User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
Residency match process under scrutiny again, this time by AMA
The American Medical Association is considering whether to study alternatives to the current residency matching program in an effort to improve residents’ compensation and other job-related issues. A recent call-to-action resolution by the AMA’s House of Delegates is the latest in a long string of debates about whether to change the annual process that matches future doctors with compatible residency programs.
AMA’s Resident and Fellow Section introduced the resolution in March, and the delegates approved it earlier in June at AMA’s annual meeting. The resolution states that the match process of the National Resident Matching Program (NRMP) “poses significant anticompetition concerns.” Those include preventing residents from negotiating for higher wages, better benefits, and improved working conditions, according to the approved resolution.
The full AMA board still has to consider the resolution and hasn’t set a date for that review, though it’s expected to be in the next few months, according to Jennifer Sellers, AMA’s public information officer. She said in an interview that the organization declined to comment, wanting to hold off until the board decides how to proceed.
The NRMP, which oversees the matching process, told this news organization that the AMA doesn’t play a role in the Match.
The organization doesn’t believe studying alternative placement methods benefits applicants and residents, and returning to a pre-Match environment, would harm applicants and programs, according to Donna Lamb, DHSc, MBA, BSN, president and CEO.
“The NRMP has no role in determining, publishing, or setting resident salaries nor does the NRMP have a role in the contracting or employment of residents, and it never has.”
Dr. Lamb said changing the Match would “subject applicants to undue pressure and coercion to accept an offer of training. This will exacerbate disparities in candidate selection already evident in medical education and potentially result in salary reductions in more competitive specialties and in more desirable geographic locations.”
The latest push to reform the match process dates back two decades to a 2002 class action antitrust lawsuit by residents and doctors against the NRMP and other organizations involved in the Match.
The residents argued at that time that by restraining competition among teaching hospitals, the matching system allowed hospitals to keep residents’ wages artificially low. The defendants, which included large teaching hospitals, successfully lobbied Congress for an exemption to the antitrust laws, and the case was subsequently dismissed.
The AMA was one of the defendants, so if it moves forward to review the match process, it likely would pit the organization against the NRMP.
Sherman Marek, the attorney who represented the residents, said in an interview that he was not surprised by the latest AMA resolution. “Maybe the AMA leadership has come around to the idea that it’s better for young physicians to not have the match in place,” he says. “I would applaud that sort of evolution.”
Tyler Ramsey, DO, an internal medicine resident and AMA member, said he believes the group’s current president, Jesse Ehrenfeld, MD, MPH, empathizes with doctors in training. “I think he understands [our] views and is more progressive.”
The NRMP also has considered ways to improve the match process to make it easier and more equitable for applicants. In its latest effort, the organization is studying whether programs should certify their rank order list in advance of applicants. This change would give applicants more flexibility to visit residency locations before the programs consider changing their rankings, Dr. Lamb explained. The NRMP also is mulling the possibilities of a two-phase match after deciding in 2022 not to move forward with a previous version of the proposal.
The recent House of Delegates resolution states that “residents are using other means to obtain fair wages, safe working conditions, and other benefits that are unable to be negotiated within the current system.”
Dr. Ramsey, who trains in North Carolina, said the “other means” may include negotiating through a union. “The AMA realizes that there is a problem and that people are unionizing,” he said. “Obviously, as an organization, we’re not doing something correctly, to the point where people are feeling the need to get their rights a different way.”
The Committee of Interns and Residents, which represents 30,000 members, reported a rise in medical trainee unions across the country in 2022.
Not everyone believes that ditching the Match would benefit applicants and residents. Sam Payabvash, MD, assistant professor of radiology at Yale, New Haven, Conn., School of Medicine, tweeted about the resolution as part of a larger Twitter discussion that alternatives are likely to be “more onerous and expensive for applicants.”
An advantage of the match program, Dr. Lamb argued, is that it “improves the reach of applicants into medically underserved communities through widespread program participation.”
Dr. Ramsey agreed that the match program has benefits and drawbacks, but he believes it favors programs over residents. “It comes as no surprise that numerous residents suffer from depression and our suicide rates are the highest amongst all professions due to the lack of control or negotiation of fair salary and working conditions. Overall, the way things are now, residents just do not have a lot of rights.”
A version of this article originally appeared on Medscape.com.
The American Medical Association is considering whether to study alternatives to the current residency matching program in an effort to improve residents’ compensation and other job-related issues. A recent call-to-action resolution by the AMA’s House of Delegates is the latest in a long string of debates about whether to change the annual process that matches future doctors with compatible residency programs.
AMA’s Resident and Fellow Section introduced the resolution in March, and the delegates approved it earlier in June at AMA’s annual meeting. The resolution states that the match process of the National Resident Matching Program (NRMP) “poses significant anticompetition concerns.” Those include preventing residents from negotiating for higher wages, better benefits, and improved working conditions, according to the approved resolution.
The full AMA board still has to consider the resolution and hasn’t set a date for that review, though it’s expected to be in the next few months, according to Jennifer Sellers, AMA’s public information officer. She said in an interview that the organization declined to comment, wanting to hold off until the board decides how to proceed.
The NRMP, which oversees the matching process, told this news organization that the AMA doesn’t play a role in the Match.
The organization doesn’t believe studying alternative placement methods benefits applicants and residents, and returning to a pre-Match environment, would harm applicants and programs, according to Donna Lamb, DHSc, MBA, BSN, president and CEO.
“The NRMP has no role in determining, publishing, or setting resident salaries nor does the NRMP have a role in the contracting or employment of residents, and it never has.”
Dr. Lamb said changing the Match would “subject applicants to undue pressure and coercion to accept an offer of training. This will exacerbate disparities in candidate selection already evident in medical education and potentially result in salary reductions in more competitive specialties and in more desirable geographic locations.”
The latest push to reform the match process dates back two decades to a 2002 class action antitrust lawsuit by residents and doctors against the NRMP and other organizations involved in the Match.
The residents argued at that time that by restraining competition among teaching hospitals, the matching system allowed hospitals to keep residents’ wages artificially low. The defendants, which included large teaching hospitals, successfully lobbied Congress for an exemption to the antitrust laws, and the case was subsequently dismissed.
The AMA was one of the defendants, so if it moves forward to review the match process, it likely would pit the organization against the NRMP.
Sherman Marek, the attorney who represented the residents, said in an interview that he was not surprised by the latest AMA resolution. “Maybe the AMA leadership has come around to the idea that it’s better for young physicians to not have the match in place,” he says. “I would applaud that sort of evolution.”
Tyler Ramsey, DO, an internal medicine resident and AMA member, said he believes the group’s current president, Jesse Ehrenfeld, MD, MPH, empathizes with doctors in training. “I think he understands [our] views and is more progressive.”
The NRMP also has considered ways to improve the match process to make it easier and more equitable for applicants. In its latest effort, the organization is studying whether programs should certify their rank order list in advance of applicants. This change would give applicants more flexibility to visit residency locations before the programs consider changing their rankings, Dr. Lamb explained. The NRMP also is mulling the possibilities of a two-phase match after deciding in 2022 not to move forward with a previous version of the proposal.
The recent House of Delegates resolution states that “residents are using other means to obtain fair wages, safe working conditions, and other benefits that are unable to be negotiated within the current system.”
Dr. Ramsey, who trains in North Carolina, said the “other means” may include negotiating through a union. “The AMA realizes that there is a problem and that people are unionizing,” he said. “Obviously, as an organization, we’re not doing something correctly, to the point where people are feeling the need to get their rights a different way.”
The Committee of Interns and Residents, which represents 30,000 members, reported a rise in medical trainee unions across the country in 2022.
Not everyone believes that ditching the Match would benefit applicants and residents. Sam Payabvash, MD, assistant professor of radiology at Yale, New Haven, Conn., School of Medicine, tweeted about the resolution as part of a larger Twitter discussion that alternatives are likely to be “more onerous and expensive for applicants.”
An advantage of the match program, Dr. Lamb argued, is that it “improves the reach of applicants into medically underserved communities through widespread program participation.”
Dr. Ramsey agreed that the match program has benefits and drawbacks, but he believes it favors programs over residents. “It comes as no surprise that numerous residents suffer from depression and our suicide rates are the highest amongst all professions due to the lack of control or negotiation of fair salary and working conditions. Overall, the way things are now, residents just do not have a lot of rights.”
A version of this article originally appeared on Medscape.com.
The American Medical Association is considering whether to study alternatives to the current residency matching program in an effort to improve residents’ compensation and other job-related issues. A recent call-to-action resolution by the AMA’s House of Delegates is the latest in a long string of debates about whether to change the annual process that matches future doctors with compatible residency programs.
AMA’s Resident and Fellow Section introduced the resolution in March, and the delegates approved it earlier in June at AMA’s annual meeting. The resolution states that the match process of the National Resident Matching Program (NRMP) “poses significant anticompetition concerns.” Those include preventing residents from negotiating for higher wages, better benefits, and improved working conditions, according to the approved resolution.
The full AMA board still has to consider the resolution and hasn’t set a date for that review, though it’s expected to be in the next few months, according to Jennifer Sellers, AMA’s public information officer. She said in an interview that the organization declined to comment, wanting to hold off until the board decides how to proceed.
The NRMP, which oversees the matching process, told this news organization that the AMA doesn’t play a role in the Match.
The organization doesn’t believe studying alternative placement methods benefits applicants and residents, and returning to a pre-Match environment, would harm applicants and programs, according to Donna Lamb, DHSc, MBA, BSN, president and CEO.
“The NRMP has no role in determining, publishing, or setting resident salaries nor does the NRMP have a role in the contracting or employment of residents, and it never has.”
Dr. Lamb said changing the Match would “subject applicants to undue pressure and coercion to accept an offer of training. This will exacerbate disparities in candidate selection already evident in medical education and potentially result in salary reductions in more competitive specialties and in more desirable geographic locations.”
The latest push to reform the match process dates back two decades to a 2002 class action antitrust lawsuit by residents and doctors against the NRMP and other organizations involved in the Match.
The residents argued at that time that by restraining competition among teaching hospitals, the matching system allowed hospitals to keep residents’ wages artificially low. The defendants, which included large teaching hospitals, successfully lobbied Congress for an exemption to the antitrust laws, and the case was subsequently dismissed.
The AMA was one of the defendants, so if it moves forward to review the match process, it likely would pit the organization against the NRMP.
Sherman Marek, the attorney who represented the residents, said in an interview that he was not surprised by the latest AMA resolution. “Maybe the AMA leadership has come around to the idea that it’s better for young physicians to not have the match in place,” he says. “I would applaud that sort of evolution.”
Tyler Ramsey, DO, an internal medicine resident and AMA member, said he believes the group’s current president, Jesse Ehrenfeld, MD, MPH, empathizes with doctors in training. “I think he understands [our] views and is more progressive.”
The NRMP also has considered ways to improve the match process to make it easier and more equitable for applicants. In its latest effort, the organization is studying whether programs should certify their rank order list in advance of applicants. This change would give applicants more flexibility to visit residency locations before the programs consider changing their rankings, Dr. Lamb explained. The NRMP also is mulling the possibilities of a two-phase match after deciding in 2022 not to move forward with a previous version of the proposal.
The recent House of Delegates resolution states that “residents are using other means to obtain fair wages, safe working conditions, and other benefits that are unable to be negotiated within the current system.”
Dr. Ramsey, who trains in North Carolina, said the “other means” may include negotiating through a union. “The AMA realizes that there is a problem and that people are unionizing,” he said. “Obviously, as an organization, we’re not doing something correctly, to the point where people are feeling the need to get their rights a different way.”
The Committee of Interns and Residents, which represents 30,000 members, reported a rise in medical trainee unions across the country in 2022.
Not everyone believes that ditching the Match would benefit applicants and residents. Sam Payabvash, MD, assistant professor of radiology at Yale, New Haven, Conn., School of Medicine, tweeted about the resolution as part of a larger Twitter discussion that alternatives are likely to be “more onerous and expensive for applicants.”
An advantage of the match program, Dr. Lamb argued, is that it “improves the reach of applicants into medically underserved communities through widespread program participation.”
Dr. Ramsey agreed that the match program has benefits and drawbacks, but he believes it favors programs over residents. “It comes as no surprise that numerous residents suffer from depression and our suicide rates are the highest amongst all professions due to the lack of control or negotiation of fair salary and working conditions. Overall, the way things are now, residents just do not have a lot of rights.”
A version of this article originally appeared on Medscape.com.
Migraine treatment with rimegepant linked to reduced barbiturate use
AUSTIN – , according to a real-world analysis. Butalbital is the only commonly prescribed short-acting barbiturate in the United States, according to Noah Rosen, MD, who presented the study at the annual meeting of the American Headache Society.
Despite its effectiveness, the drug carries a risk of abuse as well as neurologic side effects, and has also been linked to an increase in medication overuse headache, which in turn can affect quality of life and lead to more disability and health care costs. “Although acute treatment recommendations supported by AHS discourage the use of barbiturates for the acute treatment of migraine, butalbital and associated medications are still widely prescribed, so effective, low-risk novel abortive and preventive therapies that have potential barbiturate-sparing characteristics do have the potential to help people with migraine,” said Dr. Rosen during his presentation. He is the program director of neurology at Hofstra Northwell Health, Hempstead, N.Y.
His group previously showed an association between rimegepant initiation and a reduction in opioid use in another real-world analysis.
The present study retrospectively analyzed data from 34,486 patients drawn from the U.S.-based Longitudinal Access and Adjudication Data (LAAD) produced by IQVIA, which is an anonymized integrated commercial medical and prescription claims database. The period studied was between November 2015 and November 2022. The median age was 47 and 89% were female. Eligibility criteria included the presence of at least 6 months of baseline data before exposure to rimegepant and at least 6 months of follow-up, at least two rimegepant refills, and at least one butalbital prescription during the baseline period.
During the baseline period, the mean number of milligrams of butalbital dispensed was 1,012, and this dropped to 742 during follow-up (–26.7%). The mean number of butalbital prescription fills dropped from 0.47 to 0.32 (–32.0%). About half of patients (49.4%) had no butalbital refills after starting rimegepant. The researchers also examined triptan use and found no difference. “We saw that it actually made no significant difference with the deflection from baseline or discontinuation if they had been given a triptan or not. This seemed to concur with my own experiences with triptan use and not affecting barbiturate dosing,” said Dr. Rosen.
‘Good news’
The results are good news, according to Jason Sico, MD, who comoderated the session. “I remember being a PGY-2 neurology resident and hearing a lecture from Stew Tepper [now professor of medicine at Geisel School of Medicine at Dartmouth, Hanover, N.H.] that fiorinal and fioricet were the F words of headache medicine, so it’s really great to see a modality that could lower barbiturate use,” said Dr. Sico, who is an associate professor of neurology and internal medicine at Yale University, New Haven, Conn.
Dr. Rosen responded: “I don’t mean to malign a single chemical, because fioricet has provided many people treatment over time, but with the introduction of newer options, we would hope to see a trend toward that use.”
A listener on the virtual platform asked whether the decline in barbiturate use could be due to education by the provider on the dangers of barbiturate use when rimegepant was prescribed. “This is one of those big limitations of claims data analysis is we can speculate what the influence or the cause is, because this type of data analysis does not show causation. There are many different things that could influence the discontinuation. Education is a huge one, although you would hope that if somebody is prescribed butalbital on a regular basis, that there’s some physician contact or education that’s part of that as well. But it’s possible it plays a role,” said Dr. Rosen.
Any strategy to reduce butalbital use in migraine is important
Alan Rapoport, MD, who attended the session, was also asked to comment on the study. “Butalbital-containing medications can help headache pain but have not been approved by the FDA for a migraine indication. They can also decrease anxiety in the migraine patient, but if used frequently, they cause dependency. When used too often, butalbital-containing medications are major causes of medication overuse headache. They’re often used with other acute care medications such as triptans and over-the-counter products, and combinations of these drugs can be even more of a problem because one only needs to use any of these medicines in combination for 10 days a month or more, for at least 3 months, for a doctor to diagnose a patient with medication overuse headache. So any attempt and success to reduce the frequency of taking butalbital-containing medication is important. That can be done by counseling the patient to take fewer tablets per month, but this often does not work. This study shows a good success rate in reducing the use of these medications by treating the patient with rimegepant 75 mg ODT given once every other day. This dose has been approved by the FDA for prevention in migraine, but has not previously been shown as a treatment for overuse of butalbital or medication. Previous studies have shown that rimegepant reduced migraine days per month and the use of acute care medications monthly. It this study, rimegepant decreases the number of butalbital-containing medications taken,” said Dr. Rapoport, who is a clinical professor of neurology at the University of California, Los Angeles, and editor in chief of Neurology Reviews.
Dr. Rosen has financial ties to Allergan/Abbvie, Amgen, BioHaven, Eli Lilly, Lundbeck, Novartis, Supernus, and Teva. Dr. Sico did not disclose any conflicts of interest. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureaus of AbbVie, Dr. Reddy’s, Impel, Pfizer, and Teva Pharmaceutical Industries. He is editor in chief of Neurology Reviews and on the editorial board of CNS Drugs.
AUSTIN – , according to a real-world analysis. Butalbital is the only commonly prescribed short-acting barbiturate in the United States, according to Noah Rosen, MD, who presented the study at the annual meeting of the American Headache Society.
Despite its effectiveness, the drug carries a risk of abuse as well as neurologic side effects, and has also been linked to an increase in medication overuse headache, which in turn can affect quality of life and lead to more disability and health care costs. “Although acute treatment recommendations supported by AHS discourage the use of barbiturates for the acute treatment of migraine, butalbital and associated medications are still widely prescribed, so effective, low-risk novel abortive and preventive therapies that have potential barbiturate-sparing characteristics do have the potential to help people with migraine,” said Dr. Rosen during his presentation. He is the program director of neurology at Hofstra Northwell Health, Hempstead, N.Y.
