User login
From past to future
This month, the current Editor-in-Chief and his Editorial Board will conclude our 5-year term. Megan Adams MD, JD, MSc, from the University of Michigan School of Medicine will assume my position. She has a stellar academic, research, and teaching record and is one of the best writers I know. She and her Board of Editors will carry on the tradition of GIHN.
The idea of an official newspaper of the AGA came from AGA staff in 2006. The goals of the newspaper were twofold: to communicate the latest news and information to practitioners to help them stay at the forefront of patient care and to develop another revenue stream for our society. The newspaper was launched in January 2007 with Charles Lightdale MD, AGAF, as the first editor and Colin W. Howden MD, AGAF, as the second (each with 5-year terms). While they wrote occasional editorials, I began writing 300-word essays for each issue. I have tried diligently to maintain a balanced viewpoint for all my editorials, although this has been difficult in the recent past and current national environment.
The paper evolved from a simple print publication to a multimedia communications vehicle that includes online-only content, videos, supplements, quizzes, and more. Last year, we published our first “Data Trends,” a supplement containing 10 or so brief articles written by content experts, covering current topics of high interest. As the paper evolved, we broadened our target audience to include research scientists, international practitioners and others interested in digestive diseases.
As I did last month, I would like to thank the AGA and Frontline Medical Communications staff for their dedication and constant work to bring you this newspaper.
Finally, I would like to pay tribute to Tadataka “Tachi” Yamada, who died this last month at the age of 76 years. He was one of the premier advocates for global health. His contributions to our field thru research, philanthropy, and leadership were enormous. We will miss him greatly.
John I Allen, MD, MBA, AGAF
Editor in Chief
This month, the current Editor-in-Chief and his Editorial Board will conclude our 5-year term. Megan Adams MD, JD, MSc, from the University of Michigan School of Medicine will assume my position. She has a stellar academic, research, and teaching record and is one of the best writers I know. She and her Board of Editors will carry on the tradition of GIHN.
The idea of an official newspaper of the AGA came from AGA staff in 2006. The goals of the newspaper were twofold: to communicate the latest news and information to practitioners to help them stay at the forefront of patient care and to develop another revenue stream for our society. The newspaper was launched in January 2007 with Charles Lightdale MD, AGAF, as the first editor and Colin W. Howden MD, AGAF, as the second (each with 5-year terms). While they wrote occasional editorials, I began writing 300-word essays for each issue. I have tried diligently to maintain a balanced viewpoint for all my editorials, although this has been difficult in the recent past and current national environment.
The paper evolved from a simple print publication to a multimedia communications vehicle that includes online-only content, videos, supplements, quizzes, and more. Last year, we published our first “Data Trends,” a supplement containing 10 or so brief articles written by content experts, covering current topics of high interest. As the paper evolved, we broadened our target audience to include research scientists, international practitioners and others interested in digestive diseases.
As I did last month, I would like to thank the AGA and Frontline Medical Communications staff for their dedication and constant work to bring you this newspaper.
Finally, I would like to pay tribute to Tadataka “Tachi” Yamada, who died this last month at the age of 76 years. He was one of the premier advocates for global health. His contributions to our field thru research, philanthropy, and leadership were enormous. We will miss him greatly.
John I Allen, MD, MBA, AGAF
Editor in Chief
This month, the current Editor-in-Chief and his Editorial Board will conclude our 5-year term. Megan Adams MD, JD, MSc, from the University of Michigan School of Medicine will assume my position. She has a stellar academic, research, and teaching record and is one of the best writers I know. She and her Board of Editors will carry on the tradition of GIHN.
The idea of an official newspaper of the AGA came from AGA staff in 2006. The goals of the newspaper were twofold: to communicate the latest news and information to practitioners to help them stay at the forefront of patient care and to develop another revenue stream for our society. The newspaper was launched in January 2007 with Charles Lightdale MD, AGAF, as the first editor and Colin W. Howden MD, AGAF, as the second (each with 5-year terms). While they wrote occasional editorials, I began writing 300-word essays for each issue. I have tried diligently to maintain a balanced viewpoint for all my editorials, although this has been difficult in the recent past and current national environment.
The paper evolved from a simple print publication to a multimedia communications vehicle that includes online-only content, videos, supplements, quizzes, and more. Last year, we published our first “Data Trends,” a supplement containing 10 or so brief articles written by content experts, covering current topics of high interest. As the paper evolved, we broadened our target audience to include research scientists, international practitioners and others interested in digestive diseases.
As I did last month, I would like to thank the AGA and Frontline Medical Communications staff for their dedication and constant work to bring you this newspaper.
Finally, I would like to pay tribute to Tadataka “Tachi” Yamada, who died this last month at the age of 76 years. He was one of the premier advocates for global health. His contributions to our field thru research, philanthropy, and leadership were enormous. We will miss him greatly.
John I Allen, MD, MBA, AGAF
Editor in Chief
Four police suicides in the aftermath of the Capitol siege: What can we learn?
Officer Scott Davis is a passionate man who thinks and talks quickly. As a member of the Special Events Team for Montgomery County, Maryland, he was already staging in Rockville, outside of Washington, D.C., when the call came in last Jan. 6 to move their unit to the U.S. Capitol.
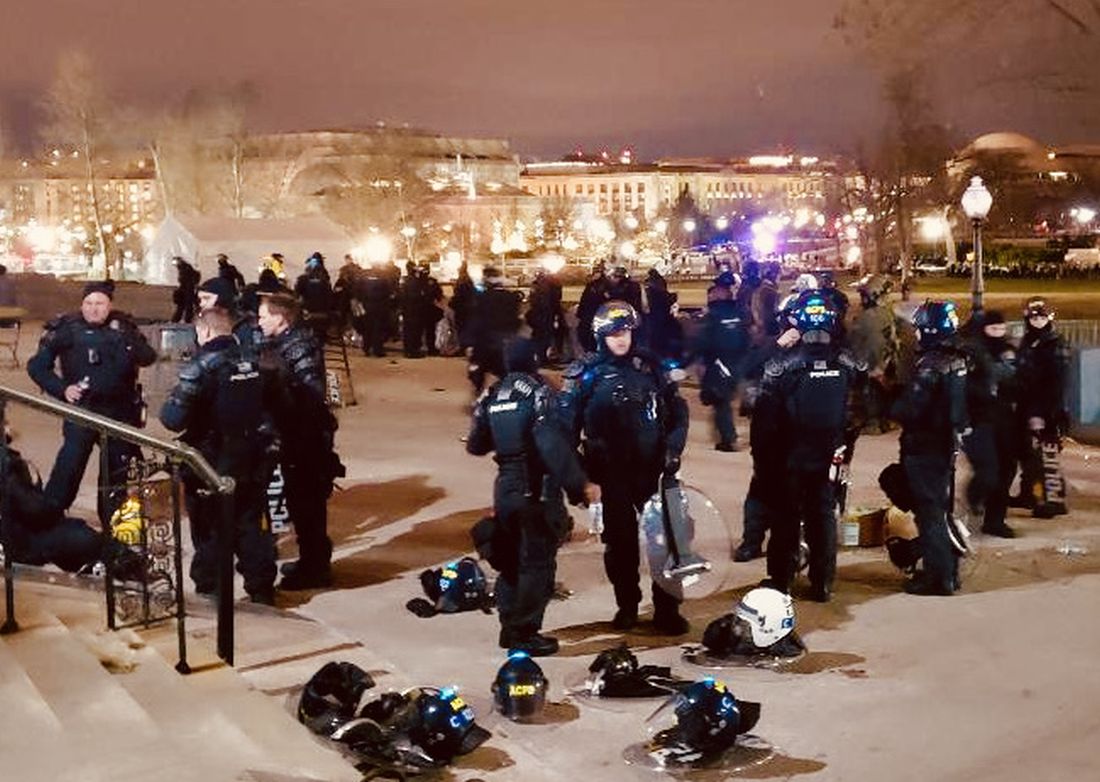
“It was surreal,” said Mr. Davis. “There were people from all different groups at the Capitol that day. Many people were trying to get out, but others surrounded us. They called us ‘human race traitors.’ And then I heard someone say, ‘It’s good you brought your shields, we’ll carry your bodies out on them.’”
Mr. Davis described hours of mayhem during which he was hit with bear spray, a brick, a chair, and a metal rod. One of the members of Mr. Davis’ unit remains on leave with a head injury nearly 9 months after the siege.
“It went on for 3 hours, but it felt like 15 minutes. Then, all of a sudden, it was over.”
For the members of law enforcement at the Capitol that day, the repercussions are still being felt, perhaps most notably in the case of the four officers who subsequently died of suicide. Three of the officers were with the Metropolitan Police Department of the District of Columbia and one worked for the Capitol Police Department.
Police officers are subjected to traumas on a regular basis and often placed in circumstances where their lives are in danger. Yet four suicides within a short time – all connected to a single event – is particularly shocking and tragic, even more so for how little attention it has garnered to date.
What contributes to the high rate of suicide among officers?
Scott Silverii, PhD, a former police officer and author of Broken and Blue: A Policeman’s Guide to Health, Hope, and Healing, commented that he “wouldn’t be surprised if there are more suicides to come.” This stems not only from the experiences of that day but also the elevated risk for suicide that law enforcement officers already experienced prior to the Capitol riots. Suicide remains a rare event, with a national all-population average of 13.9 per 100,000 citizens. But as Dr. Silverii noted, more officers die by suicide each year than are killed in the line of duty.
“Suicide is a big part of police culture – officers are doers and fixers, and it is seen as being more honorable to take yourself out of the equation than it is to ask for help,” he said. “Most officers come in with past pain, and this is a situation where they are being overwhelmed and under-respected. At the same time, police culture is a closed culture, and it is not friendly to researchers.”
Another contributor is the frequency with which law enforcement officers are exposed to trauma, according to Vernon Herron, Director of Officer Safety and Wellness for the Baltimore City Police.
Mr. Herron said, citing the psychiatric and addiction issues that officers commonly experience.
Protecting the protectors
Mr. Herron and others are working to address these problems head-on.
“We are trying to identify employees exposed to trauma and to offer counseling and intervention,” he said, “Otherwise, everything else will fall short.”
Yet implementing such measures is no easy task, given the lack of a central oversight organization for law enforcement, said Sheldon Greenberg, PhD, a former police officer and professor of management in the School of Education at Johns Hopkins University, Baltimore.
“In the United States there is no such thing as ‘The Police.’ There is no one in a position to set policy, standards, or training mandates nationally,” he said. “There are approximately 18,000 police and sheriff departments in the country, and many of them are small. No one can compel law enforcement agencies to implement officer wellness and suicide prevention programs, make counseling available to officers, or train supervisors and peers to identify suicide ideation.”
Dr. Greenberg said a further barrier to helping police officers considering self-harm is posed by the fact that even if they do seek out counseling, there is no guarantee that it will remain confidential.
“Support personnel have an obligation to report an officer who is thinking about committing suicide,” he said. “Many officers are concerned about this lack of confidentiality and that they may be branded if they seek help.”
Although Dr. Greenberg said many police officers are self-professed “action junkies,” even their unusually high capacity for stress is often tested by the realities of the job.
“Increasing demands for service, shortages of personnel, misinformation about police, COVID-19, talk about restructuring policing with little concrete direction, increased exposure to violence, greater numbers of vulnerable people, and more take a toll over time,” he lamented. “In addition, we are in a recruiting crisis in law enforcement, and there are no standards to ensure the quality of psychological screening provided to applicants. Many officers will go through their entire career and never be screened again. We know little about the stresses and strains that officers bring to the job.”
After the siege
It is not clear how many police officers were present at the Capitol on Jan. 6. During the chaos of the day, reinforcements to the Capitol Police Department arrived from Washington D.C., Maryland, and Virginia, but no official numbers on responders were obtained; Mr. Davis thought it was likely that there were at least 1,000 law enforcement officers present. Those who did respond sustained an estimated 100 injuries, including an officer who died the next day. Of the officers who died by suicide, one died 3 days after, another died 9 days later, and two more died in July – numbers that contradict the notion that this is some coincidence. Officer Alexander Kettering, a colleague of Mr. Davis who has been with Montgomery County Police for 15 years, was among those tasked with protecting the Capitol on Jan. 6. The chaos, violence, and destruction of the day has stuck with him and continues to occupy his thoughts.
“I had a front-row seat to the whole thing. It was overwhelming, and I’ve never seen people this angry,” said Mr. Kettering. “There were people up on the veranda and on the scaffolding set up for the inauguration. They were smashing windows and throwing things into the crowd. It was insane. There were decent people coming up to us and saying they would pray for us, then others calling us traitors, telling us to stand down and join them.”
In the aftermath of the Capitol siege, Mr. Kettering watched in dismay as the narrative of the day’s events began to warp.
“At first there was a consensus that what happened was so wrong, and then the politics took over. People were saying it wasn’t as bad as the media said, that it really wasn’t that violent and those speaking out are traitors or political operatives. I relive it every day, and it’s hard to escape, even in casual conversation.”
He added that the days’ events were compounded by the already heightened tensions surrounding the national debate around policing.
“It’s been 18 months of stress, of anti-police movements, and there is a fine line between addressing police brutality and being anti-police,” Mr. Kettering said, noting that the aforementioned issues have all contributed to the ongoing struggles his fellow officers are experiencing.
“It’s not a thing for cops to talk about how an event affected them,” he said. “A lot of officers have just shut down. People have careers and pensions to protect, and every time we stop a motorist, something could go wrong, even if we do everything right. There are mixed signals: They tell us, ‘Defend but don’t defend.’”
His colleague, Mr. Davis, said that officers “need more support from politicians,” noting that he felt particularly insulted by a comment made by a Montgomery County public official who accused the officers present at the Capitol of racism. “And finally, we feel a little betrayed by the public.”
More questions than answers from the Capitol’s day of chaos
What about the events of Jan. 6 led to the suicides of four law enforcement officers and what can be done to prevent more deaths in the future? There are the individual factors of each man’s personal history, circumstances, and vulnerabilities, including the sense of being personally endangered, witnessing trauma, and direct injury – one officer who died of suicide had sustained a head injury that day.
We don’t know if the officers went into the event with preexisting mental illness or addiction or if the day’s events precipitated psychiatric episodes. And with all the partisan anger surrounding the presidential election, we don’t know if each officer’s political beliefs amplified his distress over what occurred in a social media climate where police are being faulted by all sides.
When multiple suicides occur in a community, there is always concern about a “copycat” phenomena. These concerns are made more difficult to address, however, given the police culture of taboo and stigma associated with getting professional help, difficulty accessing care, and career repercussions for speaking openly about suicidal thoughts and mental health issues.
Finally, there is the current political agenda that leaves officers feeling unsupported, fearful of negative outcomes, and unappreciated. The Capitol siege in particular embodied a great deal of national distress and confusion over basic issues of truth, justice, and perceptions of reality in our polarized society.
Can we move to a place where those who enforce laws have easy access to treatment, free from stigma? Can we encourage a culture that does not tolerate brutality or racism, while also refusing to label all police as bad and lending support to their mission? Can we be more attuned to the repercussions of circumstances where officers are witnesses to trauma, are endangered themselves, and would benefit from acknowledgment of their distress?
Time will tell if our anti-police pendulum swings back. In the meantime, these four suicides among people defending our country remain tragically overlooked.
Dinah Miller, MD, is coauthor of Committed: The Battle Over Involuntary Psychiatric Care (Johns Hopkins University Press, 2016). She has a private practice in Baltimore and is an assistant professor of psychiatry and behavioral sciences at Johns Hopkins University. A version of this article first appeared on Medscape.com.
Officer Scott Davis is a passionate man who thinks and talks quickly. As a member of the Special Events Team for Montgomery County, Maryland, he was already staging in Rockville, outside of Washington, D.C., when the call came in last Jan. 6 to move their unit to the U.S. Capitol.
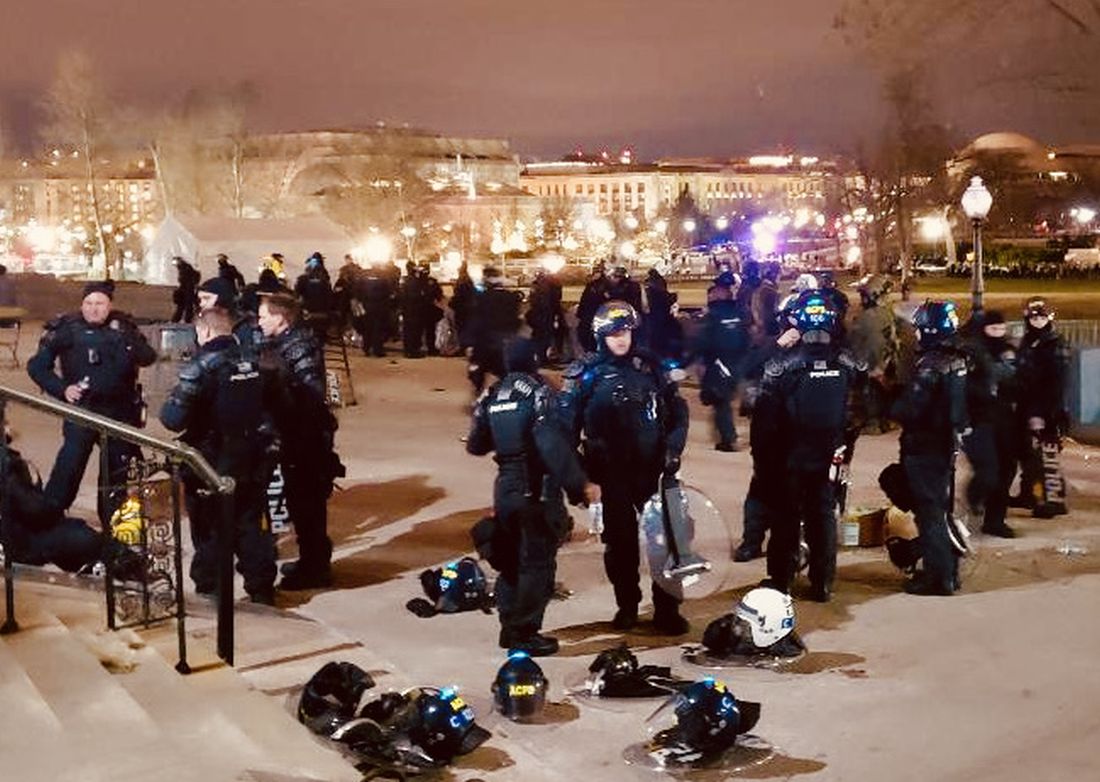
“It was surreal,” said Mr. Davis. “There were people from all different groups at the Capitol that day. Many people were trying to get out, but others surrounded us. They called us ‘human race traitors.’ And then I heard someone say, ‘It’s good you brought your shields, we’ll carry your bodies out on them.’”
