User login
MDedge latest news is breaking news from medical conferences, journals, guidelines, the FDA and CDC.
Canadian Scientists Keep Watchful Eye on H5N1 Human Case
Now that Canada has confirmed its first human case of highly pathogenic avian influenza (HPAI) linked to H5N1, virologists and infectious disease experts are urging caution around surveillance, infection control, and the potential for spread among mammals and humans.
Public health officials at the National Microbiology Laboratory in Winnipeg, Manitoba, Canada, confirmed that the virus strain is related to the ones circulating among poultry in British Columbia.
So far, the case appears to be isolated, and no additional infections have been detected among the teen’s family, friends, or healthcare workers. But Canadian and American scientists who have studied the genetic sequence of the virus have found mutations that could make it easier to infect humans. Even if this strain remains contained after the teen’s case resolves, the mere fact that mutations have occurred could be a cause for concern about future strains.
“HPAI is one of those diseases that scientists, public health specialists, animal health specialists, and physicians have been watching closely for 20 years due to its epidemic and pandemic potential, including impacts to agriculture, food security, and financial security,” Isaac Bogoch, MD, associate professor of medicine at the University of Toronto and infectious disease specialist with the University Health Network, Toronto, Ontario, Canada, said in an interview.
“The last couple of years have been notable in that the H5N1 outbreak among wild birds and migratory birds has been larger, and the spillover to dairy cows and humans in the US is obviously concerning,” he said. “As we see more viral reassortment and more mammals are impacted, the more opportunities there are for this to go awry.”
Current H5N1 Outlook
Canadian public health officials and virologists are still unsure how the teen in British Columbia became infected, Bogoch said. The case has prompted concern due to the disease severity and need for hospitalization, while other cases across North America have remained mild.
The United States has reported 53 human cases as of November 21, according to the Centers for Disease Control and Prevention. In all but one case, the infections occurred among dairy or poultry workers, primarily in California, Colorado, and Washington. In all these cases, patients have reported mild symptoms, including mild respiratory issues and conjunctivitis. None have been hospitalized.
In Canada, the teen was infected with a strain of the virus circulating in wild birds. This strain has also been found in poultry outbreaks in British Columbia and Washington during the past month. So far, the risk for infection remains low for the public, according to the Public Health Agency of Canada.
“This detection was picked up via hospital-based influenza surveillance, confirming that human influenza surveillance in British Columbia and Canada is effective at detecting avian influenza A (H5N1),” Theresa Tam, MD, Canada’s chief public health officer, said in a statement. “We must continue to remain vigilant in our efforts to prevent the spread of avian influenza between animals and to humans.”
For now, Canadian virologists are watching developments closely and urging caution among those who encounter wild or migratory birds but not recommending major changes overall.
“The fact that we have a first human case in Canada is not at all surprising, given what is happening in the US and Europe, as well as what is happening in domestic bird flocks in British Columbia,” said Brian Ward, MD, professor of medicine at McGill University, researcher with McGill’s JD MacLean Centre for Tropical Diseases, and co-director of McGill’s Vaccine Study Centre, Montreal, Quebec, Canada.
“Millions of migratory waterfowl are flying over Canada right now, many of which may be carrying or infected with the virus,” he said. “The bottom line is that increasing evidence of mammal-to-mammal spread among dairy cows, elephant seals, and mink and ermine farms is worrisome, but we don’t need to sound the sirens yet.”
Future Outbreak Measures
Looking ahead, though, the developing situation feels more threatening than benign, given the ongoing spread among dairy cattle in the United States, said Bogoch. “It’s difficult to get the genie back in the bottle. I had hoped to see the cases slow down this year, but we just haven’t seen that.”
The fact that surveillance measures such as wastewater sampling have been scaled back in some areas of Canada is cause for concern, Bogoch added.
“We have great foundations for surveillance and action; we just need to make sure they are supported adequately, that groups communicate (across too many silos), and that there are quick responses,” said Scott Weese, DVM, professor of pathobiology at the Ontario Veterinary College and director of the University of Guelph’s Centre for Public Health and Zoonoses in Ontario.
“With cattle in the US, I think it’s highlighted what can happen if the initial response is not very aggressive. There could have been a lot more proactive response to H5N1 in dairy cattle, but there are so many competing interests and unwillingness to take necessary steps that the virus continues to spread,” he said. “Hopefully we’ve learned from that. However, as is often the case, the science is sometimes the easy part. Getting people to take the required actions is the challenge.”
On a personal level, masks and social distancing work well against influenza virus, including both seasonal and avian strains, said Ward. On a broader level, healthcare providers can monitor patients and support testing, where appropriate.
“The most important thing for people to know is that there is going to be another pandemic. It might or might not be due to a variant of H5N1, but it will come at some time,” said Allison McGeer, MD, professor of laboratory medicine and pathobiology at the University of Toronto and an infectious disease specialist with the Sinai Health System, Toronto.
Healthcare providers should follow ongoing updates to public health guidance, support surveillance where possible, and work with hospital leadership and infection control officials to ensure that pandemic plans are in place, she said.
“They may not be needed in the next few months, but they will be needed,” McGeer said. “We know a lot more about influenza than we did about SARS-CoV-2, so we have more tools to mitigate the impact, but we need to have them ready and know how to use them effectively.”
A version of this article appeared on Medscape.com.
Now that Canada has confirmed its first human case of highly pathogenic avian influenza (HPAI) linked to H5N1, virologists and infectious disease experts are urging caution around surveillance, infection control, and the potential for spread among mammals and humans.
Public health officials at the National Microbiology Laboratory in Winnipeg, Manitoba, Canada, confirmed that the virus strain is related to the ones circulating among poultry in British Columbia.
So far, the case appears to be isolated, and no additional infections have been detected among the teen’s family, friends, or healthcare workers. But Canadian and American scientists who have studied the genetic sequence of the virus have found mutations that could make it easier to infect humans. Even if this strain remains contained after the teen’s case resolves, the mere fact that mutations have occurred could be a cause for concern about future strains.
“HPAI is one of those diseases that scientists, public health specialists, animal health specialists, and physicians have been watching closely for 20 years due to its epidemic and pandemic potential, including impacts to agriculture, food security, and financial security,” Isaac Bogoch, MD, associate professor of medicine at the University of Toronto and infectious disease specialist with the University Health Network, Toronto, Ontario, Canada, said in an interview.
“The last couple of years have been notable in that the H5N1 outbreak among wild birds and migratory birds has been larger, and the spillover to dairy cows and humans in the US is obviously concerning,” he said. “As we see more viral reassortment and more mammals are impacted, the more opportunities there are for this to go awry.”
Current H5N1 Outlook
Canadian public health officials and virologists are still unsure how the teen in British Columbia became infected, Bogoch said. The case has prompted concern due to the disease severity and need for hospitalization, while other cases across North America have remained mild.
The United States has reported 53 human cases as of November 21, according to the Centers for Disease Control and Prevention. In all but one case, the infections occurred among dairy or poultry workers, primarily in California, Colorado, and Washington. In all these cases, patients have reported mild symptoms, including mild respiratory issues and conjunctivitis. None have been hospitalized.
In Canada, the teen was infected with a strain of the virus circulating in wild birds. This strain has also been found in poultry outbreaks in British Columbia and Washington during the past month. So far, the risk for infection remains low for the public, according to the Public Health Agency of Canada.
“This detection was picked up via hospital-based influenza surveillance, confirming that human influenza surveillance in British Columbia and Canada is effective at detecting avian influenza A (H5N1),” Theresa Tam, MD, Canada’s chief public health officer, said in a statement. “We must continue to remain vigilant in our efforts to prevent the spread of avian influenza between animals and to humans.”
For now, Canadian virologists are watching developments closely and urging caution among those who encounter wild or migratory birds but not recommending major changes overall.
“The fact that we have a first human case in Canada is not at all surprising, given what is happening in the US and Europe, as well as what is happening in domestic bird flocks in British Columbia,” said Brian Ward, MD, professor of medicine at McGill University, researcher with McGill’s JD MacLean Centre for Tropical Diseases, and co-director of McGill’s Vaccine Study Centre, Montreal, Quebec, Canada.
“Millions of migratory waterfowl are flying over Canada right now, many of which may be carrying or infected with the virus,” he said. “The bottom line is that increasing evidence of mammal-to-mammal spread among dairy cows, elephant seals, and mink and ermine farms is worrisome, but we don’t need to sound the sirens yet.”
Future Outbreak Measures
Looking ahead, though, the developing situation feels more threatening than benign, given the ongoing spread among dairy cattle in the United States, said Bogoch. “It’s difficult to get the genie back in the bottle. I had hoped to see the cases slow down this year, but we just haven’t seen that.”
The fact that surveillance measures such as wastewater sampling have been scaled back in some areas of Canada is cause for concern, Bogoch added.
“We have great foundations for surveillance and action; we just need to make sure they are supported adequately, that groups communicate (across too many silos), and that there are quick responses,” said Scott Weese, DVM, professor of pathobiology at the Ontario Veterinary College and director of the University of Guelph’s Centre for Public Health and Zoonoses in Ontario.
“With cattle in the US, I think it’s highlighted what can happen if the initial response is not very aggressive. There could have been a lot more proactive response to H5N1 in dairy cattle, but there are so many competing interests and unwillingness to take necessary steps that the virus continues to spread,” he said. “Hopefully we’ve learned from that. However, as is often the case, the science is sometimes the easy part. Getting people to take the required actions is the challenge.”
On a personal level, masks and social distancing work well against influenza virus, including both seasonal and avian strains, said Ward. On a broader level, healthcare providers can monitor patients and support testing, where appropriate.
“The most important thing for people to know is that there is going to be another pandemic. It might or might not be due to a variant of H5N1, but it will come at some time,” said Allison McGeer, MD, professor of laboratory medicine and pathobiology at the University of Toronto and an infectious disease specialist with the Sinai Health System, Toronto.
Healthcare providers should follow ongoing updates to public health guidance, support surveillance where possible, and work with hospital leadership and infection control officials to ensure that pandemic plans are in place, she said.
“They may not be needed in the next few months, but they will be needed,” McGeer said. “We know a lot more about influenza than we did about SARS-CoV-2, so we have more tools to mitigate the impact, but we need to have them ready and know how to use them effectively.”
A version of this article appeared on Medscape.com.
Now that Canada has confirmed its first human case of highly pathogenic avian influenza (HPAI) linked to H5N1, virologists and infectious disease experts are urging caution around surveillance, infection control, and the potential for spread among mammals and humans.
Public health officials at the National Microbiology Laboratory in Winnipeg, Manitoba, Canada, confirmed that the virus strain is related to the ones circulating among poultry in British Columbia.
So far, the case appears to be isolated, and no additional infections have been detected among the teen’s family, friends, or healthcare workers. But Canadian and American scientists who have studied the genetic sequence of the virus have found mutations that could make it easier to infect humans. Even if this strain remains contained after the teen’s case resolves, the mere fact that mutations have occurred could be a cause for concern about future strains.
“HPAI is one of those diseases that scientists, public health specialists, animal health specialists, and physicians have been watching closely for 20 years due to its epidemic and pandemic potential, including impacts to agriculture, food security, and financial security,” Isaac Bogoch, MD, associate professor of medicine at the University of Toronto and infectious disease specialist with the University Health Network, Toronto, Ontario, Canada, said in an interview.
“The last couple of years have been notable in that the H5N1 outbreak among wild birds and migratory birds has been larger, and the spillover to dairy cows and humans in the US is obviously concerning,” he said. “As we see more viral reassortment and more mammals are impacted, the more opportunities there are for this to go awry.”
Current H5N1 Outlook
Canadian public health officials and virologists are still unsure how the teen in British Columbia became infected, Bogoch said. The case has prompted concern due to the disease severity and need for hospitalization, while other cases across North America have remained mild.
The United States has reported 53 human cases as of November 21, according to the Centers for Disease Control and Prevention. In all but one case, the infections occurred among dairy or poultry workers, primarily in California, Colorado, and Washington. In all these cases, patients have reported mild symptoms, including mild respiratory issues and conjunctivitis. None have been hospitalized.
In Canada, the teen was infected with a strain of the virus circulating in wild birds. This strain has also been found in poultry outbreaks in British Columbia and Washington during the past month. So far, the risk for infection remains low for the public, according to the Public Health Agency of Canada.
“This detection was picked up via hospital-based influenza surveillance, confirming that human influenza surveillance in British Columbia and Canada is effective at detecting avian influenza A (H5N1),” Theresa Tam, MD, Canada’s chief public health officer, said in a statement. “We must continue to remain vigilant in our efforts to prevent the spread of avian influenza between animals and to humans.”
For now, Canadian virologists are watching developments closely and urging caution among those who encounter wild or migratory birds but not recommending major changes overall.
“The fact that we have a first human case in Canada is not at all surprising, given what is happening in the US and Europe, as well as what is happening in domestic bird flocks in British Columbia,” said Brian Ward, MD, professor of medicine at McGill University, researcher with McGill’s JD MacLean Centre for Tropical Diseases, and co-director of McGill’s Vaccine Study Centre, Montreal, Quebec, Canada.
“Millions of migratory waterfowl are flying over Canada right now, many of which may be carrying or infected with the virus,” he said. “The bottom line is that increasing evidence of mammal-to-mammal spread among dairy cows, elephant seals, and mink and ermine farms is worrisome, but we don’t need to sound the sirens yet.”
Future Outbreak Measures
Looking ahead, though, the developing situation feels more threatening than benign, given the ongoing spread among dairy cattle in the United States, said Bogoch. “It’s difficult to get the genie back in the bottle. I had hoped to see the cases slow down this year, but we just haven’t seen that.”
The fact that surveillance measures such as wastewater sampling have been scaled back in some areas of Canada is cause for concern, Bogoch added.
“We have great foundations for surveillance and action; we just need to make sure they are supported adequately, that groups communicate (across too many silos), and that there are quick responses,” said Scott Weese, DVM, professor of pathobiology at the Ontario Veterinary College and director of the University of Guelph’s Centre for Public Health and Zoonoses in Ontario.
“With cattle in the US, I think it’s highlighted what can happen if the initial response is not very aggressive. There could have been a lot more proactive response to H5N1 in dairy cattle, but there are so many competing interests and unwillingness to take necessary steps that the virus continues to spread,” he said. “Hopefully we’ve learned from that. However, as is often the case, the science is sometimes the easy part. Getting people to take the required actions is the challenge.”
On a personal level, masks and social distancing work well against influenza virus, including both seasonal and avian strains, said Ward. On a broader level, healthcare providers can monitor patients and support testing, where appropriate.
“The most important thing for people to know is that there is going to be another pandemic. It might or might not be due to a variant of H5N1, but it will come at some time,” said Allison McGeer, MD, professor of laboratory medicine and pathobiology at the University of Toronto and an infectious disease specialist with the Sinai Health System, Toronto.
Healthcare providers should follow ongoing updates to public health guidance, support surveillance where possible, and work with hospital leadership and infection control officials to ensure that pandemic plans are in place, she said.
“They may not be needed in the next few months, but they will be needed,” McGeer said. “We know a lot more about influenza than we did about SARS-CoV-2, so we have more tools to mitigate the impact, but we need to have them ready and know how to use them effectively.”
A version of this article appeared on Medscape.com.
Oxidative Stress Marker May Signal Fracture Risk in T2D
TOPLINE:
Elevated levels of plasma F2-isoprostanes, a reliable marker of oxidative stress, are associated with an increased risk for fractures in older ambulatory patients with type 2 diabetes (T2D) independently of bone density.
METHODOLOGY:
- Patients with T2D face an increased risk for fractures at any given bone mineral density; oxidative stress levels (reflected in circulating F2-isoprostanes), which are elevated in T2D, are associated with other T2D complications, and may weaken bone integrity.
- Researchers analyzed data from an observational cohort study to investigate the association between the levels of circulating F2-isoprostanes and the risk for clinical fractures in older patients with T2D.
- The data included 703 older ambulatory adults (baseline age, 70-79 years; about half White individuals and half Black individuals ; about half men and half women) from the Health, Aging and Body Composition Study, of whom 132 had T2D.
- Plasma F2-isoprostane levels were measured using baseline serum samples; bone turnover markers were also measured including procollagen type 1 N-terminal propeptide, osteocalcin, and C-terminal telopeptide of type 1 collagen.
- Incident clinical fractures were tracked over a follow-up period of up to 17.3 years, with fractures verified through radiology reports.
TAKEAWAY:
- Overall, 25.8% patients in the T2D group and 23.5% adults in the non-diabetes group reported an incident clinical fracture during a mean follow-up period of 6.2 and 8.0 years, respectively.
- In patients with T2D, the risk for incident clinical fracture increased by 93% for every standard deviation increase in the log F2-isoprostane serum levels (hazard ratio [HR], 1.93; 95% CI, 1.26-2.95; P = .002) independently of baseline bone density, medication use, and other risk factors, with no such association reported in individuals without T2D (HR, 0.98; 95% CI, 0.81-1.18; P = .79).
- In the T2D group, elevated plasma F2-isoprostane levels were also associated with a decrease in total hip bone mineral density over 4 years (r = −0.28; P = .008), but not in the non-diabetes group.
- No correlation was found between plasma F2-isoprostane levels and circulating advanced glycoxidation end-products, bone turnover markers, or A1c levels in either group.
IN PRACTICE:
“Oxidative stress in T2D may play an important role in the decline of bone quality and not just bone quantity,” the authors wrote.
SOURCE:
This study was led by Bowen Wang, PhD, Rensselaer Polytechnic Institute, Troy, New York. It was published online in The Journal of Clinical Endocrinology & Metabolism.
LIMITATIONS:
This study was conducted in a well-functioning elderly population with only White and Black participants, which may limit the generalizability of the findings to other age groups or less healthy populations. Additionally, the study did not assess prevalent vertebral fracture risk due to the small sample size.
DISCLOSURES:
This study was supported by the US National Institute on Aging and the Intramural Research Program of the US National Institutes of Health and the Dr and Ms Sands and Sands Family for Orthopaedic Research. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Elevated levels of plasma F2-isoprostanes, a reliable marker of oxidative stress, are associated with an increased risk for fractures in older ambulatory patients with type 2 diabetes (T2D) independently of bone density.
METHODOLOGY:
- Patients with T2D face an increased risk for fractures at any given bone mineral density; oxidative stress levels (reflected in circulating F2-isoprostanes), which are elevated in T2D, are associated with other T2D complications, and may weaken bone integrity.
