User login
MDedge latest news is breaking news from medical conferences, journals, guidelines, the FDA and CDC.
Bringing HCC Patients Hope Through Trials, Advanced Treatments
For Reena Salgia, MD, the most rewarding part about working with patients with hepatocellular carcinoma is being there for their entire journey, thanks to advancements in treatment. “It brings a smile to my face just to think about it,” says Dr. Salgia, medical director of Henry Ford Health’s Liver Cancer Clinic in Detroit.
Hepatocellular carcinoma accounts for 80% of all liver cancer. When she first entered the field, Dr. Salgia often heard that survival rates 5 years after diagnosis were less than 10%. Over the last decade however, “I’ve seen an expansion in the procedural options that we offer these patients. We have an array of options both surgically as well as procedurally,” she said.
Especially over the last three to four years, “we’ve seen meaningful responses for patients with medications that we previously didn’t have in our toolbox. That’s really been exciting, along with continued involvement in clinical trials and being able to offer patients a number of different approaches to their care of liver cancer,” said Dr. Salgia.
A regular attendee and presenter at national GI meetings, Dr. Salgia participated in AGA’s Women’s Executive Leadership Conference in 2023. Her academic resume includes a long list of clinical trials to assess treatments for patients at different stages of hepatocellular carcinoma.
In an interview, she discussed the highlights of her career as a researcher and mentor of fellows, and how she guides and supports her transplant patients.
What drove you to pursue the field of hepatology and transplant hepatology?
I came across this field during my fourth year of medical school. I didn’t know anything about hepatology when I reached that stage and had the opportunity to do an elective. I just fell in love with the specialty. I liked the complex pathophysiology of liver disease, the long-term follow-up and care of patients. It appealed to the type of science that I had enjoyed back in college.
As I went into my GI fellowship training, I got to learn more about the field of transplant medicine. For instance, how you can take these patients who are incredibly ill, really at a very vulnerable point of their illness, and then offer them great hope and see their lives turn around afterwards. When I had the opportunity to see patients go from end stage liver disease to such significant improvement in their quality of life, and restoring their physical functioning beyond what we would’ve ever imagined when they were ill, it reaffirmed my interest in both hepatology as well as in transplant medicine.
How do you help those patients waiting on transplant lists for a liver?
We are intimately involved in their care all the way through their journey with liver disease, up until the time of physically getting the liver transplant, which is performed by our colleagues in transplant surgery. From the time they are transplanted, we are involved in their inpatient and outpatient post-transplant care. We’ve helped to get them on the transplant list with the work of the multidisciplinary team. If there are opportunities to help them understand their position on the list or obtaining exceptions—though that is done in a very objective fashion through the regulatory system—we help to guide them through that journey.
You’ve worked on many studies that involve treatments for hepatocellular carcinoma. Can you highlight a paper that yielded clinically significant benefits?
What really stands out the most to me was our site’s involvement in the IMbrave150 trial, which was published in 2020. This multicenter study made a big difference in the outcomes and treatments for patients, as it brought the adoption of first-line immunotherapy (atezolizumab plus bevacizumab) for patients with advanced hepatocellular carcinoma. I remember vividly the patients we had the opportunity to enroll in that trial – some who we continue to care for today. This stands out as one of the trials that I was involved in that had a lasting impact.
What were the clinical endpoints and key results of that trial?
The endpoint was to see an improvement in overall survival utilizing immunotherapy, compared with the prior standard of care then available, oral therapy. The results led to the adoption and FDA approval of immunotherapy in the first line setting for advanced unresectable hepatocellular carcinoma patients.
What are some of the highlights of serving as director of Henry Ford’s fellowship program?
Education is my passion. I went into medical training feeling that at some point I would love to blend in teaching in a formal role. Becoming program director of the gastroenterology and hepatology fellowship at Henry Ford in 2018 was one of the most meaningful things that I’ve had the opportunity to do in my career. I get to see trainees who are at a very impressionable point of their journey go on to become gastroenterologists and then launch into their first job and really develop in this field. Seeing them come in day one, not knowing how to hold a scope or do a procedure on a patient of this nature, then quickly evolve over the first year and grow over three years to achieve this specialty training [is rewarding]. I’ve learned a lot from the fellows along the way. I think of them as an extension of my family. We have 15 fellows currently in our program and we’ll be growing this summer. So that’s really been a highlight of my career thus far.
What fears did you have to push past to get to where you are in your career?
I think that there have been a few. One is certainly the fear of making the wrong choice with your first career opportunity. I did choose to leave my comfort zone from where I had done my training. I met that with some fear, but also excitement for new opportunities of personal and professional growth.
Another fear is: Am I going to be able to be ambitious in this field? Can I pursue research, become a program director, and do things that my role models and mentors were able to achieve? There’s also the fear of being able to balance a busy work life with a busy home life and figuring out how to do both well and minimize the guilt on both sides. I have a family with two girls. They are definitely a top priority.
What teacher or mentor had the greatest impact on you?
Helen Te, MD, a hepatologist at the University of Chicago. When I was a medical student there, I had the opportunity to work with her and saw her passion for this field. She really had so much enthusiasm for teaching and was a big part of why I started to fall in love with liver disease.
Karen Kim, MD, now the dean of Penn State College of Medicine, was one of my assigned mentors as a medical student. She helped me explore the fields where there were opportunities for residency and helped me make the decision to go into internal medicine, which often is a key deciding point for medical students. She was also a very influential teacher. The other individual who stands out is my fellowship program director, Hari Sree Conjeevaram, MD, MSc, at University of Michigan Health. He exhibited the qualities as an educator and program director that helped me recognize that education was something that I wanted to pursue in a formal fashion once I moved on in my career.
Describe how you would spend a free Saturday afternoon.
Likely taking a hike or go to a park with my family, enjoying the outdoors and spending time with them.
Lightning Round
If you weren’t a gastroenterologist, what would you be?
Philanthropist
Favorite city in U.S. besides the one you live in?
Chicago
Place you most want to travel?
New Zealand
Favorite breakfast?
Avocado toast
Favorite ice cream flavor?
Cookies and cream
How many cups of coffee do you drink per day?
Two…or more
Cat person or dog person?
Dog
Texting or talking?
Talk
Favorite season?
Autumn
Favorite type of music?
Pop
Favorite movie genre?
Action
For Reena Salgia, MD, the most rewarding part about working with patients with hepatocellular carcinoma is being there for their entire journey, thanks to advancements in treatment. “It brings a smile to my face just to think about it,” says Dr. Salgia, medical director of Henry Ford Health’s Liver Cancer Clinic in Detroit.
Hepatocellular carcinoma accounts for 80% of all liver cancer. When she first entered the field, Dr. Salgia often heard that survival rates 5 years after diagnosis were less than 10%. Over the last decade however, “I’ve seen an expansion in the procedural options that we offer these patients. We have an array of options both surgically as well as procedurally,” she said.
Especially over the last three to four years, “we’ve seen meaningful responses for patients with medications that we previously didn’t have in our toolbox. That’s really been exciting, along with continued involvement in clinical trials and being able to offer patients a number of different approaches to their care of liver cancer,” said Dr. Salgia.
A regular attendee and presenter at national GI meetings, Dr. Salgia participated in AGA’s Women’s Executive Leadership Conference in 2023. Her academic resume includes a long list of clinical trials to assess treatments for patients at different stages of hepatocellular carcinoma.
In an interview, she discussed the highlights of her career as a researcher and mentor of fellows, and how she guides and supports her transplant patients.
What drove you to pursue the field of hepatology and transplant hepatology?
I came across this field during my fourth year of medical school. I didn’t know anything about hepatology when I reached that stage and had the opportunity to do an elective. I just fell in love with the specialty. I liked the complex pathophysiology of liver disease, the long-term follow-up and care of patients. It appealed to the type of science that I had enjoyed back in college.
As I went into my GI fellowship training, I got to learn more about the field of transplant medicine. For instance, how you can take these patients who are incredibly ill, really at a very vulnerable point of their illness, and then offer them great hope and see their lives turn around afterwards. When I had the opportunity to see patients go from end stage liver disease to such significant improvement in their quality of life, and restoring their physical functioning beyond what we would’ve ever imagined when they were ill, it reaffirmed my interest in both hepatology as well as in transplant medicine.
How do you help those patients waiting on transplant lists for a liver?
We are intimately involved in their care all the way through their journey with liver disease, up until the time of physically getting the liver transplant, which is performed by our colleagues in transplant surgery. From the time they are transplanted, we are involved in their inpatient and outpatient post-transplant care. We’ve helped to get them on the transplant list with the work of the multidisciplinary team. If there are opportunities to help them understand their position on the list or obtaining exceptions—though that is done in a very objective fashion through the regulatory system—we help to guide them through that journey.
You’ve worked on many studies that involve treatments for hepatocellular carcinoma. Can you highlight a paper that yielded clinically significant benefits?
What really stands out the most to me was our site’s involvement in the IMbrave150 trial, which was published in 2020. This multicenter study made a big difference in the outcomes and treatments for patients, as it brought the adoption of first-line immunotherapy (atezolizumab plus bevacizumab) for patients with advanced hepatocellular carcinoma. I remember vividly the patients we had the opportunity to enroll in that trial – some who we continue to care for today. This stands out as one of the trials that I was involved in that had a lasting impact.
What were the clinical endpoints and key results of that trial?
The endpoint was to see an improvement in overall survival utilizing immunotherapy, compared with the prior standard of care then available, oral therapy. The results led to the adoption and FDA approval of immunotherapy in the first line setting for advanced unresectable hepatocellular carcinoma patients.
What are some of the highlights of serving as director of Henry Ford’s fellowship program?
Education is my passion. I went into medical training feeling that at some point I would love to blend in teaching in a formal role. Becoming program director of the gastroenterology and hepatology fellowship at Henry Ford in 2018 was one of the most meaningful things that I’ve had the opportunity to do in my career. I get to see trainees who are at a very impressionable point of their journey go on to become gastroenterologists and then launch into their first job and really develop in this field. Seeing them come in day one, not knowing how to hold a scope or do a procedure on a patient of this nature, then quickly evolve over the first year and grow over three years to achieve this specialty training [is rewarding]. I’ve learned a lot from the fellows along the way. I think of them as an extension of my family. We have 15 fellows currently in our program and we’ll be growing this summer. So that’s really been a highlight of my career thus far.
What fears did you have to push past to get to where you are in your career?
I think that there have been a few. One is certainly the fear of making the wrong choice with your first career opportunity. I did choose to leave my comfort zone from where I had done my training. I met that with some fear, but also excitement for new opportunities of personal and professional growth.
Another fear is: Am I going to be able to be ambitious in this field? Can I pursue research, become a program director, and do things that my role models and mentors were able to achieve? There’s also the fear of being able to balance a busy work life with a busy home life and figuring out how to do both well and minimize the guilt on both sides. I have a family with two girls. They are definitely a top priority.
What teacher or mentor had the greatest impact on you?
Helen Te, MD, a hepatologist at the University of Chicago. When I was a medical student there, I had the opportunity to work with her and saw her passion for this field. She really had so much enthusiasm for teaching and was a big part of why I started to fall in love with liver disease.
Karen Kim, MD, now the dean of Penn State College of Medicine, was one of my assigned mentors as a medical student. She helped me explore the fields where there were opportunities for residency and helped me make the decision to go into internal medicine, which often is a key deciding point for medical students. She was also a very influential teacher. The other individual who stands out is my fellowship program director, Hari Sree Conjeevaram, MD, MSc, at University of Michigan Health. He exhibited the qualities as an educator and program director that helped me recognize that education was something that I wanted to pursue in a formal fashion once I moved on in my career.
Describe how you would spend a free Saturday afternoon.
Likely taking a hike or go to a park with my family, enjoying the outdoors and spending time with them.
Lightning Round
If you weren’t a gastroenterologist, what would you be?
Philanthropist
Favorite city in U.S. besides the one you live in?
Chicago
Place you most want to travel?
New Zealand
Favorite breakfast?
Avocado toast
Favorite ice cream flavor?
Cookies and cream
How many cups of coffee do you drink per day?
Two…or more
Cat person or dog person?
Dog
Texting or talking?
Talk
Favorite season?
Autumn
Favorite type of music?
Pop
Favorite movie genre?
Action
For Reena Salgia, MD, the most rewarding part about working with patients with hepatocellular carcinoma is being there for their entire journey, thanks to advancements in treatment. “It brings a smile to my face just to think about it,” says Dr. Salgia, medical director of Henry Ford Health’s Liver Cancer Clinic in Detroit.
Hepatocellular carcinoma accounts for 80% of all liver cancer. When she first entered the field, Dr. Salgia often heard that survival rates 5 years after diagnosis were less than 10%. Over the last decade however, “I’ve seen an expansion in the procedural options that we offer these patients. We have an array of options both surgically as well as procedurally,” she said.
Especially over the last three to four years, “we’ve seen meaningful responses for patients with medications that we previously didn’t have in our toolbox. That’s really been exciting, along with continued involvement in clinical trials and being able to offer patients a number of different approaches to their care of liver cancer,” said Dr. Salgia.
A regular attendee and presenter at national GI meetings, Dr. Salgia participated in AGA’s Women’s Executive Leadership Conference in 2023. Her academic resume includes a long list of clinical trials to assess treatments for patients at different stages of hepatocellular carcinoma.
In an interview, she discussed the highlights of her career as a researcher and mentor of fellows, and how she guides and supports her transplant patients.
What drove you to pursue the field of hepatology and transplant hepatology?
I came across this field during my fourth year of medical school. I didn’t know anything about hepatology when I reached that stage and had the opportunity to do an elective. I just fell in love with the specialty. I liked the complex pathophysiology of liver disease, the long-term follow-up and care of patients. It appealed to the type of science that I had enjoyed back in college.
As I went into my GI fellowship training, I got to learn more about the field of transplant medicine. For instance, how you can take these patients who are incredibly ill, really at a very vulnerable point of their illness, and then offer them great hope and see their lives turn around afterwards. When I had the opportunity to see patients go from end stage liver disease to such significant improvement in their quality of life, and restoring their physical functioning beyond what we would’ve ever imagined when they were ill, it reaffirmed my interest in both hepatology as well as in transplant medicine.
How do you help those patients waiting on transplant lists for a liver?
We are intimately involved in their care all the way through their journey with liver disease, up until the time of physically getting the liver transplant, which is performed by our colleagues in transplant surgery. From the time they are transplanted, we are involved in their inpatient and outpatient post-transplant care. We’ve helped to get them on the transplant list with the work of the multidisciplinary team. If there are opportunities to help them understand their position on the list or obtaining exceptions—though that is done in a very objective fashion through the regulatory system—we help to guide them through that journey.
You’ve worked on many studies that involve treatments for hepatocellular carcinoma. Can you highlight a paper that yielded clinically significant benefits?
What really stands out the most to me was our site’s involvement in the IMbrave150 trial, which was published in 2020. This multicenter study made a big difference in the outcomes and treatments for patients, as it brought the adoption of first-line immunotherapy (atezolizumab plus bevacizumab) for patients with advanced hepatocellular carcinoma. I remember vividly the patients we had the opportunity to enroll in that trial – some who we continue to care for today. This stands out as one of the trials that I was involved in that had a lasting impact.
What were the clinical endpoints and key results of that trial?
The endpoint was to see an improvement in overall survival utilizing immunotherapy, compared with the prior standard of care then available, oral therapy. The results led to the adoption and FDA approval of immunotherapy in the first line setting for advanced unresectable hepatocellular carcinoma patients.
What are some of the highlights of serving as director of Henry Ford’s fellowship program?
Education is my passion. I went into medical training feeling that at some point I would love to blend in teaching in a formal role. Becoming program director of the gastroenterology and hepatology fellowship at Henry Ford in 2018 was one of the most meaningful things that I’ve had the opportunity to do in my career. I get to see trainees who are at a very impressionable point of their journey go on to become gastroenterologists and then launch into their first job and really develop in this field. Seeing them come in day one, not knowing how to hold a scope or do a procedure on a patient of this nature, then quickly evolve over the first year and grow over three years to achieve this specialty training [is rewarding]. I’ve learned a lot from the fellows along the way. I think of them as an extension of my family. We have 15 fellows currently in our program and we’ll be growing this summer. So that’s really been a highlight of my career thus far.
What fears did you have to push past to get to where you are in your career?
I think that there have been a few. One is certainly the fear of making the wrong choice with your first career opportunity. I did choose to leave my comfort zone from where I had done my training. I met that with some fear, but also excitement for new opportunities of personal and professional growth.
Another fear is: Am I going to be able to be ambitious in this field? Can I pursue research, become a program director, and do things that my role models and mentors were able to achieve? There’s also the fear of being able to balance a busy work life with a busy home life and figuring out how to do both well and minimize the guilt on both sides. I have a family with two girls. They are definitely a top priority.
What teacher or mentor had the greatest impact on you?
Helen Te, MD, a hepatologist at the University of Chicago. When I was a medical student there, I had the opportunity to work with her and saw her passion for this field. She really had so much enthusiasm for teaching and was a big part of why I started to fall in love with liver disease.
Karen Kim, MD, now the dean of Penn State College of Medicine, was one of my assigned mentors as a medical student. She helped me explore the fields where there were opportunities for residency and helped me make the decision to go into internal medicine, which often is a key deciding point for medical students. She was also a very influential teacher. The other individual who stands out is my fellowship program director, Hari Sree Conjeevaram, MD, MSc, at University of Michigan Health. He exhibited the qualities as an educator and program director that helped me recognize that education was something that I wanted to pursue in a formal fashion once I moved on in my career.
Describe how you would spend a free Saturday afternoon.
Likely taking a hike or go to a park with my family, enjoying the outdoors and spending time with them.
Lightning Round
If you weren’t a gastroenterologist, what would you be?
Philanthropist
Favorite city in U.S. besides the one you live in?
Chicago
Place you most want to travel?
New Zealand
Favorite breakfast?
Avocado toast
Favorite ice cream flavor?
Cookies and cream
How many cups of coffee do you drink per day?
Two…or more
Cat person or dog person?
Dog
Texting or talking?
Talk
Favorite season?
Autumn
Favorite type of music?
Pop
Favorite movie genre?
Action

Population vs Tailored Skin Cancer Screening: Which Is Best?
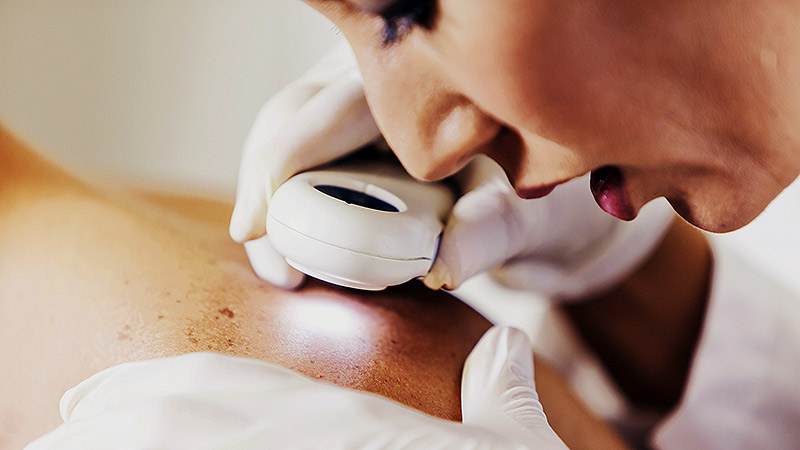
ATHENS, Greece — At the 11th World Congress of Melanoma and 21st EADO Congress 2025, experts presented divergent perspectives on the merits of population-wide skin cancer screening programs vs more targeted approaches. The debate highlighted concerns about healthcare resource allocation, overdiagnosis, and the true impact of mass skin cancer screening on mortality.
Arguing against widespread screening, particularly in low-to-medium incidence countries like Spain, was Susana Puig, MD, the head of Dermatology at Hospital Clínic de Barcelona, University of Barcelona, and a dermatologist at Barnaclínic+, Barcelona, Spain.
“It’s not efficient. We visit too many healthy individuals to detect melanoma,” she said. “We need to focus on treating patients, not checking healthy people without any risk.”
Championing for population-wide screening was Peter Mohr, MD, a dermatologist at the Clinic of Dermatology in Elbe Klinikum Buxtehude, Buxtehude, Germany, who noted a disproportionate focus on treatment rather than prevention. “The ultimate goal of screening,” he said, “is to prevent advanced disease and reduce melanoma-specific mortality.”
Avoid Population-Based Screening
Presenting data from Germany, Puig noted that population-based screening starting at any age requires examining more than 600 people and performing over 24 excisions to detect one melanoma. When setting screening to start at the age of 35 years, the number of people needed to screen to detect one melanoma decreased slightly to 559.
These findings highlight that population-based screening will include many people who don’t need it and can increase the potential for overdiagnosis, she argued.
Studies and guidelines from the United States align with Puig’s concern about broad-based screening likely leading to overdiagnosis. “The incidence of melanoma has risen sixfold in the past 40 years in the United States, while mortality has remained largely flat, an epidemiological signature consistent with overdiagnosis,” according to Adewole Adamson, MD, an assistant professor of internal medicine, in the Division of Dermatology at Dell Medical School at The University of Texas at Austin, Texas, who published findings to this effect in 2022.