Mr. Davis described hours of mayhem during which he was hit with bear spray, a brick, a chair, and a metal rod. One of the members of Mr. Davis’ unit remains on leave with a head injury nearly 9 months after the siege.
“It went on for 3 hours, but it felt like 15 minutes. Then, all of a sudden, it was over.”
For the members of law enforcement at the Capitol that day, the repercussions are still being felt, perhaps most notably in the case of the four officers who subsequently died of suicide. Three of the officers were with the Metropolitan Police Department of the District of Columbia and one worked for the Capitol Police Department.
Police officers are subjected to traumas on a regular basis and often placed in circumstances where their lives are in danger. Yet four suicides within a short time – all connected to a single event – is particularly shocking and tragic, even more so for how little attention it has garnered to date.
What contributes to the high rate of suicide among officers?
Scott Silverii, PhD, a former police officer and author of Broken and Blue: A Policeman’s Guide to Health, Hope, and Healing, commented that he “wouldn’t be surprised if there are more suicides to come.” This stems not only from the experiences of that day but also the elevated risk for suicide that law enforcement officers already experienced prior to the Capitol riots. Suicide remains a rare event, with a national all-population average of 13.9 per 100,000 citizens. But as Dr. Silverii noted, more officers die by suicide each year than are killed in the line of duty.
“Suicide is a big part of police culture – officers are doers and fixers, and it is seen as being more honorable to take yourself out of the equation than it is to ask for help,” he said. “Most officers come in with past pain, and this is a situation where they are being overwhelmed and under-respected. At the same time, police culture is a closed culture, and it is not friendly to researchers.”
Another contributor is the frequency with which law enforcement officers are exposed to trauma, according to Vernon Herron, Director of Officer Safety and Wellness for the Baltimore City Police.
Mr. Herron said, citing the psychiatric and addiction issues that officers commonly experience.
Protecting the protectors
Mr. Herron and others are working to address these problems head-on.
“We are trying to identify employees exposed to trauma and to offer counseling and intervention,” he said, “Otherwise, everything else will fall short.”
Yet implementing such measures is no easy task, given the lack of a central oversight organization for law enforcement, said Sheldon Greenberg, PhD, a former police officer and professor of management in the School of Education at Johns Hopkins University, Baltimore.
“In the United States there is no such thing as ‘The Police.’ There is no one in a position to set policy, standards, or training mandates nationally,” he said. “There are approximately 18,000 police and sheriff departments in the country, and many of them are small. No one can compel law enforcement agencies to implement officer wellness and suicide prevention programs, make counseling available to officers, or train supervisors and peers to identify suicide ideation.”
Dr. Greenberg said a further barrier to helping police officers considering self-harm is posed by the fact that even if they do seek out counseling, there is no guarantee that it will remain confidential.
“Support personnel have an obligation to report an officer who is thinking about committing suicide,” he said. “Many officers are concerned about this lack of confidentiality and that they may be branded if they seek help.”
Although Dr. Greenberg said many police officers are self-professed “action junkies,” even their unusually high capacity for stress is often tested by the realities of the job.
“Increasing demands for service, shortages of personnel, misinformation about police, COVID-19, talk about restructuring policing with little concrete direction, increased exposure to violence, greater numbers of vulnerable people, and more take a toll over time,” he lamented. “In addition, we are in a recruiting crisis in law enforcement, and there are no standards to ensure the quality of psychological screening provided to applicants. Many officers will go through their entire career and never be screened again. We know little about the stresses and strains that officers bring to the job.”
After the siege
It is not clear how many police officers were present at the Capitol on Jan. 6. During the chaos of the day, reinforcements to the Capitol Police Department arrived from Washington D.C., Maryland, and Virginia, but no official numbers on responders were obtained; Mr. Davis thought it was likely that there were at least 1,000 law enforcement officers present. Those who did respond sustained an estimated 100 injuries, including an officer who died the next day. Of the officers who died by suicide, one died 3 days after, another died 9 days later, and two more died in July – numbers that contradict the notion that this is some coincidence. Officer Alexander Kettering, a colleague of Mr. Davis who has been with Montgomery County Police for 15 years, was among those tasked with protecting the Capitol on Jan. 6. The chaos, violence, and destruction of the day has stuck with him and continues to occupy his thoughts.
“I had a front-row seat to the whole thing. It was overwhelming, and I’ve never seen people this angry,” said Mr. Kettering. “There were people up on the veranda and on the scaffolding set up for the inauguration. They were smashing windows and throwing things into the crowd. It was insane. There were decent people coming up to us and saying they would pray for us, then others calling us traitors, telling us to stand down and join them.”
In the aftermath of the Capitol siege, Mr. Kettering watched in dismay as the narrative of the day’s events began to warp.
“At first there was a consensus that what happened was so wrong, and then the politics took over. People were saying it wasn’t as bad as the media said, that it really wasn’t that violent and those speaking out are traitors or political operatives. I relive it every day, and it’s hard to escape, even in casual conversation.”
He added that the days’ events were compounded by the already heightened tensions surrounding the national debate around policing.
“It’s been 18 months of stress, of anti-police movements, and there is a fine line between addressing police brutality and being anti-police,” Mr. Kettering said, noting that the aforementioned issues have all contributed to the ongoing struggles his fellow officers are experiencing.
“It’s not a thing for cops to talk about how an event affected them,” he said. “A lot of officers have just shut down. People have careers and pensions to protect, and every time we stop a motorist, something could go wrong, even if we do everything right. There are mixed signals: They tell us, ‘Defend but don’t defend.’”
His colleague, Mr. Davis, said that officers “need more support from politicians,” noting that he felt particularly insulted by a comment made by a Montgomery County public official who accused the officers present at the Capitol of racism. “And finally, we feel a little betrayed by the public.”
More questions than answers from the Capitol’s day of chaos
What about the events of Jan. 6 led to the suicides of four law enforcement officers and what can be done to prevent more deaths in the future? There are the individual factors of each man’s personal history, circumstances, and vulnerabilities, including the sense of being personally endangered, witnessing trauma, and direct injury – one officer who died of suicide had sustained a head injury that day.
We don’t know if the officers went into the event with preexisting mental illness or addiction or if the day’s events precipitated psychiatric episodes. And with all the partisan anger surrounding the presidential election, we don’t know if each officer’s political beliefs amplified his distress over what occurred in a social media climate where police are being faulted by all sides.
When multiple suicides occur in a community, there is always concern about a “copycat” phenomena. These concerns are made more difficult to address, however, given the police culture of taboo and stigma associated with getting professional help, difficulty accessing care, and career repercussions for speaking openly about suicidal thoughts and mental health issues.
Finally, there is the current political agenda that leaves officers feeling unsupported, fearful of negative outcomes, and unappreciated. The Capitol siege in particular embodied a great deal of national distress and confusion over basic issues of truth, justice, and perceptions of reality in our polarized society.
Can we move to a place where those who enforce laws have easy access to treatment, free from stigma? Can we encourage a culture that does not tolerate brutality or racism, while also refusing to label all police as bad and lending support to their mission? Can we be more attuned to the repercussions of circumstances where officers are witnesses to trauma, are endangered themselves, and would benefit from acknowledgment of their distress?
Time will tell if our anti-police pendulum swings back. In the meantime, these four suicides among people defending our country remain tragically overlooked.
Dinah Miller, MD, is coauthor of Committed: The Battle Over Involuntary Psychiatric Care (Johns Hopkins University Press, 2016). She has a private practice in Baltimore and is an assistant professor of psychiatry and behavioral sciences at Johns Hopkins University. A version of this article first appeared on Medscape.com.
Officer Scott Davis is a passionate man who thinks and talks quickly. As a member of the Special Events Team for Montgomery County, Maryland, he was already staging in Rockville, outside of Washington, D.C., when the call came in last Jan. 6 to move their unit to the U.S. Capitol.
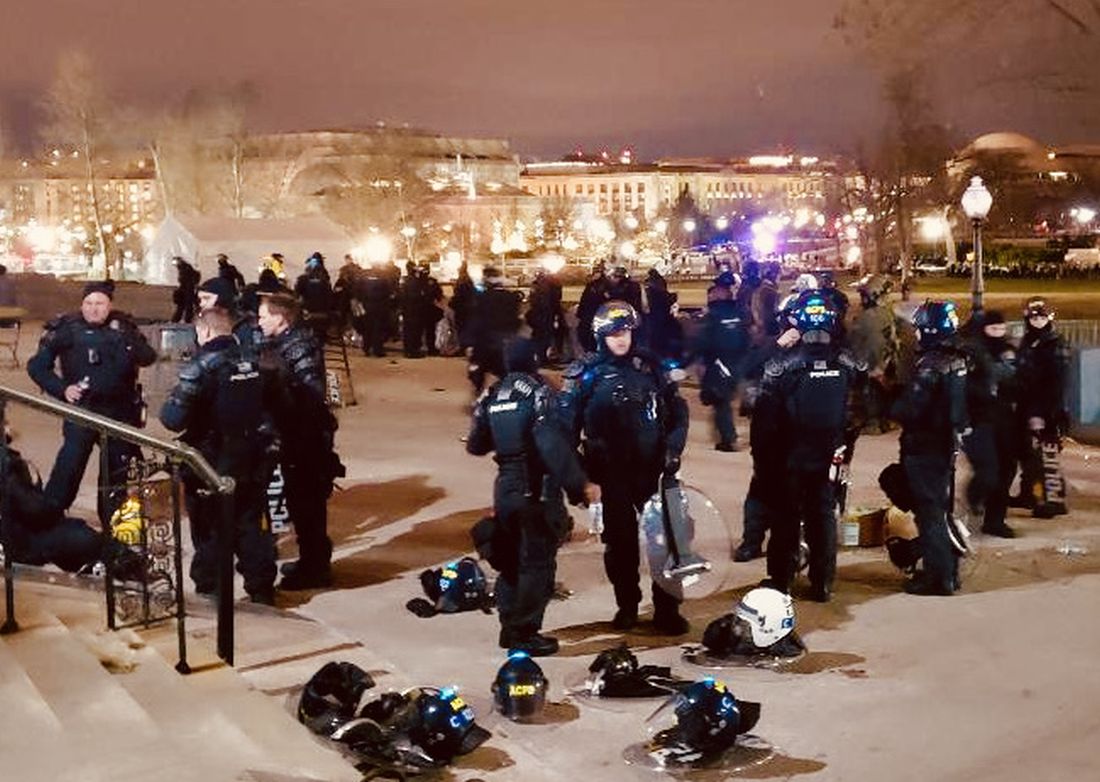
“It was surreal,” said Mr. Davis. “There were people from all different groups at the Capitol that day. Many people were trying to get out, but others surrounded us. They called us ‘human race traitors.’ And then I heard someone say, ‘It’s good you brought your shields, we’ll carry your bodies out on them.’”
Mr. Davis described hours of mayhem during which he was hit with bear spray, a brick, a chair, and a metal rod. One of the members of Mr. Davis’ unit remains on leave with a head injury nearly 9 months after the siege.
“It went on for 3 hours, but it felt like 15 minutes. Then, all of a sudden, it was over.”
For the members of law enforcement at the Capitol that day, the repercussions are still being felt, perhaps most notably in the case of the four officers who subsequently died of suicide. Three of the officers were with the Metropolitan Police Department of the District of Columbia and one worked for the Capitol Police Department.
Police officers are subjected to traumas on a regular basis and often placed in circumstances where their lives are in danger. Yet four suicides within a short time – all connected to a single event – is particularly shocking and tragic, even more so for how little attention it has garnered to date.
What contributes to the high rate of suicide among officers?
Scott Silverii, PhD, a former police officer and author of Broken and Blue: A Policeman’s Guide to Health, Hope, and Healing, commented that he “wouldn’t be surprised if there are more suicides to come.” This stems not only from the experiences of that day but also the elevated risk for suicide that law enforcement officers already experienced prior to the Capitol riots. Suicide remains a rare event, with a national all-population average of 13.9 per 100,000 citizens. But as Dr. Silverii noted, more officers die by suicide each year than are killed in the line of duty.
“Suicide is a big part of police culture – officers are doers and fixers, and it is seen as being more honorable to take yourself out of the equation than it is to ask for help,” he said. “Most officers come in with past pain, and this is a situation where they are being overwhelmed and under-respected. At the same time, police culture is a closed culture, and it is not friendly to researchers.”
Another contributor is the frequency with which law enforcement officers are exposed to trauma, according to Vernon Herron, Director of Officer Safety and Wellness for the Baltimore City Police.
Mr. Herron said, citing the psychiatric and addiction issues that officers commonly experience.
Protecting the protectors
Mr. Herron and others are working to address these problems head-on.
“We are trying to identify employees exposed to trauma and to offer counseling and intervention,” he said, “Otherwise, everything else will fall short.”
Yet implementing such measures is no easy task, given the lack of a central oversight organization for law enforcement, said Sheldon Greenberg, PhD, a former police officer and professor of management in the School of Education at Johns Hopkins University, Baltimore.
“In the United States there is no such thing as ‘The Police.’ There is no one in a position to set policy, standards, or training mandates nationally,” he said. “There are approximately 18,000 police and sheriff departments in the country, and many of them are small. No one can compel law enforcement agencies to implement officer wellness and suicide prevention programs, make counseling available to officers, or train supervisors and peers to identify suicide ideation.”
Dr. Greenberg said a further barrier to helping police officers considering self-harm is posed by the fact that even if they do seek out counseling, there is no guarantee that it will remain confidential.
“Support personnel have an obligation to report an officer who is thinking about committing suicide,” he said. “Many officers are concerned about this lack of confidentiality and that they may be branded if they seek help.”
Although Dr. Greenberg said many police officers are self-professed “action junkies,” even their unusually high capacity for stress is often tested by the realities of the job.
“Increasing demands for service, shortages of personnel, misinformation about police, COVID-19, talk about restructuring policing with little concrete direction, increased exposure to violence, greater numbers of vulnerable people, and more take a toll over time,” he lamented. “In addition, we are in a recruiting crisis in law enforcement, and there are no standards to ensure the quality of psychological screening provided to applicants. Many officers will go through their entire career and never be screened again. We know little about the stresses and strains that officers bring to the job.”
After the siege
It is not clear how many police officers were present at the Capitol on Jan. 6. During the chaos of the day, reinforcements to the Capitol Police Department arrived from Washington D.C., Maryland, and Virginia, but no official numbers on responders were obtained; Mr. Davis thought it was likely that there were at least 1,000 law enforcement officers present. Those who did respond sustained an estimated 100 injuries, including an officer who died the next day. Of the officers who died by suicide, one died 3 days after, another died 9 days later, and two more died in July – numbers that contradict the notion that this is some coincidence. Officer Alexander Kettering, a colleague of Mr. Davis who has been with Montgomery County Police for 15 years, was among those tasked with protecting the Capitol on Jan. 6. The chaos, violence, and destruction of the day has stuck with him and continues to occupy his thoughts.
“I had a front-row seat to the whole thing. It was overwhelming, and I’ve never seen people this angry,” said Mr. Kettering. “There were people up on the veranda and on the scaffolding set up for the inauguration. They were smashing windows and throwing things into the crowd. It was insane. There were decent people coming up to us and saying they would pray for us, then others calling us traitors, telling us to stand down and join them.”
In the aftermath of the Capitol siege, Mr. Kettering watched in dismay as the narrative of the day’s events began to warp.
“At first there was a consensus that what happened was so wrong, and then the politics took over. People were saying it wasn’t as bad as the media said, that it really wasn’t that violent and those speaking out are traitors or political operatives. I relive it every day, and it’s hard to escape, even in casual conversation.”
He added that the days’ events were compounded by the already heightened tensions surrounding the national debate around policing.
“It’s been 18 months of stress, of anti-police movements, and there is a fine line between addressing police brutality and being anti-police,” Mr. Kettering said, noting that the aforementioned issues have all contributed to the ongoing struggles his fellow officers are experiencing.
“It’s not a thing for cops to talk about how an event affected them,” he said. “A lot of officers have just shut down. People have careers and pensions to protect, and every time we stop a motorist, something could go wrong, even if we do everything right. There are mixed signals: They tell us, ‘Defend but don’t defend.’”
His colleague, Mr. Davis, said that officers “need more support from politicians,” noting that he felt particularly insulted by a comment made by a Montgomery County public official who accused the officers present at the Capitol of racism. “And finally, we feel a little betrayed by the public.”
More questions than answers from the Capitol’s day of chaos
What about the events of Jan. 6 led to the suicides of four law enforcement officers and what can be done to prevent more deaths in the future? There are the individual factors of each man’s personal history, circumstances, and vulnerabilities, including the sense of being personally endangered, witnessing trauma, and direct injury – one officer who died of suicide had sustained a head injury that day.
We don’t know if the officers went into the event with preexisting mental illness or addiction or if the day’s events precipitated psychiatric episodes. And with all the partisan anger surrounding the presidential election, we don’t know if each officer’s political beliefs amplified his distress over what occurred in a social media climate where police are being faulted by all sides.
