, Javier J.M. Howard, MPH, said at the Triological Society’s Combined Sections Meeting. “Prospective studies with longer follow-up are needed to better understand treatment outcomes in children with Down syndrome and mild OSA.”
An estimated 1%-6% of otherwise healthy children have obstructive sleep apnea, but the prevalence in children with Down syndrome is estimated to be between 30% and 70%, said Mr. Howard, a medical student at the University of Cincinnati. Additionally, those with Down syndrome tend to have more severe phenotypes, including significant hypoxemia and hypoventilation, compared with children without Down syndrome. “Nasal steroids, oral antileukotrienes, and supplemental oxygen have shown efficacy in the treatment of mild OSA in otherwise healthy children,” he said. “Observation is also employed in children with mild OSA, as a proportion of them will resolve spontaneously. The efficacy of these approaches in children with Down syndrome is unknown.”
In a study led by senior author Stacey L. Ishman, MD, MPH, researchers set out to examine the efficacy of single-medication therapy with either montelukast or intransal steroids versus observation versus oxygen on polysomnographic (PSG) outcomes in children with Down syndrome. They conducted a retrospective chart review of 24 children diagnosed with Down syndrome and mild OSA. The children were surgically naive and were treated between 2012 and 2017 with either supplemental oxygen, a single medication, or were observed. They had a follow-up PSG 3-12 months after initiation of treatment. The primary outcome was obstructive apnea hypopnea index (AHI), while secondary outcomes were oxygen saturation nadir, percent of total sleep time in rapid eye movement, and percentage of total sleep time with end-tidal carbon dioxide of greater than 50 mm Hg.
Of the 24 children, 58% were female, 67% were white, 13 were treated with observation, one was treated with oxygen, and 10 were treated with medication. Their baseline obstructive AHIs were 2.9, 3.5, and 3.3 events per hour, respectively. The follow-up PSGs revealed no statistically significant changes in obstructive AHI, oxygen saturation nadir, percentage of total sleep time in rapid eye movement, or percentage of total sleep time with end-tidal carbon dioxide greater than 50 mm Hg for any treatment group. OSA resolved in one patient in the observation group and in two patients in the medication group. At the same time, OSA worsened in two patients each in the medication and observation groups. Resolution of OSA was observed in 20% of patients in the medication group, compared with 7.1% of those in the observation or oxygen group (P = .82).
Mr. Howard acknowledged certain limitations of the study, including the potential for selection bias, its retrospective design, and its small sample size. “Resolution of mild OSA was low for all of our treatment groups after 3-12 months of treatment,” he said. “Resolution with medication was lower in our study, compared to published studies in otherwise healthy children.”
The researchers reported having no financial disclosures. The meeting was jointly sponsored by the Triological Society and the American College of Surgeons.
SOURCE: Howard J et al .Triological CSM, Abstracts.
REPORTING FROM TRIOLOGICAL CSM
Key clinical point: Resolution of mild OSA was low for all treatment groups after 3-12 months of treatment.
Major finding: Resolution of OSA was observed in 20% of patients in the medication group, compared with 7.1% of those in the observation or oxygen group (P = .82).
Study details: A retrospective chart review of 24 children diagnosed with Down syndrome and mild OSA.
Disclosures: The researchers reported having no financial disclosures.
Source: Howard J et al. Triological CSM, Abstracts.
Asthma, obesity, and the risk for severe sleep apnea in children
CORONADO, CALIF. –
“We have a good idea that obesity and asthma independently increase the risk of OSA, but a lot of the time in the pediatric population, these risk factors are found comorbid,” Ajay Narayanan at the Triological Society’s Combined Sections Meeting. “For this study we asked, how does the presence of asthma change the likelihood of having severe OSA in a cohort of obese patients? Knowing that both asthma and obesity independently increase the risk for OSA, we hypothesized that when they were comorbid, asthma would have a synergistic effect with obesity, causing severe OSA.”
Mr. Narayanan, a third-year student at the University of Texas Southwestern Medical Center, Dallas, and his colleagues performed a retrospective chart review of 367 children aged 9-17 years referred for a full-night polysomnography (PSG) for suspicion of having OSA. Demographic variables recorded included race, body mass index, rhinitis, gastroesophageal reflux disease, and tonsillar hypertrophy. Sleep variables recorded included apnea hypopnea index (AHI), sleep efficiency, rapid eye movement, and the peripheral capillary oxygen saturation (SpO2) nadir. The primary outcome was severe OSA defined as an AHI of 10 or greater on the PSG. They used logistic modeling to determine the association between asthma, obesity, and severe OSA.