“We cannot saturate the system with healthy people,” Puig said. Instead, “we need to use strategies to identify high-risk patients.” She proposed being more selective about who to screen by identifying those at higher risk of developing melanoma.
Identifying risk factors, such as the presence of atypical nevi and a personal or family history of melanoma, can help hone who is screened, she explained. Patients with a personal history of melanoma, in particular, face a higher risk of developing subsequent melanomas. Data show that patients with two or more primary melanomas had almost three times the risk of developing a subsequent one than those with one prior melanoma — 25.7% vs 8.6%. Puig also pointed out the significant correlation between age and melanoma risk, with people over 70 years exhibiting a 93-fold higher probability of diagnosis than those younger than 30 years.
Citing the German data, she noted that screening people 20 years and older with one risk factor reduced the number needed to screen by more than threefold — from more than 600 to 178.
Puig suggested dedicated surveillance programs for high-risk individuals alongside opportunistic screening during routine medical encounters.
“This would lead to a more efficient allocation of healthcare resources and better outcomes for those most vulnerable to melanoma,” Puig concluded.
Perform Population-Based Screening
In contrast, Mohr presented a defense of population-based skin cancer screening. Skin cancer is the most common cancer diagnosed in the United States and is prevalent worldwide, with more than 1.5 million new cases diagnosed globally in 2022.
Screening people and identifying the disease in its earliest stages is important, he said.
Mohr highlighted a recent study exploring biennial skin cancer screening in Germany and found that 4.2% of those screened had a skin cancer finding, but the number of interval melanomas was similar in both screened and unscreened populations.
However, a large retrospective cohort study from Germany involving about 1.4 million people showed a decrease in locoregional metastasis (from 13% to 4%), distant metastases (from 8% to 4%), and systemic treatments (from 21% to 11%) in screened vs unscreened people, as well as better overall survival rates in the screened population.
Mohr highlighted how Germany, in particular, is well-equipped for more broad-based, preventative screening.
Germany has had long-standing primary prevention programs, which have existed for about 24 years and involve extensive public awareness campaigns. Access to dermatologists is significantly better in Germany compared with the Netherlands, with an average waiting time for screening of around 6 weeks and only 1.2 weeks for suspicious lesions, compared with 14 weeks and 3.5 weeks, respectively, in the Netherlands. This access may make a broader screening strategy more feasible in a country like Germany.
However, Mohr did note that there are “no large, randomized trials to show us the value of skin cancer screening.”
A Role for Primary Care Physicians?
Although they disagreed about the utility of screening, both Puig and Mohr agreed on the important role primary care physicians play in improving early melanoma detection. “We cannot do it alone, and general practitioners are really fundamental,” Puig said.
Mohr said that continuous education for primary care physicians can dramatically improve their diagnostic skills. In Germany, an 8-hour training session significantly improved their ability to detect basal cell carcinoma and melanomas. However, he cautioned that this improved accuracy tended to wane within a year.
In Spain, Puig highlighted the successful implementation of teledermatology to support general practitioners. “We train them with dermoscopy, and we answer all teledermatology requests in 1 week, reducing in-person visits by 50%,” she explained. This approach allows general practitioners to assess potential skin cancer efficiently and streamline referrals.
Puig reported being on advisory boards for Almirall, Bristol Myers Squibb (BMS), ISDIN, La Roche-Posay, Leo Pharma, Novartis, Pfizer, Regeneron, Roche, Sanofi, and Sun Pharma. She conducts research and trials with AbbVie, Almirall, Amgen, BMS, Biofrontera, Canfield, Cantabria, Fotofinder, GSK, ISDIN, La Roche-Posay, Leo Pharma, MSD, MEDA, Novartis, Pfizer, Polychem, Sanofi, Roche, and Regeneron. She is involved with Athena Technology Solutions and Dermavision Solutions. Mohr reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
ATHENS, Greece — At the 11th World Congress of Melanoma and 21st EADO Congress 2025, experts presented divergent perspectives on the merits of population-wide skin cancer screening programs vs more targeted approaches. The debate highlighted concerns about healthcare resource allocation, overdiagnosis, and the true impact of mass skin cancer screening on mortality.
Arguing against widespread screening, particularly in low-to-medium incidence countries like Spain, was Susana Puig, MD, the head of Dermatology at Hospital Clínic de Barcelona, University of Barcelona, and a dermatologist at Barnaclínic+, Barcelona, Spain.
“It’s not efficient. We visit too many healthy individuals to detect melanoma,” she said. “We need to focus on treating patients, not checking healthy people without any risk.”
Championing for population-wide screening was Peter Mohr, MD, a dermatologist at the Clinic of Dermatology in Elbe Klinikum Buxtehude, Buxtehude, Germany, who noted a disproportionate focus on treatment rather than prevention. “The ultimate goal of screening,” he said, “is to prevent advanced disease and reduce melanoma-specific mortality.”
Avoid Population-Based Screening
Presenting data from Germany, Puig noted that population-based screening starting at any age requires examining more than 600 people and performing over 24 excisions to detect one melanoma. When setting screening to start at the age of 35 years, the number of people needed to screen to detect one melanoma decreased slightly to 559.
These findings highlight that population-based screening will include many people who don’t need it and can increase the potential for overdiagnosis, she argued.
Studies and guidelines from the United States align with Puig’s concern about broad-based screening likely leading to overdiagnosis. “The incidence of melanoma has risen sixfold in the past 40 years in the United States, while mortality has remained largely flat, an epidemiological signature consistent with overdiagnosis,” according to Adewole Adamson, MD, an assistant professor of internal medicine, in the Division of Dermatology at Dell Medical School at The University of Texas at Austin, Texas, who published findings to this effect in 2022.
“We cannot saturate the system with healthy people,” Puig said. Instead, “we need to use strategies to identify high-risk patients.” She proposed being more selective about who to screen by identifying those at higher risk of developing melanoma.
Identifying risk factors, such as the presence of atypical nevi and a personal or family history of melanoma, can help hone who is screened, she explained. Patients with a personal history of melanoma, in particular, face a higher risk of developing subsequent melanomas. Data show that patients with two or more primary melanomas had almost three times the risk of developing a subsequent one than those with one prior melanoma — 25.7% vs 8.6%. Puig also pointed out the significant correlation between age and melanoma risk, with people over 70 years exhibiting a 93-fold higher probability of diagnosis than those younger than 30 years.
Citing the German data, she noted that screening people 20 years and older with one risk factor reduced the number needed to screen by more than threefold — from more than 600 to 178.
Puig suggested dedicated surveillance programs for high-risk individuals alongside opportunistic screening during routine medical encounters.
“This would lead to a more efficient allocation of healthcare resources and better outcomes for those most vulnerable to melanoma,” Puig concluded.
Perform Population-Based Screening
In contrast, Mohr presented a defense of population-based skin cancer screening. Skin cancer is the most common cancer diagnosed in the United States and is prevalent worldwide, with more than 1.5 million new cases diagnosed globally in 2022.
Screening people and identifying the disease in its earliest stages is important, he said.
Mohr highlighted a recent study exploring biennial skin cancer screening in Germany and found that 4.2% of those screened had a skin cancer finding, but the number of interval melanomas was similar in both screened and unscreened populations.
However, a large retrospective cohort study from Germany involving about 1.4 million people showed a decrease in locoregional metastasis (from 13% to 4%), distant metastases (from 8% to 4%), and systemic treatments (from 21% to 11%) in screened vs unscreened people, as well as better overall survival rates in the screened population.
Mohr highlighted how Germany, in particular, is well-equipped for more broad-based, preventative screening.
Germany has had long-standing primary prevention programs, which have existed for about 24 years and involve extensive public awareness campaigns. Access to dermatologists is significantly better in Germany compared with the Netherlands, with an average waiting time for screening of around 6 weeks and only 1.2 weeks for suspicious lesions, compared with 14 weeks and 3.5 weeks, respectively, in the Netherlands. This access may make a broader screening strategy more feasible in a country like Germany.
However, Mohr did note that there are “no large, randomized trials to show us the value of skin cancer screening.”
A Role for Primary Care Physicians?
Although they disagreed about the utility of screening, both Puig and Mohr agreed on the important role primary care physicians play in improving early melanoma detection. “We cannot do it alone, and general practitioners are really fundamental,” Puig said.
Mohr said that continuous education for primary care physicians can dramatically improve their diagnostic skills. In Germany, an 8-hour training session significantly improved their ability to detect basal cell carcinoma and melanomas. However, he cautioned that this improved accuracy tended to wane within a year.
In Spain, Puig highlighted the successful implementation of teledermatology to support general practitioners. “We train them with dermoscopy, and we answer all teledermatology requests in 1 week, reducing in-person visits by 50%,” she explained. This approach allows general practitioners to assess potential skin cancer efficiently and streamline referrals.
Puig reported being on advisory boards for Almirall, Bristol Myers Squibb (BMS), ISDIN, La Roche-Posay, Leo Pharma, Novartis, Pfizer, Regeneron, Roche, Sanofi, and Sun Pharma. She conducts research and trials with AbbVie, Almirall, Amgen, BMS, Biofrontera, Canfield, Cantabria, Fotofinder, GSK, ISDIN, La Roche-Posay, Leo Pharma, MSD, MEDA, Novartis, Pfizer, Polychem, Sanofi, Roche, and Regeneron. She is involved with Athena Technology Solutions and Dermavision Solutions. Mohr reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
ATHENS, Greece — At the 11th World Congress of Melanoma and 21st EADO Congress 2025, experts presented divergent perspectives on the merits of population-wide skin cancer screening programs vs more targeted approaches. The debate highlighted concerns about healthcare resource allocation, overdiagnosis, and the true impact of mass skin cancer screening on mortality.
Arguing against widespread screening, particularly in low-to-medium incidence countries like Spain, was Susana Puig, MD, the head of Dermatology at Hospital Clínic de Barcelona, University of Barcelona, and a dermatologist at Barnaclínic+, Barcelona, Spain.
“It’s not efficient. We visit too many healthy individuals to detect melanoma,” she said. “We need to focus on treating patients, not checking healthy people without any risk.”
Championing for population-wide screening was Peter Mohr, MD, a dermatologist at the Clinic of Dermatology in Elbe Klinikum Buxtehude, Buxtehude, Germany, who noted a disproportionate focus on treatment rather than prevention. “The ultimate goal of screening,” he said, “is to prevent advanced disease and reduce melanoma-specific mortality.”
Avoid Population-Based Screening
Presenting data from Germany, Puig noted that population-based screening starting at any age requires examining more than 600 people and performing over 24 excisions to detect one melanoma. When setting screening to start at the age of 35 years, the number of people needed to screen to detect one melanoma decreased slightly to 559.
These findings highlight that population-based screening will include many people who don’t need it and can increase the potential for overdiagnosis, she argued.
Studies and guidelines from the United States align with Puig’s concern about broad-based screening likely leading to overdiagnosis. “The incidence of melanoma has risen sixfold in the past 40 years in the United States, while mortality has remained largely flat, an epidemiological signature consistent with overdiagnosis,” according to Adewole Adamson, MD, an assistant professor of internal medicine, in the Division of Dermatology at Dell Medical School at The University of Texas at Austin, Texas, who published findings to this effect in 2022.
“We cannot saturate the system with healthy people,” Puig said. Instead, “we need to use strategies to identify high-risk patients.” She proposed being more selective about who to screen by identifying those at higher risk of developing melanoma.
Identifying risk factors, such as the presence of atypical nevi and a personal or family history of melanoma, can help hone who is screened, she explained. Patients with a personal history of melanoma, in particular, face a higher risk of developing subsequent melanomas. Data show that patients with two or more primary melanomas had almost three times the risk of developing a subsequent one than those with one prior melanoma — 25.7% vs 8.6%. Puig also pointed out the significant correlation between age and melanoma risk, with people over 70 years exhibiting a 93-fold higher probability of diagnosis than those younger than 30 years.
Citing the German data, she noted that screening people 20 years and older with one risk factor reduced the number needed to screen by more than threefold — from more than 600 to 178.
Puig suggested dedicated surveillance programs for high-risk individuals alongside opportunistic screening during routine medical encounters.
“This would lead to a more efficient allocation of healthcare resources and better outcomes for those most vulnerable to melanoma,” Puig concluded.
Perform Population-Based Screening
In contrast, Mohr presented a defense of population-based skin cancer screening. Skin cancer is the most common cancer diagnosed in the United States and is prevalent worldwide, with more than 1.5 million new cases diagnosed globally in 2022.
Screening people and identifying the disease in its earliest stages is important, he said.
Mohr highlighted a recent study exploring biennial skin cancer screening in Germany and found that 4.2% of those screened had a skin cancer finding, but the number of interval melanomas was similar in both screened and unscreened populations.
However, a large retrospective cohort study from Germany involving about 1.4 million people showed a decrease in locoregional metastasis (from 13% to 4%), distant metastases (from 8% to 4%), and systemic treatments (from 21% to 11%) in screened vs unscreened people, as well as better overall survival rates in the screened population.
Mohr highlighted how Germany, in particular, is well-equipped for more broad-based, preventative screening.
Germany has had long-standing primary prevention programs, which have existed for about 24 years and involve extensive public awareness campaigns. Access to dermatologists is significantly better in Germany compared with the Netherlands, with an average waiting time for screening of around 6 weeks and only 1.2 weeks for suspicious lesions, compared with 14 weeks and 3.5 weeks, respectively, in the Netherlands. This access may make a broader screening strategy more feasible in a country like Germany.
However, Mohr did note that there are “no large, randomized trials to show us the value of skin cancer screening.”
A Role for Primary Care Physicians?
Although they disagreed about the utility of screening, both Puig and Mohr agreed on the important role primary care physicians play in improving early melanoma detection. “We cannot do it alone, and general practitioners are really fundamental,” Puig said.
Mohr said that continuous education for primary care physicians can dramatically improve their diagnostic skills. In Germany, an 8-hour training session significantly improved their ability to detect basal cell carcinoma and melanomas. However, he cautioned that this improved accuracy tended to wane within a year.
In Spain, Puig highlighted the successful implementation of teledermatology to support general practitioners. “We train them with dermoscopy, and we answer all teledermatology requests in 1 week, reducing in-person visits by 50%,” she explained. This approach allows general practitioners to assess potential skin cancer efficiently and streamline referrals.
Puig reported being on advisory boards for Almirall, Bristol Myers Squibb (BMS), ISDIN, La Roche-Posay, Leo Pharma, Novartis, Pfizer, Regeneron, Roche, Sanofi, and Sun Pharma. She conducts research and trials with AbbVie, Almirall, Amgen, BMS, Biofrontera, Canfield, Cantabria, Fotofinder, GSK, ISDIN, La Roche-Posay, Leo Pharma, MSD, MEDA, Novartis, Pfizer, Polychem, Sanofi, Roche, and Regeneron. She is involved with Athena Technology Solutions and Dermavision Solutions. Mohr reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM WCM-EADO 2025
Childhood IBD Connects PA with Her Patients
Abigail Meyers, MPAS, PA-C, was 9 years old when a diagnosis of ulcerative colitis set the trajectory of her future career.
“There weren’t a lot of medical therapies available back then,” recalls Meyers, who had to undergo multiple hospitalizations and surgeries for her condition. Medical staff would say: “Oh I know how you feel,” then retract their words when Meyers would ask if they had ever experienced a nasogastric tube or ileostomy.
“I’m going to go into healthcare. I’m going to take care of patients with inflammatory bowel disease [IBD] and I will never say ‘I know how you feel’ unless I truly mean it,” Meyers vowed to her mother one night at the hospital.
And that’s exactly what she did. During her training as a physician assistant (PA), Meyers had the opportunity to do an adult colorectal surgery rotation and a pediatric gastroenterology rotation. Another bonus: she got to work with the gastroenterologist who treated her when she was a 9-year-old patient.
Meyers has never told a patient, “I know how you feel.” Instead, she might say: “This is really hard. This is something new. This is a challenging moment. You’re allowed to feel upset, you’re allowed to feel disappointed, you’re allowed to feel scared.”
A clinical expert in gastroenterology and colon and rectal surgery, Meyers spent 10 years at the Mayo Clinic as a PA in colon and rectal surgery and gastroenterology. She currently works as the assistant director of student success and development at the Medical College of Wisconsin in Milwaukee.
On days where things are hard and the grind of the day-to-day work in healthcare becomes too challenging, “I get to remind myself that I do make an impact,” said Meyers. If a patient ever asks her, “Have you ever had an ileostomy before?” Meyers can honestly answer that she has and then describe what it was like.
“I think that allows them to have a little bit of an ‘aha’ moment or a breakthrough in their recovery journey or their acceptance journey, whatever that looks like through this disease process,” she said.
In an interview, she discussed the work she’s done on multiple fronts to guide the careers of advanced practice providers (APPs), and the special connection she has with her patients.
Tell me about your preceptor work with the Crohn’s and Colitis Foundation’s APP Preceptorship program.
It is one of my proudest accomplishments, particularly in the preceptorship program. As a patient, the Crohn’s and Colitis Foundation provided a lot of education and resources when my family was going through a tough time. To be able to give back to the foundation, whether that’s resources for patients or providers, is really great. It’s helped me grow a lot professionally. I realized I enjoyed educating not just my patients, but also my peers. While I worked at Mayo Clinic, I had a wonderful opportunity at a tertiary IBD center for students and advanced practice providers to come and shadow me in colorectal surgery and managing IBD patients.
Michele Rubin, MSN, an advanced practice nurse and Maureen Kelly, MS, RN, CPNP, a nurse practitioner, started the foundation’s preceptor program and graciously took me under their wing.
Originally, there was just one site at the University of Chicago. When I joined, it expanded to the University of North Carolina at Chapel Hill for pediatric experience, and Mayo Clinic Rochester [Minnesota]. There are now seven participating host sites for the 2025 cycle.
The curriculum varies at each site based upon what resources are available. We really tried to tailor it to each individual preceptor. If there’s a nurse practitioner that used to be an ostomy nurse, maybe she’ll get time in the ostomy nurse area, but maybe she wants more time with the pharmacist or the radiologist.
If there is somebody who’s coming through that knows nothing about surgery, maybe they want a little bit more time in the surgical sphere. I tried to, when creating the curriculum for this, create a lot of options that existed for didactic learning as well as practical application.
You’re the assistant director of student success and development at the Medical College of Wisconsin, which launched a new Physician Associate Program. What’s happened with the program so far?
We do not have enrolled students yet. We are developing the program from the bottom up. I am one of four faculty, and then we have our founding director, Christine M. Everett, PhD, MPH, PA-C.
As we develop our program we are trying to keep a holistic approach in mind. We’re thinking about what a traditional student is vs a nontraditional student, and who we think will make great physician assistants. We pull from our own personal experiences as educators and experts in our field. As somebody who is academically minded, this program really spoke to me. Many PAs and nurse practitioners (NPs) fill a primary care role. But as we search to develop academically minded physician associates to join academic medical practices in an anticipated physician shortage, we want to hone in on some of these specialty care areas, recognizing that there is a place for us in academia and asking ‘what does that look like and how do we grow in those subspecialties?’
So, how can I help to foster that type of desire and growth and professional development in my students? That will be what we’re going to be tackling in our future cohorts.
Has the program generated a lot of interest?
Most PAs train in the region they are from and end up practicing there. So, our community and institution are very excited. There’s a lot of work in creating the program and making sure that the goals we have in mind will continue to grow with the profession. One of my neighbors who just started college reached out to me and said she wants to be a PA. We get emails regularly asking what people should do to prepare for PA school, and what are we looking for. PAs and NPs are growing professions. Both are on the top five list of best jobs ranked by U.S. News & World Report right now.
You’re the co-chair of AGA’s NPPA Task Force. What are the goals of this task force, specifically for 2025?
This is a new task force. We’re really excited about it, and we feel very supported by AGA. Specifically, we are focusing on content review and optimization. We’re working through and consulting on different proposals, such as how to have an NP/PA voice within AGA, or how certain proposals can be of interest to APPs or applicable to an APP practice.
One of our other goals is to grow our APP community opportunities, to find ways that we can all communicate with each other, share in our professional accomplishments, and be mentors and sponsors to each other to open the doors for professional growth within the GI space.
We are trying to create a sense of community within all the societies that APPs are involved in, and recognize everyone’s professional development and goals. We want to create a space to connect at some of our primary conferences and touchpoints, regardless of where your society home is.
We’ve also been asked to be a representative in helping to select the AGA-Pfizer Beacon of Hope Awards for Gender and Health Equity award recipients. We’re really proud that one of our task force members is going to be sitting on that committee to help select recipients of this award.
As a clinical expert in gastroenterology and colon and rectal surgery, you often present to national organizations like AGA, the Crohn’s and Colitis Foundation, and the American Society of Colon & Rectal Surgeons. What topics do you discuss and why?
It’s always been IBD because of my background. But I’ve also grown more in the colon/rectal surgery sphere, both in the inpatient, outpatient, and operating room setting. I enjoy presenting on topics like: What could you do right before you send a patient off to a tertiary IBD referral? I talk about complex disease management, especially the surgical realm of perianal Crohn’s disease. One of my colleagues jokes that one of her favorite talks I’ve ever given is how to perform a perianal examination. It’s a sensitive exam. I feel like I’m pretty good at it!