When multiple suicides occur in a community, there is always concern about a “copycat” phenomena. These concerns are made more difficult to address, however, given the police culture of taboo and stigma associated with getting professional help, difficulty accessing care, and career repercussions for speaking openly about suicidal thoughts and mental health issues.
Finally, there is the current political agenda that leaves officers feeling unsupported, fearful of negative outcomes, and unappreciated. The Capitol siege in particular embodied a great deal of national distress and confusion over basic issues of truth, justice, and perceptions of reality in our polarized society.
Can we move to a place where those who enforce laws have easy access to treatment, free from stigma? Can we encourage a culture that does not tolerate brutality or racism, while also refusing to label all police as bad and lending support to their mission? Can we be more attuned to the repercussions of circumstances where officers are witnesses to trauma, are endangered themselves, and would benefit from acknowledgment of their distress?
Time will tell if our anti-police pendulum swings back. In the meantime, these four suicides among people defending our country remain tragically overlooked.
Dinah Miller, MD, is coauthor of Committed: The Battle Over Involuntary Psychiatric Care (Johns Hopkins University Press, 2016). She has a private practice in Baltimore and is an assistant professor of psychiatry and behavioral sciences at Johns Hopkins University. A version of this article first appeared on Medscape.com.
The other epidemic: Violence against health care workers
After working two busy evening hospital shifts, I was eating breakfast with my children when I started reading about physicians confronted and verbally abused during school board meetings for advocating for face masks in school. The pandemic changed course with the Delta variant increasing hospitalizations, and it seems to me the public response to physicians and health care workers also changed.
During the first wave of the pandemic, public support accompanied health care workers’ sacrifices. Nightly applause rang through New York City, there were donations of food, and murals reflected public backing.
We as a nation rallied. We masked up and locked down. We produced vaccines. COVID cases decreased, and by spring, a hint of normalcy bloomed.
Then the virus changed, and the Delta variant spread. Pandemic fatigue set in. Health care workers asked for help with continued masking and increased vaccinations and instead were met with threats. The summer, already made difficult, makes the prospect of winter even more daunting.
This kind of abuse is persistent
Violence against health care workers is not a new dilemma. Stories abound of patients or family members physically attacking, verbally abusing, or harassing health care workers. A 2014 survey reported almost 80% of nurses attacked during their career. Data from the Bureau of Labor Statistics also reveals health care workers experience more nonfatal workplace violence, as compared with other professions.
Nurses, who often spend the most face-to-face time with patients, receive a litany of abuse. A 2019 nursing survey reported 59% of respondents experiencing verbal abuse from patients and more than 43% experiencing verbal abuse from patients’ families. Even more concerning is 23% of survey respondents reporting physical abuse, an increase from 20% in 2018.
Physicians, likewise, are not immune from the same maltreatment. A 2014 physician survey reported more than 71% of physicians in the United States have experienced at least one incident of workplace violence in their careers. Of the physician specialties, the highest rates of violence are in the emergency department and against less experienced physicians. This is likely caused by the higher rates of patient frustration in EDs as a result of long wait times, overcrowding, and boarding while awaiting an inpatient room.
These statistics are disheartening. However, what I find most discouraging is the almost submissive acceptance of this abuse in the health care field as almost 73% of health care workers feel that the abuse is part of the job.
COVID and the increase in violence against health care workers
As the Delta variant spreads, hospitals’ capacity to handle both COVID and non-COVID issues is further strained. Compounding this stress is the public’s pandemic fatigue and the ongoing battles with masking and vaccinations.
In San Antonio, health care workers faced verbal and physical abuse as they enforced masking and visitation restrictions for COVID patients. Online, health care workers, who advocate for masking or vaccination, are often subject to death threats, threats to family members, and verbal abuse on social media. Veiled threats of “we know who you are” and “we will find you” follow physicians who advocate for masking in schools.
This problem is not isolated to the United States. In Italy, a COVID patient spat at health care workers who asked them to wait, resulting in closure of an entire hospital ward. In the United Kingdom, health care workers were subject to the same abuse as those in San Antonio when trying to enforce masking in the hospital. In India, Pakistan, and Spain, a stigma exists against health care workers for being sources of contagion.
The presence of a growing divide between health care workers and those we serve threatens to undermine not only delivery of care but also our response to the pandemic. This is in addition to the mental health burden and compassion fatigue suffered by many health care workers who find their efforts in doubt. An already strained medical system will find it difficult to withstand the loss of its essential workforce.
Standing united against health care worker abuse
Despite the level of discord surrounding COVID-19, it is important that health care workers remain united. An effective response to the increase in violence toward health care workers will greatly depend on how we address the following.
First, we must actively work to combat the spread of misinformation that erodes the public trust in science and medicine. Transparency is paramount. Policy changes and plans for implementation should be open and free of political influence. This remains a challenge due to the CDC’s standing as both a federal and scientific institution. A steadfast and explicit presentation of scientific evidence by the CDC is a vital first step in repairing this trust.
In addition, we must become our own advocates. The passage of HR 1195, the Workplace Violence Prevention for Health Care and Social Service Workers Act, in the House of Representatives with bipartisan support is an indication that the time is ripe for sweeping change. Its supporters include the American Nurses Association, American Psychiatric Nurses Association, National Nurses United, and the American College of Emergency Physicians. Active opposition includes the American Hospital Association, which cites prohibitive cost as a source of objection.
HR 1195 now waits in the U.S. Senate for approval. We should alert local, state, and health system leadership to the violence against health care workers. We should demand increased protection for our most vulnerable colleagues in EDs and hospitals. Our advocacy will produce a paradigm shift away from the acceptance of this abuse.
Lastly, we must be mindful of compassion fatigue and health care worker burnout. Cynicism threatens to take away our greatest strengths of empathy and humanity. In our work environment, we must lift each other up and increase our awareness of when our colleagues need help. Self-care and creative outlets are encouraged. Admittedly, I am blogging as a personal safeguard against compassion fatigue and burnout.
The pandemic will have enduring implications both positive and negative. It is my hope that support for health care workers not only endures but is also enhanced long after the pandemic ends.
Giancarlo Toledanes, DO, is an assistant professor of pediatrics and a pediatric hospitalist at Texas Children’s Hospital and Baylor College of Medicine, both in Houston. He has no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
After working two busy evening hospital shifts, I was eating breakfast with my children when I started reading about physicians confronted and verbally abused during school board meetings for advocating for face masks in school. The pandemic changed course with the Delta variant increasing hospitalizations, and it seems to me the public response to physicians and health care workers also changed.
During the first wave of the pandemic, public support accompanied health care workers’ sacrifices. Nightly applause rang through New York City, there were donations of food, and murals reflected public backing.
We as a nation rallied. We masked up and locked down. We produced vaccines. COVID cases decreased, and by spring, a hint of normalcy bloomed.
Then the virus changed, and the Delta variant spread. Pandemic fatigue set in. Health care workers asked for help with continued masking and increased vaccinations and instead were met with threats. The summer, already made difficult, makes the prospect of winter even more daunting.
This kind of abuse is persistent
Violence against health care workers is not a new dilemma. Stories abound of patients or family members physically attacking, verbally abusing, or harassing health care workers. A 2014 survey reported almost 80% of nurses attacked during their career. Data from the Bureau of Labor Statistics also reveals health care workers experience more nonfatal workplace violence, as compared with other professions.
Nurses, who often spend the most face-to-face time with patients, receive a litany of abuse. A 2019 nursing survey reported 59% of respondents experiencing verbal abuse from patients and more than 43% experiencing verbal abuse from patients’ families. Even more concerning is 23% of survey respondents reporting physical abuse, an increase from 20% in 2018.
Physicians, likewise, are not immune from the same maltreatment. A 2014 physician survey reported more than 71% of physicians in the United States have experienced at least one incident of workplace violence in their careers. Of the physician specialties, the highest rates of violence are in the emergency department and against less experienced physicians. This is likely caused by the higher rates of patient frustration in EDs as a result of long wait times, overcrowding, and boarding while awaiting an inpatient room.
These statistics are disheartening. However, what I find most discouraging is the almost submissive acceptance of this abuse in the health care field as almost 73% of health care workers feel that the abuse is part of the job.
COVID and the increase in violence against health care workers
As the Delta variant spreads, hospitals’ capacity to handle both COVID and non-COVID issues is further strained. Compounding this stress is the public’s pandemic fatigue and the ongoing battles with masking and vaccinations.
In San Antonio, health care workers faced verbal and physical abuse as they enforced masking and visitation restrictions for COVID patients. Online, health care workers, who advocate for masking or vaccination, are often subject to death threats, threats to family members, and verbal abuse on social media. Veiled threats of “we know who you are” and “we will find you” follow physicians who advocate for masking in schools.
This problem is not isolated to the United States. In Italy, a COVID patient spat at health care workers who asked them to wait, resulting in closure of an entire hospital ward. In the United Kingdom, health care workers were subject to the same abuse as those in San Antonio when trying to enforce masking in the hospital. In India, Pakistan, and Spain, a stigma exists against health care workers for being sources of contagion.
The presence of a growing divide between health care workers and those we serve threatens to undermine not only delivery of care but also our response to the pandemic. This is in addition to the mental health burden and compassion fatigue suffered by many health care workers who find their efforts in doubt. An already strained medical system will find it difficult to withstand the loss of its essential workforce.
Standing united against health care worker abuse
Despite the level of discord surrounding COVID-19, it is important that health care workers remain united. An effective response to the increase in violence toward health care workers will greatly depend on how we address the following.
First, we must actively work to combat the spread of misinformation that erodes the public trust in science and medicine. Transparency is paramount. Policy changes and plans for implementation should be open and free of political influence. This remains a challenge due to the CDC’s standing as both a federal and scientific institution. A steadfast and explicit presentation of scientific evidence by the CDC is a vital first step in repairing this trust.
In addition, we must become our own advocates. The passage of HR 1195, the Workplace Violence Prevention for Health Care and Social Service Workers Act, in the House of Representatives with bipartisan support is an indication that the time is ripe for sweeping change. Its supporters include the American Nurses Association, American Psychiatric Nurses Association, National Nurses United, and the American College of Emergency Physicians. Active opposition includes the American Hospital Association, which cites prohibitive cost as a source of objection.
HR 1195 now waits in the U.S. Senate for approval. We should alert local, state, and health system leadership to the violence against health care workers. We should demand increased protection for our most vulnerable colleagues in EDs and hospitals. Our advocacy will produce a paradigm shift away from the acceptance of this abuse.
Lastly, we must be mindful of compassion fatigue and health care worker burnout. Cynicism threatens to take away our greatest strengths of empathy and humanity. In our work environment, we must lift each other up and increase our awareness of when our colleagues need help. Self-care and creative outlets are encouraged. Admittedly, I am blogging as a personal safeguard against compassion fatigue and burnout.
The pandemic will have enduring implications both positive and negative. It is my hope that support for health care workers not only endures but is also enhanced long after the pandemic ends.
Giancarlo Toledanes, DO, is an assistant professor of pediatrics and a pediatric hospitalist at Texas Children’s Hospital and Baylor College of Medicine, both in Houston. He has no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
After working two busy evening hospital shifts, I was eating breakfast with my children when I started reading about physicians confronted and verbally abused during school board meetings for advocating for face masks in school. The pandemic changed course with the Delta variant increasing hospitalizations, and it seems to me the public response to physicians and health care workers also changed.
During the first wave of the pandemic, public support accompanied health care workers’ sacrifices. Nightly applause rang through New York City, there were donations of food, and murals reflected public backing.
We as a nation rallied. We masked up and locked down. We produced vaccines. COVID cases decreased, and by spring, a hint of normalcy bloomed.
Then the virus changed, and the Delta variant spread. Pandemic fatigue set in. Health care workers asked for help with continued masking and increased vaccinations and instead were met with threats. The summer, already made difficult, makes the prospect of winter even more daunting.
This kind of abuse is persistent
Violence against health care workers is not a new dilemma. Stories abound of patients or family members physically attacking, verbally abusing, or harassing health care workers. A 2014 survey reported almost 80% of nurses attacked during their career. Data from the Bureau of Labor Statistics also reveals health care workers experience more nonfatal workplace violence, as compared with other professions.
Nurses, who often spend the most face-to-face time with patients, receive a litany of abuse. A 2019 nursing survey reported 59% of respondents experiencing verbal abuse from patients and more than 43% experiencing verbal abuse from patients’ families. Even more concerning is 23% of survey respondents reporting physical abuse, an increase from 20% in 2018.
Physicians, likewise, are not immune from the same maltreatment. A 2014 physician survey reported more than 71% of physicians in the United States have experienced at least one incident of workplace violence in their careers. Of the physician specialties, the highest rates of violence are in the emergency department and against less experienced physicians. This is likely caused by the higher rates of patient frustration in EDs as a result of long wait times, overcrowding, and boarding while awaiting an inpatient room.
These statistics are disheartening. However, what I find most discouraging is the almost submissive acceptance of this abuse in the health care field as almost 73% of health care workers feel that the abuse is part of the job.
COVID and the increase in violence against health care workers
As the Delta variant spreads, hospitals’ capacity to handle both COVID and non-COVID issues is further strained. Compounding this stress is the public’s pandemic fatigue and the ongoing battles with masking and vaccinations.
In San Antonio, health care workers faced verbal and physical abuse as they enforced masking and visitation restrictions for COVID patients. Online, health care workers, who advocate for masking or vaccination, are often subject to death threats, threats to family members, and verbal abuse on social media. Veiled threats of “we know who you are” and “we will find you” follow physicians who advocate for masking in schools.
This problem is not isolated to the United States. In Italy, a COVID patient spat at health care workers who asked them to wait, resulting in closure of an entire hospital ward. In the United Kingdom, health care workers were subject to the same abuse as those in San Antonio when trying to enforce masking in the hospital. In India, Pakistan, and Spain, a stigma exists against health care workers for being sources of contagion.
The presence of a growing divide between health care workers and those we serve threatens to undermine not only delivery of care but also our response to the pandemic. This is in addition to the mental health burden and compassion fatigue suffered by many health care workers who find their efforts in doubt. An already strained medical system will find it difficult to withstand the loss of its essential workforce.
Standing united against health care worker abuse
Despite the level of discord surrounding COVID-19, it is important that health care workers remain united. An effective response to the increase in violence toward health care workers will greatly depend on how we address the following.
First, we must actively work to combat the spread of misinformation that erodes the public trust in science and medicine. Transparency is paramount. Policy changes and plans for implementation should be open and free of political influence. This remains a challenge due to the CDC’s standing as both a federal and scientific institution. A steadfast and explicit presentation of scientific evidence by the CDC is a vital first step in repairing this trust.
In addition, we must become our own advocates. The passage of HR 1195, the Workplace Violence Prevention for Health Care and Social Service Workers Act, in the House of Representatives with bipartisan support is an indication that the time is ripe for sweeping change. Its supporters include the American Nurses Association, American Psychiatric Nurses Association, National Nurses United, and the American College of Emergency Physicians. Active opposition includes the American Hospital Association, which cites prohibitive cost as a source of objection.
HR 1195 now waits in the U.S. Senate for approval. We should alert local, state, and health system leadership to the violence against health care workers. We should demand increased protection for our most vulnerable colleagues in EDs and hospitals. Our advocacy will produce a paradigm shift away from the acceptance of this abuse.
Lastly, we must be mindful of compassion fatigue and health care worker burnout. Cynicism threatens to take away our greatest strengths of empathy and humanity. In our work environment, we must lift each other up and increase our awareness of when our colleagues need help. Self-care and creative outlets are encouraged. Admittedly, I am blogging as a personal safeguard against compassion fatigue and burnout.
The pandemic will have enduring implications both positive and negative. It is my hope that support for health care workers not only endures but is also enhanced long after the pandemic ends.
Giancarlo Toledanes, DO, is an assistant professor of pediatrics and a pediatric hospitalist at Texas Children’s Hospital and Baylor College of Medicine, both in Houston. He has no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
Stop blaming the unvaccinated
As politicians battle over masks and mandates, heated rhetoric has been used to describe the fourth heartbreaking surge in COVID as a “pandemic of the unvaccinated.”
While it may serve to further divide red and blue states, I disagree with the assertion that the current surge in cases is driven simply by the unvaccinated. Why? First, the premise would assume complete efficacy with our vaccinated population, which is statistically incorrect (at least 15 million of the U.S. population never completed a second round of injections), which means they were not considered “fully vaccinated.”
Alternately, we need to examine what has occurred in nations with significantly higher vaccination rates than ours (the United Kingdom and Israel) to realize that variants have overrun the dramatic success achieved in those countries as well. Israel, once considered to be the most vaccinated country in the world, is facing a brutal fourth wave of COVID that has sent the country spiraling into another heartbreaking lockdown.
The unvaccinated could hardly be blamed for what is happening in either of these highly vaccinated countries.
The concept of blame
So why use blame? It defeats the purpose of encouraging those who are hesitant or possibly misinformed or disenfranchised to move forward. It lacks compassion. It does not encompass the art and science of nursing (for example, the University of Southern Indiana), such as those that hospitals have used to frame optimal nursing care. I abhor the idea of labeling because it denies the prospect of future comprehension.
Labeling reminds me of one of the saddest cases in my career.
An unfortunate case
I was the nurse caring for a man from a motor vehicular accident where an entire family was brutally killed. My patient was alleged to be the cause, with a blood alcohol level of 0.40%+ post hydration, intubated and ventilated, with a flailed chest and multiple orthopedic injuries as well as blunt head trauma. He was secured to the bed with handcuffs, although that was unnecessary. Multiple times I was asked how I could possibly care for such an individual, by the police and even a few colleagues. But it was not my place to judge the man.
He was in pain, and he was dying. I comforted him for the 2 weeks it took his battered body to pass into the next realm. No one visited him except the police, eagerly waiting for the man to wake up to explain the tragic events that occurred. It was my job to ease what pain I could and protect him from labels. Did he deserve the labels? Who knew? I did not care. I cared about his writhing and his physical anguish.