The mean age of the study population was 14 years, 56% were male, and 43% were Hispanic. Of the 367 patients, 77 were neither obese nor asthmatic, 93 were nonobese but were asthmatic, 102 were obese but were nonasthmatic, and 95 were both obese and asthmatic. PSG results confirmed that obesity was associated with more signs of sleep apnea. For example, the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, while the obese, nonasthmatic group had a mean AHI of 19 events per hour. “We observed a similar trend amongst our asthmatic population,” Mr. Narayanan said. “We observed an increase in the mean AHI amongst our asthmatic kids when we added obesity to the picture. Surprisingly, we found that asthma was associated with having fewer signs of sleep apnea.” Specifically, while the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, those in the nonobese, asthmatic group had a mean of 5.6 events per hour (P = .005). “The finding was similar amongst our obese kids,” he said. “We saw a decrease in the mean AHI of our obese kids when we added asthma to the picture.”
On logistic regression analysis using obesity and asthma as independent variables, the researchers found that obesity increased the risk of severe OSA by 2.4-fold, but asthma decreased the odds of having severe OSA by about half (0.55). On multiple logistic regression controlling for commonly associated factors such as tonsillar hypertrophy, black race, and Hispanic ethnicity, obesity increased the risk of severe OSA by 2.2-fold, while asthma decreased the odds of having severe OSA by about half (0.51).
“In trying to explain this finding, we can turn to how these diseases are treated,” Mr. Narayanan said. “I say this because of the proven association between preexisting asthma and new onset OSA. Some of the reasons for this association include the tendency for airway collapsibility and systemwide inflammation seen in asthma, which then might contribute to the development of OSA. If we treat asthma symptoms early on, it might prevent the progression to sleep apnea down the line.”
Considering how prevalent comorbid asthma and OSA is, he continued, “we need to confirm that it is in fact well-controlled asthma that is associated with lowering the risk of severe OSA. Once we do this, we can ask the question: Can we use asthma pharmacotherapy to treat OSA? Some studies have shown that inhaled corticosteroids and montelukast (Singulair) may be effective treatment options for kids with OSA, but there’s definitely room for more research in this field, [such as determining] which patients would most benefit from this pharmacotherapy.” The researchers reported having no financial disclosures.
SOURCE: Narayanan A et al. Triological CSM, Abstracts.
CORONADO, CALIF. –
“We have a good idea that obesity and asthma independently increase the risk of OSA, but a lot of the time in the pediatric population, these risk factors are found comorbid,” Ajay Narayanan at the Triological Society’s Combined Sections Meeting. “For this study we asked, how does the presence of asthma change the likelihood of having severe OSA in a cohort of obese patients? Knowing that both asthma and obesity independently increase the risk for OSA, we hypothesized that when they were comorbid, asthma would have a synergistic effect with obesity, causing severe OSA.”
Mr. Narayanan, a third-year student at the University of Texas Southwestern Medical Center, Dallas, and his colleagues performed a retrospective chart review of 367 children aged 9-17 years referred for a full-night polysomnography (PSG) for suspicion of having OSA. Demographic variables recorded included race, body mass index, rhinitis, gastroesophageal reflux disease, and tonsillar hypertrophy. Sleep variables recorded included apnea hypopnea index (AHI), sleep efficiency, rapid eye movement, and the peripheral capillary oxygen saturation (SpO2) nadir. The primary outcome was severe OSA defined as an AHI of 10 or greater on the PSG. They used logistic modeling to determine the association between asthma, obesity, and severe OSA.
The mean age of the study population was 14 years, 56% were male, and 43% were Hispanic. Of the 367 patients, 77 were neither obese nor asthmatic, 93 were nonobese but were asthmatic, 102 were obese but were nonasthmatic, and 95 were both obese and asthmatic. PSG results confirmed that obesity was associated with more signs of sleep apnea. For example, the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, while the obese, nonasthmatic group had a mean AHI of 19 events per hour. “We observed a similar trend amongst our asthmatic population,” Mr. Narayanan said. “We observed an increase in the mean AHI amongst our asthmatic kids when we added obesity to the picture. Surprisingly, we found that asthma was associated with having fewer signs of sleep apnea.” Specifically, while the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, those in the nonobese, asthmatic group had a mean of 5.6 events per hour (P = .005). “The finding was similar amongst our obese kids,” he said. “We saw a decrease in the mean AHI of our obese kids when we added asthma to the picture.”
On logistic regression analysis using obesity and asthma as independent variables, the researchers found that obesity increased the risk of severe OSA by 2.4-fold, but asthma decreased the odds of having severe OSA by about half (0.55). On multiple logistic regression controlling for commonly associated factors such as tonsillar hypertrophy, black race, and Hispanic ethnicity, obesity increased the risk of severe OSA by 2.2-fold, while asthma decreased the odds of having severe OSA by about half (0.51).