I also think it’s important to share information on how to write papers and how to present at conferences, because there are a lot of really smart NPs and PAs in GI and colorectal surgery who — for whatever reason — don’t know how to get their foot in the door for these types of opportunities. I love to be the person that opens that door. Do you want to be involved in a professional society? In what capacity? Making that information broadly available to everyone is something that I really love doing.
Describe a memorable patient encounter that helped shape your career.
I know this will sound so cliché, that there isn’t just one, but it’s true. There is a connection that I create with each and every one of my patients. I listen to their stories. They have whole lives outside of their disease, and I am honored that they open up to me — whether that is ongoing communication and check-ins with a patient’s family member a year after they’ve passed away, or every year receiving a Christmas card from a patient who is expanding their family because they’re finally in remission from their disease. These are the types of things that are so impactful and memorable.
Describe how you would spend a free Saturday afternoon.
I’m a mom to 7-year-old boy twins, and so I often don’t have a free Saturday. If I did, it would be sunny. I would go for a long run and then I would go out for brunch with my husband and then come home and read with my kids in a cozy blanket all day.
Lightning Round
What would you be if you weren’t a GI?
First grade teacher.
Last movie you watched?
Mufasa: The Lion King.
Best Halloween costume?
Velma from Scooby Doo.
Favorite sport?
To play – Tennis.
To watch – NBA basketball, “Go Timberwolves!”
Place you most want to travel to?
Greece
Favorite movie genre?
Rom-com.
Cat person or dog person?
Cat.
Favorite city besides the one you live in?
Manhattan.
Favorite season
Fall.
Favorite junk food?
Salty snack mix.
How many cups of coffee do you drink per day?
Three.
Abigail Meyers, MPAS, PA-C, was 9 years old when a diagnosis of ulcerative colitis set the trajectory of her future career.
“There weren’t a lot of medical therapies available back then,” recalls Meyers, who had to undergo multiple hospitalizations and surgeries for her condition. Medical staff would say: “Oh I know how you feel,” then retract their words when Meyers would ask if they had ever experienced a nasogastric tube or ileostomy.
“I’m going to go into healthcare. I’m going to take care of patients with inflammatory bowel disease [IBD] and I will never say ‘I know how you feel’ unless I truly mean it,” Meyers vowed to her mother one night at the hospital.
And that’s exactly what she did. During her training as a physician assistant (PA), Meyers had the opportunity to do an adult colorectal surgery rotation and a pediatric gastroenterology rotation. Another bonus: she got to work with the gastroenterologist who treated her when she was a 9-year-old patient.
Meyers has never told a patient, “I know how you feel.” Instead, she might say: “This is really hard. This is something new. This is a challenging moment. You’re allowed to feel upset, you’re allowed to feel disappointed, you’re allowed to feel scared.”
A clinical expert in gastroenterology and colon and rectal surgery, Meyers spent 10 years at the Mayo Clinic as a PA in colon and rectal surgery and gastroenterology. She currently works as the assistant director of student success and development at the Medical College of Wisconsin in Milwaukee.
On days where things are hard and the grind of the day-to-day work in healthcare becomes too challenging, “I get to remind myself that I do make an impact,” said Meyers. If a patient ever asks her, “Have you ever had an ileostomy before?” Meyers can honestly answer that she has and then describe what it was like.
“I think that allows them to have a little bit of an ‘aha’ moment or a breakthrough in their recovery journey or their acceptance journey, whatever that looks like through this disease process,” she said.
In an interview, she discussed the work she’s done on multiple fronts to guide the careers of advanced practice providers (APPs), and the special connection she has with her patients.
Tell me about your preceptor work with the Crohn’s and Colitis Foundation’s APP Preceptorship program.
It is one of my proudest accomplishments, particularly in the preceptorship program. As a patient, the Crohn’s and Colitis Foundation provided a lot of education and resources when my family was going through a tough time. To be able to give back to the foundation, whether that’s resources for patients or providers, is really great. It’s helped me grow a lot professionally. I realized I enjoyed educating not just my patients, but also my peers. While I worked at Mayo Clinic, I had a wonderful opportunity at a tertiary IBD center for students and advanced practice providers to come and shadow me in colorectal surgery and managing IBD patients.
Michele Rubin, MSN, an advanced practice nurse and Maureen Kelly, MS, RN, CPNP, a nurse practitioner, started the foundation’s preceptor program and graciously took me under their wing.
Originally, there was just one site at the University of Chicago. When I joined, it expanded to the University of North Carolina at Chapel Hill for pediatric experience, and Mayo Clinic Rochester [Minnesota]. There are now seven participating host sites for the 2025 cycle.
The curriculum varies at each site based upon what resources are available. We really tried to tailor it to each individual preceptor. If there’s a nurse practitioner that used to be an ostomy nurse, maybe she’ll get time in the ostomy nurse area, but maybe she wants more time with the pharmacist or the radiologist.
If there is somebody who’s coming through that knows nothing about surgery, maybe they want a little bit more time in the surgical sphere. I tried to, when creating the curriculum for this, create a lot of options that existed for didactic learning as well as practical application.
You’re the assistant director of student success and development at the Medical College of Wisconsin, which launched a new Physician Associate Program. What’s happened with the program so far?
We do not have enrolled students yet. We are developing the program from the bottom up. I am one of four faculty, and then we have our founding director, Christine M. Everett, PhD, MPH, PA-C.
As we develop our program we are trying to keep a holistic approach in mind. We’re thinking about what a traditional student is vs a nontraditional student, and who we think will make great physician assistants. We pull from our own personal experiences as educators and experts in our field. As somebody who is academically minded, this program really spoke to me. Many PAs and nurse practitioners (NPs) fill a primary care role. But as we search to develop academically minded physician associates to join academic medical practices in an anticipated physician shortage, we want to hone in on some of these specialty care areas, recognizing that there is a place for us in academia and asking ‘what does that look like and how do we grow in those subspecialties?’
So, how can I help to foster that type of desire and growth and professional development in my students? That will be what we’re going to be tackling in our future cohorts.
Has the program generated a lot of interest?
Most PAs train in the region they are from and end up practicing there. So, our community and institution are very excited. There’s a lot of work in creating the program and making sure that the goals we have in mind will continue to grow with the profession. One of my neighbors who just started college reached out to me and said she wants to be a PA. We get emails regularly asking what people should do to prepare for PA school, and what are we looking for. PAs and NPs are growing professions. Both are on the top five list of best jobs ranked by U.S. News & World Report right now.
You’re the co-chair of AGA’s NPPA Task Force. What are the goals of this task force, specifically for 2025?
This is a new task force. We’re really excited about it, and we feel very supported by AGA. Specifically, we are focusing on content review and optimization. We’re working through and consulting on different proposals, such as how to have an NP/PA voice within AGA, or how certain proposals can be of interest to APPs or applicable to an APP practice.
One of our other goals is to grow our APP community opportunities, to find ways that we can all communicate with each other, share in our professional accomplishments, and be mentors and sponsors to each other to open the doors for professional growth within the GI space.
We are trying to create a sense of community within all the societies that APPs are involved in, and recognize everyone’s professional development and goals. We want to create a space to connect at some of our primary conferences and touchpoints, regardless of where your society home is.
We’ve also been asked to be a representative in helping to select the AGA-Pfizer Beacon of Hope Awards for Gender and Health Equity award recipients. We’re really proud that one of our task force members is going to be sitting on that committee to help select recipients of this award.
As a clinical expert in gastroenterology and colon and rectal surgery, you often present to national organizations like AGA, the Crohn’s and Colitis Foundation, and the American Society of Colon & Rectal Surgeons. What topics do you discuss and why?
It’s always been IBD because of my background. But I’ve also grown more in the colon/rectal surgery sphere, both in the inpatient, outpatient, and operating room setting. I enjoy presenting on topics like: What could you do right before you send a patient off to a tertiary IBD referral? I talk about complex disease management, especially the surgical realm of perianal Crohn’s disease. One of my colleagues jokes that one of her favorite talks I’ve ever given is how to perform a perianal examination. It’s a sensitive exam. I feel like I’m pretty good at it!
I also think it’s important to share information on how to write papers and how to present at conferences, because there are a lot of really smart NPs and PAs in GI and colorectal surgery who — for whatever reason — don’t know how to get their foot in the door for these types of opportunities. I love to be the person that opens that door. Do you want to be involved in a professional society? In what capacity? Making that information broadly available to everyone is something that I really love doing.
Describe a memorable patient encounter that helped shape your career.
I know this will sound so cliché, that there isn’t just one, but it’s true. There is a connection that I create with each and every one of my patients. I listen to their stories. They have whole lives outside of their disease, and I am honored that they open up to me — whether that is ongoing communication and check-ins with a patient’s family member a year after they’ve passed away, or every year receiving a Christmas card from a patient who is expanding their family because they’re finally in remission from their disease. These are the types of things that are so impactful and memorable.
Describe how you would spend a free Saturday afternoon.
I’m a mom to 7-year-old boy twins, and so I often don’t have a free Saturday. If I did, it would be sunny. I would go for a long run and then I would go out for brunch with my husband and then come home and read with my kids in a cozy blanket all day.
Lightning Round
What would you be if you weren’t a GI?
First grade teacher.
Last movie you watched?
Mufasa: The Lion King.
Best Halloween costume?
Velma from Scooby Doo.
Favorite sport?
To play – Tennis.
To watch – NBA basketball, “Go Timberwolves!”
Place you most want to travel to?
Greece
Favorite movie genre?
Rom-com.
Cat person or dog person?
Cat.
Favorite city besides the one you live in?
Manhattan.
Favorite season
Fall.
Favorite junk food?
Salty snack mix.
How many cups of coffee do you drink per day?
Three.
Abigail Meyers, MPAS, PA-C, was 9 years old when a diagnosis of ulcerative colitis set the trajectory of her future career.
“There weren’t a lot of medical therapies available back then,” recalls Meyers, who had to undergo multiple hospitalizations and surgeries for her condition. Medical staff would say: “Oh I know how you feel,” then retract their words when Meyers would ask if they had ever experienced a nasogastric tube or ileostomy.
“I’m going to go into healthcare. I’m going to take care of patients with inflammatory bowel disease [IBD] and I will never say ‘I know how you feel’ unless I truly mean it,” Meyers vowed to her mother one night at the hospital.
And that’s exactly what she did. During her training as a physician assistant (PA), Meyers had the opportunity to do an adult colorectal surgery rotation and a pediatric gastroenterology rotation. Another bonus: she got to work with the gastroenterologist who treated her when she was a 9-year-old patient.
Meyers has never told a patient, “I know how you feel.” Instead, she might say: “This is really hard. This is something new. This is a challenging moment. You’re allowed to feel upset, you’re allowed to feel disappointed, you’re allowed to feel scared.”
A clinical expert in gastroenterology and colon and rectal surgery, Meyers spent 10 years at the Mayo Clinic as a PA in colon and rectal surgery and gastroenterology. She currently works as the assistant director of student success and development at the Medical College of Wisconsin in Milwaukee.
On days where things are hard and the grind of the day-to-day work in healthcare becomes too challenging, “I get to remind myself that I do make an impact,” said Meyers. If a patient ever asks her, “Have you ever had an ileostomy before?” Meyers can honestly answer that she has and then describe what it was like.
“I think that allows them to have a little bit of an ‘aha’ moment or a breakthrough in their recovery journey or their acceptance journey, whatever that looks like through this disease process,” she said.
In an interview, she discussed the work she’s done on multiple fronts to guide the careers of advanced practice providers (APPs), and the special connection she has with her patients.
Tell me about your preceptor work with the Crohn’s and Colitis Foundation’s APP Preceptorship program.
It is one of my proudest accomplishments, particularly in the preceptorship program. As a patient, the Crohn’s and Colitis Foundation provided a lot of education and resources when my family was going through a tough time. To be able to give back to the foundation, whether that’s resources for patients or providers, is really great. It’s helped me grow a lot professionally. I realized I enjoyed educating not just my patients, but also my peers. While I worked at Mayo Clinic, I had a wonderful opportunity at a tertiary IBD center for students and advanced practice providers to come and shadow me in colorectal surgery and managing IBD patients.
Michele Rubin, MSN, an advanced practice nurse and Maureen Kelly, MS, RN, CPNP, a nurse practitioner, started the foundation’s preceptor program and graciously took me under their wing.
Originally, there was just one site at the University of Chicago. When I joined, it expanded to the University of North Carolina at Chapel Hill for pediatric experience, and Mayo Clinic Rochester [Minnesota]. There are now seven participating host sites for the 2025 cycle.
The curriculum varies at each site based upon what resources are available. We really tried to tailor it to each individual preceptor. If there’s a nurse practitioner that used to be an ostomy nurse, maybe she’ll get time in the ostomy nurse area, but maybe she wants more time with the pharmacist or the radiologist.
If there is somebody who’s coming through that knows nothing about surgery, maybe they want a little bit more time in the surgical sphere. I tried to, when creating the curriculum for this, create a lot of options that existed for didactic learning as well as practical application.
You’re the assistant director of student success and development at the Medical College of Wisconsin, which launched a new Physician Associate Program. What’s happened with the program so far?
We do not have enrolled students yet. We are developing the program from the bottom up. I am one of four faculty, and then we have our founding director, Christine M. Everett, PhD, MPH, PA-C.
As we develop our program we are trying to keep a holistic approach in mind. We’re thinking about what a traditional student is vs a nontraditional student, and who we think will make great physician assistants. We pull from our own personal experiences as educators and experts in our field. As somebody who is academically minded, this program really spoke to me. Many PAs and nurse practitioners (NPs) fill a primary care role. But as we search to develop academically minded physician associates to join academic medical practices in an anticipated physician shortage, we want to hone in on some of these specialty care areas, recognizing that there is a place for us in academia and asking ‘what does that look like and how do we grow in those subspecialties?’
So, how can I help to foster that type of desire and growth and professional development in my students? That will be what we’re going to be tackling in our future cohorts.
Has the program generated a lot of interest?
Most PAs train in the region they are from and end up practicing there. So, our community and institution are very excited. There’s a lot of work in creating the program and making sure that the goals we have in mind will continue to grow with the profession. One of my neighbors who just started college reached out to me and said she wants to be a PA. We get emails regularly asking what people should do to prepare for PA school, and what are we looking for. PAs and NPs are growing professions. Both are on the top five list of best jobs ranked by U.S. News & World Report right now.
You’re the co-chair of AGA’s NPPA Task Force. What are the goals of this task force, specifically for 2025?
This is a new task force. We’re really excited about it, and we feel very supported by AGA. Specifically, we are focusing on content review and optimization. We’re working through and consulting on different proposals, such as how to have an NP/PA voice within AGA, or how certain proposals can be of interest to APPs or applicable to an APP practice.
One of our other goals is to grow our APP community opportunities, to find ways that we can all communicate with each other, share in our professional accomplishments, and be mentors and sponsors to each other to open the doors for professional growth within the GI space.
We are trying to create a sense of community within all the societies that APPs are involved in, and recognize everyone’s professional development and goals. We want to create a space to connect at some of our primary conferences and touchpoints, regardless of where your society home is.
We’ve also been asked to be a representative in helping to select the AGA-Pfizer Beacon of Hope Awards for Gender and Health Equity award recipients. We’re really proud that one of our task force members is going to be sitting on that committee to help select recipients of this award.
As a clinical expert in gastroenterology and colon and rectal surgery, you often present to national organizations like AGA, the Crohn’s and Colitis Foundation, and the American Society of Colon & Rectal Surgeons. What topics do you discuss and why?
It’s always been IBD because of my background. But I’ve also grown more in the colon/rectal surgery sphere, both in the inpatient, outpatient, and operating room setting. I enjoy presenting on topics like: What could you do right before you send a patient off to a tertiary IBD referral? I talk about complex disease management, especially the surgical realm of perianal Crohn’s disease. One of my colleagues jokes that one of her favorite talks I’ve ever given is how to perform a perianal examination. It’s a sensitive exam. I feel like I’m pretty good at it!
I also think it’s important to share information on how to write papers and how to present at conferences, because there are a lot of really smart NPs and PAs in GI and colorectal surgery who — for whatever reason — don’t know how to get their foot in the door for these types of opportunities. I love to be the person that opens that door. Do you want to be involved in a professional society? In what capacity? Making that information broadly available to everyone is something that I really love doing.
Describe a memorable patient encounter that helped shape your career.
I know this will sound so cliché, that there isn’t just one, but it’s true. There is a connection that I create with each and every one of my patients. I listen to their stories. They have whole lives outside of their disease, and I am honored that they open up to me — whether that is ongoing communication and check-ins with a patient’s family member a year after they’ve passed away, or every year receiving a Christmas card from a patient who is expanding their family because they’re finally in remission from their disease. These are the types of things that are so impactful and memorable.
Describe how you would spend a free Saturday afternoon.
I’m a mom to 7-year-old boy twins, and so I often don’t have a free Saturday. If I did, it would be sunny. I would go for a long run and then I would go out for brunch with my husband and then come home and read with my kids in a cozy blanket all day.
Lightning Round
What would you be if you weren’t a GI?
First grade teacher.
Last movie you watched?
Mufasa: The Lion King.
Best Halloween costume?
Velma from Scooby Doo.
Favorite sport?
To play – Tennis.
To watch – NBA basketball, “Go Timberwolves!”
Place you most want to travel to?
Greece
Favorite movie genre?
Rom-com.
Cat person or dog person?
Cat.
Favorite city besides the one you live in?
Manhattan.
Favorite season
Fall.
Favorite junk food?
Salty snack mix.
How many cups of coffee do you drink per day?
Three.

Million Veteran Program Drives Prostate Cancer Research
About 15,000 veterans are annually diagnosed with prostate cancer. Fortunately, those veterans enrolled in the US Department of Veterans Affairs (VA) Million Veteran Program (MVP) provide researchers with a deep pool of genetic data that can help identify causes, aid diagnosis, and guide targeted treatments.
More than 1,000,000 veterans have enrolled in MVP and donated their anonymized DNA to foster research. It is also one of the most genetically diverse health-related databases: 20% of participants identify as Black, 8% as Hispanic, 2% as Asian American, and 1% as Native American.
Ethnically and racially diverse data are particularly important for advancing the treatment of underserved groups. In a 2020 review, researchers found a number of areas where Black veterans differed from White veterans, including prostate-specific antigen (PSA) levels, incidence (almost 60% higher), clinical course, and mortality rate (2 to 3 times greater). To facilitate research, the MVP developed the “DNA chip,” a custom-designed tool that tests for > 750,000 genetic variants, including > 300,000 that are more common in minority populations.
“The whole thing about understanding genetics and diversity is like a circular feedback loop,” Director of MVP Dr. Sumitra Muralidhar said in a VA news article. “The more people you have represented from different racial and ethnic backgrounds, the more we’ll be able to discover genetic variants that contribute to their health. The more we discover, the more we can help that group. It’s a complete circular feedback loop.”
In addition to veterans’ blood samples and 600,000-plus baseline surveys on lifestyle, military service, and health, the MVP has collected upwards of 825,000 germline DNA samples, which have helped inform research into prostate cancer, the most commonly diagnosed solid tumor among veterans. By mining these data, researchers have built more evidence of how genes add to risk and disease progression.
In one study preprint that has not been peer reviewed, VA researchers investigated the significance of high polygenic hazard scores. The scores are strongly associated with age at diagnosis of any prostate cancer, as well as lifetime risk of metastatic and fatal prostate cancer. However, because they’re associated with any prostate cancer, the researchers say, there is concern that screening men with high polygenic risk could increase overdiagnosis of indolent cancers.
The researchers analyzed genetic and phenotypic data from 69,901 men in the MVP who have been diagnosed with prostate cancer (6413 metastatic). They found their hypothesis to be correct: Among men eventually diagnosed with prostate cancer, those with higher polygenic risk were more likely to develop metastatic disease.
Genetic risk scores like PHS601, a 601-variant polygenic score, can be performed on a saliva sample at any time during a person’s life, the researchers note. Thus, the scores provide the earliest information about age-specific risk of developing aggressive prostate cancer. These scores might be useful, they suggest, to support clinical decisions not only about whom to screen but also at what age.
Another study led by Stanford University researchers and published in Nature Genetics aimed to make screening more targeted, in this case prostate specific antigen screening. Estimates about PSA heritability vary from 40% to 45%, with genome-wide evaluations putting it at 25% to 30%, suggesting that incorporating genetic factors could improve screening.
This study involved 296,754 men (211,342 with European ancestry, 58,236 with African ancestry, 23,546 with Hispanic/Latino ancestry, and 3630 with Asian ancestry; 96.5% of participants were from MVP)—a sample size more than triple that in previous work.
The researchers detected 448 genome-wide significant variants, including 295 that were novel (to the best of their knowledge). The variance explained by genome-wide polygenic risk scores ranged from 11.6% to 16.6% for European ancestry, 5.5% to 9.5% for African ancestry, 13.5% to 18.2% for Hispanic/Latino ancestry, and 8.6% to 15.3% for Asian ancestry, and decreased with increasing age. Midlife genetically adjusted PSA levels were more strongly associated with overall and aggressive prostate cancer than unadjusted PSA levels.