The comparison
Blame did not help the situation then, nor does it help us move forward now. As nurses, we seek to work within a framework of understanding. As we tire of caring for thousands of COVID patients, we do not stop to ask if they “deserve” care or if they have taken precautions and lived reasonably prior to seeking assistance for disease. We would not be nurses if we did this.
Think about Gov. Greg Abbott, who has asked that Texans not be allowed to mandate masks for children returning to school. He has recently been diagnosed with COVID, despite assuring the public he is fully vaccinated. Politically, his diagnosis could be visualized as a fiasco for a purple state where he has been adamant in denying the efficacy of masks for children.
Yet, his diagnosis should not be fodder for the press. The first concern should be his health and well-being, similar for any man of his age and potential comorbidity.
Conclusion
We should be people first, human beings that remain interconnected by our need for care and survival, not conservatives, independents, or liberals, not “vaccinated or unvaccinated,” not seen as “breakthrough” infections, or the immunosuppressed possibly unable to mount a robust response to COVID.
Labels do not define the ability to effectively defeat coronavirus or variants, as highly vaccinated countries have demonstrated in recent months. We are in the midst of a global pandemic, and the battle is raging onward.
In fact, the longer this pandemic continues, the more likely it is we will need to live with this as an endemic disease, so we should stop blaming those who become ill and need support.
It could be any of us.
A version of this article first appeared on Medscape.com.
As politicians battle over masks and mandates, heated rhetoric has been used to describe the fourth heartbreaking surge in COVID as a “pandemic of the unvaccinated.”
While it may serve to further divide red and blue states, I disagree with the assertion that the current surge in cases is driven simply by the unvaccinated. Why? First, the premise would assume complete efficacy with our vaccinated population, which is statistically incorrect (at least 15 million of the U.S. population never completed a second round of injections), which means they were not considered “fully vaccinated.”
Alternately, we need to examine what has occurred in nations with significantly higher vaccination rates than ours (the United Kingdom and Israel) to realize that variants have overrun the dramatic success achieved in those countries as well. Israel, once considered to be the most vaccinated country in the world, is facing a brutal fourth wave of COVID that has sent the country spiraling into another heartbreaking lockdown.
The unvaccinated could hardly be blamed for what is happening in either of these highly vaccinated countries.
The concept of blame
So why use blame? It defeats the purpose of encouraging those who are hesitant or possibly misinformed or disenfranchised to move forward. It lacks compassion. It does not encompass the art and science of nursing (for example, the University of Southern Indiana), such as those that hospitals have used to frame optimal nursing care. I abhor the idea of labeling because it denies the prospect of future comprehension.
Labeling reminds me of one of the saddest cases in my career.
An unfortunate case
I was the nurse caring for a man from a motor vehicular accident where an entire family was brutally killed. My patient was alleged to be the cause, with a blood alcohol level of 0.40%+ post hydration, intubated and ventilated, with a flailed chest and multiple orthopedic injuries as well as blunt head trauma. He was secured to the bed with handcuffs, although that was unnecessary. Multiple times I was asked how I could possibly care for such an individual, by the police and even a few colleagues. But it was not my place to judge the man.
He was in pain, and he was dying. I comforted him for the 2 weeks it took his battered body to pass into the next realm. No one visited him except the police, eagerly waiting for the man to wake up to explain the tragic events that occurred. It was my job to ease what pain I could and protect him from labels. Did he deserve the labels? Who knew? I did not care. I cared about his writhing and his physical anguish.
The comparison
Blame did not help the situation then, nor does it help us move forward now. As nurses, we seek to work within a framework of understanding. As we tire of caring for thousands of COVID patients, we do not stop to ask if they “deserve” care or if they have taken precautions and lived reasonably prior to seeking assistance for disease. We would not be nurses if we did this.
Think about Gov. Greg Abbott, who has asked that Texans not be allowed to mandate masks for children returning to school. He has recently been diagnosed with COVID, despite assuring the public he is fully vaccinated. Politically, his diagnosis could be visualized as a fiasco for a purple state where he has been adamant in denying the efficacy of masks for children.
Yet, his diagnosis should not be fodder for the press. The first concern should be his health and well-being, similar for any man of his age and potential comorbidity.
Conclusion
We should be people first, human beings that remain interconnected by our need for care and survival, not conservatives, independents, or liberals, not “vaccinated or unvaccinated,” not seen as “breakthrough” infections, or the immunosuppressed possibly unable to mount a robust response to COVID.
Labels do not define the ability to effectively defeat coronavirus or variants, as highly vaccinated countries have demonstrated in recent months. We are in the midst of a global pandemic, and the battle is raging onward.
In fact, the longer this pandemic continues, the more likely it is we will need to live with this as an endemic disease, so we should stop blaming those who become ill and need support.
It could be any of us.
A version of this article first appeared on Medscape.com.
As politicians battle over masks and mandates, heated rhetoric has been used to describe the fourth heartbreaking surge in COVID as a “pandemic of the unvaccinated.”
While it may serve to further divide red and blue states, I disagree with the assertion that the current surge in cases is driven simply by the unvaccinated. Why? First, the premise would assume complete efficacy with our vaccinated population, which is statistically incorrect (at least 15 million of the U.S. population never completed a second round of injections), which means they were not considered “fully vaccinated.”
Alternately, we need to examine what has occurred in nations with significantly higher vaccination rates than ours (the United Kingdom and Israel) to realize that variants have overrun the dramatic success achieved in those countries as well. Israel, once considered to be the most vaccinated country in the world, is facing a brutal fourth wave of COVID that has sent the country spiraling into another heartbreaking lockdown.
The unvaccinated could hardly be blamed for what is happening in either of these highly vaccinated countries.
The concept of blame
So why use blame? It defeats the purpose of encouraging those who are hesitant or possibly misinformed or disenfranchised to move forward. It lacks compassion. It does not encompass the art and science of nursing (for example, the University of Southern Indiana), such as those that hospitals have used to frame optimal nursing care. I abhor the idea of labeling because it denies the prospect of future comprehension.
Labeling reminds me of one of the saddest cases in my career.
An unfortunate case
I was the nurse caring for a man from a motor vehicular accident where an entire family was brutally killed. My patient was alleged to be the cause, with a blood alcohol level of 0.40%+ post hydration, intubated and ventilated, with a flailed chest and multiple orthopedic injuries as well as blunt head trauma. He was secured to the bed with handcuffs, although that was unnecessary. Multiple times I was asked how I could possibly care for such an individual, by the police and even a few colleagues. But it was not my place to judge the man.
He was in pain, and he was dying. I comforted him for the 2 weeks it took his battered body to pass into the next realm. No one visited him except the police, eagerly waiting for the man to wake up to explain the tragic events that occurred. It was my job to ease what pain I could and protect him from labels. Did he deserve the labels? Who knew? I did not care. I cared about his writhing and his physical anguish.
The comparison
Blame did not help the situation then, nor does it help us move forward now. As nurses, we seek to work within a framework of understanding. As we tire of caring for thousands of COVID patients, we do not stop to ask if they “deserve” care or if they have taken precautions and lived reasonably prior to seeking assistance for disease. We would not be nurses if we did this.
Think about Gov. Greg Abbott, who has asked that Texans not be allowed to mandate masks for children returning to school. He has recently been diagnosed with COVID, despite assuring the public he is fully vaccinated. Politically, his diagnosis could be visualized as a fiasco for a purple state where he has been adamant in denying the efficacy of masks for children.
Yet, his diagnosis should not be fodder for the press. The first concern should be his health and well-being, similar for any man of his age and potential comorbidity.
Conclusion
We should be people first, human beings that remain interconnected by our need for care and survival, not conservatives, independents, or liberals, not “vaccinated or unvaccinated,” not seen as “breakthrough” infections, or the immunosuppressed possibly unable to mount a robust response to COVID.
Labels do not define the ability to effectively defeat coronavirus or variants, as highly vaccinated countries have demonstrated in recent months. We are in the midst of a global pandemic, and the battle is raging onward.
In fact, the longer this pandemic continues, the more likely it is we will need to live with this as an endemic disease, so we should stop blaming those who become ill and need support.
It could be any of us.
A version of this article first appeared on Medscape.com.
Gender-affirming mastectomy and breast cancer screening in transmasculine patients
Since the reversal of the Medicare exclusion in 2014, the rates of gender-affirming surgery have increased markedly in the United States.1 Gender-affirming mastectomy, otherwise known as “top surgery,” is one of the more commonly performed procedures; with 97% of patients having either undergone or expressed desire for the surgery.2 The goals of this procedure are to remove all visible breast tissue and reconstruct the chest wall so it is more masculine in appearance. For transmasculine and nonbinary patients, this procedure is associated with significant improvements in mental health and quality of life.3,4 While the mastectomy procedure is often performed by plastic surgeons, patients will see an ob.gyn. in the preoperative or postoperative period. Ob.gyns. should have a general understanding of the procedure, but most importantly know how to screen for breast cancer in patients who have undergone a gender-affirming mastectomy.
Providers will likely encounter transmasculine or nonbinary patients during annual screening examinations or for a preoperative exam. If a patient is seeking a preoperative risk assessment prior to undergoing a gender-affirming mastectomy, assessing a patient’s risk status for breast cancer is paramount. While testosterone therapy is no longer a prerequisite for gender-affirming mastectomies, documenting hormone use, age at initiation, and dosage is important.5 The overall effects of testosterone on breast tissue are inconsistent. However, studies have demonstrated that patients taking testosterone are not at an increased risk of breast cancer secondary to testosterone use.5-7 Patients should be asked about a personal of family history of breast cancer, breast surgery, history of prior breast biopsies, parity, age at menarche, smoking status, and breastfeeding history if applicable. Patients with high-risk mutations or a strong family history of breast cancer should be referred to genetic counselors, surgical oncologists, and possibly undergo genetic testing.8 Before an examination, providers should counsel patients about the nature of the examination and use gender-neutral language such as “chest” to avoid exacerbating gender dysphoria.
It is important to educate transmasculine patients about their risk for the development of breast cancer after mastectomy. Larger-scale, population-based studies of breast cancer in the transgender population have reported an incidence of 5.9 per 100,000 patients-years and an overall incidence comparable to cisgender men in age-standardized national samples.5-7 Unfortunately, data on the rates of breast cancer in transmasculine patients after gender-affirming mastectomy are limited, which makes defining postoperative guidelines challenging. Additionally, the amount of residual breast tissue remaining varies based on the surgeon and technique.
Several techniques are described for mastectomy procedures with differences that can affect the amount of residual breast tissue. The most common type of gender-affirming mastectomy is the double incision. With this procedure, the nipple-areolar complex is reduced in size, removed, and thinned to improve graft take. Dissection is then carried to the level of the breast capsule and the breast tissue and axillary tail are removed en bloc.5 During the dissection, the subcutaneous fat is left on the skin flap to provide appropriate contour and to avoid creating a concave-appearing chest wall. Prior to closure, the superior and inferior flaps are inspected for any visible residual breast tissue, which is removed if needed. In a circumareolar mastectomy, the nipple-areolar complex is also reduced but is preserved on a 1- to 1.5-cm-thick pedicle to maintain perfusion.5 The mastectomy is performed through an inferior periareolar incision and all visible breast tissue and the axillary tail are removed. Breast tissue specimens are sent for pathologic evaluation at the end of the procedure.
Following gender-affirming mastectomy, there is limited evidence to guide screening. During the patient visit, the provider should obtain a thorough history regarding mastectomy type, and if unknown, attempt to acquire the operative report detailing the procedure. For low-risk patients who undergo a subcutaneous mastectomy such as the double incision or circumareolar technique, screening mammography is not indicated nor is it technically feasible.9 For patients with a high-risk genetic mutation or a strong family history of breast cancer, monitoring with alternative modalities such as breast ultrasound or breast MRI may be beneficial, although there is no evidence to currently support this suggestion. Given the variety of surgical techniques of breast tissue removal, it is difficult to develop strong evidence-based guidelines. Annual chest wall examinations have been suggested as a screening modality; however, the clinical utility of clinical breast and chest exams has been debated and is no longer recommended as a screening method in cisgender patients.9 Clinicians can promote chest self-awareness and discuss the possibility of breast cancer in postmastectomy patients at annual examination visits. As research continues to resolve some of these unknowns, it is important that patients are informed of these areas of ambiguity and updated regarding any changes in screening recommendations.10
Dr. Brandt is an ob.gyn. and fellowship-trained gender affirming surgeon in West Reading, Pa.
References
1. American Society of Plastic Surgeons. 2018 plastic surgery statistics report. https://www.plasticsurgery.org/documents/News/Statistics/2018/plastic-surgery-statistics-full-report-2018.pdf. Accessed Aug. 20, 2021.
2. James SE et al. The report of the 2015 U.S. Transgender survey. Washington, D.C.: National Center for Transgender Equality, 2016.
3. Agarwal CA et al. J Plast Reconstr Aesthet Surg. 2018;71:651-7.
4. Poudrier G et al. Plast Reconstr Surg. 2018;80:679-83.
5. Salibian AA et al. Plast Reconstr Surg. 2020;147:213e-21e.
6. Gooren LJ et al. J Sex Med. 2013;10:3129-34.
7. Brown GR and Jones KT. Breast Cancer Res Treat. 2015;149:191-8.
8. Deutsch MF et al. Semin Reprod Med. 2017;35:434-41.
9. Phillips J et al. AJR Am J Roentgenol. 2014;202:1149-59.
10. Smith RA et al. CA Cancer J Clin. 2018;68:297-316.
Since the reversal of the Medicare exclusion in 2014, the rates of gender-affirming surgery have increased markedly in the United States.1 Gender-affirming mastectomy, otherwise known as “top surgery,” is one of the more commonly performed procedures; with 97% of patients having either undergone or expressed desire for the surgery.2 The goals of this procedure are to remove all visible breast tissue and reconstruct the chest wall so it is more masculine in appearance. For transmasculine and nonbinary patients, this procedure is associated with significant improvements in mental health and quality of life.3,4 While the mastectomy procedure is often performed by plastic surgeons, patients will see an ob.gyn. in the preoperative or postoperative period. Ob.gyns. should have a general understanding of the procedure, but most importantly know how to screen for breast cancer in patients who have undergone a gender-affirming mastectomy.
Providers will likely encounter transmasculine or nonbinary patients during annual screening examinations or for a preoperative exam. If a patient is seeking a preoperative risk assessment prior to undergoing a gender-affirming mastectomy, assessing a patient’s risk status for breast cancer is paramount. While testosterone therapy is no longer a prerequisite for gender-affirming mastectomies, documenting hormone use, age at initiation, and dosage is important.5 The overall effects of testosterone on breast tissue are inconsistent. However, studies have demonstrated that patients taking testosterone are not at an increased risk of breast cancer secondary to testosterone use.5-7 Patients should be asked about a personal of family history of breast cancer, breast surgery, history of prior breast biopsies, parity, age at menarche, smoking status, and breastfeeding history if applicable. Patients with high-risk mutations or a strong family history of breast cancer should be referred to genetic counselors, surgical oncologists, and possibly undergo genetic testing.8 Before an examination, providers should counsel patients about the nature of the examination and use gender-neutral language such as “chest” to avoid exacerbating gender dysphoria.
It is important to educate transmasculine patients about their risk for the development of breast cancer after mastectomy. Larger-scale, population-based studies of breast cancer in the transgender population have reported an incidence of 5.9 per 100,000 patients-years and an overall incidence comparable to cisgender men in age-standardized national samples.5-7 Unfortunately, data on the rates of breast cancer in transmasculine patients after gender-affirming mastectomy are limited, which makes defining postoperative guidelines challenging. Additionally, the amount of residual breast tissue remaining varies based on the surgeon and technique.
Several techniques are described for mastectomy procedures with differences that can affect the amount of residual breast tissue. The most common type of gender-affirming mastectomy is the double incision. With this procedure, the nipple-areolar complex is reduced in size, removed, and thinned to improve graft take. Dissection is then carried to the level of the breast capsule and the breast tissue and axillary tail are removed en bloc.5 During the dissection, the subcutaneous fat is left on the skin flap to provide appropriate contour and to avoid creating a concave-appearing chest wall. Prior to closure, the superior and inferior flaps are inspected for any visible residual breast tissue, which is removed if needed. In a circumareolar mastectomy, the nipple-areolar complex is also reduced but is preserved on a 1- to 1.5-cm-thick pedicle to maintain perfusion.5 The mastectomy is performed through an inferior periareolar incision and all visible breast tissue and the axillary tail are removed. Breast tissue specimens are sent for pathologic evaluation at the end of the procedure.
Following gender-affirming mastectomy, there is limited evidence to guide screening. During the patient visit, the provider should obtain a thorough history regarding mastectomy type, and if unknown, attempt to acquire the operative report detailing the procedure. For low-risk patients who undergo a subcutaneous mastectomy such as the double incision or circumareolar technique, screening mammography is not indicated nor is it technically feasible.9 For patients with a high-risk genetic mutation or a strong family history of breast cancer, monitoring with alternative modalities such as breast ultrasound or breast MRI may be beneficial, although there is no evidence to currently support this suggestion. Given the variety of surgical techniques of breast tissue removal, it is difficult to develop strong evidence-based guidelines. Annual chest wall examinations have been suggested as a screening modality; however, the clinical utility of clinical breast and chest exams has been debated and is no longer recommended as a screening method in cisgender patients.9 Clinicians can promote chest self-awareness and discuss the possibility of breast cancer in postmastectomy patients at annual examination visits. As research continues to resolve some of these unknowns, it is important that patients are informed of these areas of ambiguity and updated regarding any changes in screening recommendations.10
Dr. Brandt is an ob.gyn. and fellowship-trained gender affirming surgeon in West Reading, Pa.
References
1. American Society of Plastic Surgeons. 2018 plastic surgery statistics report. https://www.plasticsurgery.org/documents/News/Statistics/2018/plastic-surgery-statistics-full-report-2018.pdf. Accessed Aug. 20, 2021.
2. James SE et al. The report of the 2015 U.S. Transgender survey. Washington, D.C.: National Center for Transgender Equality, 2016.