His group previously showed an association between rimegepant initiation and a reduction in opioid use in another real-world analysis.
The present study retrospectively analyzed data from 34,486 patients drawn from the U.S.-based Longitudinal Access and Adjudication Data (LAAD) produced by IQVIA, which is an anonymized integrated commercial medical and prescription claims database. The period studied was between November 2015 and November 2022. The median age was 47 and 89% were female. Eligibility criteria included the presence of at least 6 months of baseline data before exposure to rimegepant and at least 6 months of follow-up, at least two rimegepant refills, and at least one butalbital prescription during the baseline period.
During the baseline period, the mean number of milligrams of butalbital dispensed was 1,012, and this dropped to 742 during follow-up (–26.7%). The mean number of butalbital prescription fills dropped from 0.47 to 0.32 (–32.0%). About half of patients (49.4%) had no butalbital refills after starting rimegepant. The researchers also examined triptan use and found no difference. “We saw that it actually made no significant difference with the deflection from baseline or discontinuation if they had been given a triptan or not. This seemed to concur with my own experiences with triptan use and not affecting barbiturate dosing,” said Dr. Rosen.
‘Good news’
The results are good news, according to Jason Sico, MD, who comoderated the session. “I remember being a PGY-2 neurology resident and hearing a lecture from Stew Tepper [now professor of medicine at Geisel School of Medicine at Dartmouth, Hanover, N.H.] that fiorinal and fioricet were the F words of headache medicine, so it’s really great to see a modality that could lower barbiturate use,” said Dr. Sico, who is an associate professor of neurology and internal medicine at Yale University, New Haven, Conn.
Dr. Rosen responded: “I don’t mean to malign a single chemical, because fioricet has provided many people treatment over time, but with the introduction of newer options, we would hope to see a trend toward that use.”
A listener on the virtual platform asked whether the decline in barbiturate use could be due to education by the provider on the dangers of barbiturate use when rimegepant was prescribed. “This is one of those big limitations of claims data analysis is we can speculate what the influence or the cause is, because this type of data analysis does not show causation. There are many different things that could influence the discontinuation. Education is a huge one, although you would hope that if somebody is prescribed butalbital on a regular basis, that there’s some physician contact or education that’s part of that as well. But it’s possible it plays a role,” said Dr. Rosen.
Any strategy to reduce butalbital use in migraine is important
Alan Rapoport, MD, who attended the session, was also asked to comment on the study. “Butalbital-containing medications can help headache pain but have not been approved by the FDA for a migraine indication. They can also decrease anxiety in the migraine patient, but if used frequently, they cause dependency. When used too often, butalbital-containing medications are major causes of medication overuse headache. They’re often used with other acute care medications such as triptans and over-the-counter products, and combinations of these drugs can be even more of a problem because one only needs to use any of these medicines in combination for 10 days a month or more, for at least 3 months, for a doctor to diagnose a patient with medication overuse headache. So any attempt and success to reduce the frequency of taking butalbital-containing medication is important. That can be done by counseling the patient to take fewer tablets per month, but this often does not work. This study shows a good success rate in reducing the use of these medications by treating the patient with rimegepant 75 mg ODT given once every other day. This dose has been approved by the FDA for prevention in migraine, but has not previously been shown as a treatment for overuse of butalbital or medication. Previous studies have shown that rimegepant reduced migraine days per month and the use of acute care medications monthly. It this study, rimegepant decreases the number of butalbital-containing medications taken,” said Dr. Rapoport, who is a clinical professor of neurology at the University of California, Los Angeles, and editor in chief of Neurology Reviews.
Dr. Rosen has financial ties to Allergan/Abbvie, Amgen, BioHaven, Eli Lilly, Lundbeck, Novartis, Supernus, and Teva. Dr. Sico did not disclose any conflicts of interest. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureaus of AbbVie, Dr. Reddy’s, Impel, Pfizer, and Teva Pharmaceutical Industries. He is editor in chief of Neurology Reviews and on the editorial board of CNS Drugs.
AUSTIN – , according to a real-world analysis. Butalbital is the only commonly prescribed short-acting barbiturate in the United States, according to Noah Rosen, MD, who presented the study at the annual meeting of the American Headache Society.
Despite its effectiveness, the drug carries a risk of abuse as well as neurologic side effects, and has also been linked to an increase in medication overuse headache, which in turn can affect quality of life and lead to more disability and health care costs. “Although acute treatment recommendations supported by AHS discourage the use of barbiturates for the acute treatment of migraine, butalbital and associated medications are still widely prescribed, so effective, low-risk novel abortive and preventive therapies that have potential barbiturate-sparing characteristics do have the potential to help people with migraine,” said Dr. Rosen during his presentation. He is the program director of neurology at Hofstra Northwell Health, Hempstead, N.Y.
His group previously showed an association between rimegepant initiation and a reduction in opioid use in another real-world analysis.
The present study retrospectively analyzed data from 34,486 patients drawn from the U.S.-based Longitudinal Access and Adjudication Data (LAAD) produced by IQVIA, which is an anonymized integrated commercial medical and prescription claims database. The period studied was between November 2015 and November 2022. The median age was 47 and 89% were female. Eligibility criteria included the presence of at least 6 months of baseline data before exposure to rimegepant and at least 6 months of follow-up, at least two rimegepant refills, and at least one butalbital prescription during the baseline period.
During the baseline period, the mean number of milligrams of butalbital dispensed was 1,012, and this dropped to 742 during follow-up (–26.7%). The mean number of butalbital prescription fills dropped from 0.47 to 0.32 (–32.0%). About half of patients (49.4%) had no butalbital refills after starting rimegepant. The researchers also examined triptan use and found no difference. “We saw that it actually made no significant difference with the deflection from baseline or discontinuation if they had been given a triptan or not. This seemed to concur with my own experiences with triptan use and not affecting barbiturate dosing,” said Dr. Rosen.
‘Good news’
The results are good news, according to Jason Sico, MD, who comoderated the session. “I remember being a PGY-2 neurology resident and hearing a lecture from Stew Tepper [now professor of medicine at Geisel School of Medicine at Dartmouth, Hanover, N.H.] that fiorinal and fioricet were the F words of headache medicine, so it’s really great to see a modality that could lower barbiturate use,” said Dr. Sico, who is an associate professor of neurology and internal medicine at Yale University, New Haven, Conn.
Dr. Rosen responded: “I don’t mean to malign a single chemical, because fioricet has provided many people treatment over time, but with the introduction of newer options, we would hope to see a trend toward that use.”
A listener on the virtual platform asked whether the decline in barbiturate use could be due to education by the provider on the dangers of barbiturate use when rimegepant was prescribed. “This is one of those big limitations of claims data analysis is we can speculate what the influence or the cause is, because this type of data analysis does not show causation. There are many different things that could influence the discontinuation. Education is a huge one, although you would hope that if somebody is prescribed butalbital on a regular basis, that there’s some physician contact or education that’s part of that as well. But it’s possible it plays a role,” said Dr. Rosen.
Any strategy to reduce butalbital use in migraine is important
Alan Rapoport, MD, who attended the session, was also asked to comment on the study. “Butalbital-containing medications can help headache pain but have not been approved by the FDA for a migraine indication. They can also decrease anxiety in the migraine patient, but if used frequently, they cause dependency. When used too often, butalbital-containing medications are major causes of medication overuse headache. They’re often used with other acute care medications such as triptans and over-the-counter products, and combinations of these drugs can be even more of a problem because one only needs to use any of these medicines in combination for 10 days a month or more, for at least 3 months, for a doctor to diagnose a patient with medication overuse headache. So any attempt and success to reduce the frequency of taking butalbital-containing medication is important. That can be done by counseling the patient to take fewer tablets per month, but this often does not work. This study shows a good success rate in reducing the use of these medications by treating the patient with rimegepant 75 mg ODT given once every other day. This dose has been approved by the FDA for prevention in migraine, but has not previously been shown as a treatment for overuse of butalbital or medication. Previous studies have shown that rimegepant reduced migraine days per month and the use of acute care medications monthly. It this study, rimegepant decreases the number of butalbital-containing medications taken,” said Dr. Rapoport, who is a clinical professor of neurology at the University of California, Los Angeles, and editor in chief of Neurology Reviews.
Dr. Rosen has financial ties to Allergan/Abbvie, Amgen, BioHaven, Eli Lilly, Lundbeck, Novartis, Supernus, and Teva. Dr. Sico did not disclose any conflicts of interest. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureaus of AbbVie, Dr. Reddy’s, Impel, Pfizer, and Teva Pharmaceutical Industries. He is editor in chief of Neurology Reviews and on the editorial board of CNS Drugs.
FROM AHS 2023
Safety first: Regulations
The word “regulations” gets a mixed response.
This is common in all industries, and certainly pharmaceuticals. On any given day there are stories on industry news sites about disputes between companies and regulatory agencies.
I’d agree that some regulation is needed. The history of pharmacy has had both remarkable successes – and failures.
Let’s look at migraines, since that’s in my field. The calcitonin gene-related peptide (CGRP) drugs have been a remarkable breakthrough, certainly the biggest one since the triptans in 1992. There are currently seven on the market for both prevention and abortive use. They’re effective and (to date) pretty safe.
But it wasn’t always that way. Look back just 14 years ago to 2009, when the first promising CGRP agent (MK-3207) had its development halted because of hepatic abnormalities. It’s cousin telcagepant (MK-0974) came to a similar end 2 years later.
Without regulations in place (and the potential for lawsuits) these might have made it to market, bringing migraine relief to some and potentially serious liver damage to others. So Merck made the right decision to axe them. Researchers learned from the experience, went back to the drawing board, and developed the current generation of far-safer drugs.
This came into sharp focus in another industry recently, when the eyes of the world were on the north Atlantic. A small tourist submarine imploded and killed five people. During the inevitable media coverage it came out that the submarine hadn’t been certified for safety by any of the agencies that handle such things, falling into a gray area in international waters where inspections aren’t required.
This isn’t to say it wasn’t safe – it had made several dives before – but obviously not safe enough. While I didn’t know the late Stockton Rush (the owner/designer) it sounds like he viewed regulations as stifling innovation, and in one interview said “at some point, safety is just pure waste.” He ignored warnings from several sides about the submersible’s ability to handle deep ocean pressure and the inevitable wear and tear repeated dives will have on the hull.
I understand there’s a margin of luck, too. Bad things can happen to any of us – or any company. Some things can’t be clearly foreseen. Some drugs don’t start to show problems until they’re on the market and reach a certain number of prescriptions.
But there’s a reason we have regulations. Pretty much every government has, going back to the Roman Empire, covering numerous things. In a perfect world we wouldn’t need them.
But people are far from perfect. And the consequences can be terrible.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
The word “regulations” gets a mixed response.
This is common in all industries, and certainly pharmaceuticals. On any given day there are stories on industry news sites about disputes between companies and regulatory agencies.
I’d agree that some regulation is needed. The history of pharmacy has had both remarkable successes – and failures.
Let’s look at migraines, since that’s in my field. The calcitonin gene-related peptide (CGRP) drugs have been a remarkable breakthrough, certainly the biggest one since the triptans in 1992. There are currently seven on the market for both prevention and abortive use. They’re effective and (to date) pretty safe.
But it wasn’t always that way. Look back just 14 years ago to 2009, when the first promising CGRP agent (MK-3207) had its development halted because of hepatic abnormalities. It’s cousin telcagepant (MK-0974) came to a similar end 2 years later.
Without regulations in place (and the potential for lawsuits) these might have made it to market, bringing migraine relief to some and potentially serious liver damage to others. So Merck made the right decision to axe them. Researchers learned from the experience, went back to the drawing board, and developed the current generation of far-safer drugs.
This came into sharp focus in another industry recently, when the eyes of the world were on the north Atlantic. A small tourist submarine imploded and killed five people. During the inevitable media coverage it came out that the submarine hadn’t been certified for safety by any of the agencies that handle such things, falling into a gray area in international waters where inspections aren’t required.
This isn’t to say it wasn’t safe – it had made several dives before – but obviously not safe enough. While I didn’t know the late Stockton Rush (the owner/designer) it sounds like he viewed regulations as stifling innovation, and in one interview said “at some point, safety is just pure waste.” He ignored warnings from several sides about the submersible’s ability to handle deep ocean pressure and the inevitable wear and tear repeated dives will have on the hull.
I understand there’s a margin of luck, too. Bad things can happen to any of us – or any company. Some things can’t be clearly foreseen. Some drugs don’t start to show problems until they’re on the market and reach a certain number of prescriptions.
But there’s a reason we have regulations. Pretty much every government has, going back to the Roman Empire, covering numerous things. In a perfect world we wouldn’t need them.
But people are far from perfect. And the consequences can be terrible.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
The word “regulations” gets a mixed response.
This is common in all industries, and certainly pharmaceuticals. On any given day there are stories on industry news sites about disputes between companies and regulatory agencies.
I’d agree that some regulation is needed. The history of pharmacy has had both remarkable successes – and failures.
Let’s look at migraines, since that’s in my field. The calcitonin gene-related peptide (CGRP) drugs have been a remarkable breakthrough, certainly the biggest one since the triptans in 1992. There are currently seven on the market for both prevention and abortive use. They’re effective and (to date) pretty safe.
But it wasn’t always that way. Look back just 14 years ago to 2009, when the first promising CGRP agent (MK-3207) had its development halted because of hepatic abnormalities. It’s cousin telcagepant (MK-0974) came to a similar end 2 years later.
Without regulations in place (and the potential for lawsuits) these might have made it to market, bringing migraine relief to some and potentially serious liver damage to others. So Merck made the right decision to axe them. Researchers learned from the experience, went back to the drawing board, and developed the current generation of far-safer drugs.
This came into sharp focus in another industry recently, when the eyes of the world were on the north Atlantic. A small tourist submarine imploded and killed five people. During the inevitable media coverage it came out that the submarine hadn’t been certified for safety by any of the agencies that handle such things, falling into a gray area in international waters where inspections aren’t required.
This isn’t to say it wasn’t safe – it had made several dives before – but obviously not safe enough. While I didn’t know the late Stockton Rush (the owner/designer) it sounds like he viewed regulations as stifling innovation, and in one interview said “at some point, safety is just pure waste.” He ignored warnings from several sides about the submersible’s ability to handle deep ocean pressure and the inevitable wear and tear repeated dives will have on the hull.
I understand there’s a margin of luck, too. Bad things can happen to any of us – or any company. Some things can’t be clearly foreseen. Some drugs don’t start to show problems until they’re on the market and reach a certain number of prescriptions.
But there’s a reason we have regulations. Pretty much every government has, going back to the Roman Empire, covering numerous things. In a perfect world we wouldn’t need them.
But people are far from perfect. And the consequences can be terrible.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
AI model interprets EEGs with near-perfect accuracy
An automated artificial intelligence (AI) model trained to read electroencephalograms (EEGs) in patients with suspected epilepsy is just as accurate as trained neurologists, new data suggest.
Known as SCORE-AI, the technology distinguishes between abnormal and normal EEG recordings and classifies irregular recordings into specific categories crucial for patient decision-making.
“SCORE-AI can be used in place of experts in underprivileged areas, where expertise is missing, or to help physicians to preselect or prescore recordings in areas where the workload is high – we can all benefit from AI,” study investigator Sándor Beniczky, MD, PhD, said in a JAMA Neurology podcast.
Dr. Beniczky is professor of clinical neurophysiology at Aarhus University in Denmark.
The findings were published online in JAMA Neurology.
Gaining a foothold
Increasingly, AI is gaining a foothold in medicine by credibly addressing patient queries and aiding radiologists.
To bring AI to EEG interpretation, the researchers developed and validated an AI model that was able to assess routine, clinical EEGs in patients with suspected epilepsy.
Beyond using AI to distinguish abnormal from normal EEG recordings, the researchers wanted to train the new system to classify abnormal recordings into the major categories that are most relevant for clinical decision-making in patients who may have epilepsy. The categories included epileptiform-focal, epileptiform-generalized, nonepileptiform-focal, and nonepileptiform-diffuse abnormalities.
The researchers trained the learning model using Standardized Computer-based Organized Reporting of EEG (SCORE) software.
In the development phase, the model was trained using more than 30,490 anonymized and highly annotated EEG recordings from 14,100 men (median age, 25 years) from a single center. The recordings had an average duration of 31 minutes and were interpreted by 17 neurologists using standardized criteria. If an EEG recording was abnormal, the physicians had to specify which abnormal features were present.
SCORE-AI then performed an analysis of the recordings based on input from the experts.
To validate the findings, investigators used two independent test datasets. The first dataset consisted of 100 representative routine EEGs from 61 men (median age, 26 years), evaluated by 11 neurologists from different centers.
The consensus of these evaluations served as the reference standard. The second dataset comprised nearly 10,000 EEGs from a single center (5,170 men; median age, 35 years), independently assessed by 14 neurologists.
Near-perfect accuracy
When compared with the experts, SCORE-AI had near-perfect accuracy with an area under the receiver operating characteristic (AUROC) curve for differentiating normal from abnormal EEG recordings of 0.95.
SCORE-AI also performed well at identifying generalized epileptiform abnormalities (AUROC, 0.96), focal epileptiform abnormalities (AUROC, 0.91), focal nonepileptiform abnormalities (AUROC, 0.89), and diffuse nonepileptiform abnormalities (AUROC, 0.93).
In addition, SCORE-AI had excellent agreement with clinicians – and sometimes agreed with individual experts more than the experts agreed with one another.
When Dr. Beniczky and team tested SCORE-AI against three previously published AI models, SCORE-AI demonstrated greater specificity than those models (90% vs. 3%-63%) but was not as sensitive (86.7%) as two of the models (96.7% and 100%).