The researchers say their study highlights how including higher proportions of participants from underrepresented populations can improve genetic prediction of PSA levels, offering the potential to personalize prostate cancer screening. Adjusting PSA for individuals’ predispositions in the absence of prostate cancer could improve the specificity (to reduce overdiagnosis) and sensitivity (to prevent more deaths) of screening.
Their findings, the researchers suggest, also explain additional variation in PSA, especially among men of African heritage, who experience the highest prostate cancer morbidity and mortality. They note that this work “moved us closer to leveraging genetic information to personalize PSA and substantially improved our understanding of PSA across diverse ancestries.”
A third study from a team at the VA Tennessee Valley Healthcare System also investigated the risk of inheriting a predisposition to prostate cancer. These researchers explored pathogenic variants using both genome-wide single-allele and identity-by-descent analytic approaches. They then tested their candidate variants for replication across independent biobanks, including MVP.
The researchers discovered the gene WNT9B E152K more than doubled the risk of familial prostate cancer. Meta-analysis, collectively encompassing 500,000 patients, confirmed the genome-wide significance. The researchers say WNT9B shares an “unexpected commonality” with the previously established prostate cancer risk genes HOXB13 and HNF1B: Each are required for embryonic prostate development. Based on that finding, the researchers also evaluated 2 additional genes, KMT2D and DHCR7, which are known to cause Mendelian genitourinary developmental defects. They, too, were nominally associated with prostate cancer under meta-analyses.
Tens of thousands of participants in MVP have had prostate cancer. The genetic research they participate in advances detection, prediction, and treatment for themselves and others, and science in general. The research is not only about finding causes, but what to do if the cancer develops. An “acting on MVP prostate cancer findings” study at VA Puget Sound Health Care System is testing how communicating with veterans about MVP prostate cancer results will affect their care. Those with prostate cancer will be screened to determine genetic contributions to their cancers. Those found to have a gene-based cancer diagnosis will be offered genetic counseling. Their immediate family will also be offered screening to test for inherited prostate cancer risk.
In 2016, the VA partnered with the Prostate Cancer Foundation to establish the Precision Oncology Program for Cancer of the Prostate (POPCaP). In collaboration with MVP and the Genomic Medicine Service, the program uses genetic information to individualize treatments for veterans with advanced prostate cancer.
US Army Veteran James Perry is one of the beneficiaries of the program. First diagnosed with prostate cancer in 2001, he was initially treated with radiation therapy, but the cancer recurred and spread to his lung. The John J. Cochran Veterans Hospital in St. Louis sent a sample of Perry's lung tumor to the laboratory for genetic testing, where they discovered he had a BRCA1 gene mutation.
His oncologist, Dr. Martin Schoen, recommended Perry enroll in AMPLITUDE, a clinical trial testing the effectiveness of poly-ADP ribose polymerase inhibitors, a new class of drugs to treat hormone-sensitive prostate cancer. One year later, Perry’s lung tumor could barely be seen on computed tomography, and his PSA levels were undetectable.
"I would highly recommend enrolling in a trial," Perry told VA Research Currents. “If a veteran has that opportunity, I would encourage it—anything that is going to give you a few more days is worth it.” In the interview, Perry said he enjoyed being part of the trial because he knows he is getting the most advanced care possible and is proud to help others like himself.
"We are honored to support VA's work to improve the lives of veterans who are living with advanced prostate cancer," Vice President and National Director of the PCF Veterans Health Initiative Rebecca Levine said. "Clinical trials play a vital role in bringing new treatments to patients who need them most. Mr. Perry's experience illustrates VA's commitment to provide state-of-the-art cancer care to all veterans who need it."
About 15,000 veterans are annually diagnosed with prostate cancer. Fortunately, those veterans enrolled in the US Department of Veterans Affairs (VA) Million Veteran Program (MVP) provide researchers with a deep pool of genetic data that can help identify causes, aid diagnosis, and guide targeted treatments.
More than 1,000,000 veterans have enrolled in MVP and donated their anonymized DNA to foster research. It is also one of the most genetically diverse health-related databases: 20% of participants identify as Black, 8% as Hispanic, 2% as Asian American, and 1% as Native American.
Ethnically and racially diverse data are particularly important for advancing the treatment of underserved groups. In a 2020 review, researchers found a number of areas where Black veterans differed from White veterans, including prostate-specific antigen (PSA) levels, incidence (almost 60% higher), clinical course, and mortality rate (2 to 3 times greater). To facilitate research, the MVP developed the “DNA chip,” a custom-designed tool that tests for > 750,000 genetic variants, including > 300,000 that are more common in minority populations.
“The whole thing about understanding genetics and diversity is like a circular feedback loop,” Director of MVP Dr. Sumitra Muralidhar said in a VA news article. “The more people you have represented from different racial and ethnic backgrounds, the more we’ll be able to discover genetic variants that contribute to their health. The more we discover, the more we can help that group. It’s a complete circular feedback loop.”
In addition to veterans’ blood samples and 600,000-plus baseline surveys on lifestyle, military service, and health, the MVP has collected upwards of 825,000 germline DNA samples, which have helped inform research into prostate cancer, the most commonly diagnosed solid tumor among veterans. By mining these data, researchers have built more evidence of how genes add to risk and disease progression.
In one study preprint that has not been peer reviewed, VA researchers investigated the significance of high polygenic hazard scores. The scores are strongly associated with age at diagnosis of any prostate cancer, as well as lifetime risk of metastatic and fatal prostate cancer. However, because they’re associated with any prostate cancer, the researchers say, there is concern that screening men with high polygenic risk could increase overdiagnosis of indolent cancers.
The researchers analyzed genetic and phenotypic data from 69,901 men in the MVP who have been diagnosed with prostate cancer (6413 metastatic). They found their hypothesis to be correct: Among men eventually diagnosed with prostate cancer, those with higher polygenic risk were more likely to develop metastatic disease.
Genetic risk scores like PHS601, a 601-variant polygenic score, can be performed on a saliva sample at any time during a person’s life, the researchers note. Thus, the scores provide the earliest information about age-specific risk of developing aggressive prostate cancer. These scores might be useful, they suggest, to support clinical decisions not only about whom to screen but also at what age.
Another study led by Stanford University researchers and published in Nature Genetics aimed to make screening more targeted, in this case prostate specific antigen screening. Estimates about PSA heritability vary from 40% to 45%, with genome-wide evaluations putting it at 25% to 30%, suggesting that incorporating genetic factors could improve screening.
This study involved 296,754 men (211,342 with European ancestry, 58,236 with African ancestry, 23,546 with Hispanic/Latino ancestry, and 3630 with Asian ancestry; 96.5% of participants were from MVP)—a sample size more than triple that in previous work.
The researchers detected 448 genome-wide significant variants, including 295 that were novel (to the best of their knowledge). The variance explained by genome-wide polygenic risk scores ranged from 11.6% to 16.6% for European ancestry, 5.5% to 9.5% for African ancestry, 13.5% to 18.2% for Hispanic/Latino ancestry, and 8.6% to 15.3% for Asian ancestry, and decreased with increasing age. Midlife genetically adjusted PSA levels were more strongly associated with overall and aggressive prostate cancer than unadjusted PSA levels.
The researchers say their study highlights how including higher proportions of participants from underrepresented populations can improve genetic prediction of PSA levels, offering the potential to personalize prostate cancer screening. Adjusting PSA for individuals’ predispositions in the absence of prostate cancer could improve the specificity (to reduce overdiagnosis) and sensitivity (to prevent more deaths) of screening.
Their findings, the researchers suggest, also explain additional variation in PSA, especially among men of African heritage, who experience the highest prostate cancer morbidity and mortality. They note that this work “moved us closer to leveraging genetic information to personalize PSA and substantially improved our understanding of PSA across diverse ancestries.”
A third study from a team at the VA Tennessee Valley Healthcare System also investigated the risk of inheriting a predisposition to prostate cancer. These researchers explored pathogenic variants using both genome-wide single-allele and identity-by-descent analytic approaches. They then tested their candidate variants for replication across independent biobanks, including MVP.
The researchers discovered the gene WNT9B E152K more than doubled the risk of familial prostate cancer. Meta-analysis, collectively encompassing 500,000 patients, confirmed the genome-wide significance. The researchers say WNT9B shares an “unexpected commonality” with the previously established prostate cancer risk genes HOXB13 and HNF1B: Each are required for embryonic prostate development. Based on that finding, the researchers also evaluated 2 additional genes, KMT2D and DHCR7, which are known to cause Mendelian genitourinary developmental defects. They, too, were nominally associated with prostate cancer under meta-analyses.
Tens of thousands of participants in MVP have had prostate cancer. The genetic research they participate in advances detection, prediction, and treatment for themselves and others, and science in general. The research is not only about finding causes, but what to do if the cancer develops. An “acting on MVP prostate cancer findings” study at VA Puget Sound Health Care System is testing how communicating with veterans about MVP prostate cancer results will affect their care. Those with prostate cancer will be screened to determine genetic contributions to their cancers. Those found to have a gene-based cancer diagnosis will be offered genetic counseling. Their immediate family will also be offered screening to test for inherited prostate cancer risk.
In 2016, the VA partnered with the Prostate Cancer Foundation to establish the Precision Oncology Program for Cancer of the Prostate (POPCaP). In collaboration with MVP and the Genomic Medicine Service, the program uses genetic information to individualize treatments for veterans with advanced prostate cancer.
US Army Veteran James Perry is one of the beneficiaries of the program. First diagnosed with prostate cancer in 2001, he was initially treated with radiation therapy, but the cancer recurred and spread to his lung. The John J. Cochran Veterans Hospital in St. Louis sent a sample of Perry's lung tumor to the laboratory for genetic testing, where they discovered he had a BRCA1 gene mutation.
His oncologist, Dr. Martin Schoen, recommended Perry enroll in AMPLITUDE, a clinical trial testing the effectiveness of poly-ADP ribose polymerase inhibitors, a new class of drugs to treat hormone-sensitive prostate cancer. One year later, Perry’s lung tumor could barely be seen on computed tomography, and his PSA levels were undetectable.
"I would highly recommend enrolling in a trial," Perry told VA Research Currents. “If a veteran has that opportunity, I would encourage it—anything that is going to give you a few more days is worth it.” In the interview, Perry said he enjoyed being part of the trial because he knows he is getting the most advanced care possible and is proud to help others like himself.
"We are honored to support VA's work to improve the lives of veterans who are living with advanced prostate cancer," Vice President and National Director of the PCF Veterans Health Initiative Rebecca Levine said. "Clinical trials play a vital role in bringing new treatments to patients who need them most. Mr. Perry's experience illustrates VA's commitment to provide state-of-the-art cancer care to all veterans who need it."
About 15,000 veterans are annually diagnosed with prostate cancer. Fortunately, those veterans enrolled in the US Department of Veterans Affairs (VA) Million Veteran Program (MVP) provide researchers with a deep pool of genetic data that can help identify causes, aid diagnosis, and guide targeted treatments.
More than 1,000,000 veterans have enrolled in MVP and donated their anonymized DNA to foster research. It is also one of the most genetically diverse health-related databases: 20% of participants identify as Black, 8% as Hispanic, 2% as Asian American, and 1% as Native American.
Ethnically and racially diverse data are particularly important for advancing the treatment of underserved groups. In a 2020 review, researchers found a number of areas where Black veterans differed from White veterans, including prostate-specific antigen (PSA) levels, incidence (almost 60% higher), clinical course, and mortality rate (2 to 3 times greater). To facilitate research, the MVP developed the “DNA chip,” a custom-designed tool that tests for > 750,000 genetic variants, including > 300,000 that are more common in minority populations.
“The whole thing about understanding genetics and diversity is like a circular feedback loop,” Director of MVP Dr. Sumitra Muralidhar said in a VA news article. “The more people you have represented from different racial and ethnic backgrounds, the more we’ll be able to discover genetic variants that contribute to their health. The more we discover, the more we can help that group. It’s a complete circular feedback loop.”
In addition to veterans’ blood samples and 600,000-plus baseline surveys on lifestyle, military service, and health, the MVP has collected upwards of 825,000 germline DNA samples, which have helped inform research into prostate cancer, the most commonly diagnosed solid tumor among veterans. By mining these data, researchers have built more evidence of how genes add to risk and disease progression.
In one study preprint that has not been peer reviewed, VA researchers investigated the significance of high polygenic hazard scores. The scores are strongly associated with age at diagnosis of any prostate cancer, as well as lifetime risk of metastatic and fatal prostate cancer. However, because they’re associated with any prostate cancer, the researchers say, there is concern that screening men with high polygenic risk could increase overdiagnosis of indolent cancers.
The researchers analyzed genetic and phenotypic data from 69,901 men in the MVP who have been diagnosed with prostate cancer (6413 metastatic). They found their hypothesis to be correct: Among men eventually diagnosed with prostate cancer, those with higher polygenic risk were more likely to develop metastatic disease.
Genetic risk scores like PHS601, a 601-variant polygenic score, can be performed on a saliva sample at any time during a person’s life, the researchers note. Thus, the scores provide the earliest information about age-specific risk of developing aggressive prostate cancer. These scores might be useful, they suggest, to support clinical decisions not only about whom to screen but also at what age.
Another study led by Stanford University researchers and published in Nature Genetics aimed to make screening more targeted, in this case prostate specific antigen screening. Estimates about PSA heritability vary from 40% to 45%, with genome-wide evaluations putting it at 25% to 30%, suggesting that incorporating genetic factors could improve screening.
This study involved 296,754 men (211,342 with European ancestry, 58,236 with African ancestry, 23,546 with Hispanic/Latino ancestry, and 3630 with Asian ancestry; 96.5% of participants were from MVP)—a sample size more than triple that in previous work.
The researchers detected 448 genome-wide significant variants, including 295 that were novel (to the best of their knowledge). The variance explained by genome-wide polygenic risk scores ranged from 11.6% to 16.6% for European ancestry, 5.5% to 9.5% for African ancestry, 13.5% to 18.2% for Hispanic/Latino ancestry, and 8.6% to 15.3% for Asian ancestry, and decreased with increasing age. Midlife genetically adjusted PSA levels were more strongly associated with overall and aggressive prostate cancer than unadjusted PSA levels.
The researchers say their study highlights how including higher proportions of participants from underrepresented populations can improve genetic prediction of PSA levels, offering the potential to personalize prostate cancer screening. Adjusting PSA for individuals’ predispositions in the absence of prostate cancer could improve the specificity (to reduce overdiagnosis) and sensitivity (to prevent more deaths) of screening.
Their findings, the researchers suggest, also explain additional variation in PSA, especially among men of African heritage, who experience the highest prostate cancer morbidity and mortality. They note that this work “moved us closer to leveraging genetic information to personalize PSA and substantially improved our understanding of PSA across diverse ancestries.”
A third study from a team at the VA Tennessee Valley Healthcare System also investigated the risk of inheriting a predisposition to prostate cancer. These researchers explored pathogenic variants using both genome-wide single-allele and identity-by-descent analytic approaches. They then tested their candidate variants for replication across independent biobanks, including MVP.
The researchers discovered the gene WNT9B E152K more than doubled the risk of familial prostate cancer. Meta-analysis, collectively encompassing 500,000 patients, confirmed the genome-wide significance. The researchers say WNT9B shares an “unexpected commonality” with the previously established prostate cancer risk genes HOXB13 and HNF1B: Each are required for embryonic prostate development. Based on that finding, the researchers also evaluated 2 additional genes, KMT2D and DHCR7, which are known to cause Mendelian genitourinary developmental defects. They, too, were nominally associated with prostate cancer under meta-analyses.
Tens of thousands of participants in MVP have had prostate cancer. The genetic research they participate in advances detection, prediction, and treatment for themselves and others, and science in general. The research is not only about finding causes, but what to do if the cancer develops. An “acting on MVP prostate cancer findings” study at VA Puget Sound Health Care System is testing how communicating with veterans about MVP prostate cancer results will affect their care. Those with prostate cancer will be screened to determine genetic contributions to their cancers. Those found to have a gene-based cancer diagnosis will be offered genetic counseling. Their immediate family will also be offered screening to test for inherited prostate cancer risk.
In 2016, the VA partnered with the Prostate Cancer Foundation to establish the Precision Oncology Program for Cancer of the Prostate (POPCaP). In collaboration with MVP and the Genomic Medicine Service, the program uses genetic information to individualize treatments for veterans with advanced prostate cancer.
US Army Veteran James Perry is one of the beneficiaries of the program. First diagnosed with prostate cancer in 2001, he was initially treated with radiation therapy, but the cancer recurred and spread to his lung. The John J. Cochran Veterans Hospital in St. Louis sent a sample of Perry's lung tumor to the laboratory for genetic testing, where they discovered he had a BRCA1 gene mutation.
His oncologist, Dr. Martin Schoen, recommended Perry enroll in AMPLITUDE, a clinical trial testing the effectiveness of poly-ADP ribose polymerase inhibitors, a new class of drugs to treat hormone-sensitive prostate cancer. One year later, Perry’s lung tumor could barely be seen on computed tomography, and his PSA levels were undetectable.
"I would highly recommend enrolling in a trial," Perry told VA Research Currents. “If a veteran has that opportunity, I would encourage it—anything that is going to give you a few more days is worth it.” In the interview, Perry said he enjoyed being part of the trial because he knows he is getting the most advanced care possible and is proud to help others like himself.
"We are honored to support VA's work to improve the lives of veterans who are living with advanced prostate cancer," Vice President and National Director of the PCF Veterans Health Initiative Rebecca Levine said. "Clinical trials play a vital role in bringing new treatments to patients who need them most. Mr. Perry's experience illustrates VA's commitment to provide state-of-the-art cancer care to all veterans who need it."
AVAHO Encourages Members to Make Voices Heard
Advocacy for veterans with cancer has always been a central part of the Association for VA Hematology/Oncology (AVAHO) mission, but that advocacy has now taken on a new focus: the fate of US Department of Veterans Affairs (VA) employees. The advocacy portal provides templated letters, a search function to find local Senators and Members of Congress, a search function to find regional media outlets, updates on voting and elections, and information on key legislation relevant to VA health care.
To ensure its members’ concerns are heard, AVAHO is encouraging members, in their own time and as private citizens, to contact their local representatives to inform them about the real impact of recent policy changes on VA employees and the veterans they care for. Members can select any of 4 letters focused on reductions in force, cancellation of VA contracts, the return to office mandate, and the National Institutes of Health’s proposed cap on indirect cost for research grants: “AVAHO recognizes the power of the individual voice. Our members have an important role in shaping the health care services provided to veterans across our nation.”
"The contracts that have been canceled and continue to be canceled included critical services related to cancer care," AVAHO notes on its Advocacy page. "We know these impacted contracts have hindered the VA’s ability to implement research protocols, process and report pharmacogenomic results, manage Electronic Health Record Modernization workgroups responsible for safety improvements, and execute new oncology services through the Close to Me initiative, just to name a few."
Advocacy for veterans with cancer has always been a central part of the Association for VA Hematology/Oncology (AVAHO) mission, but that advocacy has now taken on a new focus: the fate of US Department of Veterans Affairs (VA) employees. The advocacy portal provides templated letters, a search function to find local Senators and Members of Congress, a search function to find regional media outlets, updates on voting and elections, and information on key legislation relevant to VA health care.
To ensure its members’ concerns are heard, AVAHO is encouraging members, in their own time and as private citizens, to contact their local representatives to inform them about the real impact of recent policy changes on VA employees and the veterans they care for. Members can select any of 4 letters focused on reductions in force, cancellation of VA contracts, the return to office mandate, and the National Institutes of Health’s proposed cap on indirect cost for research grants: “AVAHO recognizes the power of the individual voice. Our members have an important role in shaping the health care services provided to veterans across our nation.”
"The contracts that have been canceled and continue to be canceled included critical services related to cancer care," AVAHO notes on its Advocacy page. "We know these impacted contracts have hindered the VA’s ability to implement research protocols, process and report pharmacogenomic results, manage Electronic Health Record Modernization workgroups responsible for safety improvements, and execute new oncology services through the Close to Me initiative, just to name a few."
Advocacy for veterans with cancer has always been a central part of the Association for VA Hematology/Oncology (AVAHO) mission, but that advocacy has now taken on a new focus: the fate of US Department of Veterans Affairs (VA) employees. The advocacy portal provides templated letters, a search function to find local Senators and Members of Congress, a search function to find regional media outlets, updates on voting and elections, and information on key legislation relevant to VA health care.
To ensure its members’ concerns are heard, AVAHO is encouraging members, in their own time and as private citizens, to contact their local representatives to inform them about the real impact of recent policy changes on VA employees and the veterans they care for. Members can select any of 4 letters focused on reductions in force, cancellation of VA contracts, the return to office mandate, and the National Institutes of Health’s proposed cap on indirect cost for research grants: “AVAHO recognizes the power of the individual voice. Our members have an important role in shaping the health care services provided to veterans across our nation.”
"The contracts that have been canceled and continue to be canceled included critical services related to cancer care," AVAHO notes on its Advocacy page. "We know these impacted contracts have hindered the VA’s ability to implement research protocols, process and report pharmacogenomic results, manage Electronic Health Record Modernization workgroups responsible for safety improvements, and execute new oncology services through the Close to Me initiative, just to name a few."