- Researchers analyzed data from an observational cohort study to investigate the association between the levels of circulating F2-isoprostanes and the risk for clinical fractures in older patients with T2D.
- The data included 703 older ambulatory adults (baseline age, 70-79 years; about half White individuals and half Black individuals ; about half men and half women) from the Health, Aging and Body Composition Study, of whom 132 had T2D.
- Plasma F2-isoprostane levels were measured using baseline serum samples; bone turnover markers were also measured including procollagen type 1 N-terminal propeptide, osteocalcin, and C-terminal telopeptide of type 1 collagen.
- Incident clinical fractures were tracked over a follow-up period of up to 17.3 years, with fractures verified through radiology reports.
TAKEAWAY:
- Overall, 25.8% patients in the T2D group and 23.5% adults in the non-diabetes group reported an incident clinical fracture during a mean follow-up period of 6.2 and 8.0 years, respectively.
- In patients with T2D, the risk for incident clinical fracture increased by 93% for every standard deviation increase in the log F2-isoprostane serum levels (hazard ratio [HR], 1.93; 95% CI, 1.26-2.95; P = .002) independently of baseline bone density, medication use, and other risk factors, with no such association reported in individuals without T2D (HR, 0.98; 95% CI, 0.81-1.18; P = .79).
- In the T2D group, elevated plasma F2-isoprostane levels were also associated with a decrease in total hip bone mineral density over 4 years (r = −0.28; P = .008), but not in the non-diabetes group.
- No correlation was found between plasma F2-isoprostane levels and circulating advanced glycoxidation end-products, bone turnover markers, or A1c levels in either group.
IN PRACTICE:
“Oxidative stress in T2D may play an important role in the decline of bone quality and not just bone quantity,” the authors wrote.
SOURCE:
This study was led by Bowen Wang, PhD, Rensselaer Polytechnic Institute, Troy, New York. It was published online in The Journal of Clinical Endocrinology & Metabolism.
LIMITATIONS:
This study was conducted in a well-functioning elderly population with only White and Black participants, which may limit the generalizability of the findings to other age groups or less healthy populations. Additionally, the study did not assess prevalent vertebral fracture risk due to the small sample size.
DISCLOSURES:
This study was supported by the US National Institute on Aging and the Intramural Research Program of the US National Institutes of Health and the Dr and Ms Sands and Sands Family for Orthopaedic Research. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Elevated levels of plasma F2-isoprostanes, a reliable marker of oxidative stress, are associated with an increased risk for fractures in older ambulatory patients with type 2 diabetes (T2D) independently of bone density.
METHODOLOGY:
- Patients with T2D face an increased risk for fractures at any given bone mineral density; oxidative stress levels (reflected in circulating F2-isoprostanes), which are elevated in T2D, are associated with other T2D complications, and may weaken bone integrity.
- Researchers analyzed data from an observational cohort study to investigate the association between the levels of circulating F2-isoprostanes and the risk for clinical fractures in older patients with T2D.
- The data included 703 older ambulatory adults (baseline age, 70-79 years; about half White individuals and half Black individuals ; about half men and half women) from the Health, Aging and Body Composition Study, of whom 132 had T2D.
- Plasma F2-isoprostane levels were measured using baseline serum samples; bone turnover markers were also measured including procollagen type 1 N-terminal propeptide, osteocalcin, and C-terminal telopeptide of type 1 collagen.
- Incident clinical fractures were tracked over a follow-up period of up to 17.3 years, with fractures verified through radiology reports.
TAKEAWAY:
- Overall, 25.8% patients in the T2D group and 23.5% adults in the non-diabetes group reported an incident clinical fracture during a mean follow-up period of 6.2 and 8.0 years, respectively.
- In patients with T2D, the risk for incident clinical fracture increased by 93% for every standard deviation increase in the log F2-isoprostane serum levels (hazard ratio [HR], 1.93; 95% CI, 1.26-2.95; P = .002) independently of baseline bone density, medication use, and other risk factors, with no such association reported in individuals without T2D (HR, 0.98; 95% CI, 0.81-1.18; P = .79).
- In the T2D group, elevated plasma F2-isoprostane levels were also associated with a decrease in total hip bone mineral density over 4 years (r = −0.28; P = .008), but not in the non-diabetes group.
- No correlation was found between plasma F2-isoprostane levels and circulating advanced glycoxidation end-products, bone turnover markers, or A1c levels in either group.
IN PRACTICE:
“Oxidative stress in T2D may play an important role in the decline of bone quality and not just bone quantity,” the authors wrote.
SOURCE:
This study was led by Bowen Wang, PhD, Rensselaer Polytechnic Institute, Troy, New York. It was published online in The Journal of Clinical Endocrinology & Metabolism.
LIMITATIONS:
This study was conducted in a well-functioning elderly population with only White and Black participants, which may limit the generalizability of the findings to other age groups or less healthy populations. Additionally, the study did not assess prevalent vertebral fracture risk due to the small sample size.
DISCLOSURES:
This study was supported by the US National Institute on Aging and the Intramural Research Program of the US National Institutes of Health and the Dr and Ms Sands and Sands Family for Orthopaedic Research. The authors reported no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
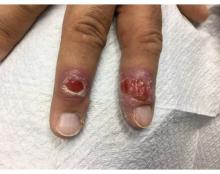
A 58-year-old White male presented with lesions on his index and middle finger for 3 months
Syphilis
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to dermnews@mdedge.com.
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
Syphilis
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to dermnews@mdedge.com.
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
Syphilis
Two biopsies by punch technique were performed; one for pathology and one for tissue culture (fungal and atypical mycobacteria). Tissue cultures showed no growth at 4 and 6 weeks, respectively. The lesions were swabbed for bacterial and viral cultures. Bacterial culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, and group C Streptococcus. Viral culture for herpes simplex virus (HSV) and varicella zoster virus (VZV) was negative. Histopathology confirmed the diagnosis of syphilis. Immunoperoxidase stain was positive for Treponema pallidum, and negative for HSV-1, HSV-2, and VZV. Special stains for PAS, GMS, Fite, and AFB were negative for organisms.
Syphilis, also known as Lues disease, is a contagious, sexually acquired disease caused by the spirochete T pallidum. The skin and mucous membranes are primarily infected. There are primary, secondary, and tertiary stages. In the primary or initial stage of syphilis, a chancre appears, usually 3-4 weeks after infection. The chancre is a painless papule or erosion that progresses to a firm ulceration. Lymphadenopathy may be present. Less often, multiple chancres may be present. Primary chancre on the finger has been reported in the literature, although it is far less common to have extragenital primary syphilis. The incidence ranges from 2% to 10%. Other extragenital areas that can be affected include lips, intraoral lesions, and the anus. Atypical chancres can be formed when other microbial agents are also present. Generally, an untreated chancre will heal spontaneously within a few months.
The patient referred to the department of health for treatment with penicillin G and further workup of sexually transmitted diseases. He was also seen by infectious disease for treatment of the superimposed bacterial infections and treated with an antibiotic regimen.
The case and photo were submitted by Dr. Bilu Martin.
Dr Bilu Martin is a board-certified dermatologist in private practice at Premier Dermatology, MD, in Aventura, Florida. More diagnostic cases are available at mdedge.com/dermatology. To submit a case for possible publication, send an email to dermnews@mdedge.com.
References
Ramoni S et al. Sex Transm Dis. 2010 Jul;37(7):468. doi: 10.1097/OLQ.0b013e3181e2cfac.
Starzycki Z. Br J Vener Dis. 1983 Jun;59(3):169-71. doi: 10.1136/sti.59.3.169.
A 58-year-old White male with no significant past medical history presented with lesions on his right index and middle fingers, which had been present for 3 months. The lesions were painless. The patient has a history of hand dermatitis. Upon questioning, the patient said he had not fished or cleaned fish tanks. He did garden occasionally (no roses). He has been using Neosporin on the lesions. He denied any fever or systemic symptoms and had no lymphadenopathy.
What's your diagnosis?
US Alcohol-Related Deaths Double Over 2 Decades, With Notable Age and Gender Disparities
TOPLINE:
US alcohol-related mortality rates increased from 10.7 to 21.6 per 100,000 between 1999 and 2020, with the largest rise of 3.8-fold observed in adults aged 25-34 years. Women experienced a 2.5-fold increase, while the Midwest region showed a similar rise in mortality rates.
METHODOLOGY:
- Analysis utilized the US Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research to examine alcohol-related mortality trends from 1999 to 2020.
- Researchers analyzed data from a total US population of 180,408,769 people aged 25 to 85+ years in 1999 and 226,635,013 people in 2020.
- International Classification of Diseases, Tenth Revision, codes were used to identify deaths with alcohol attribution, including mental and behavioral disorders, alcoholic organ damage, and alcohol-related poisoning.
TAKEAWAY:
- Overall mortality rates increased from 10.7 (95% CI, 10.6-10.8) per 100,000 in 1999 to 21.6 (95% CI, 21.4-21.8) per 100,000 in 2020, representing a significant twofold increase.
- Adults aged 55-64 years demonstrated both the steepest increase and highest absolute rates in both 1999 and 2020.
- American Indian and Alaska Native individuals experienced the steepest increase and highest absolute rates among all racial groups.
- The West region maintained the highest absolute rates in both 1999 and 2020, despite the Midwest showing the largest increase.
IN PRACTICE:
“Individuals who consume large amounts of alcohol tend to have the highest risks of total mortality as well as deaths from cardiovascular disease. Cardiovascular disease deaths are predominantly due to myocardial infarction and stroke. To mitigate these risks, health providers may wish to implement screening for alcohol use in primary care and other healthcare settings. By providing brief interventions and referrals to treatment, healthcare providers would be able to achieve the early identification of individuals at risk of alcohol-related harm and offer them the support and resources they need to reduce their alcohol consumption,” wrote the authors of the study.
SOURCE:
The study was led by Alexandra Matarazzo, BS, Charles E. Schmidt College of Medicine, Florida Atlantic University, Boca Raton. It was published online in The American Journal of Medicine.
LIMITATIONS:
According to the authors, the cross-sectional nature of the data limits the study to descriptive analysis only, making it suitable for hypothesis generation but not hypothesis testing. While the validity and generalizability within the United States are secure because of the use of complete population data, potential bias and uncontrolled confounding may exist because of different population mixes between the two time points.
DISCLOSURES:
The authors reported no relevant conflicts of interest. One coauthor disclosed serving as an independent scientist in an advisory role to investigators and sponsors as Chair of Data Monitoring Committees for Amgen and UBC, to the Food and Drug Administration, and to Up to Date. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
US alcohol-related mortality rates increased from 10.7 to 21.6 per 100,000 between 1999 and 2020, with the largest rise of 3.8-fold observed in adults aged 25-34 years. Women experienced a 2.5-fold increase, while the Midwest region showed a similar rise in mortality rates.
METHODOLOGY:
- Analysis utilized the US Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research to examine alcohol-related mortality trends from 1999 to 2020.
- Researchers analyzed data from a total US population of 180,408,769 people aged 25 to 85+ years in 1999 and 226,635,013 people in 2020.
- International Classification of Diseases, Tenth Revision, codes were used to identify deaths with alcohol attribution, including mental and behavioral disorders, alcoholic organ damage, and alcohol-related poisoning.
TAKEAWAY:
- Overall mortality rates increased from 10.7 (95% CI, 10.6-10.8) per 100,000 in 1999 to 21.6 (95% CI, 21.4-21.8) per 100,000 in 2020, representing a significant twofold increase.
- Adults aged 55-64 years demonstrated both the steepest increase and highest absolute rates in both 1999 and 2020.
- American Indian and Alaska Native individuals experienced the steepest increase and highest absolute rates among all racial groups.
- The West region maintained the highest absolute rates in both 1999 and 2020, despite the Midwest showing the largest increase.
IN PRACTICE:
“Individuals who consume large amounts of alcohol tend to have the highest risks of total mortality as well as deaths from cardiovascular disease. Cardiovascular disease deaths are predominantly due to myocardial infarction and stroke. To mitigate these risks, health providers may wish to implement screening for alcohol use in primary care and other healthcare settings. By providing brief interventions and referrals to treatment, healthcare providers would be able to achieve the early identification of individuals at risk of alcohol-related harm and offer them the support and resources they need to reduce their alcohol consumption,” wrote the authors of the study.
SOURCE:
The study was led by Alexandra Matarazzo, BS, Charles E. Schmidt College of Medicine, Florida Atlantic University, Boca Raton. It was published online in The American Journal of Medicine.
LIMITATIONS:
According to the authors, the cross-sectional nature of the data limits the study to descriptive analysis only, making it suitable for hypothesis generation but not hypothesis testing. While the validity and generalizability within the United States are secure because of the use of complete population data, potential bias and uncontrolled confounding may exist because of different population mixes between the two time points.
DISCLOSURES:
The authors reported no relevant conflicts of interest. One coauthor disclosed serving as an independent scientist in an advisory role to investigators and sponsors as Chair of Data Monitoring Committees for Amgen and UBC, to the Food and Drug Administration, and to Up to Date. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
US alcohol-related mortality rates increased from 10.7 to 21.6 per 100,000 between 1999 and 2020, with the largest rise of 3.8-fold observed in adults aged 25-34 years. Women experienced a 2.5-fold increase, while the Midwest region showed a similar rise in mortality rates.
METHODOLOGY:
- Analysis utilized the US Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research to examine alcohol-related mortality trends from 1999 to 2020.
- Researchers analyzed data from a total US population of 180,408,769 people aged 25 to 85+ years in 1999 and 226,635,013 people in 2020.
- International Classification of Diseases, Tenth Revision, codes were used to identify deaths with alcohol attribution, including mental and behavioral disorders, alcoholic organ damage, and alcohol-related poisoning.
TAKEAWAY:
- Overall mortality rates increased from 10.7 (95% CI, 10.6-10.8) per 100,000 in 1999 to 21.6 (95% CI, 21.4-21.8) per 100,000 in 2020, representing a significant twofold increase.
- Adults aged 55-64 years demonstrated both the steepest increase and highest absolute rates in both 1999 and 2020.
- American Indian and Alaska Native individuals experienced the steepest increase and highest absolute rates among all racial groups.
- The West region maintained the highest absolute rates in both 1999 and 2020, despite the Midwest showing the largest increase.
IN PRACTICE:
“Individuals who consume large amounts of alcohol tend to have the highest risks of total mortality as well as deaths from cardiovascular disease. Cardiovascular disease deaths are predominantly due to myocardial infarction and stroke. To mitigate these risks, health providers may wish to implement screening for alcohol use in primary care and other healthcare settings. By providing brief interventions and referrals to treatment, healthcare providers would be able to achieve the early identification of individuals at risk of alcohol-related harm and offer them the support and resources they need to reduce their alcohol consumption,” wrote the authors of the study.
SOURCE:
The study was led by Alexandra Matarazzo, BS, Charles E. Schmidt College of Medicine, Florida Atlantic University, Boca Raton. It was published online in The American Journal of Medicine.
LIMITATIONS:
According to the authors, the cross-sectional nature of the data limits the study to descriptive analysis only, making it suitable for hypothesis generation but not hypothesis testing. While the validity and generalizability within the United States are secure because of the use of complete population data, potential bias and uncontrolled confounding may exist because of different population mixes between the two time points.
DISCLOSURES:
The authors reported no relevant conflicts of interest. One coauthor disclosed serving as an independent scientist in an advisory role to investigators and sponsors as Chair of Data Monitoring Committees for Amgen and UBC, to the Food and Drug Administration, and to Up to Date. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Side Effects of GLP-1 Drugs: What Doctors Should Know
Just a few years after some TikTok videos spiked the demand, one in eight US adults has tried Ozempic (semaglutide) or another drug in its class. Glucagon-like peptide 1 (GLP-1) receptor agonist medications have revolutionized obesity medicine.
But they’re not without problems. In the early days of the social media craze, news reports often featured patients whose gastrointestinal side effects sent them to the emergency room (ER).
“It happened a lot then. Patients didn’t want to complain because they were losing weight, and they wound up in the ER with extreme constipation or a small bowel obstruction,” said Caroline Apovian, MD, co-director of the Center for Weight Management and Wellness at Brigham and Women’s Hospital and professor of medicine at Harvard Medical School, Boston.
“But that’s not really happening now,” she added.
Research backs up her assertion: A recent clinical review of studies found that many patients still experience side effects, but only at a mild to moderate level, while the dosage increases — and the unpleasantness tapers with time. Roughly 7% of patients discontinue the medications due to these symptoms.
Here’s what the latest research shows about GLP-1s’ side effects.
Most Common: Gastrointestinal Issues
Depending on the symptom and the specific drug, anywhere from one third to one half of patients will experience some kind of stomach trouble.
- In that clinical review, which looked at studies of three GLP-1 medications — semaglutide (Ozempic, Wegovy, Rybelsus), liraglutide (Saxenda, Victoza), and tirzepatide (Mounjaro, Zepbound) — semaglutide users fared comparatively worse.
- Nausea was reported most frequently — 44.2% of semaglutide users dealt with it, compared with 40.2% for liraglutide and 31% for tirzepatide. Diarrhea, constipation, and vomiting also struck one quarter to one third of semaglutide patients, and slightly fewer for the other two medications.
Apovian finds that careful dosage helps her patients avoid the worst effects.
“We don’t know who’s going to do well and who’s not,” she said. “We start slowly, and usually things go OK.”
If a patient does react poorly, she’ll hold off on increasing the dosage until they acclimate and advise using over-the-counter meds like MiraLAX to address the symptoms.
Few documented severe adverse gastro events appeared in the data, affecting less than 1% of liraglutide and tirzepatide patients and 2.6% of semaglutide users. The majority of these events were gallbladder-related.
Questions About Causation: Depression and Suicidality
About a year ago, a study used 18 years’ worth of data from the US Food and Drug Administration (FDA) Adverse Event Reporting System (FAERS) to examine how often patients reported suicidal ideation and/or depression while using GLP-1 medications. Compared with metformin and insulin, researchers found disproportionate reporting by patients using semaglutide and liraglutide. Other GLP-1 medications didn’t show this effect. The researchers pointed out: These statistics don’t show causation — there’s no clear reason why those two medications were linked to more reports.
Further research has been more reassuring:
- Another study also used FAERS but looked only at data from 2018 to 2022, when usage of these drugs was ramping up, and found no link between suicidal or self-injurious behaviors and GLP-1.
- A recent cohort study, which looked at data from nearly 300,000 people, found that GLP-1 users aren’t at increased risk for death by suicide.