One of the study’s limitations was the fact that SCORE-AI was developed and validated on routine EEGs that excluded neonates and critically ill patients.
In the future, Dr. Beniczky said on the podcast, the team would like to train SCORE-AI to read EEGs with more granularity, and eventually use only one single channel to record EEGs. At present, SCORE-AI is being integrated with Natus Neuro, a widely used EEG equipment system, the investigators note.
In an accompanying editorial, Jonathan Kleen, MD, PhD, and Elan Guterman, MD, said, “The overall approach taken ... in developing and validating SCORE-AI sets a standard for this work going forward.”
Dr. Kleen and Dr. Guterman note that the technological gains brought about by SCORE-AI technology “could offer an exciting prospect to improve EEG availability and clinical care for the 50 million people with epilepsy worldwide.”
A version of this article originally appeared on Medscape.com.
An automated artificial intelligence (AI) model trained to read electroencephalograms (EEGs) in patients with suspected epilepsy is just as accurate as trained neurologists, new data suggest.
Known as SCORE-AI, the technology distinguishes between abnormal and normal EEG recordings and classifies irregular recordings into specific categories crucial for patient decision-making.
“SCORE-AI can be used in place of experts in underprivileged areas, where expertise is missing, or to help physicians to preselect or prescore recordings in areas where the workload is high – we can all benefit from AI,” study investigator Sándor Beniczky, MD, PhD, said in a JAMA Neurology podcast.
Dr. Beniczky is professor of clinical neurophysiology at Aarhus University in Denmark.
The findings were published online in JAMA Neurology.
Gaining a foothold
Increasingly, AI is gaining a foothold in medicine by credibly addressing patient queries and aiding radiologists.
To bring AI to EEG interpretation, the researchers developed and validated an AI model that was able to assess routine, clinical EEGs in patients with suspected epilepsy.
Beyond using AI to distinguish abnormal from normal EEG recordings, the researchers wanted to train the new system to classify abnormal recordings into the major categories that are most relevant for clinical decision-making in patients who may have epilepsy. The categories included epileptiform-focal, epileptiform-generalized, nonepileptiform-focal, and nonepileptiform-diffuse abnormalities.
The researchers trained the learning model using Standardized Computer-based Organized Reporting of EEG (SCORE) software.
In the development phase, the model was trained using more than 30,490 anonymized and highly annotated EEG recordings from 14,100 men (median age, 25 years) from a single center. The recordings had an average duration of 31 minutes and were interpreted by 17 neurologists using standardized criteria. If an EEG recording was abnormal, the physicians had to specify which abnormal features were present.
SCORE-AI then performed an analysis of the recordings based on input from the experts.
To validate the findings, investigators used two independent test datasets. The first dataset consisted of 100 representative routine EEGs from 61 men (median age, 26 years), evaluated by 11 neurologists from different centers.
The consensus of these evaluations served as the reference standard. The second dataset comprised nearly 10,000 EEGs from a single center (5,170 men; median age, 35 years), independently assessed by 14 neurologists.
Near-perfect accuracy
When compared with the experts, SCORE-AI had near-perfect accuracy with an area under the receiver operating characteristic (AUROC) curve for differentiating normal from abnormal EEG recordings of 0.95.
SCORE-AI also performed well at identifying generalized epileptiform abnormalities (AUROC, 0.96), focal epileptiform abnormalities (AUROC, 0.91), focal nonepileptiform abnormalities (AUROC, 0.89), and diffuse nonepileptiform abnormalities (AUROC, 0.93).
In addition, SCORE-AI had excellent agreement with clinicians – and sometimes agreed with individual experts more than the experts agreed with one another.
When Dr. Beniczky and team tested SCORE-AI against three previously published AI models, SCORE-AI demonstrated greater specificity than those models (90% vs. 3%-63%) but was not as sensitive (86.7%) as two of the models (96.7% and 100%).
One of the study’s limitations was the fact that SCORE-AI was developed and validated on routine EEGs that excluded neonates and critically ill patients.
In the future, Dr. Beniczky said on the podcast, the team would like to train SCORE-AI to read EEGs with more granularity, and eventually use only one single channel to record EEGs. At present, SCORE-AI is being integrated with Natus Neuro, a widely used EEG equipment system, the investigators note.
In an accompanying editorial, Jonathan Kleen, MD, PhD, and Elan Guterman, MD, said, “The overall approach taken ... in developing and validating SCORE-AI sets a standard for this work going forward.”
Dr. Kleen and Dr. Guterman note that the technological gains brought about by SCORE-AI technology “could offer an exciting prospect to improve EEG availability and clinical care for the 50 million people with epilepsy worldwide.”
A version of this article originally appeared on Medscape.com.
An automated artificial intelligence (AI) model trained to read electroencephalograms (EEGs) in patients with suspected epilepsy is just as accurate as trained neurologists, new data suggest.
Known as SCORE-AI, the technology distinguishes between abnormal and normal EEG recordings and classifies irregular recordings into specific categories crucial for patient decision-making.
“SCORE-AI can be used in place of experts in underprivileged areas, where expertise is missing, or to help physicians to preselect or prescore recordings in areas where the workload is high – we can all benefit from AI,” study investigator Sándor Beniczky, MD, PhD, said in a JAMA Neurology podcast.
Dr. Beniczky is professor of clinical neurophysiology at Aarhus University in Denmark.
The findings were published online in JAMA Neurology.
Gaining a foothold
Increasingly, AI is gaining a foothold in medicine by credibly addressing patient queries and aiding radiologists.
To bring AI to EEG interpretation, the researchers developed and validated an AI model that was able to assess routine, clinical EEGs in patients with suspected epilepsy.
Beyond using AI to distinguish abnormal from normal EEG recordings, the researchers wanted to train the new system to classify abnormal recordings into the major categories that are most relevant for clinical decision-making in patients who may have epilepsy. The categories included epileptiform-focal, epileptiform-generalized, nonepileptiform-focal, and nonepileptiform-diffuse abnormalities.
The researchers trained the learning model using Standardized Computer-based Organized Reporting of EEG (SCORE) software.
In the development phase, the model was trained using more than 30,490 anonymized and highly annotated EEG recordings from 14,100 men (median age, 25 years) from a single center. The recordings had an average duration of 31 minutes and were interpreted by 17 neurologists using standardized criteria. If an EEG recording was abnormal, the physicians had to specify which abnormal features were present.
SCORE-AI then performed an analysis of the recordings based on input from the experts.
To validate the findings, investigators used two independent test datasets. The first dataset consisted of 100 representative routine EEGs from 61 men (median age, 26 years), evaluated by 11 neurologists from different centers.
The consensus of these evaluations served as the reference standard. The second dataset comprised nearly 10,000 EEGs from a single center (5,170 men; median age, 35 years), independently assessed by 14 neurologists.
Near-perfect accuracy
When compared with the experts, SCORE-AI had near-perfect accuracy with an area under the receiver operating characteristic (AUROC) curve for differentiating normal from abnormal EEG recordings of 0.95.
SCORE-AI also performed well at identifying generalized epileptiform abnormalities (AUROC, 0.96), focal epileptiform abnormalities (AUROC, 0.91), focal nonepileptiform abnormalities (AUROC, 0.89), and diffuse nonepileptiform abnormalities (AUROC, 0.93).
In addition, SCORE-AI had excellent agreement with clinicians – and sometimes agreed with individual experts more than the experts agreed with one another.
When Dr. Beniczky and team tested SCORE-AI against three previously published AI models, SCORE-AI demonstrated greater specificity than those models (90% vs. 3%-63%) but was not as sensitive (86.7%) as two of the models (96.7% and 100%).
One of the study’s limitations was the fact that SCORE-AI was developed and validated on routine EEGs that excluded neonates and critically ill patients.
In the future, Dr. Beniczky said on the podcast, the team would like to train SCORE-AI to read EEGs with more granularity, and eventually use only one single channel to record EEGs. At present, SCORE-AI is being integrated with Natus Neuro, a widely used EEG equipment system, the investigators note.
In an accompanying editorial, Jonathan Kleen, MD, PhD, and Elan Guterman, MD, said, “The overall approach taken ... in developing and validating SCORE-AI sets a standard for this work going forward.”
Dr. Kleen and Dr. Guterman note that the technological gains brought about by SCORE-AI technology “could offer an exciting prospect to improve EEG availability and clinical care for the 50 million people with epilepsy worldwide.”
A version of this article originally appeared on Medscape.com.
Placebo effect can be found in a cup of coffee
The best part of waking up is placebo in your cup
Coffee makes the world go round. It’s impossible to picture any workplace without a cast of forlorn characters huddled around the office coffee maker on a Monday morning, imbibing their beverage du jour until they’ve been lifted out of their semi-zombified stupor.
Millions upon millions of people swear by their morning coffee. And if they don’t get that sweet, sweet caffeine boost, they’ll make Garfield and the Boomtown Rats’ opinions of Mondays look tame. And it only makes sense that they’d believe that. After all, caffeine is a stimulant. It helps your brain focus and kicks it into overdrive. Of course drinking a beverage full of caffeine wakes you up. Right?
Not so fast, a group of Portuguese researchers say. That morning cup of coffee? It may actually be a placebo. Cue the dramatic sound effect.
Here’s the scoop: After recruiting a group of coffee drinkers (at least one cup a day), the researchers kept their test subjects off of coffee for at least 3 hours, then performed a brief functional MRI scan on all test subjects. Half an hour later, study participants received either a standard cup of coffee or pure caffeine. Half an hour after consuming their respective study product, the subjects underwent a second MRI.
As expected, both people who consumed coffee and those who consumed pure caffeine showed decreased connectivity in the default mode network after consumption, indicating preparation in the brain to move from resting to working on tasks. However, those who had pure caffeine did not show increased connectivity in the visual and executive control networks, while those who had coffee did. Simply put, caffeine may wake you up, but it doesn’t make you any sharper. Only coffee gets you in shape for that oh-so-important Monday meeting.
This doesn’t make a lot of sense. How can the drug part of coffee not be responsible for every effect the drink gives you? That’s where the placebo comes in, according to the scientists. It’s possible the effect they saw was caused by withdrawal – after just 3 hours? Yikes, hope not – but it’s more likely it comes down to psychology. We expect coffee to wake us up and make us ready for the day, so that’s exactly what it does. Hey, if that’s all it takes, time to convince ourselves that eating an entire pizza is actually an incredibly effective weight loss tool. Don’t let us down now, placebo effect.
Bread, milk, toilet paper, AFib diagnosis
Now consider the shopping cart. It does its job of carrying stuff around the store well enough, but can it lift you out of a semi-zombified stupor in the morning? No. Can it identify undiagnosed atrial fibrillation? Again, no.
Not so fast, say the investigators conducting the SHOPS-AF (Supermarket/Hypermarket Opportunistic Screening for Atrial Fibrillation) study. They built a better shopping cart. Except they call it a trolley, not a cart, since the study was conducted in England, where they sometimes have funny names for things.
Their improved shopping trolley – we’re just going to call it a cart from here on – has an electrocardiogram sensor embedded into the handlebar, so it can effectively detect AFib in shoppers who held it for at least 60 seconds. The sensor lights up red if it detects an irregular heartbeat and green if it does not. Let’s see a cup of coffee do that.
They put 10 of these modified carts in four supermarkets in Liverpool to see what would happen. Would shoppers be able to tell that we secretly replaced the fine coffee they usually serve with Folger’s crystals? Oops. Sorry about that. Coffee on the brain, apparently. Back to the carts.
A total of 2,155 adult shoppers used one of the carts over 2 months, and electrocardiogram data were available for 220 participants who either had a red light on the sensor and/or an irregular pulse that suggested atrial fibrillation. After further review by the SHOPS-AF cardiologist, AFib was diagnosed in 59 shoppers, of whom 39 were previously undiagnosed.
They’re already working to cut the scan time to 30 seconds for SHOPS-AF II, but we’re wondering about a possible flaw in the whole health-care-delivery-through-shopping-cart scenario. When we go to the local super/hyper/megamart, it seems like half of the people trundling up and down the aisles are store employees filling orders for customers who won’t even set foot inside. Is the shopping cart on its way out? Maybe. Who wants to tell the SHOPS-AF II team? Not us.
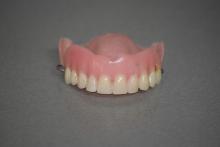
Put pneumonia where your mouth is
Getting dentures does not mean the end of dental care. If anything, new research reveals a huge reason for staying on top of one’s denture care: pneumonia.
It all started with swabs. Scientists in the United Kingdom took mouth, tongue, and denture specimens from frail elderly hospital patients who had pneumonia and wore dentures and from similar patients in care homes who wore dentures and did not have pneumonia. When they compared the microbial populations of the two groups, the investigators found about 20 times the number of respiratory pathogens on the dentures of those with pneumonia.
The research team suggested that dentures may play a role in causing pneumonia, but lead author Josh Twigg, BDS, PhD, also noted that “you certainly couldn’t say that people got pneumonia because they were wearing dentures. It’s just showing that there is an association there.” Improper cleaning, though, could lead to microbial colonization of the dentures, and patients could be inhaling those microbes into their lungs, thereby turning a dental issue into a respiratory issue.
More research needs to be done on the association between dentures and pneumonia, but Dr. Twigg hoped that the results of this study could be presented to the public. The message? “It is important to clean dentures thoroughly” and visit the dentist regularly, he said, but the best way to prevent denture-related infections is to avoid needing to wear dentures entirely.
The best part of waking up is placebo in your cup
Coffee makes the world go round. It’s impossible to picture any workplace without a cast of forlorn characters huddled around the office coffee maker on a Monday morning, imbibing their beverage du jour until they’ve been lifted out of their semi-zombified stupor.
Millions upon millions of people swear by their morning coffee. And if they don’t get that sweet, sweet caffeine boost, they’ll make Garfield and the Boomtown Rats’ opinions of Mondays look tame. And it only makes sense that they’d believe that. After all, caffeine is a stimulant. It helps your brain focus and kicks it into overdrive. Of course drinking a beverage full of caffeine wakes you up. Right?
Not so fast, a group of Portuguese researchers say. That morning cup of coffee? It may actually be a placebo. Cue the dramatic sound effect.
Here’s the scoop: After recruiting a group of coffee drinkers (at least one cup a day), the researchers kept their test subjects off of coffee for at least 3 hours, then performed a brief functional MRI scan on all test subjects. Half an hour later, study participants received either a standard cup of coffee or pure caffeine. Half an hour after consuming their respective study product, the subjects underwent a second MRI.
As expected, both people who consumed coffee and those who consumed pure caffeine showed decreased connectivity in the default mode network after consumption, indicating preparation in the brain to move from resting to working on tasks. However, those who had pure caffeine did not show increased connectivity in the visual and executive control networks, while those who had coffee did. Simply put, caffeine may wake you up, but it doesn’t make you any sharper. Only coffee gets you in shape for that oh-so-important Monday meeting.
This doesn’t make a lot of sense. How can the drug part of coffee not be responsible for every effect the drink gives you? That’s where the placebo comes in, according to the scientists. It’s possible the effect they saw was caused by withdrawal – after just 3 hours? Yikes, hope not – but it’s more likely it comes down to psychology. We expect coffee to wake us up and make us ready for the day, so that’s exactly what it does. Hey, if that’s all it takes, time to convince ourselves that eating an entire pizza is actually an incredibly effective weight loss tool. Don’t let us down now, placebo effect.
Bread, milk, toilet paper, AFib diagnosis
Now consider the shopping cart. It does its job of carrying stuff around the store well enough, but can it lift you out of a semi-zombified stupor in the morning? No. Can it identify undiagnosed atrial fibrillation? Again, no.
Not so fast, say the investigators conducting the SHOPS-AF (Supermarket/Hypermarket Opportunistic Screening for Atrial Fibrillation) study. They built a better shopping cart. Except they call it a trolley, not a cart, since the study was conducted in England, where they sometimes have funny names for things.
Their improved shopping trolley – we’re just going to call it a cart from here on – has an electrocardiogram sensor embedded into the handlebar, so it can effectively detect AFib in shoppers who held it for at least 60 seconds. The sensor lights up red if it detects an irregular heartbeat and green if it does not. Let’s see a cup of coffee do that.
They put 10 of these modified carts in four supermarkets in Liverpool to see what would happen. Would shoppers be able to tell that we secretly replaced the fine coffee they usually serve with Folger’s crystals? Oops. Sorry about that. Coffee on the brain, apparently. Back to the carts.
A total of 2,155 adult shoppers used one of the carts over 2 months, and electrocardiogram data were available for 220 participants who either had a red light on the sensor and/or an irregular pulse that suggested atrial fibrillation. After further review by the SHOPS-AF cardiologist, AFib was diagnosed in 59 shoppers, of whom 39 were previously undiagnosed.
They’re already working to cut the scan time to 30 seconds for SHOPS-AF II, but we’re wondering about a possible flaw in the whole health-care-delivery-through-shopping-cart scenario. When we go to the local super/hyper/megamart, it seems like half of the people trundling up and down the aisles are store employees filling orders for customers who won’t even set foot inside. Is the shopping cart on its way out? Maybe. Who wants to tell the SHOPS-AF II team? Not us.
Put pneumonia where your mouth is
Getting dentures does not mean the end of dental care. If anything, new research reveals a huge reason for staying on top of one’s denture care: pneumonia.
It all started with swabs. Scientists in the United Kingdom took mouth, tongue, and denture specimens from frail elderly hospital patients who had pneumonia and wore dentures and from similar patients in care homes who wore dentures and did not have pneumonia. When they compared the microbial populations of the two groups, the investigators found about 20 times the number of respiratory pathogens on the dentures of those with pneumonia.