“In trying to explain this finding, we can turn to how these diseases are treated,” Mr. Narayanan said. “I say this because of the proven association between preexisting asthma and new onset OSA. Some of the reasons for this association include the tendency for airway collapsibility and systemwide inflammation seen in asthma, which then might contribute to the development of OSA. If we treat asthma symptoms early on, it might prevent the progression to sleep apnea down the line.”
Considering how prevalent comorbid asthma and OSA is, he continued, “we need to confirm that it is in fact well-controlled asthma that is associated with lowering the risk of severe OSA. Once we do this, we can ask the question: Can we use asthma pharmacotherapy to treat OSA? Some studies have shown that inhaled corticosteroids and montelukast (Singulair) may be effective treatment options for kids with OSA, but there’s definitely room for more research in this field, [such as determining] which patients would most benefit from this pharmacotherapy.” The researchers reported having no financial disclosures.
SOURCE: Narayanan A et al. Triological CSM, Abstracts.
CORONADO, CALIF. –
“We have a good idea that obesity and asthma independently increase the risk of OSA, but a lot of the time in the pediatric population, these risk factors are found comorbid,” Ajay Narayanan at the Triological Society’s Combined Sections Meeting. “For this study we asked, how does the presence of asthma change the likelihood of having severe OSA in a cohort of obese patients? Knowing that both asthma and obesity independently increase the risk for OSA, we hypothesized that when they were comorbid, asthma would have a synergistic effect with obesity, causing severe OSA.”
Mr. Narayanan, a third-year student at the University of Texas Southwestern Medical Center, Dallas, and his colleagues performed a retrospective chart review of 367 children aged 9-17 years referred for a full-night polysomnography (PSG) for suspicion of having OSA. Demographic variables recorded included race, body mass index, rhinitis, gastroesophageal reflux disease, and tonsillar hypertrophy. Sleep variables recorded included apnea hypopnea index (AHI), sleep efficiency, rapid eye movement, and the peripheral capillary oxygen saturation (SpO2) nadir. The primary outcome was severe OSA defined as an AHI of 10 or greater on the PSG. They used logistic modeling to determine the association between asthma, obesity, and severe OSA.
The mean age of the study population was 14 years, 56% were male, and 43% were Hispanic. Of the 367 patients, 77 were neither obese nor asthmatic, 93 were nonobese but were asthmatic, 102 were obese but were nonasthmatic, and 95 were both obese and asthmatic. PSG results confirmed that obesity was associated with more signs of sleep apnea. For example, the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, while the obese, nonasthmatic group had a mean AHI of 19 events per hour. “We observed a similar trend amongst our asthmatic population,” Mr. Narayanan said. “We observed an increase in the mean AHI amongst our asthmatic kids when we added obesity to the picture. Surprisingly, we found that asthma was associated with having fewer signs of sleep apnea.” Specifically, while the nonobese, nonasthmatic group had a mean AHI of 11 events per hour, those in the nonobese, asthmatic group had a mean of 5.6 events per hour (P = .005). “The finding was similar amongst our obese kids,” he said. “We saw a decrease in the mean AHI of our obese kids when we added asthma to the picture.”
On logistic regression analysis using obesity and asthma as independent variables, the researchers found that obesity increased the risk of severe OSA by 2.4-fold, but asthma decreased the odds of having severe OSA by about half (0.55). On multiple logistic regression controlling for commonly associated factors such as tonsillar hypertrophy, black race, and Hispanic ethnicity, obesity increased the risk of severe OSA by 2.2-fold, while asthma decreased the odds of having severe OSA by about half (0.51).
“In trying to explain this finding, we can turn to how these diseases are treated,” Mr. Narayanan said. “I say this because of the proven association between preexisting asthma and new onset OSA. Some of the reasons for this association include the tendency for airway collapsibility and systemwide inflammation seen in asthma, which then might contribute to the development of OSA. If we treat asthma symptoms early on, it might prevent the progression to sleep apnea down the line.”
Considering how prevalent comorbid asthma and OSA is, he continued, “we need to confirm that it is in fact well-controlled asthma that is associated with lowering the risk of severe OSA. Once we do this, we can ask the question: Can we use asthma pharmacotherapy to treat OSA? Some studies have shown that inhaled corticosteroids and montelukast (Singulair) may be effective treatment options for kids with OSA, but there’s definitely room for more research in this field, [such as determining] which patients would most benefit from this pharmacotherapy.” The researchers reported having no financial disclosures.
SOURCE: Narayanan A et al. Triological CSM, Abstracts.