- Both the FDA and the European Medicines Agency have issued statements that the evidence doesn’t support a causal association.
There are several factors at play here. People with obesity and diabetes are more likely to have depression to begin with. And more importantly, even if there is a link, causality remains unclear. For instance, patients who lose weight via bariatric surgery are at increased risk for depression, substance abuse, and self-harm. These symptoms may be related to the weight loss itself, not the medications.
“Some people use food as something other than nutrition. They use food to soothe other psychological issues,” Apovian said. “When that’s taken away, the psychological issues are still there.”
In her practice, she’s seen the risk for mental health issues rise with more substantial weight loss — 50-100 pounds.
This lack of clarity regarding causation means it’s important to perform a detailed patient history before prescribing, so you can monitor more closely with preexisting psychiatric disorders.
Possible Link: Ocular Symptoms
Here, too, the research isn’t definitive but leans toward no clear association. Several studies have looked for a link between GLP-1 and vision-related issues:
- One examined FAERS data and network pharmacology and found semaglutide and lixisenatide were significantly associated with adverse events like blurred vision, visual impairment, and diabetic retinopathy.
- This summer, a cohort study of almost 17,000 people with diabetes or overweight/obesity suggested a link between semaglutide and nonarteritic anterior ischemic optic neuropathy (NAION), a common cause of blindness due to optic nerve damage. The study found “a substantially increased risk of NAION among individuals prescribed semaglutide relative to those prescribed other medications to treat type 2 diabetes and obesity or overweight.”
- But this month, another cohort study with 135,000 participants looked at NAION in people with type 2 diabetes, obesity, or both. It compared results with common non-GLP-1 medications and found just the opposite: No increased risk for NAION.
One drawback with all these studies is that they’re based on large databases rather than randomized controlled trials (RCTs). When researchers focused on RCTs in a 2023 meta-analysis, they found a significant association with only one form of GLP-1, albiglutide — which was withdrawn from the market in 2017. The other six FDA-approved drugs didn’t show a statistically significant link.
Possible Trouble: Pulmonary Aspiration Under Sedation
Earlier this month, the FDA updated labeling for semaglutide, liraglutide, and tirzepatide to include a warning about the risk for aspiration during surgery. While there are no published studies, several case reports have appeared.
GLP-1 medications delay gastric emptying, so even though a patient may have fasted before surgery as usual, some food or liquid may remain. In response to this possibility, a group of professional medical societies issued guidelines for using these medications during the perioperative period. They include:
- Consideration of dosage, symptoms, and other medical conditions: The risk is higher during the escalation phase, and in general, higher doses mean higher risk.
- Potential discontinuation of GLP-1 usage when assessment shows an elevated risk.
- Assessment on the day of the procedure for possible delayed gastric emptying.
- Preoperative dietary modifications, which might include switching to a liquid diet.
Rare: Serious Effects
And then there are the outliers, the frightening issues that make headlines. On their own, none of these are common enough to affect consideration of GLP-1 use:
- Studies in rats suggested an increased risk for thyroid cancer, but subsequent research has found no evidence.
- Colonic ischemia in association with tirzepatide.
- Acute pancreatitis leading to death in association with semaglutide.
- Speaking of pancreatitis, that clinical review of studies did find that both liraglutide and semaglutide led to an elevated risk for pancreatitis, bowel obstruction, and gastroparesis. But the numbers were so small as to be insignificant — for instance, just 0.2% of patients experienced pancreatitis.
Benefits Outweigh Risks
When you lay out these side effects against the countless known benefits of weight loss and blood sugar management — the lower risk for high blood pressure, heart disease, stroke, metabolic syndrome, fatty liver disease, several cancers, and more — the advantages of GLP-1 drugs seem clear. Ultimately, of course, it’s the patient’s decision whether to begin and continue taking any medication for a chronic disease.
Apovian recommends having in-depth conversations before you write that first prescription – she compares the situation to using an antihypertensive drug. If your patient understands potential side effects, they’re more likely to maintain long-term compliance.
“We educate our patients how to use these drugs, indefinitely, if you want to maintain a lower, healthier body weight,” she said. “I don’t see patients who stop using them, but they’re out there. These are people desperate to lose weight, who aren’t given the education to understand we’re treating a disease. It’s not a matter of willpower.”
And once a patient starts taking a GLP-1, monitor them closely, with in-person visits rather than telehealth, while increasing the dosage. If they experience side effects, stay at that level until they ease. And if the patient has a good weight-loss response at a lower dose, stay there. Just because you can go higher, it doesn’t mean you should.
A version of this article first appeared on Medscape.com.
Just a few years after some TikTok videos spiked the demand, one in eight US adults has tried Ozempic (semaglutide) or another drug in its class. Glucagon-like peptide 1 (GLP-1) receptor agonist medications have revolutionized obesity medicine.
But they’re not without problems. In the early days of the social media craze, news reports often featured patients whose gastrointestinal side effects sent them to the emergency room (ER).
“It happened a lot then. Patients didn’t want to complain because they were losing weight, and they wound up in the ER with extreme constipation or a small bowel obstruction,” said Caroline Apovian, MD, co-director of the Center for Weight Management and Wellness at Brigham and Women’s Hospital and professor of medicine at Harvard Medical School, Boston.
“But that’s not really happening now,” she added.
Research backs up her assertion: A recent clinical review of studies found that many patients still experience side effects, but only at a mild to moderate level, while the dosage increases — and the unpleasantness tapers with time. Roughly 7% of patients discontinue the medications due to these symptoms.
Here’s what the latest research shows about GLP-1s’ side effects.
Most Common: Gastrointestinal Issues
Depending on the symptom and the specific drug, anywhere from one third to one half of patients will experience some kind of stomach trouble.
- In that clinical review, which looked at studies of three GLP-1 medications — semaglutide (Ozempic, Wegovy, Rybelsus), liraglutide (Saxenda, Victoza), and tirzepatide (Mounjaro, Zepbound) — semaglutide users fared comparatively worse.
- Nausea was reported most frequently — 44.2% of semaglutide users dealt with it, compared with 40.2% for liraglutide and 31% for tirzepatide. Diarrhea, constipation, and vomiting also struck one quarter to one third of semaglutide patients, and slightly fewer for the other two medications.
Apovian finds that careful dosage helps her patients avoid the worst effects.
“We don’t know who’s going to do well and who’s not,” she said. “We start slowly, and usually things go OK.”
If a patient does react poorly, she’ll hold off on increasing the dosage until they acclimate and advise using over-the-counter meds like MiraLAX to address the symptoms.
Few documented severe adverse gastro events appeared in the data, affecting less than 1% of liraglutide and tirzepatide patients and 2.6% of semaglutide users. The majority of these events were gallbladder-related.
Questions About Causation: Depression and Suicidality
About a year ago, a study used 18 years’ worth of data from the US Food and Drug Administration (FDA) Adverse Event Reporting System (FAERS) to examine how often patients reported suicidal ideation and/or depression while using GLP-1 medications. Compared with metformin and insulin, researchers found disproportionate reporting by patients using semaglutide and liraglutide. Other GLP-1 medications didn’t show this effect. The researchers pointed out: These statistics don’t show causation — there’s no clear reason why those two medications were linked to more reports.
Further research has been more reassuring:
- Another study also used FAERS but looked only at data from 2018 to 2022, when usage of these drugs was ramping up, and found no link between suicidal or self-injurious behaviors and GLP-1.
- A recent cohort study, which looked at data from nearly 300,000 people, found that GLP-1 users aren’t at increased risk for death by suicide.
- Both the FDA and the European Medicines Agency have issued statements that the evidence doesn’t support a causal association.
There are several factors at play here. People with obesity and diabetes are more likely to have depression to begin with. And more importantly, even if there is a link, causality remains unclear. For instance, patients who lose weight via bariatric surgery are at increased risk for depression, substance abuse, and self-harm. These symptoms may be related to the weight loss itself, not the medications.
“Some people use food as something other than nutrition. They use food to soothe other psychological issues,” Apovian said. “When that’s taken away, the psychological issues are still there.”
In her practice, she’s seen the risk for mental health issues rise with more substantial weight loss — 50-100 pounds.
This lack of clarity regarding causation means it’s important to perform a detailed patient history before prescribing, so you can monitor more closely with preexisting psychiatric disorders.
Possible Link: Ocular Symptoms
Here, too, the research isn’t definitive but leans toward no clear association. Several studies have looked for a link between GLP-1 and vision-related issues:
- One examined FAERS data and network pharmacology and found semaglutide and lixisenatide were significantly associated with adverse events like blurred vision, visual impairment, and diabetic retinopathy.
- This summer, a cohort study of almost 17,000 people with diabetes or overweight/obesity suggested a link between semaglutide and nonarteritic anterior ischemic optic neuropathy (NAION), a common cause of blindness due to optic nerve damage. The study found “a substantially increased risk of NAION among individuals prescribed semaglutide relative to those prescribed other medications to treat type 2 diabetes and obesity or overweight.”
- But this month, another cohort study with 135,000 participants looked at NAION in people with type 2 diabetes, obesity, or both. It compared results with common non-GLP-1 medications and found just the opposite: No increased risk for NAION.
One drawback with all these studies is that they’re based on large databases rather than randomized controlled trials (RCTs). When researchers focused on RCTs in a 2023 meta-analysis, they found a significant association with only one form of GLP-1, albiglutide — which was withdrawn from the market in 2017. The other six FDA-approved drugs didn’t show a statistically significant link.
Possible Trouble: Pulmonary Aspiration Under Sedation
Earlier this month, the FDA updated labeling for semaglutide, liraglutide, and tirzepatide to include a warning about the risk for aspiration during surgery. While there are no published studies, several case reports have appeared.
GLP-1 medications delay gastric emptying, so even though a patient may have fasted before surgery as usual, some food or liquid may remain. In response to this possibility, a group of professional medical societies issued guidelines for using these medications during the perioperative period. They include:
- Consideration of dosage, symptoms, and other medical conditions: The risk is higher during the escalation phase, and in general, higher doses mean higher risk.
- Potential discontinuation of GLP-1 usage when assessment shows an elevated risk.
- Assessment on the day of the procedure for possible delayed gastric emptying.
- Preoperative dietary modifications, which might include switching to a liquid diet.
Rare: Serious Effects
And then there are the outliers, the frightening issues that make headlines. On their own, none of these are common enough to affect consideration of GLP-1 use:
- Studies in rats suggested an increased risk for thyroid cancer, but subsequent research has found no evidence.
- Colonic ischemia in association with tirzepatide.
- Acute pancreatitis leading to death in association with semaglutide.
- Speaking of pancreatitis, that clinical review of studies did find that both liraglutide and semaglutide led to an elevated risk for pancreatitis, bowel obstruction, and gastroparesis. But the numbers were so small as to be insignificant — for instance, just 0.2% of patients experienced pancreatitis.
Benefits Outweigh Risks
When you lay out these side effects against the countless known benefits of weight loss and blood sugar management — the lower risk for high blood pressure, heart disease, stroke, metabolic syndrome, fatty liver disease, several cancers, and more — the advantages of GLP-1 drugs seem clear. Ultimately, of course, it’s the patient’s decision whether to begin and continue taking any medication for a chronic disease.
Apovian recommends having in-depth conversations before you write that first prescription – she compares the situation to using an antihypertensive drug. If your patient understands potential side effects, they’re more likely to maintain long-term compliance.
“We educate our patients how to use these drugs, indefinitely, if you want to maintain a lower, healthier body weight,” she said. “I don’t see patients who stop using them, but they’re out there. These are people desperate to lose weight, who aren’t given the education to understand we’re treating a disease. It’s not a matter of willpower.”
And once a patient starts taking a GLP-1, monitor them closely, with in-person visits rather than telehealth, while increasing the dosage. If they experience side effects, stay at that level until they ease. And if the patient has a good weight-loss response at a lower dose, stay there. Just because you can go higher, it doesn’t mean you should.
A version of this article first appeared on Medscape.com.
Just a few years after some TikTok videos spiked the demand, one in eight US adults has tried Ozempic (semaglutide) or another drug in its class. Glucagon-like peptide 1 (GLP-1) receptor agonist medications have revolutionized obesity medicine.
But they’re not without problems. In the early days of the social media craze, news reports often featured patients whose gastrointestinal side effects sent them to the emergency room (ER).
“It happened a lot then. Patients didn’t want to complain because they were losing weight, and they wound up in the ER with extreme constipation or a small bowel obstruction,” said Caroline Apovian, MD, co-director of the Center for Weight Management and Wellness at Brigham and Women’s Hospital and professor of medicine at Harvard Medical School, Boston.
“But that’s not really happening now,” she added.
Research backs up her assertion: A recent clinical review of studies found that many patients still experience side effects, but only at a mild to moderate level, while the dosage increases — and the unpleasantness tapers with time. Roughly 7% of patients discontinue the medications due to these symptoms.
Here’s what the latest research shows about GLP-1s’ side effects.
Most Common: Gastrointestinal Issues
Depending on the symptom and the specific drug, anywhere from one third to one half of patients will experience some kind of stomach trouble.
- In that clinical review, which looked at studies of three GLP-1 medications — semaglutide (Ozempic, Wegovy, Rybelsus), liraglutide (Saxenda, Victoza), and tirzepatide (Mounjaro, Zepbound) — semaglutide users fared comparatively worse.
- Nausea was reported most frequently — 44.2% of semaglutide users dealt with it, compared with 40.2% for liraglutide and 31% for tirzepatide. Diarrhea, constipation, and vomiting also struck one quarter to one third of semaglutide patients, and slightly fewer for the other two medications.
Apovian finds that careful dosage helps her patients avoid the worst effects.
“We don’t know who’s going to do well and who’s not,” she said. “We start slowly, and usually things go OK.”
If a patient does react poorly, she’ll hold off on increasing the dosage until they acclimate and advise using over-the-counter meds like MiraLAX to address the symptoms.
Few documented severe adverse gastro events appeared in the data, affecting less than 1% of liraglutide and tirzepatide patients and 2.6% of semaglutide users. The majority of these events were gallbladder-related.
Questions About Causation: Depression and Suicidality
About a year ago, a study used 18 years’ worth of data from the US Food and Drug Administration (FDA) Adverse Event Reporting System (FAERS) to examine how often patients reported suicidal ideation and/or depression while using GLP-1 medications. Compared with metformin and insulin, researchers found disproportionate reporting by patients using semaglutide and liraglutide. Other GLP-1 medications didn’t show this effect. The researchers pointed out: These statistics don’t show causation — there’s no clear reason why those two medications were linked to more reports.
Further research has been more reassuring:
- Another study also used FAERS but looked only at data from 2018 to 2022, when usage of these drugs was ramping up, and found no link between suicidal or self-injurious behaviors and GLP-1.
- A recent cohort study, which looked at data from nearly 300,000 people, found that GLP-1 users aren’t at increased risk for death by suicide.
- Both the FDA and the European Medicines Agency have issued statements that the evidence doesn’t support a causal association.
There are several factors at play here. People with obesity and diabetes are more likely to have depression to begin with. And more importantly, even if there is a link, causality remains unclear. For instance, patients who lose weight via bariatric surgery are at increased risk for depression, substance abuse, and self-harm. These symptoms may be related to the weight loss itself, not the medications.
“Some people use food as something other than nutrition. They use food to soothe other psychological issues,” Apovian said. “When that’s taken away, the psychological issues are still there.”
In her practice, she’s seen the risk for mental health issues rise with more substantial weight loss — 50-100 pounds.
This lack of clarity regarding causation means it’s important to perform a detailed patient history before prescribing, so you can monitor more closely with preexisting psychiatric disorders.
Possible Link: Ocular Symptoms
Here, too, the research isn’t definitive but leans toward no clear association. Several studies have looked for a link between GLP-1 and vision-related issues:
- One examined FAERS data and network pharmacology and found semaglutide and lixisenatide were significantly associated with adverse events like blurred vision, visual impairment, and diabetic retinopathy.
- This summer, a cohort study of almost 17,000 people with diabetes or overweight/obesity suggested a link between semaglutide and nonarteritic anterior ischemic optic neuropathy (NAION), a common cause of blindness due to optic nerve damage. The study found “a substantially increased risk of NAION among individuals prescribed semaglutide relative to those prescribed other medications to treat type 2 diabetes and obesity or overweight.”
- But this month, another cohort study with 135,000 participants looked at NAION in people with type 2 diabetes, obesity, or both. It compared results with common non-GLP-1 medications and found just the opposite: No increased risk for NAION.
One drawback with all these studies is that they’re based on large databases rather than randomized controlled trials (RCTs). When researchers focused on RCTs in a 2023 meta-analysis, they found a significant association with only one form of GLP-1, albiglutide — which was withdrawn from the market in 2017. The other six FDA-approved drugs didn’t show a statistically significant link.
Possible Trouble: Pulmonary Aspiration Under Sedation
Earlier this month, the FDA updated labeling for semaglutide, liraglutide, and tirzepatide to include a warning about the risk for aspiration during surgery. While there are no published studies, several case reports have appeared.
GLP-1 medications delay gastric emptying, so even though a patient may have fasted before surgery as usual, some food or liquid may remain. In response to this possibility, a group of professional medical societies issued guidelines for using these medications during the perioperative period. They include:
- Consideration of dosage, symptoms, and other medical conditions: The risk is higher during the escalation phase, and in general, higher doses mean higher risk.
- Potential discontinuation of GLP-1 usage when assessment shows an elevated risk.
- Assessment on the day of the procedure for possible delayed gastric emptying.
- Preoperative dietary modifications, which might include switching to a liquid diet.
Rare: Serious Effects
And then there are the outliers, the frightening issues that make headlines. On their own, none of these are common enough to affect consideration of GLP-1 use:
- Studies in rats suggested an increased risk for thyroid cancer, but subsequent research has found no evidence.
- Colonic ischemia in association with tirzepatide.
- Acute pancreatitis leading to death in association with semaglutide.
- Speaking of pancreatitis, that clinical review of studies did find that both liraglutide and semaglutide led to an elevated risk for pancreatitis, bowel obstruction, and gastroparesis. But the numbers were so small as to be insignificant — for instance, just 0.2% of patients experienced pancreatitis.
Benefits Outweigh Risks
When you lay out these side effects against the countless known benefits of weight loss and blood sugar management — the lower risk for high blood pressure, heart disease, stroke, metabolic syndrome, fatty liver disease, several cancers, and more — the advantages of GLP-1 drugs seem clear. Ultimately, of course, it’s the patient’s decision whether to begin and continue taking any medication for a chronic disease.