The research team suggested that dentures may play a role in causing pneumonia, but lead author Josh Twigg, BDS, PhD, also noted that “you certainly couldn’t say that people got pneumonia because they were wearing dentures. It’s just showing that there is an association there.” Improper cleaning, though, could lead to microbial colonization of the dentures, and patients could be inhaling those microbes into their lungs, thereby turning a dental issue into a respiratory issue.
More research needs to be done on the association between dentures and pneumonia, but Dr. Twigg hoped that the results of this study could be presented to the public. The message? “It is important to clean dentures thoroughly” and visit the dentist regularly, he said, but the best way to prevent denture-related infections is to avoid needing to wear dentures entirely.
The best part of waking up is placebo in your cup
Coffee makes the world go round. It’s impossible to picture any workplace without a cast of forlorn characters huddled around the office coffee maker on a Monday morning, imbibing their beverage du jour until they’ve been lifted out of their semi-zombified stupor.
Millions upon millions of people swear by their morning coffee. And if they don’t get that sweet, sweet caffeine boost, they’ll make Garfield and the Boomtown Rats’ opinions of Mondays look tame. And it only makes sense that they’d believe that. After all, caffeine is a stimulant. It helps your brain focus and kicks it into overdrive. Of course drinking a beverage full of caffeine wakes you up. Right?
Not so fast, a group of Portuguese researchers say. That morning cup of coffee? It may actually be a placebo. Cue the dramatic sound effect.
Here’s the scoop: After recruiting a group of coffee drinkers (at least one cup a day), the researchers kept their test subjects off of coffee for at least 3 hours, then performed a brief functional MRI scan on all test subjects. Half an hour later, study participants received either a standard cup of coffee or pure caffeine. Half an hour after consuming their respective study product, the subjects underwent a second MRI.
As expected, both people who consumed coffee and those who consumed pure caffeine showed decreased connectivity in the default mode network after consumption, indicating preparation in the brain to move from resting to working on tasks. However, those who had pure caffeine did not show increased connectivity in the visual and executive control networks, while those who had coffee did. Simply put, caffeine may wake you up, but it doesn’t make you any sharper. Only coffee gets you in shape for that oh-so-important Monday meeting.
This doesn’t make a lot of sense. How can the drug part of coffee not be responsible for every effect the drink gives you? That’s where the placebo comes in, according to the scientists. It’s possible the effect they saw was caused by withdrawal – after just 3 hours? Yikes, hope not – but it’s more likely it comes down to psychology. We expect coffee to wake us up and make us ready for the day, so that’s exactly what it does. Hey, if that’s all it takes, time to convince ourselves that eating an entire pizza is actually an incredibly effective weight loss tool. Don’t let us down now, placebo effect.
Bread, milk, toilet paper, AFib diagnosis
Now consider the shopping cart. It does its job of carrying stuff around the store well enough, but can it lift you out of a semi-zombified stupor in the morning? No. Can it identify undiagnosed atrial fibrillation? Again, no.
Not so fast, say the investigators conducting the SHOPS-AF (Supermarket/Hypermarket Opportunistic Screening for Atrial Fibrillation) study. They built a better shopping cart. Except they call it a trolley, not a cart, since the study was conducted in England, where they sometimes have funny names for things.
Their improved shopping trolley – we’re just going to call it a cart from here on – has an electrocardiogram sensor embedded into the handlebar, so it can effectively detect AFib in shoppers who held it for at least 60 seconds. The sensor lights up red if it detects an irregular heartbeat and green if it does not. Let’s see a cup of coffee do that.
They put 10 of these modified carts in four supermarkets in Liverpool to see what would happen. Would shoppers be able to tell that we secretly replaced the fine coffee they usually serve with Folger’s crystals? Oops. Sorry about that. Coffee on the brain, apparently. Back to the carts.
A total of 2,155 adult shoppers used one of the carts over 2 months, and electrocardiogram data were available for 220 participants who either had a red light on the sensor and/or an irregular pulse that suggested atrial fibrillation. After further review by the SHOPS-AF cardiologist, AFib was diagnosed in 59 shoppers, of whom 39 were previously undiagnosed.
They’re already working to cut the scan time to 30 seconds for SHOPS-AF II, but we’re wondering about a possible flaw in the whole health-care-delivery-through-shopping-cart scenario. When we go to the local super/hyper/megamart, it seems like half of the people trundling up and down the aisles are store employees filling orders for customers who won’t even set foot inside. Is the shopping cart on its way out? Maybe. Who wants to tell the SHOPS-AF II team? Not us.
Put pneumonia where your mouth is
Getting dentures does not mean the end of dental care. If anything, new research reveals a huge reason for staying on top of one’s denture care: pneumonia.
It all started with swabs. Scientists in the United Kingdom took mouth, tongue, and denture specimens from frail elderly hospital patients who had pneumonia and wore dentures and from similar patients in care homes who wore dentures and did not have pneumonia. When they compared the microbial populations of the two groups, the investigators found about 20 times the number of respiratory pathogens on the dentures of those with pneumonia.
The research team suggested that dentures may play a role in causing pneumonia, but lead author Josh Twigg, BDS, PhD, also noted that “you certainly couldn’t say that people got pneumonia because they were wearing dentures. It’s just showing that there is an association there.” Improper cleaning, though, could lead to microbial colonization of the dentures, and patients could be inhaling those microbes into their lungs, thereby turning a dental issue into a respiratory issue.
More research needs to be done on the association between dentures and pneumonia, but Dr. Twigg hoped that the results of this study could be presented to the public. The message? “It is important to clean dentures thoroughly” and visit the dentist regularly, he said, but the best way to prevent denture-related infections is to avoid needing to wear dentures entirely.
Anti-CGRP monoclonal antibody offers relief from migraine and comorbid depression
AUSTIN, TEX. – , new research shows.
Patients with both conditions who were randomly assigned to receive fremanezumab showed a statistically significant reduction in both the 17-item Hamilton Depression Rating Scale (HAMD-17) and the nine-criteria Patient Health Questionnaire (PHQ-9) scores, compared with matched controls who received placebo.
The results from the UNITE trial were presented at the annual meeting of the American Headache Society.
Long-standing questions
“It’s been well known for a long time that migraine is comorbid with a number of illnesses, and one of the most common is depression,” said study investigator Richard B. Lipton, a professor of neurology at Albert Einstein College of Medicine and the director of the Montefiore Headache Center, New York.
“Do you treat the depression? Do you treat the migraine? Do you independently treat both? Those have been long-standing questions for clinicians,” Dr. Lipton said.
Investigators randomly assigned 330 adults with migraine who were diagnosed with moderate-to-severe MDD (defined as a PHQ-9 score of 10 or greater) to receive 225 mg subcutaneous monthly fremanezumab (n = 164) or placebo (n = 166) for 12 weeks.
The trial continued as an open-label trial for another 12 weeks.
During the double-blind phase of the study, the mean change from baseline in the HAMD-17 score with placebo was –4.6 at week 8 and –5.4 at week 12, compared with –6.0 with fremanezumab at week 8 (P = .0205) and –6.7 at week 12 (P = .0228).
The change from baseline in PHQ-9 total score at week 8 was –5.8 for placebo and –7.1 for fremanezumab (P = .0283). At week 12, the change was –6.3 for placebo versus –7.8 for fremanezumab (P = .0108). These reductions were maintained throughout the open-label period of the trial.
The beneficial effect on depression and migraine demonstrated in the study is interesting on several levels, Dr. Lipton said.
“One, it tells us that if the patient has migraine and depression and you treat with fremanezumab, both disorders get better to a statistically significant degree. That’s critically important,” he said.
“The other thing, and this is actually what I find most interesting about this study, is that fremanezumab doesn’t get into the brain. There are many antimigraine therapies that do, so you can treat a patient with migraine and depression with a tricyclic antidepressant.”
“It may make the migraine better and the depression better, but you don’t know if the benefit in depression comes from the improvement in migraine, because of course the antidepressant works for both conditions. Maybe there are people who would disagree with this, but my interpretation [of the trial results] is that the depression got better because the migraine got better,” he added.
The link between migraine and depression is well established, Dr. Lipton added. Longitudinal studies have shown that people with depression but without migraine develop migraine at increased rates, compared with people with no depression. Conversely, people with migraine but no depression develop depression at increased rates.
“Both disorders may have a common substrate, but I also think many forms of chronic pain lead to depression, and that’s the part we’re making better,” he said.
If fremanezumab has this dual effect on migraine and depression, it is possible that other anti-CGRP drugs will have a similar effect, Dr. Lipton said.
“Honestly, my hope is that other companies that make effective drugs will do similar studies to see if other monoclonal antibodies that target CGRP have the same effect. My guess is that all of them work but until the studies are done, I’m going to use fremanezumab, the one that has been studied, in my patients.”
He added that depression is an important comorbidity of migraine and represents a huge challenge for clinicians. “A lot of headache patients want to know what to do about comorbid anxiety or comorbid depression. I run a headache center in a specialty practice, and when people come in with migraine, they almost always come in with migraine and depression or anxiety or another pain disorder, or something else, and one of the great challenges in the practice is managing these comorbidities,” he said.
A bidirectional relationship
The overlap between migraine and depression and anxiety has been known for quite a while, agreed Elizabeth W. Loder, MD, MPH, vice chair of academic affairs, department of neurology, Brigham and Women’s Hospital, and professor of neurology at Harvard Medical School, both in Boston.
“I think the relationship is generally viewed as bidirectional and causality is uncertain. I still do not think I would assume that any drug that reduces migraine would reduce depression,” said Dr. Loder.
However, she added, the fremanezumab study data are interesting. “The effects of any drug on depression could be due to improvement of migraine or it could be due to some other effect of the treatment on depression. That is what makes these results so intriguing. If the findings are borne out by other studies, it could mean that these treatments would be preferred to those older ones in patients with depression,” Dr. Loder said.
Also commenting on the findings, Huma Sheikh, MD, CEO of NY Neurology Medicine PC, said the study is important because it confirms the strong association between migraine and depression. “Both conditions have similar underlying neurobiological pathophysiologies, and if you are impacting one area in the brain with the CGRP inhibitors, you might also be targeting some of the receptors or pathways that are involved in depression,” Dr. Sheikh said.
The study was funded by Teva Pharmaceuticals. Dr. Lipton reported financial relationships with Teva and multiple other pharmaceutical companies. Dr. Loder and Dr. Sheikh have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AUSTIN, TEX. – , new research shows.
Patients with both conditions who were randomly assigned to receive fremanezumab showed a statistically significant reduction in both the 17-item Hamilton Depression Rating Scale (HAMD-17) and the nine-criteria Patient Health Questionnaire (PHQ-9) scores, compared with matched controls who received placebo.
The results from the UNITE trial were presented at the annual meeting of the American Headache Society.
Long-standing questions
“It’s been well known for a long time that migraine is comorbid with a number of illnesses, and one of the most common is depression,” said study investigator Richard B. Lipton, a professor of neurology at Albert Einstein College of Medicine and the director of the Montefiore Headache Center, New York.
“Do you treat the depression? Do you treat the migraine? Do you independently treat both? Those have been long-standing questions for clinicians,” Dr. Lipton said.
Investigators randomly assigned 330 adults with migraine who were diagnosed with moderate-to-severe MDD (defined as a PHQ-9 score of 10 or greater) to receive 225 mg subcutaneous monthly fremanezumab (n = 164) or placebo (n = 166) for 12 weeks.
The trial continued as an open-label trial for another 12 weeks.
During the double-blind phase of the study, the mean change from baseline in the HAMD-17 score with placebo was –4.6 at week 8 and –5.4 at week 12, compared with –6.0 with fremanezumab at week 8 (P = .0205) and –6.7 at week 12 (P = .0228).
The change from baseline in PHQ-9 total score at week 8 was –5.8 for placebo and –7.1 for fremanezumab (P = .0283). At week 12, the change was –6.3 for placebo versus –7.8 for fremanezumab (P = .0108). These reductions were maintained throughout the open-label period of the trial.
The beneficial effect on depression and migraine demonstrated in the study is interesting on several levels, Dr. Lipton said.
“One, it tells us that if the patient has migraine and depression and you treat with fremanezumab, both disorders get better to a statistically significant degree. That’s critically important,” he said.
“The other thing, and this is actually what I find most interesting about this study, is that fremanezumab doesn’t get into the brain. There are many antimigraine therapies that do, so you can treat a patient with migraine and depression with a tricyclic antidepressant.”
“It may make the migraine better and the depression better, but you don’t know if the benefit in depression comes from the improvement in migraine, because of course the antidepressant works for both conditions. Maybe there are people who would disagree with this, but my interpretation [of the trial results] is that the depression got better because the migraine got better,” he added.
The link between migraine and depression is well established, Dr. Lipton added. Longitudinal studies have shown that people with depression but without migraine develop migraine at increased rates, compared with people with no depression. Conversely, people with migraine but no depression develop depression at increased rates.
“Both disorders may have a common substrate, but I also think many forms of chronic pain lead to depression, and that’s the part we’re making better,” he said.
If fremanezumab has this dual effect on migraine and depression, it is possible that other anti-CGRP drugs will have a similar effect, Dr. Lipton said.
“Honestly, my hope is that other companies that make effective drugs will do similar studies to see if other monoclonal antibodies that target CGRP have the same effect. My guess is that all of them work but until the studies are done, I’m going to use fremanezumab, the one that has been studied, in my patients.”
He added that depression is an important comorbidity of migraine and represents a huge challenge for clinicians. “A lot of headache patients want to know what to do about comorbid anxiety or comorbid depression. I run a headache center in a specialty practice, and when people come in with migraine, they almost always come in with migraine and depression or anxiety or another pain disorder, or something else, and one of the great challenges in the practice is managing these comorbidities,” he said.
A bidirectional relationship
The overlap between migraine and depression and anxiety has been known for quite a while, agreed Elizabeth W. Loder, MD, MPH, vice chair of academic affairs, department of neurology, Brigham and Women’s Hospital, and professor of neurology at Harvard Medical School, both in Boston.
“I think the relationship is generally viewed as bidirectional and causality is uncertain. I still do not think I would assume that any drug that reduces migraine would reduce depression,” said Dr. Loder.
However, she added, the fremanezumab study data are interesting. “The effects of any drug on depression could be due to improvement of migraine or it could be due to some other effect of the treatment on depression. That is what makes these results so intriguing. If the findings are borne out by other studies, it could mean that these treatments would be preferred to those older ones in patients with depression,” Dr. Loder said.
Also commenting on the findings, Huma Sheikh, MD, CEO of NY Neurology Medicine PC, said the study is important because it confirms the strong association between migraine and depression. “Both conditions have similar underlying neurobiological pathophysiologies, and if you are impacting one area in the brain with the CGRP inhibitors, you might also be targeting some of the receptors or pathways that are involved in depression,” Dr. Sheikh said.
The study was funded by Teva Pharmaceuticals. Dr. Lipton reported financial relationships with Teva and multiple other pharmaceutical companies. Dr. Loder and Dr. Sheikh have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AUSTIN, TEX. – , new research shows.
Patients with both conditions who were randomly assigned to receive fremanezumab showed a statistically significant reduction in both the 17-item Hamilton Depression Rating Scale (HAMD-17) and the nine-criteria Patient Health Questionnaire (PHQ-9) scores, compared with matched controls who received placebo.
The results from the UNITE trial were presented at the annual meeting of the American Headache Society.
Long-standing questions
“It’s been well known for a long time that migraine is comorbid with a number of illnesses, and one of the most common is depression,” said study investigator Richard B. Lipton, a professor of neurology at Albert Einstein College of Medicine and the director of the Montefiore Headache Center, New York.
“Do you treat the depression? Do you treat the migraine? Do you independently treat both? Those have been long-standing questions for clinicians,” Dr. Lipton said.
Investigators randomly assigned 330 adults with migraine who were diagnosed with moderate-to-severe MDD (defined as a PHQ-9 score of 10 or greater) to receive 225 mg subcutaneous monthly fremanezumab (n = 164) or placebo (n = 166) for 12 weeks.
The trial continued as an open-label trial for another 12 weeks.
During the double-blind phase of the study, the mean change from baseline in the HAMD-17 score with placebo was –4.6 at week 8 and –5.4 at week 12, compared with –6.0 with fremanezumab at week 8 (P = .0205) and –6.7 at week 12 (P = .0228).
The change from baseline in PHQ-9 total score at week 8 was –5.8 for placebo and –7.1 for fremanezumab (P = .0283). At week 12, the change was –6.3 for placebo versus –7.8 for fremanezumab (P = .0108). These reductions were maintained throughout the open-label period of the trial.
The beneficial effect on depression and migraine demonstrated in the study is interesting on several levels, Dr. Lipton said.
“One, it tells us that if the patient has migraine and depression and you treat with fremanezumab, both disorders get better to a statistically significant degree. That’s critically important,” he said.
“The other thing, and this is actually what I find most interesting about this study, is that fremanezumab doesn’t get into the brain. There are many antimigraine therapies that do, so you can treat a patient with migraine and depression with a tricyclic antidepressant.”
“It may make the migraine better and the depression better, but you don’t know if the benefit in depression comes from the improvement in migraine, because of course the antidepressant works for both conditions. Maybe there are people who would disagree with this, but my interpretation [of the trial results] is that the depression got better because the migraine got better,” he added.
The link between migraine and depression is well established, Dr. Lipton added. Longitudinal studies have shown that people with depression but without migraine develop migraine at increased rates, compared with people with no depression. Conversely, people with migraine but no depression develop depression at increased rates.
“Both disorders may have a common substrate, but I also think many forms of chronic pain lead to depression, and that’s the part we’re making better,” he said.