REPORTING FROM THE TRIOLOGICAL CSM
Key clinical point: In children, having asthma could decrease the risk of having severe obstructive sleep apnea, regardless of their obesity status.
Major finding: On multiple logistic regression, obesity increased the risk of severe OSA by 2.2-fold, while asthma decreased the odds of having severe OSA by about half.
Study details: A retrospective review of 367 children referred for a full-night polysomnography for suspicion of having OSA.
Disclosures: The researchers reported having no financial disclosures.
Source: Narayanan A et al. Triological CSM, Abstracts.
Cilostazol plus aspirin or clopidogrel reduces the risk of recurrent stroke
HONOLULU – The combination also entails a similar risk of major bleeding, compared with aspirin and clopidogrel alone, according to results from the Cilostazol Stroke Prevention Study for Antiplatelet Combination (CSPS.com).
Dual-antiplatelet therapy with aspirin and clopidogrel reduced the rate of recurrent stroke in previous studies. The benefit of this drug combination is relatively short-lived, however, and long-term concomitant use of aspirin and clopidogrel entails a risk of major bleeding. Other data have indicated that cilostazol, which is approved by the Food and Drug Administration to alleviate intermittent claudication in patients with peripheral vascular disease, prevents stroke recurrence without increasing the incidence of serious bleeding, compared with aspirin, said Kazunori Toyoda, MD, PhD, who presented the results of the CSPS.com trial at the International Stroke Conference sponsored by the American Heart Association.
Dr. Toyoda of the National Cerebral and Cardiovascular Center in Osaka, Japan, and his colleagues randomized 1,879 high-risk patients at 8-180 days after the onset of noncardioembolic ischemic stroke identified on MRI to receive 81 or 100 mg aspirin or 50 or 75 mg clopidogrel alone, or a combination of cilostazol 100 mg twice daily with aspirin or clopidogrel. They conducted their open-label, parallel-group trial at 292 sites in Japan from December 2013 through March 2017.
To be considered at high risk, participants had to meet one or more of the following criteria: 50% or greater stenosis of a major intracranial artery, 50% or greater stenosis of an extracranial artery, and two or more vascular risk factors. The trial’s primary efficacy outcome was the first recurrence of ischemic stroke. Safety outcomes included severe or life-threatening bleeding.
The investigators ended the trial early because of a delay in recruiting patients. They enrolled 1,884 and randomized 1,879 of an anticipated 4,000 patients. At randomization, 41% in the dual-therapy group received aspirin and 59% clopidogrel, and in the monotherapy group, 40% received aspirin and 60% clopidogrel. Baseline characteristics were similar between the treatment groups. The population’s mean age was 70. Approximately 30% of patients were women.
During a median follow-up period of 17 months, ischemic stroke recurred in 29 of 932 patients receiving dual therapy including cilostazol for an annual rate of 2.2% and in 64 of 947 patients receiving monotherapy for an annual rate of 4.5% (hazard ratio, 0.49; 95% confidence interval, 0.31-0.76; P = .001). Severe or life-threatening bleeding occurred in 8 patients (0.6% per year) receiving dual therapy and 13 patients (0.9% per year) receiving monotherapy (HR, 0.66; 95% CI, 0.27-1.60; P = .354).
The study was funded by Otsuka Pharmaceutical, which manufactures cilostazol. Dr. Toyoda reported receiving support from Bayer Yakuhin, Daiichi Sankyo, Bristol-Myers Squibb, and Nippon Boehringer Ingelheim.
SOURCE: Toyoda K et al. ISC 2019, Abstract LB3.
HONOLULU – The combination also entails a similar risk of major bleeding, compared with aspirin and clopidogrel alone, according to results from the Cilostazol Stroke Prevention Study for Antiplatelet Combination (CSPS.com).
Dual-antiplatelet therapy with aspirin and clopidogrel reduced the rate of recurrent stroke in previous studies. The benefit of this drug combination is relatively short-lived, however, and long-term concomitant use of aspirin and clopidogrel entails a risk of major bleeding. Other data have indicated that cilostazol, which is approved by the Food and Drug Administration to alleviate intermittent claudication in patients with peripheral vascular disease, prevents stroke recurrence without increasing the incidence of serious bleeding, compared with aspirin, said Kazunori Toyoda, MD, PhD, who presented the results of the CSPS.com trial at the International Stroke Conference sponsored by the American Heart Association.
Dr. Toyoda of the National Cerebral and Cardiovascular Center in Osaka, Japan, and his colleagues randomized 1,879 high-risk patients at 8-180 days after the onset of noncardioembolic ischemic stroke identified on MRI to receive 81 or 100 mg aspirin or 50 or 75 mg clopidogrel alone, or a combination of cilostazol 100 mg twice daily with aspirin or clopidogrel. They conducted their open-label, parallel-group trial at 292 sites in Japan from December 2013 through March 2017.