Apovian recommends having in-depth conversations before you write that first prescription – she compares the situation to using an antihypertensive drug. If your patient understands potential side effects, they’re more likely to maintain long-term compliance.
“We educate our patients how to use these drugs, indefinitely, if you want to maintain a lower, healthier body weight,” she said. “I don’t see patients who stop using them, but they’re out there. These are people desperate to lose weight, who aren’t given the education to understand we’re treating a disease. It’s not a matter of willpower.”
And once a patient starts taking a GLP-1, monitor them closely, with in-person visits rather than telehealth, while increasing the dosage. If they experience side effects, stay at that level until they ease. And if the patient has a good weight-loss response at a lower dose, stay there. Just because you can go higher, it doesn’t mean you should.
A version of this article first appeared on Medscape.com.
Deprescribe Low-Value Meds to Reduce Polypharmacy Harms
VANCOUVER, BRITISH COLUMBIA — While polypharmacy is inevitable for patients with multiple chronic diseases, not all medications improve patient-oriented outcomes, members of the Patients, Experience, Evidence, Research (PEER) team, a group of Canadian primary care professionals who develop evidence-based guidelines, told attendees at the Family Medicine Forum (FMF) 2024.
In a thought-provoking presentation called “Axe the Rx: Deprescribing Chronic Medications with PEER,” the panelists gave examples of medications that may be safely stopped or tapered, particularly for older adults “whose pill bag is heavier than their lunch bag.”
Curbing Cardiovascular Drugs
The 2021 Canadian Cardiovascular Society Guidelines for the Management of Dyslipidemia for the Prevention of Cardiovascular Disease in Adults call for reaching an LDL-C < 1.8 mmol/L in secondary cardiovascular prevention by potentially adding on medical therapies such as proprotein convertase subtilisin/kexin type 9 inhibitors or ezetimibe or both if that target is not reached with the maximal dosage of a statin.
But family physicians do not need to follow this guidance for their patients who have had a myocardial infarction, said Ontario family physician Jennifer Young, MD, a physician advisor in the Canadian College of Family Physicians’ Knowledge Experts and Tools Program.
Treating to below 1.8 mmol/L “means lab testing for the patients,” Young told this news organization. “It means increasing doses [of a statin] to try and get to that level.” If the patient is already on the highest dose of a statin, it means adding other medications that lower cholesterol.
“If that was translating into better outcomes like [preventing] death and another heart attack, then all of that extra effort would be worth it,” said Young. “But we don’t have evidence that it actually does have a benefit for outcomes like death and repeated heart attacks,” compared with putting them on a high dose of a potent statin.
Tapering Opioids
Before placing patients on an opioid taper, clinicians should first assess them for opioid use disorder (OUD), said Jessica Kirkwood, MD, assistant professor of family medicine at the University of Alberta in Edmonton, Canada. She suggested using the Prescription Opioid Misuse Index questionnaire to do so.
Clinicians should be much more careful in initiating a taper with patients with OUD, said Kirkwood. They must ensure that these patients are motivated to discontinue their opioids. “We’re losing 21 Canadians a day to the opioid crisis. We all know that cutting someone off their opioids and potentially having them seek opioids elsewhere through illicit means can be fatal.”
In addition, clinicians should spend more time counseling patients with OUD than those without, Kirkwood continued. They must explain to these patients how they are being tapered (eg, the intervals and doses) and highlight the benefits of a taper, such as reduced constipation. Opioid agonist therapy (such as methadone or buprenorphine) can be considered in these patients.
Some research has pointed to the importance of patient motivation as a factor in the success of opioid tapers, noted Kirkwood.
Deprescribing Benzodiazepines
Benzodiazepine receptor agonists, too, often can be deprescribed. These drugs should not be prescribed to promote sleep on a long-term basis. Yet clinicians commonly encounter patients who have been taking them for more than a year, said pharmacist Betsy Thomas, assistant adjunct professor of family medicine at the University of Alberta.
The medications “are usually fairly effective for the first couple of weeks to about a month, and then the benefits start to decrease, and we start to see more harms,” she said.
Some of the harms that have been associated with continued use of benzodiazepine receptor agonists include delayed reaction time and impaired cognition, which can affect the ability to drive, the risk for falls, and the risk for hip fractures, she noted. Some research suggests that these drugs are not an option for treating insomnia in patients aged 65 years or older.
Clinicians should encourage tapering the use of benzodiazepine receptor agonists to minimize dependence and transition patients to nonpharmacologic approaches such as cognitive behavioral therapy to manage insomnia, she said. A recent study demonstrated the efficacy of the intervention, and Thomas suggested that family physicians visit the mysleepwell.ca website for more information.
Young, Kirkwood, and Thomas reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
VANCOUVER, BRITISH COLUMBIA — While polypharmacy is inevitable for patients with multiple chronic diseases, not all medications improve patient-oriented outcomes, members of the Patients, Experience, Evidence, Research (PEER) team, a group of Canadian primary care professionals who develop evidence-based guidelines, told attendees at the Family Medicine Forum (FMF) 2024.
In a thought-provoking presentation called “Axe the Rx: Deprescribing Chronic Medications with PEER,” the panelists gave examples of medications that may be safely stopped or tapered, particularly for older adults “whose pill bag is heavier than their lunch bag.”
Curbing Cardiovascular Drugs
The 2021 Canadian Cardiovascular Society Guidelines for the Management of Dyslipidemia for the Prevention of Cardiovascular Disease in Adults call for reaching an LDL-C < 1.8 mmol/L in secondary cardiovascular prevention by potentially adding on medical therapies such as proprotein convertase subtilisin/kexin type 9 inhibitors or ezetimibe or both if that target is not reached with the maximal dosage of a statin.
But family physicians do not need to follow this guidance for their patients who have had a myocardial infarction, said Ontario family physician Jennifer Young, MD, a physician advisor in the Canadian College of Family Physicians’ Knowledge Experts and Tools Program.
Treating to below 1.8 mmol/L “means lab testing for the patients,” Young told this news organization. “It means increasing doses [of a statin] to try and get to that level.” If the patient is already on the highest dose of a statin, it means adding other medications that lower cholesterol.
“If that was translating into better outcomes like [preventing] death and another heart attack, then all of that extra effort would be worth it,” said Young. “But we don’t have evidence that it actually does have a benefit for outcomes like death and repeated heart attacks,” compared with putting them on a high dose of a potent statin.
Tapering Opioids
Before placing patients on an opioid taper, clinicians should first assess them for opioid use disorder (OUD), said Jessica Kirkwood, MD, assistant professor of family medicine at the University of Alberta in Edmonton, Canada. She suggested using the Prescription Opioid Misuse Index questionnaire to do so.
Clinicians should be much more careful in initiating a taper with patients with OUD, said Kirkwood. They must ensure that these patients are motivated to discontinue their opioids. “We’re losing 21 Canadians a day to the opioid crisis. We all know that cutting someone off their opioids and potentially having them seek opioids elsewhere through illicit means can be fatal.”
In addition, clinicians should spend more time counseling patients with OUD than those without, Kirkwood continued. They must explain to these patients how they are being tapered (eg, the intervals and doses) and highlight the benefits of a taper, such as reduced constipation. Opioid agonist therapy (such as methadone or buprenorphine) can be considered in these patients.
Some research has pointed to the importance of patient motivation as a factor in the success of opioid tapers, noted Kirkwood.
Deprescribing Benzodiazepines
Benzodiazepine receptor agonists, too, often can be deprescribed. These drugs should not be prescribed to promote sleep on a long-term basis. Yet clinicians commonly encounter patients who have been taking them for more than a year, said pharmacist Betsy Thomas, assistant adjunct professor of family medicine at the University of Alberta.
The medications “are usually fairly effective for the first couple of weeks to about a month, and then the benefits start to decrease, and we start to see more harms,” she said.
Some of the harms that have been associated with continued use of benzodiazepine receptor agonists include delayed reaction time and impaired cognition, which can affect the ability to drive, the risk for falls, and the risk for hip fractures, she noted. Some research suggests that these drugs are not an option for treating insomnia in patients aged 65 years or older.
Clinicians should encourage tapering the use of benzodiazepine receptor agonists to minimize dependence and transition patients to nonpharmacologic approaches such as cognitive behavioral therapy to manage insomnia, she said. A recent study demonstrated the efficacy of the intervention, and Thomas suggested that family physicians visit the mysleepwell.ca website for more information.
Young, Kirkwood, and Thomas reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
VANCOUVER, BRITISH COLUMBIA — While polypharmacy is inevitable for patients with multiple chronic diseases, not all medications improve patient-oriented outcomes, members of the Patients, Experience, Evidence, Research (PEER) team, a group of Canadian primary care professionals who develop evidence-based guidelines, told attendees at the Family Medicine Forum (FMF) 2024.
In a thought-provoking presentation called “Axe the Rx: Deprescribing Chronic Medications with PEER,” the panelists gave examples of medications that may be safely stopped or tapered, particularly for older adults “whose pill bag is heavier than their lunch bag.”
Curbing Cardiovascular Drugs
The 2021 Canadian Cardiovascular Society Guidelines for the Management of Dyslipidemia for the Prevention of Cardiovascular Disease in Adults call for reaching an LDL-C < 1.8 mmol/L in secondary cardiovascular prevention by potentially adding on medical therapies such as proprotein convertase subtilisin/kexin type 9 inhibitors or ezetimibe or both if that target is not reached with the maximal dosage of a statin.
But family physicians do not need to follow this guidance for their patients who have had a myocardial infarction, said Ontario family physician Jennifer Young, MD, a physician advisor in the Canadian College of Family Physicians’ Knowledge Experts and Tools Program.
Treating to below 1.8 mmol/L “means lab testing for the patients,” Young told this news organization. “It means increasing doses [of a statin] to try and get to that level.” If the patient is already on the highest dose of a statin, it means adding other medications that lower cholesterol.
“If that was translating into better outcomes like [preventing] death and another heart attack, then all of that extra effort would be worth it,” said Young. “But we don’t have evidence that it actually does have a benefit for outcomes like death and repeated heart attacks,” compared with putting them on a high dose of a potent statin.
Tapering Opioids
Before placing patients on an opioid taper, clinicians should first assess them for opioid use disorder (OUD), said Jessica Kirkwood, MD, assistant professor of family medicine at the University of Alberta in Edmonton, Canada. She suggested using the Prescription Opioid Misuse Index questionnaire to do so.
Clinicians should be much more careful in initiating a taper with patients with OUD, said Kirkwood. They must ensure that these patients are motivated to discontinue their opioids. “We’re losing 21 Canadians a day to the opioid crisis. We all know that cutting someone off their opioids and potentially having them seek opioids elsewhere through illicit means can be fatal.”
In addition, clinicians should spend more time counseling patients with OUD than those without, Kirkwood continued. They must explain to these patients how they are being tapered (eg, the intervals and doses) and highlight the benefits of a taper, such as reduced constipation. Opioid agonist therapy (such as methadone or buprenorphine) can be considered in these patients.
Some research has pointed to the importance of patient motivation as a factor in the success of opioid tapers, noted Kirkwood.
Deprescribing Benzodiazepines
Benzodiazepine receptor agonists, too, often can be deprescribed. These drugs should not be prescribed to promote sleep on a long-term basis. Yet clinicians commonly encounter patients who have been taking them for more than a year, said pharmacist Betsy Thomas, assistant adjunct professor of family medicine at the University of Alberta.
The medications “are usually fairly effective for the first couple of weeks to about a month, and then the benefits start to decrease, and we start to see more harms,” she said.
Some of the harms that have been associated with continued use of benzodiazepine receptor agonists include delayed reaction time and impaired cognition, which can affect the ability to drive, the risk for falls, and the risk for hip fractures, she noted. Some research suggests that these drugs are not an option for treating insomnia in patients aged 65 years or older.
Clinicians should encourage tapering the use of benzodiazepine receptor agonists to minimize dependence and transition patients to nonpharmacologic approaches such as cognitive behavioral therapy to manage insomnia, she said. A recent study demonstrated the efficacy of the intervention, and Thomas suggested that family physicians visit the mysleepwell.ca website for more information.
Young, Kirkwood, and Thomas reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM FMF 2024
As GLP-1 Use Surges, Clinicians Weigh Benefits and Risks
Rates of overweight and obesity have more than doubled in the United States during the last three decades, according to a new analysis. By 2050, it’s anticipated that 213 million adults (age, > 25 years) and 43 million children and adolescents will have overweight or obesity. The results led authors of a study to describe obesity as having reached a “crisis point” requiring urgent action and interventions.
Are glucagon-like peptide 1 receptor agonists (GLP-1 RAs), originally developed and prescribed for diabetes and now approved for weight loss, the answer?
Their popularity is certainly surging. Between the last 6 months of 2022 vs the last 6 months of 2024, the number of patients prescribed GLP-1 RAs increased by 132.6%. This is also reflected in a shift in public awareness, with a recent survey of US adults finding that 32% of respondents had heard “a lot” about these drugs, up from 19% in 2023.
GLP-1 RAs (including tirzepatide, which targets not only the GLP-1 receptor but also the glucose-dependent insulinotropic polypeptide receptor) have shown efficacy in weight loss. A 2022 review and meta-analysis of 22 trials (17,183 patients) found that 50.2% and 17.5% of those treated with GLP-1 RAs had a ≥ 5% and ≥ 10% weight loss, respectively, compared with placebo. A 2023 review of 41 trials (15,135 patients) found that compared with controls, GLP-1 RAs significantly reduced body weight, body mass index, waist circumference, and waist-to-hip ratio.
“GLP-1 RAs are great medications,” Andres Acosta, MD, PhD, director of the Precision Medicine for Obesity Laboratory, Mayo Clinic, Rochester, Minnesota, told Medscape Medical News. “We’ve been using them for almost two decades. But now there’s excitement about their utility in treating obesity.”
Treating the Four Categories of Obesity
Daniel Drucker, MD, senior investigator at the Lunenfeld-Tanenbaum Research Institute, Mount Sinai Hospital, Toronto, Ontario, Canada, is a pioneer in diabetes treatment and particularly in the development of GLP-1 RAs. Drucker told Medscape Medical News that despite the efficacy and enormous potential of GLP-1 RAs, “we know some people don’t lose much weight when taking these medicines and others don’t feel well and can’t take them.”
The number of individuals who don’t respond to or aren’t able to tolerate GLP-1 RAs “might be small — less than 10% of people who try to take them — but we don’t fully understand the differences in response across different individuals,” Drucker said.
Acosta agreed, adding that it’s “essential for us to identify who will be the best responders, as we do with medications for other conditions, such as cancer and cardiovascular disease.”
Acosta’s group has spent more than a decade engaged in efforts to identify unique characteristics among patients with obesity and has succeeded in identifying four obesity phenotypes.
“What matters in the space of GLP-1 is that using this classification, we can identify the best responders and those who don’t respond.”
The first phenotype, described as “Hungry Gut” (HG), includes patients with abnormal postprandial satiety. “Although they may be satiated at the end of a meal, they have accelerated gastric emptying and therefore feel hungry between meals and want to keep eating,” he said.
There are also patients who experience abnormal satiety during meals. According to Acosta, these are the patients who will return to the table for second and third helpings. “They don’t feel full and continue to eat more and more in a single sitting” — a phenomenon referred to as “Hungry Brain.”
The third phenotype — “Emotional Hunger” — consists of people who are “hedonic” about food or engage in emotional eating behavior, whereas in the fourth group, people have “an abnormal metabolism in which they don’t burn enough calories. They have an inefficient metabolic rate.” This latter phenomenon is called “Slow Burn.”
Acosta and colleagues randomized 312 patients attending a weight management center to phenotype-guided or non–phenotype-guided treatment with anti-obesity medications (phentermine, phentermine/topiramate, bupropion/naltrexone, lorcaserin, and liraglutide). The phenotype-guided approach was associated with a 1.75-fold greater weight loss after 1 year than the non–phenotype-guided approach (mean weight loss, 15.9% vs 9.0%, respectively).
GLP-1 RAs: Not One-Size-Fits-All
Acosta’s group has developed a genetic test that uses patients’ saliva to identify their obesity phenotype, with the aim of predicting the best responders to GLP-1 RAs. The test, MyPhenome genetic obesity test, is licensed by Acosta’s lab and available through Phenomix Sciences.
Acosta and colleagues presented their findings at the American Gastroenterological Association’s 2024 annual meeting regarding a machine-learning gene risk score (ML-GRS) they developed to predict HG, based on saliva and blood samples. Their genetic studies generated a ML-GRS that classified participants with obesity along a continuum from “HG Positive” (HG+) to “HG Negative” (HG−). Compared with the HG− participants, those who were HG+ had superior total body weight loss with semaglutide at 9 and 12 months. When used to predict response, the ML-GRS had an area under the curve of 0.76 (P = .04) and a positive predictive value of 0.95.
According to Acosta, HG+ patients are “the best responders to the GLP-1 RAs, although we don’t yet understand the mechanism of why they have the phenomenon of abnormal postprandial satiety. It may be an abnormal genetic pathway or abnormal secretion of GLP-1. More studies are needed.”
He noted that GLP-1 RAs “might also be helpful with the second [Hungry Brain] category, but these patients do better with phentermine-topiramate,” as demonstrated in a 2023 study conducted by Acosta and colleagues.
His group has also studied which lifestyle interventions are most effective for each phenotype. “When a unique lifestyle intervention targeting each phenotype was applied, patients lost more weight and had greater metabolic improvement,” he reported.
“Treating obesity no longer needs to be trial-and-error, but should be done using precision medicine because one size doesn’t fit all,” Acosta said.
Concerning Side Effects
The popular media has featured stories about individuals who took GLP-1 RAs for weight loss and experienced serious side effects, including a recent account of a British nurse who died after taking tirzepatide. As reported by the BBC, the nurse’s death certificate listed multiple organ failure, septic shock, and pancreatitis as the immediate causes of death, with the “use of prescribed tirzepatide” recorded as a contributing factor. The report went on to note that there were 23 suspected deaths in the United Kingdom tied to semaglutide since 2019.
Beyond brand-name products, there are also risks associated with GLP-1 RAs manufactured by compounding pharmacies. In early November, CNN reported that compounded semaglutide has been linked to at least 10 deaths. Because of a prior shortage of tirzepatide, the US Food and Drug Administration (FDA) had allowed compounding pharmacies to manufacture the drug. In October, the FDA clarified that it won’t take legal action against compounders, even now that the shortage has been resolved.