3. Agarwal CA et al. J Plast Reconstr Aesthet Surg. 2018;71:651-7.
4. Poudrier G et al. Plast Reconstr Surg. 2018;80:679-83.
5. Salibian AA et al. Plast Reconstr Surg. 2020;147:213e-21e.
6. Gooren LJ et al. J Sex Med. 2013;10:3129-34.
7. Brown GR and Jones KT. Breast Cancer Res Treat. 2015;149:191-8.
8. Deutsch MF et al. Semin Reprod Med. 2017;35:434-41.
9. Phillips J et al. AJR Am J Roentgenol. 2014;202:1149-59.
10. Smith RA et al. CA Cancer J Clin. 2018;68:297-316.
Since the reversal of the Medicare exclusion in 2014, the rates of gender-affirming surgery have increased markedly in the United States.1 Gender-affirming mastectomy, otherwise known as “top surgery,” is one of the more commonly performed procedures; with 97% of patients having either undergone or expressed desire for the surgery.2 The goals of this procedure are to remove all visible breast tissue and reconstruct the chest wall so it is more masculine in appearance. For transmasculine and nonbinary patients, this procedure is associated with significant improvements in mental health and quality of life.3,4 While the mastectomy procedure is often performed by plastic surgeons, patients will see an ob.gyn. in the preoperative or postoperative period. Ob.gyns. should have a general understanding of the procedure, but most importantly know how to screen for breast cancer in patients who have undergone a gender-affirming mastectomy.
Providers will likely encounter transmasculine or nonbinary patients during annual screening examinations or for a preoperative exam. If a patient is seeking a preoperative risk assessment prior to undergoing a gender-affirming mastectomy, assessing a patient’s risk status for breast cancer is paramount. While testosterone therapy is no longer a prerequisite for gender-affirming mastectomies, documenting hormone use, age at initiation, and dosage is important.5 The overall effects of testosterone on breast tissue are inconsistent. However, studies have demonstrated that patients taking testosterone are not at an increased risk of breast cancer secondary to testosterone use.5-7 Patients should be asked about a personal of family history of breast cancer, breast surgery, history of prior breast biopsies, parity, age at menarche, smoking status, and breastfeeding history if applicable. Patients with high-risk mutations or a strong family history of breast cancer should be referred to genetic counselors, surgical oncologists, and possibly undergo genetic testing.8 Before an examination, providers should counsel patients about the nature of the examination and use gender-neutral language such as “chest” to avoid exacerbating gender dysphoria.
It is important to educate transmasculine patients about their risk for the development of breast cancer after mastectomy. Larger-scale, population-based studies of breast cancer in the transgender population have reported an incidence of 5.9 per 100,000 patients-years and an overall incidence comparable to cisgender men in age-standardized national samples.5-7 Unfortunately, data on the rates of breast cancer in transmasculine patients after gender-affirming mastectomy are limited, which makes defining postoperative guidelines challenging. Additionally, the amount of residual breast tissue remaining varies based on the surgeon and technique.
Several techniques are described for mastectomy procedures with differences that can affect the amount of residual breast tissue. The most common type of gender-affirming mastectomy is the double incision. With this procedure, the nipple-areolar complex is reduced in size, removed, and thinned to improve graft take. Dissection is then carried to the level of the breast capsule and the breast tissue and axillary tail are removed en bloc.5 During the dissection, the subcutaneous fat is left on the skin flap to provide appropriate contour and to avoid creating a concave-appearing chest wall. Prior to closure, the superior and inferior flaps are inspected for any visible residual breast tissue, which is removed if needed. In a circumareolar mastectomy, the nipple-areolar complex is also reduced but is preserved on a 1- to 1.5-cm-thick pedicle to maintain perfusion.5 The mastectomy is performed through an inferior periareolar incision and all visible breast tissue and the axillary tail are removed. Breast tissue specimens are sent for pathologic evaluation at the end of the procedure.
Following gender-affirming mastectomy, there is limited evidence to guide screening. During the patient visit, the provider should obtain a thorough history regarding mastectomy type, and if unknown, attempt to acquire the operative report detailing the procedure. For low-risk patients who undergo a subcutaneous mastectomy such as the double incision or circumareolar technique, screening mammography is not indicated nor is it technically feasible.9 For patients with a high-risk genetic mutation or a strong family history of breast cancer, monitoring with alternative modalities such as breast ultrasound or breast MRI may be beneficial, although there is no evidence to currently support this suggestion. Given the variety of surgical techniques of breast tissue removal, it is difficult to develop strong evidence-based guidelines. Annual chest wall examinations have been suggested as a screening modality; however, the clinical utility of clinical breast and chest exams has been debated and is no longer recommended as a screening method in cisgender patients.9 Clinicians can promote chest self-awareness and discuss the possibility of breast cancer in postmastectomy patients at annual examination visits. As research continues to resolve some of these unknowns, it is important that patients are informed of these areas of ambiguity and updated regarding any changes in screening recommendations.10
Dr. Brandt is an ob.gyn. and fellowship-trained gender affirming surgeon in West Reading, Pa.
References
1. American Society of Plastic Surgeons. 2018 plastic surgery statistics report. https://www.plasticsurgery.org/documents/News/Statistics/2018/plastic-surgery-statistics-full-report-2018.pdf. Accessed Aug. 20, 2021.
2. James SE et al. The report of the 2015 U.S. Transgender survey. Washington, D.C.: National Center for Transgender Equality, 2016.
3. Agarwal CA et al. J Plast Reconstr Aesthet Surg. 2018;71:651-7.
4. Poudrier G et al. Plast Reconstr Surg. 2018;80:679-83.
5. Salibian AA et al. Plast Reconstr Surg. 2020;147:213e-21e.
6. Gooren LJ et al. J Sex Med. 2013;10:3129-34.
7. Brown GR and Jones KT. Breast Cancer Res Treat. 2015;149:191-8.
8. Deutsch MF et al. Semin Reprod Med. 2017;35:434-41.
9. Phillips J et al. AJR Am J Roentgenol. 2014;202:1149-59.
10. Smith RA et al. CA Cancer J Clin. 2018;68:297-316.
Telehealth abortions are 95% effective, similar to in-person care
Telehealth abortion may be just as safe and effective as in-person care, according to a small study published online in JAMA Network Open.
Of the 110 women from whom researchers collected remote abortion outcome data, 95% had a complete abortion without additional medical interventions, such as aspiration or surgery, and none experienced adverse events. Researchers said this efficacy rate is similar to in-person visits.
“There was no reason to expect that the medications prescribed [via telemedicine] and delivered through the mail would have different outcomes from when a patient traveled to a clinic,” study author Ushma D. Upadhyay, PhD, MPH, associate professor in the department of obstetrics, gynecology, and reproductive sciences at the University of California, San Francisco, said in an interview.
Medication abortion, which usually involves taking mifepristone (Mifeprex) followed by misoprostol (Cytotec) during the first 10 weeks of pregnancy, has been available in the United States since 2000. The Food and Drug Administration’s Risk Evaluation and Mitigation Strategy requires that mifepristone be dispensed in a medical office, clinic, or hospital, prohibiting dispensing from pharmacies in an effort to reduce potential risk for complications.
In April 2021, the FDA lifted the in-person dispensing requirement for mifepristone for the duration of the COVID-19 pandemic. However, Dr. Upadhyay hopes the findings of her current study will make this suspension permanent.
For the study, Dr. Upadhyay and colleagues examined the safety and efficacy of fully remote, medication abortion care. Eligibility for the medication was assessed using an online form that relies on patient history, or patients recalling their last period, to assess pregnancy duration and screen for ectopic pregnancy risks. Nurse practitioners reviewed the form and referred patients with unknown last menstrual period date or ectopic pregnancy risk factors for ultrasonography. A mail-order pharmacy delivered medications to eligible patients. The protocol involved three follow-up contacts: confirmation of medication administration, a 3-day assessment of symptoms, and a home pregnancy test after 4 weeks. Follow-up interactions were conducted by text, secure messaging, or telephone.
Researchers found that in addition to the 95% of the patients having a complete abortion without intervention, 5% (five) of patients required addition medical care to complete the abortion. Two of those patients were treated in EDs.
Gillian Burkhardt, MD, who was not involved in the study, said Dr. Upadhyay’s study proves what has been known all along, that medication is super safe and that women “can help to determine their own eligibility as well as in conjunction with the provider.”
“I hope that this will be one more study that the FDA can use when thinking about changing the risk evaluation administration strategy so that it’s removing the requirement that a person be in the dispensing medical office,” Dr. Burkhardt, assistant professor of family planning in the department of obstetrics & gynecology at the University of New Mexico Hospital, Albuquerque, said in an interview. “I hope it also makes providers feel more comfortable as well, because I think there’s some hesitancy among providers to provide abortion without doing an ultrasound or without seeing the patient typically in front of them.”
This isn’t the first study to suggest the safety of telemedicine abortion. A 2019 study published in Obstetrics & Gynecology, which analyzed records from nearly 6,000 patients receiving medication abortion either through telemedicine or in person at 26 Planned Parenthood health centers in four states found that ongoing pregnancy and aspiration procedures were less common among telemedicine patients. Another 2017 study published in BMJ found that women who used an online consultation service and self-sourced medical abortion during a 3-year period were able to successfully end their pregnancies with few adverse events.
Dr. Upadhyay said one limitation of the current study is its sample size, so more studies should be conducted to prove telemedicine abortion’s safety.
“I think that we need continued research on this model of care just so we have more multiple studies that contribute to the evidence that can convince providers as well that they don’t need a lot of tests and that they can mail,” Dr. Upadhyay said.
Neither Dr. Upadhyay nor Dr. Burkhardt reported conflicts of interests.
Telehealth abortion may be just as safe and effective as in-person care, according to a small study published online in JAMA Network Open.
Of the 110 women from whom researchers collected remote abortion outcome data, 95% had a complete abortion without additional medical interventions, such as aspiration or surgery, and none experienced adverse events. Researchers said this efficacy rate is similar to in-person visits.
“There was no reason to expect that the medications prescribed [via telemedicine] and delivered through the mail would have different outcomes from when a patient traveled to a clinic,” study author Ushma D. Upadhyay, PhD, MPH, associate professor in the department of obstetrics, gynecology, and reproductive sciences at the University of California, San Francisco, said in an interview.
Medication abortion, which usually involves taking mifepristone (Mifeprex) followed by misoprostol (Cytotec) during the first 10 weeks of pregnancy, has been available in the United States since 2000. The Food and Drug Administration’s Risk Evaluation and Mitigation Strategy requires that mifepristone be dispensed in a medical office, clinic, or hospital, prohibiting dispensing from pharmacies in an effort to reduce potential risk for complications.
In April 2021, the FDA lifted the in-person dispensing requirement for mifepristone for the duration of the COVID-19 pandemic. However, Dr. Upadhyay hopes the findings of her current study will make this suspension permanent.
For the study, Dr. Upadhyay and colleagues examined the safety and efficacy of fully remote, medication abortion care. Eligibility for the medication was assessed using an online form that relies on patient history, or patients recalling their last period, to assess pregnancy duration and screen for ectopic pregnancy risks. Nurse practitioners reviewed the form and referred patients with unknown last menstrual period date or ectopic pregnancy risk factors for ultrasonography. A mail-order pharmacy delivered medications to eligible patients. The protocol involved three follow-up contacts: confirmation of medication administration, a 3-day assessment of symptoms, and a home pregnancy test after 4 weeks. Follow-up interactions were conducted by text, secure messaging, or telephone.
Researchers found that in addition to the 95% of the patients having a complete abortion without intervention, 5% (five) of patients required addition medical care to complete the abortion. Two of those patients were treated in EDs.
Gillian Burkhardt, MD, who was not involved in the study, said Dr. Upadhyay’s study proves what has been known all along, that medication is super safe and that women “can help to determine their own eligibility as well as in conjunction with the provider.”
“I hope that this will be one more study that the FDA can use when thinking about changing the risk evaluation administration strategy so that it’s removing the requirement that a person be in the dispensing medical office,” Dr. Burkhardt, assistant professor of family planning in the department of obstetrics & gynecology at the University of New Mexico Hospital, Albuquerque, said in an interview. “I hope it also makes providers feel more comfortable as well, because I think there’s some hesitancy among providers to provide abortion without doing an ultrasound or without seeing the patient typically in front of them.”
This isn’t the first study to suggest the safety of telemedicine abortion. A 2019 study published in Obstetrics & Gynecology, which analyzed records from nearly 6,000 patients receiving medication abortion either through telemedicine or in person at 26 Planned Parenthood health centers in four states found that ongoing pregnancy and aspiration procedures were less common among telemedicine patients. Another 2017 study published in BMJ found that women who used an online consultation service and self-sourced medical abortion during a 3-year period were able to successfully end their pregnancies with few adverse events.
Dr. Upadhyay said one limitation of the current study is its sample size, so more studies should be conducted to prove telemedicine abortion’s safety.
“I think that we need continued research on this model of care just so we have more multiple studies that contribute to the evidence that can convince providers as well that they don’t need a lot of tests and that they can mail,” Dr. Upadhyay said.
Neither Dr. Upadhyay nor Dr. Burkhardt reported conflicts of interests.
Telehealth abortion may be just as safe and effective as in-person care, according to a small study published online in JAMA Network Open.
Of the 110 women from whom researchers collected remote abortion outcome data, 95% had a complete abortion without additional medical interventions, such as aspiration or surgery, and none experienced adverse events. Researchers said this efficacy rate is similar to in-person visits.
“There was no reason to expect that the medications prescribed [via telemedicine] and delivered through the mail would have different outcomes from when a patient traveled to a clinic,” study author Ushma D. Upadhyay, PhD, MPH, associate professor in the department of obstetrics, gynecology, and reproductive sciences at the University of California, San Francisco, said in an interview.
Medication abortion, which usually involves taking mifepristone (Mifeprex) followed by misoprostol (Cytotec) during the first 10 weeks of pregnancy, has been available in the United States since 2000. The Food and Drug Administration’s Risk Evaluation and Mitigation Strategy requires that mifepristone be dispensed in a medical office, clinic, or hospital, prohibiting dispensing from pharmacies in an effort to reduce potential risk for complications.
In April 2021, the FDA lifted the in-person dispensing requirement for mifepristone for the duration of the COVID-19 pandemic. However, Dr. Upadhyay hopes the findings of her current study will make this suspension permanent.
For the study, Dr. Upadhyay and colleagues examined the safety and efficacy of fully remote, medication abortion care. Eligibility for the medication was assessed using an online form that relies on patient history, or patients recalling their last period, to assess pregnancy duration and screen for ectopic pregnancy risks. Nurse practitioners reviewed the form and referred patients with unknown last menstrual period date or ectopic pregnancy risk factors for ultrasonography. A mail-order pharmacy delivered medications to eligible patients. The protocol involved three follow-up contacts: confirmation of medication administration, a 3-day assessment of symptoms, and a home pregnancy test after 4 weeks. Follow-up interactions were conducted by text, secure messaging, or telephone.
Researchers found that in addition to the 95% of the patients having a complete abortion without intervention, 5% (five) of patients required addition medical care to complete the abortion. Two of those patients were treated in EDs.
Gillian Burkhardt, MD, who was not involved in the study, said Dr. Upadhyay’s study proves what has been known all along, that medication is super safe and that women “can help to determine their own eligibility as well as in conjunction with the provider.”
“I hope that this will be one more study that the FDA can use when thinking about changing the risk evaluation administration strategy so that it’s removing the requirement that a person be in the dispensing medical office,” Dr. Burkhardt, assistant professor of family planning in the department of obstetrics & gynecology at the University of New Mexico Hospital, Albuquerque, said in an interview. “I hope it also makes providers feel more comfortable as well, because I think there’s some hesitancy among providers to provide abortion without doing an ultrasound or without seeing the patient typically in front of them.”
This isn’t the first study to suggest the safety of telemedicine abortion. A 2019 study published in Obstetrics & Gynecology, which analyzed records from nearly 6,000 patients receiving medication abortion either through telemedicine or in person at 26 Planned Parenthood health centers in four states found that ongoing pregnancy and aspiration procedures were less common among telemedicine patients. Another 2017 study published in BMJ found that women who used an online consultation service and self-sourced medical abortion during a 3-year period were able to successfully end their pregnancies with few adverse events.
Dr. Upadhyay said one limitation of the current study is its sample size, so more studies should be conducted to prove telemedicine abortion’s safety.
“I think that we need continued research on this model of care just so we have more multiple studies that contribute to the evidence that can convince providers as well that they don’t need a lot of tests and that they can mail,” Dr. Upadhyay said.
Neither Dr. Upadhyay nor Dr. Burkhardt reported conflicts of interests.
FROM JAMA NETWORK OPEN
Recommendations from a gynecologic oncologist to a general ob.gyn., part 2
In this month’s column we continue to discuss recommendations from the gynecologic oncologist to the general gynecologist.
Don’t screen average-risk women for ovarian cancer.
Ovarian cancer is most often diagnosed at an advanced stage, which limits the curability of the disease. Consequently, there is a strong focus on attempting to diagnose the disease at earlier, more curable stages. This leads to the impulse by some well-intentioned providers to implement screening tests, such as ultrasounds and tumor markers, for all women. Unfortunately, the screening of “average risk” women for ovarian cancer is not recommended. Randomized controlled trials of tens of thousands of women have not observed a clinically significant decrease in ovarian cancer mortality with the addition of screening with tumor markers and ultrasound.1 These studies did observe a false-positive rate of 5%. While that may seem like a low rate of false-positive testing, the definitive diagnostic test which follows is a major abdominal surgery (oophorectomy) and serious complications are encountered in 15% of patients undergoing surgery for false-positive ovarian cancer screening.1 Therefore, quite simply, the harms are not balanced by benefits.
The key to offering patients appropriate and effective screening is case selection. It is important to identify which patients are at higher risk for ovarian cancer and offer those women testing for germline mutations and screening strategies. An important component of a well-woman visit is to take a thorough family history of cancer. Women are considered at high risk for having hereditary predisposition to ovarian cancer if they have a first- or second-degree relative with breast cancer younger than 45-50 years, or any age if Ashkenazi Jewish, triple-negative breast cancer younger than 60 years of age, two or more primary breast cancers with the first diagnosed at less than 50 years of age, male breast cancer, ovarian cancer, pancreatic cancer, a known BRCA 1/2 mutation, or a personal history of those same conditions. These women should be recommended to undergo genetic testing for BRCA 1, 2, and Lynch syndrome. They should not automatically be offered ovarian cancer screening. If a patient has a more remote family history for ovarian cancer, their personal risk may be somewhat elevated above the baseline population risk, however, not substantially enough to justify implementing screening in the absence of a confirmed genetic mutation.
While screening tests may not be appropriate for all patients, all patients should be asked about the early symptoms of ovarian cancer because these are consistently present, and frequently overlooked, prior to the eventual diagnosis of advanced disease. Those symptoms include abdominal discomfort, abdominal swelling and bloating, and urinary urgency.2 Consider offering all patients a dedicated ovarian cancer specific review of systems that includes inquiries about these symptoms at their annual wellness visits.
Opt for vertical midline incisions when surgery is anticipated to be complex
What is the first thing gynecologic oncologists do when called in to assist in a difficult gynecologic procedure? Get better exposure. Exposure is the cornerstone of safe, effective surgery. Sometimes this simply means placing a more effective retractor. In other cases, it might mean extending the incision. However, if the incision is a low transverse incision (the go-to for many gynecologists because of its favorable cosmetic and pain-producing profile) this proves to be difficult. Attempting to assist in a complicated case, such as a frozen pelvis, severed ureter or rectal injury, through a pfannensteil incision can be extraordinarily difficult, and while these incisions can be extended by incising the rectus muscle bellies, upper abdominal visualization remains elusive in most patients. This is particularly problematic if the ureter or splenic flexure need to be mobilized, or if extensive lysis of adhesions is necessary to ensure there is no occult enterotomy. As my mentor Dr. John Soper once described to me: “It’s like trying to scratch your armpit by reaching through your fly.”
While pfannensteil incisions come naturally, and comfortably, to most gynecologists, likely because of their frequent application during cesarean section, all gynecologists should be confident in the steps and anatomy for vertical midline, or paramedian incisions. This is not only beneficial for complex gynecologic cases, but also in the event of vascular emergency. In the hands of an experienced abdominal/pelvic surgeon, the vertical midline incision is the quickest way to safely enter the abdomen, and provides the kind of exposure that may be critical in safely repairing or controlling hemorrhage from a major vessel.
While low transverse incisions may be more cosmetic, less painful, and associated with fewer wound complications, our first concern as surgeons should be mitigating complications. In situations where risks of complications are high, it is best to not handicap ourselves with the incision location. And always remember, wound complications are highest when a transverse incision needs to be converted to a vertical one with a “T.”
It’s not just about diagnosis of cancer, it’s also prevention
Detection of cancer is an important role of the obstetrician gynecologist. However, equally important is being able to seize opportunities for cancer prevention. Cervical, vulvar, endometrial and ovarian cancer are all known to have preventative strategies.
All patients up to the age of 45 should be offered vaccination against HPV. Initial indications for HPV vaccination were for women up to age 26; however, recent data support the safety and efficacy of the vaccine in older women.3 HPV vaccination is most effective at preventing cancer when administered prior to exposure (ideally age 9-11), leaving this in the hands of our pediatrician colleagues. However, we must be vigilant to inquire about vaccination status for all our patients and encourage vaccines for those who were missed earlier in their life.
Patients should be counseled regarding the significant risk reduction for cancer that is gained from use of oral hormonal contraceptives and progestin-releasing IUDs (especially for endometrial and ovarian cancers). Providing them with knowledge of this information when considering options for contraception or menstrual cycle management is important in their decision-making process.
Endometrial cancer incidence is sadly on the rise in the United States, likely secondary to increasing rates of obesity. Pregnancy is a time when many women begin to gain, and accumulate, weight and therefore obstetric providers have a unique opportunity to assist patients in strategies to normalize their weight after pregnancy. Many of my patients with endometrial cancer state that they have never heard that it is associated with obesity. This suggests that more can be done to educate patients on the carcinogenic effect of obesity (for both endometrial and breast cancer), which may aid in motivating change of modifiable behaviors.
The fallopian tubes are the source of many ovarian cancers and knowledge of this has led to the recommendation to perform opportunistic salpingectomy as a cancer risk-reducing strategy. Hysterectomy and sterilization procedures are most apropos for this modification. While prospective data to confirm a reduced risk of ovarian cancer with opportunistic salpingectomy are lacking, a reduced incidence of cancer has been observed when the tubes have been removed for indicated surgeries; there appear to be no significant deleterious sequelae.4,5 A focus should be made on removal of the entire distal third of the tube, particularly the fimbriated ends, as this is the portion most implicated in malignancy.
Dr. Rossi is assistant professor in the division of gynecologic oncology at the University of North Carolina at Chapel Hill. She has no relevant disclosures. Contact her at obnews@mdedge.com.
References
1. Buys SS et al. JAMA. 2011;305(22):2295.
2. Goff BA et al. JAMA. 2004;291(22):2705.
3. Castellsagué X et al. Br J Cancer. 2011;105(1):28.
4. Yoon SH et al. Eur J Cancer. 2016 Mar;55:38-46.
5. Hanley GE et al. Am J Obstet Gynecol. 2018;219(2):172.
In this month’s column we continue to discuss recommendations from the gynecologic oncologist to the general gynecologist.
Don’t screen average-risk women for ovarian cancer.
Ovarian cancer is most often diagnosed at an advanced stage, which limits the curability of the disease. Consequently, there is a strong focus on attempting to diagnose the disease at earlier, more curable stages. This leads to the impulse by some well-intentioned providers to implement screening tests, such as ultrasounds and tumor markers, for all women. Unfortunately, the screening of “average risk” women for ovarian cancer is not recommended. Randomized controlled trials of tens of thousands of women have not observed a clinically significant decrease in ovarian cancer mortality with the addition of screening with tumor markers and ultrasound.1 These studies did observe a false-positive rate of 5%. While that may seem like a low rate of false-positive testing, the definitive diagnostic test which follows is a major abdominal surgery (oophorectomy) and serious complications are encountered in 15% of patients undergoing surgery for false-positive ovarian cancer screening.1 Therefore, quite simply, the harms are not balanced by benefits.
The key to offering patients appropriate and effective screening is case selection. It is important to identify which patients are at higher risk for ovarian cancer and offer those women testing for germline mutations and screening strategies. An important component of a well-woman visit is to take a thorough family history of cancer. Women are considered at high risk for having hereditary predisposition to ovarian cancer if they have a first- or second-degree relative with breast cancer younger than 45-50 years, or any age if Ashkenazi Jewish, triple-negative breast cancer younger than 60 years of age, two or more primary breast cancers with the first diagnosed at less than 50 years of age, male breast cancer, ovarian cancer, pancreatic cancer, a known BRCA 1/2 mutation, or a personal history of those same conditions. These women should be recommended to undergo genetic testing for BRCA 1, 2, and Lynch syndrome. They should not automatically be offered ovarian cancer screening. If a patient has a more remote family history for ovarian cancer, their personal risk may be somewhat elevated above the baseline population risk, however, not substantially enough to justify implementing screening in the absence of a confirmed genetic mutation.
While screening tests may not be appropriate for all patients, all patients should be asked about the early symptoms of ovarian cancer because these are consistently present, and frequently overlooked, prior to the eventual diagnosis of advanced disease. Those symptoms include abdominal discomfort, abdominal swelling and bloating, and urinary urgency.2 Consider offering all patients a dedicated ovarian cancer specific review of systems that includes inquiries about these symptoms at their annual wellness visits.
Opt for vertical midline incisions when surgery is anticipated to be complex
What is the first thing gynecologic oncologists do when called in to assist in a difficult gynecologic procedure? Get better exposure. Exposure is the cornerstone of safe, effective surgery. Sometimes this simply means placing a more effective retractor. In other cases, it might mean extending the incision. However, if the incision is a low transverse incision (the go-to for many gynecologists because of its favorable cosmetic and pain-producing profile) this proves to be difficult. Attempting to assist in a complicated case, such as a frozen pelvis, severed ureter or rectal injury, through a pfannensteil incision can be extraordinarily difficult, and while these incisions can be extended by incising the rectus muscle bellies, upper abdominal visualization remains elusive in most patients. This is particularly problematic if the ureter or splenic flexure need to be mobilized, or if extensive lysis of adhesions is necessary to ensure there is no occult enterotomy. As my mentor Dr. John Soper once described to me: “It’s like trying to scratch your armpit by reaching through your fly.”
While pfannensteil incisions come naturally, and comfortably, to most gynecologists, likely because of their frequent application during cesarean section, all gynecologists should be confident in the steps and anatomy for vertical midline, or paramedian incisions. This is not only beneficial for complex gynecologic cases, but also in the event of vascular emergency. In the hands of an experienced abdominal/pelvic surgeon, the vertical midline incision is the quickest way to safely enter the abdomen, and provides the kind of exposure that may be critical in safely repairing or controlling hemorrhage from a major vessel.
While low transverse incisions may be more cosmetic, less painful, and associated with fewer wound complications, our first concern as surgeons should be mitigating complications. In situations where risks of complications are high, it is best to not handicap ourselves with the incision location. And always remember, wound complications are highest when a transverse incision needs to be converted to a vertical one with a “T.”
It’s not just about diagnosis of cancer, it’s also prevention
Detection of cancer is an important role of the obstetrician gynecologist. However, equally important is being able to seize opportunities for cancer prevention. Cervical, vulvar, endometrial and ovarian cancer are all known to have preventative strategies.
All patients up to the age of 45 should be offered vaccination against HPV. Initial indications for HPV vaccination were for women up to age 26; however, recent data support the safety and efficacy of the vaccine in older women.3 HPV vaccination is most effective at preventing cancer when administered prior to exposure (ideally age 9-11), leaving this in the hands of our pediatrician colleagues. However, we must be vigilant to inquire about vaccination status for all our patients and encourage vaccines for those who were missed earlier in their life.
Patients should be counseled regarding the significant risk reduction for cancer that is gained from use of oral hormonal contraceptives and progestin-releasing IUDs (especially for endometrial and ovarian cancers). Providing them with knowledge of this information when considering options for contraception or menstrual cycle management is important in their decision-making process.
Endometrial cancer incidence is sadly on the rise in the United States, likely secondary to increasing rates of obesity. Pregnancy is a time when many women begin to gain, and accumulate, weight and therefore obstetric providers have a unique opportunity to assist patients in strategies to normalize their weight after pregnancy. Many of my patients with endometrial cancer state that they have never heard that it is associated with obesity. This suggests that more can be done to educate patients on the carcinogenic effect of obesity (for both endometrial and breast cancer), which may aid in motivating change of modifiable behaviors.
The fallopian tubes are the source of many ovarian cancers and knowledge of this has led to the recommendation to perform opportunistic salpingectomy as a cancer risk-reducing strategy. Hysterectomy and sterilization procedures are most apropos for this modification. While prospective data to confirm a reduced risk of ovarian cancer with opportunistic salpingectomy are lacking, a reduced incidence of cancer has been observed when the tubes have been removed for indicated surgeries; there appear to be no significant deleterious sequelae.4,5 A focus should be made on removal of the entire distal third of the tube, particularly the fimbriated ends, as this is the portion most implicated in malignancy.
Dr. Rossi is assistant professor in the division of gynecologic oncology at the University of North Carolina at Chapel Hill. She has no relevant disclosures. Contact her at obnews@mdedge.com.
References
1. Buys SS et al. JAMA. 2011;305(22):2295.
2. Goff BA et al. JAMA. 2004;291(22):2705.
3. Castellsagué X et al. Br J Cancer. 2011;105(1):28.
4. Yoon SH et al. Eur J Cancer. 2016 Mar;55:38-46.
5. Hanley GE et al. Am J Obstet Gynecol. 2018;219(2):172.
In this month’s column we continue to discuss recommendations from the gynecologic oncologist to the general gynecologist.
Don’t screen average-risk women for ovarian cancer.
Ovarian cancer is most often diagnosed at an advanced stage, which limits the curability of the disease. Consequently, there is a strong focus on attempting to diagnose the disease at earlier, more curable stages. This leads to the impulse by some well-intentioned providers to implement screening tests, such as ultrasounds and tumor markers, for all women. Unfortunately, the screening of “average risk” women for ovarian cancer is not recommended. Randomized controlled trials of tens of thousands of women have not observed a clinically significant decrease in ovarian cancer mortality with the addition of screening with tumor markers and ultrasound.1 These studies did observe a false-positive rate of 5%. While that may seem like a low rate of false-positive testing, the definitive diagnostic test which follows is a major abdominal surgery (oophorectomy) and serious complications are encountered in 15% of patients undergoing surgery for false-positive ovarian cancer screening.1 Therefore, quite simply, the harms are not balanced by benefits.
The key to offering patients appropriate and effective screening is case selection. It is important to identify which patients are at higher risk for ovarian cancer and offer those women testing for germline mutations and screening strategies. An important component of a well-woman visit is to take a thorough family history of cancer. Women are considered at high risk for having hereditary predisposition to ovarian cancer if they have a first- or second-degree relative with breast cancer younger than 45-50 years, or any age if Ashkenazi Jewish, triple-negative breast cancer younger than 60 years of age, two or more primary breast cancers with the first diagnosed at less than 50 years of age, male breast cancer, ovarian cancer, pancreatic cancer, a known BRCA 1/2 mutation, or a personal history of those same conditions. These women should be recommended to undergo genetic testing for BRCA 1, 2, and Lynch syndrome. They should not automatically be offered ovarian cancer screening. If a patient has a more remote family history for ovarian cancer, their personal risk may be somewhat elevated above the baseline population risk, however, not substantially enough to justify implementing screening in the absence of a confirmed genetic mutation.
While screening tests may not be appropriate for all patients, all patients should be asked about the early symptoms of ovarian cancer because these are consistently present, and frequently overlooked, prior to the eventual diagnosis of advanced disease. Those symptoms include abdominal discomfort, abdominal swelling and bloating, and urinary urgency.2 Consider offering all patients a dedicated ovarian cancer specific review of systems that includes inquiries about these symptoms at their annual wellness visits.
Opt for vertical midline incisions when surgery is anticipated to be complex
What is the first thing gynecologic oncologists do when called in to assist in a difficult gynecologic procedure? Get better exposure. Exposure is the cornerstone of safe, effective surgery. Sometimes this simply means placing a more effective retractor. In other cases, it might mean extending the incision. However, if the incision is a low transverse incision (the go-to for many gynecologists because of its favorable cosmetic and pain-producing profile) this proves to be difficult. Attempting to assist in a complicated case, such as a frozen pelvis, severed ureter or rectal injury, through a pfannensteil incision can be extraordinarily difficult, and while these incisions can be extended by incising the rectus muscle bellies, upper abdominal visualization remains elusive in most patients. This is particularly problematic if the ureter or splenic flexure need to be mobilized, or if extensive lysis of adhesions is necessary to ensure there is no occult enterotomy. As my mentor Dr. John Soper once described to me: “It’s like trying to scratch your armpit by reaching through your fly.”
While pfannensteil incisions come naturally, and comfortably, to most gynecologists, likely because of their frequent application during cesarean section, all gynecologists should be confident in the steps and anatomy for vertical midline, or paramedian incisions. This is not only beneficial for complex gynecologic cases, but also in the event of vascular emergency. In the hands of an experienced abdominal/pelvic surgeon, the vertical midline incision is the quickest way to safely enter the abdomen, and provides the kind of exposure that may be critical in safely repairing or controlling hemorrhage from a major vessel.
While low transverse incisions may be more cosmetic, less painful, and associated with fewer wound complications, our first concern as surgeons should be mitigating complications. In situations where risks of complications are high, it is best to not handicap ourselves with the incision location. And always remember, wound complications are highest when a transverse incision needs to be converted to a vertical one with a “T.”
It’s not just about diagnosis of cancer, it’s also prevention
Detection of cancer is an important role of the obstetrician gynecologist. However, equally important is being able to seize opportunities for cancer prevention. Cervical, vulvar, endometrial and ovarian cancer are all known to have preventative strategies.
All patients up to the age of 45 should be offered vaccination against HPV. Initial indications for HPV vaccination were for women up to age 26; however, recent data support the safety and efficacy of the vaccine in older women.3 HPV vaccination is most effective at preventing cancer when administered prior to exposure (ideally age 9-11), leaving this in the hands of our pediatrician colleagues. However, we must be vigilant to inquire about vaccination status for all our patients and encourage vaccines for those who were missed earlier in their life.
Patients should be counseled regarding the significant risk reduction for cancer that is gained from use of oral hormonal contraceptives and progestin-releasing IUDs (especially for endometrial and ovarian cancers). Providing them with knowledge of this information when considering options for contraception or menstrual cycle management is important in their decision-making process.
Endometrial cancer incidence is sadly on the rise in the United States, likely secondary to increasing rates of obesity. Pregnancy is a time when many women begin to gain, and accumulate, weight and therefore obstetric providers have a unique opportunity to assist patients in strategies to normalize their weight after pregnancy. Many of my patients with endometrial cancer state that they have never heard that it is associated with obesity. This suggests that more can be done to educate patients on the carcinogenic effect of obesity (for both endometrial and breast cancer), which may aid in motivating change of modifiable behaviors.
The fallopian tubes are the source of many ovarian cancers and knowledge of this has led to the recommendation to perform opportunistic salpingectomy as a cancer risk-reducing strategy. Hysterectomy and sterilization procedures are most apropos for this modification. While prospective data to confirm a reduced risk of ovarian cancer with opportunistic salpingectomy are lacking, a reduced incidence of cancer has been observed when the tubes have been removed for indicated surgeries; there appear to be no significant deleterious sequelae.4,5 A focus should be made on removal of the entire distal third of the tube, particularly the fimbriated ends, as this is the portion most implicated in malignancy.
Dr. Rossi is assistant professor in the division of gynecologic oncology at the University of North Carolina at Chapel Hill. She has no relevant disclosures. Contact her at obnews@mdedge.com.
References
1. Buys SS et al. JAMA. 2011;305(22):2295.
2. Goff BA et al. JAMA. 2004;291(22):2705.
3. Castellsagué X et al. Br J Cancer. 2011;105(1):28.
4. Yoon SH et al. Eur J Cancer. 2016 Mar;55:38-46.
5. Hanley GE et al. Am J Obstet Gynecol. 2018;219(2):172.
Not so fast food
As long as I can remember, children have been notoriously wasteful when dining in school cafeterias. Even those children who bring their own food often return home in the afternoon with their lunches half eaten. Not surprisingly, the food tossed out is often the healthier portion of the meal. Schools have tried a variety of strategies to curb this wastage, including using volunteer student monitors to police and encourage ecologically based recycling.
The authors of a recent study published on JAMA Network Open observed that when elementary and middle-school students were allowed a 20-minute seated lunch period they consumed more food and there was significantly less waste of fruits and vegetable compared with when the students’ lunch period was limited to 10 minutes. Interestingly, there was no difference in the beverage and entrée consumption when the lunch period was doubled.
The authors postulate that younger children may not have acquired the dexterity to feed themselves optimally in the shorter lunch period. I’m not sure I buy that argument. It may be simply that the children ate and drank their favorites first and needed a bit more time to allow their little guts to move things along. But, regardless of the explanation, the investigators’ observations deserve further study.
When I was in high school our lunch period was a full hour, which allowed me to make the half mile walk to home and back to eat a home-prepared meal. The noon hour was when school clubs and committees met and there was a full schedule of diversions to fill out the hour. I don’t recall the seated portion of the lunch period having any time restriction.
By the time my own children were in middle school, lunch periods lasted no longer than 20 minutes. I was not surprised to learn from this recent study that in some schools the seated lunch period has been shortened to 10 minutes. In some cases the truncated lunch periods are a response to space and time limitations. I fear that occasionally, educators and administrators have found it so difficult to keep young children who are accustomed to watching television while they eat engaged that the periods have been shortened to minimize the chaos.
Here in Maine, the governor has just announced plans to offer free breakfast and lunch to every student in response to a federal initiative. If we intend to make nutrition a cornerstone of the educational process this study from the University of Illinois at Urbana-Champaign suggests that we must do more than simply provide the food at no cost. We must somehow carve out more time in the day for the children to eat a healthy diet.
But, where is this time going to come from? Many school systems have already cannibalized physical education to the point that most children are not getting a healthy amount of exercise. It is unfortunate that we have come to expect public school systems to solve all of our societal ills and compensate for less-than-healthy home environments. But that is the reality. If we think nutrition and physical activity are important components of our children’s educations then we must make the time necessary to provide them.
Will this mean longer school days? And will those longer days cost money? You bet they will, but that may be the price we have to pay for healthier, better educated children.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
As long as I can remember, children have been notoriously wasteful when dining in school cafeterias. Even those children who bring their own food often return home in the afternoon with their lunches half eaten. Not surprisingly, the food tossed out is often the healthier portion of the meal. Schools have tried a variety of strategies to curb this wastage, including using volunteer student monitors to police and encourage ecologically based recycling.
The authors of a recent study published on JAMA Network Open observed that when elementary and middle-school students were allowed a 20-minute seated lunch period they consumed more food and there was significantly less waste of fruits and vegetable compared with when the students’ lunch period was limited to 10 minutes. Interestingly, there was no difference in the beverage and entrée consumption when the lunch period was doubled.
The authors postulate that younger children may not have acquired the dexterity to feed themselves optimally in the shorter lunch period. I’m not sure I buy that argument. It may be simply that the children ate and drank their favorites first and needed a bit more time to allow their little guts to move things along. But, regardless of the explanation, the investigators’ observations deserve further study.
When I was in high school our lunch period was a full hour, which allowed me to make the half mile walk to home and back to eat a home-prepared meal. The noon hour was when school clubs and committees met and there was a full schedule of diversions to fill out the hour. I don’t recall the seated portion of the lunch period having any time restriction.
By the time my own children were in middle school, lunch periods lasted no longer than 20 minutes. I was not surprised to learn from this recent study that in some schools the seated lunch period has been shortened to 10 minutes. In some cases the truncated lunch periods are a response to space and time limitations. I fear that occasionally, educators and administrators have found it so difficult to keep young children who are accustomed to watching television while they eat engaged that the periods have been shortened to minimize the chaos.
Here in Maine, the governor has just announced plans to offer free breakfast and lunch to every student in response to a federal initiative. If we intend to make nutrition a cornerstone of the educational process this study from the University of Illinois at Urbana-Champaign suggests that we must do more than simply provide the food at no cost. We must somehow carve out more time in the day for the children to eat a healthy diet.
But, where is this time going to come from? Many school systems have already cannibalized physical education to the point that most children are not getting a healthy amount of exercise. It is unfortunate that we have come to expect public school systems to solve all of our societal ills and compensate for less-than-healthy home environments. But that is the reality. If we think nutrition and physical activity are important components of our children’s educations then we must make the time necessary to provide them.
Will this mean longer school days? And will those longer days cost money? You bet they will, but that may be the price we have to pay for healthier, better educated children.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
As long as I can remember, children have been notoriously wasteful when dining in school cafeterias. Even those children who bring their own food often return home in the afternoon with their lunches half eaten. Not surprisingly, the food tossed out is often the healthier portion of the meal. Schools have tried a variety of strategies to curb this wastage, including using volunteer student monitors to police and encourage ecologically based recycling.
The authors of a recent study published on JAMA Network Open observed that when elementary and middle-school students were allowed a 20-minute seated lunch period they consumed more food and there was significantly less waste of fruits and vegetable compared with when the students’ lunch period was limited to 10 minutes. Interestingly, there was no difference in the beverage and entrée consumption when the lunch period was doubled.
The authors postulate that younger children may not have acquired the dexterity to feed themselves optimally in the shorter lunch period. I’m not sure I buy that argument. It may be simply that the children ate and drank their favorites first and needed a bit more time to allow their little guts to move things along. But, regardless of the explanation, the investigators’ observations deserve further study.
When I was in high school our lunch period was a full hour, which allowed me to make the half mile walk to home and back to eat a home-prepared meal. The noon hour was when school clubs and committees met and there was a full schedule of diversions to fill out the hour. I don’t recall the seated portion of the lunch period having any time restriction.
By the time my own children were in middle school, lunch periods lasted no longer than 20 minutes. I was not surprised to learn from this recent study that in some schools the seated lunch period has been shortened to 10 minutes. In some cases the truncated lunch periods are a response to space and time limitations. I fear that occasionally, educators and administrators have found it so difficult to keep young children who are accustomed to watching television while they eat engaged that the periods have been shortened to minimize the chaos.
Here in Maine, the governor has just announced plans to offer free breakfast and lunch to every student in response to a federal initiative. If we intend to make nutrition a cornerstone of the educational process this study from the University of Illinois at Urbana-Champaign suggests that we must do more than simply provide the food at no cost. We must somehow carve out more time in the day for the children to eat a healthy diet.
But, where is this time going to come from? Many school systems have already cannibalized physical education to the point that most children are not getting a healthy amount of exercise. It is unfortunate that we have come to expect public school systems to solve all of our societal ills and compensate for less-than-healthy home environments. But that is the reality. If we think nutrition and physical activity are important components of our children’s educations then we must make the time necessary to provide them.
Will this mean longer school days? And will those longer days cost money? You bet they will, but that may be the price we have to pay for healthier, better educated children.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
Q&A: Get flu shot early this year? Same time as COVID vaccine?
With first-time COVID-19 immunizations continuing and the plan to offer booster vaccines to most Americans starting next month, what are the considerations for getting COVID-19 and flu shots at the same time?
This news organization asked Andrew T. Pavia, MD, for his advice. He is the George and Esther Gross Presidential Professor and chief of the division of pediatric infectious diseases at the University of Utah, Salt Lake City, and a fellow of the Infectious Diseases Society of America.
Q: With COVID-19 cases surging, is it a good idea to get the flu shot early this season?
Dr. Pavia: I don’t think there is a rush to do it in August, but it is a good idea to get a flu shot this season. The consequences of getting the flu while COVID is circulating are serious.
Q: What are the implications?
There are some we know and some we don’t know. If you develop flu-like symptoms, you’re going to have to get tested. You’re going to have to stay home quite a bit longer if you get a definitive (positive COVID-19) test than you would simply with flu symptoms. Also, you’re probably going to miss work when your workplace is very stressed or your children are stressed by having COVID circulating in schools.
The part we know less about are the implications of getting the flu and COVID together. There is some reason to believe if you get them together, the illness will be more severe. We are seeing that with RSV (respiratory syncytial virus) and parainfluenza and COVID coinfections in children. They appear to be quite severe.
But for flu, we just don’t have the data yet. That’s because there really was no cocirculation of COVID and influenza with the exception of parts of China for a brief part of February and March.
Q: Will the planned administration of booster COVID-19 shots this fall affect the number of people who get the flu vaccine or how it’s distributed?
It creates a lot of logistical challenges, particularly for hospitals and other places that need to vaccinate a large number of their employees for flu and that will need to give COVID boosters at about the same time period. It also creates logistical challenges for doctors’ offices.
But we don’t know of any reason why you can’t give the two shots together.
Q: Is it possible flu season will be more severe because we isolated and wore masks, etc., last winter? Any science behind that?
The more you study flu, the less you can predict, and I’ve been studying flu for a long time. There are reasons that might suggest a severe flu season – there has been limited immunity, and some people are not wearing masks effectively and they are gathering again. Those are things we believe protected us from influenza last season.
But we have not seen flu emerge yet. Normally we look to Australia, New Zealand, and South Africa during their winter – which is our summer – to get some idea of what is over the horizon for the Northern Hemisphere. Flu activity in Australia has been very modest this year.
That might mean flu may not show up for a while, but I would be loathe to make a prediction.
Q: What are the chances we’ll see a flu outbreak like we’re seeing with RSV, which is normally a winter illness?
The fact that we had a summer RSV surge just gives you an idea of how the normal epidemiology of viral infections has been disrupted. It means anything could happen with influenza. It could show up late summer or fall or wait until next spring.
We really don’t understand how those interactions work. When a new flu strain emerges, it often ignores the traditional behavior and shows up in the spring or fall. It happened in the 2009 pandemic, it happened in 1918.
The one thing I would safely predict about the next flu wave is that it will surprise us.
Q: Are you hopeful that combination vaccines in development from a number of companies, such as Moderna, Novavax, and Vivaldi, will be effective?
It is beginning to look like COVID will be with us for the foreseeable future – maybe as a seasonal virus or maybe as an ongoing pandemic. We are going to need to protect (ourselves) simultaneously against the flu and COVID. A single shot is a great way to do that – nobody wants two needles; nobody wants two trips to get vaccinated.
An effective combination vaccine would be a really great tool.
We have to wait to see what the science shows us, because they are quite different viruses. We won’t know if a combination vaccine works well and has acceptable side effects until we do those studies.
Q. Do you know at this point whether the side effects from two vaccines would be additive? Is there any way to predict that?
There is no way to predict. There are so many things that go into whether someone has side effects that we don’t understand. With fairly reactogenic vaccines like the mRNA vaccines, lots of people have no side effects whatsoever and others are really uncomfortable for 24 hours.
Flu is generally a better tolerated vaccine. There are still people who get muscle aches and very sore arms. I don’t think we can predict if getting two will be additive or just the same as getting one vaccine.
Q: Other than convenience and the benefit for people who are needle-phobic, are there any other advantages of combining them into one shot?
The logistics alone are enough to justify having one effective product if we can make one. It should reduce the overall cost of administration and reduce time off from work.
The combination vaccines given by pediatricians have been very successful. They reduce the number of needles for kids and make it much easier for parents and the pediatricians administering them. The same principle should apply to adults, who sometimes are less brave about needles than kids are.
Historically, combined vaccines in general have worked as well as vaccines given alone, but there have been exceptions. We just have to see what the products look like.
Q: For now, the flu vaccine and COVID-19 vaccine are single products. If you get them separately, is it better to put some time between the two?
We don’t know. There are studies that probably won’t be out in time to decide in September. They are looking at whether you get an equivalent immune response if you give them together or apart.
For now, I would say the advantage of getting them together is if you do get side effects, you’ll only get them once – one day to suffer through them. Also, it’s one trip to the doctor.
The potential advantage of separating them is that is how we developed and tested the vaccines. If you do react to them, side effects could be milder, but it will be on two separate days.
I would recommend doing whatever works so that you get both vaccines in a timely manner.
I’m going to get my flu shot as soon as it’s available. If I’m due for a COVID booster at that time, I would probably do them together.
Q: Do you foresee a point in the future when the predominant strain of SARS-CoV-2 will be one of the components of a flu vaccine, like we did in the past with H1N1, etc?
It really remains to be seen, but it is very conceivable it could happen. The same companies that developed COVID-19 vaccines are working on flu vaccines.
Q: Any other advice for people concerned about getting immunized against both COVID-19 and influenza in the coming months?
There is no side effect of the vaccine that begins to approach the risk you face from either disease. It’s really one of the best things you can do to protect yourself is to get vaccinated.
In the case of flu, the vaccine is only modestly effective, but it still saves tens of thousands of lives each year. The SARS-CoV-2 vaccine is a much better vaccine and a deadlier disease.
Dr. Pavia consulted for GlaxoSmithKline on influenza testing.
A version of this article first appeared on Medscape.com.
With first-time COVID-19 immunizations continuing and the plan to offer booster vaccines to most Americans starting next month, what are the considerations for getting COVID-19 and flu shots at the same time?
This news organization asked Andrew T. Pavia, MD, for his advice. He is the George and Esther Gross Presidential Professor and chief of the division of pediatric infectious diseases at the University of Utah, Salt Lake City, and a fellow of the Infectious Diseases Society of America.
Q: With COVID-19 cases surging, is it a good idea to get the flu shot early this season?
Dr. Pavia: I don’t think there is a rush to do it in August, but it is a good idea to get a flu shot this season. The consequences of getting the flu while COVID is circulating are serious.
Q: What are the implications?
There are some we know and some we don’t know. If you develop flu-like symptoms, you’re going to have to get tested. You’re going to have to stay home quite a bit longer if you get a definitive (positive COVID-19) test than you would simply with flu symptoms. Also, you’re probably going to miss work when your workplace is very stressed or your children are stressed by having COVID circulating in schools.
The part we know less about are the implications of getting the flu and COVID together. There is some reason to believe if you get them together, the illness will be more severe. We are seeing that with RSV (respiratory syncytial virus) and parainfluenza and COVID coinfections in children. They appear to be quite severe.
But for flu, we just don’t have the data yet. That’s because there really was no cocirculation of COVID and influenza with the exception of parts of China for a brief part of February and March.
Q: Will the planned administration of booster COVID-19 shots this fall affect the number of people who get the flu vaccine or how it’s distributed?
It creates a lot of logistical challenges, particularly for hospitals and other places that need to vaccinate a large number of their employees for flu and that will need to give COVID boosters at about the same time period. It also creates logistical challenges for doctors’ offices.
But we don’t know of any reason why you can’t give the two shots together.
Q: Is it possible flu season will be more severe because we isolated and wore masks, etc., last winter? Any science behind that?
The more you study flu, the less you can predict, and I’ve been studying flu for a long time. There are reasons that might suggest a severe flu season – there has been limited immunity, and some people are not wearing masks effectively and they are gathering again. Those are things we believe protected us from influenza last season.
But we have not seen flu emerge yet. Normally we look to Australia, New Zealand, and South Africa during their winter – which is our summer – to get some idea of what is over the horizon for the Northern Hemisphere. Flu activity in Australia has been very modest this year.
That might mean flu may not show up for a while, but I would be loathe to make a prediction.
Q: What are the chances we’ll see a flu outbreak like we’re seeing with RSV, which is normally a winter illness?
The fact that we had a summer RSV surge just gives you an idea of how the normal epidemiology of viral infections has been disrupted. It means anything could happen with influenza. It could show up late summer or fall or wait until next spring.
We really don’t understand how those interactions work. When a new flu strain emerges, it often ignores the traditional behavior and shows up in the spring or fall. It happened in the 2009 pandemic, it happened in 1918.
The one thing I would safely predict about the next flu wave is that it will surprise us.
Q: Are you hopeful that combination vaccines in development from a number of companies, such as Moderna, Novavax, and Vivaldi, will be effective?
It is beginning to look like COVID will be with us for the foreseeable future – maybe as a seasonal virus or maybe as an ongoing pandemic. We are going to need to protect (ourselves) simultaneously against the flu and COVID. A single shot is a great way to do that – nobody wants two needles; nobody wants two trips to get vaccinated.
An effective combination vaccine would be a really great tool.
We have to wait to see what the science shows us, because they are quite different viruses. We won’t know if a combination vaccine works well and has acceptable side effects until we do those studies.
Q. Do you know at this point whether the side effects from two vaccines would be additive? Is there any way to predict that?
There is no way to predict. There are so many things that go into whether someone has side effects that we don’t understand. With fairly reactogenic vaccines like the mRNA vaccines, lots of people have no side effects whatsoever and others are really uncomfortable for 24 hours.
Flu is generally a better tolerated vaccine. There are still people who get muscle aches and very sore arms. I don’t think we can predict if getting two will be additive or just the same as getting one vaccine.
Q: Other than convenience and the benefit for people who are needle-phobic, are there any other advantages of combining them into one shot?
The logistics alone are enough to justify having one effective product if we can make one. It should reduce the overall cost of administration and reduce time off from work.