To be considered at high risk, participants had to meet one or more of the following criteria: 50% or greater stenosis of a major intracranial artery, 50% or greater stenosis of an extracranial artery, and two or more vascular risk factors. The trial’s primary efficacy outcome was the first recurrence of ischemic stroke. Safety outcomes included severe or life-threatening bleeding.
The investigators ended the trial early because of a delay in recruiting patients. They enrolled 1,884 and randomized 1,879 of an anticipated 4,000 patients. At randomization, 41% in the dual-therapy group received aspirin and 59% clopidogrel, and in the monotherapy group, 40% received aspirin and 60% clopidogrel. Baseline characteristics were similar between the treatment groups. The population’s mean age was 70. Approximately 30% of patients were women.
During a median follow-up period of 17 months, ischemic stroke recurred in 29 of 932 patients receiving dual therapy including cilostazol for an annual rate of 2.2% and in 64 of 947 patients receiving monotherapy for an annual rate of 4.5% (hazard ratio, 0.49; 95% confidence interval, 0.31-0.76; P = .001). Severe or life-threatening bleeding occurred in 8 patients (0.6% per year) receiving dual therapy and 13 patients (0.9% per year) receiving monotherapy (HR, 0.66; 95% CI, 0.27-1.60; P = .354).
The study was funded by Otsuka Pharmaceutical, which manufactures cilostazol. Dr. Toyoda reported receiving support from Bayer Yakuhin, Daiichi Sankyo, Bristol-Myers Squibb, and Nippon Boehringer Ingelheim.
SOURCE: Toyoda K et al. ISC 2019, Abstract LB3.
HONOLULU – The combination also entails a similar risk of major bleeding, compared with aspirin and clopidogrel alone, according to results from the Cilostazol Stroke Prevention Study for Antiplatelet Combination (CSPS.com).
Dual-antiplatelet therapy with aspirin and clopidogrel reduced the rate of recurrent stroke in previous studies. The benefit of this drug combination is relatively short-lived, however, and long-term concomitant use of aspirin and clopidogrel entails a risk of major bleeding. Other data have indicated that cilostazol, which is approved by the Food and Drug Administration to alleviate intermittent claudication in patients with peripheral vascular disease, prevents stroke recurrence without increasing the incidence of serious bleeding, compared with aspirin, said Kazunori Toyoda, MD, PhD, who presented the results of the CSPS.com trial at the International Stroke Conference sponsored by the American Heart Association.
Dr. Toyoda of the National Cerebral and Cardiovascular Center in Osaka, Japan, and his colleagues randomized 1,879 high-risk patients at 8-180 days after the onset of noncardioembolic ischemic stroke identified on MRI to receive 81 or 100 mg aspirin or 50 or 75 mg clopidogrel alone, or a combination of cilostazol 100 mg twice daily with aspirin or clopidogrel. They conducted their open-label, parallel-group trial at 292 sites in Japan from December 2013 through March 2017.
To be considered at high risk, participants had to meet one or more of the following criteria: 50% or greater stenosis of a major intracranial artery, 50% or greater stenosis of an extracranial artery, and two or more vascular risk factors. The trial’s primary efficacy outcome was the first recurrence of ischemic stroke. Safety outcomes included severe or life-threatening bleeding.
The investigators ended the trial early because of a delay in recruiting patients. They enrolled 1,884 and randomized 1,879 of an anticipated 4,000 patients. At randomization, 41% in the dual-therapy group received aspirin and 59% clopidogrel, and in the monotherapy group, 40% received aspirin and 60% clopidogrel. Baseline characteristics were similar between the treatment groups. The population’s mean age was 70. Approximately 30% of patients were women.
During a median follow-up period of 17 months, ischemic stroke recurred in 29 of 932 patients receiving dual therapy including cilostazol for an annual rate of 2.2% and in 64 of 947 patients receiving monotherapy for an annual rate of 4.5% (hazard ratio, 0.49; 95% confidence interval, 0.31-0.76; P = .001). Severe or life-threatening bleeding occurred in 8 patients (0.6% per year) receiving dual therapy and 13 patients (0.9% per year) receiving monotherapy (HR, 0.66; 95% CI, 0.27-1.60; P = .354).
The study was funded by Otsuka Pharmaceutical, which manufactures cilostazol. Dr. Toyoda reported receiving support from Bayer Yakuhin, Daiichi Sankyo, Bristol-Myers Squibb, and Nippon Boehringer Ingelheim.
SOURCE: Toyoda K et al. ISC 2019, Abstract LB3.