GI Doc Empowers Female Patients ‘To Be Themselves’
Pooja Singhal, MD, AGAF, will never forget the time a female patient came in for gastroesophageal reflux disease and dysphagia treatment, revealing that she had already gone through multiple gastroenterologists to help diagnose and treat her ailments.
“We spent a whole visit talking about it,” said Dr. Singhal, a gastroenterologist, hepatologist, and obesity medicine specialist at Oklahoma Gastro Health and Wellness in Oklahoma City. During the exam, she discovered that her middle-aged patient was wearing an adult diaper for diarrhea and leakage.
Previous GI doctors told the patient they couldn’t help her and that she had to live with these symptoms. “I was just so shocked. I told her: This is not normal. Let’s talk more about it. Let’s figure out how we can manage it,” said Dr. Singhal, who has spent her career advocating for more education about GI conditions.
There are real barriers to patients opening up and sharing their symptoms, especially if they’re female. while ensuring that the correct knowledge gets across to the public, said Dr. Singhal.
An alumna of the American Gastroenterological Association’s (AGA) Future Leaders Program, Dr. Singhal has served as the private practice course director for AGA’s Midwest Women in GI Workshop. She is a also a four-time recipient of the SCOPY award for her work in raising community awareness of colorectal cancer prevention in Oklahoma. In an interview, she discussed the critical role women GI doctors play in assisting the unique needs of female patients, and why it takes a village of doctors to treat the complexities of GI disorders.
Why did you choose GI, and more specifically, what brought about your interest in women’s GI issues?
GI is simply the best field. While I was doing my rotation in GI as a resident, I was enthralled and humbled that the field of gastroenterology offered an opportunity to prevent cancer. Colon cancer is the second leading cause of cancer related deaths, and when I realized that we could do these micro-interventions during a procedure to remove polyps that could potentially turn into cancer — or give us an opportunity to remove carcinoma in situ — that’s what really inspired me and piqued my interest in GI. As I continued to learn and explore GI more, I appreciated the opportunity the field gave us in terms of using both sides of our brains equally, the right side and the left side.
I love the diagnostic part of medicine. You have this privilege to be able to diagnose so many different diseases and perform procedures using technical skills, exploring everything from the esophagus, liver, pancreas, small bowel, and colon.
But what I really appreciate about gastroenterology is how it’s piqued my interest in women’s digestive health. How it became very close to my heart is really from my patients. I’ve learned a lot from my patients throughout the years. When I was much younger, I don’t know if I really appreciated the vulnerability it takes as a woman to go to a physician and talk about hemorrhoids and diarrhea.
One of the comments I often receive is: ‘Oh, thank God you’re a female GI. I can be myself. I can share something personal and you would understand.’
Your practice places a specific emphasis on health and wellness. Can you provide some examples of how you incorporate wellness into treatment?
I feel like wellness is very commonplace now. To me, the definition of wellness is about practicing healthy habits to attain your maximum potential, both physically and mentally — to feel the best you can. My practice specifically tries to achieve that goal by placing a strong emphasis on education and communication. We provide journals where patients can keep track of their symptoms. We encourage a lot of discussion during visits, where we talk about GI diseases and how to prevent them, or to prevent them from happening again. If you’re going to do a hemorrhoid treatment that offers hemorrhoid banding, we talk about it in detail with the patient; we don’t just do the procedure.
We have a dietitian on staff for conditions like inflammatory bowel disease, Crohn’s and ulcerative colitis, celiac disease, IBS. Some of our older patients have pelvic organ prolapse and fecal incontinence. We have a pelvic floor therapist and a urogynecologist, and we work very closely with ob-gyn teams. My practice also takes pride in communicating with primary care physicians. We’ve had patients who have had memory loss or dementia or are grieving the loss of a loved one. And we prioritize communicating and treating patients as a whole and not focusing on just their GI symptoms.
As an advocate for community education on GI disorders, where is education lacking in this field?
I think education is lacking because there is an information delivery gap. I feel the public consumes information in the form of short social media reels. The attention span is so short and any scientific information, especially around diseases, can be scary and overwhelming. Whereas I think a lot of the medical community still interacts and exchanges information in terms of journals and publications. So, we are not really trained necessarily to talk about diseases in very simple terms.
We need more advocacy efforts on Capitol Hill. AGA has been good about doing advocacy work. I had an opportunity to go to Capitol Hill a couple of times and really advocate for policy around obesity medicine coverage and procedure coverage. I was fortunate to learn so much about healthcare policy, but it also made me appreciate that there are a lot of gaps in terms of understanding common medical diseases.
You’re trained in the Orbera Intragastric balloon system for weight reduction. How does this procedure differentiate from other bariatric procedures?
Intragastric balloon is Food and Drug Administration approved for weight loss. It’s a temporary medical device, so it’s reversible. No. 2, it’s a nonsurgical intervention, so it’s usually done in an outpatient setting. We basically place a deflated gastric balloon endoscopically, similar to an upper endoscopy method. We take a pin endoscope, a deflated balloon, which is made of medical-grade material, and we inflate it with adequate fluid. The concept is when the balloon is inflated, it provides satiety. It reduces the amount of space in the stomach for food. It slows down how quickly the food is going to leave. So you feel full much of the time. And it also helps decrease a hormone called ghrelin, which is responsible for hunger. It can make a big difference when people are gaining weight and in that category of overweight before they progress to obese.
As I tell everybody, obesity is a chronic lifelong disease that is very complex and requires lifelong efforts. So, it’s truly a journey. What’s made this procedure a success is follow-up and the continued efforts of dietitians and counseling and incorporating physical exercise, because maintenance of that weight loss is also very important. Our goal is always sustained weight loss and not just short-term weight loss.
As the practice course director for the AGA’s Midwest Women in GI Workshop, can you tell me how this course came about? What does the workshop cover?
This workshop is a brainchild of AGA. This will be the third year of having these workshops. It’s been divided into regional workshops, so more people can attend. But it arose from the recognition that there is a need to have a support system, a forum where discussions on navigating career and life transitions with grace can happen, and more resources for success can be provided.
There is so much power in learning from shared experiences. And I think that was huge, to realize that we are not alone. We can celebrate our achievements together and acknowledge our challenges together, and then come together to brainstorm and innovate to solve problems and advocate for health equity.
You’ve been involved with community, non-profit organizations like the Homeless Alliance in Oklahoma City. How has this work enriched your life outside of medicine?
I feel like we sometimes get tunnel vision, talking to people in the same line of work. It was extremely important for me to broaden my horizons by learning from people outside of the medical community and from organizations like Homeless Alliance, which allowed me a platform to understand what my community needs. It’s an incredible organization that helps provide shelter not only for human beings, but also pets. The freezing temperatures over the last few months provided unique challenges like overflow in homeless shelters. I’ve learned so many things, such as how to ask for grants and how to allocate those funds. It has been absolutely enriching to me to learn about my community needs and see what an amazing difference people in the community are making.
Pooja Singhal, MD, AGAF, will never forget the time a female patient came in for gastroesophageal reflux disease and dysphagia treatment, revealing that she had already gone through multiple gastroenterologists to help diagnose and treat her ailments.
“We spent a whole visit talking about it,” said Dr. Singhal, a gastroenterologist, hepatologist, and obesity medicine specialist at Oklahoma Gastro Health and Wellness in Oklahoma City. During the exam, she discovered that her middle-aged patient was wearing an adult diaper for diarrhea and leakage.
Previous GI doctors told the patient they couldn’t help her and that she had to live with these symptoms. “I was just so shocked. I told her: This is not normal. Let’s talk more about it. Let’s figure out how we can manage it,” said Dr. Singhal, who has spent her career advocating for more education about GI conditions.
There are real barriers to patients opening up and sharing their symptoms, especially if they’re female. while ensuring that the correct knowledge gets across to the public, said Dr. Singhal.
An alumna of the American Gastroenterological Association’s (AGA) Future Leaders Program, Dr. Singhal has served as the private practice course director for AGA’s Midwest Women in GI Workshop. She is a also a four-time recipient of the SCOPY award for her work in raising community awareness of colorectal cancer prevention in Oklahoma. In an interview, she discussed the critical role women GI doctors play in assisting the unique needs of female patients, and why it takes a village of doctors to treat the complexities of GI disorders.
Why did you choose GI, and more specifically, what brought about your interest in women’s GI issues?
GI is simply the best field. While I was doing my rotation in GI as a resident, I was enthralled and humbled that the field of gastroenterology offered an opportunity to prevent cancer. Colon cancer is the second leading cause of cancer related deaths, and when I realized that we could do these micro-interventions during a procedure to remove polyps that could potentially turn into cancer — or give us an opportunity to remove carcinoma in situ — that’s what really inspired me and piqued my interest in GI. As I continued to learn and explore GI more, I appreciated the opportunity the field gave us in terms of using both sides of our brains equally, the right side and the left side.
I love the diagnostic part of medicine. You have this privilege to be able to diagnose so many different diseases and perform procedures using technical skills, exploring everything from the esophagus, liver, pancreas, small bowel, and colon.
But what I really appreciate about gastroenterology is how it’s piqued my interest in women’s digestive health. How it became very close to my heart is really from my patients. I’ve learned a lot from my patients throughout the years. When I was much younger, I don’t know if I really appreciated the vulnerability it takes as a woman to go to a physician and talk about hemorrhoids and diarrhea.
One of the comments I often receive is: ‘Oh, thank God you’re a female GI. I can be myself. I can share something personal and you would understand.’
Your practice places a specific emphasis on health and wellness. Can you provide some examples of how you incorporate wellness into treatment?
I feel like wellness is very commonplace now. To me, the definition of wellness is about practicing healthy habits to attain your maximum potential, both physically and mentally — to feel the best you can. My practice specifically tries to achieve that goal by placing a strong emphasis on education and communication. We provide journals where patients can keep track of their symptoms. We encourage a lot of discussion during visits, where we talk about GI diseases and how to prevent them, or to prevent them from happening again. If you’re going to do a hemorrhoid treatment that offers hemorrhoid banding, we talk about it in detail with the patient; we don’t just do the procedure.
We have a dietitian on staff for conditions like inflammatory bowel disease, Crohn’s and ulcerative colitis, celiac disease, IBS. Some of our older patients have pelvic organ prolapse and fecal incontinence. We have a pelvic floor therapist and a urogynecologist, and we work very closely with ob-gyn teams. My practice also takes pride in communicating with primary care physicians. We’ve had patients who have had memory loss or dementia or are grieving the loss of a loved one. And we prioritize communicating and treating patients as a whole and not focusing on just their GI symptoms.
As an advocate for community education on GI disorders, where is education lacking in this field?
I think education is lacking because there is an information delivery gap. I feel the public consumes information in the form of short social media reels. The attention span is so short and any scientific information, especially around diseases, can be scary and overwhelming. Whereas I think a lot of the medical community still interacts and exchanges information in terms of journals and publications. So, we are not really trained necessarily to talk about diseases in very simple terms.
We need more advocacy efforts on Capitol Hill. AGA has been good about doing advocacy work. I had an opportunity to go to Capitol Hill a couple of times and really advocate for policy around obesity medicine coverage and procedure coverage. I was fortunate to learn so much about healthcare policy, but it also made me appreciate that there are a lot of gaps in terms of understanding common medical diseases.
You’re trained in the Orbera Intragastric balloon system for weight reduction. How does this procedure differentiate from other bariatric procedures?
Intragastric balloon is Food and Drug Administration approved for weight loss. It’s a temporary medical device, so it’s reversible. No. 2, it’s a nonsurgical intervention, so it’s usually done in an outpatient setting. We basically place a deflated gastric balloon endoscopically, similar to an upper endoscopy method. We take a pin endoscope, a deflated balloon, which is made of medical-grade material, and we inflate it with adequate fluid. The concept is when the balloon is inflated, it provides satiety. It reduces the amount of space in the stomach for food. It slows down how quickly the food is going to leave. So you feel full much of the time. And it also helps decrease a hormone called ghrelin, which is responsible for hunger. It can make a big difference when people are gaining weight and in that category of overweight before they progress to obese.
As I tell everybody, obesity is a chronic lifelong disease that is very complex and requires lifelong efforts. So, it’s truly a journey. What’s made this procedure a success is follow-up and the continued efforts of dietitians and counseling and incorporating physical exercise, because maintenance of that weight loss is also very important. Our goal is always sustained weight loss and not just short-term weight loss.
As the practice course director for the AGA’s Midwest Women in GI Workshop, can you tell me how this course came about? What does the workshop cover?
This workshop is a brainchild of AGA. This will be the third year of having these workshops. It’s been divided into regional workshops, so more people can attend. But it arose from the recognition that there is a need to have a support system, a forum where discussions on navigating career and life transitions with grace can happen, and more resources for success can be provided.
There is so much power in learning from shared experiences. And I think that was huge, to realize that we are not alone. We can celebrate our achievements together and acknowledge our challenges together, and then come together to brainstorm and innovate to solve problems and advocate for health equity.
You’ve been involved with community, non-profit organizations like the Homeless Alliance in Oklahoma City. How has this work enriched your life outside of medicine?
I feel like we sometimes get tunnel vision, talking to people in the same line of work. It was extremely important for me to broaden my horizons by learning from people outside of the medical community and from organizations like Homeless Alliance, which allowed me a platform to understand what my community needs. It’s an incredible organization that helps provide shelter not only for human beings, but also pets. The freezing temperatures over the last few months provided unique challenges like overflow in homeless shelters. I’ve learned so many things, such as how to ask for grants and how to allocate those funds. It has been absolutely enriching to me to learn about my community needs and see what an amazing difference people in the community are making.
Pooja Singhal, MD, AGAF, will never forget the time a female patient came in for gastroesophageal reflux disease and dysphagia treatment, revealing that she had already gone through multiple gastroenterologists to help diagnose and treat her ailments.
“We spent a whole visit talking about it,” said Dr. Singhal, a gastroenterologist, hepatologist, and obesity medicine specialist at Oklahoma Gastro Health and Wellness in Oklahoma City. During the exam, she discovered that her middle-aged patient was wearing an adult diaper for diarrhea and leakage.
Previous GI doctors told the patient they couldn’t help her and that she had to live with these symptoms. “I was just so shocked. I told her: This is not normal. Let’s talk more about it. Let’s figure out how we can manage it,” said Dr. Singhal, who has spent her career advocating for more education about GI conditions.
There are real barriers to patients opening up and sharing their symptoms, especially if they’re female. while ensuring that the correct knowledge gets across to the public, said Dr. Singhal.
An alumna of the American Gastroenterological Association’s (AGA) Future Leaders Program, Dr. Singhal has served as the private practice course director for AGA’s Midwest Women in GI Workshop. She is a also a four-time recipient of the SCOPY award for her work in raising community awareness of colorectal cancer prevention in Oklahoma. In an interview, she discussed the critical role women GI doctors play in assisting the unique needs of female patients, and why it takes a village of doctors to treat the complexities of GI disorders.
Why did you choose GI, and more specifically, what brought about your interest in women’s GI issues?
GI is simply the best field. While I was doing my rotation in GI as a resident, I was enthralled and humbled that the field of gastroenterology offered an opportunity to prevent cancer. Colon cancer is the second leading cause of cancer related deaths, and when I realized that we could do these micro-interventions during a procedure to remove polyps that could potentially turn into cancer — or give us an opportunity to remove carcinoma in situ — that’s what really inspired me and piqued my interest in GI. As I continued to learn and explore GI more, I appreciated the opportunity the field gave us in terms of using both sides of our brains equally, the right side and the left side.
I love the diagnostic part of medicine. You have this privilege to be able to diagnose so many different diseases and perform procedures using technical skills, exploring everything from the esophagus, liver, pancreas, small bowel, and colon.
But what I really appreciate about gastroenterology is how it’s piqued my interest in women’s digestive health. How it became very close to my heart is really from my patients. I’ve learned a lot from my patients throughout the years. When I was much younger, I don’t know if I really appreciated the vulnerability it takes as a woman to go to a physician and talk about hemorrhoids and diarrhea.
One of the comments I often receive is: ‘Oh, thank God you’re a female GI. I can be myself. I can share something personal and you would understand.’
Your practice places a specific emphasis on health and wellness. Can you provide some examples of how you incorporate wellness into treatment?
I feel like wellness is very commonplace now. To me, the definition of wellness is about practicing healthy habits to attain your maximum potential, both physically and mentally — to feel the best you can. My practice specifically tries to achieve that goal by placing a strong emphasis on education and communication. We provide journals where patients can keep track of their symptoms. We encourage a lot of discussion during visits, where we talk about GI diseases and how to prevent them, or to prevent them from happening again. If you’re going to do a hemorrhoid treatment that offers hemorrhoid banding, we talk about it in detail with the patient; we don’t just do the procedure.
We have a dietitian on staff for conditions like inflammatory bowel disease, Crohn’s and ulcerative colitis, celiac disease, IBS. Some of our older patients have pelvic organ prolapse and fecal incontinence. We have a pelvic floor therapist and a urogynecologist, and we work very closely with ob-gyn teams. My practice also takes pride in communicating with primary care physicians. We’ve had patients who have had memory loss or dementia or are grieving the loss of a loved one. And we prioritize communicating and treating patients as a whole and not focusing on just their GI symptoms.
As an advocate for community education on GI disorders, where is education lacking in this field?
I think education is lacking because there is an information delivery gap. I feel the public consumes information in the form of short social media reels. The attention span is so short and any scientific information, especially around diseases, can be scary and overwhelming. Whereas I think a lot of the medical community still interacts and exchanges information in terms of journals and publications. So, we are not really trained necessarily to talk about diseases in very simple terms.
We need more advocacy efforts on Capitol Hill. AGA has been good about doing advocacy work. I had an opportunity to go to Capitol Hill a couple of times and really advocate for policy around obesity medicine coverage and procedure coverage. I was fortunate to learn so much about healthcare policy, but it also made me appreciate that there are a lot of gaps in terms of understanding common medical diseases.
You’re trained in the Orbera Intragastric balloon system for weight reduction. How does this procedure differentiate from other bariatric procedures?
Intragastric balloon is Food and Drug Administration approved for weight loss. It’s a temporary medical device, so it’s reversible. No. 2, it’s a nonsurgical intervention, so it’s usually done in an outpatient setting. We basically place a deflated gastric balloon endoscopically, similar to an upper endoscopy method. We take a pin endoscope, a deflated balloon, which is made of medical-grade material, and we inflate it with adequate fluid. The concept is when the balloon is inflated, it provides satiety. It reduces the amount of space in the stomach for food. It slows down how quickly the food is going to leave. So you feel full much of the time. And it also helps decrease a hormone called ghrelin, which is responsible for hunger. It can make a big difference when people are gaining weight and in that category of overweight before they progress to obese.
As I tell everybody, obesity is a chronic lifelong disease that is very complex and requires lifelong efforts. So, it’s truly a journey. What’s made this procedure a success is follow-up and the continued efforts of dietitians and counseling and incorporating physical exercise, because maintenance of that weight loss is also very important. Our goal is always sustained weight loss and not just short-term weight loss.
As the practice course director for the AGA’s Midwest Women in GI Workshop, can you tell me how this course came about? What does the workshop cover?
This workshop is a brainchild of AGA. This will be the third year of having these workshops. It’s been divided into regional workshops, so more people can attend. But it arose from the recognition that there is a need to have a support system, a forum where discussions on navigating career and life transitions with grace can happen, and more resources for success can be provided.
There is so much power in learning from shared experiences. And I think that was huge, to realize that we are not alone. We can celebrate our achievements together and acknowledge our challenges together, and then come together to brainstorm and innovate to solve problems and advocate for health equity.
You’ve been involved with community, non-profit organizations like the Homeless Alliance in Oklahoma City. How has this work enriched your life outside of medicine?
I feel like we sometimes get tunnel vision, talking to people in the same line of work. It was extremely important for me to broaden my horizons by learning from people outside of the medical community and from organizations like Homeless Alliance, which allowed me a platform to understand what my community needs. It’s an incredible organization that helps provide shelter not only for human beings, but also pets. The freezing temperatures over the last few months provided unique challenges like overflow in homeless shelters. I’ve learned so many things, such as how to ask for grants and how to allocate those funds. It has been absolutely enriching to me to learn about my community needs and see what an amazing difference people in the community are making.

Endoscopist Brings Cutting-Edge Tech to Asia-Pacific Region
As the COVID-19 crisis unfolded in early 2020, Tossapol Kerdsirichairat, MD, faced another challenge: his mother’s ovarian cancer diagnosis.
“She chose to remain in Thailand, so I decided to relocate to care for her,” said Dr. Kerdsirichairat, an interventional endoscopist who completed fellowships at the University of Michigan, Ann Arbor, and Johns Hopkins University in Baltimore. The move to Bangkok turned out to be one of the best decisions of his life, he said, as he could support his mother while introducing advanced endoscopic techniques and devices to the region.
“Bangkok is a hub for medical innovation in Asia, offering opportunities to work with a diverse patient population and access to cutting-edge technology,” said Dr. Kerdsirichairat, who works at Bumrungrad International Hospital as a clinical associate professor.
The program is the first of its kind in Thailand and one of the few in the Asia-Pacific region.
“I guide patients and families through understanding their risks and implementing preventive strategies, collaborating with multidisciplinary teams to ensure comprehensive care. It’s incredibly rewarding to see the impact of early tumor detection,” said Dr. Kerdsirichairat, an international member of AGA who was a participant in the AGA Young Delegates Program.