If fremanezumab has this dual effect on migraine and depression, it is possible that other anti-CGRP drugs will have a similar effect, Dr. Lipton said.
“Honestly, my hope is that other companies that make effective drugs will do similar studies to see if other monoclonal antibodies that target CGRP have the same effect. My guess is that all of them work but until the studies are done, I’m going to use fremanezumab, the one that has been studied, in my patients.”
He added that depression is an important comorbidity of migraine and represents a huge challenge for clinicians. “A lot of headache patients want to know what to do about comorbid anxiety or comorbid depression. I run a headache center in a specialty practice, and when people come in with migraine, they almost always come in with migraine and depression or anxiety or another pain disorder, or something else, and one of the great challenges in the practice is managing these comorbidities,” he said.
A bidirectional relationship
The overlap between migraine and depression and anxiety has been known for quite a while, agreed Elizabeth W. Loder, MD, MPH, vice chair of academic affairs, department of neurology, Brigham and Women’s Hospital, and professor of neurology at Harvard Medical School, both in Boston.
“I think the relationship is generally viewed as bidirectional and causality is uncertain. I still do not think I would assume that any drug that reduces migraine would reduce depression,” said Dr. Loder.
However, she added, the fremanezumab study data are interesting. “The effects of any drug on depression could be due to improvement of migraine or it could be due to some other effect of the treatment on depression. That is what makes these results so intriguing. If the findings are borne out by other studies, it could mean that these treatments would be preferred to those older ones in patients with depression,” Dr. Loder said.
Also commenting on the findings, Huma Sheikh, MD, CEO of NY Neurology Medicine PC, said the study is important because it confirms the strong association between migraine and depression. “Both conditions have similar underlying neurobiological pathophysiologies, and if you are impacting one area in the brain with the CGRP inhibitors, you might also be targeting some of the receptors or pathways that are involved in depression,” Dr. Sheikh said.
The study was funded by Teva Pharmaceuticals. Dr. Lipton reported financial relationships with Teva and multiple other pharmaceutical companies. Dr. Loder and Dr. Sheikh have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AT AHS 2023
Physician suicide roundtable: 8 important initiatives that can help
Physician suicide continues to be a challenging problem in the United States. Each year, 1 in 10 doctors think about or attempt suicide, and 400 die by suicide each year. More than half of the doctors reading this know a colleague who has attempted or died by suicide.
These are part of a public health suicide prevention strategy, the preferred method for prevention, in hospitals and institutions around the country. A public health model for preventing suicide is a multifaceted approach that includes universal education, health promotion, selective and targeted prevention, and treatment and recovery.
These physicians hope to continue creating and implementing these and other risk-reduction measures across all health care organizations.
Our physician experts for this discussion
Mary Moffit, PhD, is an associate professor in the department of psychiatry at Oregon Health & Science University, Portland. She directs the resident and faculty wellness program and is director of the OHSU peer support program. She helped design and developed a comprehensive wellness program that is now a national model for academic medical centers.
Christine Yu Moutier, MD, is the chief medical officer of the American Foundation for Suicide Prevention. She is the author of “Suicide Prevention,” a Cambridge University Press clinical handbook. She has been a practicing psychiatrist, professor of psychiatry, dean in the medical school at the University of California, San Diego, and medical director of the inpatient psychiatric unit at the VA Medical Center in La Jolla, Calif.
Michael F. Myers, MD, is a professor of clinical psychiatry in the department of psychiatry & behavioral sciences at the State University of New York, Brooklyn. He is recent past vice-chair of education and director of training in the department of psychiatry & behavioral sciences at the university. He is the author of several books, including “Why Physicians Die By Suicide,” “The Physician as Patient,” and “Touched by Suicide.”
The participants discussed these risk-reduction initiatives as having much potential for helping physicians at risk for suicide and suicidal ideations.
The importance of peer support programs
Peer support program models may differ across institutions but typically describe colleagues providing some degree of emotional first aid to peers who may be at risk.
Dr. Moffit: The Pew support program that we have in place at OHSU, similar to what’s available in many hospitals and systems nationwide, trains individual physicians across multiple specialties in a peer support model. It’s not specifically emotional first aid, although that’s integral to it. It’s also for adverse events: Having a tragic patient death, having learned that you will be named in a lawsuit, and exposure to trauma in the medical role.
Peer to peer is not where we anticipate physicians seeking someone to talk to about their marital relationship not going well. However, the peer supporter will know about resources throughout the university and the community for what is needed. We’ve got 20-30 peer supporters. We try to match them – for example, a surgeon with a surgeon, a primary care doc with a primary care doc. Physicians who use peer support aren’t tracked, and no notes are taken or documented. It takes place informally but has changed the culture and lowered a barrier. We have a waiting list of people who want to be peer supporters.
Dr. Moutier: Peer-to-peer support is usually part of a multi-pronged program and is usually not the only effort going on. Depending on how they’re set up, the goals may be slightly different for each program. Peer-to-peer can be one of the most powerful ways to augment awareness raising and education, which is almost always a basic first step.
Dr. Myers: It doesn’t feel as threatening when people start in a peer-to-peer support group. Users may have been afraid of getting a mental health diagnosis, but with peers, many of whom are often not psychiatrists, that eases distress. Peer support can break down that sense of isolation and loneliness so that someone can take the next step.
Dr. Moutier: To be connected to family, to any community resource, frankly, is a protective factor that mitigates suicide risk. So that’s the logic model from a suicide prevention standpoint. It may be the only opportunity for someone to start disclosing what they’re experiencing, receive validation and support, and not a judgmental response. It can open up the avenue toward help-seeking.
Opt-in/opt-out support for medical residents
This initiative matches residents with a counselor as part of their orientation.
Dr. Moffit: Each resident has a meet and greet with a counselor when they arrive or in their first 6 months at their university. The resident can opt out and cancel the meeting, but they’re scheduled for it as part of their “curriculum.” Institutions like Michigan, Columbia, Montefiore, Mount Sinai, and the University of California, San Diego, have this in place. It starts something like: ‘Hello. Good afternoon. How’s it going? I’m Dr. Moffitt, and here are the services available in this program.’
Dr. Myers: It’s another excellent example of normalizing the stress in the rigors of training and making it part of the wellness initiative.
Dr. Moutier: It’s just a normal part of orientation. Again, as a universal strategy, one thing that I was doing at UCSD with a particular group of medical students, who were at higher risk, was a postbaccalaureate program that found students from underrepresented, under-resourced backgrounds and brought them into this post-bacc year. I was directing it and mentoring these students.
So, I could afford a lot more intensive time and attention to them because it was a small group, but every one of them had regular meetings with me every 2 weeks. My approach was to help them uncover their unique strengths and vulnerabilities as they started this program. They all made it into med school.
It was a very intensive and more concierge-personalized approach. It’s like personalized medicine. What specific self-care, mentoring, and mental health care plan would each student codesign with me to stay on track?
And it would involve very holistic things, like if part of their vulnerability was that leaving their Chicano family was creating stress because their father had said: ‘You’re leaving our culture and our family by going into the profession of medicine,’ then we had specific plans around how to care for that aspect of their struggle. It was a much more informed, customized mentoring approach called the UCSD CAP (Conditional Acceptance Post-Baccalaureate Program). It could be a feature in a more specialized opt-in/opt-out program.
One-question survey: How full is your gas tank?
This initiative is a one-question survey emailed/texted to residents to check in on their wellness. We ask, how full is your gas tank? Select 1 to 5 (Empty to Full). If they flag low, they receive a follow-up.
Dr. Moffit: It’s certainly a metaphor that we use. It’s the idea of being depleted in combination with being extremely sleep deprived and the inability to access the usual sources of support or outlets, and how that can create a perfect storm of a level of distress that can put physicians at risk.
Dr. Moutier: It is a way to help people realize that there are things they can do proactively to keep that tank at least somewhat full enough.
Dr. Myers: Using colloquial or figurative language can get better buy-in than “Here’s a PHQ-9.” It also has a caring or intimate tone to it. Somebody could feel they’re a 1 in this rotation but a 4-5 the next. We know from a lot of the literature that when residents get a good, welcoming orientation, their satisfaction with that rotation is uniformly better than if they’re thrown to the wolves. And we know trial by fire can put trainees at risk.
A buddy to check in with
This initiative is when you’re assigned a buddy in or out of residency that you regularly check in with about how you’re doing.
Dr. Myers: Not to be cynical, but there has been some mentor/mentee research that if you’re assigned a mentor, the results are not nearly as good. And if it’s left to the individual to find a mentor, results could be marginal as well. You need a guide to say, ‘Here are some potential mentors for you, but you decide.’ We do a lot of that at (SUNY) Downstate instead of assigning a person. So, it may require some oversight. Picking a check-in buddy from a list provided rather than having one assigned may be more beneficial.
A lot of what we’re talking about are universal strategies that allow for increased interpersonal connection, which is a protective factor that normalizes help-seeking.
A platform or social media forum to share experiences
An online forum or platform where medical students, residents, and physicians can discuss mental health and suicide prevention. Physicians with personal experience could provide testimonials.
Dr. Myers: I’ve recently signed a book contract, and the working title is “Physicians With Lived Experience: How Their Stories Give Clinical Guidance.” When I talk with doctors who have published their personal stories in the New England Journal of Medicine, JAMA, or sometimes The Washington Post or The New York Times, many of them have said they had no idea at the beginning of their journey that they would do something like this: be transparent about their story. It’s a measure of their health, growth, and grace.
Dr. Moutier: The current president of the Academic Association of Surgeons, Carrie Cunningham, MD, MPH, used her platform at the annual AAS conference in 2022 to focus on suicide prevention. She told her own recent story of having gotten into recovery after having been near suicide and struggling with addiction. It was a groundbreaking moment for the field of surgery and produced a ripple effect. She risked everything to tell her story, which was highly emotional since it was still raw. It got everyone engaged, a real turning point for that field. Storytelling and a place for trainees to discuss suicide prevention, and physicians to recall their lived experiences can be highly beneficial.
Interactive Screening Program
The Interactive Screening Program (ISP) is used in higher education to allow physicians to take a safe, confidential screening test and receive a personalized response that can connect them to mental health services before a crisis emerges.
Dr. Moutier: ISP is a tool within a public health model that can afford anonymity to the user so they can safely have their needs addressed. It’s a way for high-risk individuals to sync up with treatment and support. It’s sometimes used in the universal approach because it can be offered to everyone within the health system community of physicians and staff.
It can produce a ripple effect of normalizing that we all have mental health to take care of. Its intended value is in identifying those with a higher risk for suicide, but it doesn’t stop at identifying those at risk. It helps physicians move past a stage of suffering in silence.
Our data show that 86% of a very high-risk group (currently having suicidal ideation, a recent attempt, or other high-risk factors for suicide) aren’t in any form of treatment and have not disclosed their situation to anyone. A fairly high percentage of those going through ISP request a referral to treatment. It’s a unique, very niche tool, and because users remain anonymous, that affords safety around confidentiality.
It’s usually part of a multipronged approach with education, stigma reduction, storytelling, peer support, and other modalities. In my experience with the UCSD HEAR (Healer Assessment Education and Recovery) program, which is still going strong in about its 15th year, the program went from seeing 13 physicians die by suicide in the years leading up to its launch and in the 15 years since it’s been going, one suicide. We all believe that the ISP is the heart of prevention.
Even though all of the universal strategies are important, they probably wouldn’t be sufficient by themselves because the risk [for suicide] is dynamic, and you have to catch people when they are suffering and ready to seek treatment. Suicide prevention is challenging and must be strategic, multifaceted, and sustained over time.
The importance of confidentiality for physicians
In the past, physicians may have been hesitant to seek treatment when struggling with mental health, substance use disorder and suicidal ideations because they heard stories from doctors who said they had to disclose mental health treatment to medical and state licensing boards.
Dr. Myers: There is so much dated stuff out there, and it gets propagated by people who have had a bad experience. I’m not challenging the authenticity of that, but I feel like those are in the minority. The vast majority of people are seeking help. The Federation of State Physician Health Programs is working with state boards to update and get rid of antiquated questions, and they’re working with credentialing groups.
When I was in practice and my patient was petrified of having to come into the hospital [because of confidentiality] I would just be their physician and say: “Look, I know that this is a worry for you [licensing and credentialing issues] but trust me, I’m going to help you get well; that’s my job. And I’m going to help you sort all that out afterward.” It was part of my work as their physician that if they were going to have to jump through hurdles to get their license reinstated, etc., I could help.
The Dr. Lorna Breen Heroes’ Foundation is also doing so much good work in this area, especially with their toolkits to audit, change, remove, and communicate the changes about intrusive language in licensing applications and credentialing. (Dr. Breen was a New York City ED physician who died by suicide in April 2020 during the early days and height of the COVID-19 pandemic. Her father was quoted as saying: “She was in the trenches. She was a hero.”)
Dr. Moutier: We’re seeing hundreds of physicians get therapy and psychiatric treatment annually. And the advocacy effort is incredibly important, and I think we are witnessing a swifter pace to eliminate those inappropriate and illegal questions about mental health and mental health treatment for physicians and nurses.
Dr. Moffit: We have lowered barriers, not only in individual institutions but also with programming. We have also worked with the Federation of State Medical Boards and The Lorna Breen Foundation to change the legislation. The Foundation has audited and changed 20 state medical boards to remove intrusive language from licensing applications.
Support for colleagues working to help each other
Dr. Myers: One final note for those physicians who need to take time out for medical leave: In my clinical experience, I find that they felt lonely as they were getting well. I can’t tell you how much it made a difference for those who received a phone call, a card, or an email from their colleagues at work. It doesn’t take long for a vibrant, active physician to feel out of the loop when ill.
We know from suicide literature that when somebody’s discharged from the hospital or the emergency department, caring communications, brief expressions of care and concern by email, letter, card, text message, etc., can make all the difference to their recovery. Reaching out to those struggling and those in recovery can help your fellow physician.
A version of this article originally appeared on Medscape.com.
Physician suicide continues to be a challenging problem in the United States. Each year, 1 in 10 doctors think about or attempt suicide, and 400 die by suicide each year. More than half of the doctors reading this know a colleague who has attempted or died by suicide.
These are part of a public health suicide prevention strategy, the preferred method for prevention, in hospitals and institutions around the country. A public health model for preventing suicide is a multifaceted approach that includes universal education, health promotion, selective and targeted prevention, and treatment and recovery.
These physicians hope to continue creating and implementing these and other risk-reduction measures across all health care organizations.
Our physician experts for this discussion
Mary Moffit, PhD, is an associate professor in the department of psychiatry at Oregon Health & Science University, Portland. She directs the resident and faculty wellness program and is director of the OHSU peer support program. She helped design and developed a comprehensive wellness program that is now a national model for academic medical centers.
Christine Yu Moutier, MD, is the chief medical officer of the American Foundation for Suicide Prevention. She is the author of “Suicide Prevention,” a Cambridge University Press clinical handbook. She has been a practicing psychiatrist, professor of psychiatry, dean in the medical school at the University of California, San Diego, and medical director of the inpatient psychiatric unit at the VA Medical Center in La Jolla, Calif.
Michael F. Myers, MD, is a professor of clinical psychiatry in the department of psychiatry & behavioral sciences at the State University of New York, Brooklyn. He is recent past vice-chair of education and director of training in the department of psychiatry & behavioral sciences at the university. He is the author of several books, including “Why Physicians Die By Suicide,” “The Physician as Patient,” and “Touched by Suicide.”
The participants discussed these risk-reduction initiatives as having much potential for helping physicians at risk for suicide and suicidal ideations.
The importance of peer support programs
Peer support program models may differ across institutions but typically describe colleagues providing some degree of emotional first aid to peers who may be at risk.
Dr. Moffit: The Pew support program that we have in place at OHSU, similar to what’s available in many hospitals and systems nationwide, trains individual physicians across multiple specialties in a peer support model. It’s not specifically emotional first aid, although that’s integral to it. It’s also for adverse events: Having a tragic patient death, having learned that you will be named in a lawsuit, and exposure to trauma in the medical role.
Peer to peer is not where we anticipate physicians seeking someone to talk to about their marital relationship not going well. However, the peer supporter will know about resources throughout the university and the community for what is needed. We’ve got 20-30 peer supporters. We try to match them – for example, a surgeon with a surgeon, a primary care doc with a primary care doc. Physicians who use peer support aren’t tracked, and no notes are taken or documented. It takes place informally but has changed the culture and lowered a barrier. We have a waiting list of people who want to be peer supporters.
Dr. Moutier: Peer-to-peer support is usually part of a multi-pronged program and is usually not the only effort going on. Depending on how they’re set up, the goals may be slightly different for each program. Peer-to-peer can be one of the most powerful ways to augment awareness raising and education, which is almost always a basic first step.
Dr. Myers: It doesn’t feel as threatening when people start in a peer-to-peer support group. Users may have been afraid of getting a mental health diagnosis, but with peers, many of whom are often not psychiatrists, that eases distress. Peer support can break down that sense of isolation and loneliness so that someone can take the next step.
Dr. Moutier: To be connected to family, to any community resource, frankly, is a protective factor that mitigates suicide risk. So that’s the logic model from a suicide prevention standpoint. It may be the only opportunity for someone to start disclosing what they’re experiencing, receive validation and support, and not a judgmental response. It can open up the avenue toward help-seeking.
Opt-in/opt-out support for medical residents
This initiative matches residents with a counselor as part of their orientation.
Dr. Moffit: Each resident has a meet and greet with a counselor when they arrive or in their first 6 months at their university. The resident can opt out and cancel the meeting, but they’re scheduled for it as part of their “curriculum.” Institutions like Michigan, Columbia, Montefiore, Mount Sinai, and the University of California, San Diego, have this in place. It starts something like: ‘Hello. Good afternoon. How’s it going? I’m Dr. Moffitt, and here are the services available in this program.’