REPORTING FROM ISC
Key clinical point: Treating patients at high risk of recurrent stroke with cilostazol and aspirin or clopidogrel reduced the risk of recurrent stroke more than either aspirin or clopidogrel alone and was just as safe.
Major finding: Dual therapy with cilostazol and aspirin or clopidogrel reduced the risk of recurrent stroke by approximately half, compared with aspirin or clopidogrel alone.
Study details: A multicenter, randomized, open-label, parallel-group trial including 1,879 patients at high risk of recurrent stroke.
Disclosures: Otsuka Pharmaceutical funded the study. The presenter reported receiving support from Bayer Yakuhin, Daiichi Sankyo, Bristol-Myers Squibb, and Nippon Boehringer Ingelheim.
Source: Toyoda K et al. ISC 2019, Abstract LB3.
Intensive insulin added no benefit for hyperglycemia after ischemic stroke
HONOLULU – In patients who were hyperglycemic following an acute ischemic stroke, intensive insulin control using a continuous insulin drip and an aggressive blood glucose target of 80-130 mg/dL provided no incremental benefit in clinical outcome, compared with a more standard approach of serial, subcutaneous insulin injections and a moderate blood glucose target in a multicenter, U.S. trial with more than 1,100 patients.
The results also highlighted the potential downside to aggressive insulin treatment, with an associated 2.6% incidence of severe hypoglycemia, defined as blood glucose falling below 40 mg/dL, Karen C. Johnston, MD, said at the International Stroke Conference sponsored by the American Heart Association.
“Our data suggest that subcutaneously administered insulin with a target blood glucose level of less than 180 mg/dL is the preferred treatment” because it produces similar efficacy without causing any episodes of severe hypoglycemia, concluded Dr. Johnston, professor and chair of neurology at the University of Virginia in Charlottesville. “There should be no further debate” over the potential superiority of a glucose target substantially below 180 mg/dL, she added in an interview.
Continuing to use a glucose target of less than 180 mg/dL and treating patients with subcutaneous insulin injections every 6 hours to achieve this will mean substantially less resource use and precludes the need for keeping patients in intensive care beds as is needed with an insulin drip, Dr. Johnston noted. A treatment target of less than 180 mg/dL is also consistent with the most recent American Heart Association stroke treatment guidelines, which listed a blood glucose target of 140-180 mg/dL as a class IIa recommendation (Stroke. 2018 March;49[3]:e66-99).
The SHINE (Stroke Hyperglycemia Insulin Network Effort) trial enrolled 1,151 adults diagnosed with an acute ischemic stroke at 63 U.S. centers during 2012-2018, excluding patients with type 1 diabetes. Patients had to enter the study within 12 hours of their last known well time, and with an elevated blood glucose level, above 110 mg/dL in patients with type 2 diabetes or at or above 150 mg/dL in other patients. The median glucose level of enrolled patients was about 188 mg/dL. Enrolled patients averaged 66 years old, and about 80% had type 2 diabetes. The median time from last known well to randomization was just over 7 hours. Almost two-thirds of the patients received thrombolytic treatment, and about 13% underwent thrombectomy.
During up to 72 hours of treatment following enrollment the patients in the standard-treatment arm showed a fairly steady average blood glucose level of 179 mg/dL; patients in the intensive arm showed a steady average of 118 mg/dL.
The study’s primary end point was the percentage of patients with a favorable outcome 90 days after enrollment based on their modified Rankin scale score at that time, with the scores that qualified for this end point varying depending on stroke severity at baseline. The percentage of patients achieving this was 20.5% among the intensive patients and 21.6% among those who received standard insulin treatment, a difference that was not statistically significant.
The findings left open the question of how to better manage acute ischemic stroke patients who present with hyperglycemia.
“Hyperglycemic stroke patients have worse outcomes than stroke patients without hyperglycemia. More aggressively treating the hyperglycemia did not help these patients, We need to figure out what will help them,” Dr. Johnson said.
SOURCE: Johnston KC et al. ISC 2019, Abstract LB1.
SHINE was a well-designed trial that was run with a high degree of rigor, and its results advance the field. The results left no doubt that the result was neutral, that , while resulting in an excess of severe hypoglycemia episodes.
Using a less intensive insulin regimen that does not require a continuous drip is easier. The question of how aggressive treatment needs to be when managing glucose in acute ischemic stroke patients is something that U.S. clinicians who care for stroke patients argue about virtually daily. At my center, Cedars-Sinai in Los Angeles, we have recently used an approach that blended standard insulin treatment with more aggressive treatment. The SHINE results may not be practice changing, but they will be argument changing. The new results will make a difference. We will now stop arguing. We now know what we need to do.