A pharmacovigilance study using the FDA Adverse Event Reporting System identified “potential safety signals of increased mortality and serious adverse event reporting” associated with certain GLP-1 RAs — especially in younger patients and women (P < .0001 for both groups).
The most common side effects reported with GLP-1 RAs are gastrointestinal events, such as nausea, diarrhea, constipation, and vomiting. Most occur during dose initiation and escalation and wane over the following weeks. However, studies have also reported severe side effects, including a higher risk for pancreatitis, bowel obstruction, and gastroparesis, as well as a significantly higher risk for gallbladder and biliary diseases. In fact, according to one study, patients with diabetes taking GLP-1 RAs reported gastrointestinal-related issues as a “prominent factor” in their decision to discontinue taking these medications.
Several types of cancer are potentially associated with GLP-1 RAs, but findings regarding this potential link have been inconsistent. In a recent review article, Drucker noted there were only inconsistent data linking GLP-1 RAs with thyroid cancer and medullary thyroid cancer and that their potential association with pancreatic has “not been supported by results from randomized controlled trials or real-world data.”
Concerns have been raised about loss of lean mass and muscle strength and function, especially in older individuals with obesity and advanced liver, cardiovascular, or kidney disease. However, as Drucker pointed out in his review article, muscle function may not correlate with the loss of lean mass. In fact, there are “consistent reductions” in lean mass after bariatric surgery, but “little evidence to date for impairment of muscle function.” He added that newer GLP-1 agents under development for obesity treatment are focusing on “developing complementary therapies that preferentially reduce adipose tissue, while sparing lean mass.”
As covered by Medscape Medical News, there have been reports of potential suicidal ideation associated with GLP-1 RAs. This triggered a 2023 review from the European Medicines Agency. However, recent results from a cohort study and a post hoc analysis of randomized controlled trials concluded that there is no evidence that these drugs increase suicidal ideation or behavior.
In early November, the FDA updated the labels for the GLP-1 RAs to include a warning regarding pulmonary aspiration during general anesthesia or deep sedation. Guidance from a group of societies, led by the American Society of Anesthesiologists, contains recommendations regarding nuances of addressing this concern in surgical patients taking these agents.
Not a Standalone Treatment
Marc-Andre Cornier, MD, professor of medicine, James A. Keating Endowed Chair in Diabetes, and director of the Division of Endocrinology, Diabetes and Metabolic Diseases, Department of Medicine, Medical University of South Carolina, Charleston, South Carolina, told Medscape Medical News that GLP-1 RAs should not be viewed as cosmetic interventions but rather as medical treatments, “not only for weight loss but to reverse obesity-associated complications.”
Moreover, they should be used “as an adjunct to lifestyle changes,” emphasized Cornier. “We want our patients to have a high-quality diet with high protein content, fluid, vitamins, and minerals, and we want them to exercise.” Especially with the concern of potential loss of muscle mass with these agents, “resistance exercise might help mitigate that concern.”
Recently published recommendations can assist clinicians in guiding patients taking GLP-1 RAs to optimize nutrition. The recommendations note that patients should be referred to a registered dietitian to “complement and support” treatment with anti-obesity medications.
What Do Patients Want?
Despite the ever-rising popularity of GLP-1 RAs, a new national survey of over 2200 US adults conducted by the Physicians Committee for Responsible Medicine suggests that most Americans don’t want to use them. Among those who wanted to lose weight, almost three-quarters “disagreed” or “strongly disagreed” with the idea of taking a weight-loss injectable, and 68% of those who wanted to lose weight “agreed” or “strongly agreed” that they would be willing to try a plant-based diet, if it could lead to significant weight loss.
Moreover, many individuals treated with GLP-1 RAs discontinue their use, despite the probability of regaining the weight, according to a report that found only 46.3% of GLP-1 users were still taking the medications at 6 months and only 32.3% at 1 year. The authors commented that their real-world findings show a “substantially lower” 1-year persistence rate, compared with the rate reported in clinical trials. They suggest that the financial burden (> $12,000/year) may contribute to discontinuation.
Discontinuation of GLP-1 RAs can lead to worsening cardiometabolic parameters, with a potential increased risk for adverse outcomes; moreover, weight cycling (“yo-yo dieting”) carries its own risks. In light of these concerns, it’s particularly important to select appropriate patients and to determine whether potential short-term therapy has any enduring benefit.
Acosta agreed. “It’s exciting when looking at the data on how to find the best responders and who should make the effort to take these medications — not only in terms of side effects but also in terms of cost and which patients will receive maximum benefits and should be covered by insurance.”
Drucker has served as a consultant or speaker for Altimmune, Amgen, AstraZeneca, Arrowhead, Boehringer Ingelheim, Kallyope, Merck Research Laboratories, Novo Nordisk, Pfizer, and Zealand Pharma. He holds nonexercised options in Kallyope. Mount Sinai Hospital receives research support for investigator-initiated studies in the Drucker laboratory from Amgen, Novo Nordisk, Pfizer, and Zealand Pharma. Gila Therapeutics and Phenomix Sciences have licensed Acosta’s research technologies from University of Florida and Mayo Clinic. Acosta received consultant fees in the last 5 years from Rhythm Pharmaceuticals, Gila Therapeutics, Amgen, General Mills, Regeneron Pharmaceuticals, Boehringer Ingelheim, Novo Nordisk, Currax, Nestlé, Phenomix Sciences, Bausch Health, and Rare Disease. He received funding support from the National Institutes of Health, Vivus Pharmaceuticals, Novo Nordisk, Apollo Endosurgery, Satiogen Pharmaceuticals, Spatz Medical, Rhythm Pharmaceuticals, Regeneron Pharmaceuticals, Boehringer Ingelheim, and Novo Nordisk. In the past, Cornier has served as a consultant for Novo Nordisk.
A version of this article first appeared on Medscape.com.
Rates of overweight and obesity have more than doubled in the United States during the last three decades, according to a new analysis. By 2050, it’s anticipated that 213 million adults (age, > 25 years) and 43 million children and adolescents will have overweight or obesity. The results led authors of a study to describe obesity as having reached a “crisis point” requiring urgent action and interventions.
Are glucagon-like peptide 1 receptor agonists (GLP-1 RAs), originally developed and prescribed for diabetes and now approved for weight loss, the answer?
Their popularity is certainly surging. Between the last 6 months of 2022 vs the last 6 months of 2024, the number of patients prescribed GLP-1 RAs increased by 132.6%. This is also reflected in a shift in public awareness, with a recent survey of US adults finding that 32% of respondents had heard “a lot” about these drugs, up from 19% in 2023.
GLP-1 RAs (including tirzepatide, which targets not only the GLP-1 receptor but also the glucose-dependent insulinotropic polypeptide receptor) have shown efficacy in weight loss. A 2022 review and meta-analysis of 22 trials (17,183 patients) found that 50.2% and 17.5% of those treated with GLP-1 RAs had a ≥ 5% and ≥ 10% weight loss, respectively, compared with placebo. A 2023 review of 41 trials (15,135 patients) found that compared with controls, GLP-1 RAs significantly reduced body weight, body mass index, waist circumference, and waist-to-hip ratio.
“GLP-1 RAs are great medications,” Andres Acosta, MD, PhD, director of the Precision Medicine for Obesity Laboratory, Mayo Clinic, Rochester, Minnesota, told Medscape Medical News. “We’ve been using them for almost two decades. But now there’s excitement about their utility in treating obesity.”
Treating the Four Categories of Obesity
Daniel Drucker, MD, senior investigator at the Lunenfeld-Tanenbaum Research Institute, Mount Sinai Hospital, Toronto, Ontario, Canada, is a pioneer in diabetes treatment and particularly in the development of GLP-1 RAs. Drucker told Medscape Medical News that despite the efficacy and enormous potential of GLP-1 RAs, “we know some people don’t lose much weight when taking these medicines and others don’t feel well and can’t take them.”
The number of individuals who don’t respond to or aren’t able to tolerate GLP-1 RAs “might be small — less than 10% of people who try to take them — but we don’t fully understand the differences in response across different individuals,” Drucker said.
Acosta agreed, adding that it’s “essential for us to identify who will be the best responders, as we do with medications for other conditions, such as cancer and cardiovascular disease.”
Acosta’s group has spent more than a decade engaged in efforts to identify unique characteristics among patients with obesity and has succeeded in identifying four obesity phenotypes.
“What matters in the space of GLP-1 is that using this classification, we can identify the best responders and those who don’t respond.”
The first phenotype, described as “Hungry Gut” (HG), includes patients with abnormal postprandial satiety. “Although they may be satiated at the end of a meal, they have accelerated gastric emptying and therefore feel hungry between meals and want to keep eating,” he said.
There are also patients who experience abnormal satiety during meals. According to Acosta, these are the patients who will return to the table for second and third helpings. “They don’t feel full and continue to eat more and more in a single sitting” — a phenomenon referred to as “Hungry Brain.”
The third phenotype — “Emotional Hunger” — consists of people who are “hedonic” about food or engage in emotional eating behavior, whereas in the fourth group, people have “an abnormal metabolism in which they don’t burn enough calories. They have an inefficient metabolic rate.” This latter phenomenon is called “Slow Burn.”
Acosta and colleagues randomized 312 patients attending a weight management center to phenotype-guided or non–phenotype-guided treatment with anti-obesity medications (phentermine, phentermine/topiramate, bupropion/naltrexone, lorcaserin, and liraglutide). The phenotype-guided approach was associated with a 1.75-fold greater weight loss after 1 year than the non–phenotype-guided approach (mean weight loss, 15.9% vs 9.0%, respectively).
GLP-1 RAs: Not One-Size-Fits-All
Acosta’s group has developed a genetic test that uses patients’ saliva to identify their obesity phenotype, with the aim of predicting the best responders to GLP-1 RAs. The test, MyPhenome genetic obesity test, is licensed by Acosta’s lab and available through Phenomix Sciences.
Acosta and colleagues presented their findings at the American Gastroenterological Association’s 2024 annual meeting regarding a machine-learning gene risk score (ML-GRS) they developed to predict HG, based on saliva and blood samples. Their genetic studies generated a ML-GRS that classified participants with obesity along a continuum from “HG Positive” (HG+) to “HG Negative” (HG−). Compared with the HG− participants, those who were HG+ had superior total body weight loss with semaglutide at 9 and 12 months. When used to predict response, the ML-GRS had an area under the curve of 0.76 (P = .04) and a positive predictive value of 0.95.
According to Acosta, HG+ patients are “the best responders to the GLP-1 RAs, although we don’t yet understand the mechanism of why they have the phenomenon of abnormal postprandial satiety. It may be an abnormal genetic pathway or abnormal secretion of GLP-1. More studies are needed.”
He noted that GLP-1 RAs “might also be helpful with the second [Hungry Brain] category, but these patients do better with phentermine-topiramate,” as demonstrated in a 2023 study conducted by Acosta and colleagues.
His group has also studied which lifestyle interventions are most effective for each phenotype. “When a unique lifestyle intervention targeting each phenotype was applied, patients lost more weight and had greater metabolic improvement,” he reported.
“Treating obesity no longer needs to be trial-and-error, but should be done using precision medicine because one size doesn’t fit all,” Acosta said.
Concerning Side Effects
The popular media has featured stories about individuals who took GLP-1 RAs for weight loss and experienced serious side effects, including a recent account of a British nurse who died after taking tirzepatide. As reported by the BBC, the nurse’s death certificate listed multiple organ failure, septic shock, and pancreatitis as the immediate causes of death, with the “use of prescribed tirzepatide” recorded as a contributing factor. The report went on to note that there were 23 suspected deaths in the United Kingdom tied to semaglutide since 2019.
Beyond brand-name products, there are also risks associated with GLP-1 RAs manufactured by compounding pharmacies. In early November, CNN reported that compounded semaglutide has been linked to at least 10 deaths. Because of a prior shortage of tirzepatide, the US Food and Drug Administration (FDA) had allowed compounding pharmacies to manufacture the drug. In October, the FDA clarified that it won’t take legal action against compounders, even now that the shortage has been resolved.
A pharmacovigilance study using the FDA Adverse Event Reporting System identified “potential safety signals of increased mortality and serious adverse event reporting” associated with certain GLP-1 RAs — especially in younger patients and women (P < .0001 for both groups).
The most common side effects reported with GLP-1 RAs are gastrointestinal events, such as nausea, diarrhea, constipation, and vomiting. Most occur during dose initiation and escalation and wane over the following weeks. However, studies have also reported severe side effects, including a higher risk for pancreatitis, bowel obstruction, and gastroparesis, as well as a significantly higher risk for gallbladder and biliary diseases. In fact, according to one study, patients with diabetes taking GLP-1 RAs reported gastrointestinal-related issues as a “prominent factor” in their decision to discontinue taking these medications.
Several types of cancer are potentially associated with GLP-1 RAs, but findings regarding this potential link have been inconsistent. In a recent review article, Drucker noted there were only inconsistent data linking GLP-1 RAs with thyroid cancer and medullary thyroid cancer and that their potential association with pancreatic has “not been supported by results from randomized controlled trials or real-world data.”
Concerns have been raised about loss of lean mass and muscle strength and function, especially in older individuals with obesity and advanced liver, cardiovascular, or kidney disease. However, as Drucker pointed out in his review article, muscle function may not correlate with the loss of lean mass. In fact, there are “consistent reductions” in lean mass after bariatric surgery, but “little evidence to date for impairment of muscle function.” He added that newer GLP-1 agents under development for obesity treatment are focusing on “developing complementary therapies that preferentially reduce adipose tissue, while sparing lean mass.”
As covered by Medscape Medical News, there have been reports of potential suicidal ideation associated with GLP-1 RAs. This triggered a 2023 review from the European Medicines Agency. However, recent results from a cohort study and a post hoc analysis of randomized controlled trials concluded that there is no evidence that these drugs increase suicidal ideation or behavior.
In early November, the FDA updated the labels for the GLP-1 RAs to include a warning regarding pulmonary aspiration during general anesthesia or deep sedation. Guidance from a group of societies, led by the American Society of Anesthesiologists, contains recommendations regarding nuances of addressing this concern in surgical patients taking these agents.
Not a Standalone Treatment
Marc-Andre Cornier, MD, professor of medicine, James A. Keating Endowed Chair in Diabetes, and director of the Division of Endocrinology, Diabetes and Metabolic Diseases, Department of Medicine, Medical University of South Carolina, Charleston, South Carolina, told Medscape Medical News that GLP-1 RAs should not be viewed as cosmetic interventions but rather as medical treatments, “not only for weight loss but to reverse obesity-associated complications.”
Moreover, they should be used “as an adjunct to lifestyle changes,” emphasized Cornier. “We want our patients to have a high-quality diet with high protein content, fluid, vitamins, and minerals, and we want them to exercise.” Especially with the concern of potential loss of muscle mass with these agents, “resistance exercise might help mitigate that concern.”
Recently published recommendations can assist clinicians in guiding patients taking GLP-1 RAs to optimize nutrition. The recommendations note that patients should be referred to a registered dietitian to “complement and support” treatment with anti-obesity medications.
What Do Patients Want?
Despite the ever-rising popularity of GLP-1 RAs, a new national survey of over 2200 US adults conducted by the Physicians Committee for Responsible Medicine suggests that most Americans don’t want to use them. Among those who wanted to lose weight, almost three-quarters “disagreed” or “strongly disagreed” with the idea of taking a weight-loss injectable, and 68% of those who wanted to lose weight “agreed” or “strongly agreed” that they would be willing to try a plant-based diet, if it could lead to significant weight loss.
Moreover, many individuals treated with GLP-1 RAs discontinue their use, despite the probability of regaining the weight, according to a report that found only 46.3% of GLP-1 users were still taking the medications at 6 months and only 32.3% at 1 year. The authors commented that their real-world findings show a “substantially lower” 1-year persistence rate, compared with the rate reported in clinical trials. They suggest that the financial burden (> $12,000/year) may contribute to discontinuation.
Discontinuation of GLP-1 RAs can lead to worsening cardiometabolic parameters, with a potential increased risk for adverse outcomes; moreover, weight cycling (“yo-yo dieting”) carries its own risks. In light of these concerns, it’s particularly important to select appropriate patients and to determine whether potential short-term therapy has any enduring benefit.
Acosta agreed. “It’s exciting when looking at the data on how to find the best responders and who should make the effort to take these medications — not only in terms of side effects but also in terms of cost and which patients will receive maximum benefits and should be covered by insurance.”
Drucker has served as a consultant or speaker for Altimmune, Amgen, AstraZeneca, Arrowhead, Boehringer Ingelheim, Kallyope, Merck Research Laboratories, Novo Nordisk, Pfizer, and Zealand Pharma. He holds nonexercised options in Kallyope. Mount Sinai Hospital receives research support for investigator-initiated studies in the Drucker laboratory from Amgen, Novo Nordisk, Pfizer, and Zealand Pharma. Gila Therapeutics and Phenomix Sciences have licensed Acosta’s research technologies from University of Florida and Mayo Clinic. Acosta received consultant fees in the last 5 years from Rhythm Pharmaceuticals, Gila Therapeutics, Amgen, General Mills, Regeneron Pharmaceuticals, Boehringer Ingelheim, Novo Nordisk, Currax, Nestlé, Phenomix Sciences, Bausch Health, and Rare Disease. He received funding support from the National Institutes of Health, Vivus Pharmaceuticals, Novo Nordisk, Apollo Endosurgery, Satiogen Pharmaceuticals, Spatz Medical, Rhythm Pharmaceuticals, Regeneron Pharmaceuticals, Boehringer Ingelheim, and Novo Nordisk. In the past, Cornier has served as a consultant for Novo Nordisk.
A version of this article first appeared on Medscape.com.
Rates of overweight and obesity have more than doubled in the United States during the last three decades, according to a new analysis. By 2050, it’s anticipated that 213 million adults (age, > 25 years) and 43 million children and adolescents will have overweight or obesity. The results led authors of a study to describe obesity as having reached a “crisis point” requiring urgent action and interventions.
Are glucagon-like peptide 1 receptor agonists (GLP-1 RAs), originally developed and prescribed for diabetes and now approved for weight loss, the answer?
Their popularity is certainly surging. Between the last 6 months of 2022 vs the last 6 months of 2024, the number of patients prescribed GLP-1 RAs increased by 132.6%. This is also reflected in a shift in public awareness, with a recent survey of US adults finding that 32% of respondents had heard “a lot” about these drugs, up from 19% in 2023.
GLP-1 RAs (including tirzepatide, which targets not only the GLP-1 receptor but also the glucose-dependent insulinotropic polypeptide receptor) have shown efficacy in weight loss. A 2022 review and meta-analysis of 22 trials (17,183 patients) found that 50.2% and 17.5% of those treated with GLP-1 RAs had a ≥ 5% and ≥ 10% weight loss, respectively, compared with placebo. A 2023 review of 41 trials (15,135 patients) found that compared with controls, GLP-1 RAs significantly reduced body weight, body mass index, waist circumference, and waist-to-hip ratio.
“GLP-1 RAs are great medications,” Andres Acosta, MD, PhD, director of the Precision Medicine for Obesity Laboratory, Mayo Clinic, Rochester, Minnesota, told Medscape Medical News. “We’ve been using them for almost two decades. But now there’s excitement about their utility in treating obesity.”
Treating the Four Categories of Obesity
Daniel Drucker, MD, senior investigator at the Lunenfeld-Tanenbaum Research Institute, Mount Sinai Hospital, Toronto, Ontario, Canada, is a pioneer in diabetes treatment and particularly in the development of GLP-1 RAs. Drucker told Medscape Medical News that despite the efficacy and enormous potential of GLP-1 RAs, “we know some people don’t lose much weight when taking these medicines and others don’t feel well and can’t take them.”
The number of individuals who don’t respond to or aren’t able to tolerate GLP-1 RAs “might be small — less than 10% of people who try to take them — but we don’t fully understand the differences in response across different individuals,” Drucker said.
Acosta agreed, adding that it’s “essential for us to identify who will be the best responders, as we do with medications for other conditions, such as cancer and cardiovascular disease.”
Acosta’s group has spent more than a decade engaged in efforts to identify unique characteristics among patients with obesity and has succeeded in identifying four obesity phenotypes.
“What matters in the space of GLP-1 is that using this classification, we can identify the best responders and those who don’t respond.”
The first phenotype, described as “Hungry Gut” (HG), includes patients with abnormal postprandial satiety. “Although they may be satiated at the end of a meal, they have accelerated gastric emptying and therefore feel hungry between meals and want to keep eating,” he said.
There are also patients who experience abnormal satiety during meals. According to Acosta, these are the patients who will return to the table for second and third helpings. “They don’t feel full and continue to eat more and more in a single sitting” — a phenomenon referred to as “Hungry Brain.”
The third phenotype — “Emotional Hunger” — consists of people who are “hedonic” about food or engage in emotional eating behavior, whereas in the fourth group, people have “an abnormal metabolism in which they don’t burn enough calories. They have an inefficient metabolic rate.” This latter phenomenon is called “Slow Burn.”
Acosta and colleagues randomized 312 patients attending a weight management center to phenotype-guided or non–phenotype-guided treatment with anti-obesity medications (phentermine, phentermine/topiramate, bupropion/naltrexone, lorcaserin, and liraglutide). The phenotype-guided approach was associated with a 1.75-fold greater weight loss after 1 year than the non–phenotype-guided approach (mean weight loss, 15.9% vs 9.0%, respectively).
GLP-1 RAs: Not One-Size-Fits-All
Acosta’s group has developed a genetic test that uses patients’ saliva to identify their obesity phenotype, with the aim of predicting the best responders to GLP-1 RAs. The test, MyPhenome genetic obesity test, is licensed by Acosta’s lab and available through Phenomix Sciences.
Acosta and colleagues presented their findings at the American Gastroenterological Association’s 2024 annual meeting regarding a machine-learning gene risk score (ML-GRS) they developed to predict HG, based on saliva and blood samples. Their genetic studies generated a ML-GRS that classified participants with obesity along a continuum from “HG Positive” (HG+) to “HG Negative” (HG−). Compared with the HG− participants, those who were HG+ had superior total body weight loss with semaglutide at 9 and 12 months. When used to predict response, the ML-GRS had an area under the curve of 0.76 (P = .04) and a positive predictive value of 0.95.
According to Acosta, HG+ patients are “the best responders to the GLP-1 RAs, although we don’t yet understand the mechanism of why they have the phenomenon of abnormal postprandial satiety. It may be an abnormal genetic pathway or abnormal secretion of GLP-1. More studies are needed.”
He noted that GLP-1 RAs “might also be helpful with the second [Hungry Brain] category, but these patients do better with phentermine-topiramate,” as demonstrated in a 2023 study conducted by Acosta and colleagues.
His group has also studied which lifestyle interventions are most effective for each phenotype. “When a unique lifestyle intervention targeting each phenotype was applied, patients lost more weight and had greater metabolic improvement,” he reported.
“Treating obesity no longer needs to be trial-and-error, but should be done using precision medicine because one size doesn’t fit all,” Acosta said.
Concerning Side Effects
The popular media has featured stories about individuals who took GLP-1 RAs for weight loss and experienced serious side effects, including a recent account of a British nurse who died after taking tirzepatide. As reported by the BBC, the nurse’s death certificate listed multiple organ failure, septic shock, and pancreatitis as the immediate causes of death, with the “use of prescribed tirzepatide” recorded as a contributing factor. The report went on to note that there were 23 suspected deaths in the United Kingdom tied to semaglutide since 2019.
Beyond brand-name products, there are also risks associated with GLP-1 RAs manufactured by compounding pharmacies. In early November, CNN reported that compounded semaglutide has been linked to at least 10 deaths. Because of a prior shortage of tirzepatide, the US Food and Drug Administration (FDA) had allowed compounding pharmacies to manufacture the drug. In October, the FDA clarified that it won’t take legal action against compounders, even now that the shortage has been resolved.
A pharmacovigilance study using the FDA Adverse Event Reporting System identified “potential safety signals of increased mortality and serious adverse event reporting” associated with certain GLP-1 RAs — especially in younger patients and women (P < .0001 for both groups).
The most common side effects reported with GLP-1 RAs are gastrointestinal events, such as nausea, diarrhea, constipation, and vomiting. Most occur during dose initiation and escalation and wane over the following weeks. However, studies have also reported severe side effects, including a higher risk for pancreatitis, bowel obstruction, and gastroparesis, as well as a significantly higher risk for gallbladder and biliary diseases. In fact, according to one study, patients with diabetes taking GLP-1 RAs reported gastrointestinal-related issues as a “prominent factor” in their decision to discontinue taking these medications.
Several types of cancer are potentially associated with GLP-1 RAs, but findings regarding this potential link have been inconsistent. In a recent review article, Drucker noted there were only inconsistent data linking GLP-1 RAs with thyroid cancer and medullary thyroid cancer and that their potential association with pancreatic has “not been supported by results from randomized controlled trials or real-world data.”
Concerns have been raised about loss of lean mass and muscle strength and function, especially in older individuals with obesity and advanced liver, cardiovascular, or kidney disease. However, as Drucker pointed out in his review article, muscle function may not correlate with the loss of lean mass. In fact, there are “consistent reductions” in lean mass after bariatric surgery, but “little evidence to date for impairment of muscle function.” He added that newer GLP-1 agents under development for obesity treatment are focusing on “developing complementary therapies that preferentially reduce adipose tissue, while sparing lean mass.”
As covered by Medscape Medical News, there have been reports of potential suicidal ideation associated with GLP-1 RAs. This triggered a 2023 review from the European Medicines Agency. However, recent results from a cohort study and a post hoc analysis of randomized controlled trials concluded that there is no evidence that these drugs increase suicidal ideation or behavior.
In early November, the FDA updated the labels for the GLP-1 RAs to include a warning regarding pulmonary aspiration during general anesthesia or deep sedation. Guidance from a group of societies, led by the American Society of Anesthesiologists, contains recommendations regarding nuances of addressing this concern in surgical patients taking these agents.
Not a Standalone Treatment
Marc-Andre Cornier, MD, professor of medicine, James A. Keating Endowed Chair in Diabetes, and director of the Division of Endocrinology, Diabetes and Metabolic Diseases, Department of Medicine, Medical University of South Carolina, Charleston, South Carolina, told Medscape Medical News that GLP-1 RAs should not be viewed as cosmetic interventions but rather as medical treatments, “not only for weight loss but to reverse obesity-associated complications.”
Moreover, they should be used “as an adjunct to lifestyle changes,” emphasized Cornier. “We want our patients to have a high-quality diet with high protein content, fluid, vitamins, and minerals, and we want them to exercise.” Especially with the concern of potential loss of muscle mass with these agents, “resistance exercise might help mitigate that concern.”
Recently published recommendations can assist clinicians in guiding patients taking GLP-1 RAs to optimize nutrition. The recommendations note that patients should be referred to a registered dietitian to “complement and support” treatment with anti-obesity medications.
What Do Patients Want?
Despite the ever-rising popularity of GLP-1 RAs, a new national survey of over 2200 US adults conducted by the Physicians Committee for Responsible Medicine suggests that most Americans don’t want to use them. Among those who wanted to lose weight, almost three-quarters “disagreed” or “strongly disagreed” with the idea of taking a weight-loss injectable, and 68% of those who wanted to lose weight “agreed” or “strongly agreed” that they would be willing to try a plant-based diet, if it could lead to significant weight loss.
Moreover, many individuals treated with GLP-1 RAs discontinue their use, despite the probability of regaining the weight, according to a report that found only 46.3% of GLP-1 users were still taking the medications at 6 months and only 32.3% at 1 year. The authors commented that their real-world findings show a “substantially lower” 1-year persistence rate, compared with the rate reported in clinical trials. They suggest that the financial burden (> $12,000/year) may contribute to discontinuation.
Discontinuation of GLP-1 RAs can lead to worsening cardiometabolic parameters, with a potential increased risk for adverse outcomes; moreover, weight cycling (“yo-yo dieting”) carries its own risks. In light of these concerns, it’s particularly important to select appropriate patients and to determine whether potential short-term therapy has any enduring benefit.
Acosta agreed. “It’s exciting when looking at the data on how to find the best responders and who should make the effort to take these medications — not only in terms of side effects but also in terms of cost and which patients will receive maximum benefits and should be covered by insurance.”
Drucker has served as a consultant or speaker for Altimmune, Amgen, AstraZeneca, Arrowhead, Boehringer Ingelheim, Kallyope, Merck Research Laboratories, Novo Nordisk, Pfizer, and Zealand Pharma. He holds nonexercised options in Kallyope. Mount Sinai Hospital receives research support for investigator-initiated studies in the Drucker laboratory from Amgen, Novo Nordisk, Pfizer, and Zealand Pharma. Gila Therapeutics and Phenomix Sciences have licensed Acosta’s research technologies from University of Florida and Mayo Clinic. Acosta received consultant fees in the last 5 years from Rhythm Pharmaceuticals, Gila Therapeutics, Amgen, General Mills, Regeneron Pharmaceuticals, Boehringer Ingelheim, Novo Nordisk, Currax, Nestlé, Phenomix Sciences, Bausch Health, and Rare Disease. He received funding support from the National Institutes of Health, Vivus Pharmaceuticals, Novo Nordisk, Apollo Endosurgery, Satiogen Pharmaceuticals, Spatz Medical, Rhythm Pharmaceuticals, Regeneron Pharmaceuticals, Boehringer Ingelheim, and Novo Nordisk. In the past, Cornier has served as a consultant for Novo Nordisk.
A version of this article first appeared on Medscape.com.
Vaping Linked to Higher Risk of Blurred Vision & Eye Pain
TOPLINE:
Adults who use electronic cigarettes (e-cigarettes/vapes) had more than double the risk for developing uveitis than nonusers, with elevated risks persisting for up to 4 years after initial use. This increased risk was observed across all age groups and affected both men and women as well as various ethnic groups.
METHODOLOGY:
- Researchers used the TriNetX global database, which contains data from over 100 million patients across the United States, Europe, the Middle East, and Africa, to examine the risk for developing uveitis among e-cigarette users.
- 419,325 e-cigarette users over the age of 18 years (mean age, 51.41 years; 48.65% women) were included, based on diagnosis codes for vaping and unspecified nicotine dependence.
- The e-cigarette users were propensity score–matched to non-e-cigarette-users.
- People were excluded if they had comorbid conditions that might have influenced the risk for uveitis.
- The primary outcome measure was the first-time encounter diagnosis of uveitis using diagnosis codes for iridocyclitis, unspecified choroidal inflammation, posterior cyclitis, choroidal degeneration, retinal vasculitis, and pan-uveitis.
TAKEAWAY:
- E-cigarette users had a significantly higher risk for developing uveitis than nonusers (hazard ratio [HR], 2.53; 95% CI, 2.33-2.76 ), for iridocyclitis (HR, 2.59), unspecified chorioretinal inflammation (HR, 2.34), and retinal vasculitis (HR, 1.95).
- This increased risk for uveitis was observed across all age groups, affecting all genders and patients from Asian, Black or African American, and White ethnic backgrounds.
- The risk for uveitis increased as early as within 7 days after smoking an e-cigarettes (HR, 6.35) and was present even at 4 years (HR, 2.58) after initial use.
- A higher risk for uveitis was observed among individuals with a history of both e-cigarette and traditional cigarette use than among those who used traditional cigarettes only (HR, 1.39).
IN PRACTICE:
“This study has real-world implications as clinicians caring for patients with e-cigarette history should be aware of the potentially increased risk of new-onset uveitis,” the authors wrote.
SOURCE:
The study was led by Alan Y. Hsu, MD, from the Department of Ophthalmology at China Medical University Hospital in Taichung, Taiwan, and was published online on November 12, 2024, in Ophthalmology.
LIMITATIONS:
The retrospective nature of the study limited the determination of direct causality between e-cigarette use and the risk for uveitis. The study lacked information on the duration and quantity of e-cigarette exposure, which may have impacted the findings. Moreover, researchers could not isolate the effect of secondhand exposure to vaping or traditional cigarettes.
DISCLOSURES:
Study authors reported no relevant financial disclosures.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
TOPLINE:
Adults who use electronic cigarettes (e-cigarettes/vapes) had more than double the risk for developing uveitis than nonusers, with elevated risks persisting for up to 4 years after initial use. This increased risk was observed across all age groups and affected both men and women as well as various ethnic groups.
METHODOLOGY:
- Researchers used the TriNetX global database, which contains data from over 100 million patients across the United States, Europe, the Middle East, and Africa, to examine the risk for developing uveitis among e-cigarette users.
- 419,325 e-cigarette users over the age of 18 years (mean age, 51.41 years; 48.65% women) were included, based on diagnosis codes for vaping and unspecified nicotine dependence.
- The e-cigarette users were propensity score–matched to non-e-cigarette-users.
- People were excluded if they had comorbid conditions that might have influenced the risk for uveitis.
- The primary outcome measure was the first-time encounter diagnosis of uveitis using diagnosis codes for iridocyclitis, unspecified choroidal inflammation, posterior cyclitis, choroidal degeneration, retinal vasculitis, and pan-uveitis.
TAKEAWAY:
- E-cigarette users had a significantly higher risk for developing uveitis than nonusers (hazard ratio [HR], 2.53; 95% CI, 2.33-2.76 ), for iridocyclitis (HR, 2.59), unspecified chorioretinal inflammation (HR, 2.34), and retinal vasculitis (HR, 1.95).
- This increased risk for uveitis was observed across all age groups, affecting all genders and patients from Asian, Black or African American, and White ethnic backgrounds.
- The risk for uveitis increased as early as within 7 days after smoking an e-cigarettes (HR, 6.35) and was present even at 4 years (HR, 2.58) after initial use.
- A higher risk for uveitis was observed among individuals with a history of both e-cigarette and traditional cigarette use than among those who used traditional cigarettes only (HR, 1.39).
IN PRACTICE:
“This study has real-world implications as clinicians caring for patients with e-cigarette history should be aware of the potentially increased risk of new-onset uveitis,” the authors wrote.
SOURCE:
The study was led by Alan Y. Hsu, MD, from the Department of Ophthalmology at China Medical University Hospital in Taichung, Taiwan, and was published online on November 12, 2024, in Ophthalmology.
LIMITATIONS:
The retrospective nature of the study limited the determination of direct causality between e-cigarette use and the risk for uveitis. The study lacked information on the duration and quantity of e-cigarette exposure, which may have impacted the findings. Moreover, researchers could not isolate the effect of secondhand exposure to vaping or traditional cigarettes.
DISCLOSURES:
Study authors reported no relevant financial disclosures.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
TOPLINE:
Adults who use electronic cigarettes (e-cigarettes/vapes) had more than double the risk for developing uveitis than nonusers, with elevated risks persisting for up to 4 years after initial use. This increased risk was observed across all age groups and affected both men and women as well as various ethnic groups.
METHODOLOGY:
- Researchers used the TriNetX global database, which contains data from over 100 million patients across the United States, Europe, the Middle East, and Africa, to examine the risk for developing uveitis among e-cigarette users.
- 419,325 e-cigarette users over the age of 18 years (mean age, 51.41 years; 48.65% women) were included, based on diagnosis codes for vaping and unspecified nicotine dependence.
- The e-cigarette users were propensity score–matched to non-e-cigarette-users.
- People were excluded if they had comorbid conditions that might have influenced the risk for uveitis.
- The primary outcome measure was the first-time encounter diagnosis of uveitis using diagnosis codes for iridocyclitis, unspecified choroidal inflammation, posterior cyclitis, choroidal degeneration, retinal vasculitis, and pan-uveitis.
TAKEAWAY:
- E-cigarette users had a significantly higher risk for developing uveitis than nonusers (hazard ratio [HR], 2.53; 95% CI, 2.33-2.76 ), for iridocyclitis (HR, 2.59), unspecified chorioretinal inflammation (HR, 2.34), and retinal vasculitis (HR, 1.95).
- This increased risk for uveitis was observed across all age groups, affecting all genders and patients from Asian, Black or African American, and White ethnic backgrounds.
- The risk for uveitis increased as early as within 7 days after smoking an e-cigarettes (HR, 6.35) and was present even at 4 years (HR, 2.58) after initial use.
- A higher risk for uveitis was observed among individuals with a history of both e-cigarette and traditional cigarette use than among those who used traditional cigarettes only (HR, 1.39).
IN PRACTICE:
“This study has real-world implications as clinicians caring for patients with e-cigarette history should be aware of the potentially increased risk of new-onset uveitis,” the authors wrote.
SOURCE:
The study was led by Alan Y. Hsu, MD, from the Department of Ophthalmology at China Medical University Hospital in Taichung, Taiwan, and was published online on November 12, 2024, in Ophthalmology.
LIMITATIONS:
The retrospective nature of the study limited the determination of direct causality between e-cigarette use and the risk for uveitis. The study lacked information on the duration and quantity of e-cigarette exposure, which may have impacted the findings. Moreover, researchers could not isolate the effect of secondhand exposure to vaping or traditional cigarettes.
DISCLOSURES:
Study authors reported no relevant financial disclosures.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
Could Probiotics Tuned to Reduce Intestinal Urate Counter Gout?
Efforts to combat hyperuricemia may find help from gut microbes, according to Dylan Dodd, MD, PhD, who spoke at the annual research symposium of the Gout, Hyperuricemia, and Crystal-Associated Disease Network.
Dodd is an assistant professor of pathology and microbiology and immunology at Stanford University, Palo Alto, California, where he studies novel metabolic pathways in microbes. “The idea is that we can leverage these novel pathways that microbes have as therapeutics to promote human health, and in particular for this meeting today, we’re focused on hyperuricemia and how microbes that break down purines may actually have a role as urate-lowering therapies,” Dodd said during his presentation.
Specifically, he highlighted the fact that some microbes found in the gut break down purines as a food source, producing both energy and molecular building blocks for their own use. Dietary purines, left intact, can otherwise be absorbed and metabolized by the body to produce urate.
Nucleic acids like DNA and RNA in the diet are first broken down by enzymes produced in the pancreas, resulting in purine nucleosides, which in turn are believed to be the source of purines absorbed in the small intestine and eventually into circulation, according to Dodd. “I really view urate in the intestine as being in equilibrium between being secreted into the lumen but also being reabsorbed, and specifically, as it pertains to microbes in the gut. If the microbes degrade the urate, then it will limit its reabsorption, and that could increase net excretion,” Dodd said.
There is evidence that some strains of Lactobacillus species, which are the most important group in the human gut, can metabolize purine nucleosides, he said. In recent years, researchers have screened for Lactobacillus species capable of metabolizing purine nucleosides. The research shows some strain-to-strain variation, but most are proprietary, making it impossible to conduct follow-up research. A small number of human trials have suggested efficacy, but they have generally been conducted in few patients with mixed results. “Overall, I think it’s promising that these lactobacilli probiotics could potentially be used as urate-lowering therapies,” Dodd said.
Aside from direct metabolism of purines, Dodd’s group has identified an additional pathway that some microbes can use to break down urate into short-chain fatty acids. His group cultured various purine nucleosides with various bacterial strains, including two Lactobacillus strains, under anaerobic conditions. The Lactobacillus strains did not degrade urate, but some bacterial species did. The group also found that Lactobacillus could convert nucleosides, including those derived from purines, into the smaller nucleobase compounds, but they did not consume the resultant purines. Some other types of bacteria consumed all purines “voraciously,” according to Dodd, and his team is working to identify the bacterial genetic pathways that drive the metabolic pathways.
Such studies may open up various therapeutic pathways, he said. One is to employ Lactobacillus probiotics to convert purine nucleosides to their nucleobases, which could reduce absorption in the small intestine. Other bacteria could potentially be used to convert urate produced by paracellular reabsorption to short-chain fatty acids, which have potential benefits through their anti-inflammatory properties. Finally, probiotics could be engineered to degrade urate produced in the intestine.
Dodd noted that probiotics would have the advantage of high patient acceptance and are generally regarded as safe. Some existing products might have purine-degrading capabilities but haven’t been tested, he said. However, there is strain-to-strain variation and the probiotic formulas would likely need to be optimized to reduce nucleobases. On the other hand, bacteria that degrade urate are likely safe since they have been found in the guts of healthy individuals. However, there are still potential safety concerns, and it is unknown if they could withstand the harsh conditions of the upper gastrointestinal tract or if they would remain active even in the presence of oxygen found in the small intestine, he said.
During the Q&A period after his talk, Dodd was asked whether fructose consumption could suppress the function of anaerobic bacteria that naturally degrade purine. “When people talk about fructose-induced hyperuricemia, they talk about the ATP degradation in fructose metabolism in the liver or small intestine, [but] they never talk about this potential pathway in the gut,” the questioner said.
Dodd responded that his group found that some carbohydrates suppress urate degradation in some bacterial strains. “It’s certainly a possible mechanism that increased fructose intake could suppress microbial urate degradation in the gut, and that could contribute to hyperuricemia, but obviously more studies need to be done,” he said.
Another audience member wondered if antibiotic use could be tied to gout risk and whether serum urate levels might rise after antibiotic use. “Do you have any data on serum urate before and after antibiotic use, where you might expect to see changes which might support your hypothesis?” she asked. Dodd said that the group had done a retrospective analysis of data from Stanford’s medical records and did not find a change in serum urate after antibiotic exposure. However, a controlled feeding study of healthy individuals who later received antibiotics showed a large increase in urate levels, but the study did not include plasma samples. “It’s a really good question, and we hope to be able to follow that up,” he said.
Dodd disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Efforts to combat hyperuricemia may find help from gut microbes, according to Dylan Dodd, MD, PhD, who spoke at the annual research symposium of the Gout, Hyperuricemia, and Crystal-Associated Disease Network.
Dodd is an assistant professor of pathology and microbiology and immunology at Stanford University, Palo Alto, California, where he studies novel metabolic pathways in microbes. “The idea is that we can leverage these novel pathways that microbes have as therapeutics to promote human health, and in particular for this meeting today, we’re focused on hyperuricemia and how microbes that break down purines may actually have a role as urate-lowering therapies,” Dodd said during his presentation.
Specifically, he highlighted the fact that some microbes found in the gut break down purines as a food source, producing both energy and molecular building blocks for their own use. Dietary purines, left intact, can otherwise be absorbed and metabolized by the body to produce urate.
Nucleic acids like DNA and RNA in the diet are first broken down by enzymes produced in the pancreas, resulting in purine nucleosides, which in turn are believed to be the source of purines absorbed in the small intestine and eventually into circulation, according to Dodd. “I really view urate in the intestine as being in equilibrium between being secreted into the lumen but also being reabsorbed, and specifically, as it pertains to microbes in the gut. If the microbes degrade the urate, then it will limit its reabsorption, and that could increase net excretion,” Dodd said.
There is evidence that some strains of Lactobacillus species, which are the most important group in the human gut, can metabolize purine nucleosides, he said. In recent years, researchers have screened for Lactobacillus species capable of metabolizing purine nucleosides. The research shows some strain-to-strain variation, but most are proprietary, making it impossible to conduct follow-up research. A small number of human trials have suggested efficacy, but they have generally been conducted in few patients with mixed results. “Overall, I think it’s promising that these lactobacilli probiotics could potentially be used as urate-lowering therapies,” Dodd said.
Aside from direct metabolism of purines, Dodd’s group has identified an additional pathway that some microbes can use to break down urate into short-chain fatty acids. His group cultured various purine nucleosides with various bacterial strains, including two Lactobacillus strains, under anaerobic conditions. The Lactobacillus strains did not degrade urate, but some bacterial species did. The group also found that Lactobacillus could convert nucleosides, including those derived from purines, into the smaller nucleobase compounds, but they did not consume the resultant purines. Some other types of bacteria consumed all purines “voraciously,” according to Dodd, and his team is working to identify the bacterial genetic pathways that drive the metabolic pathways.
Such studies may open up various therapeutic pathways, he said. One is to employ Lactobacillus probiotics to convert purine nucleosides to their nucleobases, which could reduce absorption in the small intestine. Other bacteria could potentially be used to convert urate produced by paracellular reabsorption to short-chain fatty acids, which have potential benefits through their anti-inflammatory properties. Finally, probiotics could be engineered to degrade urate produced in the intestine.
Dodd noted that probiotics would have the advantage of high patient acceptance and are generally regarded as safe. Some existing products might have purine-degrading capabilities but haven’t been tested, he said. However, there is strain-to-strain variation and the probiotic formulas would likely need to be optimized to reduce nucleobases. On the other hand, bacteria that degrade urate are likely safe since they have been found in the guts of healthy individuals. However, there are still potential safety concerns, and it is unknown if they could withstand the harsh conditions of the upper gastrointestinal tract or if they would remain active even in the presence of oxygen found in the small intestine, he said.
During the Q&A period after his talk, Dodd was asked whether fructose consumption could suppress the function of anaerobic bacteria that naturally degrade purine. “When people talk about fructose-induced hyperuricemia, they talk about the ATP degradation in fructose metabolism in the liver or small intestine, [but] they never talk about this potential pathway in the gut,” the questioner said.
Dodd responded that his group found that some carbohydrates suppress urate degradation in some bacterial strains. “It’s certainly a possible mechanism that increased fructose intake could suppress microbial urate degradation in the gut, and that could contribute to hyperuricemia, but obviously more studies need to be done,” he said.
Another audience member wondered if antibiotic use could be tied to gout risk and whether serum urate levels might rise after antibiotic use. “Do you have any data on serum urate before and after antibiotic use, where you might expect to see changes which might support your hypothesis?” she asked. Dodd said that the group had done a retrospective analysis of data from Stanford’s medical records and did not find a change in serum urate after antibiotic exposure. However, a controlled feeding study of healthy individuals who later received antibiotics showed a large increase in urate levels, but the study did not include plasma samples. “It’s a really good question, and we hope to be able to follow that up,” he said.
Dodd disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Efforts to combat hyperuricemia may find help from gut microbes, according to Dylan Dodd, MD, PhD, who spoke at the annual research symposium of the Gout, Hyperuricemia, and Crystal-Associated Disease Network.
Dodd is an assistant professor of pathology and microbiology and immunology at Stanford University, Palo Alto, California, where he studies novel metabolic pathways in microbes. “The idea is that we can leverage these novel pathways that microbes have as therapeutics to promote human health, and in particular for this meeting today, we’re focused on hyperuricemia and how microbes that break down purines may actually have a role as urate-lowering therapies,” Dodd said during his presentation.
Specifically, he highlighted the fact that some microbes found in the gut break down purines as a food source, producing both energy and molecular building blocks for their own use. Dietary purines, left intact, can otherwise be absorbed and metabolized by the body to produce urate.
Nucleic acids like DNA and RNA in the diet are first broken down by enzymes produced in the pancreas, resulting in purine nucleosides, which in turn are believed to be the source of purines absorbed in the small intestine and eventually into circulation, according to Dodd. “I really view urate in the intestine as being in equilibrium between being secreted into the lumen but also being reabsorbed, and specifically, as it pertains to microbes in the gut. If the microbes degrade the urate, then it will limit its reabsorption, and that could increase net excretion,” Dodd said.
There is evidence that some strains of Lactobacillus species, which are the most important group in the human gut, can metabolize purine nucleosides, he said. In recent years, researchers have screened for Lactobacillus species capable of metabolizing purine nucleosides. The research shows some strain-to-strain variation, but most are proprietary, making it impossible to conduct follow-up research. A small number of human trials have suggested efficacy, but they have generally been conducted in few patients with mixed results. “Overall, I think it’s promising that these lactobacilli probiotics could potentially be used as urate-lowering therapies,” Dodd said.
Aside from direct metabolism of purines, Dodd’s group has identified an additional pathway that some microbes can use to break down urate into short-chain fatty acids. His group cultured various purine nucleosides with various bacterial strains, including two Lactobacillus strains, under anaerobic conditions. The Lactobacillus strains did not degrade urate, but some bacterial species did. The group also found that Lactobacillus could convert nucleosides, including those derived from purines, into the smaller nucleobase compounds, but they did not consume the resultant purines. Some other types of bacteria consumed all purines “voraciously,” according to Dodd, and his team is working to identify the bacterial genetic pathways that drive the metabolic pathways.
Such studies may open up various therapeutic pathways, he said. One is to employ Lactobacillus probiotics to convert purine nucleosides to their nucleobases, which could reduce absorption in the small intestine. Other bacteria could potentially be used to convert urate produced by paracellular reabsorption to short-chain fatty acids, which have potential benefits through their anti-inflammatory properties. Finally, probiotics could be engineered to degrade urate produced in the intestine.
Dodd noted that probiotics would have the advantage of high patient acceptance and are generally regarded as safe. Some existing products might have purine-degrading capabilities but haven’t been tested, he said. However, there is strain-to-strain variation and the probiotic formulas would likely need to be optimized to reduce nucleobases. On the other hand, bacteria that degrade urate are likely safe since they have been found in the guts of healthy individuals. However, there are still potential safety concerns, and it is unknown if they could withstand the harsh conditions of the upper gastrointestinal tract or if they would remain active even in the presence of oxygen found in the small intestine, he said.
During the Q&A period after his talk, Dodd was asked whether fructose consumption could suppress the function of anaerobic bacteria that naturally degrade purine. “When people talk about fructose-induced hyperuricemia, they talk about the ATP degradation in fructose metabolism in the liver or small intestine, [but] they never talk about this potential pathway in the gut,” the questioner said.
Dodd responded that his group found that some carbohydrates suppress urate degradation in some bacterial strains. “It’s certainly a possible mechanism that increased fructose intake could suppress microbial urate degradation in the gut, and that could contribute to hyperuricemia, but obviously more studies need to be done,” he said.
Another audience member wondered if antibiotic use could be tied to gout risk and whether serum urate levels might rise after antibiotic use. “Do you have any data on serum urate before and after antibiotic use, where you might expect to see changes which might support your hypothesis?” she asked. Dodd said that the group had done a retrospective analysis of data from Stanford’s medical records and did not find a change in serum urate after antibiotic exposure. However, a controlled feeding study of healthy individuals who later received antibiotics showed a large increase in urate levels, but the study did not include plasma samples. “It’s a really good question, and we hope to be able to follow that up,” he said.
Dodd disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
FROM G-CAN 2024
ASH 2024 Myeloma Studies: My Top 10 Picks
First, let me place my selected studies in context by acknowledging my biases. As a clinician, I’m prone to choosing clinical rather than basic science or translational work — even if translational work might well end up exerting a pivotal impact on practice in the future. And now — in no particular order — here are my picks:
IFM 2017-03 Phase 3 Study
Frail patients are underrepresented in most myeloma studies, yet in this randomized trial for newly diagnosed myeloma, exclusively frail patients were enrolled. The trial compared daratumumab/lenalidomide to lenalidomide/dexamethasone, and the most recent follow/up shows a progression-free survival (PFS) (48.5 vs 21 months) and overall survival (OS) (not reached vs 36 months) benefit to daratumumab/lenalidomide. What I see in practice is that anti-CD38 monoclonal antibodies are the best-tolerated drugs in this space and should be the backbone of any regimen for frail patients. Steroids should be omitted as early as possible. Future trials may optimize what to give in addition to the anti-CD38 therapy, and how to adapt/escalate therapy to frailty and clinical status, as lenalidomide remains difficult for such patients to tolerate.
AQUILA Study
This is a randomized, phase 3 comparison of daratumumab to observation for patients with smoldering myeloma. The endpoint was PFS. For context, similar studies done in asymptomatic CLL have shown improved PFS, but not OS, and the authors of such studies have concluded that improvement in PFS alone should not justify a change in approach.
This study shows that daratumumab can improve laboratory markers and reduce progression (60-month PFS rates of 63.1% for daratumumab vs 40.8% with observation). However, several important caveats remain. The protocol only mandated spine/pelvis MRI imaging, not whole-body MRI imaging, and such imaging was only performed once a year, which may not be frequent enough to catch lesions at an earlier stage. These details have important implications, as previous research shows that up to half of lesions can be missed by doing only a spine MRI, as opposed to a whole-body MRI.
All of this means that had more comprehensive imaging been done, many more patients may have been diagnosed with myeloma. Such patients may have been undertreated, and single agent daratumumab, with a response rate of just 63%, may not have been enough. Conversely, some patients may also have been overtreated using this approach, as the protocol allowed patients who had been diagnosed with smoldering myeloma up to 5 years earlier to be enrolled. Many of these people could have had indolent disease for years prior to enrollment and may not have ever progressed.
Further information is needed to help us understand this study better. What was the nature of the progression events: asymptomatic lab changes or morbid end organ damage? Was daratumumab given when patients in the control arm progressed to myeloma? My concern is that if patients in the control arm do not universally receive modern daratumumab-containing therapies when they develop myeloma, then an overall survival advantage may be shown simply because patients in the intervention arm are getting a good drug earlier in the disease, while those in the control arm are not getting a good drug at all. Nevertheless, despite these limitations, it is likely this trial will lead to regulatory approval of daratumumab in this space, and lots of discussions from patients and clinicians alike.
Extended Follow-Up of Anito-Cel in its First In-Human study
Two chimeric antigen receptor therapy (CAR-T) products are currently approved for myeloma. Cilta-cel is clearly effective but is associated with problematic late-onset neurological toxicities. Ide-cel appears much less effective. There is clearly a need for a product that is both effective and safe.
Anito-cel has two relevant abstracts this meeting that show much promise. Extended follow-up of anito-cel from its first in human study shows a promising 27-month PFS of 52%, and with no cases of delayed neurotoxicity. I also eagerly await further information from the registrational single-arm study of anti-cel being presented at ASH 2024, which should (hopefully) lead to its accelerated approval.
Screening for Myeloma for all People With Vertebral Fractures Likely Unnecessary
This elegant study of over 9,000 people with vertebral fractures shows that absolute risks for myeloma were 0.43% and 0.63% in women and men with grade 2-3 fractures, respectively, indicating that there is likely little benefit in evaluating asymptomatic individuals with incidentally discovered vertebral fractures for myeloma, unless other features are present. Spread the word.
Further Information on Cevostamab, Another Bispecific Option
We do need effective treatments for targets beyond just BCMA and GPRC5D. Cevostamab, a bispecific targeting FCRH5, represents another option, with updated data on 167 patients. With an overall response rate of 43% (duration of response, 10 months), and a response rate of about 30% in those with prior bispecific exposure, this data helps us contextualize expected benefits as we look forward to the eventual approval of this drug. The efficacy is relatively modest in those who have already progressed on bispecifics, but cevostamab would still be a welcome addition to our arsenal.
Is GPRC5D a Better Target for Car T Rather Than Bispecifics?
Our currently available GPRC5D bispecific (talquetamab) leads to high rates of skin, oral, and nail toxicity. This drug can also bring significant weight loss. These side effects make me consider that continuous targeting of GPRC5D through a bispecific may not be ideal, and that GPRC5D may be better as a one-time CAR T target. At ASH 2024, we will have 15-month follow-up data from BMS-986393, a GPRC5D CAR T. Response rates for this heavily pretreated population (76% of whom had triple refractory disease) were at 87%, with a median PFS of 14.5 months. Only 6% of patients experienced treatment-related weight loss, and nail (19%), skin (30%), and oral (31%) toxicities were relatively low. I look forward to updated data, as well as data on the resolution of the toxicities seen.
Daratumumab, a Game-Changer for AL Amyloidosis
A truly effective drug given early can change the natural history of disease, even if patients in the control arm only receive the drug later. A case in point is daratumumab. The 5-year survival rate was 76.1% for the daratumumab/cyclophosphamide/bortezomib/dexamethasone arm and 64.7% for cyclophosphamide/bortezomib/dexamethasone arm. This happened despite the fact that 67% of the control arm patients (among those who received therapy) went on to receive daratumumab later in the disease course.
Understanding how SMM Progresses to MM
We often hear that we should treat SMM and not just watch carefully because fractures may suddenly happen, or a patient may end up on dialysis. What this retrospective study tells us that amongst 427 patients with SMM, 42 had progression to myeloma, and amongst those 42, only 1 developed renal dysfunction (unclear if this resolved), and only 1 had lytic lesions that were symptomatic. The remainder were all asymptomatic lab and imaging changes. This is a retrospective study, and one should assume that follow-up was thus highly variable. It does not appear that diffusion weighted whole-body MRI imaging (our most sensitive imaging test) was employed universally or very frequently. Nevertheless, these powerful findings reassure us that, with close observation, morbidity is unlikely. Our group has designed a prospective study incorporating frequent diffusion weighted whole body MRI imaging to formally test this hypothesis (SPOTLIGHT, NCT06212323).
The Underperformance of Daratumumab/Lenalidomide/Dexamethasone in the Real World
At every major meeting I am reminded of the disconnect between real-world efficacy and clinical trial efficacy. Case in point: In this Austrian experience, daratumumab/lenalidomide/dexamethasone led to a PFS of 22.7 months vs 61.9 months in the MAIA trial of daratumumab/lenalidomide/dexamethasone. Such a sobering difference! And if you think this is an isolated experience, even in a US real-world cohort, consider that in a recently published comparative study dara/len/dex underperformed, although the time to next treatment or death was longer (37.8 months).
Delayed Neurotoxicity may not be Just a Consequence of high tumor burden
We currently think that some of the scariest side effects of cilta-cel, such as delayed neurotoxicity, may be a consequence of a high number of cancer cells and may be prevented by better disease control at the time of infusion. This study, a sobering analysis of 52 patients with delayed neurotoxicity occurring after CAR T, included 8 patients (15%) who were not heavily pretreated, and all had less than 5% plasma cells at the time of infusion. None of these patients had extramedullary disease. This result worries me, especially because cilta-cel is being studied and is poised for future approval in earlier line settings. It suggests that this toxicity may not always be a product of disease burden, contrary to our current belief.
I will be paying close attention to these 10 myeloma studies at ASH 2024, where I look forward to meeting you and learning more.Dr. Mohyuddin is assistant professor in the multiple myeloma program at the Huntsman Cancer Institute at the University of Utah, Salt Lake City.
First, let me place my selected studies in context by acknowledging my biases. As a clinician, I’m prone to choosing clinical rather than basic science or translational work — even if translational work might well end up exerting a pivotal impact on practice in the future. And now — in no particular order — here are my picks:
IFM 2017-03 Phase 3 Study
Frail patients are underrepresented in most myeloma studies, yet in this randomized trial for newly diagnosed myeloma, exclusively frail patients were enrolled. The trial compared daratumumab/lenalidomide to lenalidomide/dexamethasone, and the most recent follow/up shows a progression-free survival (PFS) (48.5 vs 21 months) and overall survival (OS) (not reached vs 36 months) benefit to daratumumab/lenalidomide. What I see in practice is that anti-CD38 monoclonal antibodies are the best-tolerated drugs in this space and should be the backbone of any regimen for frail patients. Steroids should be omitted as early as possible. Future trials may optimize what to give in addition to the anti-CD38 therapy, and how to adapt/escalate therapy to frailty and clinical status, as lenalidomide remains difficult for such patients to tolerate.
AQUILA Study
This is a randomized, phase 3 comparison of daratumumab to observation for patients with smoldering myeloma. The endpoint was PFS. For context, similar studies done in asymptomatic CLL have shown improved PFS, but not OS, and the authors of such studies have concluded that improvement in PFS alone should not justify a change in approach.
This study shows that daratumumab can improve laboratory markers and reduce progression (60-month PFS rates of 63.1% for daratumumab vs 40.8% with observation). However, several important caveats remain. The protocol only mandated spine/pelvis MRI imaging, not whole-body MRI imaging, and such imaging was only performed once a year, which may not be frequent enough to catch lesions at an earlier stage. These details have important implications, as previous research shows that up to half of lesions can be missed by doing only a spine MRI, as opposed to a whole-body MRI.
All of this means that had more comprehensive imaging been done, many more patients may have been diagnosed with myeloma. Such patients may have been undertreated, and single agent daratumumab, with a response rate of just 63%, may not have been enough. Conversely, some patients may also have been overtreated using this approach, as the protocol allowed patients who had been diagnosed with smoldering myeloma up to 5 years earlier to be enrolled. Many of these people could have had indolent disease for years prior to enrollment and may not have ever progressed.
Further information is needed to help us understand this study better. What was the nature of the progression events: asymptomatic lab changes or morbid end organ damage? Was daratumumab given when patients in the control arm progressed to myeloma? My concern is that if patients in the control arm do not universally receive modern daratumumab-containing therapies when they develop myeloma, then an overall survival advantage may be shown simply because patients in the intervention arm are getting a good drug earlier in the disease, while those in the control arm are not getting a good drug at all. Nevertheless, despite these limitations, it is likely this trial will lead to regulatory approval of daratumumab in this space, and lots of discussions from patients and clinicians alike.
Extended Follow-Up of Anito-Cel in its First In-Human study
Two chimeric antigen receptor therapy (CAR-T) products are currently approved for myeloma. Cilta-cel is clearly effective but is associated with problematic late-onset neurological toxicities. Ide-cel appears much less effective. There is clearly a need for a product that is both effective and safe.
Anito-cel has two relevant abstracts this meeting that show much promise. Extended follow-up of anito-cel from its first in human study shows a promising 27-month PFS of 52%, and with no cases of delayed neurotoxicity. I also eagerly await further information from the registrational single-arm study of anti-cel being presented at ASH 2024, which should (hopefully) lead to its accelerated approval.
Screening for Myeloma for all People With Vertebral Fractures Likely Unnecessary
This elegant study of over 9,000 people with vertebral fractures shows that absolute risks for myeloma were 0.43% and 0.63% in women and men with grade 2-3 fractures, respectively, indicating that there is likely little benefit in evaluating asymptomatic individuals with incidentally discovered vertebral fractures for myeloma, unless other features are present. Spread the word.
Further Information on Cevostamab, Another Bispecific Option
We do need effective treatments for targets beyond just BCMA and GPRC5D. Cevostamab, a bispecific targeting FCRH5, represents another option, with updated data on 167 patients. With an overall response rate of 43% (duration of response, 10 months), and a response rate of about 30% in those with prior bispecific exposure, this data helps us contextualize expected benefits as we look forward to the eventual approval of this drug. The efficacy is relatively modest in those who have already progressed on bispecifics, but cevostamab would still be a welcome addition to our arsenal.
Is GPRC5D a Better Target for Car T Rather Than Bispecifics?
Our currently available GPRC5D bispecific (talquetamab) leads to high rates of skin, oral, and nail toxicity. This drug can also bring significant weight loss. These side effects make me consider that continuous targeting of GPRC5D through a bispecific may not be ideal, and that GPRC5D may be better as a one-time CAR T target. At ASH 2024, we will have 15-month follow-up data from BMS-986393, a GPRC5D CAR T. Response rates for this heavily pretreated population (76% of whom had triple refractory disease) were at 87%, with a median PFS of 14.5 months. Only 6% of patients experienced treatment-related weight loss, and nail (19%), skin (30%), and oral (31%) toxicities were relatively low. I look forward to updated data, as well as data on the resolution of the toxicities seen.
Daratumumab, a Game-Changer for AL Amyloidosis
A truly effective drug given early can change the natural history of disease, even if patients in the control arm only receive the drug later. A case in point is daratumumab. The 5-year survival rate was 76.1% for the daratumumab/cyclophosphamide/bortezomib/dexamethasone arm and 64.7% for cyclophosphamide/bortezomib/dexamethasone arm. This happened despite the fact that 67% of the control arm patients (among those who received therapy) went on to receive daratumumab later in the disease course.
Understanding how SMM Progresses to MM
We often hear that we should treat SMM and not just watch carefully because fractures may suddenly happen, or a patient may end up on dialysis. What this retrospective study tells us that amongst 427 patients with SMM, 42 had progression to myeloma, and amongst those 42, only 1 developed renal dysfunction (unclear if this resolved), and only 1 had lytic lesions that were symptomatic. The remainder were all asymptomatic lab and imaging changes. This is a retrospective study, and one should assume that follow-up was thus highly variable. It does not appear that diffusion weighted whole-body MRI imaging (our most sensitive imaging test) was employed universally or very frequently. Nevertheless, these powerful findings reassure us that, with close observation, morbidity is unlikely. Our group has designed a prospective study incorporating frequent diffusion weighted whole body MRI imaging to formally test this hypothesis (SPOTLIGHT, NCT06212323).
The Underperformance of Daratumumab/Lenalidomide/Dexamethasone in the Real World
At every major meeting I am reminded of the disconnect between real-world efficacy and clinical trial efficacy. Case in point: In this Austrian experience, daratumumab/lenalidomide/dexamethasone led to a PFS of 22.7 months vs 61.9 months in the MAIA trial of daratumumab/lenalidomide/dexamethasone. Such a sobering difference! And if you think this is an isolated experience, even in a US real-world cohort, consider that in a recently published comparative study dara/len/dex underperformed, although the time to next treatment or death was longer (37.8 months).
Delayed Neurotoxicity may not be Just a Consequence of high tumor burden
We currently think that some of the scariest side effects of cilta-cel, such as delayed neurotoxicity, may be a consequence of a high number of cancer cells and may be prevented by better disease control at the time of infusion. This study, a sobering analysis of 52 patients with delayed neurotoxicity occurring after CAR T, included 8 patients (15%) who were not heavily pretreated, and all had less than 5% plasma cells at the time of infusion. None of these patients had extramedullary disease. This result worries me, especially because cilta-cel is being studied and is poised for future approval in earlier line settings. It suggests that this toxicity may not always be a product of disease burden, contrary to our current belief.
I will be paying close attention to these 10 myeloma studies at ASH 2024, where I look forward to meeting you and learning more.Dr. Mohyuddin is assistant professor in the multiple myeloma program at the Huntsman Cancer Institute at the University of Utah, Salt Lake City.
First, let me place my selected studies in context by acknowledging my biases. As a clinician, I’m prone to choosing clinical rather than basic science or translational work — even if translational work might well end up exerting a pivotal impact on practice in the future. And now — in no particular order — here are my picks:
IFM 2017-03 Phase 3 Study
Frail patients are underrepresented in most myeloma studies, yet in this randomized trial for newly diagnosed myeloma, exclusively frail patients were enrolled. The trial compared daratumumab/lenalidomide to lenalidomide/dexamethasone, and the most recent follow/up shows a progression-free survival (PFS) (48.5 vs 21 months) and overall survival (OS) (not reached vs 36 months) benefit to daratumumab/lenalidomide. What I see in practice is that anti-CD38 monoclonal antibodies are the best-tolerated drugs in this space and should be the backbone of any regimen for frail patients. Steroids should be omitted as early as possible. Future trials may optimize what to give in addition to the anti-CD38 therapy, and how to adapt/escalate therapy to frailty and clinical status, as lenalidomide remains difficult for such patients to tolerate.
AQUILA Study
This is a randomized, phase 3 comparison of daratumumab to observation for patients with smoldering myeloma. The endpoint was PFS. For context, similar studies done in asymptomatic CLL have shown improved PFS, but not OS, and the authors of such studies have concluded that improvement in PFS alone should not justify a change in approach.
This study shows that daratumumab can improve laboratory markers and reduce progression (60-month PFS rates of 63.1% for daratumumab vs 40.8% with observation). However, several important caveats remain. The protocol only mandated spine/pelvis MRI imaging, not whole-body MRI imaging, and such imaging was only performed once a year, which may not be frequent enough to catch lesions at an earlier stage. These details have important implications, as previous research shows that up to half of lesions can be missed by doing only a spine MRI, as opposed to a whole-body MRI.
All of this means that had more comprehensive imaging been done, many more patients may have been diagnosed with myeloma. Such patients may have been undertreated, and single agent daratumumab, with a response rate of just 63%, may not have been enough. Conversely, some patients may also have been overtreated using this approach, as the protocol allowed patients who had been diagnosed with smoldering myeloma up to 5 years earlier to be enrolled. Many of these people could have had indolent disease for years prior to enrollment and may not have ever progressed.
Further information is needed to help us understand this study better. What was the nature of the progression events: asymptomatic lab changes or morbid end organ damage? Was daratumumab given when patients in the control arm progressed to myeloma? My concern is that if patients in the control arm do not universally receive modern daratumumab-containing therapies when they develop myeloma, then an overall survival advantage may be shown simply because patients in the intervention arm are getting a good drug earlier in the disease, while those in the control arm are not getting a good drug at all. Nevertheless, despite these limitations, it is likely this trial will lead to regulatory approval of daratumumab in this space, and lots of discussions from patients and clinicians alike.
Extended Follow-Up of Anito-Cel in its First In-Human study
Two chimeric antigen receptor therapy (CAR-T) products are currently approved for myeloma. Cilta-cel is clearly effective but is associated with problematic late-onset neurological toxicities. Ide-cel appears much less effective. There is clearly a need for a product that is both effective and safe.
Anito-cel has two relevant abstracts this meeting that show much promise. Extended follow-up of anito-cel from its first in human study shows a promising 27-month PFS of 52%, and with no cases of delayed neurotoxicity. I also eagerly await further information from the registrational single-arm study of anti-cel being presented at ASH 2024, which should (hopefully) lead to its accelerated approval.
Screening for Myeloma for all People With Vertebral Fractures Likely Unnecessary
This elegant study of over 9,000 people with vertebral fractures shows that absolute risks for myeloma were 0.43% and 0.63% in women and men with grade 2-3 fractures, respectively, indicating that there is likely little benefit in evaluating asymptomatic individuals with incidentally discovered vertebral fractures for myeloma, unless other features are present. Spread the word.
Further Information on Cevostamab, Another Bispecific Option
We do need effective treatments for targets beyond just BCMA and GPRC5D. Cevostamab, a bispecific targeting FCRH5, represents another option, with updated data on 167 patients. With an overall response rate of 43% (duration of response, 10 months), and a response rate of about 30% in those with prior bispecific exposure, this data helps us contextualize expected benefits as we look forward to the eventual approval of this drug. The efficacy is relatively modest in those who have already progressed on bispecifics, but cevostamab would still be a welcome addition to our arsenal.
Is GPRC5D a Better Target for Car T Rather Than Bispecifics?
Our currently available GPRC5D bispecific (talquetamab) leads to high rates of skin, oral, and nail toxicity. This drug can also bring significant weight loss. These side effects make me consider that continuous targeting of GPRC5D through a bispecific may not be ideal, and that GPRC5D may be better as a one-time CAR T target. At ASH 2024, we will have 15-month follow-up data from BMS-986393, a GPRC5D CAR T. Response rates for this heavily pretreated population (76% of whom had triple refractory disease) were at 87%, with a median PFS of 14.5 months. Only 6% of patients experienced treatment-related weight loss, and nail (19%), skin (30%), and oral (31%) toxicities were relatively low. I look forward to updated data, as well as data on the resolution of the toxicities seen.
Daratumumab, a Game-Changer for AL Amyloidosis
A truly effective drug given early can change the natural history of disease, even if patients in the control arm only receive the drug later. A case in point is daratumumab. The 5-year survival rate was 76.1% for the daratumumab/cyclophosphamide/bortezomib/dexamethasone arm and 64.7% for cyclophosphamide/bortezomib/dexamethasone arm. This happened despite the fact that 67% of the control arm patients (among those who received therapy) went on to receive daratumumab later in the disease course.
Understanding how SMM Progresses to MM
We often hear that we should treat SMM and not just watch carefully because fractures may suddenly happen, or a patient may end up on dialysis. What this retrospective study tells us that amongst 427 patients with SMM, 42 had progression to myeloma, and amongst those 42, only 1 developed renal dysfunction (unclear if this resolved), and only 1 had lytic lesions that were symptomatic. The remainder were all asymptomatic lab and imaging changes. This is a retrospective study, and one should assume that follow-up was thus highly variable. It does not appear that diffusion weighted whole-body MRI imaging (our most sensitive imaging test) was employed universally or very frequently. Nevertheless, these powerful findings reassure us that, with close observation, morbidity is unlikely. Our group has designed a prospective study incorporating frequent diffusion weighted whole body MRI imaging to formally test this hypothesis (SPOTLIGHT, NCT06212323).
The Underperformance of Daratumumab/Lenalidomide/Dexamethasone in the Real World
At every major meeting I am reminded of the disconnect between real-world efficacy and clinical trial efficacy. Case in point: In this Austrian experience, daratumumab/lenalidomide/dexamethasone led to a PFS of 22.7 months vs 61.9 months in the MAIA trial of daratumumab/lenalidomide/dexamethasone. Such a sobering difference! And if you think this is an isolated experience, even in a US real-world cohort, consider that in a recently published comparative study dara/len/dex underperformed, although the time to next treatment or death was longer (37.8 months).
Delayed Neurotoxicity may not be Just a Consequence of high tumor burden
We currently think that some of the scariest side effects of cilta-cel, such as delayed neurotoxicity, may be a consequence of a high number of cancer cells and may be prevented by better disease control at the time of infusion. This study, a sobering analysis of 52 patients with delayed neurotoxicity occurring after CAR T, included 8 patients (15%) who were not heavily pretreated, and all had less than 5% plasma cells at the time of infusion. None of these patients had extramedullary disease. This result worries me, especially because cilta-cel is being studied and is poised for future approval in earlier line settings. It suggests that this toxicity may not always be a product of disease burden, contrary to our current belief.
I will be paying close attention to these 10 myeloma studies at ASH 2024, where I look forward to meeting you and learning more.Dr. Mohyuddin is assistant professor in the multiple myeloma program at the Huntsman Cancer Institute at the University of Utah, Salt Lake City.