Dr. Myers: It’s another excellent example of normalizing the stress in the rigors of training and making it part of the wellness initiative.
Dr. Moutier: It’s just a normal part of orientation. Again, as a universal strategy, one thing that I was doing at UCSD with a particular group of medical students, who were at higher risk, was a postbaccalaureate program that found students from underrepresented, under-resourced backgrounds and brought them into this post-bacc year. I was directing it and mentoring these students.
So, I could afford a lot more intensive time and attention to them because it was a small group, but every one of them had regular meetings with me every 2 weeks. My approach was to help them uncover their unique strengths and vulnerabilities as they started this program. They all made it into med school.
It was a very intensive and more concierge-personalized approach. It’s like personalized medicine. What specific self-care, mentoring, and mental health care plan would each student codesign with me to stay on track?
And it would involve very holistic things, like if part of their vulnerability was that leaving their Chicano family was creating stress because their father had said: ‘You’re leaving our culture and our family by going into the profession of medicine,’ then we had specific plans around how to care for that aspect of their struggle. It was a much more informed, customized mentoring approach called the UCSD CAP (Conditional Acceptance Post-Baccalaureate Program). It could be a feature in a more specialized opt-in/opt-out program.
One-question survey: How full is your gas tank?
This initiative is a one-question survey emailed/texted to residents to check in on their wellness. We ask, how full is your gas tank? Select 1 to 5 (Empty to Full). If they flag low, they receive a follow-up.
Dr. Moffit: It’s certainly a metaphor that we use. It’s the idea of being depleted in combination with being extremely sleep deprived and the inability to access the usual sources of support or outlets, and how that can create a perfect storm of a level of distress that can put physicians at risk.
Dr. Moutier: It is a way to help people realize that there are things they can do proactively to keep that tank at least somewhat full enough.
Dr. Myers: Using colloquial or figurative language can get better buy-in than “Here’s a PHQ-9.” It also has a caring or intimate tone to it. Somebody could feel they’re a 1 in this rotation but a 4-5 the next. We know from a lot of the literature that when residents get a good, welcoming orientation, their satisfaction with that rotation is uniformly better than if they’re thrown to the wolves. And we know trial by fire can put trainees at risk.
A buddy to check in with
This initiative is when you’re assigned a buddy in or out of residency that you regularly check in with about how you’re doing.
Dr. Myers: Not to be cynical, but there has been some mentor/mentee research that if you’re assigned a mentor, the results are not nearly as good. And if it’s left to the individual to find a mentor, results could be marginal as well. You need a guide to say, ‘Here are some potential mentors for you, but you decide.’ We do a lot of that at (SUNY) Downstate instead of assigning a person. So, it may require some oversight. Picking a check-in buddy from a list provided rather than having one assigned may be more beneficial.
A lot of what we’re talking about are universal strategies that allow for increased interpersonal connection, which is a protective factor that normalizes help-seeking.
A platform or social media forum to share experiences
An online forum or platform where medical students, residents, and physicians can discuss mental health and suicide prevention. Physicians with personal experience could provide testimonials.
Dr. Myers: I’ve recently signed a book contract, and the working title is “Physicians With Lived Experience: How Their Stories Give Clinical Guidance.” When I talk with doctors who have published their personal stories in the New England Journal of Medicine, JAMA, or sometimes The Washington Post or The New York Times, many of them have said they had no idea at the beginning of their journey that they would do something like this: be transparent about their story. It’s a measure of their health, growth, and grace.
Dr. Moutier: The current president of the Academic Association of Surgeons, Carrie Cunningham, MD, MPH, used her platform at the annual AAS conference in 2022 to focus on suicide prevention. She told her own recent story of having gotten into recovery after having been near suicide and struggling with addiction. It was a groundbreaking moment for the field of surgery and produced a ripple effect. She risked everything to tell her story, which was highly emotional since it was still raw. It got everyone engaged, a real turning point for that field. Storytelling and a place for trainees to discuss suicide prevention, and physicians to recall their lived experiences can be highly beneficial.
Interactive Screening Program
The Interactive Screening Program (ISP) is used in higher education to allow physicians to take a safe, confidential screening test and receive a personalized response that can connect them to mental health services before a crisis emerges.
Dr. Moutier: ISP is a tool within a public health model that can afford anonymity to the user so they can safely have their needs addressed. It’s a way for high-risk individuals to sync up with treatment and support. It’s sometimes used in the universal approach because it can be offered to everyone within the health system community of physicians and staff.
It can produce a ripple effect of normalizing that we all have mental health to take care of. Its intended value is in identifying those with a higher risk for suicide, but it doesn’t stop at identifying those at risk. It helps physicians move past a stage of suffering in silence.
Our data show that 86% of a very high-risk group (currently having suicidal ideation, a recent attempt, or other high-risk factors for suicide) aren’t in any form of treatment and have not disclosed their situation to anyone. A fairly high percentage of those going through ISP request a referral to treatment. It’s a unique, very niche tool, and because users remain anonymous, that affords safety around confidentiality.
It’s usually part of a multipronged approach with education, stigma reduction, storytelling, peer support, and other modalities. In my experience with the UCSD HEAR (Healer Assessment Education and Recovery) program, which is still going strong in about its 15th year, the program went from seeing 13 physicians die by suicide in the years leading up to its launch and in the 15 years since it’s been going, one suicide. We all believe that the ISP is the heart of prevention.
Even though all of the universal strategies are important, they probably wouldn’t be sufficient by themselves because the risk [for suicide] is dynamic, and you have to catch people when they are suffering and ready to seek treatment. Suicide prevention is challenging and must be strategic, multifaceted, and sustained over time.
The importance of confidentiality for physicians
In the past, physicians may have been hesitant to seek treatment when struggling with mental health, substance use disorder and suicidal ideations because they heard stories from doctors who said they had to disclose mental health treatment to medical and state licensing boards.
Dr. Myers: There is so much dated stuff out there, and it gets propagated by people who have had a bad experience. I’m not challenging the authenticity of that, but I feel like those are in the minority. The vast majority of people are seeking help. The Federation of State Physician Health Programs is working with state boards to update and get rid of antiquated questions, and they’re working with credentialing groups.
When I was in practice and my patient was petrified of having to come into the hospital [because of confidentiality] I would just be their physician and say: “Look, I know that this is a worry for you [licensing and credentialing issues] but trust me, I’m going to help you get well; that’s my job. And I’m going to help you sort all that out afterward.” It was part of my work as their physician that if they were going to have to jump through hurdles to get their license reinstated, etc., I could help.
The Dr. Lorna Breen Heroes’ Foundation is also doing so much good work in this area, especially with their toolkits to audit, change, remove, and communicate the changes about intrusive language in licensing applications and credentialing. (Dr. Breen was a New York City ED physician who died by suicide in April 2020 during the early days and height of the COVID-19 pandemic. Her father was quoted as saying: “She was in the trenches. She was a hero.”)
Dr. Moutier: We’re seeing hundreds of physicians get therapy and psychiatric treatment annually. And the advocacy effort is incredibly important, and I think we are witnessing a swifter pace to eliminate those inappropriate and illegal questions about mental health and mental health treatment for physicians and nurses.
Dr. Moffit: We have lowered barriers, not only in individual institutions but also with programming. We have also worked with the Federation of State Medical Boards and The Lorna Breen Foundation to change the legislation. The Foundation has audited and changed 20 state medical boards to remove intrusive language from licensing applications.
Support for colleagues working to help each other
Dr. Myers: One final note for those physicians who need to take time out for medical leave: In my clinical experience, I find that they felt lonely as they were getting well. I can’t tell you how much it made a difference for those who received a phone call, a card, or an email from their colleagues at work. It doesn’t take long for a vibrant, active physician to feel out of the loop when ill.
We know from suicide literature that when somebody’s discharged from the hospital or the emergency department, caring communications, brief expressions of care and concern by email, letter, card, text message, etc., can make all the difference to their recovery. Reaching out to those struggling and those in recovery can help your fellow physician.
A version of this article originally appeared on Medscape.com.
Physician suicide continues to be a challenging problem in the United States. Each year, 1 in 10 doctors think about or attempt suicide, and 400 die by suicide each year. More than half of the doctors reading this know a colleague who has attempted or died by suicide.
These are part of a public health suicide prevention strategy, the preferred method for prevention, in hospitals and institutions around the country. A public health model for preventing suicide is a multifaceted approach that includes universal education, health promotion, selective and targeted prevention, and treatment and recovery.
These physicians hope to continue creating and implementing these and other risk-reduction measures across all health care organizations.
Our physician experts for this discussion
Mary Moffit, PhD, is an associate professor in the department of psychiatry at Oregon Health & Science University, Portland. She directs the resident and faculty wellness program and is director of the OHSU peer support program. She helped design and developed a comprehensive wellness program that is now a national model for academic medical centers.
Christine Yu Moutier, MD, is the chief medical officer of the American Foundation for Suicide Prevention. She is the author of “Suicide Prevention,” a Cambridge University Press clinical handbook. She has been a practicing psychiatrist, professor of psychiatry, dean in the medical school at the University of California, San Diego, and medical director of the inpatient psychiatric unit at the VA Medical Center in La Jolla, Calif.
Michael F. Myers, MD, is a professor of clinical psychiatry in the department of psychiatry & behavioral sciences at the State University of New York, Brooklyn. He is recent past vice-chair of education and director of training in the department of psychiatry & behavioral sciences at the university. He is the author of several books, including “Why Physicians Die By Suicide,” “The Physician as Patient,” and “Touched by Suicide.”
The participants discussed these risk-reduction initiatives as having much potential for helping physicians at risk for suicide and suicidal ideations.
The importance of peer support programs
Peer support program models may differ across institutions but typically describe colleagues providing some degree of emotional first aid to peers who may be at risk.
Dr. Moffit: The Pew support program that we have in place at OHSU, similar to what’s available in many hospitals and systems nationwide, trains individual physicians across multiple specialties in a peer support model. It’s not specifically emotional first aid, although that’s integral to it. It’s also for adverse events: Having a tragic patient death, having learned that you will be named in a lawsuit, and exposure to trauma in the medical role.
Peer to peer is not where we anticipate physicians seeking someone to talk to about their marital relationship not going well. However, the peer supporter will know about resources throughout the university and the community for what is needed. We’ve got 20-30 peer supporters. We try to match them – for example, a surgeon with a surgeon, a primary care doc with a primary care doc. Physicians who use peer support aren’t tracked, and no notes are taken or documented. It takes place informally but has changed the culture and lowered a barrier. We have a waiting list of people who want to be peer supporters.
Dr. Moutier: Peer-to-peer support is usually part of a multi-pronged program and is usually not the only effort going on. Depending on how they’re set up, the goals may be slightly different for each program. Peer-to-peer can be one of the most powerful ways to augment awareness raising and education, which is almost always a basic first step.
Dr. Myers: It doesn’t feel as threatening when people start in a peer-to-peer support group. Users may have been afraid of getting a mental health diagnosis, but with peers, many of whom are often not psychiatrists, that eases distress. Peer support can break down that sense of isolation and loneliness so that someone can take the next step.
Dr. Moutier: To be connected to family, to any community resource, frankly, is a protective factor that mitigates suicide risk. So that’s the logic model from a suicide prevention standpoint. It may be the only opportunity for someone to start disclosing what they’re experiencing, receive validation and support, and not a judgmental response. It can open up the avenue toward help-seeking.
Opt-in/opt-out support for medical residents
This initiative matches residents with a counselor as part of their orientation.
Dr. Moffit: Each resident has a meet and greet with a counselor when they arrive or in their first 6 months at their university. The resident can opt out and cancel the meeting, but they’re scheduled for it as part of their “curriculum.” Institutions like Michigan, Columbia, Montefiore, Mount Sinai, and the University of California, San Diego, have this in place. It starts something like: ‘Hello. Good afternoon. How’s it going? I’m Dr. Moffitt, and here are the services available in this program.’
Dr. Myers: It’s another excellent example of normalizing the stress in the rigors of training and making it part of the wellness initiative.
Dr. Moutier: It’s just a normal part of orientation. Again, as a universal strategy, one thing that I was doing at UCSD with a particular group of medical students, who were at higher risk, was a postbaccalaureate program that found students from underrepresented, under-resourced backgrounds and brought them into this post-bacc year. I was directing it and mentoring these students.
So, I could afford a lot more intensive time and attention to them because it was a small group, but every one of them had regular meetings with me every 2 weeks. My approach was to help them uncover their unique strengths and vulnerabilities as they started this program. They all made it into med school.
It was a very intensive and more concierge-personalized approach. It’s like personalized medicine. What specific self-care, mentoring, and mental health care plan would each student codesign with me to stay on track?
And it would involve very holistic things, like if part of their vulnerability was that leaving their Chicano family was creating stress because their father had said: ‘You’re leaving our culture and our family by going into the profession of medicine,’ then we had specific plans around how to care for that aspect of their struggle. It was a much more informed, customized mentoring approach called the UCSD CAP (Conditional Acceptance Post-Baccalaureate Program). It could be a feature in a more specialized opt-in/opt-out program.
One-question survey: How full is your gas tank?
This initiative is a one-question survey emailed/texted to residents to check in on their wellness. We ask, how full is your gas tank? Select 1 to 5 (Empty to Full). If they flag low, they receive a follow-up.
Dr. Moffit: It’s certainly a metaphor that we use. It’s the idea of being depleted in combination with being extremely sleep deprived and the inability to access the usual sources of support or outlets, and how that can create a perfect storm of a level of distress that can put physicians at risk.
Dr. Moutier: It is a way to help people realize that there are things they can do proactively to keep that tank at least somewhat full enough.
Dr. Myers: Using colloquial or figurative language can get better buy-in than “Here’s a PHQ-9.” It also has a caring or intimate tone to it. Somebody could feel they’re a 1 in this rotation but a 4-5 the next. We know from a lot of the literature that when residents get a good, welcoming orientation, their satisfaction with that rotation is uniformly better than if they’re thrown to the wolves. And we know trial by fire can put trainees at risk.
A buddy to check in with
This initiative is when you’re assigned a buddy in or out of residency that you regularly check in with about how you’re doing.
Dr. Myers: Not to be cynical, but there has been some mentor/mentee research that if you’re assigned a mentor, the results are not nearly as good. And if it’s left to the individual to find a mentor, results could be marginal as well. You need a guide to say, ‘Here are some potential mentors for you, but you decide.’ We do a lot of that at (SUNY) Downstate instead of assigning a person. So, it may require some oversight. Picking a check-in buddy from a list provided rather than having one assigned may be more beneficial.
A lot of what we’re talking about are universal strategies that allow for increased interpersonal connection, which is a protective factor that normalizes help-seeking.
A platform or social media forum to share experiences
An online forum or platform where medical students, residents, and physicians can discuss mental health and suicide prevention. Physicians with personal experience could provide testimonials.
Dr. Myers: I’ve recently signed a book contract, and the working title is “Physicians With Lived Experience: How Their Stories Give Clinical Guidance.” When I talk with doctors who have published their personal stories in the New England Journal of Medicine, JAMA, or sometimes The Washington Post or The New York Times, many of them have said they had no idea at the beginning of their journey that they would do something like this: be transparent about their story. It’s a measure of their health, growth, and grace.
Dr. Moutier: The current president of the Academic Association of Surgeons, Carrie Cunningham, MD, MPH, used her platform at the annual AAS conference in 2022 to focus on suicide prevention. She told her own recent story of having gotten into recovery after having been near suicide and struggling with addiction. It was a groundbreaking moment for the field of surgery and produced a ripple effect. She risked everything to tell her story, which was highly emotional since it was still raw. It got everyone engaged, a real turning point for that field. Storytelling and a place for trainees to discuss suicide prevention, and physicians to recall their lived experiences can be highly beneficial.
Interactive Screening Program
The Interactive Screening Program (ISP) is used in higher education to allow physicians to take a safe, confidential screening test and receive a personalized response that can connect them to mental health services before a crisis emerges.
Dr. Moutier: ISP is a tool within a public health model that can afford anonymity to the user so they can safely have their needs addressed. It’s a way for high-risk individuals to sync up with treatment and support. It’s sometimes used in the universal approach because it can be offered to everyone within the health system community of physicians and staff.
It can produce a ripple effect of normalizing that we all have mental health to take care of. Its intended value is in identifying those with a higher risk for suicide, but it doesn’t stop at identifying those at risk. It helps physicians move past a stage of suffering in silence.
Our data show that 86% of a very high-risk group (currently having suicidal ideation, a recent attempt, or other high-risk factors for suicide) aren’t in any form of treatment and have not disclosed their situation to anyone. A fairly high percentage of those going through ISP request a referral to treatment. It’s a unique, very niche tool, and because users remain anonymous, that affords safety around confidentiality.
It’s usually part of a multipronged approach with education, stigma reduction, storytelling, peer support, and other modalities. In my experience with the UCSD HEAR (Healer Assessment Education and Recovery) program, which is still going strong in about its 15th year, the program went from seeing 13 physicians die by suicide in the years leading up to its launch and in the 15 years since it’s been going, one suicide. We all believe that the ISP is the heart of prevention.
Even though all of the universal strategies are important, they probably wouldn’t be sufficient by themselves because the risk [for suicide] is dynamic, and you have to catch people when they are suffering and ready to seek treatment. Suicide prevention is challenging and must be strategic, multifaceted, and sustained over time.
The importance of confidentiality for physicians
In the past, physicians may have been hesitant to seek treatment when struggling with mental health, substance use disorder and suicidal ideations because they heard stories from doctors who said they had to disclose mental health treatment to medical and state licensing boards.
Dr. Myers: There is so much dated stuff out there, and it gets propagated by people who have had a bad experience. I’m not challenging the authenticity of that, but I feel like those are in the minority. The vast majority of people are seeking help. The Federation of State Physician Health Programs is working with state boards to update and get rid of antiquated questions, and they’re working with credentialing groups.
When I was in practice and my patient was petrified of having to come into the hospital [because of confidentiality] I would just be their physician and say: “Look, I know that this is a worry for you [licensing and credentialing issues] but trust me, I’m going to help you get well; that’s my job. And I’m going to help you sort all that out afterward.” It was part of my work as their physician that if they were going to have to jump through hurdles to get their license reinstated, etc., I could help.
The Dr. Lorna Breen Heroes’ Foundation is also doing so much good work in this area, especially with their toolkits to audit, change, remove, and communicate the changes about intrusive language in licensing applications and credentialing. (Dr. Breen was a New York City ED physician who died by suicide in April 2020 during the early days and height of the COVID-19 pandemic. Her father was quoted as saying: “She was in the trenches. She was a hero.”)
Dr. Moutier: We’re seeing hundreds of physicians get therapy and psychiatric treatment annually. And the advocacy effort is incredibly important, and I think we are witnessing a swifter pace to eliminate those inappropriate and illegal questions about mental health and mental health treatment for physicians and nurses.
Dr. Moffit: We have lowered barriers, not only in individual institutions but also with programming. We have also worked with the Federation of State Medical Boards and The Lorna Breen Foundation to change the legislation. The Foundation has audited and changed 20 state medical boards to remove intrusive language from licensing applications.
Support for colleagues working to help each other
Dr. Myers: One final note for those physicians who need to take time out for medical leave: In my clinical experience, I find that they felt lonely as they were getting well. I can’t tell you how much it made a difference for those who received a phone call, a card, or an email from their colleagues at work. It doesn’t take long for a vibrant, active physician to feel out of the loop when ill.
We know from suicide literature that when somebody’s discharged from the hospital or the emergency department, caring communications, brief expressions of care and concern by email, letter, card, text message, etc., can make all the difference to their recovery. Reaching out to those struggling and those in recovery can help your fellow physician.
A version of this article originally appeared on Medscape.com.
Can a puff of cool air up the nose stop acute migraine?
AUSTIN, TEX. – , according to the results of a small study. Most patients reported relief of their symptoms after receiving 15 minutes of transnasal evaporative cooling, without any need for rescue medication.
The cooling may modulate the sphenopalatine ganglion, a large ganglion implicated in migraine, said lead author Larry Charleston IV, MD, director of the headache and facial pain division, and professor of neurology at Michigan State University, East Lansing.
“The transnasal evaporative cooling device cools by blowing dry, ambient air across the nasal turbinates and may work by neuromodulation via the sphenopalatine ganglion for migraine,” Dr. Charleston said.
The findings were presented at the annual meeting of the American Headache Society.
A ‘cool’ approach to migraine treatment
“Everyone who has migraine disease needs abortive treatment,” Dr. Charleston said. “There is a need for safe and effective acute treatment for migraine. As we understand more about the pathophysiology of migraine, we learn that peripheral input plays a role in migraine disease.
“I was excited to learn of the device and to learn how we might take advantage of our knowledge of the sphenopalatine ganglia in the treatment of migraine, and was very enthusiastic to be involved in researching a nonpharmacological treatment to abort migraine attacks,” he said. “I thought this approach to migraine treatment was really ‘cool.’ ”
Twenty-four patients who met diagnostic criteria for episodic migraine with or without aura were randomized to receive 15 minutes of cooling induced by the CoolStat Transnasal Thermal Regulating Device (CoolTech LLC), or to a sham treatment with a CoolStat sham device.
Participants receiving active treatment were further randomized to receive one of the following flow rates: 24 liters per minute (LPM; n = 6 patients), 18 LPM (n = 9 patients), and 6 LPM (n = 9 patients).
All patients were instructed to get to their headache clinic during a migraine attack to start treatment.
The researchers looked at pain levels and most bothersome symptoms at baseline, and then at 2 and 24 hours after treatment. The primary endpoint was pain relief at 2 hours. Other endpoints included tolerability, relief from most bothersome symptoms, and freedom from pain at 2 hours.
The results showed that 88% (8/9 patients) of the 6-LPM group reported pain relief at 2 hours. Of these, 44% (4/9) reported being pain free at 2 hours, all without need for rescue medication. Similarly, pain relief at 2 hours occurred in 44% (4/9) of patients in the 18-LPM group, and in 50% (3/6) of the patients in the 24-LPM group.
No participants in the 18-LPM or the 24-LPM groups reported pain freedom at 2 hours.
Most bothersome symptoms were reduced. Response was greater with 6-LPM treatment. At 2 hours, 77% (7/9) of patients in the 6-LPM group reported relief of their symptoms, followed by 66% (6/9) of the 18-LPM group and 50% (3/6) of the 24-LPM group.
However, nasal discomfort was a bothersome adverse effect, Dr. Charleston noted. The rate of nasal discomfort occurred in all groups but was lower in the 6-LPM group.
Moderate intranasal discomfort during treatment was reported by 11% of the 6-LPM group, compared with 33% (3/9) in the 18-LPM group and 83% (5/6) in the 24-LPM group.
However, the study was terminated due to insufficient subject accrual rate.
“Originally, 87 participants were recruited and consented. It may have been challenging for some to come in to study clinic sites for the study treatment at the onset of their migraine attacks. The next iteration of the treatment device is a more portable model and study treatment may be used at home. This will likely be more convenient and enhance study participation,” Dr. Charleston said.
The data in the current study will help inform dose ranging analyses in future studies, to optimize efficacy and increase tolerability, he added.
The findings are promising and merit further assessment in a larger study with a sham control group, said Richard B. Lipton, MD, Edwin S. Lowe Professor and vice chair of neurology, and director of the Montefiore Headache Center, Albert Einstein College of Medicine, New York.
“Charleston et al. report that the lowest flow dose (6 liters per minute) was most effective, with a 2-hour pain-relief rate of 88% and a 2-hour pain-free rate of 50%, but, though these rates of pain relief and pain freedom are high, caution in interpretation is required,” Dr. Lipton said.
“The sample size is very modest with only nine patients in the 6-liter-per-minute treatment arm. In addition, the study lacks results from the group that got the sham device, making it difficult to contextualize the findings,” Dr. Lipton said.
He added that it is unusual for higher doses to be less effective but that may be because air flow higher than 6 LPM is irritating to the nasal mucosa during migraine attacks.
Always a need for effective nonpharmaceuticals
Also commenting on this study, Nina Riggins, MD, director of the Headache Center at the University of California, San Diego, said she found the novel device “exciting and really clever.
“I really enjoyed reviewing this abstract because I am a big fan of sphenopalatine ganglion block in the palatine ganglion. When we do those, we basically apply numbing medication to decrease the sensation and discharges coming from this group of neural cells in order to decrease pain,” Dr. Riggins said. “The procedure is very well tolerated and usually sphenopalatine ganglion blocks are used in patients when we do not want any side effects, such as in pregnant and postpartum women.”
The novel technique has the potential to have fewer side effects than those of oral medications, she said. “For example, the triptans are effective drugs but they constrict the blood vessels and we don’t want to use them in people with heart disease or history of stroke. This is where these potentially safer devices can play an important role. We can have more options to offer our patients,” Dr. Riggins said.
“I am super excited and looking forward to see what will come out of future research. I am really grateful that the authors are looking into new neuromodulation devices which can be so useful,” she said.
Migraine is the second leading cause of disability worldwide, Dr. Riggins noted. “It peaks in the years when people are most productive and affects families and communities. Medications are good, of course, but now with these novel devices, these are wonderful areas for research. Also now, we can offer so much more to people with migraine and other headache disorders,” she said.
“When I started in the field, I remember we were very limited in resources, and now, it’s just so wonderful.”
The study was sponsored by CoolTech Corp LLC. Dr. Charleston reports financial relationships with Allergan/AbbVie, Amgen, Amneal, Biohaven, Haleon, Linpharma, Satsuma, and Teva, and that he has received CME honoraria from the American Headache Society and the American Academy of Neurology. Dr. Lipton reports financial relationships with multiple pharmaceutical companies. Dr. Riggins reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AUSTIN, TEX. – , according to the results of a small study. Most patients reported relief of their symptoms after receiving 15 minutes of transnasal evaporative cooling, without any need for rescue medication.
The cooling may modulate the sphenopalatine ganglion, a large ganglion implicated in migraine, said lead author Larry Charleston IV, MD, director of the headache and facial pain division, and professor of neurology at Michigan State University, East Lansing.
“The transnasal evaporative cooling device cools by blowing dry, ambient air across the nasal turbinates and may work by neuromodulation via the sphenopalatine ganglion for migraine,” Dr. Charleston said.
The findings were presented at the annual meeting of the American Headache Society.
A ‘cool’ approach to migraine treatment
“Everyone who has migraine disease needs abortive treatment,” Dr. Charleston said. “There is a need for safe and effective acute treatment for migraine. As we understand more about the pathophysiology of migraine, we learn that peripheral input plays a role in migraine disease.
“I was excited to learn of the device and to learn how we might take advantage of our knowledge of the sphenopalatine ganglia in the treatment of migraine, and was very enthusiastic to be involved in researching a nonpharmacological treatment to abort migraine attacks,” he said. “I thought this approach to migraine treatment was really ‘cool.’ ”
Twenty-four patients who met diagnostic criteria for episodic migraine with or without aura were randomized to receive 15 minutes of cooling induced by the CoolStat Transnasal Thermal Regulating Device (CoolTech LLC), or to a sham treatment with a CoolStat sham device.
Participants receiving active treatment were further randomized to receive one of the following flow rates: 24 liters per minute (LPM; n = 6 patients), 18 LPM (n = 9 patients), and 6 LPM (n = 9 patients).
All patients were instructed to get to their headache clinic during a migraine attack to start treatment.
The researchers looked at pain levels and most bothersome symptoms at baseline, and then at 2 and 24 hours after treatment. The primary endpoint was pain relief at 2 hours. Other endpoints included tolerability, relief from most bothersome symptoms, and freedom from pain at 2 hours.
The results showed that 88% (8/9 patients) of the 6-LPM group reported pain relief at 2 hours. Of these, 44% (4/9) reported being pain free at 2 hours, all without need for rescue medication. Similarly, pain relief at 2 hours occurred in 44% (4/9) of patients in the 18-LPM group, and in 50% (3/6) of the patients in the 24-LPM group.
No participants in the 18-LPM or the 24-LPM groups reported pain freedom at 2 hours.
Most bothersome symptoms were reduced. Response was greater with 6-LPM treatment. At 2 hours, 77% (7/9) of patients in the 6-LPM group reported relief of their symptoms, followed by 66% (6/9) of the 18-LPM group and 50% (3/6) of the 24-LPM group.
However, nasal discomfort was a bothersome adverse effect, Dr. Charleston noted. The rate of nasal discomfort occurred in all groups but was lower in the 6-LPM group.
Moderate intranasal discomfort during treatment was reported by 11% of the 6-LPM group, compared with 33% (3/9) in the 18-LPM group and 83% (5/6) in the 24-LPM group.
However, the study was terminated due to insufficient subject accrual rate.
“Originally, 87 participants were recruited and consented. It may have been challenging for some to come in to study clinic sites for the study treatment at the onset of their migraine attacks. The next iteration of the treatment device is a more portable model and study treatment may be used at home. This will likely be more convenient and enhance study participation,” Dr. Charleston said.
The data in the current study will help inform dose ranging analyses in future studies, to optimize efficacy and increase tolerability, he added.
The findings are promising and merit further assessment in a larger study with a sham control group, said Richard B. Lipton, MD, Edwin S. Lowe Professor and vice chair of neurology, and director of the Montefiore Headache Center, Albert Einstein College of Medicine, New York.
“Charleston et al. report that the lowest flow dose (6 liters per minute) was most effective, with a 2-hour pain-relief rate of 88% and a 2-hour pain-free rate of 50%, but, though these rates of pain relief and pain freedom are high, caution in interpretation is required,” Dr. Lipton said.
“The sample size is very modest with only nine patients in the 6-liter-per-minute treatment arm. In addition, the study lacks results from the group that got the sham device, making it difficult to contextualize the findings,” Dr. Lipton said.
He added that it is unusual for higher doses to be less effective but that may be because air flow higher than 6 LPM is irritating to the nasal mucosa during migraine attacks.
Always a need for effective nonpharmaceuticals
Also commenting on this study, Nina Riggins, MD, director of the Headache Center at the University of California, San Diego, said she found the novel device “exciting and really clever.
“I really enjoyed reviewing this abstract because I am a big fan of sphenopalatine ganglion block in the palatine ganglion. When we do those, we basically apply numbing medication to decrease the sensation and discharges coming from this group of neural cells in order to decrease pain,” Dr. Riggins said. “The procedure is very well tolerated and usually sphenopalatine ganglion blocks are used in patients when we do not want any side effects, such as in pregnant and postpartum women.”
The novel technique has the potential to have fewer side effects than those of oral medications, she said. “For example, the triptans are effective drugs but they constrict the blood vessels and we don’t want to use them in people with heart disease or history of stroke. This is where these potentially safer devices can play an important role. We can have more options to offer our patients,” Dr. Riggins said.
“I am super excited and looking forward to see what will come out of future research. I am really grateful that the authors are looking into new neuromodulation devices which can be so useful,” she said.
Migraine is the second leading cause of disability worldwide, Dr. Riggins noted. “It peaks in the years when people are most productive and affects families and communities. Medications are good, of course, but now with these novel devices, these are wonderful areas for research. Also now, we can offer so much more to people with migraine and other headache disorders,” she said.
“When I started in the field, I remember we were very limited in resources, and now, it’s just so wonderful.”
The study was sponsored by CoolTech Corp LLC. Dr. Charleston reports financial relationships with Allergan/AbbVie, Amgen, Amneal, Biohaven, Haleon, Linpharma, Satsuma, and Teva, and that he has received CME honoraria from the American Headache Society and the American Academy of Neurology. Dr. Lipton reports financial relationships with multiple pharmaceutical companies. Dr. Riggins reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
AUSTIN, TEX. – , according to the results of a small study. Most patients reported relief of their symptoms after receiving 15 minutes of transnasal evaporative cooling, without any need for rescue medication.
The cooling may modulate the sphenopalatine ganglion, a large ganglion implicated in migraine, said lead author Larry Charleston IV, MD, director of the headache and facial pain division, and professor of neurology at Michigan State University, East Lansing.
“The transnasal evaporative cooling device cools by blowing dry, ambient air across the nasal turbinates and may work by neuromodulation via the sphenopalatine ganglion for migraine,” Dr. Charleston said.
The findings were presented at the annual meeting of the American Headache Society.
A ‘cool’ approach to migraine treatment
“Everyone who has migraine disease needs abortive treatment,” Dr. Charleston said. “There is a need for safe and effective acute treatment for migraine. As we understand more about the pathophysiology of migraine, we learn that peripheral input plays a role in migraine disease.
“I was excited to learn of the device and to learn how we might take advantage of our knowledge of the sphenopalatine ganglia in the treatment of migraine, and was very enthusiastic to be involved in researching a nonpharmacological treatment to abort migraine attacks,” he said. “I thought this approach to migraine treatment was really ‘cool.’ ”
Twenty-four patients who met diagnostic criteria for episodic migraine with or without aura were randomized to receive 15 minutes of cooling induced by the CoolStat Transnasal Thermal Regulating Device (CoolTech LLC), or to a sham treatment with a CoolStat sham device.
Participants receiving active treatment were further randomized to receive one of the following flow rates: 24 liters per minute (LPM; n = 6 patients), 18 LPM (n = 9 patients), and 6 LPM (n = 9 patients).
All patients were instructed to get to their headache clinic during a migraine attack to start treatment.
The researchers looked at pain levels and most bothersome symptoms at baseline, and then at 2 and 24 hours after treatment. The primary endpoint was pain relief at 2 hours. Other endpoints included tolerability, relief from most bothersome symptoms, and freedom from pain at 2 hours.
The results showed that 88% (8/9 patients) of the 6-LPM group reported pain relief at 2 hours. Of these, 44% (4/9) reported being pain free at 2 hours, all without need for rescue medication. Similarly, pain relief at 2 hours occurred in 44% (4/9) of patients in the 18-LPM group, and in 50% (3/6) of the patients in the 24-LPM group.
No participants in the 18-LPM or the 24-LPM groups reported pain freedom at 2 hours.
Most bothersome symptoms were reduced. Response was greater with 6-LPM treatment. At 2 hours, 77% (7/9) of patients in the 6-LPM group reported relief of their symptoms, followed by 66% (6/9) of the 18-LPM group and 50% (3/6) of the 24-LPM group.
However, nasal discomfort was a bothersome adverse effect, Dr. Charleston noted. The rate of nasal discomfort occurred in all groups but was lower in the 6-LPM group.
Moderate intranasal discomfort during treatment was reported by 11% of the 6-LPM group, compared with 33% (3/9) in the 18-LPM group and 83% (5/6) in the 24-LPM group.
However, the study was terminated due to insufficient subject accrual rate.
“Originally, 87 participants were recruited and consented. It may have been challenging for some to come in to study clinic sites for the study treatment at the onset of their migraine attacks. The next iteration of the treatment device is a more portable model and study treatment may be used at home. This will likely be more convenient and enhance study participation,” Dr. Charleston said.
The data in the current study will help inform dose ranging analyses in future studies, to optimize efficacy and increase tolerability, he added.
The findings are promising and merit further assessment in a larger study with a sham control group, said Richard B. Lipton, MD, Edwin S. Lowe Professor and vice chair of neurology, and director of the Montefiore Headache Center, Albert Einstein College of Medicine, New York.
“Charleston et al. report that the lowest flow dose (6 liters per minute) was most effective, with a 2-hour pain-relief rate of 88% and a 2-hour pain-free rate of 50%, but, though these rates of pain relief and pain freedom are high, caution in interpretation is required,” Dr. Lipton said.
“The sample size is very modest with only nine patients in the 6-liter-per-minute treatment arm. In addition, the study lacks results from the group that got the sham device, making it difficult to contextualize the findings,” Dr. Lipton said.
He added that it is unusual for higher doses to be less effective but that may be because air flow higher than 6 LPM is irritating to the nasal mucosa during migraine attacks.
Always a need for effective nonpharmaceuticals
Also commenting on this study, Nina Riggins, MD, director of the Headache Center at the University of California, San Diego, said she found the novel device “exciting and really clever.
“I really enjoyed reviewing this abstract because I am a big fan of sphenopalatine ganglion block in the palatine ganglion. When we do those, we basically apply numbing medication to decrease the sensation and discharges coming from this group of neural cells in order to decrease pain,” Dr. Riggins said. “The procedure is very well tolerated and usually sphenopalatine ganglion blocks are used in patients when we do not want any side effects, such as in pregnant and postpartum women.”
The novel technique has the potential to have fewer side effects than those of oral medications, she said. “For example, the triptans are effective drugs but they constrict the blood vessels and we don’t want to use them in people with heart disease or history of stroke. This is where these potentially safer devices can play an important role. We can have more options to offer our patients,” Dr. Riggins said.
“I am super excited and looking forward to see what will come out of future research. I am really grateful that the authors are looking into new neuromodulation devices which can be so useful,” she said.
Migraine is the second leading cause of disability worldwide, Dr. Riggins noted. “It peaks in the years when people are most productive and affects families and communities. Medications are good, of course, but now with these novel devices, these are wonderful areas for research. Also now, we can offer so much more to people with migraine and other headache disorders,” she said.
“When I started in the field, I remember we were very limited in resources, and now, it’s just so wonderful.”
The study was sponsored by CoolTech Corp LLC. Dr. Charleston reports financial relationships with Allergan/AbbVie, Amgen, Amneal, Biohaven, Haleon, Linpharma, Satsuma, and Teva, and that he has received CME honoraria from the American Headache Society and the American Academy of Neurology. Dr. Lipton reports financial relationships with multiple pharmaceutical companies. Dr. Riggins reports no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
At ASH 2023
New data on traumatic brain injury show it’s chronic, evolving
The data show that patients with TBI may continue to improve or decline during a period of up to 7 years after injury, making it more of a chronic condition, the investigators report.
“Our results dispute the notion that TBI is a discrete, isolated medical event with a finite, static functional outcome following a relatively short period of upward recovery (typically up to 1 year),” Benjamin Brett, PhD, assistant professor, departments of neurosurgery and neurology, Medical College of Wisconsin, Milwaukee, told this news organization.
“Rather, individuals continue to exhibit improvement and decline across a range of domains, including psychiatric, cognitive, and functional outcomes, even 2-7 years after their injury,” Dr. Brett said.
“Ultimately, our findings support conceptualizing TBI as a chronic condition for many patients, which requires routine follow-up, medical monitoring, responsive care, and support, adapting to their evolving needs many years following injury,” he said.
Results of the TRACK TBI LONG (Transforming Research and Clinical Knowledge in TBI Longitudinal study) were published online in Neurology.
Chronic and evolving
The results are based on 1,264 adults (mean age at injury, 41 years) from the initial TRACK TBI study, including 917 with mild TBI (mTBI) and 193 with moderate/severe TBI (msTBI), who were matched to 154 control patients who had experienced orthopedic trauma without evidence of head injury (OTC).
The participants were followed annually for up to 7 years after injury using the Glasgow Outcome Scale–Extended (GOSE), Brief Symptom Inventory–18 (BSI), and the Brief Test of Adult Cognition by Telephone (BTACT), as well as a self-reported perception of function. The researchers calculated rates of change (classified as stable, improved, or declined) for individual outcomes at each long-term follow-up.
In general, “stable” was the most frequent change outcome for the individual measures from postinjury baseline assessment to 7 years post injury.
However, a substantial proportion of patients with TBI (regardless of severity) experienced changes in psychiatric status, cognition, and functional outcomes over the years.
When the GOSE, BSI, and BTACT were considered collectively, rates of decline were 21% for mTBI, 26% for msTBI, and 15% for OTC.
The highest rates of decline were in functional outcomes (GOSE scores). On average, over the course of 2-7 years post injury, 29% of patients with mTBI and 23% of those with msTBI experienced a decline in the ability to function with daily activities.
A pattern of improvement on the GOSE was noted in 36% of patients with msTBI and 22% patients with mTBI.
Notably, said Dr. Brett, patients who experienced greater difficulties near the time of injury showed improvement for a period of 2-7 years post injury. Patient factors, such as older age at the time of the injury, were associated with greater risk of long-term decline.
“Our findings highlight the need to embrace conceptualization of TBI as a chronic condition in order to establish systems of care that provide continued follow-up with treatment and supports that adapt to evolving patient needs, regardless of the directions of change,” Dr. Brett told this news organization.
Important and novel work
In a linked editorial, Robynne Braun, MD, PhD, with the department of neurology, University of Maryland, Baltimore, notes that there have been “few prospective studies examining postinjury outcomes on this longer timescale, especially in mild TBI, making this an important and novel body of work.”
The study “effectively demonstrates that changes in function across multiple domains continue to occur well beyond the conventionally tracked 6- to 12-month period of injury recovery,” Dr. Braun writes.
The observation that over the 7-year follow-up, a substantial proportion of patients with mTBI and msTBI exhibited a pattern of decline on the GOSE suggests that they “may have needed more ongoing medical monitoring, rehabilitation, or supportive services to prevent worsening,” Dr. Braun adds.
At the same time, the improvement pattern on the GOSE suggests “opportunities for recovery that further rehabilitative or medical services might have enhanced.”
The study was funded by the National Institute of Neurological Disorders and Stroke, the National Institute on Aging, the National Football League Scientific Advisory Board, and the U.S. Department of Defense. Dr. Brett and Dr. Braun have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
The data show that patients with TBI may continue to improve or decline during a period of up to 7 years after injury, making it more of a chronic condition, the investigators report.
“Our results dispute the notion that TBI is a discrete, isolated medical event with a finite, static functional outcome following a relatively short period of upward recovery (typically up to 1 year),” Benjamin Brett, PhD, assistant professor, departments of neurosurgery and neurology, Medical College of Wisconsin, Milwaukee, told this news organization.
“Rather, individuals continue to exhibit improvement and decline across a range of domains, including psychiatric, cognitive, and functional outcomes, even 2-7 years after their injury,” Dr. Brett said.
“Ultimately, our findings support conceptualizing TBI as a chronic condition for many patients, which requires routine follow-up, medical monitoring, responsive care, and support, adapting to their evolving needs many years following injury,” he said.
Results of the TRACK TBI LONG (Transforming Research and Clinical Knowledge in TBI Longitudinal study) were published online in Neurology.
Chronic and evolving
The results are based on 1,264 adults (mean age at injury, 41 years) from the initial TRACK TBI study, including 917 with mild TBI (mTBI) and 193 with moderate/severe TBI (msTBI), who were matched to 154 control patients who had experienced orthopedic trauma without evidence of head injury (OTC).
The participants were followed annually for up to 7 years after injury using the Glasgow Outcome Scale–Extended (GOSE), Brief Symptom Inventory–18 (BSI), and the Brief Test of Adult Cognition by Telephone (BTACT), as well as a self-reported perception of function. The researchers calculated rates of change (classified as stable, improved, or declined) for individual outcomes at each long-term follow-up.
In general, “stable” was the most frequent change outcome for the individual measures from postinjury baseline assessment to 7 years post injury.
However, a substantial proportion of patients with TBI (regardless of severity) experienced changes in psychiatric status, cognition, and functional outcomes over the years.
When the GOSE, BSI, and BTACT were considered collectively, rates of decline were 21% for mTBI, 26% for msTBI, and 15% for OTC.
The highest rates of decline were in functional outcomes (GOSE scores). On average, over the course of 2-7 years post injury, 29% of patients with mTBI and 23% of those with msTBI experienced a decline in the ability to function with daily activities.
A pattern of improvement on the GOSE was noted in 36% of patients with msTBI and 22% patients with mTBI.
Notably, said Dr. Brett, patients who experienced greater difficulties near the time of injury showed improvement for a period of 2-7 years post injury. Patient factors, such as older age at the time of the injury, were associated with greater risk of long-term decline.
“Our findings highlight the need to embrace conceptualization of TBI as a chronic condition in order to establish systems of care that provide continued follow-up with treatment and supports that adapt to evolving patient needs, regardless of the directions of change,” Dr. Brett told this news organization.
Important and novel work
In a linked editorial, Robynne Braun, MD, PhD, with the department of neurology, University of Maryland, Baltimore, notes that there have been “few prospective studies examining postinjury outcomes on this longer timescale, especially in mild TBI, making this an important and novel body of work.”
The study “effectively demonstrates that changes in function across multiple domains continue to occur well beyond the conventionally tracked 6- to 12-month period of injury recovery,” Dr. Braun writes.
The observation that over the 7-year follow-up, a substantial proportion of patients with mTBI and msTBI exhibited a pattern of decline on the GOSE suggests that they “may have needed more ongoing medical monitoring, rehabilitation, or supportive services to prevent worsening,” Dr. Braun adds.
At the same time, the improvement pattern on the GOSE suggests “opportunities for recovery that further rehabilitative or medical services might have enhanced.”
The study was funded by the National Institute of Neurological Disorders and Stroke, the National Institute on Aging, the National Football League Scientific Advisory Board, and the U.S. Department of Defense. Dr. Brett and Dr. Braun have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
The data show that patients with TBI may continue to improve or decline during a period of up to 7 years after injury, making it more of a chronic condition, the investigators report.
“Our results dispute the notion that TBI is a discrete, isolated medical event with a finite, static functional outcome following a relatively short period of upward recovery (typically up to 1 year),” Benjamin Brett, PhD, assistant professor, departments of neurosurgery and neurology, Medical College of Wisconsin, Milwaukee, told this news organization.
“Rather, individuals continue to exhibit improvement and decline across a range of domains, including psychiatric, cognitive, and functional outcomes, even 2-7 years after their injury,” Dr. Brett said.
“Ultimately, our findings support conceptualizing TBI as a chronic condition for many patients, which requires routine follow-up, medical monitoring, responsive care, and support, adapting to their evolving needs many years following injury,” he said.
Results of the TRACK TBI LONG (Transforming Research and Clinical Knowledge in TBI Longitudinal study) were published online in Neurology.
Chronic and evolving
The results are based on 1,264 adults (mean age at injury, 41 years) from the initial TRACK TBI study, including 917 with mild TBI (mTBI) and 193 with moderate/severe TBI (msTBI), who were matched to 154 control patients who had experienced orthopedic trauma without evidence of head injury (OTC).
The participants were followed annually for up to 7 years after injury using the Glasgow Outcome Scale–Extended (GOSE), Brief Symptom Inventory–18 (BSI), and the Brief Test of Adult Cognition by Telephone (BTACT), as well as a self-reported perception of function. The researchers calculated rates of change (classified as stable, improved, or declined) for individual outcomes at each long-term follow-up.
In general, “stable” was the most frequent change outcome for the individual measures from postinjury baseline assessment to 7 years post injury.
However, a substantial proportion of patients with TBI (regardless of severity) experienced changes in psychiatric status, cognition, and functional outcomes over the years.
When the GOSE, BSI, and BTACT were considered collectively, rates of decline were 21% for mTBI, 26% for msTBI, and 15% for OTC.
The highest rates of decline were in functional outcomes (GOSE scores). On average, over the course of 2-7 years post injury, 29% of patients with mTBI and 23% of those with msTBI experienced a decline in the ability to function with daily activities.
A pattern of improvement on the GOSE was noted in 36% of patients with msTBI and 22% patients with mTBI.
Notably, said Dr. Brett, patients who experienced greater difficulties near the time of injury showed improvement for a period of 2-7 years post injury. Patient factors, such as older age at the time of the injury, were associated with greater risk of long-term decline.
“Our findings highlight the need to embrace conceptualization of TBI as a chronic condition in order to establish systems of care that provide continued follow-up with treatment and supports that adapt to evolving patient needs, regardless of the directions of change,” Dr. Brett told this news organization.
Important and novel work
In a linked editorial, Robynne Braun, MD, PhD, with the department of neurology, University of Maryland, Baltimore, notes that there have been “few prospective studies examining postinjury outcomes on this longer timescale, especially in mild TBI, making this an important and novel body of work.”
The study “effectively demonstrates that changes in function across multiple domains continue to occur well beyond the conventionally tracked 6- to 12-month period of injury recovery,” Dr. Braun writes.
The observation that over the 7-year follow-up, a substantial proportion of patients with mTBI and msTBI exhibited a pattern of decline on the GOSE suggests that they “may have needed more ongoing medical monitoring, rehabilitation, or supportive services to prevent worsening,” Dr. Braun adds.
At the same time, the improvement pattern on the GOSE suggests “opportunities for recovery that further rehabilitative or medical services might have enhanced.”
The study was funded by the National Institute of Neurological Disorders and Stroke, the National Institute on Aging, the National Football League Scientific Advisory Board, and the U.S. Department of Defense. Dr. Brett and Dr. Braun have disclosed no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
FROM NEUROLOGY
Myasthenia gravis drug gets FDA nod
, the drug’s manufacturer, UCB, has announced.
Rozanolixizumab is a subcutaneous-infused humanized IgG4 monoclonal antibody that binds to the neonatal Fc receptor (FcRn), reducing the concentration of pathogenic IgG autoantibodies.
U.S. approval is based on results of the phase 3 MycarinG study involving 200 patients with AChR or MuSK autoantibody-positive gMG. Patients were randomly assigned to one of two rozanolixizumab groups (7 mg/kg or 10 mg/kg) or placebo for 6 weeks.
As reported last month in Lancet Neurology, rozanolixizumab led to statistically significant improvements in gMG-specific outcomes, including everyday activities such as breathing, talking, swallowing, and being able to rise from a chair.
“There is a significant need for new, innovative treatment options to reduce the day-to-day burden of gMG,” lead investigator Vera Bril, MD, professor of medicine (neurology), University of Toronto, said in a news release.
Rozanolixizumab is “a new treatment option, targeting one of the mechanisms of disease to provide symptom improvement in patient- and physician-reported outcomes at day 43,” Dr. Bril added.
The most common adverse reactions (reported in at least 10% of patients treated with rozanolixizumab) were headache, infections, diarrhea, pyrexia, hypersensitivity reactions, and nausea.
The company expects rozanolixizumab to be available in the United States during the third quarter of 2023.
The FDA granted the application for rozanolixizumab in gMG priority review.
A version of this article first appeared on Medscape.com.
, the drug’s manufacturer, UCB, has announced.
Rozanolixizumab is a subcutaneous-infused humanized IgG4 monoclonal antibody that binds to the neonatal Fc receptor (FcRn), reducing the concentration of pathogenic IgG autoantibodies.
U.S. approval is based on results of the phase 3 MycarinG study involving 200 patients with AChR or MuSK autoantibody-positive gMG. Patients were randomly assigned to one of two rozanolixizumab groups (7 mg/kg or 10 mg/kg) or placebo for 6 weeks.
As reported last month in Lancet Neurology, rozanolixizumab led to statistically significant improvements in gMG-specific outcomes, including everyday activities such as breathing, talking, swallowing, and being able to rise from a chair.
“There is a significant need for new, innovative treatment options to reduce the day-to-day burden of gMG,” lead investigator Vera Bril, MD, professor of medicine (neurology), University of Toronto, said in a news release.
Rozanolixizumab is “a new treatment option, targeting one of the mechanisms of disease to provide symptom improvement in patient- and physician-reported outcomes at day 43,” Dr. Bril added.
The most common adverse reactions (reported in at least 10% of patients treated with rozanolixizumab) were headache, infections, diarrhea, pyrexia, hypersensitivity reactions, and nausea.
The company expects rozanolixizumab to be available in the United States during the third quarter of 2023.
The FDA granted the application for rozanolixizumab in gMG priority review.
A version of this article first appeared on Medscape.com.
, the drug’s manufacturer, UCB, has announced.
Rozanolixizumab is a subcutaneous-infused humanized IgG4 monoclonal antibody that binds to the neonatal Fc receptor (FcRn), reducing the concentration of pathogenic IgG autoantibodies.
U.S. approval is based on results of the phase 3 MycarinG study involving 200 patients with AChR or MuSK autoantibody-positive gMG. Patients were randomly assigned to one of two rozanolixizumab groups (7 mg/kg or 10 mg/kg) or placebo for 6 weeks.
As reported last month in Lancet Neurology, rozanolixizumab led to statistically significant improvements in gMG-specific outcomes, including everyday activities such as breathing, talking, swallowing, and being able to rise from a chair.
“There is a significant need for new, innovative treatment options to reduce the day-to-day burden of gMG,” lead investigator Vera Bril, MD, professor of medicine (neurology), University of Toronto, said in a news release.
Rozanolixizumab is “a new treatment option, targeting one of the mechanisms of disease to provide symptom improvement in patient- and physician-reported outcomes at day 43,” Dr. Bril added.
The most common adverse reactions (reported in at least 10% of patients treated with rozanolixizumab) were headache, infections, diarrhea, pyrexia, hypersensitivity reactions, and nausea.
The company expects rozanolixizumab to be available in the United States during the third quarter of 2023.
The FDA granted the application for rozanolixizumab in gMG priority review.
A version of this article first appeared on Medscape.com.