Patrick D. Lyden, MD , is professor and chair of neurology at Cedars-Sinai Medical Center in Los Angeles. He had no relevant disclosures. He made these comments in an interview.
SHINE was a well-designed trial that was run with a high degree of rigor, and its results advance the field. The results left no doubt that the result was neutral, that , while resulting in an excess of severe hypoglycemia episodes.
Using a less intensive insulin regimen that does not require a continuous drip is easier. The question of how aggressive treatment needs to be when managing glucose in acute ischemic stroke patients is something that U.S. clinicians who care for stroke patients argue about virtually daily. At my center, Cedars-Sinai in Los Angeles, we have recently used an approach that blended standard insulin treatment with more aggressive treatment. The SHINE results may not be practice changing, but they will be argument changing. The new results will make a difference. We will now stop arguing. We now know what we need to do.
Patrick D. Lyden, MD , is professor and chair of neurology at Cedars-Sinai Medical Center in Los Angeles. He had no relevant disclosures. He made these comments in an interview.
SHINE was a well-designed trial that was run with a high degree of rigor, and its results advance the field. The results left no doubt that the result was neutral, that , while resulting in an excess of severe hypoglycemia episodes.
Using a less intensive insulin regimen that does not require a continuous drip is easier. The question of how aggressive treatment needs to be when managing glucose in acute ischemic stroke patients is something that U.S. clinicians who care for stroke patients argue about virtually daily. At my center, Cedars-Sinai in Los Angeles, we have recently used an approach that blended standard insulin treatment with more aggressive treatment. The SHINE results may not be practice changing, but they will be argument changing. The new results will make a difference. We will now stop arguing. We now know what we need to do.
Patrick D. Lyden, MD , is professor and chair of neurology at Cedars-Sinai Medical Center in Los Angeles. He had no relevant disclosures. He made these comments in an interview.
HONOLULU – In patients who were hyperglycemic following an acute ischemic stroke, intensive insulin control using a continuous insulin drip and an aggressive blood glucose target of 80-130 mg/dL provided no incremental benefit in clinical outcome, compared with a more standard approach of serial, subcutaneous insulin injections and a moderate blood glucose target in a multicenter, U.S. trial with more than 1,100 patients.
The results also highlighted the potential downside to aggressive insulin treatment, with an associated 2.6% incidence of severe hypoglycemia, defined as blood glucose falling below 40 mg/dL, Karen C. Johnston, MD, said at the International Stroke Conference sponsored by the American Heart Association.
“Our data suggest that subcutaneously administered insulin with a target blood glucose level of less than 180 mg/dL is the preferred treatment” because it produces similar efficacy without causing any episodes of severe hypoglycemia, concluded Dr. Johnston, professor and chair of neurology at the University of Virginia in Charlottesville. “There should be no further debate” over the potential superiority of a glucose target substantially below 180 mg/dL, she added in an interview.
Continuing to use a glucose target of less than 180 mg/dL and treating patients with subcutaneous insulin injections every 6 hours to achieve this will mean substantially less resource use and precludes the need for keeping patients in intensive care beds as is needed with an insulin drip, Dr. Johnston noted. A treatment target of less than 180 mg/dL is also consistent with the most recent American Heart Association stroke treatment guidelines, which listed a blood glucose target of 140-180 mg/dL as a class IIa recommendation (Stroke. 2018 March;49[3]:e66-99).
The SHINE (Stroke Hyperglycemia Insulin Network Effort) trial enrolled 1,151 adults diagnosed with an acute ischemic stroke at 63 U.S. centers during 2012-2018, excluding patients with type 1 diabetes. Patients had to enter the study within 12 hours of their last known well time, and with an elevated blood glucose level, above 110 mg/dL in patients with type 2 diabetes or at or above 150 mg/dL in other patients. The median glucose level of enrolled patients was about 188 mg/dL. Enrolled patients averaged 66 years old, and about 80% had type 2 diabetes. The median time from last known well to randomization was just over 7 hours. Almost two-thirds of the patients received thrombolytic treatment, and about 13% underwent thrombectomy.
During up to 72 hours of treatment following enrollment the patients in the standard-treatment arm showed a fairly steady average blood glucose level of 179 mg/dL; patients in the intensive arm showed a steady average of 118 mg/dL.
The study’s primary end point was the percentage of patients with a favorable outcome 90 days after enrollment based on their modified Rankin scale score at that time, with the scores that qualified for this end point varying depending on stroke severity at baseline. The percentage of patients achieving this was 20.5% among the intensive patients and 21.6% among those who received standard insulin treatment, a difference that was not statistically significant.
The findings left open the question of how to better manage acute ischemic stroke patients who present with hyperglycemia.