The combination vaccines given by pediatricians have been very successful. They reduce the number of needles for kids and make it much easier for parents and the pediatricians administering them. The same principle should apply to adults, who sometimes are less brave about needles than kids are.
Historically, combined vaccines in general have worked as well as vaccines given alone, but there have been exceptions. We just have to see what the products look like.
Q: For now, the flu vaccine and COVID-19 vaccine are single products. If you get them separately, is it better to put some time between the two?
We don’t know. There are studies that probably won’t be out in time to decide in September. They are looking at whether you get an equivalent immune response if you give them together or apart.
For now, I would say the advantage of getting them together is if you do get side effects, you’ll only get them once – one day to suffer through them. Also, it’s one trip to the doctor.
The potential advantage of separating them is that is how we developed and tested the vaccines. If you do react to them, side effects could be milder, but it will be on two separate days.
I would recommend doing whatever works so that you get both vaccines in a timely manner.
I’m going to get my flu shot as soon as it’s available. If I’m due for a COVID booster at that time, I would probably do them together.
Q: Do you foresee a point in the future when the predominant strain of SARS-CoV-2 will be one of the components of a flu vaccine, like we did in the past with H1N1, etc?
It really remains to be seen, but it is very conceivable it could happen. The same companies that developed COVID-19 vaccines are working on flu vaccines.
Q: Any other advice for people concerned about getting immunized against both COVID-19 and influenza in the coming months?
There is no side effect of the vaccine that begins to approach the risk you face from either disease. It’s really one of the best things you can do to protect yourself is to get vaccinated.
In the case of flu, the vaccine is only modestly effective, but it still saves tens of thousands of lives each year. The SARS-CoV-2 vaccine is a much better vaccine and a deadlier disease.
Dr. Pavia consulted for GlaxoSmithKline on influenza testing.
A version of this article first appeared on Medscape.com.
With first-time COVID-19 immunizations continuing and the plan to offer booster vaccines to most Americans starting next month, what are the considerations for getting COVID-19 and flu shots at the same time?
This news organization asked Andrew T. Pavia, MD, for his advice. He is the George and Esther Gross Presidential Professor and chief of the division of pediatric infectious diseases at the University of Utah, Salt Lake City, and a fellow of the Infectious Diseases Society of America.
Q: With COVID-19 cases surging, is it a good idea to get the flu shot early this season?
Dr. Pavia: I don’t think there is a rush to do it in August, but it is a good idea to get a flu shot this season. The consequences of getting the flu while COVID is circulating are serious.
Q: What are the implications?
There are some we know and some we don’t know. If you develop flu-like symptoms, you’re going to have to get tested. You’re going to have to stay home quite a bit longer if you get a definitive (positive COVID-19) test than you would simply with flu symptoms. Also, you’re probably going to miss work when your workplace is very stressed or your children are stressed by having COVID circulating in schools.
The part we know less about are the implications of getting the flu and COVID together. There is some reason to believe if you get them together, the illness will be more severe. We are seeing that with RSV (respiratory syncytial virus) and parainfluenza and COVID coinfections in children. They appear to be quite severe.
But for flu, we just don’t have the data yet. That’s because there really was no cocirculation of COVID and influenza with the exception of parts of China for a brief part of February and March.
Q: Will the planned administration of booster COVID-19 shots this fall affect the number of people who get the flu vaccine or how it’s distributed?
It creates a lot of logistical challenges, particularly for hospitals and other places that need to vaccinate a large number of their employees for flu and that will need to give COVID boosters at about the same time period. It also creates logistical challenges for doctors’ offices.
But we don’t know of any reason why you can’t give the two shots together.
Q: Is it possible flu season will be more severe because we isolated and wore masks, etc., last winter? Any science behind that?
The more you study flu, the less you can predict, and I’ve been studying flu for a long time. There are reasons that might suggest a severe flu season – there has been limited immunity, and some people are not wearing masks effectively and they are gathering again. Those are things we believe protected us from influenza last season.
But we have not seen flu emerge yet. Normally we look to Australia, New Zealand, and South Africa during their winter – which is our summer – to get some idea of what is over the horizon for the Northern Hemisphere. Flu activity in Australia has been very modest this year.
That might mean flu may not show up for a while, but I would be loathe to make a prediction.
Q: What are the chances we’ll see a flu outbreak like we’re seeing with RSV, which is normally a winter illness?
The fact that we had a summer RSV surge just gives you an idea of how the normal epidemiology of viral infections has been disrupted. It means anything could happen with influenza. It could show up late summer or fall or wait until next spring.
We really don’t understand how those interactions work. When a new flu strain emerges, it often ignores the traditional behavior and shows up in the spring or fall. It happened in the 2009 pandemic, it happened in 1918.
The one thing I would safely predict about the next flu wave is that it will surprise us.
Q: Are you hopeful that combination vaccines in development from a number of companies, such as Moderna, Novavax, and Vivaldi, will be effective?
It is beginning to look like COVID will be with us for the foreseeable future – maybe as a seasonal virus or maybe as an ongoing pandemic. We are going to need to protect (ourselves) simultaneously against the flu and COVID. A single shot is a great way to do that – nobody wants two needles; nobody wants two trips to get vaccinated.
An effective combination vaccine would be a really great tool.
We have to wait to see what the science shows us, because they are quite different viruses. We won’t know if a combination vaccine works well and has acceptable side effects until we do those studies.
Q. Do you know at this point whether the side effects from two vaccines would be additive? Is there any way to predict that?
There is no way to predict. There are so many things that go into whether someone has side effects that we don’t understand. With fairly reactogenic vaccines like the mRNA vaccines, lots of people have no side effects whatsoever and others are really uncomfortable for 24 hours.
Flu is generally a better tolerated vaccine. There are still people who get muscle aches and very sore arms. I don’t think we can predict if getting two will be additive or just the same as getting one vaccine.
Q: Other than convenience and the benefit for people who are needle-phobic, are there any other advantages of combining them into one shot?
The logistics alone are enough to justify having one effective product if we can make one. It should reduce the overall cost of administration and reduce time off from work.
The combination vaccines given by pediatricians have been very successful. They reduce the number of needles for kids and make it much easier for parents and the pediatricians administering them. The same principle should apply to adults, who sometimes are less brave about needles than kids are.
Historically, combined vaccines in general have worked as well as vaccines given alone, but there have been exceptions. We just have to see what the products look like.
Q: For now, the flu vaccine and COVID-19 vaccine are single products. If you get them separately, is it better to put some time between the two?
We don’t know. There are studies that probably won’t be out in time to decide in September. They are looking at whether you get an equivalent immune response if you give them together or apart.
For now, I would say the advantage of getting them together is if you do get side effects, you’ll only get them once – one day to suffer through them. Also, it’s one trip to the doctor.
The potential advantage of separating them is that is how we developed and tested the vaccines. If you do react to them, side effects could be milder, but it will be on two separate days.
I would recommend doing whatever works so that you get both vaccines in a timely manner.
I’m going to get my flu shot as soon as it’s available. If I’m due for a COVID booster at that time, I would probably do them together.
Q: Do you foresee a point in the future when the predominant strain of SARS-CoV-2 will be one of the components of a flu vaccine, like we did in the past with H1N1, etc?
It really remains to be seen, but it is very conceivable it could happen. The same companies that developed COVID-19 vaccines are working on flu vaccines.
Q: Any other advice for people concerned about getting immunized against both COVID-19 and influenza in the coming months?
There is no side effect of the vaccine that begins to approach the risk you face from either disease. It’s really one of the best things you can do to protect yourself is to get vaccinated.
In the case of flu, the vaccine is only modestly effective, but it still saves tens of thousands of lives each year. The SARS-CoV-2 vaccine is a much better vaccine and a deadlier disease.
Dr. Pavia consulted for GlaxoSmithKline on influenza testing.
A version of this article first appeared on Medscape.com.
Mifepristone freed of restrictions for the pandemic
Since evidence shows that medication abortion is extremely safe, why is mifepristone so restricted? And should it be? Mifepristone, used with misoprostol for medication abortion for pregnancies up to 10 weeks’ gestation, is highly regulated in the United States. Going back to 2000, when the Food and Drug Administration approved Mifeprex (brand name of mifepristone), its access was restricted under the FDA Risk Evaluation and Mitigation Strategy (REMS).
REMS is an FDA drug safety program, where certain medications with serious safety concerns are subject to restrictions intended to ensure that the benefits of the medication outweigh its risks. For example, the drug vigabatrin, with a side effect of permanent vision loss, is used to treat epilepsy. The REMS for vigabatrin requires counseling on the risk of vision loss and periodic vision monitoring.
The FDA claims that rare side effects of mifepristone – heavy vaginal bleeding, severe infection, and incomplete abortion – are risks that warrant the REMS, despite the known safety of medication abortion, with less than 1% of patients requiring emergency intervention for heavy vaginal bleeding or infection. The mifepristone REMS requires that the drug is dispensed in a hospital, clinic or medical office by a certified health care provider and not in a pharmacy as is the case with most prescribed medications, and that patients must read and sign the patient agreement form in the physical presence of the dispensing physician and may not receive counseling via telemedicine, for example.
Since FDA approval over 20 years ago, much evidence shows that the REMS is unnecessary and creates a major obstacle to access. Many clinicians cannot meet the REMS requirements. Many women must travel great distances to obtain mifepristone or delay their abortion past the acceptable gestational age for medication abortion.
In spring 2020, at the onset of the COVID-19 pandemic, the Centers for Disease Control and Prevention issued general guidance recommending use of telemedicine to limit in-person medical visits to reduce risk of exposure to the SARS-CoV-2 virus, and to ensure access to medication abortion, the ACLU filed a federal lawsuit against the FDA to suspend the requirement for in-person mifepristone dispensing. In July 2020, a Maryland District Judge granted a preliminary injunction, preventing the FDA from enforcing the in-person dispensing requirement for the duration of the declared public health emergency, allowing telemedicine medication abortion using mail or delivery service for administration of mifepristone. All other REMS requirements remained in effect.
In January 2021, the FDA appealed, seeking to reinstate the REMS. The U.S. Supreme Court, with its conservative majority, ruled to reimpose the REMS. Following this decision, a large coalition of reproductive rights groups petitioned the Biden administration to suspend the mifepristone in-person requirement during the public health emergency of the pandemic. In April 2021, the FDA announced it would use discretion and cease to enforce the in-person dispensing requirement throughout the remainder of the public health emergency.
We applaud the FDA for doing the right thing, taking the advice of numerous scientific and advocacy groups to expand access to mifepristone by at least temporarily nullifying unnecessary and burdensome restrictions that disproportionately affect people of color; young people; and people who live in rural areas, have lower incomes, and/or who are undocumented. We join the voices of numerous colleagues and organizations, including the American College of Obstetricians and Gynecologists, our premier women’s health organization, in calling for a permanent end to the mifepristone REMS.
Dr. Dale is an obstetrics and gynecology specialist in Albuquerque, N.M.; Dr. Black is an obstetrics and gynecology specialist in Albuquerque, N.M., who currently practices at the University of New Mexico Children’s Psychiatric Center, Albuquerque; and Dr. Espey is professor and chair of the department of ob.gyn. and family planning, and fellowship director at the University of New Mexico, Albuquerque.
This article was updated 8/24/21.
Since evidence shows that medication abortion is extremely safe, why is mifepristone so restricted? And should it be? Mifepristone, used with misoprostol for medication abortion for pregnancies up to 10 weeks’ gestation, is highly regulated in the United States. Going back to 2000, when the Food and Drug Administration approved Mifeprex (brand name of mifepristone), its access was restricted under the FDA Risk Evaluation and Mitigation Strategy (REMS).
REMS is an FDA drug safety program, where certain medications with serious safety concerns are subject to restrictions intended to ensure that the benefits of the medication outweigh its risks. For example, the drug vigabatrin, with a side effect of permanent vision loss, is used to treat epilepsy. The REMS for vigabatrin requires counseling on the risk of vision loss and periodic vision monitoring.
The FDA claims that rare side effects of mifepristone – heavy vaginal bleeding, severe infection, and incomplete abortion – are risks that warrant the REMS, despite the known safety of medication abortion, with less than 1% of patients requiring emergency intervention for heavy vaginal bleeding or infection. The mifepristone REMS requires that the drug is dispensed in a hospital, clinic or medical office by a certified health care provider and not in a pharmacy as is the case with most prescribed medications, and that patients must read and sign the patient agreement form in the physical presence of the dispensing physician and may not receive counseling via telemedicine, for example.
Since FDA approval over 20 years ago, much evidence shows that the REMS is unnecessary and creates a major obstacle to access. Many clinicians cannot meet the REMS requirements. Many women must travel great distances to obtain mifepristone or delay their abortion past the acceptable gestational age for medication abortion.
In spring 2020, at the onset of the COVID-19 pandemic, the Centers for Disease Control and Prevention issued general guidance recommending use of telemedicine to limit in-person medical visits to reduce risk of exposure to the SARS-CoV-2 virus, and to ensure access to medication abortion, the ACLU filed a federal lawsuit against the FDA to suspend the requirement for in-person mifepristone dispensing. In July 2020, a Maryland District Judge granted a preliminary injunction, preventing the FDA from enforcing the in-person dispensing requirement for the duration of the declared public health emergency, allowing telemedicine medication abortion using mail or delivery service for administration of mifepristone. All other REMS requirements remained in effect.
In January 2021, the FDA appealed, seeking to reinstate the REMS. The U.S. Supreme Court, with its conservative majority, ruled to reimpose the REMS. Following this decision, a large coalition of reproductive rights groups petitioned the Biden administration to suspend the mifepristone in-person requirement during the public health emergency of the pandemic. In April 2021, the FDA announced it would use discretion and cease to enforce the in-person dispensing requirement throughout the remainder of the public health emergency.
We applaud the FDA for doing the right thing, taking the advice of numerous scientific and advocacy groups to expand access to mifepristone by at least temporarily nullifying unnecessary and burdensome restrictions that disproportionately affect people of color; young people; and people who live in rural areas, have lower incomes, and/or who are undocumented. We join the voices of numerous colleagues and organizations, including the American College of Obstetricians and Gynecologists, our premier women’s health organization, in calling for a permanent end to the mifepristone REMS.
Dr. Dale is an obstetrics and gynecology specialist in Albuquerque, N.M.; Dr. Black is an obstetrics and gynecology specialist in Albuquerque, N.M., who currently practices at the University of New Mexico Children’s Psychiatric Center, Albuquerque; and Dr. Espey is professor and chair of the department of ob.gyn. and family planning, and fellowship director at the University of New Mexico, Albuquerque.
This article was updated 8/24/21.
Since evidence shows that medication abortion is extremely safe, why is mifepristone so restricted? And should it be? Mifepristone, used with misoprostol for medication abortion for pregnancies up to 10 weeks’ gestation, is highly regulated in the United States. Going back to 2000, when the Food and Drug Administration approved Mifeprex (brand name of mifepristone), its access was restricted under the FDA Risk Evaluation and Mitigation Strategy (REMS).
REMS is an FDA drug safety program, where certain medications with serious safety concerns are subject to restrictions intended to ensure that the benefits of the medication outweigh its risks. For example, the drug vigabatrin, with a side effect of permanent vision loss, is used to treat epilepsy. The REMS for vigabatrin requires counseling on the risk of vision loss and periodic vision monitoring.
The FDA claims that rare side effects of mifepristone – heavy vaginal bleeding, severe infection, and incomplete abortion – are risks that warrant the REMS, despite the known safety of medication abortion, with less than 1% of patients requiring emergency intervention for heavy vaginal bleeding or infection. The mifepristone REMS requires that the drug is dispensed in a hospital, clinic or medical office by a certified health care provider and not in a pharmacy as is the case with most prescribed medications, and that patients must read and sign the patient agreement form in the physical presence of the dispensing physician and may not receive counseling via telemedicine, for example.
Since FDA approval over 20 years ago, much evidence shows that the REMS is unnecessary and creates a major obstacle to access. Many clinicians cannot meet the REMS requirements. Many women must travel great distances to obtain mifepristone or delay their abortion past the acceptable gestational age for medication abortion.
In spring 2020, at the onset of the COVID-19 pandemic, the Centers for Disease Control and Prevention issued general guidance recommending use of telemedicine to limit in-person medical visits to reduce risk of exposure to the SARS-CoV-2 virus, and to ensure access to medication abortion, the ACLU filed a federal lawsuit against the FDA to suspend the requirement for in-person mifepristone dispensing. In July 2020, a Maryland District Judge granted a preliminary injunction, preventing the FDA from enforcing the in-person dispensing requirement for the duration of the declared public health emergency, allowing telemedicine medication abortion using mail or delivery service for administration of mifepristone. All other REMS requirements remained in effect.
In January 2021, the FDA appealed, seeking to reinstate the REMS. The U.S. Supreme Court, with its conservative majority, ruled to reimpose the REMS. Following this decision, a large coalition of reproductive rights groups petitioned the Biden administration to suspend the mifepristone in-person requirement during the public health emergency of the pandemic. In April 2021, the FDA announced it would use discretion and cease to enforce the in-person dispensing requirement throughout the remainder of the public health emergency.
We applaud the FDA for doing the right thing, taking the advice of numerous scientific and advocacy groups to expand access to mifepristone by at least temporarily nullifying unnecessary and burdensome restrictions that disproportionately affect people of color; young people; and people who live in rural areas, have lower incomes, and/or who are undocumented. We join the voices of numerous colleagues and organizations, including the American College of Obstetricians and Gynecologists, our premier women’s health organization, in calling for a permanent end to the mifepristone REMS.
Dr. Dale is an obstetrics and gynecology specialist in Albuquerque, N.M.; Dr. Black is an obstetrics and gynecology specialist in Albuquerque, N.M., who currently practices at the University of New Mexico Children’s Psychiatric Center, Albuquerque; and Dr. Espey is professor and chair of the department of ob.gyn. and family planning, and fellowship director at the University of New Mexico, Albuquerque.
This article was updated 8/24/21.