He has set several records in Thailand for the smallest tumor detected, including a 0.3-millimeter (mm) esophageal tumor, a 0.8-mm tumor for stomach cancer, a 5-mm pancreatic tumor, and a 1-mm tumor for colon cancer.
“These were detected through high-standard screening programs, as patients often do not develop symptoms from these subtle lesions,” said Dr. Kerdsirichairat, who discussed in an interview the unique challenges of practicing overseas.
Why did you choose GI?
Gastroenterology is a specialty that uniquely integrates procedural skill, clinical decision making, and a deep understanding of complex biological systems. I was drawn especially to the ability to make a direct and meaningful impact in patients’ lives through advanced endoscopic procedures, while also addressing both acute and chronic diseases, and focusing on cancer prevention. It is incredibly rewarding to perform an endoscopic retrograde cholangiopancreatography (ERCP) for cholangitis and see a patient return to normal the very next day, or to perform an endoscopic ultrasound (EUS) for pancreatic cancer screening in high-risk individuals and detect a sub-centimeter pancreatic tumor.
Realizing that early detection can improve survival by threefold after surgery is a powerful reminder of the difference we can make in patients’ lives. This specialty requires a delicate balance of precision and empathy, which perfectly aligns with my strengths and values as a physician.
You have a wide variety of clinical interests, from endoscopic procedures to cancer research to GERD. What’s your key subspecialty and why?
My primary specialty is advanced endoscopy, which includes techniques such as EUS, ERCP, and endoscopic resection of precancerous and early cancerous lesions. I also focus on cutting-edge, evidence-based techniques recently included in clinical guidelines, such as Transoral Incisionless Fundoplication (TIF). These minimally invasive options allow me to diagnose and treat conditions that once required surgery. The precision and innovation involved in advanced endoscopy enable me to effectively manage complex cases—from diagnosing early cancers to managing bile duct obstructions and resecting precancerous lesions.
Can you describe your work in cancer genetics and screening?
I am deeply committed to the early detection of gastrointestinal cancers, particularly through screening for precancerous conditions and hereditary syndromes. During my general GI training at the University of Michigan, I had the privilege of working with Grace Elta, MD, AGAF, and Michelle Anderson, MD, MSc, renowned experts in pancreatic cancer management. I was later trained by Anne Marie Lennon, PhD, AGAF, who pioneered the liquid biopsy technique for cancer screening through the CancerSEEK project, and Marcia (Mimi) Canto, MD, MHS, who initiated the Cancer of the Pancreas Screening project for high-risk individuals of pancreatic cancer.
I also had the distinction of being the first at Bumrungrad International Hospital to perform endoscopic drainage for pancreatic fluid collections in the setting of multi-organ failure. This endoscopic approach has been extensively validated in the medical literature as significantly improving survival rates compared to surgical drainage. My training in this specialized procedure was conducted under the guidance of the premier group for necrotizing pancreatitis, led by Martin Freeman, MD, at the University of Minnesota.
Later, I contributed to overseeing the Inherited Gastrointestinal Malignancy Clinic of MyCode, a large-scale population-based cohort program focused on cancer screening in Pennsylvania. By December 2024, MyCode had collected blood samples from over 258,000 individuals, analyzed DNA sequences from over 184,000, and provided clinical data that benefits over 142,000 patients. It’s not uncommon for healthy 25-year-old patients to come to our clinic for colon cancer screening after learning from the program that they carry a cancer syndrome, and early screening can potentially save their lives.
What are the key differences between training and practicing medicine in the United States and in an Asian country?
The U.S. healthcare system is deeply rooted in evidence-based protocols and multidisciplinary care, driven by an insurance-based model. In contrast, many Asian countries face challenges such as the dependency on government approval for certain treatments and insurance limitations. Practicing in Asia requires navigating unique cultural, economic, and systemic differences, including varying resource availability and disease prevalence.
What specific challenges have you faced as a GI in Thailand?
As an advanced endoscopist, one of the biggest challenges I faced initially was the difficulty in obtaining the same devices I used in the U.S. for use in Thailand. With support from device companies and mentors in the U.S., I was able to perform groundbreaking procedures, such as the TIF in Southeast Asia and the first use of a full-thickness resection device in Thailand. I am also proud to be part of one of the first few centers worldwide performing the combination of injectable semaglutide and endoscopic sleeve gastroplasty, resulting in a remarkable weight reduction of 44%, comparable to surgical gastric bypass.
In addition, Bumrungrad International Hospital, where I practice, sees over 1.1 million visits annually from patients from more than 190 countries. This offers a unique opportunity to engage with a global patient base and learn from diverse cultures. Over time, although the hospital has professional interpreters for all languages, I have become able to communicate basic sentences with international patients in their preferred languages, including Chinese, Japanese, and Arabic, which has enriched my practice.
What’s your favorite thing to do when you’re not practicing GI?
I enjoy traveling, exploring new cuisines, and spending quality time with family and friends. These activities help me recharge and offer fresh perspectives on life.
Lightning Round
Texting or talking?
Talking. It’s more personal and meaningful.
Favorite city in the U.S.?
Ann Arbor, Michigan
Cat or dog person?
Dog person
Favorite junk food?
Pizza
How many cups of coffee do you drink per day?
Two – just enough to stay sharp, but not jittery.
If you weren’t a GI, what would you be?
Architect
Best place you went on vacation?
Kyoto, Japan
Favorite sport?
Skiing
Favorite ice cream?
Matcha green tea
What song do you have to sing along with when you hear it?
“Everybody” by Backstreet Boys
Favorite movie or TV show?
Forrest Gump and Friends
Optimist or pessimist?
Optimist. I believe in focusing on solutions and possibilities.
As the COVID-19 crisis unfolded in early 2020, Tossapol Kerdsirichairat, MD, faced another challenge: his mother’s ovarian cancer diagnosis.
“She chose to remain in Thailand, so I decided to relocate to care for her,” said Dr. Kerdsirichairat, an interventional endoscopist who completed fellowships at the University of Michigan, Ann Arbor, and Johns Hopkins University in Baltimore. The move to Bangkok turned out to be one of the best decisions of his life, he said, as he could support his mother while introducing advanced endoscopic techniques and devices to the region.
“Bangkok is a hub for medical innovation in Asia, offering opportunities to work with a diverse patient population and access to cutting-edge technology,” said Dr. Kerdsirichairat, who works at Bumrungrad International Hospital as a clinical associate professor.
The program is the first of its kind in Thailand and one of the few in the Asia-Pacific region.
“I guide patients and families through understanding their risks and implementing preventive strategies, collaborating with multidisciplinary teams to ensure comprehensive care. It’s incredibly rewarding to see the impact of early tumor detection,” said Dr. Kerdsirichairat, an international member of AGA who was a participant in the AGA Young Delegates Program.
He has set several records in Thailand for the smallest tumor detected, including a 0.3-millimeter (mm) esophageal tumor, a 0.8-mm tumor for stomach cancer, a 5-mm pancreatic tumor, and a 1-mm tumor for colon cancer.
“These were detected through high-standard screening programs, as patients often do not develop symptoms from these subtle lesions,” said Dr. Kerdsirichairat, who discussed in an interview the unique challenges of practicing overseas.
Why did you choose GI?
Gastroenterology is a specialty that uniquely integrates procedural skill, clinical decision making, and a deep understanding of complex biological systems. I was drawn especially to the ability to make a direct and meaningful impact in patients’ lives through advanced endoscopic procedures, while also addressing both acute and chronic diseases, and focusing on cancer prevention. It is incredibly rewarding to perform an endoscopic retrograde cholangiopancreatography (ERCP) for cholangitis and see a patient return to normal the very next day, or to perform an endoscopic ultrasound (EUS) for pancreatic cancer screening in high-risk individuals and detect a sub-centimeter pancreatic tumor.
Realizing that early detection can improve survival by threefold after surgery is a powerful reminder of the difference we can make in patients’ lives. This specialty requires a delicate balance of precision and empathy, which perfectly aligns with my strengths and values as a physician.
You have a wide variety of clinical interests, from endoscopic procedures to cancer research to GERD. What’s your key subspecialty and why?
My primary specialty is advanced endoscopy, which includes techniques such as EUS, ERCP, and endoscopic resection of precancerous and early cancerous lesions. I also focus on cutting-edge, evidence-based techniques recently included in clinical guidelines, such as Transoral Incisionless Fundoplication (TIF). These minimally invasive options allow me to diagnose and treat conditions that once required surgery. The precision and innovation involved in advanced endoscopy enable me to effectively manage complex cases—from diagnosing early cancers to managing bile duct obstructions and resecting precancerous lesions.
Can you describe your work in cancer genetics and screening?
I am deeply committed to the early detection of gastrointestinal cancers, particularly through screening for precancerous conditions and hereditary syndromes. During my general GI training at the University of Michigan, I had the privilege of working with Grace Elta, MD, AGAF, and Michelle Anderson, MD, MSc, renowned experts in pancreatic cancer management. I was later trained by Anne Marie Lennon, PhD, AGAF, who pioneered the liquid biopsy technique for cancer screening through the CancerSEEK project, and Marcia (Mimi) Canto, MD, MHS, who initiated the Cancer of the Pancreas Screening project for high-risk individuals of pancreatic cancer.
I also had the distinction of being the first at Bumrungrad International Hospital to perform endoscopic drainage for pancreatic fluid collections in the setting of multi-organ failure. This endoscopic approach has been extensively validated in the medical literature as significantly improving survival rates compared to surgical drainage. My training in this specialized procedure was conducted under the guidance of the premier group for necrotizing pancreatitis, led by Martin Freeman, MD, at the University of Minnesota.
Later, I contributed to overseeing the Inherited Gastrointestinal Malignancy Clinic of MyCode, a large-scale population-based cohort program focused on cancer screening in Pennsylvania. By December 2024, MyCode had collected blood samples from over 258,000 individuals, analyzed DNA sequences from over 184,000, and provided clinical data that benefits over 142,000 patients. It’s not uncommon for healthy 25-year-old patients to come to our clinic for colon cancer screening after learning from the program that they carry a cancer syndrome, and early screening can potentially save their lives.
What are the key differences between training and practicing medicine in the United States and in an Asian country?
The U.S. healthcare system is deeply rooted in evidence-based protocols and multidisciplinary care, driven by an insurance-based model. In contrast, many Asian countries face challenges such as the dependency on government approval for certain treatments and insurance limitations. Practicing in Asia requires navigating unique cultural, economic, and systemic differences, including varying resource availability and disease prevalence.
What specific challenges have you faced as a GI in Thailand?
As an advanced endoscopist, one of the biggest challenges I faced initially was the difficulty in obtaining the same devices I used in the U.S. for use in Thailand. With support from device companies and mentors in the U.S., I was able to perform groundbreaking procedures, such as the TIF in Southeast Asia and the first use of a full-thickness resection device in Thailand. I am also proud to be part of one of the first few centers worldwide performing the combination of injectable semaglutide and endoscopic sleeve gastroplasty, resulting in a remarkable weight reduction of 44%, comparable to surgical gastric bypass.
In addition, Bumrungrad International Hospital, where I practice, sees over 1.1 million visits annually from patients from more than 190 countries. This offers a unique opportunity to engage with a global patient base and learn from diverse cultures. Over time, although the hospital has professional interpreters for all languages, I have become able to communicate basic sentences with international patients in their preferred languages, including Chinese, Japanese, and Arabic, which has enriched my practice.
What’s your favorite thing to do when you’re not practicing GI?
I enjoy traveling, exploring new cuisines, and spending quality time with family and friends. These activities help me recharge and offer fresh perspectives on life.
Lightning Round
Texting or talking?
Talking. It’s more personal and meaningful.
Favorite city in the U.S.?
Ann Arbor, Michigan
Cat or dog person?
Dog person
Favorite junk food?
Pizza
How many cups of coffee do you drink per day?
Two – just enough to stay sharp, but not jittery.
If you weren’t a GI, what would you be?
Architect
Best place you went on vacation?
Kyoto, Japan
Favorite sport?
Skiing
Favorite ice cream?
Matcha green tea
What song do you have to sing along with when you hear it?
“Everybody” by Backstreet Boys
Favorite movie or TV show?
Forrest Gump and Friends
Optimist or pessimist?
Optimist. I believe in focusing on solutions and possibilities.
As the COVID-19 crisis unfolded in early 2020, Tossapol Kerdsirichairat, MD, faced another challenge: his mother’s ovarian cancer diagnosis.
“She chose to remain in Thailand, so I decided to relocate to care for her,” said Dr. Kerdsirichairat, an interventional endoscopist who completed fellowships at the University of Michigan, Ann Arbor, and Johns Hopkins University in Baltimore. The move to Bangkok turned out to be one of the best decisions of his life, he said, as he could support his mother while introducing advanced endoscopic techniques and devices to the region.
“Bangkok is a hub for medical innovation in Asia, offering opportunities to work with a diverse patient population and access to cutting-edge technology,” said Dr. Kerdsirichairat, who works at Bumrungrad International Hospital as a clinical associate professor.
The program is the first of its kind in Thailand and one of the few in the Asia-Pacific region.
“I guide patients and families through understanding their risks and implementing preventive strategies, collaborating with multidisciplinary teams to ensure comprehensive care. It’s incredibly rewarding to see the impact of early tumor detection,” said Dr. Kerdsirichairat, an international member of AGA who was a participant in the AGA Young Delegates Program.
He has set several records in Thailand for the smallest tumor detected, including a 0.3-millimeter (mm) esophageal tumor, a 0.8-mm tumor for stomach cancer, a 5-mm pancreatic tumor, and a 1-mm tumor for colon cancer.
“These were detected through high-standard screening programs, as patients often do not develop symptoms from these subtle lesions,” said Dr. Kerdsirichairat, who discussed in an interview the unique challenges of practicing overseas.
Why did you choose GI?
Gastroenterology is a specialty that uniquely integrates procedural skill, clinical decision making, and a deep understanding of complex biological systems. I was drawn especially to the ability to make a direct and meaningful impact in patients’ lives through advanced endoscopic procedures, while also addressing both acute and chronic diseases, and focusing on cancer prevention. It is incredibly rewarding to perform an endoscopic retrograde cholangiopancreatography (ERCP) for cholangitis and see a patient return to normal the very next day, or to perform an endoscopic ultrasound (EUS) for pancreatic cancer screening in high-risk individuals and detect a sub-centimeter pancreatic tumor.
Realizing that early detection can improve survival by threefold after surgery is a powerful reminder of the difference we can make in patients’ lives. This specialty requires a delicate balance of precision and empathy, which perfectly aligns with my strengths and values as a physician.
You have a wide variety of clinical interests, from endoscopic procedures to cancer research to GERD. What’s your key subspecialty and why?
My primary specialty is advanced endoscopy, which includes techniques such as EUS, ERCP, and endoscopic resection of precancerous and early cancerous lesions. I also focus on cutting-edge, evidence-based techniques recently included in clinical guidelines, such as Transoral Incisionless Fundoplication (TIF). These minimally invasive options allow me to diagnose and treat conditions that once required surgery. The precision and innovation involved in advanced endoscopy enable me to effectively manage complex cases—from diagnosing early cancers to managing bile duct obstructions and resecting precancerous lesions.
Can you describe your work in cancer genetics and screening?
I am deeply committed to the early detection of gastrointestinal cancers, particularly through screening for precancerous conditions and hereditary syndromes. During my general GI training at the University of Michigan, I had the privilege of working with Grace Elta, MD, AGAF, and Michelle Anderson, MD, MSc, renowned experts in pancreatic cancer management. I was later trained by Anne Marie Lennon, PhD, AGAF, who pioneered the liquid biopsy technique for cancer screening through the CancerSEEK project, and Marcia (Mimi) Canto, MD, MHS, who initiated the Cancer of the Pancreas Screening project for high-risk individuals of pancreatic cancer.
I also had the distinction of being the first at Bumrungrad International Hospital to perform endoscopic drainage for pancreatic fluid collections in the setting of multi-organ failure. This endoscopic approach has been extensively validated in the medical literature as significantly improving survival rates compared to surgical drainage. My training in this specialized procedure was conducted under the guidance of the premier group for necrotizing pancreatitis, led by Martin Freeman, MD, at the University of Minnesota.
Later, I contributed to overseeing the Inherited Gastrointestinal Malignancy Clinic of MyCode, a large-scale population-based cohort program focused on cancer screening in Pennsylvania. By December 2024, MyCode had collected blood samples from over 258,000 individuals, analyzed DNA sequences from over 184,000, and provided clinical data that benefits over 142,000 patients. It’s not uncommon for healthy 25-year-old patients to come to our clinic for colon cancer screening after learning from the program that they carry a cancer syndrome, and early screening can potentially save their lives.
What are the key differences between training and practicing medicine in the United States and in an Asian country?
The U.S. healthcare system is deeply rooted in evidence-based protocols and multidisciplinary care, driven by an insurance-based model. In contrast, many Asian countries face challenges such as the dependency on government approval for certain treatments and insurance limitations. Practicing in Asia requires navigating unique cultural, economic, and systemic differences, including varying resource availability and disease prevalence.
What specific challenges have you faced as a GI in Thailand?
As an advanced endoscopist, one of the biggest challenges I faced initially was the difficulty in obtaining the same devices I used in the U.S. for use in Thailand. With support from device companies and mentors in the U.S., I was able to perform groundbreaking procedures, such as the TIF in Southeast Asia and the first use of a full-thickness resection device in Thailand. I am also proud to be part of one of the first few centers worldwide performing the combination of injectable semaglutide and endoscopic sleeve gastroplasty, resulting in a remarkable weight reduction of 44%, comparable to surgical gastric bypass.
In addition, Bumrungrad International Hospital, where I practice, sees over 1.1 million visits annually from patients from more than 190 countries. This offers a unique opportunity to engage with a global patient base and learn from diverse cultures. Over time, although the hospital has professional interpreters for all languages, I have become able to communicate basic sentences with international patients in their preferred languages, including Chinese, Japanese, and Arabic, which has enriched my practice.
What’s your favorite thing to do when you’re not practicing GI?
I enjoy traveling, exploring new cuisines, and spending quality time with family and friends. These activities help me recharge and offer fresh perspectives on life.
Lightning Round
Texting or talking?
Talking. It’s more personal and meaningful.
Favorite city in the U.S.?
Ann Arbor, Michigan
Cat or dog person?
Dog person
Favorite junk food?
Pizza
How many cups of coffee do you drink per day?
Two – just enough to stay sharp, but not jittery.
If you weren’t a GI, what would you be?
Architect
Best place you went on vacation?
Kyoto, Japan
Favorite sport?
Skiing
Favorite ice cream?
Matcha green tea
What song do you have to sing along with when you hear it?
“Everybody” by Backstreet Boys
Favorite movie or TV show?
Forrest Gump and Friends
Optimist or pessimist?
Optimist. I believe in focusing on solutions and possibilities.

Service Connection Expanded to Additional Cancers
The US Department of Veterans Affairs (VA) is "lowering the burden of proof" for thousands, making acute and chronic leukemias, multiple myelomas, myelodysplastic syndromes, myelofibrosis, urinary bladder, ureter, and related genitourinary cancers presumptive for service connection.
The Jan. 8 decision included Gulf War veterans, those who served in Somalia or the Southwest Asia theater of operations during the Persian Gulf War on or after Aug. 2, 1990; and post-9/11 veterans, those who served in Afghanistan, Iraq, Djibouti, Egypt, Jordan, Lebanon, Syria, Yemen, or Uzbekistan and the airspace above these locations during the Gulf War on or after Sept. 11, 2001. It also includes veterans who served at the Karshi-Khanabad (K2) base in Uzbekistan after Sept. 11, 2001.
Veterans no longer must prove their service caused their condition to receive benefits. This landmark decision allows them access to free health care for that condition.
According to the VA, these steps are also part of a comprehensive effort to ensure that K2 veterans—and their survivors—receive the care and benefits they deserve. K2 veterans have higher claim and approval rates than any other cohort of veterans: 13,002 are enrolled in VA health care, and the average K2 veteran is service connected for 14.6 conditions.
The 2022 PACT Act was the largest expansion of veteran benefits in generations. The VA then made millions of veterans eligible for health care and benefits years earlier than called for by the law. It also launched the largest outreach campaign in the history of the VA to encourage veterans to apply.
Nearly 890,000 veterans have signed up for VA health care since the bill was signed into law, a nearly 40% increase over the previous equivalent period, and veterans have submitted > 4.8 million applications for VA benefits (a 42% increase over the previous equivalent period and an all-time record). The VA has delivered > $600 billion in earned benefits directly to veterans, their families, and survivors during that time.
The VA encourages all eligible veterans—including those with previously denied claims—to apply for benefits. To apply for benefits, veterans and survivors may visit VA.gov or call 1-800-MYVA411.
The US Department of Veterans Affairs (VA) is "lowering the burden of proof" for thousands, making acute and chronic leukemias, multiple myelomas, myelodysplastic syndromes, myelofibrosis, urinary bladder, ureter, and related genitourinary cancers presumptive for service connection.
The Jan. 8 decision included Gulf War veterans, those who served in Somalia or the Southwest Asia theater of operations during the Persian Gulf War on or after Aug. 2, 1990; and post-9/11 veterans, those who served in Afghanistan, Iraq, Djibouti, Egypt, Jordan, Lebanon, Syria, Yemen, or Uzbekistan and the airspace above these locations during the Gulf War on or after Sept. 11, 2001. It also includes veterans who served at the Karshi-Khanabad (K2) base in Uzbekistan after Sept. 11, 2001.
Veterans no longer must prove their service caused their condition to receive benefits. This landmark decision allows them access to free health care for that condition.
According to the VA, these steps are also part of a comprehensive effort to ensure that K2 veterans—and their survivors—receive the care and benefits they deserve. K2 veterans have higher claim and approval rates than any other cohort of veterans: 13,002 are enrolled in VA health care, and the average K2 veteran is service connected for 14.6 conditions.
The 2022 PACT Act was the largest expansion of veteran benefits in generations. The VA then made millions of veterans eligible for health care and benefits years earlier than called for by the law. It also launched the largest outreach campaign in the history of the VA to encourage veterans to apply.
Nearly 890,000 veterans have signed up for VA health care since the bill was signed into law, a nearly 40% increase over the previous equivalent period, and veterans have submitted > 4.8 million applications for VA benefits (a 42% increase over the previous equivalent period and an all-time record). The VA has delivered > $600 billion in earned benefits directly to veterans, their families, and survivors during that time.
The VA encourages all eligible veterans—including those with previously denied claims—to apply for benefits. To apply for benefits, veterans and survivors may visit VA.gov or call 1-800-MYVA411.
The US Department of Veterans Affairs (VA) is "lowering the burden of proof" for thousands, making acute and chronic leukemias, multiple myelomas, myelodysplastic syndromes, myelofibrosis, urinary bladder, ureter, and related genitourinary cancers presumptive for service connection.
The Jan. 8 decision included Gulf War veterans, those who served in Somalia or the Southwest Asia theater of operations during the Persian Gulf War on or after Aug. 2, 1990; and post-9/11 veterans, those who served in Afghanistan, Iraq, Djibouti, Egypt, Jordan, Lebanon, Syria, Yemen, or Uzbekistan and the airspace above these locations during the Gulf War on or after Sept. 11, 2001. It also includes veterans who served at the Karshi-Khanabad (K2) base in Uzbekistan after Sept. 11, 2001.
Veterans no longer must prove their service caused their condition to receive benefits. This landmark decision allows them access to free health care for that condition.
According to the VA, these steps are also part of a comprehensive effort to ensure that K2 veterans—and their survivors—receive the care and benefits they deserve. K2 veterans have higher claim and approval rates than any other cohort of veterans: 13,002 are enrolled in VA health care, and the average K2 veteran is service connected for 14.6 conditions.
The 2022 PACT Act was the largest expansion of veteran benefits in generations. The VA then made millions of veterans eligible for health care and benefits years earlier than called for by the law. It also launched the largest outreach campaign in the history of the VA to encourage veterans to apply.
Nearly 890,000 veterans have signed up for VA health care since the bill was signed into law, a nearly 40% increase over the previous equivalent period, and veterans have submitted > 4.8 million applications for VA benefits (a 42% increase over the previous equivalent period and an all-time record). The VA has delivered > $600 billion in earned benefits directly to veterans, their families, and survivors during that time.
The VA encourages all eligible veterans—including those with previously denied claims—to apply for benefits. To apply for benefits, veterans and survivors may visit VA.gov or call 1-800-MYVA411.
Three Sisters Embrace ‘Collaborative Spirit’ of GI Science
They all share the same genes—and job title.
Each has her own lab, working in different specialties. But if one sister needs the others, it’s reassuring to know they’re not far away.
“We have very different points of view. I’m interested in microbes. Amy’s really interested in myosin mediated trafficking and Kristen’s interested in viruses and purinergic signaling. It’s awesome that we can all work in the same field but have very different questions. And there’s so many questions that we can tackle,” said Mindy Engevik, the oldest of the trio.
If Mindy’s students need help with staining, she sends them to Amy’s lab. If they need help with calcium signaling and live cell imaging, she’ll send them to Kristen’s lab. “We interchange our expertise a lot,” said Mindy.
It’s nice to have a sister down the hall at work who can advise you on RNA sequencing analysis or immunofluorescence imaging, noted Amy Engevik. “You can ask them: ‘Can you just walk my student through this for a minute?’ Or, could they help with organoid cultures you don’t have time for right now?”
Kristen, who joined her older sisters at MUSC in 2024, observed that “having a little bit of the variety with our backgrounds and training really helps bring out the collaborative spirit of science.”
In an interview, the Engevik sisters spoke more about their familial network, their shared love of gastroenterology (GI) science, and how they’ve parlayed their expertise into other critical areas of research.
Growing up, did you ever think that you would choose similar career paths? How did you all become interested in GI research?
Mindy Engevik: As kids we were all interested in nature and the world around us. We all liked being outside. Amy and I were obsessed with rocks and classifying plants and rocks. We all had a general interest in science. But I personally didn’t think that all three of us would go into the same thing and that we’d be working together as adults.
Amy Engevik: Once we got into high school and college, we all became very close and we all majored in biology. That set the stage for our interest in science and our love of science. Then, we all kind of fell in love with the GI tract and chose postdocs that were GI focused. Since Mindy and I graduated a year apart, ultimately our goal was to form a lab and work together.
Kristen Engevik: I was interested in science when my sisters were both at college studying for biology and talking about the things they were learning in microbiology and physiology. But I don’t think until I joined the PhD program that I was ever like: ‘Oh yeah, we’re all going to be in science and it’s all going to be one big giant collaborative multi-lab collaboration.’
What do each of you love about the field of gastroenterology?
Mindy Engevik: At our heart, we’re all people that love problem solving. A fun fact about us is on Thursdays once a month, we do a puzzle competition here in Charleston. We’re really into it. But I think we genuinely like the problem-solving nature of the GI tract, and there’s so many diverse questions that you can answer.
Amy Engevik: I love that the scientific community in the GI community is so wonderful. They are very kind, helpful people. Some other fields are more competitive and more cutthroat. I feel like I have such a great network of people to reach out to if I have problems or questions. And I think other fields don’t have such a wonderful welcoming community that is very inclusive and dynamic.
Kristen Engevik: The nice thing with studying the GI tract is all things essentially lead to the gut. You can collaborate with other scientists and go into the gut-brain axis, or there’s the cardiovascular-gut axis and all these different places that you can also go, or different diseases that don’t necessarily seem to originate at the gut but have a lot of effects on the gut. There’s a lot of variation that we can do within GI.
Each of you has focused on a different area of digestive disease. Can each of you briefly discuss your areas of study and any findings or discoveries you’d like to highlight?
Mindy Engevik: My research focuses on microbial-host interactions. We’re really interested in how microbes colonize the gastrointestinal tract, how they interact with mucus – which I think is an important aspect of the gut that sometimes is overlooked – and how their metabolites really impact host health. One thing that I’m particularly proud of is we’ve really been starting to understand the neurotransmitters that bacteria generate and how they influence specific cells within the gut. It’s an exciting time to be doing both microbiology and gut physiology.
Amy Engevik: I study the host side of things; the gastric or the GI epithelium, and how a specific molecular motor contributes to trafficking in the GI tract. Recently, I’ve been going back to some of my PhD work in the stomach. In a high fat diet model, we’re finding that there are early metaplastic changes in the stomach. I think the stomach is very often overlooked within the GI tract. And I think it really sets the stage for the lower GI tract for the microbiome that colonizes the colon and the small intestine. I think that changes in the stomach really should come to the forefront of GI. Those changes have profound impacts on things like colorectal cancer and inflammatory bowel disease.
Kristen Engevik: I’m also more on the epithelial side with Amy. My new lab’s work is going to be focusing on understanding cell communications, specifically through extracellular purines, which is known as purinergic signaling, and understanding what the effects are during both homeostasis and disease, since it hasn’t been studied within the gut itself. From my work in postdoctoral training, we found that this communication is important for a lot of aspects, specifically during viral infection. But I have some preliminary data that shows it may also have an important role during disease, like colitis. My lab is interested in understanding what this epithelial communication is and are there ways to increase or decrease the signaling depending on the disease.
You’re all skilled in analyzing bioinformatics data. How do you apply this skill in your GI research?
Mindy Engevik: We all got our PhDs in systems biology and physiology, so we were forced to take computational analysis classes. I remember at the time thinking, ‘Oh, I’m probably not going to use a bunch of this.’ And then it really captured our attention. We realized how valuable it was and how much information you could glean.
We do a lot of work using publicly available data sets. I think there’s a wealth of information out there now with single cell sequencing data and bulk RNA sequencing data of different sites in the GI tract. It’s been a very valuable time to data mine and look especially at inflammatory bowel disease and colorectal cancer. We’ve been really focused on all our favorite genes of interest. I’ve been looking at a lot of the mucins and IBD (inflammatory bowel disease) and cancer. Amy’s been looking at Myosin-Vb and other myosin and binding partners like Rabs, and Kristen has been looking at purinergic signaling receptors.
All three of you recently worked together to identify a possible genetic driver of uterine corpus endometrial cancer, the fourth deadliest cancer in women. Where are you in the research process right now?
Mindy Engevik: Our mom was diagnosed with cancer, so we took quite a bit of time off to go to California to help her with her chemotherapy, surgery, and radiation. While we were there, we decided to do some computational analyses of cancers that affect women as our way to deal with this devastating disease. We were really fascinated to find that Myosin-Vb, which is Amy’s favorite gene of interest, was highly up-regulated in tumors from uterine and corpus endometrial cancer.
This was independent of the age of the patient, the stage of the cancer, the grade of the tumors. We figured out that the promoter region of the gene was hypomethylated, so it was having a higher expression. And that led to changes in metabolism and it linked very closely with what we were seeing in the gut, what Myosin-Vb was doing. We have some uterine cancer tumor cells in the lab that we’ve been growing and we’re going to really prove that it’s Myosin-Vb that’s driving some of these metabolism phenotypes. And the nice thing is at least there is a Myosin-Vb inhibitor available.
We also have a paper under review, identifying what Myosin-Vb is doing in cancer in the colon. So we’re excited to continue both the uterine cancer part but then also the colorectal cancer part using our same processes.
Amy Engevik: We’re going to be generating a mouse model that I think will be helpful since it’s in vivo. Sometimes things in vivo behave very differently than they do in vitro, so I think it’ll be a nice coupling of in vitro data with in vivo, taking that computational base and expanding it into more mechanistic studies and more experimental approaches where we can actually develop uterine cancer in the mice and then see if we can knock out Myosin-Vb specifically in that tissue and prevent it from either happening in the first place or decrease its pathogenesis.
What challenges have you faced in your career? How do you offer each other support?
Mindy Engevik: I think for any female scientists trying to have an independent career, there are some hurdles. An article in Nature recently stated that women receive less credit than their male counterparts and another article in Science demonstrated that women who are last authors on publications are cited less. That’s something that all women must deal with everywhere. I think it’s been incredibly helpful for us since there’s three of us. I think it gives us extra visibility in the field.
Amy Engevik: There’s a lot of microaggressions and things that can hinder your career success. I think that we’ve definitely had that. And I think the academic landscape is changing a little bit now that more women are becoming principal investigators and then rising through the ranks of academia. So I think there’s a lot of hope for the future women, but I think it’s still quite challenging.
Kristen Engevik: Things do seem to be getting better as there are more women as faculty members in certain departments. Science is getting better as things progress. However, there are still a lot of difficulties in trying to get credit for what you do, and getting the promotions.
Mindy Engevik: We have a built-in sisterhood, if you will. So I’m always going to champion Amy or Kristen. If there’s an award that I can nominate them for, I’m always going to do it. If there’s something that I think they should apply for that maybe they hadn’t seen, I’m going to make sure I put it on the radar. I think that’s just incredibly helpful, having people that have your best interest in mind.
Every project we have is basically a big collaboration. We have a lot of papers from our postdocs where we are coauthors. Now, as principal investigators, we have a lot of papers together. And I think in the future you’ll be seeing a lot of coauthored publications from our group as well.
Lightning Round
Texting or talking?
KE: Talking
Favorite city in US besides the one you live in?
AE: Boston
Favorite breakfast?
ME: Biscuits and grits
Place you most want to travel?
KE: Antarctica
Favorite junk food?
AE: French fries
Favorite season?
ME: Fall
Favorite ice cream flavor?
KE: Black raspberry chip
Number of cups of coffee you drink per day?
AE: None, I like Diet Coke
Last movie you watched?
ME: Inside Out 2
If you weren’t a gastroenterologist, what would you be?
KE: National Park ranger
Best Halloween costume you ever wore?
AE: Princess Leia
Favorite type of music?
ME: ABBA
Favorite movie genre?
KE: Romantic comedies
Cat person or dog person?
AE: Neither, I like rabbits
Favorite sport?
ME: Surfing
What song do you have to sing along with when you hear it?
KE: Mama Mia
Introvert or extrovert?
AE: Introvert
Favorite holiday?
ME: Halloween
They all share the same genes—and job title.
Each has her own lab, working in different specialties. But if one sister needs the others, it’s reassuring to know they’re not far away.
“We have very different points of view. I’m interested in microbes. Amy’s really interested in myosin mediated trafficking and Kristen’s interested in viruses and purinergic signaling. It’s awesome that we can all work in the same field but have very different questions. And there’s so many questions that we can tackle,” said Mindy Engevik, the oldest of the trio.
If Mindy’s students need help with staining, she sends them to Amy’s lab. If they need help with calcium signaling and live cell imaging, she’ll send them to Kristen’s lab. “We interchange our expertise a lot,” said Mindy.
It’s nice to have a sister down the hall at work who can advise you on RNA sequencing analysis or immunofluorescence imaging, noted Amy Engevik. “You can ask them: ‘Can you just walk my student through this for a minute?’ Or, could they help with organoid cultures you don’t have time for right now?”
Kristen, who joined her older sisters at MUSC in 2024, observed that “having a little bit of the variety with our backgrounds and training really helps bring out the collaborative spirit of science.”
In an interview, the Engevik sisters spoke more about their familial network, their shared love of gastroenterology (GI) science, and how they’ve parlayed their expertise into other critical areas of research.
Growing up, did you ever think that you would choose similar career paths? How did you all become interested in GI research?
Mindy Engevik: As kids we were all interested in nature and the world around us. We all liked being outside. Amy and I were obsessed with rocks and classifying plants and rocks. We all had a general interest in science. But I personally didn’t think that all three of us would go into the same thing and that we’d be working together as adults.
Amy Engevik: Once we got into high school and college, we all became very close and we all majored in biology. That set the stage for our interest in science and our love of science. Then, we all kind of fell in love with the GI tract and chose postdocs that were GI focused. Since Mindy and I graduated a year apart, ultimately our goal was to form a lab and work together.
Kristen Engevik: I was interested in science when my sisters were both at college studying for biology and talking about the things they were learning in microbiology and physiology. But I don’t think until I joined the PhD program that I was ever like: ‘Oh yeah, we’re all going to be in science and it’s all going to be one big giant collaborative multi-lab collaboration.’
What do each of you love about the field of gastroenterology?
Mindy Engevik: At our heart, we’re all people that love problem solving. A fun fact about us is on Thursdays once a month, we do a puzzle competition here in Charleston. We’re really into it. But I think we genuinely like the problem-solving nature of the GI tract, and there’s so many diverse questions that you can answer.
Amy Engevik: I love that the scientific community in the GI community is so wonderful. They are very kind, helpful people. Some other fields are more competitive and more cutthroat. I feel like I have such a great network of people to reach out to if I have problems or questions. And I think other fields don’t have such a wonderful welcoming community that is very inclusive and dynamic.
Kristen Engevik: The nice thing with studying the GI tract is all things essentially lead to the gut. You can collaborate with other scientists and go into the gut-brain axis, or there’s the cardiovascular-gut axis and all these different places that you can also go, or different diseases that don’t necessarily seem to originate at the gut but have a lot of effects on the gut. There’s a lot of variation that we can do within GI.
Each of you has focused on a different area of digestive disease. Can each of you briefly discuss your areas of study and any findings or discoveries you’d like to highlight?
Mindy Engevik: My research focuses on microbial-host interactions. We’re really interested in how microbes colonize the gastrointestinal tract, how they interact with mucus – which I think is an important aspect of the gut that sometimes is overlooked – and how their metabolites really impact host health. One thing that I’m particularly proud of is we’ve really been starting to understand the neurotransmitters that bacteria generate and how they influence specific cells within the gut. It’s an exciting time to be doing both microbiology and gut physiology.
Amy Engevik: I study the host side of things; the gastric or the GI epithelium, and how a specific molecular motor contributes to trafficking in the GI tract. Recently, I’ve been going back to some of my PhD work in the stomach. In a high fat diet model, we’re finding that there are early metaplastic changes in the stomach. I think the stomach is very often overlooked within the GI tract. And I think it really sets the stage for the lower GI tract for the microbiome that colonizes the colon and the small intestine. I think that changes in the stomach really should come to the forefront of GI. Those changes have profound impacts on things like colorectal cancer and inflammatory bowel disease.
Kristen Engevik: I’m also more on the epithelial side with Amy. My new lab’s work is going to be focusing on understanding cell communications, specifically through extracellular purines, which is known as purinergic signaling, and understanding what the effects are during both homeostasis and disease, since it hasn’t been studied within the gut itself. From my work in postdoctoral training, we found that this communication is important for a lot of aspects, specifically during viral infection. But I have some preliminary data that shows it may also have an important role during disease, like colitis. My lab is interested in understanding what this epithelial communication is and are there ways to increase or decrease the signaling depending on the disease.
You’re all skilled in analyzing bioinformatics data. How do you apply this skill in your GI research?
Mindy Engevik: We all got our PhDs in systems biology and physiology, so we were forced to take computational analysis classes. I remember at the time thinking, ‘Oh, I’m probably not going to use a bunch of this.’ And then it really captured our attention. We realized how valuable it was and how much information you could glean.
We do a lot of work using publicly available data sets. I think there’s a wealth of information out there now with single cell sequencing data and bulk RNA sequencing data of different sites in the GI tract. It’s been a very valuable time to data mine and look especially at inflammatory bowel disease and colorectal cancer. We’ve been really focused on all our favorite genes of interest. I’ve been looking at a lot of the mucins and IBD (inflammatory bowel disease) and cancer. Amy’s been looking at Myosin-Vb and other myosin and binding partners like Rabs, and Kristen has been looking at purinergic signaling receptors.
All three of you recently worked together to identify a possible genetic driver of uterine corpus endometrial cancer, the fourth deadliest cancer in women. Where are you in the research process right now?
Mindy Engevik: Our mom was diagnosed with cancer, so we took quite a bit of time off to go to California to help her with her chemotherapy, surgery, and radiation. While we were there, we decided to do some computational analyses of cancers that affect women as our way to deal with this devastating disease. We were really fascinated to find that Myosin-Vb, which is Amy’s favorite gene of interest, was highly up-regulated in tumors from uterine and corpus endometrial cancer.
This was independent of the age of the patient, the stage of the cancer, the grade of the tumors. We figured out that the promoter region of the gene was hypomethylated, so it was having a higher expression. And that led to changes in metabolism and it linked very closely with what we were seeing in the gut, what Myosin-Vb was doing. We have some uterine cancer tumor cells in the lab that we’ve been growing and we’re going to really prove that it’s Myosin-Vb that’s driving some of these metabolism phenotypes. And the nice thing is at least there is a Myosin-Vb inhibitor available.
We also have a paper under review, identifying what Myosin-Vb is doing in cancer in the colon. So we’re excited to continue both the uterine cancer part but then also the colorectal cancer part using our same processes.
Amy Engevik: We’re going to be generating a mouse model that I think will be helpful since it’s in vivo. Sometimes things in vivo behave very differently than they do in vitro, so I think it’ll be a nice coupling of in vitro data with in vivo, taking that computational base and expanding it into more mechanistic studies and more experimental approaches where we can actually develop uterine cancer in the mice and then see if we can knock out Myosin-Vb specifically in that tissue and prevent it from either happening in the first place or decrease its pathogenesis.
What challenges have you faced in your career? How do you offer each other support?
Mindy Engevik: I think for any female scientists trying to have an independent career, there are some hurdles. An article in Nature recently stated that women receive less credit than their male counterparts and another article in Science demonstrated that women who are last authors on publications are cited less. That’s something that all women must deal with everywhere. I think it’s been incredibly helpful for us since there’s three of us. I think it gives us extra visibility in the field.
Amy Engevik: There’s a lot of microaggressions and things that can hinder your career success. I think that we’ve definitely had that. And I think the academic landscape is changing a little bit now that more women are becoming principal investigators and then rising through the ranks of academia. So I think there’s a lot of hope for the future women, but I think it’s still quite challenging.
Kristen Engevik: Things do seem to be getting better as there are more women as faculty members in certain departments. Science is getting better as things progress. However, there are still a lot of difficulties in trying to get credit for what you do, and getting the promotions.
Mindy Engevik: We have a built-in sisterhood, if you will. So I’m always going to champion Amy or Kristen. If there’s an award that I can nominate them for, I’m always going to do it. If there’s something that I think they should apply for that maybe they hadn’t seen, I’m going to make sure I put it on the radar. I think that’s just incredibly helpful, having people that have your best interest in mind.
Every project we have is basically a big collaboration. We have a lot of papers from our postdocs where we are coauthors. Now, as principal investigators, we have a lot of papers together. And I think in the future you’ll be seeing a lot of coauthored publications from our group as well.
Lightning Round
Texting or talking?
KE: Talking
Favorite city in US besides the one you live in?
AE: Boston
Favorite breakfast?
ME: Biscuits and grits
Place you most want to travel?
KE: Antarctica
Favorite junk food?
AE: French fries
Favorite season?
ME: Fall
Favorite ice cream flavor?
KE: Black raspberry chip
Number of cups of coffee you drink per day?
AE: None, I like Diet Coke
Last movie you watched?
ME: Inside Out 2
If you weren’t a gastroenterologist, what would you be?
KE: National Park ranger
Best Halloween costume you ever wore?
AE: Princess Leia
Favorite type of music?
ME: ABBA
Favorite movie genre?
KE: Romantic comedies
Cat person or dog person?
AE: Neither, I like rabbits
Favorite sport?
ME: Surfing
What song do you have to sing along with when you hear it?
KE: Mama Mia
Introvert or extrovert?
AE: Introvert
Favorite holiday?
ME: Halloween
They all share the same genes—and job title.
Each has her own lab, working in different specialties. But if one sister needs the others, it’s reassuring to know they’re not far away.
“We have very different points of view. I’m interested in microbes. Amy’s really interested in myosin mediated trafficking and Kristen’s interested in viruses and purinergic signaling. It’s awesome that we can all work in the same field but have very different questions. And there’s so many questions that we can tackle,” said Mindy Engevik, the oldest of the trio.
If Mindy’s students need help with staining, she sends them to Amy’s lab. If they need help with calcium signaling and live cell imaging, she’ll send them to Kristen’s lab. “We interchange our expertise a lot,” said Mindy.
It’s nice to have a sister down the hall at work who can advise you on RNA sequencing analysis or immunofluorescence imaging, noted Amy Engevik. “You can ask them: ‘Can you just walk my student through this for a minute?’ Or, could they help with organoid cultures you don’t have time for right now?”
Kristen, who joined her older sisters at MUSC in 2024, observed that “having a little bit of the variety with our backgrounds and training really helps bring out the collaborative spirit of science.”
In an interview, the Engevik sisters spoke more about their familial network, their shared love of gastroenterology (GI) science, and how they’ve parlayed their expertise into other critical areas of research.
Growing up, did you ever think that you would choose similar career paths? How did you all become interested in GI research?
Mindy Engevik: As kids we were all interested in nature and the world around us. We all liked being outside. Amy and I were obsessed with rocks and classifying plants and rocks. We all had a general interest in science. But I personally didn’t think that all three of us would go into the same thing and that we’d be working together as adults.
Amy Engevik: Once we got into high school and college, we all became very close and we all majored in biology. That set the stage for our interest in science and our love of science. Then, we all kind of fell in love with the GI tract and chose postdocs that were GI focused. Since Mindy and I graduated a year apart, ultimately our goal was to form a lab and work together.
Kristen Engevik: I was interested in science when my sisters were both at college studying for biology and talking about the things they were learning in microbiology and physiology. But I don’t think until I joined the PhD program that I was ever like: ‘Oh yeah, we’re all going to be in science and it’s all going to be one big giant collaborative multi-lab collaboration.’
What do each of you love about the field of gastroenterology?
Mindy Engevik: At our heart, we’re all people that love problem solving. A fun fact about us is on Thursdays once a month, we do a puzzle competition here in Charleston. We’re really into it. But I think we genuinely like the problem-solving nature of the GI tract, and there’s so many diverse questions that you can answer.
Amy Engevik: I love that the scientific community in the GI community is so wonderful. They are very kind, helpful people. Some other fields are more competitive and more cutthroat. I feel like I have such a great network of people to reach out to if I have problems or questions. And I think other fields don’t have such a wonderful welcoming community that is very inclusive and dynamic.
Kristen Engevik: The nice thing with studying the GI tract is all things essentially lead to the gut. You can collaborate with other scientists and go into the gut-brain axis, or there’s the cardiovascular-gut axis and all these different places that you can also go, or different diseases that don’t necessarily seem to originate at the gut but have a lot of effects on the gut. There’s a lot of variation that we can do within GI.
Each of you has focused on a different area of digestive disease. Can each of you briefly discuss your areas of study and any findings or discoveries you’d like to highlight?
Mindy Engevik: My research focuses on microbial-host interactions. We’re really interested in how microbes colonize the gastrointestinal tract, how they interact with mucus – which I think is an important aspect of the gut that sometimes is overlooked – and how their metabolites really impact host health. One thing that I’m particularly proud of is we’ve really been starting to understand the neurotransmitters that bacteria generate and how they influence specific cells within the gut. It’s an exciting time to be doing both microbiology and gut physiology.
Amy Engevik: I study the host side of things; the gastric or the GI epithelium, and how a specific molecular motor contributes to trafficking in the GI tract. Recently, I’ve been going back to some of my PhD work in the stomach. In a high fat diet model, we’re finding that there are early metaplastic changes in the stomach. I think the stomach is very often overlooked within the GI tract. And I think it really sets the stage for the lower GI tract for the microbiome that colonizes the colon and the small intestine. I think that changes in the stomach really should come to the forefront of GI. Those changes have profound impacts on things like colorectal cancer and inflammatory bowel disease.
Kristen Engevik: I’m also more on the epithelial side with Amy. My new lab’s work is going to be focusing on understanding cell communications, specifically through extracellular purines, which is known as purinergic signaling, and understanding what the effects are during both homeostasis and disease, since it hasn’t been studied within the gut itself. From my work in postdoctoral training, we found that this communication is important for a lot of aspects, specifically during viral infection. But I have some preliminary data that shows it may also have an important role during disease, like colitis. My lab is interested in understanding what this epithelial communication is and are there ways to increase or decrease the signaling depending on the disease.
You’re all skilled in analyzing bioinformatics data. How do you apply this skill in your GI research?
Mindy Engevik: We all got our PhDs in systems biology and physiology, so we were forced to take computational analysis classes. I remember at the time thinking, ‘Oh, I’m probably not going to use a bunch of this.’ And then it really captured our attention. We realized how valuable it was and how much information you could glean.
We do a lot of work using publicly available data sets. I think there’s a wealth of information out there now with single cell sequencing data and bulk RNA sequencing data of different sites in the GI tract. It’s been a very valuable time to data mine and look especially at inflammatory bowel disease and colorectal cancer. We’ve been really focused on all our favorite genes of interest. I’ve been looking at a lot of the mucins and IBD (inflammatory bowel disease) and cancer. Amy’s been looking at Myosin-Vb and other myosin and binding partners like Rabs, and Kristen has been looking at purinergic signaling receptors.
All three of you recently worked together to identify a possible genetic driver of uterine corpus endometrial cancer, the fourth deadliest cancer in women. Where are you in the research process right now?
Mindy Engevik: Our mom was diagnosed with cancer, so we took quite a bit of time off to go to California to help her with her chemotherapy, surgery, and radiation. While we were there, we decided to do some computational analyses of cancers that affect women as our way to deal with this devastating disease. We were really fascinated to find that Myosin-Vb, which is Amy’s favorite gene of interest, was highly up-regulated in tumors from uterine and corpus endometrial cancer.
This was independent of the age of the patient, the stage of the cancer, the grade of the tumors. We figured out that the promoter region of the gene was hypomethylated, so it was having a higher expression. And that led to changes in metabolism and it linked very closely with what we were seeing in the gut, what Myosin-Vb was doing. We have some uterine cancer tumor cells in the lab that we’ve been growing and we’re going to really prove that it’s Myosin-Vb that’s driving some of these metabolism phenotypes. And the nice thing is at least there is a Myosin-Vb inhibitor available.
We also have a paper under review, identifying what Myosin-Vb is doing in cancer in the colon. So we’re excited to continue both the uterine cancer part but then also the colorectal cancer part using our same processes.
Amy Engevik: We’re going to be generating a mouse model that I think will be helpful since it’s in vivo. Sometimes things in vivo behave very differently than they do in vitro, so I think it’ll be a nice coupling of in vitro data with in vivo, taking that computational base and expanding it into more mechanistic studies and more experimental approaches where we can actually develop uterine cancer in the mice and then see if we can knock out Myosin-Vb specifically in that tissue and prevent it from either happening in the first place or decrease its pathogenesis.
What challenges have you faced in your career? How do you offer each other support?
Mindy Engevik: I think for any female scientists trying to have an independent career, there are some hurdles. An article in Nature recently stated that women receive less credit than their male counterparts and another article in Science demonstrated that women who are last authors on publications are cited less. That’s something that all women must deal with everywhere. I think it’s been incredibly helpful for us since there’s three of us. I think it gives us extra visibility in the field.
Amy Engevik: There’s a lot of microaggressions and things that can hinder your career success. I think that we’ve definitely had that. And I think the academic landscape is changing a little bit now that more women are becoming principal investigators and then rising through the ranks of academia. So I think there’s a lot of hope for the future women, but I think it’s still quite challenging.
Kristen Engevik: Things do seem to be getting better as there are more women as faculty members in certain departments. Science is getting better as things progress. However, there are still a lot of difficulties in trying to get credit for what you do, and getting the promotions.
Mindy Engevik: We have a built-in sisterhood, if you will. So I’m always going to champion Amy or Kristen. If there’s an award that I can nominate them for, I’m always going to do it. If there’s something that I think they should apply for that maybe they hadn’t seen, I’m going to make sure I put it on the radar. I think that’s just incredibly helpful, having people that have your best interest in mind.
Every project we have is basically a big collaboration. We have a lot of papers from our postdocs where we are coauthors. Now, as principal investigators, we have a lot of papers together. And I think in the future you’ll be seeing a lot of coauthored publications from our group as well.
Lightning Round
Texting or talking?
KE: Talking
Favorite city in US besides the one you live in?
AE: Boston
Favorite breakfast?
ME: Biscuits and grits
Place you most want to travel?
KE: Antarctica
Favorite junk food?
AE: French fries
Favorite season?
ME: Fall
Favorite ice cream flavor?
KE: Black raspberry chip
Number of cups of coffee you drink per day?
AE: None, I like Diet Coke
Last movie you watched?
ME: Inside Out 2
If you weren’t a gastroenterologist, what would you be?
KE: National Park ranger
Best Halloween costume you ever wore?
AE: Princess Leia
Favorite type of music?
ME: ABBA
Favorite movie genre?
KE: Romantic comedies
Cat person or dog person?
AE: Neither, I like rabbits
Favorite sport?
ME: Surfing
What song do you have to sing along with when you hear it?
KE: Mama Mia
Introvert or extrovert?
AE: Introvert
Favorite holiday?
ME: Halloween

Contraceptive Care Clinic Focuses on Military Readiness
SAN DIEGO — Not surprisingly, the contraception clinic at Madigan Army Medical Center near Tacoma, Wash., is popular among female soldiers seeking to avoid pregnancy. However, about half of the patients drop by for other reasons, the military pharmacist who runs the program told colleagues here at the Joint Federal Pharmacy Seminar.
“They come to suppress menstruation, to get help with pain, to get help with PCOS [polycystic ovary syndrome] symptoms. They're coming for a wide range of indications that we use contraception to treat,” said Sarah Abel, PharmD, a clinical pharmacist.
Regardless of the reason, Abel emphasized that contraceptives can significantly impact the ability of female soldiers to do their jobs. “If you have heavy periods and can't make it in work, or you have endometriosis and requiring a lot of doctor's appointments, or you're deployed and you get pregnant, these are all situations where contraceptive care matters,” she said. Rates of unintended pregnancy are higher in servicewomen than in the general population.
Abel, who opened the medical center’s contraceptive clinic about 10 years ago, stressed that it’s crucial to military readiness considering that the percentage of women in the American military is approaching 20%.
Thanks to a 2022 edict, military hospitals and clinics are required to offer walk-in contraceptive services with same-day access, no requirements for appointments or referrals. An announcement about the mandate noted that these contraceptive services, such as preventing unplanned pregnancy and decreasing menstrual periods, “support the overall well-being of the force and optimize personal warrior readiness.”
As Abel noted, 29 states and Washington D.C. allow pharmacists to prescribe contraception to outpatients, although the requirements vary. “Can we start practicing at the top of our license and start prescribing in the outpatient setting? Absolutely we should,” she said. “Pharmacists have a very unique opportunity to be a part of this.”
Abel also shared that setting up a contraceptive program requires patience and education. “I cannot tell you how many women have come to me who don't know the different names of their body parts, women who've had two babies that don't understand how their body works. So, I constantly find myself taking extra time to do general sexual education,” she said.
There are many lessons to impart to patients about sexual health. For example, birth control drugs and devices do not prevent transmission of sexually transmitted infections (STIs). “So I have bowls of condoms literally everywhere because condoms are the only thing that protects against STIs,” Abel said.
In terms of devices, “we have diaphragms available and cervical caps,” she said. “The Caya diaphragm is a TRICARE-covered benefit. It’s a small purple diaphragm, one size fits most. We can prescribe it, and it is good for 2 years. Unfortunately, spermicide, which you have to use with these things, is not a TRICARE-covered benefit.”
Hormonal contraceptives are also available, with Abel recommending the continuous monophasic type for most women. “Please don't tell women they have to have their periods. They don't,” she said. “What I'm trying to do is give a woman some stability in her hormones. She can know and expect what she's going to feel like. She's not going to wake up and say, ‘Oh God, today's the day. I'm going to be like this for a week.’”
Patches are another option, and a flurry of patients have been asking about them because of recent TikTok videos promoting their use. “We have the Xulane patch, our bread and butter. They wear it on their shoulder, their hip, their butt, or their back. They leave it in place for a week at a time. And every week, they will change that patch. I usually have to walk patients through a whole month to help them understand how that works.”
Another option, the NuvaRing, is notable because it’s linked to low amounts of breakthrough bleeding Abel noted. An extended form is now available that doesn’t need to be removed during menstrual periods.
Medroxyprogesterone injections, which are linked to bone loss, and subdermal implants, which may be less effective in women over 130% of their ideal weight are also available, she said.
Finally, IUDs are an option, although when they fail, they’re linked to ectopic pregnancies.
Abel has no disclosures.
SAN DIEGO — Not surprisingly, the contraception clinic at Madigan Army Medical Center near Tacoma, Wash., is popular among female soldiers seeking to avoid pregnancy. However, about half of the patients drop by for other reasons, the military pharmacist who runs the program told colleagues here at the Joint Federal Pharmacy Seminar.
“They come to suppress menstruation, to get help with pain, to get help with PCOS [polycystic ovary syndrome] symptoms. They're coming for a wide range of indications that we use contraception to treat,” said Sarah Abel, PharmD, a clinical pharmacist.
Regardless of the reason, Abel emphasized that contraceptives can significantly impact the ability of female soldiers to do their jobs. “If you have heavy periods and can't make it in work, or you have endometriosis and requiring a lot of doctor's appointments, or you're deployed and you get pregnant, these are all situations where contraceptive care matters,” she said. Rates of unintended pregnancy are higher in servicewomen than in the general population.
Abel, who opened the medical center’s contraceptive clinic about 10 years ago, stressed that it’s crucial to military readiness considering that the percentage of women in the American military is approaching 20%.
Thanks to a 2022 edict, military hospitals and clinics are required to offer walk-in contraceptive services with same-day access, no requirements for appointments or referrals. An announcement about the mandate noted that these contraceptive services, such as preventing unplanned pregnancy and decreasing menstrual periods, “support the overall well-being of the force and optimize personal warrior readiness.”
As Abel noted, 29 states and Washington D.C. allow pharmacists to prescribe contraception to outpatients, although the requirements vary. “Can we start practicing at the top of our license and start prescribing in the outpatient setting? Absolutely we should,” she said. “Pharmacists have a very unique opportunity to be a part of this.”
Abel also shared that setting up a contraceptive program requires patience and education. “I cannot tell you how many women have come to me who don't know the different names of their body parts, women who've had two babies that don't understand how their body works. So, I constantly find myself taking extra time to do general sexual education,” she said.
There are many lessons to impart to patients about sexual health. For example, birth control drugs and devices do not prevent transmission of sexually transmitted infections (STIs). “So I have bowls of condoms literally everywhere because condoms are the only thing that protects against STIs,” Abel said.
In terms of devices, “we have diaphragms available and cervical caps,” she said. “The Caya diaphragm is a TRICARE-covered benefit. It’s a small purple diaphragm, one size fits most. We can prescribe it, and it is good for 2 years. Unfortunately, spermicide, which you have to use with these things, is not a TRICARE-covered benefit.”
Hormonal contraceptives are also available, with Abel recommending the continuous monophasic type for most women. “Please don't tell women they have to have their periods. They don't,” she said. “What I'm trying to do is give a woman some stability in her hormones. She can know and expect what she's going to feel like. She's not going to wake up and say, ‘Oh God, today's the day. I'm going to be like this for a week.’”
Patches are another option, and a flurry of patients have been asking about them because of recent TikTok videos promoting their use. “We have the Xulane patch, our bread and butter. They wear it on their shoulder, their hip, their butt, or their back. They leave it in place for a week at a time. And every week, they will change that patch. I usually have to walk patients through a whole month to help them understand how that works.”
Another option, the NuvaRing, is notable because it’s linked to low amounts of breakthrough bleeding Abel noted. An extended form is now available that doesn’t need to be removed during menstrual periods.
Medroxyprogesterone injections, which are linked to bone loss, and subdermal implants, which may be less effective in women over 130% of their ideal weight are also available, she said.
Finally, IUDs are an option, although when they fail, they’re linked to ectopic pregnancies.
Abel has no disclosures.
SAN DIEGO — Not surprisingly, the contraception clinic at Madigan Army Medical Center near Tacoma, Wash., is popular among female soldiers seeking to avoid pregnancy. However, about half of the patients drop by for other reasons, the military pharmacist who runs the program told colleagues here at the Joint Federal Pharmacy Seminar.
“They come to suppress menstruation, to get help with pain, to get help with PCOS [polycystic ovary syndrome] symptoms. They're coming for a wide range of indications that we use contraception to treat,” said Sarah Abel, PharmD, a clinical pharmacist.
Regardless of the reason, Abel emphasized that contraceptives can significantly impact the ability of female soldiers to do their jobs. “If you have heavy periods and can't make it in work, or you have endometriosis and requiring a lot of doctor's appointments, or you're deployed and you get pregnant, these are all situations where contraceptive care matters,” she said. Rates of unintended pregnancy are higher in servicewomen than in the general population.
Abel, who opened the medical center’s contraceptive clinic about 10 years ago, stressed that it’s crucial to military readiness considering that the percentage of women in the American military is approaching 20%.
Thanks to a 2022 edict, military hospitals and clinics are required to offer walk-in contraceptive services with same-day access, no requirements for appointments or referrals. An announcement about the mandate noted that these contraceptive services, such as preventing unplanned pregnancy and decreasing menstrual periods, “support the overall well-being of the force and optimize personal warrior readiness.”
As Abel noted, 29 states and Washington D.C. allow pharmacists to prescribe contraception to outpatients, although the requirements vary. “Can we start practicing at the top of our license and start prescribing in the outpatient setting? Absolutely we should,” she said. “Pharmacists have a very unique opportunity to be a part of this.”
Abel also shared that setting up a contraceptive program requires patience and education. “I cannot tell you how many women have come to me who don't know the different names of their body parts, women who've had two babies that don't understand how their body works. So, I constantly find myself taking extra time to do general sexual education,” she said.
There are many lessons to impart to patients about sexual health. For example, birth control drugs and devices do not prevent transmission of sexually transmitted infections (STIs). “So I have bowls of condoms literally everywhere because condoms are the only thing that protects against STIs,” Abel said.
In terms of devices, “we have diaphragms available and cervical caps,” she said. “The Caya diaphragm is a TRICARE-covered benefit. It’s a small purple diaphragm, one size fits most. We can prescribe it, and it is good for 2 years. Unfortunately, spermicide, which you have to use with these things, is not a TRICARE-covered benefit.”
Hormonal contraceptives are also available, with Abel recommending the continuous monophasic type for most women. “Please don't tell women they have to have their periods. They don't,” she said. “What I'm trying to do is give a woman some stability in her hormones. She can know and expect what she's going to feel like. She's not going to wake up and say, ‘Oh God, today's the day. I'm going to be like this for a week.’”
Patches are another option, and a flurry of patients have been asking about them because of recent TikTok videos promoting their use. “We have the Xulane patch, our bread and butter. They wear it on their shoulder, their hip, their butt, or their back. They leave it in place for a week at a time. And every week, they will change that patch. I usually have to walk patients through a whole month to help them understand how that works.”
Another option, the NuvaRing, is notable because it’s linked to low amounts of breakthrough bleeding Abel noted. An extended form is now available that doesn’t need to be removed during menstrual periods.
Medroxyprogesterone injections, which are linked to bone loss, and subdermal implants, which may be less effective in women over 130% of their ideal weight are also available, she said.
Finally, IUDs are an option, although when they fail, they’re linked to ectopic pregnancies.
Abel has no disclosures.