“Hyperglycemic stroke patients have worse outcomes than stroke patients without hyperglycemia. More aggressively treating the hyperglycemia did not help these patients, We need to figure out what will help them,” Dr. Johnson said.
SOURCE: Johnston KC et al. ISC 2019, Abstract LB1.
HONOLULU – In patients who were hyperglycemic following an acute ischemic stroke, intensive insulin control using a continuous insulin drip and an aggressive blood glucose target of 80-130 mg/dL provided no incremental benefit in clinical outcome, compared with a more standard approach of serial, subcutaneous insulin injections and a moderate blood glucose target in a multicenter, U.S. trial with more than 1,100 patients.
The results also highlighted the potential downside to aggressive insulin treatment, with an associated 2.6% incidence of severe hypoglycemia, defined as blood glucose falling below 40 mg/dL, Karen C. Johnston, MD, said at the International Stroke Conference sponsored by the American Heart Association.
“Our data suggest that subcutaneously administered insulin with a target blood glucose level of less than 180 mg/dL is the preferred treatment” because it produces similar efficacy without causing any episodes of severe hypoglycemia, concluded Dr. Johnston, professor and chair of neurology at the University of Virginia in Charlottesville. “There should be no further debate” over the potential superiority of a glucose target substantially below 180 mg/dL, she added in an interview.
Continuing to use a glucose target of less than 180 mg/dL and treating patients with subcutaneous insulin injections every 6 hours to achieve this will mean substantially less resource use and precludes the need for keeping patients in intensive care beds as is needed with an insulin drip, Dr. Johnston noted. A treatment target of less than 180 mg/dL is also consistent with the most recent American Heart Association stroke treatment guidelines, which listed a blood glucose target of 140-180 mg/dL as a class IIa recommendation (Stroke. 2018 March;49[3]:e66-99).
The SHINE (Stroke Hyperglycemia Insulin Network Effort) trial enrolled 1,151 adults diagnosed with an acute ischemic stroke at 63 U.S. centers during 2012-2018, excluding patients with type 1 diabetes. Patients had to enter the study within 12 hours of their last known well time, and with an elevated blood glucose level, above 110 mg/dL in patients with type 2 diabetes or at or above 150 mg/dL in other patients. The median glucose level of enrolled patients was about 188 mg/dL. Enrolled patients averaged 66 years old, and about 80% had type 2 diabetes. The median time from last known well to randomization was just over 7 hours. Almost two-thirds of the patients received thrombolytic treatment, and about 13% underwent thrombectomy.
During up to 72 hours of treatment following enrollment the patients in the standard-treatment arm showed a fairly steady average blood glucose level of 179 mg/dL; patients in the intensive arm showed a steady average of 118 mg/dL.
The study’s primary end point was the percentage of patients with a favorable outcome 90 days after enrollment based on their modified Rankin scale score at that time, with the scores that qualified for this end point varying depending on stroke severity at baseline. The percentage of patients achieving this was 20.5% among the intensive patients and 21.6% among those who received standard insulin treatment, a difference that was not statistically significant.
The findings left open the question of how to better manage acute ischemic stroke patients who present with hyperglycemia.
“Hyperglycemic stroke patients have worse outcomes than stroke patients without hyperglycemia. More aggressively treating the hyperglycemia did not help these patients, We need to figure out what will help them,” Dr. Johnson said.
SOURCE: Johnston KC et al. ISC 2019, Abstract LB1.
REPORTING FROM ISC 2019
Key clinical point: Aggressive insulin management of hyperglycemia following an ischemic stroke gave no clinical benefit, compared with a standard approach.
Major finding: After 90 days, favorable outcomes occurred in 21% of patients on aggressive insulin treatment and 22% on standard treatment.
Study details: SHINE, a multicenter, randomized trial with 1,151 acute ischemic stroke patients.
Disclosures: SHINE received no commercial funding. Dr. Johnston had no disclosures.
Source: Johnston KC et al. ISC 2019, Abstract LB1.
Rise in HCV linked to OxyContin reformulation
Also today, public health experts have attributed to the opioid epidemic the recent alarming rise in the rate of hepatitis C virus infection. medical advice prompts unneeded emergency visits by patients with atrial fibrillation, and legal marijuana may complicate substance use disorder treatment in adolescents.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, public health experts have attributed to the opioid epidemic the recent alarming rise in the rate of hepatitis C virus infection. medical advice prompts unneeded emergency visits by patients with atrial fibrillation, and legal marijuana may complicate substance use disorder treatment in adolescents.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, public health experts have attributed to the opioid epidemic the recent alarming rise in the rate of hepatitis C virus infection. medical advice prompts unneeded emergency visits by patients with atrial fibrillation, and legal marijuana may complicate substance use disorder treatment in adolescents.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify